Community Mental Health Teams (CMHTs) are at the heart of the modern mental health service. Stress among the staff of these teams is a concern both in its own right as an occupational health issue and also because it is likely to have a detrimental effect on the functioning of a team. Mental health nurses have been found to experience greater stress in community settings than their hospital-based colleagues (Reference Carson, Leary and De VilliersCarson et al, 1995; Reference Prosser, Johnson and KuipersProsser et al, 1996). Patient suicide is a significant contributor to staff stress. It has been shown to affect adversely the health and well-being of consultant psychiatrists (Reference Alexander, Klein and GrayAlexander et al, 2000), psychiatric trainees (Reference Dewar, Eagles and KleinDewar et al, 2000), clinical psychologists (Reference Bucknall and UnsworthBucknall & Unsworth, 1997) and nurses (Reference CooperCooper, 1995), with some staff displaying symptoms of depression, anxiety and post-traumatic stress disorder.
A patient's suicide can adversely affect not only the individual staff members but also the functioning of a unit, such as a psychiatric ward, in which the staff member works (Reference Kayton and FreedKayton & Freed, 1967). In a similar way a suicide by a patient may have a detrimental effect on a CMHT as a whole. Although there have been many studies of the effects of a suicide on individual professional groups, there have been none on multi-disciplinary CMHTs. Studies of this kind may be of value because they indicate the type of support that could be helpful for such teams in order to reduce the adverse impact of disturbing events such as a patient suicide.
The present study aimed to investigate the effect of patient suicide on the members of multi-disciplinary CMHTs in inner-city London.
The study
All 77 members of five CMHTs were sent confidential questionnaires. The CMHTs covered the London Borough of Islington, which is an inner-city area with high levels of social deprivation and mental health problems. The questionnaire was based closely on that used by Alexander et al (Reference Alexander, Klein and Gray2000) in their study of consultant psychiatrists' responses to suicide. The questionnaire was adapted for a multi-disciplinary group. The questionnaire had two sections: the first asked about personal non-identifying information and the second asked about the ‘most distressing’ suicide. There was also space for free text responses, and additional comments were invited. The questionnaires were administered and analysed by two trainee clinical psychologists who had no other connection with the service (J.W. and S.D.), which helped to preserve the anonymity of the responses.
Results
Forty-four completed questionnaires were received (a response rate of 57%). Some staff were absent during the data collection period so we cannot be certain that all team members received their copy of the questionnaire. This may account for the rather low response rate. Twenty-eight of the respondents were female, 14 were male and two did not complete that item of the questionnaire. The majority of the respondents were either community psychiatric nurses (18) or social workers (15). Of the remainder, two were psychiatrists, four were clinical psychologists, two were occupational therapists, two were managers and one was an administrator. The mean number of years since qualification was 12.9 (s.d.=9.2) and the mean number of years in the current post was 3.8 (s.d.=4.7).
Thirty-eight (86%) of the respondents reported that they had experienced at least one patient suicide in their career, with an average of 4.2 (s.d.=5.1) suicides. Twenty-eight team members (64%) had experienced a patient suicide in their current job.
The effects of a patient's suicide
Staff were asked about the effects of the most distressing suicide. Many of the respondents reported that it had a noticeable impact on both their personal and professional lives (see Table 1).
Table 1. Impact of patient suicide on community mental health team staff

| No response | No impact | Some impact | Great impact | |
|---|---|---|---|---|
| How would you rate the impact that the suicide had on your personal life? | 3 | 6 | 19 | 10 |
| How would you rate the impact that the suicide had on your professional life? | 3 | 3 | 23 | 9 |
Staff reported experiencing a range of symptoms and emotions following a patient's suicide (see Table 2). Some of these symptoms were transient, however 15 (40%) acknowledged symptoms that persisted for over 1 month. The effects on professional life also were long-lasting and 17 (45%) reported adverse effects lasting longer than 1 month. Some of these effects were serious enough to influence professional behaviour in negative ways, such as avoiding clients who abuse alcohol and drugs, increased anxiety at work, irritability with employers, increased distance between self and clients and an increased desire to change jobs. A small number of staff, however, reported positive effects such as improved notekeeping and an increased likelihood to seek support and peer supervision from colleagues. Only three respondents (7%) took time off work following a patient's death.
Table 2. Adverse effects of patient suicide on community mental health team staff

| Effects on personal life | Effects on professional life |
|---|---|
| Grief/sadness (4) | Self-doubt (3) |
| Preoccupation with work (2) | Anxiety of work (5) |
| Self-doubt/uncertainty (2) | Avoidance of clients perceived as at risk (2) |
| Disturbed sleep (1) | Irritable with institution (1) |
| Poor concentration (1) | Overresponsible attitude towards patients (1) |
| Decreased appetite (1) | Increased desire to change job (1) |
| Becoming tired/apathetic (1) | Increased workload (1) |
| Distancing from clients (1) |
Support following a suicide
Staff were asked what ‘support’ meant to them. Twenty-three of the respondents defined support primarily as having time to talk and having someone to listen. Six appreciated skilled supervision on the case, five felt that receiving acknowledgement of the impact of the event was important while not being blamed and four valued having time off.
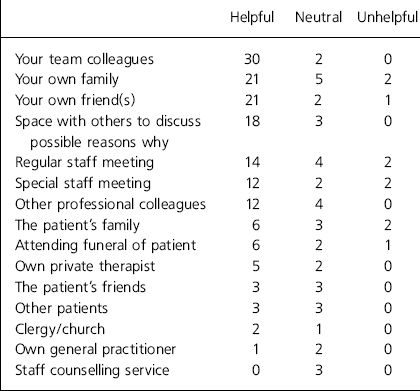
The most common source of support was from immediate colleagues, followed by partners, friends and family (see Table 3). Where special staff meetings to discuss the suicide and provide support were held, they were generally viewed as being of value, but there was some comment that they must be handled carefully. Staff closely involved with clients who have killed themselves often feel judged and vulnerable to criticism. In this context, official enquiries into the background on the suicide were viewed equivocally. Although an attempt to gain an understanding of the suicide and learn from it was valued, there was considerable unease about the manner in which formal investigative enquiries are conducted.
Table 3. Sources of support utilised following patient suicide
| Helpful | Neutral | Unhelpful | |
|---|---|---|---|
| Your team colleagues | 30 | 2 | 0 |
| Your own family | 21 | 5 | 2 |
| Your own friend(s) | 21 | 2 | 1 |
| Space with others to discuss possible reasons why | 18 | 3 | 0 |
| Regular staff meeting | 14 | 4 | 2 |
| Special staff meeting | 12 | 2 | 2 |
| Other professional colleagues | 12 | 4 | 0 |
| The patient's family | 6 | 3 | 2 |
| Attending funeral of patient | 6 | 2 | 1 |
| Own private therapist | 5 | 2 | 0 |
| The patient's friends | 3 | 3 | 0 |
| Other patients | 3 | 3 | 0 |
| Clergy/church | 2 | 1 | 0 |
| Own general practitioner | 1 | 2 | 0 |
| Staff counselling service | 0 | 3 | 0 |
Thirty staff recommended that in future special meetings to discuss a suicide could be helpful and, most importantly, that senior staff should publicly acknowledge how disturbing a suicide can be for teams and team members. Thirty-one of the respondents, a majority, had felt inadequately prepared for dealing with a suicide by their initial professional training (although they all felt trained in risk assessment) and would welcome further help in this regard. In particular, developing an attitude of acceptance that suicides are likely to happen in CMHT work and that they are not always preventable was thought to be helpful.
Discussion and recommendations
The multi-disciplinary group of staff sampled in this study reported a high incidence of patient suicide during their careers and in their current posts. Although the study sample was small it is clear that, as with other groups of mental health workers, these suicides had a significant detrimental effect on the personal and professional lives of CMHT staff. The incidence of suicide, however, appears to be higher than that reported by consultant psychiatrists (Reference Alexander, Klein and GrayAlexander et al, 2000) and psychiatric trainees (Reference Dewar, Eagles and KleinDewar et al, 2000) and results in a similar degree of distress. This may not, however, reflect a greater number of suicides overall, but is more likely to be a result of multi-disciplinary teamwork in which cases are shared. This sharing of cases makes support from colleagues more possible than working single-handed, but also means that a patient suicide affects a greater number of people. The effect of this can be very uneven. In one of the teams, for example, there had been several suicides in close proximity. One of the patients was well known to all members of the team, whereas the other patients were known to only the particular members of staff who were the patients' key workers. This is a key issue that needs consideration when providing support to a team following a suicide.
There is little published on team support following serious incidents such as suicide. Recommendations for individual support have included discussion with colleagues, attending patients' funerals, detailed case reviews, special staff meetings and training in the likelihood and expectation of suicide as a normal part of the mental health worker's role (as part of initial and ongoing training). All these were confirmed in the present study. Suggestions for team support have included holding special staff meetings and the use of the specific technique of psychological or critical incident stress debriefing (Reference FarringtonFarrington, 1995). This is now considered a controversial technique because in some cases routine psychological debriefing may cause more harm than good. A more appropriate form of intervention is a dedicated team review that focuses on establishing and sharing the facts of the case, normalising individual responses to the situation (by, for example, describing the findings of studies such as this one) and allowing staff to offer support and encouragement to each other. Care must be taken, by an experienced group facilitator, to ensure that the expression of strong emotions such as guilt, shame, fear and grief are contained and normalised, rather than encouraged or explored in depth.
Support by senior members of the team and management was considered by our respondents to be particularly helpful. Dewar et al (Reference Dewar, Eagles and Klein2000) reported that trainee psychiatrists valued the support and guidance of their consultants. Similarly, CMHT members greatly appreciate comments from senior colleagues acknowledging the impact of a suicide. There are often formal enquiries into the background to a suicide and there is a risk that these can add to the trauma for staff if they are not handled sensitively. It is in the interests of good team functioning that the issues of professional responsibility and good practice are highlighted and examined in a context that supports rather than threatens staff, during a time that is already highly stressful with raised personal and professional vulnerability.
Acknowledgement
We are grateful to Professor Paul Bebbington for his helpful comments on an earlier draft of this article.






eLetters
No eLetters have been published for this article.