Vitamin K is an essential cofactor for the carboxylation of glutamic acid residues into γ-carboxyglutamate (Gla) in a limited number of proteins, including plasma prothrombin, plasma pro-coagulants (coagulation factors VII, IX and X) and anticoagulants (proteins C and S), which participate in the coagulation cascade (Shearer, Reference Shearer2000; Institute of Medicine, 2001). In addition, there has been considerable interest in the role of vitamin K in bone metabolism and bone health since the identification of Gla-containing proteins in bone, notably osteocalcin and matrix Gla protein (Binkley & Suttie, Reference Binkley and Suttie1995; Institute of Medicine, 2001; Weber, Reference Weber2001; Bügel, Reference Bügel2003). The dietary reference value for phylloquinone intake of 1 μg/kg per d was based on the maintenance of plasma prothrombin concentration (Department of Health, 1991). However, it has been suggested that the dietary vitamin K intakes needed to maintain normal blood coagulation may be insufficient to cover the requirements for optimal bone metabolism and may thus be suboptimal for bone health (Vermeer et al. Reference Vermeer, Gijsbers, Craciun, Groenen-Van Dooren and Knapen1996; Shearer, Reference Shearer2000). In the USA, the recommendation for vitamin K intake has recently been revised upwards, with the Food and Nutrition Board establishing an adequate intake of 90 and 120 μg phylloquinone/d for women and men, respectively (Institute of Medicine, 2001). A typical European diet is estimated to contain between 80 and 250 μg phylloquinone/d on average (Schurgers et al. Reference Schurgers, Geleijnse, Grobbee, Pols, Hofman, Wittemann and Vermeer1999; Thane et al. Reference Thane, Paul, Bates, Bolton-Smith, Prentice and Shearer2002), which is sufficient to cover the hepatic requirement for the maintenance of normal haemostasis. While the liver has been shown to be the primary target tissue for vitamin K when phylloquinone intakes are low, other tissues in addition accumulate vitamin K at higher intakes (Ronden et al. Reference Ronden, Thijssen and Vermeer1998). It is likely, therefore, that intakes well above current recommendations are required for adequate carboxylation of extrahepatic Gla proteins (Vermeer & Braam, Reference Vermeer and Braam2001).
The circulating concentration of under-(-carboxylated osteocalcin (ucOC), a sensitive marker of vitamin K nutritional status (Sokoll & Sadowski, Reference Sokoll and Sadowski1996), has been reported to be a marker of hip fracture risk (Szulc et al. Reference Szulc, Chapuy, Meunier and Delmas1993; Vergnaud et al. Reference Vergnaud, Garnero, Meunier, Breart, Kamihagi and Delmas1997; Booth et al. Reference Booth, Tucker and Chen2000) and a predictor of bone mineral density (BMD) and bone turnover (Szulc et al. Reference Szulc, Arlot, Chapuy, Duboeuf, Muenier and Delmas1994; Institute of Medicine, 2001; Weber, Reference Weber2001). Moreover, the findings of two large prospective cohort studies, the Nurses' Health Study (Feskanich et al. Reference Feskanich, Weber, Willett, Rockett, Booth and Colditz1999) and the Framingham Heart Study (Booth et al. Reference Booth, Tucker and Chen2000), support an association between relative risk of hip fracture and vitamin K intake. Booth et al. (Reference Booth, Broe, Gagnon, Tucker, Hannan, McLean, Dawson-Hughes, Wilson, Cupples and Kiel2003) reported that adult women (from the Framingham Heart Study) in the lowest quartile of vitamin K intake ( < 70 μg/d) had significantly lower (P < 0·005) mean BMD than did those in the highest quartile of vitamin K intake (309 μg/d), an association which was not evident in men. However, one consistent criticism of such epidemiological data is the difficulty in excluding a confounding effect of overall poor nutrition rather than a specific deficit of vitamin K (Binkley & Suttie, Reference Binkley and Suttie1995). Furthermore, the mechanism of action of vitamin K on BMD and fracture remains unclear. Booth et al. (Reference Booth, Lichtenstein, O'Brien-Morse, McKeown, Wood, Saltzman and Gundberg2001) showed that 15 d of dietary vitamin K depletion led to an increased rate of bone turnover as assessed by serum total osteocalcin (tOC) and urinary type I collagen cross-linked N-telopeptides (NTx); these markers were subsequently normalised by 10 d of phylloquinone repletion (about 200 μg/d). Binkley et al. (Reference Binkley, Krueger, Engelke, Foley and Suttie2000) showed that supplementation with 1 mg phylloquinone for 2 weeks reduced serum tOC but did not alter other markers of bone turnover. Phylloquinone supplementation for 3 years (co-administered with minerals and vitamin D) has been shown to reduce postmenopausal bone (femoral neck) loss, but had no effect on markers of bone turnover (Braam et al. Reference Braam, Knapen, Geusens, Brouns, Hamulyak, Gerichhausen and Vermeer2003). Therefore, further research on the influence of vitamin K intake on bone turnover is warranted.
Thus, the aim of the present study was to investigate the effects of increasing the phylloquinone intake, above the usual dietary intake, for 6 weeks on various markers of vitamin K status, including γ-carboxylated osteocalcin (cOC) and ucOC, as indices of bone vitamin K requirements, as well as on biochemical markers of bone turnover in postmenopausal women.
Materials and methods
Subjects
Forty-eight postmenopausal women (>5 years since last menses) were recruited from the area of Copenhagen through advertising in local newspapers, posters and letters through the Danish Civil Registration System, of which thirty-one completed all three intervention periods. The seventeen subjects that dropped out of the study did so for personal reasons not related to the study. None of the subjects took dietary supplements, other than prescribed by the study, during and for at least 2 months before the beginning of the study. None of the recruited subjects performed excessive physical activity. Other exclusion criteria included smoking, hormone replacement therapy, chronic illness, and drugs known to affect vitamin K status or Ca or bone metabolism. All subjects were given a brief medical examination at recruitment by a physician.
Ethical considerations
The research protocol was approved by the Municipal Ethical Committee of Copenhagen and Frederiksberg (KF no. 01-104/00), and a written consent was obtained from each subject.
Experimental design
The study was performed as a supplementation study in free-living subjects and consisted of a randomised cross-over trial of three successive intervention periods, each of 6 weeks, with intervening 3-week washout periods. The total duration of the study was 24 weeks from August to February. In the washout periods, the subjects consumed their usual diets and were instructed not to change their diet throughout the study period. The regimens were ‘placebo’ (usual diet plus 0 μg phylloquinone/d), ‘200 μg phylloquinone supplemented’ (usual diet plus 200 μg phylloquinone/d) or ‘500 μg phylloquinone supplemented’ (usual diet plus 500 μg phylloquinone/d). The subjects were instructed to return the glass with tablets, and compliance was determined by counting the remaining tablets. In addition, each subject was supplemented throughout the study period with 10 μg vitamin D3/d, commencing 2 months before the first intervention, so as to avoid seasonal changes in vitamin D status. Phylloquinone-containing (200 or 500 μg) and matching placebo tablets (F Hoffmann-LaRoche Ltd, Basel, Switzerland) were given daily (in a double-blinded fashion) from day 1 to day 42 in each intervention period. Blood and urine samples were collected at the initiation of the study (baseline measurements) and at the end of each intervention period (see later).
Dietary analysis
Usual dietary intakes of Ca, P and protein were estimated by a validated food-frequency questionnaire (Mølgaard et al. Reference Mølgaard, Sandström and Michaelsen1998). Questionnaires were mailed to the subjects and returned before the intervention study began.
Bone mineral density
BMD of the postero-anterior lumbar spine (L2–L4) and total hip (femoral neck, trochanter and intertrochanter) was measured using a LUNAR DPX-IQ scanner (Lunar Corporation Ltd, Madison, WI, USA). Standardised positioning and utilisation of the software was used. The scans were acquired using the pencil-beam mode and they were analysed using Lunar software version 4.6c using the compare feature.
Urinary specimens
From days 1–3 and 40–42 for each intervention period, 24 h urine was collected in acid-washed plastic bottles containing 1 m-HNO3 (10 ml). Collection of urine on all urine-sampling days entailed collection of the first morning void sample and the following 24 h sample separately. The start time of the collection was not standardised but the first morning void was noted daily. To ensure complete collection of urine, p-aminobenzoic acid tablets (3 × 80 mg/d; local pharmacy of The Royal Veterinary and Agricultural University (KVL), Frederiksberg, Denmark) were given on days of urine collection, as described elsewhere (Bingham & Cummings, Reference Bingham and Cummings1983).
Blood samples
Blood samples were drawn at the beginning and end of each intervention period. The participants were asked to fast for 12 h and abstain from severe physical activity, intake of any kind of drugs for 48 h, and from alcohol for 24 h before sampling. Samples were collected in the morning (08.00–10.00 hours). Blood samples were processed to serums or plasma and stored at − 20 and − 80°C, as appropriate, until required for analysis. Hb was measured in a whole-blood sample on the day of blood collection.
For a number of blood and urine analyses, all samples from one individual were measured in one run, and thus no inter-assay variation is given.
Serum phylloquinone, carboxylated and undercarboxylated osteocalcin
Serum phylloquinone concentrations were assessed by HPLC and fluorescence detection (excitation 244 nm, emission 430 nm) after on-line electrochemical reduction of the effluent (Gijsbers et al. Reference Gijsbers, Jie and Vermeer1996; Schurgers et al. Reference Schurgers, Geleijnse, Grobbee, Pols, Hofman, Wittemann and Vermeer1999). In short, a 0·5 ml sample was supplemented with 0·5 ml distilled water, 2 ml ethanol and 1 ng internal standard (2,3-dihydrophylloquinone; F Hoffmann-LaRoche Ltd, Basel, Switzerland) and extracted with 4 ml hexane. After centrifugation for 2 min at 2000 g the hexane phase was removed, evaporated under a stream of N2 gas, and the residue was redissolved in 2 ml hexane. Pre-purification of the sample was performed with silica sep-pack cartridges (Millipore Corp., Milford, MA, USA) before analysis on a BDS Hypersil C18 column (ThermoHypersil-Keystone; Thermo Electron Corp., Bellefonte, PA, USA). Both ucOC and cOC were measured with a sandwich ELISA based on a monoclonal antibody against tOC as a capture antibody and conformation-specific antibodies as second antibodies for ucOC and cOC, respectively (Glu-OC and Gla-OC test kit; Takara Shuzo Corp., Tokyo, Japan). The Gla residues are located at positions 17, 21 and 24 and not directly at the N terminus, thus large degradation products missing the N terminus may also be detected. The specificity for the respective conformations is high with less than 5 % cross-reaction. The intra-assay and inter-assay CV for cOC analysis were 3·5 and 4·5 %, respectively. The intra-assay and inter-assay CV for ucOC analysis were 5 and 6 %, respectively. The assay CV for the ucOC:cOC ratio was 11 %.
Serum 25-hydroxyvitamin D
Serum proteins were precipitated with ethanol, and deproteinised serum was subsequently applied to a MFC18 solid-phase extraction column (Isolute®; International Sorbent Technology Ltd, Pontypridd, Mid Glamorgan, UK) for elution of the serum 25-hydroxyvitamin D (25(OH)D) fraction with ethyl acetate:n-heptane (10:90). The extracted 25(OH)D was injected onto an HPLC-system (Waters Corp., Milford, MA, USA) equipped with a 600 controller and pump, a refrigerated 717PLUS Autosampler, a 996 diode array detector (set at 220–320 nm) for detection, and a 2487 absorbance detector (set at 265 nm) for quantification. The HPLC column used for separation was a cyano (Luna; Phenomenex Inc., Torrance, CA, USA) in which 25(OH)D2 and 25(OH)D3 was eluted separately with 2-propanol:n-heptane (1·5:98·5). However, none of the samples contained 25(OH)D2. Samples were analysed in duplicate on different days, showing a CV of 6·0 %. The accuracy of the analysis was monitored by participation in the Vitamin D External Quality Assessment Scheme (DEQAS; Charing Cross Hospital, London, UK).
Serum 1,25-dihydroxyvitamin D
A RIA (no. 65100E; DiaSorin Ltd, Stillwater, MN, USA) was used for the quantification of serum 1,25-dihydroxyvitamin D (1,25(OH)2D) levels. The manufacturer's method was modified slightly as solid-phase extraction was performed on MFC18 columns (Isolute®; International Sorbent Technology Ltd). Samples were analysed in duplicate on different days, showing an inter-assay CV of 12·6 %. The accuracy of the analysis was monitored by participation in the Vitamin D External Quality Assessment Scheme (Charing Cross Hospital, London, UK).
Plasma parathyroid hormone
Plasma samples were analysed in duplicate for intact parathyroid hormone with a chemiluminescent immunometric assay (IMMULITE®; Diagnostic Products Corp., Los Angeles, CA, USA). The intra-assay CV for this assay was 5·8 %, while inter-assay variation was 10 %.
Serum total osteocalcin and bone-specific alkaline phosphatase
Serum tOC levels were measured in serum samples using an ELISA (BRI-Diagnostics Ltd, Dublin, Republic of Ireland). The intra-assay CV has been measured as 3·7 %. Serum bone-specific alkaline phosphatase (BAP) levels were measured in serum samples using a recently developed ELISA (Alkphase-B™; MetraBiosystems Ltd, Wheatley, Oxon, UK). The intra-assay CV has been measured as 4·5 %.
Haemoglobin and serum α1-antichymotrypsin
Hb was analysed in whole-blood samples by photometric absorption measurements with sodium lauryl sulfate as the haemolysing agent on a Sysmex KX-21 apparatus (Sysmex Corp., Kobe, Japan). The intra-assay CV for this assay was 0·5 % (n 12) and the inter-assay CV was 0·6 % (n 27). Serum α1-antichymotrypsin was measured by turbidimetric detection of antigen–antibody reaction on Cobas Mira apparatus (Roche Diagnostic Systems, F Hoffmann-La Roche Ltd, Basel, Switzerland) using rabbit antihuman α1-antichymotrypsin (DAKO, Glostrup, Denmark). The intra-assay CV for this assay was 2·1 % (n 12) and the inter-assay CV was 4·19 % (n 79).
Urinary free γ-carboxyglutamate
Free Gla was analysed in 24 h urine samples using the procedure developed by Kuwada & Katayama (Reference Kuwada and Katayama1983). In short, the urine samples were diluted with distilled water and analysed by HPLC, using a Nucleosil 100-5 SB anion exchange resin (5 μm particles; Macherey-Nagel, GmbH & Co. KG, Düren, Germany) at a flow rate of 1 ml/min. Reference curves were prepared from samples with known concentration of authentic Gla (Sigma-Aldrich Corp., St Louis, MO, USA). The inter-assay CV was 5 %.
Urinary pyridinoline and deoxypyridinoline
The morning urine samples (first morning void) were analysed in triplicate for urinary pyridinoline (Pyr) and deoxypyridinoline (Dpyr) using a three-step procedure. Urine was firstly hydrolysed with an equal volume of 12 m-HCl at 100°C for 18 h. The cross-links were then extracted by CF1 cellulose chromatography with the use of an internal standard (acetylated Pyr; MetraBiosystems Ltd, Wheatley, Oxon, UK) and the samples were analysed using reversed-phase HPLC with fluorescence detection (Colwell et al. Reference Colwell, Russel and Eastell1993). The acetylated Pyr was applied in accordance with the method described by Calabresi et al. (Reference Calabresi, Lasagni, Franceschelli, Bartolini, Serio and Brandi1994) and Robins et al. (Reference Robins, Stead and Duncan1994). The content of cross-links in the urine was quantified by external standardisation using a commercially available Pyr/Dpyr HPLC calibrator (MetaBiosystems Ltd, Wheatley, Oxon, UK). The intra-assay CV for Pyr and Dpyr measured as the variation between ten chromatograms obtained between column regenerations as described by Colwell et al. (Reference Colwell, Russel and Eastell1993) have previously been measured as 6 and 7 %, respectively.
Urinary creatinine
Creatinine was determined in the morning urine samples (first morning void) using a diagnostic kit (Metra Creatinine Assay Kit; Quidel Corp., San Diego, CA, USA). The intra-assay CV was 1·6 %.
Urinary type I collagen cross-linked N-telopeptides
NTx were measured in the morning urine samples (first morning void) by an ELISA (Osteomark®; Ostex International Inc., Seattle, WA, USA). The intra-assay CV was 5 %.
Statistical analyses
All analyses and calculations were performed using the Statistical Analysis System software package, version 8.2 (SAS Institute, Cary, NC, USA). Univariate mixed model analyses of covariance (ANCOVA) were performed in the ‘MIXED’ procedure with Tukey's post hoc test. In the statistical model, biochemical markers were evaluated as the dependent variable. Treatment, order and treatment × order were included as independent fixed variables and baseline values as covariates. Subjects were included as a random effect. In models with significant treatment × order (phylloquinone, cOC, and BAP), the interaction was adjusted for by including the preceding value at each period as covariate.
Denoting the ith subject's (1, 2,… , 31) jth dependent variable (serum phylloquinone, 25(OH)D, 1,25(OH)2D, tOC, ucOC, cOC, ucOC:cOC, and BAP, and urinary NTx, Pyr, Dpyr, and Gla) in period t (0 (baseline), 1, 2, 3), the statistical models with significant treatment × order were as follows:
where δs are subject-specific random effects and ɛs are independently distributed random variables.
Homogeneity of variance and normal distribution among random effects were investigated by plots of residuals. Shapiro–Wilk's test for normal distribution was performed. The investigations showed it necessary to log-transform all dependent biochemical variables, except serum phylloquinone (which was transformed by square root), tOC, cOC and BAP. Where necessary, transformed data were back-transformed, and data are presented as means and sd or means and sem where appropriate.
Results
Descriptive data
Baseline anthropometric data as well as baseline Hb, ferritin and α1-antichymotrypsin, and BMD measurements of the postmenopausal women who participated in the study are shown in Table 1. All women were of average height and weight for their age group. None of the postmenopausal women were suffering from Fe deficiency. Mean Hb concentration was 7·9 (sd 0·4) mmol/l (range 7·2–8·7 mmol/l; 95th percentile 8·6 mmol/l) and mean ferritin concentration was 107·1 (sd 130·4) μg/l (range 11·4–621·2 μg/l; 95th percentile 348·9 μg/l). The mean concentration of serum 25(OH)D at baseline was 58 (sd 18) nmol/l, and the mean plasma parathyroid hormone concentration was 5·3 (sd 1·6) pmol/l. The overall mean concentration of the acute-phase protein α1-antichymotrypsin was 0·30 (sd 0·05) g/l (range 0·21–0·49 g/l; 95th percentile 0·38 g/l) during the entire intervention study and the mean recovery of p-aminobenzoic acid tablets was 100 (sd 25) %. Fifteen of the thirty-one women who completed the study had low bone density (thirteen had osteopenia and two had osteoporosis, as indicated by T-score) at the spine and/or femur. Habitual dietary intakes of Ca, P and protein, as recorded by food-frequency questionnaires, are shown in Table 1. Of the glasses with tablets, 48 % were returned; based on these, compliance was determined to be 98·9 (sd 1·9) %.
Table 1 Subject characteristics (Mean values and standard deviations)
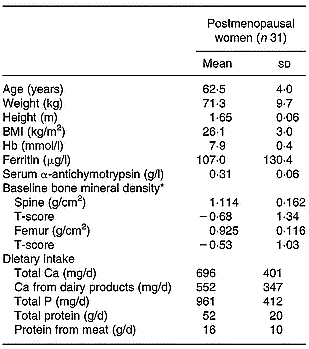
* Diagnostic criteria for osteoporosis and osteopenia, based on bone mineral density, include: normal, more than − 1 sd of young adult reference mean for the population; osteopenia, between − 1 and − 2·5 sd of the young adult mean; osteoporosis, more than − 2·5 sd below the young adult mean (World Health Organization, 1994).
Effect of phylloquinone supplementation on markers of vitamin K status
The effects of phylloquinone supplementation on vitamin K status markers are shown in Table 2. No significant difference in mean serum phylloquinone concentration was observed between the placebo and the 200 μg/d phylloquinone supplementation period (P = 0·15). However, mean serum phylloquinone concentration during the 500 μg phylloquinone/d supplementation period was significantly (P < 0·001) higher than that during either of the other two intervention periods. There was a significant (P < 0·001) dose-dependent increase and decrease in serum cOC and ucOC concentrations, respectively, with increasing phylloquinone intake in postmenopausal women. A corresponding significant (P < 0·001) decrease in the serum ucOC:cOC ratio was revealed with increasing phylloquinone intake. The reduction in ucOC:cOC ratio was shown to be 62 and 94 % after supplementation with 200 and 500 μg phylloquinone/d, respectively. Correspondingly, a 27 and 81 % increase in serum phylloquinone concentration was seen after supplementation with 200 and 500 μg phylloquinone/d, respectively (Table 2). Urinary Gla concentration was unaffected by phylloquinone supplementation.
Table 2 Effect of vitamin K1 supplementation in addition to 10 μg vitamin D/d for 6 weeks on vitamin K status markers in postmenopausal women (n 31)* (Mean values with their standard errors)
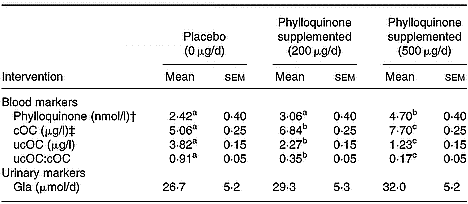
cOC, serum carboxylated osteocalcin; ucOC, serum undercarboxylated osteocalcin; Gla, free γ-carboxyglutamate.
a,b,c Mean values within a row with unlike superscript letters were significantly different (P < 0·001; Tukey's honestly significant difference test).
* The presented results were obtained on the last day of the 6-week supplementation period.
† Porder×treatment=0· 025 (conversion factor: μg/l = 0·45 × nmol/l).
‡ Porder×treatment=0·032.
Effect of phylloquinone supplementation on biochemical markers of bone turnover
The effects of phylloquinone supplementation on biochemical markers of bone turnover in postmenopausal women are shown in Table 3. Phylloquinone supplementation had no effect on urinary Pyr, Dpyr or NTx concentration (all expressed per mmol creatinine). Similarly, phylloquinone supplementation had no effect on serum BAP, 25(OH)D or 1,25(OH)2D or plasma parathyroid hormone concentrations. While there was no significant difference in mean serum tOC concentration between the placebo and the 200 μg/d phylloquinone supplementation period, mean serum tOC concentration during the 500 μg/d phylloquinone supplementation period was significantly (P < 0·001) higher than that during the placebo intervention period. However, there was no significant difference in serum tOC concentration between the two phylloquinone-supplemented periods.
Table 3 Effect of vitamin K1 supplementation in addition to 10 μg vitamin D/d for 6 weeks on circulating parathyroid hormone (PTH), vitamin D metabolites and biochemical markers of bone turnover in postmenopausal women (n 31)* (Mean values with their standard errors)
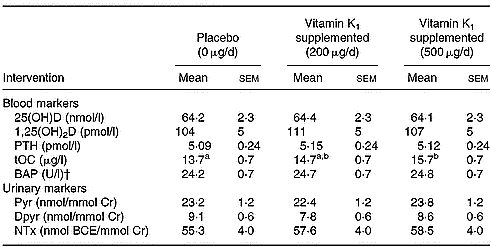
25(OH)D, serum 25 hydroxyvitamin D; 1,25(OH)2D, serum 1,25 dihydroxyvitamin D; tOC, serum total osteocalcin; BAP, serum bone-specific alkaline phosphatase; Pyr, pyridinoline; Cr, creatinine; Dpyr, deoxypyridinoline; NTx, type I collagen cross-linked N-telopeptides; BCE, bone collagen equivalent.
a,b Mean values within a row with unlike superscript letters were significantly different (P < 0·001; Tukey's honestly significant difference test).
* The presented results were obtained on the last day of the 6-week supplementation period.
† Porder×treatment=0·003.
Discussion
The postmenopausal women who participated in the present study were non-anaemic, well nourished and apparently healthy according to the α1-antichymotrypsin measurement. The recorded mean dietary intake of Ca in the present study was lower than recommended in the USA for this age group but above the lower limit for recommended intake of Ca in Denmark (Institute of Medicine, 1997; Becker et al. Reference Becker, Lyhne, Pedersen, Aro, Fogelhol, Pedersen, Alexander, Andersen, Meltzer and Pórsdóttir2004). However, the Ca intake was lower than expected, and thus Ca supplementation was not provided together with the daily vitamin D supplementation.
The serum concentration of ucOC obtained after placebo treatment would suggest that subclinical vitamin K deficiency was relatively common in these postmenopausal women, in agreement with the findings of others (Knapen et al. Reference Knapen, Hamulyák and Vermeer1989; Plantalech et al. Reference Plantalech, Chapuy, Guillaumont, Chapuy, Leclerq, Delmas, Christiansen and Overgaard1990; Binkley et al. Reference Binkley, Krueger, Engelke, Foley and Suttie2000). Whether this insufficiency has physiological or clinical relevance is unclear. However, the degree of undercarboxylation seen in the present study (30 % ucOC in the placebo period) is not uncommon. It has ranged from 7·5 % to 50 % in other studies in postmenopausal women, whose estimated intake of phylloquinone was 90–220 μg/d (Knapen et al. Reference Knapen, Hamulyák and Vermeer1989; Plantalech et al. Reference Plantalech, Chapuy, Guillaumont, Chapuy, Leclerq, Delmas, Christiansen and Overgaard1990; Booth et al. Reference Booth, Webb and Peters1999, Reference Booth, Broe, Gagnon, Tucker, Hannan, McLean, Dawson-Hughes, Wilson, Cupples and Kiel2003; Binkley et al. Reference Binkley, Krueger, Engelke, Foley and Suttie2000; McKeown et al. Reference McKeown, Jacques, Gundberg, Peterson, Tucker, Kiel, Wilson and Booth2002). Possible explanations for this variation in carboxylation degree include the use of different assays in different studies and variation in phylloquinone intake. However, a high serum ucOC concentration has been associated with increased bone turnover (Knapen et al. Reference Knapen, Jie, Hamulyák and Vermeer1993), low BMD (Szulc et al. Reference Szulc, Arlot, Chapuy, Duboeuf, Muenier and Delmas1994) and increased risk of osteoporotic fractures (Szulc et al. Reference Szulc, Chapuy, Meunier and Delmas1993, Reference Szulc, Chapuy, Meunier and Delmas1996; Vergnaud et al. Reference Vergnaud, Garnero, Meunier, Breart, Kamihagi and Delmas1997). If ucOC produces adverse skeletal consequences, increased phylloquinone intake should lower the degree of undercarboxylation of OC as well as benefiting bone turnover, BMD and/or fracture risk.
In the present study, supplementation of the usual diet with additional phylloquinone increased the degree of carboxylation, and consequently decreased the degree of undercarboxylation of OC, in a dose-dependent manner (by 40 and 68 %, with 200 and 500 μg phylloquinone/d, respectively). This occurred in apparently healthy subjects whose serum phylloquinone concentrations were well within the normal range for healthy women of this age group (Sadowski et al. Reference Sadowski, Hood, Dallal and Garry1989; Institute of Medicine, 2001). Older healthy subjects appear to have higher serum phylloquinone concentrations than younger subjects regardless of dietary intake (Sokoll & Sadowski, Reference Sokoll and Sadowski1996). As regards the records of vitamin K intakes, they seem to be wide-ranging, reporting intakes from 50 to 250 μg phylloquinone/d (Booth et al. Reference Booth, Webb and Peters1999; Schurgers et al. Reference Schurgers, Geleijnse, Grobbee, Pols, Hofman, Wittemann and Vermeer1999; Thane et al. Reference Thane, Paul, Bates, Bolton-Smith, Prentice and Shearer2002; Duggan et al. Reference Duggan, Cashman, Flynn, Bolton-Smith and Kiely2004). The dietary assessment tool used in the present study was designed to estimate habitual intakes of Ca, and was not appropriate to estimate habitual dietary phylloquinone intake. Making such an estimate is further complicated by the lack of sufficient data on the phylloquinone content of Danish foods in Danish Food Databases. However, the mean usual dietary intakes of phylloquinone of similarly-aged women (n 28) were estimated recently using 6 d (2 × 3 d) of food diaries using a Dutch food database as part of a different study (ISOHEART). The mean phylloquinone intake in that study was found to be 189 (sd 182) μg/d (S Bügel, unpublished results).
Therefore, it seems likely, although not measured, that the Danish women in the present study would have a higher consumption of phylloquinone than that reported in the USA and UK, contributing to relatively high, though within normal range, concentrations of serum phylloquinone (Booth et al. Reference Booth, Webb and Peters1999; Institute of Medicine, 2001; Thane et al. Reference Thane, Paul, Bates, Bolton-Smith, Prentice and Shearer2002; Vermeer et al. Reference Vermeer, Shearer, Zittermann, Bolton-Smith, Szulc, Hodges, Walter, Rambeck, Stöcklin and Weber2004). Despite this, the ucOC:cOC ratio shown to be 0·91 in the placebo intervention suggests that the usual dietary intakes of phylloquinone in the present women were inadequate to allow maximal γ-carboxylation of osteocalcin. Phylloquinone supplementation (ranging from 0 to 1000 μg/d) for 2 weeks has been shown to dose-dependently decrease (P < 0·001) the percentage undercarboxylation of osteocalcin in adult men and women (Binkley et al. Reference Binkley, Krueger, Kawahara, Engelke, Chappell and Suttie2002). Furthermore, in a second sub-study, the same authors reported that while supplementation with 1000 and 2000 μg doses of phylloquinone produced greater reductions in the percentage undercarboxylation of osteocalcin than a 500 μg phylloquinone dose, there was no significant difference in the reductions in the percentage undercarboxylation of osteocalcin between the higher doses, suggesting that at least 1000 μg phylloquinone is required to maximally γ-carboxylate osteocalcin (Binkley et al. Reference Binkley, Krueger, Kawahara, Engelke, Chappell and Suttie2002).
Supplementation with 500 μg phylloquinone/d (but not 200 μg) for 6 weeks significantly increased serum phylloquinone (by about 2-fold) in postmenopausal women in the present study. Phylloquinone supplementation for 1–2 weeks has been shown to significantly increase serum phylloquinone concentration in adults in other studies (Binkley et al. Reference Binkley, Krueger, Engelke, Foley and Suttie2000, Reference Binkley, Krueger, Kawahara, Engelke, Chappell and Suttie2002). On the other hand, urinary Gla concentration did not respond to phylloquinone supplementation over 6 weeks in the present study. Booth et al. (Reference Booth, Lichtenstein, O'Brien-Morse, McKeown, Wood, Saltzman and Gundberg2001) have suggested that urinary Gla, a measure of turnover of all vitamin K-dependent proteins, is less responsive to short-term phylloquinone changes than is ucOC, but a lack of responsiveness may also be reflected by the subjects' apparently adequate habitual intake of phylloquinone. Blood lipid levels are also known to influence phylloquinone serum concentrations. However, all subjects who completed the study were within the normal range of both serum triacylglycerol and cholesterol levels (M Kristensen, J Kudsk, S Bügel, unpublished results).
In the present study, there was a modest (about 15 %) but significant (P < 0·05) increase in serum tOC concentration with phylloquinone supplementation adding 500 μg phylloquinone/d (but not 200 μg/d) to the usual diet for 6 weeks. In contrast, supplementation with 1000 μg phylloquinone/d was reported to have either no effect in younger and older adults (Knapen et al. Reference Knapen, Hamulyák and Vermeer1989, Douglas et al. Reference Douglas, Robins, Hutchison, Porter, Stewart and Reid1995; Binkley et al. Reference Binkley, Krueger, Kawahara, Engelke, Chappell and Suttie2002) or result in an observed age-independent decrease in serum tOC concentration (Binkley et al. Reference Binkley, Krueger, Engelke, Foley and Suttie2000). It has been suggested that the use of different antibodies to measure tOC in different studies causes the discrepancy in results, which may be an artifact of the variation in affinities of different antibodies for the carboxylated form (Gundberg et al. Reference Gundberg, Nieman, Abrams and Rosen1998). There is some evidence that there may be an interaction between vitamin K and vitamin D in relation to production of fully functional osteocalcin (Shearer, Reference Shearer1997); however, a potential confounding effect of vitamin D was eliminated in the present study as the subjects were supplemented with vitamin D for 2 months before the study and throughout the study period. The increase in serum tOC with phylloquinone supplementation may have been due to the fully carboxylated OC being secreted more efficiently from the osteoblasts whereas the under- or non-carboxylated species have a tendency to accumulate in the cell (Nishimoto & Price, Reference Nishimoto and Price1985; Wu et al. Reference Wu, Bancroft and Suttie1996). In support of this, we saw no effect of phylloquinone supplementation on serum BAP concentration. This is in agreement with the findings of Binkley et al. (Reference Binkley, Krueger, Engelke, Foley and Suttie2000) and Braam et al. (Reference Braam, Knapen, Geusens, Brouns, Hamulyak, Gerichhausen and Vermeer2003), which showed that supplementation with 1 mg phylloquinone for 2 weeks and 3 years, respectively, had no effect on serum BAP. In addition, the findings of the present study show no effect of phylloquinone supplementation for 6 weeks on urinary Pyr, Dpyr and NTx, suggesting a lack of effect on the rate of bone resorption, in agreement with the findings of Binkley et al. (Reference Binkley, Krueger, Engelke, Foley and Suttie2000). It can be argued that the lack of effect of phylloquinone supplementation on markers of bone turnover that are not γ-carboxylated may be due to the relatively short duration of the study. However, Braam et al. (Reference Braam, Knapen, Geusens, Brouns, Hamulyak, Gerichhausen and Vermeer2003) did not see an effect on urinary Dpyr and serum BAP activity after phylloquinone supplementation for 3 years, even though, interestingly, the rate of bone loss at the femoral neck was significantly reduced (Braam et al. Reference Braam, Knapen, Geusens, Brouns, Hamulyak, Gerichhausen and Vermeer2003).
It cannot be ruled out that, had the women been supplemented with Ca in addition to vitamin D, the effect of a vitamin K supplement would have been different. Braam et al. (Reference Braam, Knapen, Geusens, Brouns, Hamulyak, Gerichhausen and Vermeer2003) report that vitamin K given as a supplement in addition to minerals and vitamin D had a more pronounced effect on bone loss over 3 years than mineral and vitamin D supplementation alone. However, it is not known whether the effect of vitamin K is dependent on Ca intake, and thus it should be emphasised that the present results apply to women with suboptimal Ca intakes.
In conclusion, the findings of the present study showed that increasing phylloquinone intake of postmenopausal women by 200 and 500 μg/d significantly increased the degree of γ-carboxylation of OC and, consequently, led to a reduction in concentrations of ucOC, an independent risk factor for osteoporotic fracture (Szulc et al. Reference Szulc, Chapuy, Meunier and Delmas1993, Reference Szulc, Chapuy, Meunier and Delmas1996; Vergnaud et al. Reference Vergnaud, Garnero, Meunier, Breart, Kamihagi and Delmas1997). The reduction in ucOC concentration (and ucOC:cOC ratio) achieved by phylloquinone supplementation, however, had no apparent modulating effect on bone turnover. This may be explained by an apparently adequate habitual intake of phylloquinone and it is possible that very large doses of phylloquinone are required to see a response. Therefore, further research is warranted to investigate the mechanisms of action of phylloquinone on BMD and fracture risk, as well as further clarification of the physiological and clinical relevance of submaximal γ-carboxylation of OC, including its role as a status indicator for vitamin K nutriture. This issue is of importance for further consideration of the dietary requirement for phylloquinone, as the findings of the present and other studies would suggest that usual dietary intakes of several population sub-groups provide inadequate phylloquinone to allow maximal γ-carboxylation of OC.
Acknowledgements
The present study was carried out with financial support from the European Commission, Quality of Life, Fifth Framework Programme QLK1-1999-00 752 ‘Optimal Nutrition towards Osteoporosis Prevention: Impact of Diet and Gene-Nutrient Interactions on Calcium and Bone Metabolism’. F. Hoffmann La-Roche Ltd, Basel, Switzerland is appreciated for providing the placebo and the phylloquinone-containing capsules and also for delivering the internal standard 2,3-dihydrophylloquinone used in the analysis of serum vitamin K. We gratefully acknowledge Vivian Anker, Ella Jessen, and Hanne Lysdal Pedersen, Department of Human Nutrition, Centre for Advanced Food Studies, The Royal and Veterinary Agricultural University, Denmark for their excellent technical assistance and the volunteers who participated in the present study. Project manager Professor Britt-Marie Sandström, Department of Human Nutrition, Centre for Advanced Food Studies, The Royal and Veterinary Agricultural University, Denmark unfortunately passsed away after a long period of illness. She will be honoured, remembered, and missed by all her colleagues.





