Individuals with dementia commonly manifest behavioural and psychiatric symptoms of dementia (BPSD) such as aggression, agitation, psychotic symptoms, sleep disturbance and wandering. The off-label use of antipsychotic drugs to treat BPSD is widespread. Studies from around the world have reported that 25–40% of elderly residents in long-term institutional care receive antipsychotics (Reference Hagen, Esther and IkutaHagen et al, 2005; Reference Snowdon, Day and BakerSnowdon et al, 2005; Reference Alanen, Finne-Soveri and NoroAlanen et al, 2006; Rochan, 2007). A UK survey found 32% of patients in care homes with dementia were prescribed antipsychotics (Reference Alldred, Petty and BowieAlldred et al, 2007). In 2004, the Committee on Safety of Medicines warned of the increased risk of cerebrovascular events with risperidone and olanzapine and said these drugs should not be used to treat behavioural problems in older adults with dementia (Committee on Safety of Medicines, 2004). The Royal College of Psychiatrists’ Faculty of the Psychiatry of Old Age and other stakeholders responded by issuing guidance laying down good practice guidelines for the use of antipsychotics in the treatment of BPSD (Working Group, 2004). Further guidance from the Royal College of Psychiatrists was later thought necessary due to reports of inappropriate interpretations of the earlier documents, for example patients having their antipsychotics abruptly withdrawn (Royal College of Psychiatrists, 2005). More recently, the National Institute for Health and Clinical Excellence (NICE) has issued a national clinical practice guideline on dementia with firm recommendations about the pharmacological treatment of dementia (National Collaborating Centre for Mental Health, 2007).
What do old age psychiatrists feel about all this guidance, some of it highly specific and prescriptive? Is it applicable to the real world of everyday National Health Service (NHS) practice? Does it leave enough room for clinicians to exercise their clinical judgement or do psychiatrists feel they have been left without support when they prescribe antipsychotics? We surveyed the views of career old age psychiatrists to see whether or not they considered the most recent Royal College of Psychiatrists’ document (forthwith referred to as the RCPsych 2005 guidance) supportive of their practice and the NICE dementia guideline too restrictive. We wanted to know whether any psychiatrists thought antipsychotics should never be used for BPSD. We sought to determine the percentage of patients with BPSD for whom old age psychiatrists prescribe antipsychotics and which drugs they prescribe most frequently.
Method
We talked to a number of old age psychiatrists to determine their views about the two sources of guidance. Although a range of opinions were expressed, the overall feeling was that the RCPsych 2005 guidance struck a better balance over the use of antipsychotics for BPSD than the NICE dementia guideline. Very few psychiatrists were of the opinion that antipsychotics should never be used. We set out to confirm or refute these views in the questionnaire, which was first piloted in our own hospital. In May 2007, after obtaining approval from the College, we sent a single mailing of an anonymous postal questionnaire to the 608 consultants and 40 associate specialists listed by the College as specialising in old age psychiatry. The questionnaire asked respondents to rate on a ten-point scale (1 – strongly agree, 10 – strongly disagree) their agreement/disagreement with the following statements.
-
1. The NICE guideline on dementia places clinically inappropriate restrictions on the use of antipsychotics in the treatment of BPSD.
-
2. The RCPsych 2005 guidance Atypical Antipsychotics and Behavioural and Psychiatric Symptoms of Dementia: Prescribing Update for Old Age Psychiatrists supports psychiatrists in prescribing antipsychotics for selected cases of BPSD.
-
3. Antipsychotics should never be prescribed for BPSD.
Respondents were invited to comment on the NICE and the RCPsych 2005 guidance on dementia and to indicate the percentage of their patients with BPSD for whom they prescribe antipsychotics. They were also asked about the clinical circumstances under which they prescribe antipsychotics for BPSD and the three antipsychotics they use most commonly (with dosage ranges). (The questionnaire is available from the corresponding author on request.)
Numerical analyses were conducted using SPSS version 14.0 for Windows. Participants’ comments were subjected to qualitative analysis for commonly occurring themes. Two of the authors independently derived a list of topics from the comments and then met to reach a consensus on the major themes.
Results
Of the 648 questionnaires sent out, 207 were returned, of which 202 (31.2%) had been completed. Almost all respondents (176 of 202, 87.1%) worked in NHS community and in-patient settings, 14 (6.9%) worked in NHS community services and most of the rest (n=8, 4.0%) in specialist services.
The majority (130 of 197, 66.0%) of respondents thought the NICE guideline on dementia placed clinically inappropriate restrictions on the use of antipsychotics in the treatment of BPSD. Median score on the scale of 1–10 (1 – strongly agree, 10 – strongly disagree) was 4 (interquartile range IQR=3–7).
Most respondents (154 of 198, 77.8%) thought the RCPsych 2005 guidance supported psychiatrists in prescribing atypical antipsychotics for selected patients with BPSD. Median score on the 1–10 scale (1 – strongly agree, 10 – strongly disagree) was 3 (IQR=2–5).
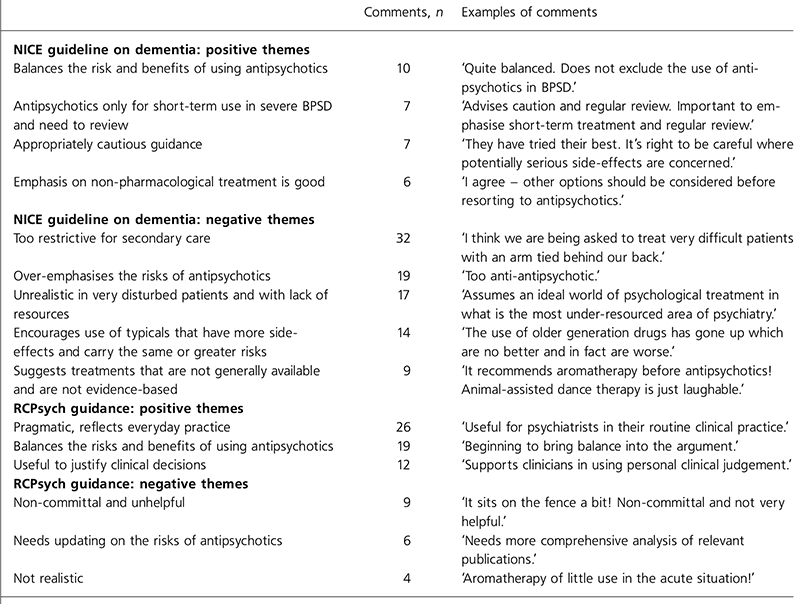
A total of 162 comments on the NICE guideline on dementia were received: 40 positive (24.7%), 111 negative (68.5%) and 11 in which the respondent had not read or could not recall the guidance (6.8%). Comments fell into several broadly defined themes (Table 1). Of the 135 comments on the RCPsych 2005 guidance, 105 were positive (77.8%), 20 were negative (14.8%) and 10 had not read or could not remember the document (7.4%). Overall, the NICE guideline on dementia was perceived as too restrictive for secondary care, as placing too great an emphasis on the risks of antipsychotics in BPSD and unrealistic given current resources. The RCPsych 2005 guidance was seen as more balanced, practical and useful to justify prescribing decisions.
Table 1. NICE and RCPsych guidelines: psychiatrists' comments by the most common themes
| Comments, n | Examples of comments | |
|---|---|---|
| NICE guideline on dementia: positive themes | ||
| Balances the risk and benefits of using antipsychotics | 10 | ‘Quite balanced. Does not exclude the use of antipsychotics in BPSD.’ |
| Antipsychotics only for short-term use in severe BPSD and need to review | 7 | ‘Advises caution and regular review. Important to emphasise short-term treatment and regular review.’ |
| Appropriately cautious guidance | 7 | ‘They have tried their best. It's right to be careful where potentially serious side-effects are concerned.’ |
| Emphasis on non-pharmacological treatment is good | 6 | ‘I agree — other options should be considered before restoring to antipsychotics.’ |
| NICE guideline on dementia: negative themes | ||
| Too restrictive for secondary care | 32 | ‘I think we are being asked to treat very difficult patients with an arm tied behind our back.’ |
| Over-emphasises the risks of antipsychotics | 19 | ‘Too anti-antipsychotic.’ |
| Unrealistic in very disturbed patients and with lack of resources | 17 | ‘Assumes an ideal world of psychological treatment in what is the most under-resourced area of psychiatry.’ |
| Encourages use of typicals that have more side-effects and carry the same or greater risks | 14 | ‘The use of older generation drugs has gone up which are no better and in fact are worse.’ |
| Suggests treatments that are not generally available and are not evidence-based | 9 | ‘It recommends aromatherapy before antipsychotics! Animal-assisted dance therapy is just laughable.’ |
| RCPsych guidance: positive themes | ||
| Pragmatic, reflects everyday practice | 26 | ‘Useful for psychiatrists in their routine clinical practice.’ |
| Balances the risks and benefits of using antipsychotics | 19 | ‘Beginning to bring balance into the argument.’ |
| Useful to justify clinical decisions | 12 | ‘Supports clinicians in using personal clinical judgement.’ |
| RCPsych guidance: negative themes | ||
| Non-committal and unhelpful | 9 | ‘It sits on the fence a bit! Non-committal and not very helpful.’ |
| Needs updating on the risks of antipsychotics | 6 | ‘Needs more comprehensive analysis of relevant publications.’ |
| Not realistic | 4 | ‘Aromatherapy of little use in the acute situation!’ |
Almost all respondents (190 of 199, 95.5%) disagreed with the statement that antipsychotics should never be prescribed for patients with any type of dementia. Median score on the 1–10 scale (1 – strongly agree, 10 – strongly disagree) was 10 (IQR=9–10). All respondents reported that they prescribed antipsychotics for BPSD. The median percentage of their patients with BPSD for whom they prescribed antipsychotics was 40% (range 5–90). The most common indications for antipsychotics were: psychosis (93.3%), aggression (89.1%), agitation (72.0%) and sexual disinhibition (50.3%). Other indications included: when other measures (including non-pharmacological ones) had failed, risk of harm to self or others, severe intractable distress and where a patient's placement was at risk. Some emphasised the importance of first trying other measures before antipsychotics, for example antidepressants and non-pharmacological interventions, and the need to balance risks against benefits. Quality of life was also important: ‘the angry, distressed, deluded, unhappy patient would not willingly choose to be like that’, ‘in dementia it is quality of life that is important, not quantity’.
The three most commonly prescribed antipsychotics for BPSD are given in Table 2, together with the median usual dosage ranges. Quetiapine was by far the most commonly prescribed antipsychotic. Although atypicals were used more often than typicals, haloperidol was the second most popular antipsychotic and several other typicals were also prescribed, albeit less frequently.
Table 2. Antipsychotics for BPSD: psychiatrists' reports of their three most commonly prescribed antipsychotics and usual dosage range

| Antipsychotic | Psychiatrists prescribing the antipsychotic,1 n | Usual daily dosage range (median values), mg |
|---|---|---|
| Quetiapine | 165 | 25-150 |
| Haloperidol | 89 | 0.5-2 |
| Risperidone | 85 | 0.5-2 |
| Amisulpride | 85 | 50-150 |
| Olanzapine | 64 | 2.5-10 |
| Sulpiride | 23 | 100-200 |
| Promazine | 14 | 25-150 |
| Trifluoperazine | 13 | 1-4 |
| Aripiprazole | 9 | 5-17.5 |
| Other typical antipsychotics | 10 | - |
Discussion
In this survey of old age psychiatrists, two-thirds of respondents thought the NICE guideline on dementia was too restrictive, whereas over three-quarters felt the RCPsych 2005 guidance supported psychiatrists in prescribing these drugs to individuals with dementia. The NICE guideline provoked a larger number of comments (mostly negative) compared with the RCPsych 2005 guidance which received mostly positive comments. All respondents reported that they prescribed antipsychotics for at least some of their patients with BPSD (on average 40%) and the overwhelming majority disagreed with the statement that antipsychotics should never be prescribed for BPSD. Quetiapine and haloperidol were the most frequently prescribed antipsychotics.
Limitations
The study has a number of limitations. The response rate to the questionnaire was 31%, which was low (although not unusual for a single mailing of an anonymous questionnaire) and could reflect sample bias. It may be that those psychiatrists who responded were more negative in their attitudes towards the NICE guideline on dementia and/or more frequently prescribed antipsychotics for BPSD. The questions we asked were designed to be provocative but are likely to have introduced bias. Another possible source of bias was the categorisation of comments as either positive or negative and by theme, even though ratings were made independently by two authors.
The fact that quetiapine was the most commonly prescribed antipsychotic is likely to relate to the Committee on Safety of Medicines (2004) alert about risperidone and olanzapine. There is now evidence that the increased risk of death applies to all atypicals (Reference Schneider, Dagerman and InselSchneider et al, 2005). Several respondents thought the NICE guideline on dementia encourages the prescribing of the older typical drugs. In our survey, haloperidol was very commonly prescribed and some respondents reported using other typicals. Several studies have reported the risk of cerebrovascular events and increased mortality to be similar for typicals and atypicals (e.g. Reference Gill, Rochon and HerrmannGill et al, 2005; Reference Trifirò, Verhamme and ZiereTrifirò et al, 2007), with two recent studies reporting a higher risk of death in patients receiving typicals than atypicals (Reference Wang, Schneeweiss and AvornWang et al, 2005; Reference Gill, Bronskill and NormandGill et al, 2007). Some respondents pointed out that the increased risk of cerebrovascular events and death with antipsychotics is likely to be a class effect. Evidence of efficacy in BPSD, though limited, is greatest for risperidone and olanzapine, the antipsychotics featured in the Committee of Safety of Medicines alert (Reference Lee, Gill and FreedmanLee et al, 2004).
Both the NICE guideline and the RCPsych guidance discuss the use of antipsychotics in BPSD and appear to come to similar conclusions about the use of these drugs in dementia, yet the psychiatrists in our survey perceived the NICE guideline in a much more negative light. This may be due to the following features of the NICE document: its tone (‘people with Alzheimer's disease, vascular dementia or mixed dementias with mild-to-moderate non-cognitive symptoms should not be prescribed antipsychotic drugs’), source (large organisation set up by the Government) and content (inclusion of non-pharmacological measures lacking an evidence base, for example animal-assisted therapy and massage). However, NICE has pointed out their guidance is not binding on clinicians, although it should be taken into account when making clinical decisions (Anonymous, 2007). Many old age psychiatrists appear to be troubled by the NICE guideline on dementia, although they feel the RCPsych 2005 guidance goes some way to redressing the imbalance. Of course, there are other treatments for BPSD which should be considered, such as cholinesterase inhibitors for Lewy body dementia, as well as non-pharmacological interventions.
Declaration of interest
None.





eLetters
No eLetters have been published for this article.