Satisfactory diet, physical activity and nutritional status are recognized as major determinants of health. Many epidemiological studies have shown a significant association between nutrition and CVD, certain cancers, type 2 diabetes and other age-related diseases(1). Healthcare expenses that could be spared through nutritional prevention, especially of obesity, are subject to debate(Reference Dalziel and Segal2). Indeed, when obesity-related mortality is prevented and life expectancy increases, the cost of less lethal illnesses may also increase(Reference van Baal, Polder and de Wit3). Nonetheless, prevention of diseases associated with nutrition remains a priority. Benefits in terms of health and life expectancy that could be expected from population intervention, via promotion of satisfactory nutrition, have been internationally published(1) and public health programmes have been widely implemented especially in Europe(Reference Lachat, Van Camp and de Henauw4).
In France, in 2002, obesity-related costs were estimated at 2·1–6·2 billion euros, i.e. 1·5–4·6 % of total health expenditures(Reference Emery, Dinet and Lafuma5). In 2005, over 155 000 people died from cancer and 149 000 from CVD (29·5 and 28·4 % of total causes of mortality, respectively)(Reference Belot, Grosclaude and Bossard6). France appears to be relatively well protected from cardiovascular mortality compared to other European countries(Reference Muller-Nordhorn, Binting and Roll7), possibly due to lifestyle and environmental factors such as smoking, treatment and care, in addition to nutritional characteristics. In the mid-2000s, subjects being treated for diabetes were estimated at 3·7 %(Reference Kusnik-Joinville, Weill and Salanave8) and those treated for hypertension at 22·8 %(Reference Samson, Ricordeau and Pépin9). In 2001, the Ministry of Health implemented a national public health programme on nutrition, the ‘Programme national nutrition santé’ (PNNS), in order to improve population health status(Reference Hercberg, Chat-Yung and Chauliac10). Public health objectives have been defined concerning diet, nutritional status and physical activity. To attain these objectives, various recommendations have been provided to the population through simple and accessible guidelines.
National surveys describing diet, physical activity and nutritional status are necessary in order to monitor changes directly or indirectly associated with public health projects. In the USA, the National Health and Nutrition Examination Survey has been regularly conducted for more than three decades. Numerous analyses of these data have provided an overview of nutritional changes and the recent situation in the USA(Reference Briefel and Johnson11, Reference Ong, Cheung and Man12). In Europe, despite specificities regarding nutritional behaviour, obesity and chronic disease frequencies(Reference Elmadfa, Weichselbaum and Konig13), such national descriptions are less systematically disseminated as a whole(Reference Reinivuo, Valsta and Laatikainen14–Reference Turrini, Saba and Perrone16). In France, data available for nutritional surveillance were disparate up until the year 2000. They separately concerned diet(Reference Volatier and Verger17) or body mass(Reference Charles, Eschwege and Basdevant18), involved research cohorts(Reference Kesse, Boutron-Ruault and Clavel-Chapelon19) or were limited to certain regions(Reference Perrin, Dallongeville and Ducimetiere20). In the framework of the PNNS, a national monitoring system dedicated to surveillance of the nutritional status of the population was specifically implemented. One of the challenges for surveillance is to obtain representative and comprehensive data that could contribute to public health policies.
In 2006–7, the French nutrition and health survey (Etude nationale nutrition santé (ENNS)) was conducted in order to describe dietary intake, physical activity and nutritional status in a national sample of adults and children living in France. The objective of the present analyses is to describe these nutritional issues in adults, especially with respect to current French recommendations.
Methods
Study design and recruitment
The ENNS survey was a cross-sectional study with a multistage sampling design. Recruitment was carried out throughout the entire territory of continental France for one year (February 2006 to March 2007) so as to account for seasonality of diet. The first stage of sampling involved random selection of 190 geographic zones (municipalities or groups of municipalities). This was stratified on eight large regions and on the degree of urbanization (four groups, from ‘rural’ to ‘towns of more than 100 000 inhabitants’). The number of individuals included in each stratum was defined proportionally to the population size, with a minimum of twenty-four dwellings to be investigated. The second stage involved random selection of dwellings based on randomly generated phone lists; dwellings owned landlines, with or without phone number spread on free lists, or mobile phones only. When the detailed postal address was retrieved, an information letter was sent prior to the first phone contact with the selected household. The third stage of sampling involved selection of eligible subjects to be included in the study.
Criteria for adult eligibility were the following: residence in continental France during the period of the study, age 18–74 years, normal living accommodation for at least 5 d a week (not in an institution) with phone contact, an understanding of the issues of the study, no artificial feeding, and agreement to participate in the study. The aim of the first home visit with a study dietitian was to explain in detail the protocol of participation and to obtain agreement for participating. No incentive was given, but each subject was offered to receive his/her individual results as well as general conclusions of the study. Three runs of inclusion were distributed during the year of the study; during each run, all 190 geographical zones were investigated.
The survey protocol received the approval of the Ethical Committee (Hôpital Cochin, Paris, no. 2264), the Consultative Committee on Information Treatment of the Ministry of Research and the French Data Protection Authority (Commission nationale de l'informatique et des libertés, authorization no. 905481). Adults who participated in clinical and biochemical examinations signed informed consents separately for the scheduled analysis and for the biobank.
Data collection
Data comprised dietary intake description, clinical and biochemical marker measurements, physical activity and complementary items by questionnaires. They were collected either at home (questionnaires and, if subjects did not want to go to a health centre, anthropometry and blood pressure measurements and biochemical samples with a nurse), by phone (24 h diet recalls) or at a health examination centre of the National Health Insurance System (Caisse nationale d'assurance maladie des travailleurs salariés).
Repeated 24 h dietary recalls
Dietary intake was assessed by three 24 h recalls, one of which was on the weekend, randomly distributed within a period of 2 weeks. Trained dietitians asked subjects to describe all foods and beverages consumed the day before the interview, from midnight to midnight. Subjects gave information on food composition, recipes (especially when they were homemade) and trademark. Amounts consumed were described using a validated photography manual(Reference Le Moullec, Deheeger and Preziosi21) or according to standard measurements (home containers, grams indicated on the package, etc.). Data were entered on software developed for the study that included more than 3400 foods and beverages (NutriXpert®; Medical Expert System, Paris, France). Nutritional values for energy, macronutrients and main micronutrients came from a nutrient database previously published(Reference Hercberg22) and completed for recent market foods and recipes. Individuals were not previously informed of the call day so as to limit changes in diet. Information on home-added fat and addition of salt during food preparation and consumption was separately collected.
Physical activity and sedentary lifestyle
The short-form of the International Physical Activity Questionnaire (IPAQ)(Reference Craig, Marshall and Sjostrom23) in the French language was used. In brief, the numbers of days over the past week in which the subject spent more than 10 min walking and carrying out physical activity of moderate or vigorous intensity were collected. The respective durations on one of these days were collected. Physical activity description was completed by data on time spent sitting down and time spent in front of a screen (television, computer and videogames) during the past 7 d.
Anthropometry and blood pressure measurements
After the diet collection period, adults were offered the possibility of undergoing a clinical and biochemical examination. Anthropometry was measured using identical devices and according to standardized procedures adapted from WHO recommendations(24). Weight was measured to the nearest 100 g on an electronic scale (SECA®) with the subject lightly dressed (wearing mainly underwear) without shoes. Height was measured without shoes to the nearest 0·5 cm with a microgauge (SECA®) attached to the wall. Waist and hip circumferences were measured with a flexible double-graduated tape measure to the nearest 0·1 cm, and the operator was seated at the side. Waist circumference was taken midway between the inferior margin of the last rib and the crest of the ilium.
On the same day, three measurements of diastolic and systolic blood pressure were taken on the left arm using an automatic validated device (OMRON M5-I®) and size cuff for obese subjects, when appropriate. The rest period in the same position prior to measurement was at least 5 min, and measurements were 1 min apart. The arm was placed on a support in that the elbow was in the plane of the heart. A second run of three measurements was carried out if a difference of 10 mm Hg was observed between two recordings.
Biochemical measurements
A peripheral blood sample was taken after a recommended minimum of 12 h of fasting. Eventual food and beverage consumption was collected if taken during the last 12 h. Subjects were asked to collect morning urine and store it at +4°C. Samples were then carried up to the field laboratories within 4 h after collection in frozen containers. Blood samples were immediately centrifuged when appropriate and analysed for cholesterol (total and HDL-cholesterol), TAG, glucose, Hb and ferritin. Most biochemical analyses were performed on an automated Olympus®. Serum cholesterol (total and HDL-cholesterol) and TAG were determined by enzymatic colorimetric methods; LDL-cholesterol was calculated using the ad hoc formula when TAG were < 4·6 mmol/l(Reference Friedewald, Levy and Fredrickson25). Plasma glucose was determined using the hexokinase method and colorimetric measurement. ELISA measurement was used for ferritin determination. Full blood count, including Hb measurement, was performed on a PENTRA® automat. Plasma 25-hydroxyvitamin D was measured by RIA technique and plasma folate and vitamin B12 by competitive immunoassay with direct chemiluminescence detection. Part of the biochemical material was stored at − 80°C until its transport to central laboratories for vitamin D, folate and B12 measurements and long-term storage.
Complementary questionnaires
Social and demographic information was collected through face-to-face questionnaires. Previous illnesses such as CVD and diabetes, as well as current drug intake, were described.
Statistical analyses
The theoretical study size was based on recommendations of the EFCOSUM project which advocated performing at least two repeated 24 h recalls in 2000 individuals in order to describe dietary intake at the country level(Reference Brussaard, Lowik and Steingrimsdottir26). Gender-stratified analyses were previously scheduled due to known differences in diet between men and women.
Descriptive analysis of dietary intake comprised subjects with at least two 24 h recalls and basic social and demographic data. Initial weighting was based on the number of eligible individuals multiplied by the inverse of the probability of dwelling selection in the stratum. Calibration was made, separately for each gender, according to the national census data on age, education diploma and whether the household included or did not include at least one child. The final weighting also included the period of data collection. After exclusion of diet-underreporting subjects (see later), a second set of weighting was estimated in subjects who provided a plausible description of their diet. A third weighting set was calculated for the description of nutritional clinical status in subjects with weight and height available, and a fourth weighting set in subjects with at least the total cholesterol concentration available in order to describe biochemical status. Month of biochemical sample was also taken into account. Means and frequencies with their standard errors were estimated using the STATA® V.10 (Stata Corporation, College Station, TX, USA) declaration for the complex sampling scheme (‘svyset’ function) and ‘svy:’ option.
The social and demographic description was made using raw and weighted data in order to evaluate effects of the weighting procedure. Social characteristics were also compared between included and not-included-in-analyses subjects by t test and χ2 tests when appropriate. Factors associated with inclusion at α < 20 % were included in initial multivariate logistic models. The final model included confounding factors and characteristics associated at P value < 5 %. These investigations were performed in subjects included for diet description (v. underreporting subjects), anthropometry and blood pressure measurements (v. those not included in initial sample) and nutritional markers (v. those not included in initial sample and v. those included for anthropometry and blood pressure description). Throughout the descriptive analyses, a comparison of male and female data was carried out using test procedures adapted to weighted data.
Dietary intake description
Diet-underreporting subjects were identified by the method proposed by Black(Reference Black27). We used Schofield equations to estimate the BMR according to sex, age and weight (and height when available)(Reference Schofield28). When weight was missing, BMR was estimated through regression imputation stratified according to age and sex. BMR was compared to energy intake without alcohol (EI) and by taking into account the physical activity level. A physical activity level of 0·88 was used to identify extremely underreporting subjects and a physical activity level of 1·55 to identify other underreporting subjects. Study-internal coefficients were used for the intra-individual energy CV (CVwEI), while those proposed by Black were used for the BMR CV (CVwB = 8·5 %) and physical activity CV (CVtP = 15 %)(Reference Black27). Comments collected during 24 h recalls were investigated to identify specific conditions that could objectively explain low EI, such as acute disease or low-energy diet to lose weight. Subjects who provided such information were not considered as underreporting subjects, while the other underreporting subjects were excluded from the diet description.
Diet was described as mean energy intake through macronutrients reported on total EI and in grams of food and nutrient intake. Percentages of subjects who attained current national recommendations were estimated. Recommended complex carbohydrate energy (27·5 %EI) was based on total carbohydrate intake, added simple sugars and intrinsic sugars. The recommendation for simple sugars from sweetened foods (12·5 %) was 10 % of added sugars plus 2·5 % of intrinsic simple sugars (essentially from milk and fruits). Foods were classified according to the information provided in the PNNS guides(Reference Hercberg, Chat-Yung and Chauliac10). Some foods were excluded from a group when the PNNS guides clearly indicated their absence from this group. One dish could pertain to several groups or subgroups if it was composed of several components. Daily mean of each food group intake quantity was computerized in grams. The frequency of consumption was the amount consumed divided by a portion size which was specific to the type of foods. These frequencies were then compared to PNNS recommendations. When a PNNS recommendation was not clearly quantified(Reference Hercberg, Chat-Yung and Chauliac10), international and national recommendations were used.
Physical activity
Data obtained by the IPAQ were computed for a metabolic equivalent task (MET-min/week) following recommendations of the IPAQ group(Reference Craig, Marshall and Sjostrom23). The principle is to multiply the metabolic equivalent task value of each level of physical activity intensity (walking, moderate or vigorous) by the time spent per week. Recommended IPAQ categories of physical activity (low, moderate and high) were used in our analyses(Reference Craig, Marshall and Sjostrom23). Sedentary lifestyle was considered as spending more than 3 h/d in front of a screen (television, computer or videogames).
Nutritional markers
Pregnant women were excluded from the anthropometric description. BMI was calculated as weight in kg/height2 in m2. The WHO classification was used to define thinness, overweight and obesity, including three grades of obesity(24). The European reference for waist circumference was used to define central obesity in men ( ≥ 94 cm) and women ( ≥ 80 cm)(Reference Balkau and Charles29). The waist:hip ratio was also calculated; abdominal fat accumulation was estimated through a waist:hip ratio >1·0 in men and >0·85 in women(30). The mean of the last two measurements of blood pressure was used in analyses. Hypertension was defined by systolic blood pressure ≥ 140 mmHg and/or diastolic blood pressure ≥ 90 mmHg (French recommendations as in other countries)(Reference Pickering, Hall and Appel31) and/or intake of drugs affecting blood pressure according to the Anatomical Therapeutic Chemical classification (C02, C03, C07, C08 and C09) (available at http://www.whocc.no/atcddd/). Subjects with fasting duration < 12 h were excluded from analysis based on lipid profile and glucose. Percentages of adults with lipid components or glucose higher than recommended concentrations in France(32, 33) were described, as well as those taking drugs affecting such components (lipid-lowering drugs (C10) or antidiabetic drugs (A10)). International references were used for anaemia (Hb < 130 g/l in men and < 120 g/l in women) and for depleted iron stores (ferritin < 15·0 μg/l)(34). Finally, references usually cited in the literature were used for low vitamin D status(Reference Lips35) and risk of folate deficiency was assessed by plasma folate(Reference Jacques, Selhub and Bostom36).
Results
Participant characteristics
When accounting for withdrawals after initial agreement to participate, the participation rate according to inclusion criteria in analyses for the dietary component of the study was estimated at 59·7 % (3115/(4483 eligible households +734 households in which the contacted person refused to give information on household composition)) (Fig. 1). Missing social and demographic data accounted for 0·8 % of subjects having done at least two 24 h recalls. Among subjects who participated in the dietary component of the study, 77·5 % were measured for weight and height, and blood samples were taken for 67·5 % (Fig. 1).

Fig. 1 Inclusion diagram.
Mean age, birthplace, marital status, presence of a child at home and smoking habits were unmodified by the weighting procedure (Table 1). Weighted proportions of young adults were higher than raw proportions. Low education level was poorly represented in the sample; primary school level rose about 20 % after the weighting procedure. While proportions of service/manual workers and management/intermediate occupations were close in the initial sample, this was no longer the case for weighted proportions (Table 1).
Table 1 Social and demographic characteristics
(Mean values or percentages)

* Weighting accounted for multilevel sampling design and for social and demographic characteristics compared to the national census (age, school diploma, household including at least one child or not).
Nutrient and dietary intake
Diet was described in 2734 subjects after exclusion of underreporting subjects (12·2 %). The risk of being an underreporting subject increased with increasing age (OR = 1·01, 95 % CI 1·00, 1·02, for 1 year), and with place of birth outside France (Europe OR = 1·96, 95 % CI 1·14, 3·36; Africa OR = 1·15, 95 % CI 0·72, 1·86; other place of birth OR = 3·3, 95 % CI 1·56, 6·97, compared to France). Moreover, compared to those who had a primary school level, subjects with a university level were at lower risk of being underreporting subjects (OR = 0·39, 95 % CI 0·27, 0·56). Other social and demographic characteristics were comparable between the two groups.
Nutrient intake was higher in men than in women for EI with or without alcohol, complex carbohydrates (%EI), simple sugars (g/d and %EI), total dietary fibre (g/d), calcium (mg/d) (P < 0·001 for all tests) and saturated fats (%total lipids; P = 0·02) (Table 2). Men also showed a nutrient intake in accordance with recommendations for complex carbohydrates, fibres and calcium that was higher than for women (P < 0·001 for all tests) (Table 2). In both sexes, most adults had simple sugar ( < 12·5 %EI: 74·5 (se 1·2) %) and calcium ( ≥ 2/3 French RDA: 76·4 (se 1·1) %) intake in accordance with recommendations, but compliance with nutrient recommendations was lower for total carbohydrates (>50 %EI: 26·4 (se 1·2) %), total fibre (>25 g/d: 13·7 (se 0·9) %) and SFA ( < 35 % total lipids: 18·5 (se 1·0) %).
Table 2 Daily mean energy and nutrient intake and percentage of adherence to guidelines*
(Mean values or percentages with their standard errors)

EI, energy intake without alcohol.
* For details of subjects and procedures, see Methods and Table 1.
† American Association of Analytical Chemists method.
‡ French RDA: 900 mg/d in adults >18 years, excepting 1200 mg/d in women >55 years and men >65 years.
The male diet was characterized by intake of ‘bread, cereals and legumes’, home-added fats and non-alcoholic beverages mostly in accordance with PNNS recommendations (Table 3). Consumption of fruits and vegetables, seafood and vegetable home-added fat (relatively to animal added fat) was too low compared with PNNS recommendations, while salt intake was too high on average (Table 3). Less than one-third of men had dairy product intake in accordance with the PNNS guidelines (Table 3) and 25·8 (se 1·8) % had a higher intake than the PNNS guidelines. With an intake of 383 g/d on average, consumption of fruits and vegetables was 400 g/d or higher in 44 % of men. Alcohol consumption was higher than the recommendation for 20·0 (se 1·7) % of men. In addition, 25·6 (se 1·9) % had salt intake higher than 12 g/d. In women, ‘meat, seafood and egg’ intake was adequate for most of them, as was home-added fat, sweetened and alcoholic beverages, and salt (Table 3). Dairy product intake was lower than the PNNS guidelines in 54·6 (se 1·6) % of them, while about one-quarter had satisfactory consumption. Intake of ‘bread, cereals and legumes’ was also much too low (Table 3), with 59·6 (se 1·5) % of women consuming less than the PNNS guidelines. Finally, more than half of women had fruit and vegetable intake lower than 400 g/d.
Table 3 Daily mean diet intake and percentages of adherence to guidelines*
(Mean values or percentages with their standard errors)

EI, energy intake without alcohol.
* For details of subjects and procedures, see Methods and Table 1. For each food group, components of composite dishes were proportionally accounted for.
† Including 100 % juices, processed fruit and vegetables; excluding legumes, beans, starchy plants and potatoes.
‡ Excluding desserts with high contents of sugar and fat. Range in 55–74-year-old adults: 2·5–4·5 servings/d.
§ One serving is equivalent to a glass of wine, i.e. 10 g alcohol; only includes consumers.
∥ Including salt added when cooking and during meals; estimated using 24 h recalls.
Physical activity and sedentary lifestyle
Behaviours were described in 2971 subjects due to the fact that there were 4·6 % ‘I don't know’-type answers along with missing data on physical activity. Social and demographic characteristics were comparable between subjects included and not included in physical activity analysis. According to the IPAQ classification, 36·8 (se 1·2) % of adults had a low level of physical activity, 36·7 (se 1·1) % an intermediate level and 26·5 (se 1·1) % had a high level of physical activity. Low physical activity was comparable in men and women, but the proportion of men with a high level of physical activity was higher than that of women (P = 0·02) (Table 4).
Table 4 Physical activity and sedentary lifestyle indicators*
(Mean values or percentages with their standard errors)

IPAQ, International Physical Activity Questionnaire; MET, metabolic equivalent task.
* For details of subjects and procedures, see Methods and Table 1.
† Weighted mean of working days and leisure days.
Time spent in front of a screen was about 3 h 20 min/d, which was overall much higher in men than in women (P < 0·001) (Table 4). During working days, such sedentary activity (mean duration: 161 (se 3·3) min/d) was, as expected, less long than during leisure days (mean duration: 222 (se 3·9) min/d). During working days, television viewing time was comparable between men and women, but not during leisure days (P = 0·03) (Table 4). Finally, some two-thirds of adults spent more than 2 h/d watching television, whatever the day.
Clinical and biochemical markers of nutritional status
Anthropometry and blood pressure were described in 2413 adults. These subjects were not comparable to those not included (n 702) for age (OR = 1·02, 95 % CI 1·01, 1·03, for 1 year), living status (living with a partner OR = 1·32, 95 % CI 1·04, 1·68, compared to being single) or school level (secondary school OR = 1·37, 95 % CI 1·02, 1·84; high school OR = 1·40, 95 % CI 1·01, 1·95; university OR = 1·85, 95 % CI 1·36, 2·52, compared to primary school). Biochemical markers were described in 2102 subjects who were older (OR = 1·02, 95 % CI 1·01, 1·02, for 1 year) and had a higher education level (secondary OR = 1·48, 95 % CI 1·14, 1·92; high school OR = 1·39, 95 % CI 1·04, 1·86; university OR = 2·11, 95 % CI 1·60, 2·78, compared to primary school level) than those not included (n 1013). In the end, subjects included in the biochemical description were different from those included in anthropometry and blood pressure descriptions in terms of sex (women OR = 0·72, 95 % CI 0·55, 0·95, compared to men) or school level (university OR = 2·06, 95 % CI 1·38, 3·08, compared to primary school).
About half of adults were found to be at high cardiovascular risk based on hypercholesterolaemia and intake of lipid-lowering treatments (61·4 (se 1·6) %), overweight (49·3 (se 1·4) %) and dyslipidaemia (44·1 (se 1·6) %). Frequencies of high waist:hip ratio (21·1 (se 1·2) %) and hypertension (30·9 (se 1·3) %) were lower. Despite comparable obesity frequency, women were more frequently at cardiovascular risk than men, based on waist circumference (P = 0·002), waist:hip ratio (P < 0·001) and elevated cholesterol (not taking into account drug intake; P = 0·04) (Table 5). In contrast, men were more frequently affected by high blood pressure (P < 0·001), hypertension (P = 0·02), dyslipidaemia (P < 0·001), hyperglycaemia (P = 0·015) and diabetes (P = 0·015) (Table 5).
Table 5 Anthropometry, blood pressure, cholesterol and glucose status*
(Mean values or percentages with their standard errors)

BP, blood pressure; M, men; W, women.
* For details of subjects and procedures, see Methods and Table 1.
† Pregnant women excluded (n 25).
‡ Systolic BP ≥ 140 mm Hg and/or diastolic BP ≥ 90 mm Hg.
§ Elevated BP and/or taking drugs acting on BP.
∥ TAG ≥ 1·7 mmol/l and/or LDL-cholesterol ≥ 4·1 mmol/l and/or HDL-cholesterol ≤ 1·0 mmol/l and/or lipid-lowering drug intake.
¶ Non-fasting in subjects taking anti-diabetic drugs.
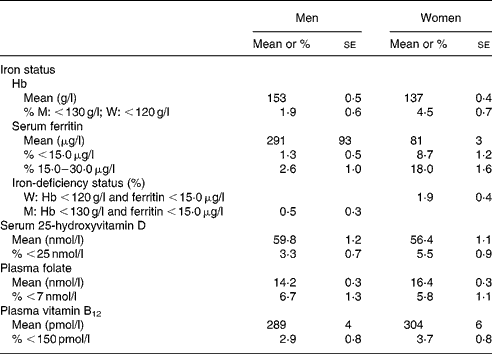
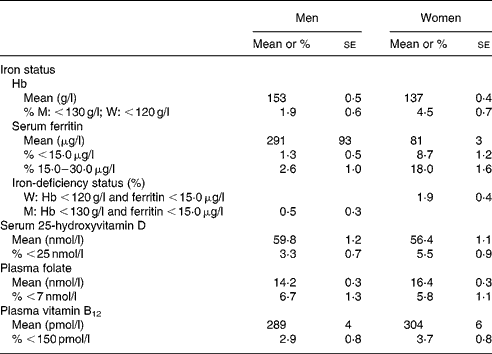
Iron deficiency was more frequent in women than in men (P = 0·03) (Table 6). In women of childbearing age (18–49 years of age), frequency of iron deficiency was 3·0 (se 0·7) %, frequency of anaemia was 5·7 (se 1·0) %, and 13·5 (se 1·8) % of them had depleted iron stores based on concentrations of plasma ferritin. Risk of folate deficiency was observed in 6·2 (se 0·9) % of adults. Mean plasma folate was higher in women than in men (P < 0·001), but the frequency risk of deficiency was comparable (Table 6). A total of 7·7 (se 1·7) % of women of childbearing age presented such a risk. Low vitamin D status was revealed in 4·5 % (se 0·6) of adults, with higher risk in women than in men (P = 0·04) (Table 6). Finally, low status of plasma vitamin B12 was observed in 3·3 (se 0·6) % of adults.
Discussion
The ENNS survey provides a recent overview on dietary intake, physical activity and nutritional status in 18–74-year-old adults in France. The diet appears to be heterogeneous, with satisfactory intakes of total energy, simple sugar, calcium and alcohol, but does not have a well-balanced intake of macronutrient, SFA or total fibre according to current recommendations. While fruit and vegetable consumption and fish intake were lower than current PNNS guidelines, food intake was generally in compliance with recommendations for other food groups. However intake of salt and dairy products was too high in men. In contrast, ‘bread, cereals and legumes’ and dairy product consumption was below the guidelines in women. According to anthropometry, blood pressure and lipid profiles, cardiovascular risk was elevated in 18–74-year-old adults. In other respects, vitamin status was at risk of deficiency in less than 10 % of adults. Finally, over two-third of adults had satisfactory physical activity, but most spent a long time in front of a screen.
The present survey, the first of its kind to be conducted in France, is of interest in surveillance and monitoring of public health programmes. In the present study, the participation rate in diet data collection attained 60 %, considered statistically acceptable, but the overall participation rate fell to 40 % for biochemical sampling. Improvement in the participation rate is a critical point in such studies so as to minimize the selection bias as much as possible. It is unknown as to whether initial contact, organized home visits, survey topics, individual and global result return, and staff quality had an effect upon the participation rate(Reference Mapstone, Elbourne and Roberts37). No incentive was offered to subjects but participation in the health examination was expanded by home visits from a nurse. Despite a high acceptability rate and quality of the data, the home visit strategy is costly(Reference Siemiatycki38). Comparisons of crude and weighting data as well as subject characteristics according to their entire or partial participation showed recruitment biases. In particular, low-income subjects were less often included than would be desirable. These biases were compensated for by weighting statistics.
Nutrient and dietary intake
Comparisons to Western nutritional surveys are limited due to variations in sampling schemes and dietary collection methods. Data treatment also has an impact on observations (food group classification, nutritional value table). However, the diet description shows patterns comparable to previous descriptive Western studies, including insufficient carbohydrate and elevated fat intake, especially that of saturated fats(Reference Elmadfa, Weichselbaum and Konig13). Recent US trends show a decrease in fat energy intake along with an increase in total energy and carbohydrate intake(Reference Briefel and Johnson11). Repeated European surveys do not clearly indicate whether such changes are ongoing or not(Reference Turrini, Saba and Perrone16, Reference Serra-Majem, Ribas-Barba and Salvador39). Trends are difficult to interpret in France due to the absence of published studies using comparable methods(Reference Volatier and Verger17). Salt intake was generally too high, especially in men, although it seemed to progressively attain current French recommendations. As previously shown(Reference Reinivuo, Valsta and Laatikainen14), this might be related to a decrease in energy intake.
These patterns are consistent with food group consumption described as complying with PNNS recommendations. The insufficient calcium intake in women is partly related to insufficient consumption of dairy products and milk. In France, lipid intake seems to depend more on consumption of foods that contain fat such as processed meat, cheese, snacking foods etc. rather than on home-added fats such as butter, margarine, oils etc. Indeed, while the lipid intake remained too high, home-added fat consumption was satisfactory. Regarding food groups globally, the French nutritional situation would appear to be intermediate between a protective Mediterranean diet in southern Europe and a northern European diet(Reference Slimani, Fahey and Welch40). Variations had also been observed within the French territory up until recently(Reference Kesse, Boutron-Ruault and Clavel-Chapelon19). Regional variations were taken into account in our survey, by recruiting throughout continental France.
The dietary overview provided by the ENNS survey must be interpreted with caution, since some limitations were present. Three 24 h recalls were carried out in a 15 d period: at the individual level, this is not sufficient to describe the usual intake. The description of some nutrient intakes (carbohydrates and calcium, for instance) might require more than three 24 h recalls(Reference Mennen, Bertrais and Galan41). However, the present data are reliable at the group level, since recruitment and diet information collection were carried out throughout the entire territory during a 1-year period(Reference Brussaard, Lowik and Steingrimsdottir26). For calcium intake, supplements are not taken into account, since PNNS guidelines explicitly discourage their consumption, with a few specific exceptions(Reference Hercberg, Chat-Yung and Chauliac10).
Physical activity and sedentary lifestyle
Regarding physical activity, one European survey, using the short-form IPAQ, showed that the prevalence of satisfactory activity (e.g. the high category of IPAQ) in France (24·1 %) was among the lowest frequencies in Europe, while frequencies in Germany (40·2 %) and the Netherlands (44·2 %) were among the highest(Reference Sjostrom, Oja and Hagstromer42). The difference between men and women might be explained by leisure-time physical activity, especially sports, more commonly practised by men than women in France(Reference Oppert, Thomas and Charles43). Despite conclusive validation(Reference Craig, Marshall and Sjostrom23), IPAQ use is considered to lead to overestimation of moderate and vigorous physical activity. The quality of the interview is crucial and must be carefully prepared. Indeed, it is a useful tool for surveillance, since physical activity is examined under all conditions (work, transportation, leisure time, etc.)
Clinical and biochemical markers of nutritional status
The French dietary pattern, along with insufficient physical activity, helps to explain the high prevalence of cardiovascular risk observed in the ENNS survey. In France, body mass changes have been mainly monitored during the last decade by surveys using self-measured weight and height(Reference Charles, Eschwege and Basdevant18). Between 1997 and 2006, a continuous increase in overweight and obesity has been observed in both male and female adults (obesity prevalence equal to 12·5 and 13·6 %, respectively, in 2006). As expected(Reference Niedhammer, Bugel and Bonenfant44), we found a higher cross-sectional prevalence of obesity based on measured anthropometry. Based on declared anthropometry, the French frequency of overweight and obesity was among the lowest in Europe up until the beginning of the 2000s(Reference Seidell45), but comparisons should now be made using measured anthropometry. For example, when compared to the 14·2 % obesity based on measured data in 2003–5 in 18–64-year-old Portuguese adults(Reference doCarmo, DosSantos and Camolas46), the French prevalence was somewhat higher.
Using comparable methods of measurement but different age categories (18–74 years v. ≥ 18 years), the prevalence of hypertension in 2006–7 in France was equal to the frequency observed in 2003–4 in the USA (29·6 %)(Reference Ong, Cheung and Man12). Compared to European data, mean systolic blood pressure in France in 2001 was comparable to the mean reported in 19–64-year-old adults in the UK (130 mm Hg in men and 122 mm Hg in women), whereas this was not the case for diastolic blood pressure (73 and 68 mm Hg, respectively)(Reference Ruston, Hoare and Henderson47). Methods of measurements must be taken into account when interpreting variations across surveys.
In France, adults appeared to be exposed to factors leading to metabolic syndrome, diabetes and their associated cardiovascular manifestations, but differed from other Western countries. For example, the mean total cholesterol and frequency of elevated total cholesterol were higher than reported values from the 1999–2004 National Health and Nutrition Examination Survey but with a frequency of high LDL-cholesterol comparable in women and lower in men(Reference Hyre, Muntner and Menke48). The same tendency was observed when comparison was made with similar surveys in the UK(Reference Ruston, Hoare and Henderson47) and in Finland(Reference Ilanne-Parikka, Eriksson and Lindstrom49). This illustrates the widely described ‘French paradox’ of elevated total cholesterol and dyslipidaemia but lower LDL-cholesterol and higher HDL-cholesterol concentrations. Despite an insufficient explanation per se, such variations could contribute to understanding variations in cardiovascular mortality across Europe(Reference Muller-Nordhorn, Binting and Roll7).
For biomarkers of vitamin and mineral status, comparable surveys aimed at describing overall nutritional status are lacking, except for the National Diet and Nutrition Survey conducted in 2001–2 in the UK(Reference Ruston, Hoare and Henderson47). One of our limitations compared to the UK survey was that Hb and ferritin were measured in field laboratories, while UK analyses were centralized. However, folate, vitamin B12 and vitamin D measurements were centralized in the ENNS survey, the assay methods being comparable with those used in the UK survey. Anaemia and serum ferritin depletion were more frequent in France, especially in women, than in the UK. Folate status was also less satisfactory in France than in the UK, possibly due to supplements and enriched foods, which may be less frequently consumed in France. The vitamin B12 status was comparable, however, in the two surveys. In contrast, and as expected, the vitamin D status was much more satisfactory in France than in the UK, where about 14 % of adults(Reference Ruston, Hoare and Henderson47) were at risk of deficiency compared to 4·5 % in France. Variations in diet between the two countries should be carefully examined in order to understand these results.
The ENNS survey provides a complete description of nutritional characteristics in adults using reference methods recommended for diet, physical activity and nutritional status investigation. The present study elucidates a contrasting but globally unsatisfactory nutritional situation in France. This data set constitutes an essential tool for monitoring public health programmes such as the PNNS. Beyond national monitoring, such data are useful for international comparisons in order to better understand morbidity and mortality variations across countries.
Acknowledgements
ENNS was supported by the French Institut de veille sanitaire (InVS), the Université de Paris 13, and the Caisse nationale d'assurance maladie des travailleurs salariés (CnamTS). We thank the dietitians, nurses and physicians, the staff of Health Examination Centres of CnamTS, their laboratories, the Grenoble Universitary Hospital Center (Département de Biologie Intégrée), U.631 Inserm and the Pasteur Institute which contributed to data collection and biochemical analyses. K. C. designed the study, managed the data acquisition, performed statistical analysis, interpreted the data and wrote the manuscript. M. V., A. M., B. S. and V. D. contributed to the management of data collection, performed the statistical analysis, interpreted the data and revised the manuscript. C. R., A. O. and E. S. contributed to the data collection, provided administrative and material support, and participated in the statistical analysis. S. H. designed the study, contributed to the interpretation of results and revised the manuscript. All authors read and approved the final version of the manuscript. All authors declare no personal or financial interest in the content of the paper.