The metabolic syndrome (MetS) can be defined as a set of metabolic risk factors involved in the development of CVD and/or type 2 diabetes( Reference Grundy, Cleeman and Daniels 1 ). Abdominal obesity and insulin resistance play a key role in the genesis of this syndrome.
The MetS has increased in epidemic proportions worldwide( Reference Lakka, De and Ta 2 – Reference Erejuwa, Sulaiman and Ab Wahab 5 ). Currently, the search for other factors that cause the MetS, or alternatives that may prevent its occurrence, is often associated with the intestinal microbiota. Indeed, recent findings indicate that altered gut microbial composition and diversity have a vital role in the pathophysiology of metabolic disorders, as the commensal gut microbes modulate host metabolism by affecting energy extraction from food and by biochemically converting molecules derived from the host or from the gut microbes themselves( Reference Erejuwa, Sulaiman and Ab Wahab 5 – Reference Shen, Obin and Zhao 7 ).
The imbalance of the intestinal microbiota has been strongly associated with the occurrence of cardiovascular and neurological diseases, decrease of immune function, increase in oxidative stress and many other dysbiosis( Reference Bäckhed, Ley and Sonnenburg 8 – Reference Carding, Verbeke and Vipond 11 ).
In contrast, consumption of probiotics has been associated with the gut microbial balance and, consequently, various positive actions on host health are reported, including beneficial effects on lipid and glucose metabolism, inflammatory state and oxidative stress in healthy subjects and in those with many metabolic and inflammatory diseases( Reference Nagpal, Kumar and Kumar 12 , Reference Miglioranza Scavuzzi, Miglioranza and Henrique 13 ). Although the effects of probiotics on oxidative stress are still conflicting( Reference Salehi-Abargouei, Ghiasvand and Hariri 14 ), several reports showed that probiotics in patients with metabolic diseases resulted in favourable metabolic consequences especially reducing oxidative stress in diabetic patients( Reference Salehi-Abargouei, Ghiasvand and Hariri 14 , Reference Mirmiran 15 ). However, studies of probiotics in relation to oxidative stress in patients with the MetS have not been performed yet.
In a previous study, we reported the effects of Bifidobacterium lactis HN019 in patients with the MetS( Reference Bernini, Simão and Alfieri 16 ). The group that ingested probiotic milk for 45 d presented favourable effects on lipid profile and inflammatory biomarkers (TNF-α and IL-6) when compared with the control group, which did not receive the probiotic milk.
However, some questions have emerged after the aforementioned study: which differences would be shown in a study comparing healthy subjects with the MetS patients? How would oxidative stress biomarkers behave in such a comparison? Would the beneficial effects of the same probiotic last for even longer periods of time? Thus, the aim of this study was to evaluate the effects on inflammatory state and oxidative stress of B. lactis HN019 in patients with and without the MetS, whose diet was supplemented with the probiotic fermented milk for 90 d.
Methods
Study design
The study was conducted according to the guidelines in the Declaration of Helsinki and approved by the Ethical Committee involving humans of the University of Londrina, Parana, Brazil, protocol number 469.555/201. This was a randomised and double-blind study. A total of thirty-three patients, men and women, aged between 18 and 60 years were recruited from a health facility in the city of Jataizinho, Parana State, Brazil, and received detailed information about the purpose and procedures of the study and agreed to participate and signed a consent form. Thus, the volunteers were divided in two groups: patients without the MetS (control group, n 14) and patients with the MetS (n 19). Patients with the MetS were selected among volunteers who presented three or more of the following five criteria: (1) waist circumference (WC) ≥102 cm in men and 88 cm in women, (2) fasting TAG levels ≥150 mg/dl (≥1·7 mmol/l), (3) HDL ≤40 mg/dl (≤1·0 mmol/l) in men or ≤50 mg/dl (≤1·3mmol/l) in women, (4) blood pressure ≥130/85 mmHg (or anti-hypertensive medication use) and (5) fasting glucose levels ≥100 mg/dl (≥5·6 mmol/l) or the use of antidiabetic medication( Reference Grundy, Cleeman and Daniels 1 ).
All individuals daily ingested 80 ml of the probiotic milk containing an average of 3·4×108 colony-forming units (CFU)/ml of Bifidobacterium animalis subsp. lactis subsp. nov. HN019 for 90 d. Anthropometric measurements and biochemical parameters were assessed in blood or plasma samples before (T0) and after 90 d (T90) of probiotic milk ingestion.
Inclusion and exclusion criteria
Inclusion criteria were the ages between 18 and 60 years, and the MetS diagnosis criteria according to the National Cholesterol Education Program, Adult Treatment Panel III( Reference Grundy, Cleeman and Daniels 1 ). Exclusion criteria were thyroid, adrenal, renal, hepatic, gastrointestinal, infectious or oncological diseases; the utilisation of hormone replacement therapy; vitamins; antioxidant supplements; antibiotics and anti-inflammatories; and ingestion of foods or supplements containing probiotic micro-organisms, besides lactose-intolerant individuals. The individuals of both groups did not drink alcohol regularly. In addition, the volunteers were instructed not to modify their eating habits and/or physical activities and other lifestyle factors, as well as to not use another probiotic or antibiotic throughout the intervention period.
Milk fermented with probiotics
The commercial strain Bifido HOWARU® Bifidobacterium lactis HN019 (Danisco) was used to produce the probiotic milk with 3·4×108 CFU/ml. The probiotic milk was produced and packaged aseptically at the Laboratory of Microbiology of the University of North Parana, according to the current Brazilian legislation( 17 ). The product ready for consumption presented 0·38 % acidity (lactic acid), a pH of 5·15, 2·80 % protein, 7·54 % carbohydrates, 0·0 % fat, 12·08 % total solids and 0·48 % ash, which resulted in 33·09 energy content/bottle. In addition, the final product contained 0·01 % (v/v) orange and/or vanilla flavour( Reference Bernini, Simão and Alfieri 16 ). Pathogens were not detected, as required by legislation( 18 ); thus, the product was characterised as suitable for consumption. Weekly, seven bottles of 80 ml were distributed to each volunteer during 13 weeks (90 d), and the patients were instructed to drink one bottle daily for breakfast.
Waist circumference and blood pressure measurements
WC was measured with a soft tape on subjects in a standing position midway between the lowest rib and the iliac crest. Three blood pressure measurements, systolic (SBP) and diastolic blood pressures (DBP), taken with a 1-min interval between them after the subject had been seated were recorded. The mean of these measurements was used in the analysis( Reference Pickering, Hall and Appel 19 ).
Measurements of serum high-sensitivity C-reactive protein, cytokines and immune mediators
Blood samples were obtained after 12 h of fasting at the Central Health facility in the city of Jataizinho, Parana State, Brazil. The samples were collected and taken to the Clinical Immunology Laboratory at the Londrina University Hospital for analysis. The plasma and serum were divided into aliquots and stored in a freezer at −70°C (Indrel) until analysis. For further analysis, the samples followed routine examinations in that laboratory. Serum high-sensitivity C-reactive protein (hsCRP) was measured using a nephelometric assay (DadeBehring). Serum homocysteine level was determined by chemiluminescence microparticule immunoassay (Architect; Abbott Laboratory). In addition, IL-6, leptin and adiponectin were measured by a sandwich ELISA using a commercial immunoassay (R&D System).
Oxidative and nitrosative stress markers
Tert-butyl hydroperoxide-initiated chemiluminescence
Plasma levels of lipid hydroperoxide were evaluated by tert-butyl hydroperoxide-initiated chemiluminescence (CL-LOOH) as described previously( Reference Gonzalez Flecha, Llesuy and Boveris 20 ), and the results were expressed in relative light units.
Determination of nitric oxide metabolites
Serum levels of nitric oxide metabolites (NOx) were assessed by nitrite (NO2 −) concentration according to the Griess reaction, supplemented by the reduction of nitrate to nitrite with cadmium( Reference Guevara, Iwanejko and Dembińska-Kieć 21 , Reference Navarro-Gonzálvez, García-Benayas and Arenas 22 ).
Total radical-trapping antioxidant parameter
Total radical-trapping antioxidant parameter (TRAP) was determined as reported by Repetto et al. ( Reference Repetto, Reides and Gomez Carretero 23 ). This method detects hydrosoluble and/or liposoluble plasma antioxidants by measuring the chemiluminescence inhibition time induced by 2,2-azobis (2-amidinopropane). The system was calibrated with the vitamin E analogue Trolox. Serum uric acid levels were determined using a biochemical auto-analyser (Dimension Dade AR; Dade Behring) and were used to correct the TRAP values. TRAP measurements in conditions associated with hyperuricaemia, such as the MetS, may be inaccurate because uric acid concentration accounts for 60 % of total plasma antioxidant capacity. Thus, a correction of TRAP based on uric acid concentration was performed( Reference Venturini, Simão and Scripes 24 ).
Sulphydryl groups
Sulphydryl (SH) groups of proteins were evaluated in plasma samples by a spectrophotometric assay based on 2,2-dithiobisnitrobenzoic acid, as reported previously, and the results are expressed in μm ( Reference Hu 25 ).
Statistical analysis
The sample size was calculated to obtain a statistically significant result when changes of the parameters evaluated were at >10 % level. This study was performed to obtain 80 % statistic power. The Shapiro–Wilk test was used to assess normality of distribution. Logarithmic transformation of continuous data was used in the analyses (SBP, DBP, hsCRP and leptin) when the variables were not normally distributed or when there was heterogeneity of variance (as assessed with the Levene test). Analyses of contingency tables (χ 2 or Fisher’s test) were used to check the associations between categorical variables (sex, ethnicity, smoking, physical exercise, hypertension, diabetes mellitus, the MetS and insulin resistance), and data were expressed as absolute number (n) and percentage (%). Student’s t test (WC, blood pressure measurements, homocysteine, hsCRP and oxidative and nitrosative stress (O&NS) markers) or Mann–Whitney (IL-6) test was performed to compare differences between parameters of groups at baseline and differences across treatment groups (intergroup changes). Paired Student’s t test (WC, blood pressure measurements, homocysteine, hsCRP and O&NS markers) or Wilcoxon matched pairs test (IL-6) was performed to verify changes from baseline (intra-group changes), and data were expressed as means with their standard errors. All statistical analyses were performed using IBM SPSS windows version 22( 26 ). Tests were two-tailed, and an α level of 0·05 indicated statistically significant results.
Results
All participants completed the study after 90 d. There were no differences between the groups without the MetS and with the MetS in relation to age, sex, ethnicity, smoking habit, physical exercise and the number of patients with diabetes mellitus and insulin resistance. The majority of the patients (58 %) from the MetS group presented with hypertension (P<0·001), whereas this characteristic was not seen in any subject of the control group (Table 1). A total of three patients in each group used statins, whereas none of the patients in the control group and six patients in the MetS group used anti-hypertensive medications (data not shown).
Table 1 Characteristics of the study populationFootnote * (Numbers and percentages; mean values with their standard errors)
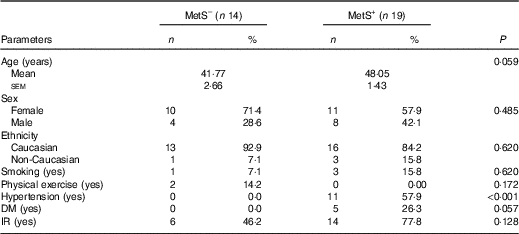
MetS–, subjects without the metabolic syndrome; MetS+, subjects with the metabolic syndrome; DM, diabetes mellitus; IR, insulin resistance (homeostatic model assessment for insulin resistance ≥2·5).
* Student’s t test was used.
There were no significant inter- or intra-group differences observed in SBP, DBP, hsCRP, SH and leptin levels (Table 2). On the other hand, in relation to the baseline values (intra-group changes), subjects in both groups showed a decrease in homocysteine (P=0·02 and P=0·03, respectively), hydroperoxides (P=0·02 and P=0·01, respectively) and IL-6 levels (P=0·02). In addition, increased adiponectin and NOx levels were observed only in the group with the MetS (Fig. 1(a) and (b)). In contrast, only the individuals without the MetS had increases in TRAP levels (P=0·002) (Fig. 1(c)).

Fig. 1 Concentrations of adiponectin (a), nitric oxide metabolites (NOx) (b) and total radical-trapping antioxidant parameter (TRAP) (c) in patients with the metabolic syndrome (MetS+) and without (MetS–), evaluated at the beginning of the study (T0, ![]() ) and after 90 d (T90,
) and after 90 d (T90, ![]() ) of probiotic milk ingestion. The t test was performed to compare differences between parameters of groups at baseline and differences across treatment groups (intergroup changes). Values are means, with their standard errors represented by vertical bars.
) of probiotic milk ingestion. The t test was performed to compare differences between parameters of groups at baseline and differences across treatment groups (intergroup changes). Values are means, with their standard errors represented by vertical bars.
Table 2 Effects of consuming Bifidobacterium lactis HN019 in subjects with the metabolic syndrome (MetS, MetS+) and without the MetS (MetS−) evaluated at the beginning of the experiment (T0) and after 90 d (T90) (Mean values with their standard errors)
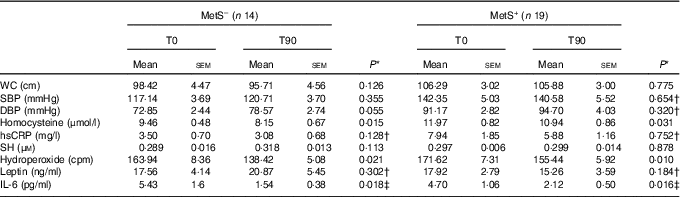
WC, waist circumference; SBP, systolic blood pressure; DBP, diastolic blood pressure; hsCRP, high-sensitivity C-reactive protein; SH, sulfhydryl groups of proteins; cpm, counts per million.
* Paired Student’s t test was used.
† Variables processed in logarithmic transformation.
‡ Non-parametric paired test: Wilcoxon.
Discussion
Principal findings
The main finding of this study was the beneficial effects of B. lactis HN019 on adiponectin and NOx levels in the group of patients with the MetS and on TRAP in the group of patients without the MetS. In addition, B. lactis HN019 showed beneficial effects on homocysteine, hydroperoxides and IL-6 independently of the presence of the MetS.
Beneficial effects of Bifidobacterium lactis HN019 in patients with and without the metabolic syndrome
Although inflammation has been recently considered as a mechanism of immune defence and repair( Reference Lu, Yu and Guo 27 ), the intriguing pro- and/or anti-inflammatory actions of IL-6 is still a matter of discussion( Reference Eder, Baffy and Falus 28 , Reference Scheller, Chalaris and Schmidt-Arras 29 ). In the present study, it is feasible to suggest that the reduction in IL-6, which occurred together with the decrease in homocysteine and hydroperoxide levels, can be considered a beneficial effect. Our group has performed some studies that also reported that the consumption of Lactobacillus plantarum ( Reference Barreto, Colado Simão and Morimoto 30 ) and B. lactis ( Reference Bernini, Simão and Alfieri 16 ) reduced IL-6 levels in patients with the MetS. In addition, the reduction of cytokine IL-6 corroborates the study of Cani et al.( Reference Cani, Neyrinck and Fava 31 ) that associated the decrease of pro-inflammatory cytokines with the increased levels of Bifidobacterium species in high-fat-diet-induced diabetes in mice.
We are not aware of any study to date that has evaluated oxidative stress with probiotics in patients with the MetS. Probiotics have been shown to reduce pro-oxidant biomarkers in patients with diabetes mellitus type 2( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 , Reference Hariri, Salehi and Feizi 33 ). Ejtahed et al. ( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 ) reported a reduction in malondialdehyde (MDA) levels using a yogurt enriched with B. lactis and Lactobacillus acidophilus, whereas Hariri et al.( Reference Hariri, Salehi and Feizi 33 ) found a decrease in 8-hydroxy-2'-deoxyguanosine levels using probiotic soya milk containing L. plantarum. In addition, in healthy volunteers with high levels of γ-glutamyltransferase, Kang et al.( Reference Kang and Lee 34 ) showed a decrease in MDA levels with Lactobacillus brevis. Although we used a different methodology (CL-LOOH) to evaluate oxidative stress, our results with B. lactis in healthy subjects and patients with the MetS are in agreement with the aforementioned studies. In contrast, other reports have not shown changes in oxidative stress in healthy aged individuals using the probiotic VSL#3, a multistrain cocktail composed of Streptococcus thermophilus and several species of Lactobacillus and bifidobacteria( Reference Valentini, Pinto and Bourdel-Marchasson 35 ), and in patients with diabetes mellitus type 2 using L. acidophilus and B. lactis ( Reference Tonucci, Olbrich dos Santos and Licursi de Oliveira 36 ). The decrease in inflammation and oxidative stress by probiotics has been attributed to their effects on scavenging superoxide and hydroxyl radicals, decreasing expression of IL-6 in adipocytes and decreasing adiposity( Reference Asemi, Zare and Shakeri 37 ).
Regarding homocysteine, studies have proposed that increased concentration of total plasma homocysteine could represent an additional independent risk factor for CVD( Reference Fruchart 38 ). A meta-analysis of prospective cohort studies demonstrated that, after accounting for known CVD risk, a 25 % lower homocysteine level was associated with about an 11 % lower risk of ischaemic heart disease and about a 19 % lower risk of stroke( 39 ). Elevated homocysteine levels can occur owing to a lack of vitamins, in particular folate and/or cobalamin, which are required cofactors for homocysteine metabolism through the re-methylation pathway( Reference Selhub 40 ). Milk is a moderate dietary source of folic acid( Reference Sybesma, Starrenburg and Tijsseling 41 , Reference Konstantinova, Vollset and Berstad 42 ). Nevertheless, some micro-organisms that are important for fermented food and/or gut microbiota, such as bifidobacteria, can synthesise folate de novo ( Reference Deguchi, Morishita and Mutai 43 – Reference D’Aimmo, Mattarelli and Biavati 45 ). The recommended daily intake of folate is 300 μg for men, 400 μg for women and 500 μg for lactating or pregnant women. However, these levels are not easy to reach( Reference D’Aimmo, Mattarelli and Biavati 45 ). Milk provides 20–50 µg folate/l, whereas in fermented milk this amount increases to 110 µg/l( Reference Sybesma, Starrenburg and Tijsseling 41 ). In this study, the beneficial effect found on homocysteine levels in both groups permits one to suggest that even a moderate quantity of folic acid present in probiotic milk can decrease this CVD risk factor. This is the first study, to our knowledge, to show decreased homocysteine levels with a probiotic Bifidobacterium species. However, other studies performed with L. plantarum ( Reference Barreto, Colado Simão and Morimoto 30 ) and L. acidophilus ( Reference Mohammad, Molloy, Scott and Hussein 46 ) have already reported this finding.
Link between the effects of homocysteine and oxidative stress
The association between homocysteine and oxidative stress has been shown in patients with type 2 diabetes mellitus, hypertension, atherosclerosis and the MetS( Reference Tyagi 47 , Reference Dominguez, Galioto and Pineo 48 ). Tyagi( Reference Tyagi 47 ) showed that homocysteine induces oxidative stress by increasing nitric oxide synthase while decreasing endothelial nitric oxide synthase (eNOS) in cardiac microvascular endothelial cells. In the present study, the effects of probiotics decreasing concomitantly homocysteine and hydroperoxide levels seem to reinforce this association.
Beneficial effects of Bifidobacterium lactis HN019 only demonstrated in patients with the metabolic syndrome
The adipose tissue also secretes adiponectin, a protein showing anti-inflammatory activity, which inhibits TNF-α production, adhesion molecule expression and nuclear transcriptional factor κB signalling, a pivotal pathway in inflammatory reactions in endothelial cells. In addition, adiponectin is anti-atherogenic and is an insulin-sensitising agent( Reference Ouchi, Kihara and Arita 49 , Reference Hotta, Funahashi and Bodkin 50 ). Obesity, especially visceral obesity, may lead to a decreased secretion of adiponectin through feedback inhibition, thereby suppressing the beneficial effects of adiponectin on insulin sensitivity, and decreased adiponectin levels have been found in patients with obesity, type 2 diabetes mellitus, arterial hypertension and the MetS( Reference Santaniemi, Kesäniemi and Ukkola 51 , Reference Simão, Lozovoy and Simão 52 ). Similarly to the results obtained in the current work, adiponectin levels also increased in obese subjects using Lactobacillus gasseri ( Reference Kim, Park and Kim 53 ). In addition, an experimental study showed an increase in adiponectin levels with Lactobacillus rhamnosus supplementation in high-fat-diet-fed mice( Reference Kadooka, Sato and Imaizumi 54 ).
The mechanisms by which probiotics increase adiponectin levels are largely unknown. Although it is conceivable to suggest an effect related to the decrease in pro-inflammatory cytokines, such as IL-6, demonstrated in the present study, other mechanistic insights cannot be discharged. For example, conjugated linoleic acid is produced by some species of Lactobacillus (e.g. acidophilus, plantarum, paracasei and casei) and has the potential to act as a PPARγ agonist, which up-regulates adiponectin and down-regulates inflammation and adiposity( Reference Nakamura and Omaye 55 ).
Although endothelial dysfunction has been considered an important issue in patients with the MetS, results of studies on serum NOx levels in these patients have been contradictory( Reference Sun, Hu and XH 56 – Reference Simão, Lozovoy and Simão 58 ). The majority of the studies support the hypothesis that even in low-grade inflammatory processes, such as in the MetS, NO is consumed in a reaction with superoxide anion yielding a strong oxidant species, ONOO−, which in turn accelerates the lipid peroxidation reaction( Reference Tao, Gao and Jiao 59 ). The increase in NOx levels with B. lactis is coherent with both improvement in endothelium dysfunction and decreased oxidative stress found in this study. Other reports also showed an increase in NOx after utilisation of probiotics in rats; VSL#3 prevented endothelial dysfunction in rats with portal hypertension( Reference Rashid, Khodja and Auger 60 ), whereas kefir, a probiotic containing different strains, restored the production and release of NOx in streptozocin-induced diabetic rats( Reference Maciel, Punaro and Rodrigues 61 ). Esposito et al. ( Reference Esposito, Iacono and Bianco 62 ) reported that VSL#3 reduced several pro-inflammatory and pro-oxidant biomarkers, including NF-κB, in rats with non-alcoholic fatty liver disease, a condition strongly associated with the MetS. In addition, the same authors reported that probiotics increased PPARα expression, which explained the important anti-inflammatory and antioxidant effects on O&NS demonstrated with VSL#3.
Link between the effects of adiponectin and nitric oxide
Epidemiological studies based on different ethnic groups have identified adiponectin deficiency as an independent risk factor for endothelial dysfunction, hypertension, CHD, myocardial infarction and other cardiovascular complications. On the other hand, decreased bioavailability and/or impaired production of NO is considered a major cause of endothelial dysfunction, which is now recognised as one of the earliest changes in atherosclerosis( Reference Goldstein and Scalia 63 , Reference Zhu, Cheng and Vanhoutte 64 ).
In experimental studies, adiponectin has shown to enhance NO production in cultured aortic endothelial cells( Reference Tan, Xu and Chow 65 ), to significantly increase eNOS (83 %) and reduce inducible nitric oxide synthase (70 %) in hyperlipidaemic rats( Reference Li, Wang and Zhang 66 ), and to improve obesity-related hypertension in mice( Reference Ohashi, Kihara and Ouchi 67 ). Adiponectin has anti-inflammatory effects and augments blood flow by enhancing nitric oxide production and activating eNOS, and it may act as a modulator of vascular remodelling by suppressing smooth muscle cell migration, which possibly plays a role in the regulation of atherosclerosis( Reference Ziemke and Mantzoros 68 ). In a previous study, our group has already demonstrated that the association of hypoadiponectinaemia and increased NOx is one of the main reasons of decreasing blood pressure in patients with the MetS using fish oil and soya( Reference Simão, Lozovoy and Bahls 69 ).
Beneficial effects of Bifidobacterium lactis HN019 only demonstrated in subjects without the metabolic syndrome
Several studies have shown the increase in antioxidant defences with probiotics in healthy people and diabetic patients, but, to our knowledge, this is the first study that reported the antioxidant status in patients with the MetS using probiotics. In healthy subjects, significant increases in antioxidants have been seen with different strains of Lactobacillus ( Reference Kang and Lee 34 , Reference Asemi, Zare and Shakeri 37 , Reference Kullisaar, Songisepp and Mikelsaar 70 , Reference Songisepp, Kals and Kullisaar 71 ) and with different methodologies, such as total antioxidant capacity (TAC)( Reference Kullisaar, Songisepp and Mikelsaar 70 , Reference Songisepp, Kals and Kullisaar 71 ), superoxide dismutase (SOD)( Reference Kang and Lee 34 ) and total GSH( Reference Asemi, Jazayeri and Najafi 72 ). Similarly, in diabetic patients, these increases have been reported not only with L. plantarum ( Reference Hariri, Salehi and Feizi 33 ) but also with L. acidophilus associated with B. lactis ( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 ) and cocktails that used some strains of Lactobacillus, Bifidobacterium and S. thermophilus (VSL#3)( Reference Asemi, Zare and Shakeri 37 ); these beneficial effects have been demonstrated by increased TAC( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 ), SOD( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 , Reference Hariri, Salehi and Feizi 33 ) and GSH( Reference Asemi, Zare and Shakeri 37 ). On the other hand, a study using VSL#3 in diabetic patients did not find significant changes in TAC( Reference Tonucci, Olbrich dos Santos and Licursi de Oliveira 36 ). The antioxidant action of Lactobacillus strains has been attributed to the antioxidative effect of bioactive peptides released during fermentation by proteolytic lactic acid bacteria, the expression of MnSOD activity, elimination of hydroxyl and peroxyl radicals and as having the complete glutathione system necessary for glutathione recycling, transporting and synthesis( Reference Ejtahed, Mohtadi-Nia and Homayouni-Rad 32 , Reference Hariri, Salehi and Feizi 33 ). However, the mechanism by which Bifidobacterium strains decreased TAC has still to be elucidated. Unexpectedly, in the current study, antioxidant defences only improved in healthy subjects, but not in the MetS patients. Nevertheless, it is feasible to suggest that lack of TRAP increase in the group with the MetS could be due to the presence of higher body fat, which becomes difficult because of adequate responses of the antioxidant defence mechanisms( Reference Chrysohoou, Panagiotakos and Pitsavos 73 ).
Limitations and strengths
There are some limitations that must be considered in this study. The first limitation is the small number of subjects in the groups. Second, this study does not allow extrapolation of the results with different strains, especially the data on oxidative stress, which can be highly specific( Reference Tonucci, Olbrich dos Santos and Licursi de Oliveira 36 ). However, some strengths of the study can be pointed out. The study is original under some aspects, as follows: first, this is a unique report with probiotics, in which oxidative stress was studied in patients with the MetS; second, even in patients with diabetes mellitus type 2, studies with B. lactis are still scarce; third, the original design of the study compares healthy subjects and patients with the MetS using the same fermented milk with probiotics.
In conclusion, B. lactis HN019 has several beneficial effects on inflammatory and oxidative biomarkers in healthy subjects and the MetS patients supplemented with the same probiotics as our previous study, but for a longer period. Patients with the MetS showed a specific improvement in adiponectin and NOx levels, whereas a specific favourable effect was shown in the antioxidant defences in healthy subjects. If the results obtained in the present study are confirmed, discussion on supplementation of fermented milk with probiotics in healthy subjects and diseases in which insulin resistance is the pièce de resistance may be warranted.
Acknowledgements
The authors thank the CONFEPAR – Agro-Industrial Cooperativa Central for milk donation, Duas Rodas Industrial for flavors donation and the PROSUP – Programa de Suporte à Pós-Graduação de Instituições de Ensino Particulares – for financial support to L. G. S.
This work was supported by Fundação Nacional de Desenvolvimento de Ensino Superior Particular.
L. J. B. was responsible for recruiting the patients, interpretation of the results and the writing of the manuscript. C. H. B. d. S. and L. G. S. were responsible for writing of the manuscript; D. F. A. was responsible for recruiting the patients and the laboratorial analysis. A. N. C. S. and I. D. were responsible for interpretation of the results and the writing of the manuscript. G. N. C. was responsible for the original concept of the study, the study design, interpretation of the results and the writing of the manuscript. All authors read and approved the final manuscript.
The authors declare that there are no conflicts of interest.






