Introduction
Psychoanalytical views of psychoses
In his analysis of the Schreber delusional system, Reference Freud and StracheyFreud (1911) set the tone for psychological treatments for schizophrenia and allied psychoses for a generation. First, he argued that Schreber's grandiose and persecutory system was meaningful, and we have much to be grateful for in that. This was not simply the aberrant firing of misplaced neurons, but a delusional system that was understandable in terms of both form and content. The delusional system was seen as a ‘sticking plaster’ over the unconscious, and the content related to repressed libidinal desire. Psychotic transference was opined to make psychoanalysis non-viable, and the likelihood of further regression within free association to lead to a high probability of relapse. Thus, psychoanalysis in its pure form was simply non-viable. Reference Jung and HullJung (1911/1912), however, viewed the experience of psychotic symptoms as a necessary phase of individuation and as a crucial driver for psychological development, including creativity and spirituality. For Freud the ‘sticking plaster’ was a form of self-defence; for Jung the emergence of psychosis was a sign of psychological development to be understood and integrated.
Cognitive therapies
As in so many areas, Beck did not accept the psychoanalytical orthodoxy. In 1952 he treated and markedly improved the distress and functioning of a patient with a substantial persecutory delusional system using collaborative questioning and reality testing. He was also able to generate a cognitive formulation and use schema-level techniques to work with unbearable protected affect. In this case the delusional system protected against guilt. Having described this approach (Reference BeckBeck 1952), he moved on from schizophrenia to work with anxiety and depression.
By the early 1990s, groups of UK psychologists and psychiatrists were developing pioneering new cognitive–behavioural techniques for schizophrenia. The breakthroughs began in Sheffield/North Nottinghamshire, Manchester, London/East Anglia, Birmingham, Glasgow and Liverpool.
In Sheffield/North Nottinghamshire, Kingdon & Turkington (D. T.) showed the safety and acceptability of Beckian cognitive therapy for out-patients with chronic schizophrenia (Reference Kingdon and TurkingtonKingdon 1991). Recognising that direct engagement with the psychotic patient in working on voices, delusions, thought disorder and negative symptoms was crucial for progress, the old approach of avoiding all such discussion was abandoned. They described a crucial component of cognitive–behavioural therapy (CBT) in reducing stigma, the concept of normalising (Reference Kingdon and TurkingtonKingdon 1991). Patients with schizophrenia are now informed that, although their voices and delusions are certainly troublesome, such symptoms are quite common in the general population (meta-analysis reveals approximately 5% prevalence and 3% incidence; Reference van Os, Linscott and Myin-Germeysvan Os 2009). Their voices and paranoid thoughts are described as a common human experience with the potential to improve over time. Similarly, they are informed that these psychotic symptoms usually have a clear ‘down to earth’ cause such as sleep deprivation, hallucinogen use, unresolved bereavement or childhood adversity and other traumas. Also, an accurate prognosis is given for schizophrenia showing that by 25-year follow-up the majority of patients are no longer troubled by voices or delusions (Reference Harrison, Hopper and CraigHarrison 2001). This increase in hope is enhanced by reference to famous voice hearers such as Anthony Hopkins (actor) John Frusciante (guitarist) and Vinnie Jones (footballer and actor). Following on from Bleuler, Reference Kingdon and TurkingtonKingdon & Turkington (2005) have described subgroups of schizophrenia with different aetiological components and different trajectories towards recovery.
Meanwhile in Manchester, inspired by the work of David Clark in anxiety disorders, Tony Morrison described a model of psychotic symptom maintenance that was to become hugely influential (Reference MorrisonMorrison 1998). He placed appraisal of anomalous experiences such as hallucinations, paranoid thoughts, intrusions and delusional mood right at the heart of psychosis. Such appraisals (e.g. ‘the Devil has possessed me’, ‘a computer is controlling my thoughts’ or ‘aliens are trying to hack into my mind’) correlate with insomnia and powerful affects such as anxiety, shame and anger. In line with such appraisals, safety behaviours are activated such as avoidance of social interaction, thought suppression, repeated checking and hypervigilance. All of these perpetuate the experience of psychosis in a vicious cycle of maintenance acting together to prevent recovery. Cognitive therapy therefore became a viable and model-based treatment option. In London/East Anglia, an integrated cognitive model was described (Reference Garety, Kuipers and FowlerGarety 2001) and a therapy developed that stressed the crucial importance of engagement, collaboration and individualised case conceptualisation (Reference Fowler, Garety and KuipersFowler 1995).
Other new therapies
Family therapy also has a robust evidence base. Meta-analysis of 32 randomised controlled trials (RCTs) found a moderately strong effect on relapse prevention, with numbers needed to treat (NNT) of 4 (95% CI 3.23–5.88) at the end of therapy and 6 (95% CI 3.85–9.09) up to 12 months after treatment (National Collaborating Centre for Mental Health 2014). Psychoeducation, in terms of relapse delay, and cognitive remediation, in terms of attentional and memory improvement, were not supported by the same quality of evidence and the National Institute for Health and Care Excellence (NICE 2014) did not recommend routine implementation. There is preliminary evidence from RCTs for eye movement desensitisation and reprocessing (EMDR), acceptance and commitment therapy (ACT) and cognitive adaptation training. The other new treatments are supported only by cohort-level evidence. As regards positive psychology, a systematic review looking at the well-being of people with psychosis reported a ‘small and methodologically weak’ evidence base (Reference Schrank, Bird and TyleeSchrank 2013).
What is the state of the current evidence base?
Current meta-analyses are fairly consistent in their findings. CBT v. treatment as usual (TAU) delivers a moderate effect size benefit on overall symptoms, positive symptoms, negative symptoms and functioning (Reference Jauhar, McKenna and RaduaJauhar 2014). However, other psychological treatments are also beneficial: for example, befriending and supportive psychotherapy both tend to have a detectable but small effect size. The effectiveness of these interventions (which were not specifically designed for schizophrenia) most probably relates to the extreme social isolation of people with schizophrenia in Western society. Interestingly, befriending has a differential effect on different psychotic symptoms. It is ineffective for hallucinations, but a viable adjunctive treatment for persecutory paranoia (Reference Samarasekara, Kingdon and SkiddleSamarasekara 2007). In head-to-head comparisons of CBT v. another psychological treatment with patients already stabilised on antipsychotic medication, CBT has a small but statistically significant benefit over all head-to-head comparators (Reference Jauhar, McKenna and RaduaJauhar 2014). CBT has also been shown to be acceptable and safe in patients with schizophrenia who refuse antipsychotic medication: one RCT recorded an effect size of 0.43 (similar to that of antipsychotic medication) (Reference Morrison, Turkington and PyleMorrison 2015).
New directions
There are numerous exciting new directions in the psychosocial treatment of schizophrenia to supplement ongoing efforts to improve the side-effect profiles of dopamine blockade and to discover new antipsychotic medications with different mechanisms of action. These treatments include compassion-focused therapy (CFT), EMDR, ACT, open dialogue, positive psychology interventions, transdiagnostic therapy based on the method of levels (MoL), metacognitive therapy, cognitive adaptation training and mindfulness training. The key components of each of these and their typical response profile are described below.
Compassion-focused therapy for critical hallucinations and shame in psychosis
CFT is based on the concept of self-nurture having been ‘switched off’ and the principle that we can reactivate our ability to be caring and self-nurturing. People often lose the ability to self-nurture and express compassion for others as a result of adverse life events in childhood and adolescence. People experiencing psychosis can be self-critical, self-blaming and have a negative outlook on the external world, along with strong feelings of shame which can maintain both positive and negative symptoms. Often, they do not feel deserving of therapy and this can lead to drop out from sessions (Box 1).
BOX 1 A candidate for compassion-focused therapy (CFT)
Adam, a young man aged 23 with a history of physical and emotional abuse, has always been self-critical and has low self-esteem. A bullying incident at work led to the emergence of critical auditory hallucinations. Adam would be the ideal type of person to benefit from CFT.
CFT helps to make sense of these self-blaming and critical thinking styles and to replace them with a more sympathetic and warm inner ‘voice’. This can be achieved through practising self-nurturing and compassionate behaviours and thinking using rational responding (Reference GilbertGilbert 2009). CFT comprises many components, one of which is the process of creating an image/fantasy of the ideal nurturer and working with this image repeatedly until self-nurture becomes second nature. Other compassion-based approaches include writing a compassionate letter to yourself which is written in a kind, supportive and caring manner, loving-kindness meditation and compassion-based homework exercises (recording of compassionate actions in a diary), all designed to develop the ability to nurture the self and others (Reference Wright, Turkington and KellyWright 2014: pp. 189–191). Evidence suggests that CFT can reduce distress for patients in acute in-patient settings (Reference Heriot-Maitland, Vidal and BallHeriot-Maitland 2014) and can reduce distress from critical auditory hallucinations (Reference Mayhew and GilbertMayhew 2008). While CFT would appear to be a viable complement to the cognitive model, there are no randomised trials of CFT in the treatment of psychosis to date.
Eye movement desensitisation and reprocessing for comorbid psychosis and PTSD
EMDR is based on a clear biological model and it leads to reprocessing of distorted, distressing trauma memories. Treatment consists of eight phases (Reference ShapiroShapiro 2001):
-
1 gathering a comprehensive assessment of the patient's life history and developing a treatment plan
-
preparing the patient
-
assessing traumatic events
-
desensitisation and reprocessing of trauma
-
installation of positive cognitions
-
body scanning
-
closure
-
re-evaluation.
EMDR has been shown to be an effective treatment for post-traumatic stress disorder (PTSD). In adult psychosis there is a strong link between childhood vulnerability, trauma and hallucinations, with a dose–response relationship (Reference Read, van Os and MorrisonRead 2005). Since many people who have experienced psychosis have a history of trauma, EMDR potentially has a place in the treatment of psychosis (Box 2). It is important that we treat the trauma, as it may be maintaining the patient's psychotic symptoms. Promising evidence suggests that mental imagery (which is a component of EMDR) can lead to reduction of psychotic symptoms (Reference MorrisonMorrison 2004). An increasing number of studies support the efficacy of EMDR in psychosis (Reference van den Berg and van der Gaagvan den Berg 2012, Reference van den Berg, de Bont and van der Vleugel2015; Reference de Bont, van den Berg and van der Vleugelde Bont 2013a,Reference de Bont, van Minnen and de Jonghb). EMDR would therefore appear to be a safe and acceptable treatment for people with comorbid psychosis and PTSD, but randomised trials are needed.
BOX 2 A candidate for eye movement desensitisation and reprocessing (EMDR)
Paul, a 45-year-old man with a history of childhood sexual abuse, struggles to deal with this trauma. In a psychotic episode triggered by memories of this abuse, he experienced both auditory and visual hallucinations of the perpetrator. Paul would be the ideal type of person to benefit from EMDR.
Acceptance and commitment therapy to improve functioning in chronic schizophrenia
ACT is a ‘third-wave’ therapy (following on from behavioural therapy and then cognitive therapy). It is based on acceptance, cognitive flexibility, cognitive defusion rather than cognitive fusion, mindfulness and empowerment through the development of new skills. ACT promotes the practice of committed action to move the individual towards identified values (Reference Hayes, Luoma and BondHayes 2006). It is common for people with chronic psychosis to become involved in repetitive negative behaviours such as shouting back at their voices in an attempt to suppress them; this behaviour tends to make the voices worse. Similarly, in the setting of a persecutory delusional system, social isolation can become an entrenched behaviour. Such behavioural approaches markedly diminish quality of life and social functioning, never mind achieving recovery targets such as valued goals (being a good parent, a good friend, etc.). If patients are able to learn how to accept the presence of their voices/delusions and to focus their attention instead on positive goals linked to values, this may reduce the distress of psychosis and provide more options for improved coping and reality testing. ACT encourages people to accept their symptoms of psychosis rather than avoid and suppress them; evidence suggests that ACT can reduce the risk of further hospital admissions and lower individuals’ conviction in their delusions (Reference Bach and HayesBach 2002). Increasing commitment to change may also increase engagement in positive action. Reference White, Gumley and McTaggartWhite et al (2011) found that people with psychosis who had received ACT had lower levels of depression and negative symptoms. Box 3 gives an example of how ACT can be used in managing voices.
BOX 3 A candidate for acceptance and commitment therapy (ACT)
Ella, a 36-year-old woman with schizophrenia, had always wanted to get involved in caring for animals. Her long history of schizophrenia, with voices and paranoid delusions, had stopped her from ever attempting to achieve her altruistic goal. Instead, she had been locked in battle with her voices and suspected persecutors, constantly listening to the voices and responding angrily to them. Training in the principles of acceptance with mindfulness exercises allowed her to change her attitude to the voices and paranoia, and enrol as a volunteer at a local animal refuge. This led to further reduction in voice hearing and paranoia, and improved self-esteem and social functioning.
Open dialogue to maintain social contact in early psychosis
Open dialogue is an approach piloted in Finland, and it is based on family/group therapy and a social constructivist approach. It emphasises the collaborative nature of much learning and stresses that early psychosis requires consistency and a group response. The approach works by engaging the patient, their family and their social network in open dialogue about the experience of psychosis. Ideally, this treatment is implemented within 24 h of initial contact with mental health services (Reference Seikkula, Alkare and AaltonenSeikkula 2001). The main principles of this approach are outlined in Box 4.
BOX 4 The seven main principles of open dialogue
-
1 An initial meeting is set up within 24 hours of the patient's first contact with services, to minimise the chance of hospital admission
-
The patient's wider social network is involved, so that they can be a source of support for both the patient and their family
-
The treatment team responds to the crisis in a flexible and adaptive manner, modifying treatment to suit the patient
-
The member of staff who was the first contact initiates a team meeting at which the team decides jointly which treatment is the most appropriate; the patient is included in the decision-making process
-
The team continues with its support of the family and patient, and continues to monitor the treatment plan using a variety of methods (e.g. individual or group therapy)
-
To help develop a secure relationship, the team holds regular meetings with the family and encourages their meaningful involvement; changes in treatment are discussed and introduced gradually
-
The patient and family are given opportunities to discuss questions and problems with team members; the team analyses the dialogue and language for emerging themes and encourages further discussions to help the family construct new ways of understanding the psychosis
Promising results have come from studies investigating open dialogue for psychosis. In a preliminary cohort study, at the 2-year point 64% of patients receiving open dialogue had never taken antipsychotic medication and 83% were working, studying or seeking employment (Reference Seikkula, Alakare and AaltonenSeikkula 2003). At the 5-year point, social outcomes in terms of being in employment or in full-time education remained greatly increased for individuals who had received open dialogue (Reference Seikkula, Aaltonen and AlkareSeikkula 2006). Again, randomised trials are awaited.
Positive psychology techniques for negative symptoms of schizophrenia
Classic psychosocial approaches for negative symptoms of schizophrenia are based mostly on behavioural activation, with mastery and pleasure recording. Positive psychology techniques, including the scheduling of ‘flow activities’, fit in well (Reference Meyer, Parks and SchuelllerMeyer 2014). Typically, patients with negative symptoms experience reduced motivation and anhedonia, seeming to be stuck in a rut, with little volition to attempt or little capacity to enjoy new activities. Discussion with a relative can unearth old hobbies and interests that can be added to activity schedules. One patient who used to be a bird watcher became more motivated on considering the birds he could hear outside the window. He showed some increase in pleasure as he started to catalogue the different species. This gradually led to discussions about migration patterns.
Similarly, if there is affective blunting and alogia, a longitudinal formulation (time line) can search for peak experiences and attempt to recreate experiences of joy, success and exhilaration using imagery exercises. Most people with schizophrenia need help to rediscover such positive experiences and affects and then to practise re-experiencing them. Again, this can lead to breakthroughs in functioning. One woman who was able to recall a time of being extremely at peace when visiting a historic site decided that she wished to visit some nearby sites to see if she could re-experience that positive affective state.
Transdiagnostic therapy based on the method of levels
This approach to therapy is based on an engineering model of how the brain functions – perceptual control theory (PCT) (Reference PowersPowers 1973). MoL therapy was designed by Tim Reference CareyCarey (2006) as a clinical application of perceptual control theory. We all face goal conflicts all the time, such as ‘I should tell the truth’ versus ‘I shouldn't hurt anyone's feelings’, and usually the mind spontaneously resolves such conflicts. The basic principle of Carey's model is that mental distress can arise from emotionally ‘hot’ goal conflicts, and individuals may need help to identify these and resolve them. Carey postulates that the therapist needs to keep going ‘up a level’ to find any ‘hot’ goal conflict. This is achieved by asking the patient questions in relation to what it would mean to them if they did not achieve a stated goal. Conflicts can be witnessed in breaches in social contact, i.e. disruptions in the flow of speech or eye contact such as looking away or laughing at key points in the discussion. At these points the therapist asks which thought went through the mind just then.
A good example of a hot goal conflict might be a woman who was sexually assaulted by her father in childhood who now also has feelings of needing to care for him in his old age. This conflict might theoretically manifest as increased arousal, with hallucinations in various modalities, thought disorder and/or paranoia (Reference Carey, Mansell and TaiCarey 2014). So while a life-threatening event might lead to PTSD, a conflicted event could trigger psychosis.
The key techniques of MoL include questioning both sides of the conflict, accessing imagery that expresses the conflict and not relying on homework or agendas (Reference TaiTai 2009). All of the therapy work is done in session and the patient has full control over the number of sessions needed. This approach has never been used in its pure form for psychosis, but the questioning techniques have been used as a means of overcoming roadblocks in therapy. MoL techniques are therefore best used in cases of treatment-resistant psychosis when medication and other therapies are not leading to the expected progress.
Metacognitive therapy
This form of cognitive therapy was first described by Adrian Reference WellsWells (2009). The basic model is the self-referencing executive function (S-REF) model, which postulates that when symptoms persist, the patient has become locked into a cognitive attentional state (CAS). In the CAS a patient with a paranoid delusion might hold contrary beliefs about paranoia, such as ‘being paranoid will keep me safe’ and ‘paranoia means that I will be violent someday’. These contrary beliefs maintain an attentional focus on the paranoid belief, driving high levels of arousal and the activation of mental safety behaviours such as worry, rumination and thought suppression/control. Metacognitive therapy for psychosis became viable through recognition that worry and rumination directly exacerbate psychotic symptoms such as persecutory paranoia and distressing hallucinations (Reference Morrison, Pyle and ChapmanMorrison 2014).
Key techniques include considering the pros and cons of worry and rumination in terms of their effectiveness in ensuring safety, worry/rumination periods (15 minute spells during which intense worrying/rumination are encouraged) and worry/rumination postponement, along with exercises to change attentional focus. Detached mindfulness as a technique is taught within metacognitive therapy to help reduce distress related to voices and paranoid thoughts. These strategies all lend themselves to a briefer form of cognitive therapy focused on process rather than content. This approach was piloted for psychotic disorders by Reference Morrison, Pyle and ChapmanMorrison et al (2014). Worry/rumination periods and postponement have proven to be of value for patients with persecutory delusions (Reference Freeman, Dunn and StartupFreeman 2015). These early results are promising, in that patients with prominent rumination and worry who are able to understand the model seem capable of deriving benefit, but it must be said that some patients just don't get it. This is particularly true of those with prominent cognitive deficits and primary negative symptoms (Box 5).
BOX 5 A candidate for metacognitive therapy
A typical good-outcome referral for metacognitive therapy might be a young man with social anxiety and persecutory paranoia who is particularly worried about being out in public.
Cognitive adaptation training for those with severe cognitive deficits
People with chronic schizophrenia tend to complain most about their cognitive difficulties. Cognitive remediation attempts to remedy these cognitive, social and thinking deficits and errors using a series of exercises. It has been shown that attention and short-term memory can thus be improved, but the effect size is small and non-durable, and there is only modest generalisation to function (Reference Wykes, Huddy and CellardWykes 2011). Social skills training is a form of social remediation and has a stronger evidence base. It is a prominent psychosocial treatment, particularly in North America. At the level of cognitive deficits such as theory of mind and the ‘jumping to conclusions’ error, cognitive training programmes have recently been piloted and have been shown to be of benefit (Reference Moritz, Andreou and SchneiderMoritz 2014).
Cognitive adaptation training is a clinical intervention that takes cognitive remediation out of the classroom and into the patient's home environment. Cognitive adaptation training theory postulates that individuals with poor executive function require high levels of environmental structure and more obviously placed environmental cues. Electronic cueing devices, arrows, lists, pillboxes that play tunes, signs and other environmental aids are all individually organised according to each patient's comprehensive cognitive assessment. A trained therapist visits weekly to monitor progress and adapt the intervention as needed. This approach has been shown to improve functioning and treatment adherence and reduce hallucinatory intensity in chronic schizophrenia (Reference Velligan, Tai and RobertsVelligan 2015). Reference Allott, Killackey and SunAllott et al (2016) also demonstrated the feasibility and acceptability of cognitive adaptation training in first-episode psychosis. Box 6 illustrates a typical patient who might be responsive to cognitive adaptation training.
BOX 6 A candidate for cognitive adaptation training
Jane is 52 years of age with chronic schizophrenia. Her self-care is poor. She frequently forgets to shower, take clothes to the laundry and attend the dentist. She often forgets to take her medication. She wears clothing in a bizarre and inappropriate manner, which increases stigma and social isolation. Cognitive adaptation training might benefit Jane by introducing order and environmental cues in her home.
Mindfulness training
Mindfulness is a core concept of Buddhist religious practice and takes many forms. There is mindful walking, mindful breathing, mindful eating (e.g. the raisin exercise) and mindfulness meditation. The key principle is to develop the faculty of being aware of your own consciousness and to neutrally observe the flow of thoughts and other mental experiences without feeling the need to do something about them or becoming distressed by them. Thoughts are viewed as being transient experiences and the patient as a non-judgemental observer. The capacity to be mindful therefore fits in well as a treatment modality for those with distressing paranoid thoughts/beliefs and hallucinatory experiences. Mindfulness would be classified as a metacognitive coping style and it can completely change a person's attitude to their experience of psychosis. Mindfulness may also be cost-effective as it is usually practised in a group setting as a complement to other treatment modalities. There are, however, caveats. For example, some mindfulness exercises (such as the body scan) can be distressing for those with an undisclosed history of trauma.
Mindfulness training is a very useful new direction in the treatment of psychosis, as long as the intensity is titrated against degree of disability and rate of progress. The various exercises, once taught, are usually given as homework exercises carried out in a ‘pulsed format’, i.e. in brief bursts (Reference Wright, Turkington and KellyWright 2014): it is not recommended that people with psychosis spend prolonged periods in meditative states. An exercise might be to take a mindful breath whenever they walk through a door or whenever the adverts come on the television. The most successful applications to date have been in the area of voice hearing and persecutory paranoia (Reference ChadwickChadwick 2014). Although mindfulness is a promising approach for schizophrenia spectrum disorder, the current evidence base is very limited. The ideal patient for a mindfulness group might be someone who is distressed and preoccupied by the experience of voice hearing.
Conclusions
Although antipsychotic medication remains the mainstay of the treatment of schizophrenia, medications are not always effective, can have unpleasant side-effects and are often prematurely discontinued. There is a pressing need for pharmacological breakthroughs in terms of both mechanism of action and side-effect profiles.
Following on from the general acceptance of the evidence base for psychosocial interventions for schizophrenia such as CBT, family therapy, psychoeducation and cognitive remediation, there has been a rapid evolution of new models and therapy modalities. Arrays of new psychological treatments for schizophrenia are now being tested not only in case series and randomised trials against TAU, but also as head-to-head comparisons and in amalgamated forms. The cognitive model of psychosis continues to develop and many of the techniques mentioned here are now being delivered within CBT. It must be said that clinical practice has now outpaced the evidence base, and it is important that all negative as well as positive outcomes with these interventions are adequately documented and published. One further caveat must be that CBT, family therapy, psychoeducation and cognitive remediation are by no means fully implemented in the National Health Service and new therapies will need funding to arrange training workshops and supervision systems. This is an exciting time of incremental development in the psychological treatment of schizophrenia, but implementation must be paced in line with clear evidence of efficacy and guidance for targeting these interventions.
MCQs
Select the single best option for each question stem
-
1 The evidence base shows the level of effect of CBT compared with befriending in schizophrenia to be:
-
a none (0%)
-
b small (up to 20%)
-
c moderate (20–40%)
-
d large (40–80%)
-
e indeterminable.
-
-
2 Compassion-focused therapy for psychosis includes:
-
a reliving distressing events
-
b formulation
-
c working with an ideal nurturing image
-
d interpretation
-
e ignoring painful emotion.
-
-
3 EMDR would be potentially useful for a patient presenting with:
-
a thought disorder
-
b cognitive deficits and negative symptoms
-
c acute hebephrenia
-
d catatonia
-
e command hallucinations and a history of trauma.
-
-
4 According to the self-referencing executive function model, psychotic symptoms persist when:
-
a the patient has become locked into a cognitive attentional state
-
b the patient has become locked into a behavioural attentional state
-
c the patient has become locked into a state of cognitive fusion
-
d the patient has accepted symptoms and has become hopeless
-
e the patient has successfully practised worry postponement and worry periods.
-
-
5 The techniques of cognitive adaptation training include:
-
a normalising
-
b exposure
-
c social constructivism
-
d electronic cues
-
e acceptance.
-
MCQ answers
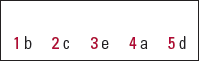
| 1 | b | 2 | c | 3 | e | 4 | a | 5 | d |



eLetters
No eLetters have been published for this article.