By 2020 depressive disorders are expected to be the second highest cause of disease burden worldwide (Reference BrownBrown, 2001). Community surveys in the UK have estimated that 2% of the population suffer from depression (Reference HaleHale, 1997). Two previous UK studies have calculated the cost of depression (Reference Kind and SorensonKind & Sorenson, 1993; Reference Jönsson and BebbingtonJönsson & Bebbington, 1994) and reported it as £3.4 billion (£3.4 × 109), with direct treatment costs estimated at £ 222 million for the UK in one study (Reference Jönsson and BebbingtonJönsson & Bebbington, 1994) and £416 million for England and Wales in the other (Reference Kind and SorensonKind & Sorenson, 1993). However, these figures are based on cost data from a decade ago and are likely to be out of date. Furthermore, the underlying assumptions of the original analysis can be revised in the light of changes in treatment patterns in the UK and the availability of more accurate data. This study calculates the cost of depression in people aged over 15 years in England.
METHOD
A prevalence-based approach was used to measure the burden of depression among adults aged over 15 years in England in 2000. This burden comprises the direct treatment costs of depression, including primary and secondary care, and the indirect costs of depression arising from people's inability to work owing to their illness (Reference Kind and SorensonKind & Sorenson, 1993). Indirect costs include both lost working days (morbidity costs) and lost life-years due to premature death (mortality costs). Rates of depression were taken from Key Health Statistics from General Practice (Office for National Statistics, 1998) and applied to population data for England in 2000 to generate the most recent number of cases of treated depression. The prevalence data for depression are important as they give the distribution of cases of depression by age and gender, which is used to apportion certain aspects of the cost data. Direct treatment costs were calculated using the latest available data on in-patient and day case admissions, out-patient consultations, general practitioner consultations and numbers of prescriptions. Unit costs were then applied to each category to give an estimate of the overall cost of treating depression. All costs reported are 2000 prices.
Cost of hospital contacts
The number of hospitalisations for depressive disorder and recurrent depressive disorder was taken from Hospital Episode Statistics (Department of Health, 2000a ). Two ICD–10 (World Health Organization, 1992) diagnosis codes were applicable: F32 (depressive episode) and F33 (recurrent depressive disorder). The total numbers of day cases, defined as treatment during the course of the day that does not require an overnight stay (Department of Health, 2000a ), for depressive disorder and recurrent depressive disorder were reported in Hospital Episode Statistics. The cost of admissions and day cases was then calculated by multiplying the number of admissions and day cases by the mean average cost per admission and day case given in Healthcare Resource Group data (P18, psychiatric disorders), from the national schedule of reference costs (Department of Health, 2000c ).
Out-patient consultations
Out-patient consultation data were available by sector and specialty from Consultant Outpatient Attendances by Sector (Department of Health, 2001), but there was no specific figure for consultations for depression. Therefore the number of in-patient episodes due to depression as a proportion of all mental health episodes was calculated (16%) and this percentage was applied to the total number of mental health out-patient attendances. This is likely to be an underestimation in view of the finding that only 5% of depression is treated in the hospital setting (Reference Jönsson and BebbingtonJönsson & Bebbington, 1994). (For comparison, an earlier study estimated that affective disorders contributed 21% of the total cost of mental illness in the USA in 1990 (Reference Rice and MillerRice & Miller, 1995).) Data from Key Health Statistics from General Practice (Office for National Statistics, 1998) were also examined to identify a more accurate estimate of out-patient consultations. However, in this source out-patient referral rates were only available for psychiatry as a whole rather than specific to depression; these data therefore were subject to the same limitations and would not be as recent as the published figures that were used. The cost of depression-specific out-patient consultations was then calculated from Reference Costs 2000 (Department of Health, 2000c ) on the basis of specialty code 710 (mental illness).
General practice consultations
Rates of general practitioner consultations by patients with depression (ICD–9 classifications 298, 300.4 and 311; World Health Organization, 1978) were obtained from Morbidity Statistics from General Practice (Office for National Statistics, 1995). These rates were applied to the 2000 population data and the cost calculated using unit costs of health and social care (Reference Netten and CurtisNetten & Curtis, 2000).
Drug consumption
Prescription cost analysis data (Department of Health, 2000b ) give the number of prescriptions and net ingredient cost per prescription of antidepressant drugs prescribed, categorised by antidepressant class. Key Health Statistics from General Practice (Office for National Statistics, 1998) gives the proportion of drugs in each anti-depressant class prescribed for patients with treated depression, analysed by age and gender. The cost of antidepressant medication was then calculated using the net ingredient cost per script as given in the prescription cost analysis data.
Indirect costs
Indirect costs of depression arise when people with this disorder are unable to function as a result of their illness (Reference Kind and SorensonKind & Sorenson, 1993), manifested by the inability to work (morbidity costs). Furthermore, a proportion of people with depression die from suicide or accidental poisoning that is related to the diagnosis of depression (mortality costs).
Morbidity costs
The total number of days of incapacity benefit for the period 1 April 1999 to 31 March 2000 for the diagnosis of depression and recurrent depression (ICD–10 classifications F32 and F33) were obtained on application from the former Department of Social Security. These figures were apportioned according to age and gender using the prevalence data, for male patients aged up to 64 years only (assuming that those aged 65 or over would not claim incapacity benefit). For female patients the age limit was 59 years. The average weekly wages for each age band reported by the New Earnings Survey (Office for National Statistics, 2000c ) were used to calculate the indirect costs of depression due to lost earnings.
Mortality data
The number of deaths due to suicide and self-inflicted injury is available categorised by gender and age band (Office for National Statistics, 2000b ). Seventy per cent of suicides are estimated to be related to depression (Reference Hotopf and LewisHotopf & Lewis, 1997), and this figure was used to calculate the number of suicides that were attributable to depression. The number of deaths due to accidental poisoning by antidepressants in 2000 (Office for National Statistics, 2000b ) was also examined, to give the number of deaths due to accidental poisoning that are related to depression. Taking the life expectancy data from Health Statistics Quarterly 11 (Office for National Statistics, 2001) classified by age and gender, the number of life-years lost was calculated for all deaths due to depression. The residual life expectancy was discounted at 6%. Using data on the proportion of men and women who are in paid employment derived from the Labour Force Survey (Office for National Statistics, 2000a ), we calculated the number of working life-years lost through depression. Multiplying the average weekly earnings (Office for National Statistics, 2000c ) to estimate the annual earnings by age group and gender enabled the cost of the life-years lost due to depression to be calculated.
RESULTS
Prevalence of depression
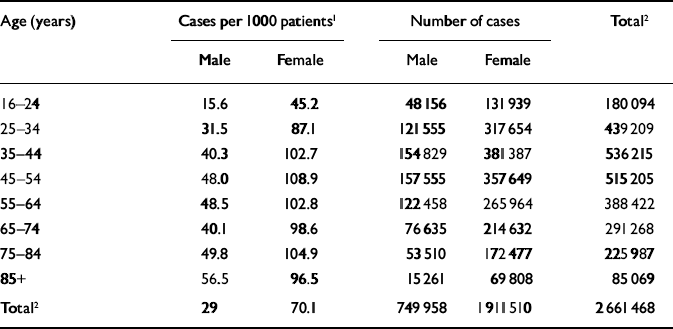
There were estimated to be 2.6 million cases of depression in England in 2000 (Table 1). In 72% of cases the patient was female, and 20% of cases occurred in the 35–44 years age band.
Table 1 Prevalence of depression in England in 2000
| Age (years) | Cases per 1000 patients1 | Number of cases | Total2 | ||
|---|---|---|---|---|---|
| Male | Female | Male | Female | ||
| 16—24 | 15.6 | 45.2 | 48 156 | 131 939 | 180 094 |
| 25—34 | 31.5 | 87.1 | 121 555 | 317 654 | 439 209 |
| 35—44 | 40.3 | 102.7 | 154 829 | 381 387 | 536 215 |
| 45—54 | 48.0 | 108.9 | 157 555 | 357 649 | 515 205 |
| 55—64 | 48.5 | 102.8 | 122 458 | 265 964 | 388 422 |
| 65—74 | 40.1 | 98.6 | 76 635 | 214 632 | 291 268 |
| 75—84 | 49.8 | 104.9 | 53 510 | 172 477 | 225 987 |
| 85+ | 56.5 | 96.5 | 15 261 | 69 808 | 85 069 |
| Total2 | 29 | 70.1 | 749 958 | 1 911 510 | 2 661 468 |
Direct costs
The components of the direct costs of treating depression that are borne by the National Health Service (NHS) are estimated to be £369 865 000 (Table 2). These comprise in-patient, day and out-patient care, general practitioner consultations and medication. The cost of each component and its respective proportion of the total direct cost is also indicated.
Table 2 Components of the direct National Health Service treatment cost of depression

| Direct costs | £ ('000) | % |
|---|---|---|
| In-patient care | 28 660 | 7.7 |
| Day case | 476 | 0.1 |
| Out-patient care | 22 133 | 6.0 |
| General practitioner consultations | 8217 | 2.2 |
| Antidepressant medication | 310 378 | 84 |
| Total | 369 865 | 100 |
Morbidity costs
Claims for incapacity benefit for people in England with a diagnosis of depression (F32 and F33) indicate that 109.7 million working days were lost as a result of depression. The total of lost earnings is estimated at over £ 8 billion. Table 3 lists the number of working days lost by men and women in various age groups; almost a fifth of the days were lost by women aged 35–44 years, who have the highest prevalence of depression.
Table 3 Working days lost owing to depression in 1999—2000

| Days lost ('000) | |||
|---|---|---|---|
| Age range (years) | Men | Women | Total |
| 15—24 | 2590 | 7109 | 9699 |
| 25—34 | 6416 | 16 843 | 23 259 |
| 35—44 | 8205 | 20 354 | 28 559 |
| 45—54 | 8372 | 19 061 | 27 433 |
| 55—64 | 6535 | 14 283 | 20 818 |
| Total | 32 118 | 77 650 | 109 768 |
Mortality costs
There were 3583 suicides in the year studied, and 2507 of these are estimated to be related to depression. Suicides in people with depression were most frequent in men aged 25–34 years. In the same year there were also 1058 deaths due to accidental poisoning with drugs, medicaments and biologicals, an estimated 108 of which were due to poisoning with antidepressants. The total number of deaths in England in 2000 estimated to be associated with depression is 2615 (Table 4). To estimate the loss of future lifetime earnings arising from premature death related to depression, the number of deaths was multiplied by discounted life expectancy data, resulting in a loss of an estimated £ 562 million.
Table 4 Deaths associated with depression

| Deaths (n) | |||
|---|---|---|---|
| Age range (years) | Men | Women | Total |
| 15—24 | 213 | 65 | 278 |
| 25—34 | 471 | 107 | 578 |
| 35—44 | 451 | 120 | 571 |
| 45—54 | 348 | 116 | 464 |
| 55—64 | 209 | 85 | 294 |
| 65—74 | 148 | 66 | 214 |
| 75+ | 138 | 78 | 216 |
| Total | 1978 | 637 | 2615 |
Total costs
The total cost of depression in England among adults over 15 years old in 2000 is estimated at over £9 billion. Table 5 presents the direct and indirect cost components compared with estimates from previous studies.
Table 5 Total costs of depression in 2000 compared with two earlier studies

| Kind & Sorenson (Reference Kind and Sorenson1993) | Jönsson & Bebbington (Reference Jönsson and Bebbington1994) | ||
|---|---|---|---|
| Cost year | 2000 | 1990—1991 | 1990 |
| Primary care costs (£000) | |||
| GP consultations/visits | 8217 | 126 399 | NS |
| CPN | 16 285 | NS | |
| Medication | 310 378 | 47 280 | 41 722 |
| Secondary care costs (£000) | |||
| In-patient | 28 660 | 177 365 | NS |
| Day-case | 477 | — | NS |
| Out-patient | 22 133 | 9146 | NS |
| Social care costs (£000) | 40 183 | ||
| Morbidity cost (£000) | 8 123 258 | 2 973 000 | |
| Mortality cost (£000)1 | 562 151 | ||
| Total cost (£000) | 9 055 274 | 3 389 658 | 222 000 |
DISCUSSION
A survey of adults in the community estimated that the prevalence of depression was 28 per 1000 in women and 24 per 1000 in men (Office for National Statistics, 2000d ). Our study used data based on depression diagnosed in patients who presented for treatment in England (Office for National Statistics, 1998) and applied them to the 2000 population data to estimate the number of cases. This approach aims to present the real costs of treating depression, although these figures are likely to be an underestimate of the actual numbers of people with depression owing to possible misdiagnosis. This study used published data sources (such as Hospital Episode Statistics and Prescription Cost Analysis) rather than expert opinion in an attempt to reduce the uncertainty of the estimates. Using national data sources to provide details of the resources and costs incurred by the treatment of depression is subject to limitations, including the validity of extrapolating sample-based estimates to the population as a whole and the margin of error in classification and coding of the data inputs. In addition, the lack of availability of depression-specific data necessitates estimation of some of the resource components, such as out-patient and general practitioner consultations. We therefore calculated the latter figure using the general practice morbidity statistics from 1991 (Office for National Statistics, 1995). However, given the general trend of increased use of health services over time, the number of consultations is likely to be an underestimate.
All of the direct treatment costs used in the analysis are based on the mean reported costs, which may be an under- or overestimation of the real costs of treating patients with depression. For example, the cost of a general practitioner consultation is based on an average surgery consultation lasting 9.36 min (Reference Netten and CurtisNetten & Curtis, 2000), which costs £15. Previous cost of depression studies have argued that the time and consequently the cost of a consultation for someone with depression will be approximately double that of the average consultation (Reference Kind and SorensonKind & Sorensen, 1993; Reference Jönsson and BebbingtonJönsson & Bebbington, 1994). Prescription Cost Analysis (Department of Health, 2000b ) bases the prescription costs on the net ingredient cost, and does not include any data on dispensing costs or any adjustment when a prescription charge is paid by the patient. As such costs and adjustments affect the overall cost to society, they should be considered in a cost-of-illness analysis. Furthermore, patients with depression may also receive other types of medication, such as anxiolytics, as well as treatment for adverse events such as gastrointestinal upsets. However, as it could be argued that antidepressants such as selective serotonin reuptake inhibitors may be prescribed for conditions other than depression (such as eating disorders or panic disorders), the overall estimation for cost of medication may be regarded as accurate.
This study calculated the costs of treating depression based on health care resource use data pertaining to adults with a diagnosis of depression in England in 2000. However, we recognise that certain aspects of patient management have been excluded from this analysis. This is largely due to lack of availability of reliable estimates of health resource use for certain components, such as the number of home visits to patients by the general practitioner and other health care workers such as community psychiatric nurses. Similarly, the cost of community psychiatric teams, who may also be involved in the management of patients with depressive illness, were excluded from the analysis owing to the lack of accurate data. There is evidence to suggest that the use of counselling for depression is increasing (Reference Wagner and SimonWagner & Simon, 2001), but a reliable estimate of the number of counselling consultations for patients with depression was not identified. This potentially represents an additional cost. The use of psychotherapy such as cognitive–behavioural therapy is also increasing in both the NHS and the private sector; again, reliable estimates of the number and costs of this treatment were not identified. Patient-related costs are not included in this analysis owing to the lack of reliable data. These might include direct costs, such as the cost of prescription or over-the-counter preparations, and indirect costs, such as those incurred for travelling to an out-patient or general practitioner consultation.
Overall, it is likely that direct cost estimates represent an underestimation rather than an overestimation of the actual costs of depression.
Indirect costs
Indirect costs represent the value of lost production to society. Average earnings rates used to calculate the indirect costs may not be an accurate reflection of the wages of people with depression, who may be below-average earners. In this study we use the human capital approach, which is defined as lost income during the time that the patient is absent from work because of sickness, and the lost future gross income due to premature death (Reference LiljasLiljas, 1998). Criticisms of the human capital approach are that it discriminates against those who are not in employment, such as elderly people. In this analysis no cost is calculated for morbidity and mortality in men over 65 years old or women over 60 years old. Furthermore, in reality when people are absent from work, colleagues may cover their work in the short term and in the long term a replacement worker may be appointed. However, the inability to work does represent a societal and personal burden to those who are affected. Our study derived the number of lost days from incapacity claims that were classified by a diagnostic code for depression. Therefore, the number of days lost is a fair representation of this burden, although the cost estimates may not be. Claims for benefits may be an underestimation of the actual number of working days lost, as employers make claims for sickness benefit only after an employee has been absent for 5 days.
Deaths due to depression
The lifetime risk of suicide among people with depression has been estimated at 6% (Reference Inskip, Harris and BarracloughInskip et al, 1998). It is widely assumed that early and accurate identification of depressive disorders will reduce the risk of suicide, and one of the targets set in the recent National Service Framework for Mental Health (Department of Health, 1999) is to reduce the number of suicides. Our study assumes that only 70% of suicides were due to depression. However, it could be argued that all people who die by suicide are suffering from depression. Furthermore, mortality data are likely to be an underestimate, because in a number of reported suicides it is not determined whether death was accidentally or purposely inflicted; these deaths are not included in the analysis but may also be due to an underlying diagnosis of depression. Suicide figures may also suffer from a bias in recording in order to avoid inflicting further suffering on the surviving family (Reference Kind and SorensonKind & Sorenson, 1993).
Deaths due to accidental poisonings were assumed to be related to depression only if they were caused by an antidepressant; however, people with depression may overdose inadvertently on other substances, such as paracetamol. Conversely, it could be argued that not all accidental poisonings with antidepressants occur in people with depression – for example, a family member might take the wrong medication in error. We also recognise that people suffering from depression have an increased risk of mortality from other related conditions, and therefore the number of deaths associated with depression is likely to be an underestimate. Despite these limitations, the number of deaths related to depression is an important indication of the human loss due to unsuccessful recognition of illness or failure of treatment.
Interpretation of the findings
This study estimates that the total direct cost of depression in England is almost £370 million. Previously published estimates of the cost of depression were £222 million in the UK (Reference Jönsson and BebbingtonJönsson & Bebbington, 1994) and £416 million in England and Wales (Reference Kind and SorensonKind & Sorenson, 1993). However, the contribution of hospital admissions in the latter study was almost 40% and this was generated mainly from admissions to specialised mental institutions rather than to general hospitals. The changes in patterns of care and the closure of many such institutions reflect the shift found in our study for the highest contributor to costs to be antidepressant medication rather than hospital care. Conversely, in Kind & Sorenson's study the medication component represented only 11.3% of the total direct costs, which also reflects the greater usage of the cheaper tricyclic antidepressants.
Morbidity costs are nine-tenths of the overall total cost of depression in our study. This is in keeping with the clinical course of depression, which is a chronic and relapsing condition that can successfully respond to treatment. Unfortunately, as patients comply poorly with medication – some studies suggest up to 50% (Reference HaleHale, 1997) – this may lead to a greater chance of relapse and recurrence. We estimated the morbidity costs to be £8.1 billion, which is almost three times the cost estimated by Kind & Sorenson (Reference Kind and Sorenson1993). This may be explained by two factors. First, in the earlier study morbidity costs were estimated on the basis of assumed disease severity and absence from work; in our study, these costs were estimated according to reported incapacity benefit claims, which are likely to be more accurate. Second, average wages have increased over the past decade, and our estimates of labour market participation are higher than those used by Kind & Sorenson.
The ratio of indirect to direct costs in our study is 23, whereas previous studies reported a 7-fold difference (Reference Kind and SorensonKind & Sorenson, 1993). This difference may be largely due to the differences in methodology, along with greater recognition and awareness of depression by patients and clinicians. Although the number of life-years lost was estimated in the Kind & Sorenson study, mortality costs were not calculated. We estimated these to be £562 million in our study, which also results in an overall increase in indirect costs. The cost estimates calculated in our study are based on the most recent national health care resource data available for England. Furthermore, the calculation of both the direct and indirect costs of depression are revisions of those provided in previous studies and incorporate more accurate estimates of resource use by people with depression. Given the number of limitations that remain when performing any cost-of-illness study, the costs we calculated are likely to be an underestimate rather than an overestimate of the burden of depression.
In summary, the cost of depression in England represents a substantial burden on both society and the individual despite improved recognition and awareness, and the availability of effective and accessible treatments. The total cost of managing depression in adults in England in 2000 is estimated at over £9 billion, including almost £370 million of direct treatment costs. These results provide a more accurate estimate of current costs and reflect the shifts in patterns of care and the availability of more accurate health care resource data. The contribution of the cost of antidepressant medication to the direct treatment costs is substantial and provides evidence of the wider recognition and better management of the disease. However, anti-depressant medication costs are a minor proportion of the overall cost of depression. There is a substantial indirect burden associated with depression: in 2000 there were 109.7 million working days lost as a result of depression, and 2615 deaths. The intangible elements of pain and suffering of people with depressive disorders and their families and the effects on quality of life cannot be quantified in monetary terms.
The accuracy of cost estimates is always subject to the limitations of the available data. However, using a ‘top-down’ approach gives an estimation of the actual costs that were allocated in a given year to treating a disease at the population rather than the patient level. The use of mean costs can provide the decision-maker with the average amount that a patient might incur but does not give an indication of the likelihood of that cost occurring. Although population-based cost estimates are incomplete, knowledge of how costs are allocated is important given the excess demand for scarce health care resources. Finally, the contribution of the different components to the overall cost of depression may provide an indication of where strategies to reduce the consequences of disease have the potential to offset significant costs that could be more efficiently allocated elsewhere in society.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The cost of depression in the UK remains high despite availability of effective treatment.
-
▪ Morbidity costs comprise 90% of the total costs, illustrating individuals' incapacity to work.
-
▪ Drug treatment represents a minor proportion of the overall cost of depression.
LIMITATIONS
-
▪ Data are drawn from a variety of sources, which do not use uniform reporting mechanisms.
-
▪ There is a lack of depression-specific data for certain components.
-
▪ Caution should be used when interpreting the mortality/morbidity costs.








eLetters
No eLetters have been published for this article.