The diagnosis of somatisation disorder in DSM-IV 1 is based on numerous ‘medically unexplained’ symptoms but this diagnosis has been criticised as the measurement of medically unexplained symptoms is unreliable and the concept is inherently dualistic. Reference Creed, Guthrie, Fink, Henningsen, Rief and Sharpe2,Reference Dimsdale and Creed3 These difficulties, together with measurement problems, have meant that many population-based surveys have omitted somatoform disorders, and healthcare planners have tended to ignore these disorders. Reference Creed4 By contrast, clinical studies have used a checklist of all somatic symptoms and found that total somatic symptom score correlates well with the outcomes of impaired function and medical help-seeking even after adjustment for mental disorders. Reference Kroenke, Spitzer and Williams5-Reference Barsky, Orav and Bates7 The current project examined whether these relationships are similar in population-based samples, which are free of any bias related to treatment-seeking. The study aimed to determine whether the associations between somatic symptom score, health status and healthcare use remain after adjustment for important confounders including depression, anxiety and the presence or absence of a medical condition. If so, this would help to determine the value of total somatic symptom score as a clinically useful predictor over and above the presence or absence of depression, anxiety and medical conditions. The present study concerned secondary analysis of data collected in population-based studies and was more comprehensive than previous studies as it included potential key confounders. Reference Barsky, Orav and Bates7-Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 We hypothesised that total somatic symptom score contributes further to the association with, or prediction of, impairment or healthcare use beyond that of the most important confounders including depression, anxiety and the presence or absence of a medical condition. If this hypothesis is supported this strengthens the validity of syndromes or disorders based on somatic symptom presentations. The study had two secondary aims: (a) to compare total somatic symptom score with medically unexplained symptoms and (b) to examine the effect on outcome of numerous somatic symptoms when this is accompanied by additional health concerns and health anxiety. This combination of burdensome somatic symptoms and other psychological features form part of the diagnostic criteria of DSM-5 ‘somatic symptom disorder’. 11
Method
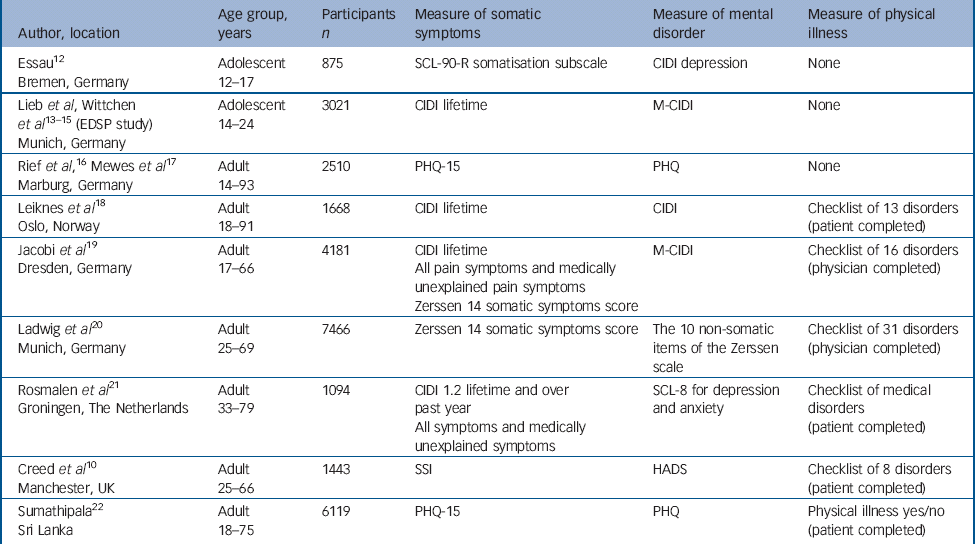
Data came from nine population-based studies (total n = 28 377). Details are shown in Table 1. The sites were chosen as their samples were all reasonably large, they had used recognised instruments, the investigators were willing and able to send their data to Manchester for analysis (seven sites did so) or they were prepared to analyse their own data in an identical way. The Manchester statistician (B.T.) supplied Oslo and Munich (Early Developmental Stages of Psychopathology (EDSP) study) with SPSS syntax files and excel file templates to this end.
Measurement of somatic symptoms
Five sites used a self-administered questionnaire asking respondents to mark those somatic symptoms that they found bothersome. Two sites each used the Patient Health Questionnaire (PHQ-15) Reference Kroenke, Spitzer and Williams5 (Marburg Reference Rief, Mewes, Martin, Glaesmer and Brähler16,Reference Mewes, Rief, Brahler, Martin and Glaesmer17 and Sri Lanka Reference Sumathipala22 ) and the Zerssen scale Reference Zerssen23 (Munich Reference Ladwig, Marten-Mittag, Formanek and Dammann20 and Dresden Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb19 ); one used the Symptom Checklist-90-Revised (SCL-90-R) Reference Derogatis24 somatisation subscale (Bremen Reference Essau12 ) and one site used the Somatic Symptom Inventory (SSI) Reference Derogatis, Lipman, Rickels, Uhlenhuth and Covi25 (Manchester Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 ) (Table 1). Four sites used the Composite International Diagnostic Interview (CIDI), Reference Wittchen26 which allowed direct comparison between medically unexplained and total number of somatic symptoms (Dreseden, Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb19 Munich (EDSP study), Reference Lieb, Zimmermann, Friis, Hofler, Tholen and Wittchen13-Reference Lieb, Isensee, von Sydow and Wittchen15 Groningen, Reference Rosmalen, Tak and de Jonge21 Oslo Reference Leiknes, Finset and Moum18 ).
We omitted gender-specific (for example painful menstruation) and depression-related items (for example impaired sleep) prior to the creation of a total somatic symptom score. For the self-rated questionnaires total somatic symptom score reflected both the number of somatic symptoms and their severity (how bothersome they were). As these symptoms were rated on a three- or four-point scale of severity, their scores ranged as follows: SCL-90-R somatisation items (0-48), PHQ-12 (after removal of gender-specific and depression-related items: 0-24), Zerssen (0-42), SSI (13-52). For the CIDI, after excluding four female-specific items, we agreed a list of 37 somatic symptoms, each of which was rated as present or absent (irrespective of whether they were clinically significant, the effect of drug intake or as a result of a medical condition). Thus, for the CIDI total symptom score was a simple symptom count. For the secondary analysis we examined separately those symptoms that were not fully explainable by a medical condition or have not always been caused by the intake of any substances. These are defined on the CIDI as those symptoms that are ‘clinically significant’ (indicated either by seeking help from a medical doctor or other mental health professional, repeated intake of medication or significant distress and interference with daily life because of the symptom) and for which no underlying physical illness had been diagnosed by the doctor and which have not always been the effect of drug intake (such symptoms form the basis of the CIDI diagnostic algorithm for DSM-IV somatoform disorders).
Outcome measures
Health status was measured at four sites using the Short Form Health Survey (SF-36 or SF-12) Reference Gandek, Ware, Aaronson, Apolone, Bjorner and Brazier27 physical and mental health component summary scores or the EQ-5D. Reference Williams28 At other sites individual questions were used (online Table DS1). Healthcare use was measured at all but two sites. It was measured retrospectively except at one site, where it was also measured prospectively (online Table DS2).
Table 1 Participating sitesFootnote a

| Author, location | Age group, years |
Participants n |
Measure of somatic symptoms |
Measure of mental disorder |
Measure of physical illness |
|---|---|---|---|---|---|
| EssauReference Essau 12 Bremen, Germany | Adolescent 12-17 | 875 | SCL-90-R somatisation subscale | CIDI depression | None |
| Lieb et al, Wittchen et al Reference Lieb, Zimmermann, Friis, Hofler, Tholen and Wittchen 13 - Reference Lieb, Isensee, von Sydow and Wittchen 15 (EDSP study) Munich, Germany | Adolescent 14-24 | 3021 | CIDI lifetime | M-CIDI | None |
| Rief et al,Reference Rief, Mewes, Martin, Glaesmer and Brähler 16 Mewes et al Reference Mewes, Rief, Brahler, Martin and Glaesmer 17 Marburg, Germany | Adult 14-93 | 2510 | PHQ-15 | PHQ | None |
| Leiknes et al Reference Leiknes, Finset and Moum 18 Oslo, Norway | Adult 18-91 | 1668 | CIDI lifetime | CIDI | Checklist of 13 disorders (patient completed) |
| Jacobi et al Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb 19 Dresden, Germany | Adult 17-66 | 4181 | CIDI lifetime | M-CIDI | Checklist of 16 disorders (physician completed) |
| All pain symptoms and medically unexplained pain symptoms | |||||
| Zerssen 14 somatic symptoms score | |||||
| Ladwig et al Reference Ladwig, Marten-Mittag, Formanek and Dammann 20 Munich, Germany | Adult 25-69 | 7466 | Zerssen 14 somatic symptoms score | The 10 non-somatic items of the Zerssen scale | Checklist of 31 disorders (physician completed) |
| Rosmalen et al Reference Rosmalen, Tak and de Jonge 21 Groningen, The Netherlands | Adult 33-79 | 1094 | CIDI 1.2 lifetime and over past year | SCL-8 for depression and anxiety | Checklist of medical disorders (patient completed) |
| All symptoms and medically unexplained symptoms | |||||
| Creed et al Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson 10 Manchester, UK | Adult 25-66 | 1443 | SSI | HADS | Checklist of 8 disorders (patient completed) |
| SumathipalaReference Sumathipala 22 Sri Lanka | Adult 18-75 | 6119 | PHQ-15 | PHQ | Physical illness yes/no (patient completed) |
SCL-90-R, Symptom Checklist-90-Revised; CIDI, Composite International Diagnostic Interview; EDSP, Early Developmental Stages of Psychopathology Study; M-CIDI, Munich version of CIDI; PHQ-15, Patient Health Questionnaire; SSI, Somatic Symptom Inventory; HADS, Hospital Anxiety and Depression Scale.
a. See online supplements DS1 and DS2 for details of measures used for somatic symptoms.
Covariates
Anxiety and depressive diagnoses or measures of anxiety or depressive symptoms were recorded at all sites (five sites used the CIDI, two used PHQ-9 Reference Kroenke, Spitzer and Williams29 depression and PHQ-7 anxiety (or ‘GAD-7’), Reference Spitzer, Kroenke, Williams and Lowe30 one used the Hospital Anxiety and Depression Scale (HADS) Reference Zigmond and Snaith31 and one the Zerssen psychological items). General medical illnesses had been measured at four sites using self-administered checklists, by a doctor in Dresden Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb19 and Munich (Ladwig et al) Reference Ladwig, Marten-Mittag, Formanek and Dammann20 and by a single question in Sri Lanka. Reference Sumathipala22 At six sites we were able to use a core set of covariates in the multivariate analyses: age, gender, anxiety, depression and general medical illness. At three sites there was no measure of general medical illness (Table 2).
At one site only (Manchester) Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 we assessed the proportion of participants who fulfilled the criteria of numerous somatic symptoms, concerns about seriousness of symptoms and marked health anxiety (criteria A and B of DSM-5 somatic symptom disorder). For this purpose we identified those in the top 20% of SSI scores (this corresponds to six somatic symptoms that bothered the respondent quite a bit or worse), and who worried ‘quite a bit’ or ‘a great deal’ (a) about there being something seriously wrong with their body and (b) about their health.
Statistical analysis
In order to demonstrate the distribution of scores in the populations, data are presented in graphical form as a frequency/density plot of total symptom scores (and for medically unexplained symptoms), split by gender, anxiety, depression or physical illnesses.
In order to establish the variables that were correlated with total somatic symptom score at each site we used multiple regression analysis with total somatic symptom score as the dependent variable. The independent variables were: age, gender, anxiety, depression (all sites) and number of general medical illnesses (six sites only). Unstandardised regression coefficients are presented.
In order to test the main hypothesis, we used multivariable analysis to assess the association between somatic symptom score (as an independent variable) and health status and healthcare use (as dependent variables). The following potential confounders were included as independent variables: age, gender, anxiety, depression, general medical disorders (if available) and any other relevant confounders (listed in column 3 in Tables DS1 and DS2). We used multiple regression analysis for continuous dependent variables, logistic regression for dichotomous dependent variables and negative binomial regression when the dependent variable was a number of visits to the doctor. At two sites, no health status or healthcare use data were available. Results presented are standardised regression coefficients for multiple regression analyses, odds ratios per standard deviation for logistic regression or incidence rate ratios per standard deviation for negative binomial regression. This allowed direct comparison of coefficients for total symptom score and medically unexplained symptoms score; the significance of any difference between these was assessed using the stata test command.
To compare total somatic symptom score, number of medically unexplained symptoms and anxiety/depression score as predictors of health status, we used data from Groningen. Reference Rosmalen, Tak and de Jonge21 We performed receiver operating characteristic (ROC) curve analyses to compare each of these as predictors of five EQ-5D subscales at a 2-year follow-up.
Table 2 Correlates of somatic symptom scores using multiple regressionFootnote a

| Author, location | Age group | Instrument | Recent or lifetime symptoms |
Significant correlates of somatic symptoms score | |
|---|---|---|---|---|---|
| Studies that assessed MUS and total somatic symptom score using CIDI | |||||
| Lieb et al, Wittchen et al Reference Lieb, Zimmermann, Friis, Hofler, Tholen and Wittchen 13 - Reference Lieb, Isensee, von Sydow and Wittchen 15 (EDSP study) Munich, Germany | Adolescent | M-CIDI lifetime | All lifetime symptoms | Age (b = 0.09 per year), female (b = 0.47), anxiety (b = 1.75), depression (b = 1.62). No measure of physical illness available | |
| Leiknes et al Reference Leiknes, Finset and Moum 18 Oslo, Norway | Adult | CIDI lifetime | All lifetime symptoms | Female (b = 0.87), severe physical illnesses (out of 13) (b = 0.95), anxiety and/or depression (b = 2.32). Age not significant | |
| Rosmalen et al Reference Rosmalen, Tak and de Jonge 21 Groningen, The Netherlands | Adult | Lifetime CIDI 1.2 | All lifetime symptoms | Age (b = −0.04), female (b = 1.48), number of physical illnesses (b = 2.29), any CIDI diagnosis, major depressive disorder, panic or generalised anxiety disorder (b = 2.87) | |
| Jacobi et al Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb 19 Dresden, Germany | Adult | M-CIDI somatic symptoms | All lifetime pain symptoms | Age (b = −0.01), female (b = 0.21), physical illnesses (b = 0.40), major depressive disorder (b = 0.41), anxiety disorder (b = 0.51) | |
| Studies that assessed total somatic symptom score using questionnaires | |||||
| EssauReference Essau 12 Bremen, Germany | Adolescent | SCL-90-R somatisation subscale | Recent | Female (b = 1.57), major depressive disorder (b = 2.80).Footnote b No measure of physical illness available | |
| Rief et al,Reference Rief, Mewes, Martin, Glaesmer and Brähler 16 Mewes et al Reference Mewes, Rief, Brahler, Martin and Glaesmer 17 Marburg, Germany | Adult | PHQ-15Footnote c | Recent | Age (b = 0.02 per year), female (b = 0. 29), anxiety (b = 0.52), depression (b = 0.24). No measure of physical illness available | |
| Jacobi et al Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb 19 Dresden, Germany | Adult | Zerssen 14 somatic symptoms score | Recent | Age (b = 0.08 per year), female (b = 1.24), physical illnesses (b = 2.14), major depressive disorder (b = 2.14), anxiety disorder (b = 3.52), panic disorder (b = 2.18) | |
| Ladwig et al Reference Ladwig, Marten-Mittag, Formanek and Dammann 20 Munich, Germany | Adult | Zerssen 14 somatic symptoms score | Recent | Age (b = 0.03 per year), female (b = 0.60), physical illnesses (b = 0.58 per diagnosis), Zerssen ‘depression’ (b = 1.00) | |
| Creed et al Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson 10 Manchester, UK | Adult | SSI score only | Recent | Female (b = 1.12), physical illnesses (b = 3.05 per illness), HADS anxiety score (b = 0.49), HADS depression score (b = 0.62). Age not significant | |
| SumathipalaReference Sumathipala 22 Sri Lanka | Adult | PHQ-15Footnote c | Recent | Age (b = 0.02 per year), female (b = 0.58), physical illnesses yes/no (b = 1.45), PHQ-7 anxiety score (b = −0.05), PHQ-9 depression score (b = 0.41) | |
MUS, medically unexplained symptoms; EDSP, Early Developmental Stages of Psychopathology Study; M-CIDI, Munich version of Composite International Diagnostic Interview; CIDI, Composite International Diagnostic Interview; SCL-90-R, Symptom Checklist-90-Revised; PHQ, Patient Health Questionnaire; SSI, Somatic Symptom Inventory; HADS, Hospital Anxiety and Depression scale.
a. The dependent variable was the relevant measure of somatic symptoms used at each site. The independent variables were age, gender, anxiety, depression and general medical illness, where available. Figures are the unstandardised regression coefficient, b, for each correlate.
b. Only included adolescents aged 12-17 years. No measure of physical illness was available. Only depression was entered as a psychiatric diagnosis, since anxiety was only reported by one participant, who also had depression.
c. The PHQ-15 excluding two depression items and one female-only item.
Using data from Manchester Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 we identified participants with high SSI scores and marked worry about the seriousness of their symptoms and marked health anxiety as defined above. We compared the physical and mental summary scores of SF-12 and the thermometer measure of EQ-5D for this group with the remainder of the participants using ANCOVA to adjust for age, gender, number of general medical illnesses and HADS score. Analyses were carried out in SPSS version 16 or 19, and Stata version 11 on Windows.
Results
Total somatic symptom score in the population
The most common somatic symptoms reported were: back, joint, head and abdominal pains and pain in the extremities. These were reported by 11-77% of respondents on most measures. By contrast, medically unexplained somatic symptoms were reported by 11% or fewer of respondents (online supplements DS1 and DS2).
At all sites the somatic symptom score was distributed as a positively skewed continuous distribution. This was true for total somatic symptom score (Fig. 1) and for medically unexplained symptoms only (Figs 2(c) and 2(d)). The curve is moved to the right in women and for participants who had anxiety or depressive disorder or general medical illnesses (Fig. 1). This effect of anxiety, depressive or general medical disorders is similar for total somatic symptom score (Figs 2(a) and (b)) and for medically unexplained symptoms (Figs 2(c) and (d)).

Fig. 1 Dresden data: probability density plots for Zerssen somatic symptom scores by (a) gender, (b) anxiety disorder, (c) number of physical illnesses and (d) major depressive disorder.
CIDI, Composite International Diagnostic Interview.
Correlates of total somatic symptom score
The correlates of total somatic symptom score for each site are shown in Table 2. At all sites female gender, anxiety, depression and general medical illnesses (where measured) were significantly correlated with a higher somatic symptom score. Older age was associated with increased number of somatic symptoms at five sites.
Total somatic symptom score and health status
After adjustment for age, gender, anxiety/depression, general medical illness (where available), and other relevant covariates, total somatic symptom score was a correlate of health status at all seven sites where this was assessed (Table DS1). Five of these analyses were cross-sectional, but at the two sites with prospective data (Groningen Reference Rosmalen, Tak and de Jonge21 and Manchester Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 ) baseline total somatic symptom score predicted subsequent health status (1-2 years later) after adjustment for confounders.
Total somatic symptom score and healthcare use
In all five cross-sectional analyses, where relevant data were available, total somatic symptom score was significantly correlated with (retrospectively reported) healthcare use after adjustment for confounders (Table DS2). In one prospective study (Manchester Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 ), baseline total somatic symptom score (SSI) was correlated with retrospective, but not prospective, healthcare use.
Comparison of total somatic symptom score and medically unexplained symptoms
At the four sites where we could analyse both, the correlates of number of medically unexplained symptoms were similar to those shown for total somatic symptom score (Table 2, further details available from the authors on request).
For the four sites where data were available (Table DS1) the association with health status, after adjustment for confounders, was stronger for total somatic symptom score than for number of medically unexplained symptoms. This difference was significant for Munich (EDSP study) Reference Lieb, Zimmermann, Friis, Hofler, Tholen and Wittchen13-Reference Lieb, Isensee, von Sydow and Wittchen15 (P = 0.006); Oslo Reference Leiknes, Finset and Moum18 (P<0.001); and Dresden Reference Jacobi, Wittchen, Muller, Holting, Sommer and Lieb19 (P<0.001 for SF-36 physical but not SF-36 mental component score) and Groningen Reference Rosmalen, Tak and de Jonge21 (mobility (P = 0.044), self-care (P = 0.002), usual activities (P<0.001) and pain/discomfort (P = 0.007)).
The prospective data from Groningen Reference Rosmalen, Tak and de Jonge21 indicated also that total somatic symptom score was a more accurate predictor of follow-up EQ-5D scores than the number of medically unexplained symptoms (Table 3). For the four EQ-5D subscales except anxiety/depression, the area under the curve (AUC) was significantly greater for total symptom score (AUC = 0.76-0.84) than for medically unexplained symptoms (AUC = 0.61-0.69).
Outcome when both numerous somatic symptoms and additional health concerns and anxiety are present
The data from Manchester Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10 showed that the participants who had a high total somatic symptom score (SSI score of 26 or more) and who also expressed concerns about the seriousness of their bodily symptoms and marked health anxiety (n = 23, 2.5% of the sample) had more impaired health status than participants who had a low total somatic symptom score or a high total somatic symptom score without the additional psychological features (Table 4).

Fig. 2 Groningen data: probability density plots for lifetime (a) total symptoms by number of physical illnesses, (b) total symptoms by number of psychiatric disorders, (c) medically unexplained symptoms (MUS) only by number of physical illnesses and (d) medically unexplained symptoms only by number of any psychiatric disorders.
Psychiatric disorder: major depressive disorder, generalised anxiety or panic disorder.
Discussion
Main findings
This study has two new important findings. First, whichever somatic symptom measure was used, total somatic symptom score was associated with female gender, anxiety, depression and general medical illness at all sites where these were measured. Second, and most importantly, after adjustment for these confounders, total somatic symptom score was associated with health status and healthcare use in cross-sectional analyses and predicted health status in the two prospective studies. Furthermore, our results suggest strongly that the association with (physical) health status and healthcare use was somewhat stronger for total somatic symptom score than for number of medically unexplained symptoms alone. We were able to test, at one site only, whether outcome is impaired most markedly when a high total somatic symptom score was accompanied by high health anxiety and marked concern about the seriousness of bodily symptoms, and found this to be the case.
Table 3 Groningen dataFootnote a

| EQ-5D scores | |||||
|---|---|---|---|---|---|
| Mobility | Self-care | Usual activities | Pain/discomfort | Anxiety/depression | |
| Total somatic symptom score, AUC (95% CI) | 0.76 (0.73-0.80) | 0.84 (0.78-0.89) | 0.77 (0.73-0.81) | 0.77 (0.74-0.80) | 0.68 (0.63-0.72) |
| Number of MUS, AUC (95% CI) | 0.62 (0.57-0.67) | 0.61 (0.49-0.73) | 0.67 (0.62-0.72) | 0.69 (0.65-0.72) | 0.67 (0.62-0.71) |
| Difference between AUC for total somatic symptom score and AUC for MUS, P | <0.001 | <0.001 | 0.002 | <0.001 | 0.76 |
| Symptom Checklist (SCL-8) score, AUC (95% CI) | 0.60 (0.55-0.65) | 0.73 (0.65-0.82) | 0.71 (0.67-0.75) | 0.64 (0.61-0.68) | 0.82 (0.78-0.85) |
AUC, area under the curve derived from receiver operating characteristic curve analysis; SCL, Symptom Checklist; MUS, medically unexplained symptoms.
a. Comparison of Composite International Diagnostic Interview (CIDI) symptoms over previous year using total somatic symptom score and medically unexplained symptoms only as predictors of EQ-5D scores at 2-year follow-up. Data for five EQ-5D scores (mobility, self care, etc.) scored as any problem in each domain v. no problem.
Strengths and limitations
The study has strengths and limitations that must be recognised. One of the main limitations of this study is the variety of instruments used at the different sites, which meant that we were not able to combine the results from different sites or make exact comparisons between sites. Another limitation was that, at most sites, we had only a checklist of medical illnesses completed by the respondent and we did not have a measure of severity of general medical illnesses. Only at two sites were the medical diagnoses verified by a doctor. We found that general medical illness was an important confounder of the association between number of somatic symptoms and outcome, accounting for a proportion of the variance similar to that of depression or anxiety. It is possible that severity of general medical illness might have accounted for a greater proportion of the variance; this has been inadequately considered in most previous studies. The inclusion of a single site from a different culture (Sri Lanka) Reference Sumathipala22 is also a limitation; a greater number of sites from different cultures would be necessary before making any observation about the relationship between variables across different cultures.
Table 4 Manchester dataFootnote a

| Mean (95% CI) | |||||
|---|---|---|---|---|---|
| SSI <26 (n = 737) |
SSI⩾26 but without health anxiety or marked concerns that something seriously wrong with body (n = 138) |
SSI⩾26 with either health anxiety or marked concerns that something seriously wrong with body (n = 27) |
SSI⩾26 and both health anxiety and marked concerns that something seriously wrong with body (n = 23) |
Adjusted P | |
| EQ-5D thermometer | 81.34 (80.4-82.3) | 77.4 (75.3-79.7) | 72.0 (67.0-76.9) | 61.0 (55.5-66.6)Footnote b | <0.001 |
| SF-12 physical component score | 52.2 (51.6-52.7) | 47.1 (45.8-48.4) | 44.5 (41.6-47.5) | 36.9 (33.6-40.3)Footnote b | <0.001 |
| SF-12 mental component scoreFootnote c | 50.0 (49.3-50.7) | 42.5 (40.9-44.2) | 37.4 (33.6-41.1) | 34.0 (29.8-38.3)Footnote b | <0.001 |
SSI, Somatic Symptom Inventory.
a. The EQ-5D thermometer and Short Form Health Survey (SF-12) physical and mental component scores for groups with a high total somatic symptom score with or without health anxiety and marked concerns that something is seriously wrong with body. Scores adjusted for age, gender, total number of physical illnesses and Hospital Anxiety and Depression Scale.
b. Health status significantly reduced for patients with SSI⩾26 and both health anxiety and marked concerns that something seriously wrong with body more than for the two intermediate groups, SSI⩾26 and only one or neither of health anxiety and marked concerns that something seriously wrong with body. (Bonferroni corrections were made for multiple pair-wise group comparisons).
c. Hospital Anxiety and Depression Scale total score excluded as covariate in view of high correlation with SF-12 mental component score.
On the other hand, the similarity of the results across sites, even though different measures were used, might be regarded as a strength as well as a limitation, as it suggests greater generalisability of the findings. This variation also applies to the measures of covariates (anxiety, depressive and general medical disorders), which differed at the different sites. More prospective studies are required as somatic symptoms have been excluded from many large-scale epidemiological studies, in spite of the high frequency of somatoform disorders in population studies. Reference Creed4,Reference Lieb, Meinlschmidt and Araya8,Reference Wittchen and Jacobi32,Reference Creed and Barsky33
The total number of participants in this study (total n = 28 377) makes this the largest study of its kind and the samples were all population based, thus removing the possibility of bias from treatment-seeking and weighting towards patients with mental health concerns, which is a limitation of primary care studies in the area. Reference Üün and Sartorius34
Explanation for our findings
There is a very close relationship between number of somatic symptoms, anxiety/depression and general medical illness. The number of somatic symptoms in chronic general medical illness increases with anxiety and depression Reference Katon, Lin and Kroenke35 but we have shown in this study that somatic symptoms, number of reported general medical illnesses and anxiety/depression are all independent correlates of health status. It is known that numerous somatic symptoms predict a poor outcome of depressive disorder Reference Huijbregts, van der Feltz-Cornelis, van Marwijk, de Jong, van der Windt and Beekman36 and a poor outcome of medical disorders. Reference Creed37 In this study we have shown that this negative impact of numerous somatic symptoms on outcome is a general one found in studies at several different sites, even after adjustment for confounders.
The association between total somatic symptom score and health status may have been stronger than that for medically unexplained symptoms because total somatic symptom score includes a measure of how bothersome each symptom is regarded to be by the respondent. This leads to a larger spread of scores and, in addition, includes a dimension of emotional response associated with the somatic symptom, which may add to the predictive value of the measure. This explanation cannot explain the difference between CIDI total symptom score and CIDI medically unexplained symptoms (Table DS1), as both were simple symptom scores.
There has been one previous large study of primary care attenders that demonstrated that the association between numerous somatic symptoms and impaired health status occurred with both medically explained and medically unexplained somatic symptoms; the association was strongest for people with both types of somatic symptoms. Reference Kisely, Goldberg and Simon6,Reference Kisely, Goldberg and Simon38 One clinic study has shown that the pattern of association between number of somatic symptoms and health status and healthcare costs was very similar whether the presenting symptoms were medically explained or unexplained. Reference Creed37,Reference Jackson, Fiddler, Kapur, Wells, Tomenson and Creed39 This association has been demonstrated recently in cancer and sickle cell disease, where it may be impossible to distinguish explained and unexplained somatic symptoms. Reference Kroenke, Zhong, Theobald, Wu, Tu and Carpenter40,Reference Sogutlu, Levenson, McClish, Rosef and Smith41 Our study demonstrated that even medically unexplained symptoms are associated with general medical illness. Such findings suggest that the adverse effect on outcome of multiple bothersome somatic symptoms may affect all patients whether or not they have general medical illnesses. This moves away from the view that patients with medically unexplained symptoms are a separate group; a fact that has been recognised in the DSM-5 somatic symptom disorder diagnostic category. Reference Dimsdale and Creed3
Implications
Diagnostic concepts in mental health disciplines may not be separated by natural boundaries but many have high clinical utility as they provide useful information concerning outcome, aetiology and treatment response. Reference Kendell and Jablensky42 Within this framework, our findings are important in identifying total somatic symptom score as a predictor or correlate of outcome (health status and healthcare use), independent of anxiety, depression and general medical illnesses. Thus, somatic symptoms cannot be regarded as primarily a reflection of concurrent anxiety and depression. Reference Mayou, Kirmayer, Simon, Kroenke and Sharpe43 Indeed, there is some evidence that the number of somatic symptoms is a predictor of treatment response in depression as well as other conditions. Reference Klengel, Heck, Pfister, Brückl, Hennings and Menke44-Reference Creed, Tomenson, Guthrie, Ratcliffe, Fernandes and Read46 Our findings support the validity of a separate dimension based on numerous bothersome somatic symptoms that could be a useful measure in clinical or epidemiological studies aimed at predicting health status. A diagnostic category, such as that in DSM-5, that includes distressing somatic symptoms as one criterion, should have greater clinical utility than one based on medically unexplained somatic symptoms.
Further prospective studies are needed to replicate the results presented here that total somatic symptom score is a predictor of subsequent health status and to determine whether this does indeed predict subsequent healthcare use. From the data presented here it seems likely that a short questionnaire measuring bothersome somatic symptoms might be used in large-scale population-based studies to clarify the true importance of somatic symptoms as a predictor of outcome. Reference Creed, Davies, Jackson, Littlewood, Chew-Graham and Tomenson10
The analysis of data from a single site in this study suggests that the presence of certain psychological features (criteria B of the new DSM-5 diagnosis) as well as numerous bothersome symptoms describes a group with greater impairment of health status. However, this result is limited by small numbers.
In sum, these findings are important in view of the changes to the diagnostic criteria for DSM-5 somatic symptom disorder, which move away from ‘medically unexplained symptoms’ as the core diagnostic feature to ‘any severely distressing somatic symptoms’. Reference Dimsdale and Creed3
Funding
The American Psychiatric Association funded this study. The original studies, whose data have been used in this paper were funded by: German Federal Ministry of Research, Education and Science, BMBF, Deutsche Forschungsgemeinschaft (DFG), Netherlands Organisation for Scientific Research (NOW), Norwegian Research Council, UK Medical Research Council.








eLetters
No eLetters have been published for this article.