Type 2 diabetes (T2DM) affects an estimated 55 million adults in Europe alone( 1 ). It confers an increased mortality risk, and is associated with multiple co-morbidities, decreased quality of life and a significant economic burden. Dietary modification is one of the cornerstones of T2DM management, aiming the adoption of a healthful diet that optimises metabolic control( Reference Klein, Sheard and Pi-Sunyer 2 ).
While numerous factors potentially influence the ability of individuals to turn understanding, of what constitutes a healthy diet, into practice, some nutrition knowledge is necessary to achieve this goal( Reference Spronk, Kullen and Burdon 3 ). Consequently, a key objective of self-management education in T2DM is to facilitate the acquisition of nutrition knowledge and skills, and to support informed decision-making and self-care that improves clinical outcomes, health status and quality of life( Reference Funnell, Brown and Childs 4 ). Historically, studies in T2DM examining the relationship between knowledge and clinical outcomes have focused on glycaemic control and have generally failed to identify any direct relationship( Reference Speight and Bradley 5 , Reference Van der Heide, Uiters and Rademakers 6 ). To date, a significant limitation of studies, however, has been the use of ‘total knowledge scores’ (i.e. summing of scores across multiple areas of diabetes-related knowledge), rather than measuring knowledge item by item and assessing it with respect to specific outcomes that are directly relevant to the items measured( Reference Speight and Bradley 5 ).
In the general population, a weakly positive relationship exists between nutrition knowledge and dietary intake, with the most frequent association found between higher knowledge and higher fruit/vegetable consumption( Reference Spronk, Kullen and Burdon 3 , Reference Wardle, Parmenter and Waller 7 ). However, the relationship between nutrition knowledge and dietary intake in T2DM has not been widely evaluated previously. The aim of the present study was (1) to examine diabetes-related nutrition knowledge using a validated instrument, food label use and weight satisfaction in a sample of T2DM adults managed in usual care, and (2) to investigate the relationship between diabetes-related nutrition knowledge and nutrient intake.
Materials and methods
Participants
A total of 124 adults with T2DM were recruited from the Diabetes Service, St Columcille's Hospital, Dublin, Ireland between January 2011 and June 2012. Participants were over 18 years of age, were diagnosed with T2DM at least 6 months previously, and were not pregnant or lactating. The present study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures were approved by the Ethics and Medical Research Committee, St Vincent's Healthcare Group. All patients gave written informed consent before participation.
Upon entering the service, all T2DM patients received standard dietary advice for T2DM, focused on following a healthy eating plan. In Ireland, healthy eating advice provided for T2DM is based on the Irish Food Pyramid( 8 ). This tool promotes a wide variety of portion-controlled foods including fruit and vegetables, whole-grain cereals, low-fat dairy products and protein foods, with the aim of achieving a distribution of 45–60 % carbohydrate, < 35 % fat and < 10 % saturated fat. Foods high in fat, sugar and salt such as confectioneries are recommended in moderation only( 8 ).
General diabetes knowledge and diabetes-related nutrition knowledge
General diabetes knowledge and diabetes-related nutrition knowledge was measured using the self-administered Audit of Diabetes Knowledge (ADKnowl) questionnaire, which was developed and validated for use as a cross-sectional survey instrument in T2DM populations( Reference Speight and Bradley 5 ). Further details on the ADKnowl questionnaire can be accessed at www.healthpsychologyresearch.com. The questionnaire contained twenty-seven item sets (114 items) relating to treatments, glycaemic control, physical activity, complication risks, foot care, and food and nutrition. The ADKnowl questionnaire was specifically developed and validated item by item, so that items that were not relevant to a particular purpose were removed without affecting the validity of the instrument. Scores were calculated as a percentage of items answered correctly out of all the applicable items answered, for the total instrument or for specific subscales, with a possible percentage score range of 0–100 %. The questionnaire contained two nutrition-specific subscales (item sets 11 and 12, totalling sixteen questions) that were applicable to all T2DM participants regardless of diabetes treatment type. A higher score reflected a higher knowledge level. As knowledge of nutrition facts alone may not translate through to skills or ‘process knowledge’( Reference Spronk, Kullen and Burdon 3 ), we also asked the participants about food label use, asking how frequently food labels were used in food selection and how often the content of a range of nutrients and food constituents was checked, using similar questions to those of Fitzgerald et al. ( Reference Fitzgerald, Damio and Segura-Pérez 9 ).
Dietary assessment
Procedures for the measurement, assessment and analysis of food intake in T2DM subjects have been described in detail previously( Reference Breen, Ryan and McNulty 10 ). In brief, participants were asked not to alter their usual dietary intake and to record all food and beverages consumed over four consecutive days, which included at least one weekend day. Participants were asked to give as much detail as possible regarding the types and brands of foods in addition to cooking and preparation methods. Participants quantified food intakes using a portable food-weighing scale (Tanita KD-400), manufacturers' information on food packaging, household measures (e.g. cups or tablespoons), and/or a photographic food atlas.
Dietary data were analysed, as described previously( Reference Breen, Ryan and McNulty 10 ), using the Weighed Intake Software Programme (version 3; Tinuviel Software), which contains food composition data derived from the 5th and 6th edition of McCance and Widdowson's Food Composition Tables plus all nine supplemental volumes( Reference Holland, Welch and Unwin 11 , 12 ). In addition, modifications were made to the food composition database to include composite dishes, nutritional supplements and generic Irish foods( Reference Black, Ireland and Møller 13 ). In cases where portion size was not detailed sufficiently, average food portion sizes( 14 , 15 ) were used or quantities estimated by the researcher based on their knowledge of the respondent's general eating habits as observed during the recording period. A food intake database was extracted from the Weighed Intake Software Programme, containing the nutrient breakdown for each item consumed.
BMR was estimated using the predictive equation of Henry( Reference Henry 16 ). An assessment of energy intake (EI) was conducted using the method of Goldberg et al. ( Reference Goldberg, Black and Jebb 17 ), showing the ratio of EI:BMR.
Anthropometry and sociodemographic assessment
Data on sociodemographic variables, medication use and previous diabetes education were collected. Weight was measured to the nearest 0·1 kg, in light clothing and without shoes using a Seca 665 weighing scale (Seca Limited). Height was measured to the nearest 0·1 cm using a Seca 242 stadiometer (Seca Limited). BMI was calculated using the standard formula (weight (kg)/height squared (m2)). Waist circumference was measured in duplicate, at the end of a normal expiration, to the nearest 0·1 cm, at the midpoint between the lowest rib and the iliac crest.
Biochemistry
Blood samples were drawn following an overnight fast. Glycosylated Hb (HbA1c) was measured with an automated HPLC instrument–reagent system (model HLC-723 G7; Tosoh Europe NV).
Statistical analysis
All statistical analysis was performed using PASW Statistics version 20. Continuous variables are expressed as means and standard deviations. Between-group comparisons were made using an independent-samples t test for parametric data and Mann–Whitney U test for non-parametric data. Dichotomous vari ables were compared using the χ2 test. Multivariable linear regression analysis was used to examine the relationship between nutrition knowledge and nutrient intake, adjusting for possible confounders including age, BMI, sex, EI:BMR ratio, food label use and social class. Linearity between dependent and independent variables was assessed using box plots and normal P–P plots. Scatterplots of standardised residuals were used to check for normality, linearity, extreme outliers and homoscedasticity. Undue influence of outliers was assessed with Cook's distance, and multicollinearity was also assessed. The level of statistical significance was set at P< 0·05 for all analyses.
Results
Participant characteristics
The completed ADKnowl questionnaires were returned by 118 participants (95 %). Participants were aged 57·4 (sd 5·7) years, with a mean BMI of 32·5 (sd 5·9) kg/m2 and the majority (64 %) were male. Participants were diagnosed with T2DM on average 7·7 (sd 4·8) years previously, and had moderate glycaemic control with a HbA1c of 61·2 (sd 17·7) mmol/mol. The majority (69·4 %) of the participants managed their diabetes with lifestyle plus oral hypoglycaemic agents, while 19 % also used insulin and a minority (11·6 %) did not use any medications for glycaemic management. A total of 118 individuals (95 %) recalled and self-reported the setting in which their initial diabetes dietary education was delivered: 53 % in a group-education setting delivered jointly by a dietitian and diabetes nurse specialist and 42 % in a one-to-one setting with a dietitian and/or diabetes nurse specialist. Of the T2DM participants in the study, 63 % self-reported that it was longer than 12 months since they last received dietary advice regarding T2DM from a health care professional. In the absence of a national diabetes register in Ireland, the participants' sociodemographic characteristics were found to be comparable to other baseline or cross-sectional Irish T2DM populations described in recent published literature( Reference James, Goodchild and Bashir 18 – Reference Smith, Paul and Kelly 21 ) (Table 1).
Table 1 Sociodemographic profile of Irish type 2 diabetes (T2DM) populations described in recent published literature (Mean values and standard deviations; number of participants and percentages)

OHA, oral hypoglycaemic agents; HbA1c, glycosylated Hb.
* Data were only available for the participants (n 1321) who attended retinopathy screening.
Audit of diabetes knowledge
The overall mean ADKnowl correct score was 62·3 (sd 15·1) %. There were over 70 % correct responses for subsections relating to general diabetes management, complications, physical activity, sick-day management, insulin, injecting and foot care. In contrast, subsections on diet and food, alcohol, hypoglycaemia and blood glucose control scored 60 % or less for correct responses (Fig. 1).

Fig. 1 Overall Audit of Diabetes Knowledge (ADKnowl) percentage scores. ![]() , Percentage of correct responses;
, Percentage of correct responses; ![]() , percentage of incorrect responses;
, percentage of incorrect responses; ![]() , percentage of ‘don't know’ responses.
, percentage of ‘don't know’ responses.
Audit of diabetes knowledge diet and food subscales
The average ADKnowl dietary subscale score was 59·2 (sd 16·4) %. The percentage of correct scores for individual questions on this subscale is shown in Fig. 2. Over 80 % of the participants were aware of the links between salt and blood pressure and the high fat content of fried foods, pastry and cakes. Among the participants, 92 % were aware that sugar increased blood glucose levels, while a small percentage (66·9 %) correctly identified that starchy foods also increased blood glucose levels. Of the participants, 62·9 and 59·3 %, respectively, were aware of the potential influence of fruit and fruit juice on blood glucose levels. Only 44·4 % knew that some margarines and spreads had comparable energy with butter, while a lesser number (29·8 %) were aware that not all fats and oils adversely affected cholesterol levels. There was a significant degree of confusion regarding the influence of macronutrients on blood glucose levels; 36·3 and 16·1 %, respectively, knew that the protein and fat content of foods did not directly influence blood glucose levels. Over 66 % believed that people with diabetes should avoid foods containing any sugar, while the most poorly answered question also related to carbohydrate, with only 12·1 % correctly identifying that sugar and starch require the same amount of insulin based on their carbohydrate content.

Fig. 2 Audit of Diabetes Knowledge (ADKnowl) dietary subscale questions and percentage of correct responses. BGL, blood glucose level; CHO, carbohydrate.
Nutrition knowledge and nutrient intake
When the participants were divided into two groups based on their diabetes-related nutrition knowledge score on the ADKnowl subscale, the mean EI:BMR ratio was significantly lower in participants with a lower nutrition knowledge score (1·1 (sd 0·3) v. 1·4 (sd 0·5), P< 0·005), suggesting a greater degree of dietary under-reporting (Table 2). Sociodemographic and biochemical variables, including age, BMI, social class, T2DM treatment, HbA1c, and length of diagnosis, did not differ significantly across the two groups (Table 2). Similarly, the percentage of energy from total carbohydrate, protein, fats, glycaemic load, fibre and starch did not differ across the two groups (Table 3). The percentage of energy from sugar (10·8 (sd 4·7) v. 13·7 (sd 4·6) %, P< 0·001), non-milk sugar (9·1 (sd 4·8) v. 12·1 (sd 4·7) %, P< 0·001) and fruit/vegetable intake (230·8 (sd 175·1) v. 322·8 (sd 179·7) g, P< 0·001) were significantly lower among the participants with lower nutrition knowledge, while dietary glycaemic index (61·4 (sd 4·5) v. 58·4 (sd 4·6), P< 0·002) was significantly higher. These relationships remained significant after adjusting for potential confounders, including the EI:BMR ratio (Table 3).
Table 2 Nutrition knowledge and sociodemographic variables and nutrient intake (Mean values and standard deviations; number of participants and percentages)

β, Coefficient of regression; T2DM, type 2 diabetes; OHA, oral hypoglycaemic agents; EI:BMR, energy intake:BMR; HbA1c, glycosylated Hb.
* P 1 values were calculated using one-way ANOVA or χ2 test.
† P 2 values were calculated using multivariable regression analyses, adjusting for age, BMI, EI:BMR ratio, sex, social class and food label use.
Table 3 Nutrition knowledge and nutrient intake (Mean values and standard deviations)

β, Coefficient of regression; %E, percentage of energy; AOAC, Association of Analytical Communities.
* P 1 values were calculated using one-way ANOVA or χ2 test.
† P 2 values were calculated using multivariable regression analyses, adjusting for age, BMI, EI:BMR ratio, sex, social class and food label use.
Weight satisfaction and food label use
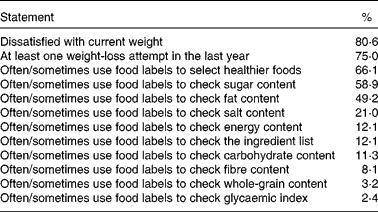
Over 80 % of the participants were dissatisfied with their current body weight, and the majority had made at least one weight-loss attempt in the last year (Table 4). The majority of the participants (66·1 %) reported reading food labels often or sometimes to select healthier foods. Participants were most likely to use nutritional labels to check the sugar content (58·9 %), followed by the fat content (49·2 %) and the salt content (21 %) of foods. A minority of the participants checked foods for their energy content (12·1 %), carbohydrate content (11·3 %) or glycaemic index (2·4 %) (Table 4).
Table 4 Weight satisfaction and food label use
Discussion
In the present study of 118 T2DM individuals managed in usual care in Ireland, the level of nutrition knowledge was lower than knowledge levels relating to many other aspects of T2DM self-management. While recognition of the role of patient knowledge has become unfashionable in recent years( Reference Speight and Bradley 5 ), dietary modification is still considered a cornerstone of effective T2DM self-management and, as such, is one of the most important areas for patients to understand, support informed decision-making and self-care. Concerning the highest levels of knowledge relating to the development and management of diabetes complications, it is arguable that having acute awareness of the negative consequences of poorly controlled T2DM without the requisite knowledge to self-manage effectively could disempower, rather than empower, patients in their diabetes management.
It appears that some fundamental dietary messages, such as the high fat content of fried foods and the links between salt and blood pressure, are reaching T2DM patients. Understanding appeared poorer in relation to more detailed or nuanced areas of diabetes-related nutrition knowledge. Specific knowledge deficits associated with the impact of macronutrients and foods on blood glucose levels were identified. The majority of the participants understood the impact of sugar on blood glucose levels, but incorrectly believed that people with T2DM needed to avoid foods containing any sugar, while a small percentage identified that starchy foods also increased blood glucose levels and required the same amount of insulin as sugar. There was also a significant degree of confusion relating to fats and oils, their energy content and their impact on cholesterol levels. The challenge of translating complex nutritional science into effective food-based dietary guidance for patients involves supporting individuals to appreciate the unique value and contribution of each nutrient (and its food sources) in their diet. Understanding the role of total carbohydrate, and not solely sugar, is fundamental to supporting food choices that promote good glycaemic control, while recognising the differences between saturated and unsaturated fat sources is key for the management of cardiovascular risk factors( Reference Evert, Boucher and Cypress 22 ). These are specific areas that clearly require greater emphasis and reinforcement during T2DM dietary education.
Previous studies using the ADKnowl measure to assess knowledge have also found deficits with respect to diabetes-related nutrition knowledge among patients managed in usual care. In a large-scale study using the ADKnowl measure to examine nutrition knowledge among 789 patients in two hospital-based UK diabetes clinics, significant knowledge deficits were identified on diet and food subscales( Reference Speight and Bradley 5 ). Also, Dyson et al. ( Reference Dyson, Beatty and Matthews 23 ) reported an average score of 61 %, which was similar to the present study, using the ADKnowl subscales on general management, diet, physical activity and alcohol, in newly diagnosed T2DM patients managed in usual care in the UK. Usual diabetes care in Ireland typically involves formal diabetes dietary education on diagnosis, but the type and frequency of ongoing education then becomes non-standardised and ad hoc. Messages relating to the fundamental role of diet in T2DM management may or may not be reinforced at 6- to 12-month intervals by the doctor, diabetes nurse and/or dietitian when the patient attends for medical review, where the primary focus is medication intensification based primarily on HbA1c levels. In the present study, 63 % of the participants self-reported that it was longer than 12 months since they last received dietary advice regarding T2DM from a health care professional. To optimise outcomes, and improve knowledge and understanding, usual care must evolve to integrate diabetes self-management education with medication management throughout the lifespan of T2DM, as recommended by the European Association for the Study of Diabetes and the American Diabetes Association( Reference Inzucchi, Bergenstal and Buse 24 ). This may involve increased dietetic resourcing on diabetes care teams and upskilling other health care professionals to competently and confidently promote dietary self-management among T2DM patients. Translation of knowledge into practical advice may benefit from more novel, experiential education strategies such as ‘teaching kitchens’ for nutrition and lifestyle classes and wearable technologies for tracking behaviours( Reference Eisenberg and Burgess 25 ).
The relationship between nutrition knowledge and dietary intake has not been widely evaluated previously in T2DM. One of the few studies was conducted by Fitzgerald et al. ( Reference Fitzgerald, Damio and Segura-Pérez 9 ) who examined this association among 200 US Latinas, 100 of whom had T2DM, using an adapted general nutrition knowledge scale and FFQ. They found a positive association between knowledge and food intake; however, this association was attenuated by food label use( Reference Fitzgerald, Damio and Segura-Pérez 9 ). As advised by Spronk et al. ( Reference Spronk, Kullen and Burdon 3 ) and Speight & Bradley( Reference Speight and Bradley 5 ), we used a nutrition subscale of a well-validated diabetes-specific instrument (the ADKnowl), and related this to nutrient intake assessed using the ‘gold’ standard methodology of a 4 d semi-weighed food diary. After having adjusted for food label use and energy under-reporting, we found that participants with higher nutrition knowledge scores had higher sugar, non-milk sugar and fruit/vegetable intake, while their overall dietary glycaemic index was lower. The finding of higher fruit and vegetable intake in individuals with a higher level of nutrition knowledge is in keeping with the existing literature in non-diabetic populations( Reference Spronk, Kullen and Burdon 3 , Reference Wardle, Parmenter and Waller 7 ). While the cross-sectional nature of the data limits conclusions about cause and effect, this may reflect an overall more balanced, healthy-eating approach to T2DM management in those with higher knowledge levels, rather than preoccupation with the restriction of specific nutrients such as sugar. These associations certainly warrant a more detailed future investigation in a larger sample. There is evidence to suggest that restriction on dietary freedom is one of the factors that has the most negative impact on quality of life in individuals with diabetes( Reference Bradley, Todd and Gorton 26 – Reference Singh and Bradley 28 ). If patients mistakenly believe that they need to avoid all foods containing any sugar, their dietary freedom will be unnecessarily restricted with potential negative consequences for quality of life. Greater nutritional knowledge will allow individuals with T2DM to make healthier food choices with less impact on quality of life, and hence improve the prospect of weight loss and longer-term maintenance of a healthier weight.
Participants reported a high level of dissatisfaction with their weight, which is unsurprising in a population with a mean BMI of 32·5 kg/m2. Weight management and energy balance is a key therapeutic task in T2DM( Reference Diabetes 29 ). The majority of the participants had a desire to manage their weight and reported using food labels to select healthier foods. In this context, the lack of focus on the energy value of food labels is of concern, but similar to the findings of Fitzgerald et al. ( Reference Fitzgerald, Damio and Segura-Pérez 9 ) where food label use was largely limited to checking the sugar content of foods. Again, supporting patients to understand the contribution of all nutrients to the energy content of foods, and the value of using this information on food labels to place energy balance in context in a practical way is a fundamental message and skill that requires greater emphasis during T2DM education.
There are a number of limitations to the present study. The data collected were cross-sectional in nature, and relied on self-reported data. The use of self-reported dietary data is open to misreporting of dietary intake, a recognised phenomenon in all self-reported dietary assessments. Participants with lower dietary knowledge had a lower EI:BMR ratio than those with higher dietary knowledge, indicating a greater degree of dietary under-reporting. However, this was adjusted for in the analysis exploring the association between nutrition knowledge and nutrient intake, reducing the potential confounding effect of dietary misreporting in this relationship. It is also possible that foods perceived as less ‘socially acceptable’ in T2DM may have been under-reported to a greater degree, and selective under-reporting of sucrose-containing foods, perceived as ‘socially undesirable’ in T2DM, may have occurred. The sample size in the present study was limited to 118 individuals with T2DM, and selection bias is a possibility in all population-based studies. However, the participants included in the present analysis are likely to be representative of the wider population, in terms of age, BMI and glycaemic control, given their similarity to other Irish T2DM populations described in the literature (Table 1)( Reference James, Goodchild and Bashir 18 – Reference Smith, Paul and Kelly 21 ).
In conclusion, the present study found significant nutrition knowledge deficits relating to the impact of macronutrients and foods on blood glucose and lipids among T2DM patients managed in usual care in Ireland. Subjects with lower nutrition knowledge reported lower sugar and fruit/vegetable intake and had an overall higher dietary glycaemic index than those with higher levels of diabetes-related nutrition knowledge. Weight management was a concern for the participants; however, they were not equipped with skills and knowledge for effective self-management of EI. Improved knowledge and understanding of food groups, macronutrients and EI for glycaemic control, weight and cardiovascular risk management is needed. This may promote a more balanced approach to dietary self-management of T2DM, rather than an overemphasis on sugar restriction. In the present study, we propose strategies for more intensive and integrated approaches to dietary education throughout the lifespan of T2DM, which may improve knowledge and skills for self-management and optimise metabolic outcomes and quality of life.
Acknowledgements
The present study was supported by the UCD Foundation Bray Lions Club Scholarship in Diabetes. The authors thank the participants, staff of the Endocrine Unit, and the Centre for Support and Training in Analysis and Research for assistance with the statistical analysis. The authors also thank Professor Clare Bradley and Rosalind Plowright for their invaluable comments on earlier drafts of the manuscript.
The authors' contributions are as follows: C. B. co-conceived the initial idea and design of the study, undertook all data collection, carried out the data analysis, and wrote the drafts of the manuscript; M. R. and M. J. G. contributed to the initial design of the study and to the redrafting of the manuscript; D. O'. S. was the study supervisor and was involved in co-conceiving the study, reviewing the data analysis, and writing and reviewing the drafts of the manuscript. All authors critically reviewed the manuscript and approved the final version of the manuscript.
The authors declare that they have no conflict of interest.









