A 61-year-old male presented to our hospital complaining of claudication: bilateral leg weakness impeding mobility. Symptoms started after 100 m of walk and recede after several minutes of rest. The patient was obese, with a body mass index (BMI) of 41 kg/m2 and reported a weight gain of about 55 pounds in the last year. Patient’s comorbidities were dyslipidemia, hypertension, and antithrombin III deficiency. The patient also suffered from chronic low-back pain recently worsened and cervical pain. Pulses in the lower limbs were present. Neurological examination was also unremarkable.
The patient was submitted to magnetic resonance imaging (MRI) of the lumbar spine that revealed a severe circumferential compression of the dural sac (from L2 to S1) caused by a relevant hypertrophy of the intracanal epidural fat (Figure 1). These findings are the characteristics of spinal epidural lipomatosis (SEL), grade 2 according to Borré, a condition already known as a rare cause of spinal stenosis.Reference Fassett and Schmidt1,Reference Borré, Borré, Aude and Palmieri2 In a previous MRI, performed 5 years before the weight gain (BMI = 33 kg/m2), for low-back pain, when claudication symptoms were not present, the epidural fat was well represented but significantly less voluminous (grade 1) (Figure 2).
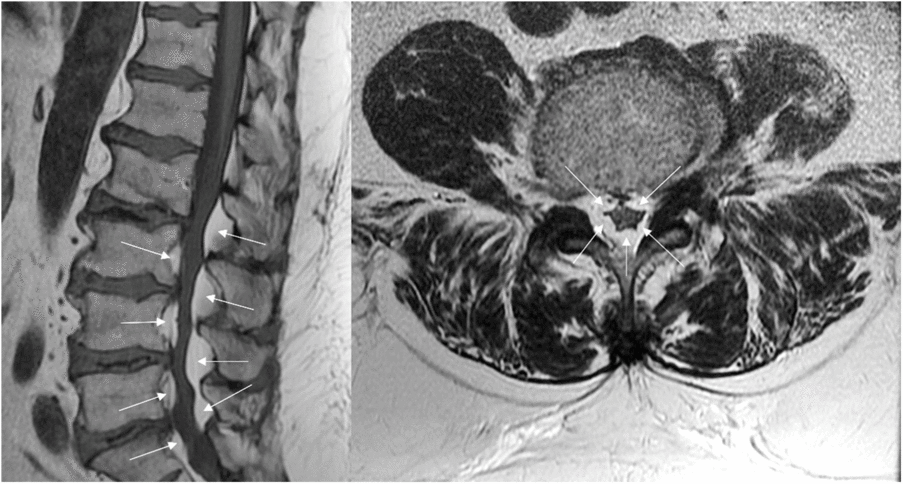
Figure 1: MRI study (T1w sagittal image on the left and T2w axial image on the right) shows a circumferential compression of the dural sac due to relevant hypertrophy of spinal epidural fat from L2 to S1 (arrows).
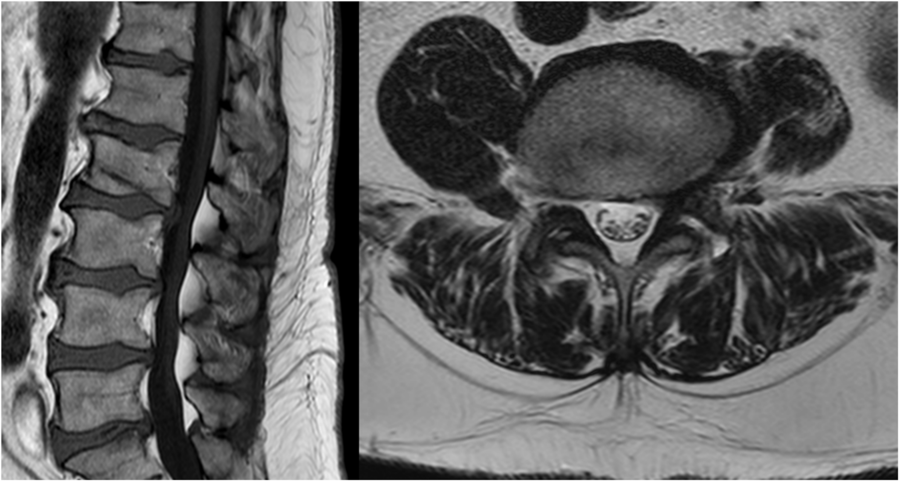
Figure 2: In an MRI study (T1w sagittal image on the left and T2w axial image on the right), performed 5 years before the weight gain, the epidural fat was significantly less voluminous.
The patient was referred to a specific program for weight loss.
SEL is an uncommon condition that usually arises in association with chronic steroid therapy, as well as in Cushing’s syndrome or obesity.Reference Fassett and Schmidt1,Reference Ishihara, Fujita and Azuma3 Moreover, recent studies suggest that SEL should be considered as a manifestation of metabolic syndrome correlated with BMI, abdominal circumference, visceral fat, and liver fat deposition.Reference Ishihara, Fujita and Azuma3,Reference Abe, Miyazaki and Ishihara4
The hypertrophic epidural adipose tissue may be located both in thoracic or lumbar spine, causing narrowing of spinal canal, compression of neural structures with a wide range of symptoms, including claudication (as in the case), progressive myelopathy, and radicular symptoms.Reference Fassett and Schmidt1
MRI is considered the best imaging modality for detecting and grading this condition; SEL grade 1 is usually asymptomatic, grade 2 is symptomatic in some cases, while grade 3 is always symptomatic.Reference Borré, Borré, Aude and Palmieri2
Weight loss and/or suspension of steroids therapy represent effective conservative treatment strategies.Reference Fassett and Schmidt1 Surgical decompression is recommended when conservative treatments fail.Reference Bayerl, Dinkelbach and Heiden5
Acknowledgements
The authors gratefully acknowledge Luciano Ussia, Senior Diagnostic Radiographer (IRCCS, Istituto Ortopedico Rizzoli), for MRI acquisition and for his enthusiastic dedication to his work.
Conflict of interest
The authors have no conflict of interest to declare.




