Introduction
As clinical researchers at academic medical institutions across the United States increasingly become the gatekeepers of complex clinical databases and registries, they often lack the statistical expertise needed to utilize the data for research purposes. This statistical inadequacy prevents junior investigators from disseminating clinical findings in top-tier, peer-reviewed journals and makes it very difficult for them to successfully obtain research funding, which in turn hampers the academic promotion process.
Underrepresented minorities (URMs), in particular, confront unique challenges as clinical investigators. First, since URMs are less likely to have participated in research-related activities during their graduate medical education, they often have more difficulty acquiring full-time faculty appointments in academic medicine than Whites [Reference Jeffe, Yan and Andriole1]. Second, URMs are less likely to be awarded National Institutes of Health (NIH) R01 grants than Whites [Reference Ginther2]. Third, URM faculty with assistant and associate professorial ranks are 32% and 19%, respectively, less likely to be promoted than similarly ranked White faculty at US medical centers [Reference Fang3].
Increasing recruitment and retention of diverse leaders and investigators in academic medicine requires comprehensive, multilevel solutions. One mechanism by which academic medical institutions can better ensure the success of both URM trainees and faculty members is by providing them with frequent opportunities to improve their methodological skills.
To fill this major gap in the statistical training of junior faculty and fellows, we developed the Applied Statistical Independence in Biological Systems (ASIBS) Short Course, a 5-year educational initiative funded by the National Institute of General Medical Sciences in 2015. The overall goal of ASIBS is to provide formal applied statistical training, via 7 weeks of distance learning and 1 week of in-person statistical computing and instruction, to junior faculty and fellows actively involved in research at US academic medical institutions, with a special emphasis on URMs.
In this paper, we present an overview of the design and implementation of ASIBS, along with our short-term evaluation of its impact from the first cohort of ASIBS participants.
Methods
Target Population
ASIBS was developed for junior faculty at the rank of Instructor or Assistant Professor and postdoctoral researchers and clinical fellows from academic medical institutions nationwide who are: (1) actively participating or will begin participating within 1 year in at least 1 biological-, social-, or behavioral-related research project, and (2) US citizens or eligible non-citizens. Up to 40 participants out of all eligible applicants are accepted each year. To ensure geographic and racial/ethnic diversity, 80% of accepted applicants are expected to be from outside of ASIBS’ academic home, the Icahn School of Medicine at Mount Sinai (ISMMS), and 50% should be URMs as defined by the NIH.
General Participant Recruitment Strategies
In the first year of ASIBS, we employed a 2-pronged participant recruitment strategy. Flyers were emailed to Centers for Medical Education and Clinical and Translational Science Award (CTSA) hubs nationwide. Our goal with this approach was to have partner Centers for Medical Education and CTSAs circulate and disseminate information about the ASIBS Short Course through their own internal communication channels. To increase visibility and outreach online, we established an easily accessible, informative and attractive Web site (currently accessible at www.asibs-statistics.com) that would appear in key-word triggered internet searches. The ASIBS Web site provides detailed information about the mission and core objectives of the course, acknowledgment of NIGMS funding, dates of instruction, eligibility, curriculum, instructors and staff, application instructions, the registration fee (i.e., $375) and deadlines, diversity fellowships, and lodging.
URM Participant Recruitment Strategies
To ensure that we could meet our recruitment goal of at least 50% URMs, we established the Diversity Recruitment Advisory Board (DRAB), which is composed of faculty (Drs A.S.P., L.N.B., and M.K.) with a long-standing commitment to mentorship and successful promotion of URM clinical and translational investigators. The primary tasks of the Diversity Recruitment Advisory Board members are as follows:
-
(1) Identify barriers to recruitment of URMs with the understanding that such barriers may differ by rank or stage in academic medical career, specialty or track, level of institutional commitment to diversity, and geographic region.
-
(2) Make effective recommendations that address the identified barriers to recruitment of URMs.
-
(3) Build on existing networks while developing new relationships with leaders of other Academic Medical Institutions, CTSAs, Centers of Excellence in Minority Medical Education, and national organizations and medical societies to expand nationwide URM recruitment outreach efforts.
-
(4) Develop methods to annually evaluate the effectiveness of URM recruitment strategies.
-
(5) Make improvements to URM recruitment efforts based on results of the annual evaluations.
ASIBS Curriculum
The ASIBS curriculum can be separated into 2 complementary components: a 7-week, online statistical theory module and a 5-day, in-person collaborative review and statistical computing instruction module hosted at the ISMMS. The specific topics of instruction and structure of the online and in-person curricula are described in detail in Tables 1 and 2, respectively.
Table 1 Detailed schedule of the 7-week, online Applied Statistical Independence in Biological Systems (ASIBS) statistical theory curriculum

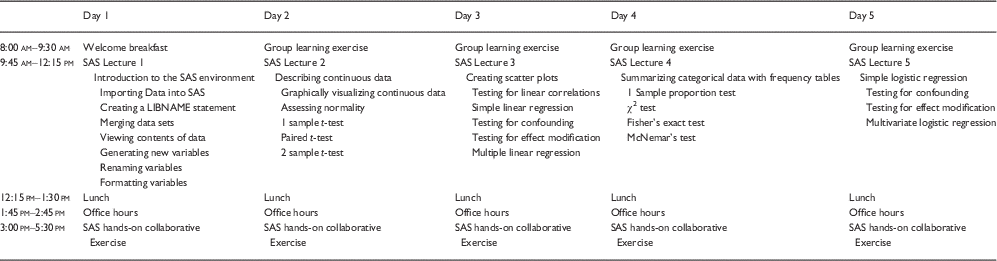
Table 2 Detailed schedule of the Applied Statistical Independence in Biological Systems (ASIBS) Short Course 1-week, in-person statistical computing curriculum
ASIBS Online Curriculum
All 7 online lectures are formatted to provide a strong but not too mathematically advanced foundation in statistical methodology. Statistical concepts are introduced through motivating real-world examples. In total, 3-hour weekly lectures are delivered via web conferencing software, which allows for real-time interaction between instructors and participants.
In developing the online curriculum we considered an optimal sequence of concepts and topics that would provide the participants with a solid working knowledge of the most commonly used introductory statistical methodologies. In the first 2 weeks, ASIBS participants become familiar with the basic concepts of statistics, study design, and probability. We then introduce 1-sample and 2-sample inference with continuous data in week 3, correlations and simple linear regression in week 4, multiple linear regression in week 5, 1-sample and 2-sample inference with categorical data in week 6, and logistic regression in the last week.
The weekly online lectures are complemented by online critical thinking/problem solving assessments to prepare participants to apply their newly gained statistical knowledge outside of the classroom. Questions are supplemented with problems taken from the medical literature or from results of actual data. Participants are asked to use the knowledge acquired through the weekly lectures to comment on the statistical approach described in the medical literature, interpret the results, and propose alternative approaches and/or to critique the researchers’ methodology.
ASIBS In-Person Curriculum
The in-person, statistical computing phase of ASIBS (Table 2) takes place over a 5-day period (Monday through Friday). This face-to-face instruction provides participants with intensive, hands-on SAS (Cary, NC, USA) instruction that complements the online curriculum. During the in-person statistical computing sessions, participants learn data management strategies and SAS programming instruction specific to the analytical topics covered in their online biostatistics lectures as well as how to interpret the statistical output. In the SAS hands-on collaborative exercises, under the guidance of the instructors, participants write their own SAS programs using publicly available data sets and work in groups to interpret their statistical output and discuss the implications of their findings in the context of the research questions of interest.
Program Evaluation
The short-term program evaluation of ASIBS consists of 3 online components: a competencies-related, a curriculum-related, and a quality-related evaluation. The competencies-related evaluation consists of a pre- and post-assessment of the ASIBS participants’ confidence in applying their topic-specific biostatistics knowledge and analyzing data using SAS. Anonymous IDs link participants’ pre- and post-assessment responses. In the curriculum-related evaluation, conducted after the completion of ASIBS, participants are asked to evaluate the strengths and limitations of the curriculum. For each topic covered in the online and in-person sessions, we assess, on a scale of 1 to 5, the clarity of the lectures, quality of the teaching material, difficulty of the material, satisfaction with the topics covered, and efficient use of time and resources. Finally, for the quality-related evaluation, also administered upon completion of ASIBS, participants evaluate organizational aspects of the course such as scheduling and logistics, meals and accommodations, proficiency and availability of instructors and teaching assistants, program coordination, and recruitment strategies.
The long-term evaluation of ASIBS assesses the impact that the short course has on participants’ research-related activities at their academic medical institutions through a short survey at 6 months and 24 months after the completion of ASIBS. In addition, the long-term evaluation facilitates the creation of a community of ASIBS alumni that allows us to follow their progress in the academic and research environment. All evaluations are conducted via REDCap [Reference Harris4].
Results
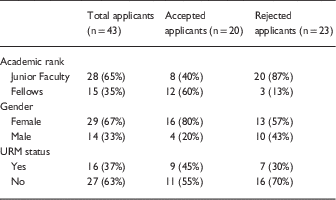
In 2016, which was the first year of ASIBS, there were a total of 43 eligible applicants (Table 3). Of these, 46.5% (n=20) were accepted into the short course, of which 80% (n=16) were female, 45% (n=9) were URMs, and 60% (n=12) were fellows. Accepted and rejected applicants were similar with respect to gender and race/ethnicity (URM vs. non-URM), while the proportion of junior faculty among the rejected applicants was more than double that of the accepted cohort (87% vs. 40%). Two major reasons for rejection were as follows: (1) personal statements in which applicants failed to articulate how participation in ASIBS and increasing their statistical competency could positively impact their long-term success as a clinical and translational researcher, and (2) applicants who were more advanced (i.e., very successful research career, more than 5 years at the assistant professor rank, etc.) than the earlier stage population ASIBS was designed to target.
Table 3 Descriptive characteristics of applicants and selected participants for the first year of the Applied Statistical Independence in Biological Systems (ASIBS) Short Course
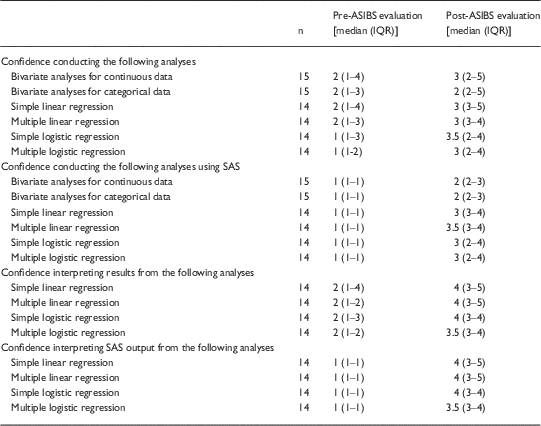
Approximately 70% (n=14) to 75% (n=15) of participants completed the pre-post competencies-related evaluation. Among those, we observed substantial improvements in their confidence conducting and interpreting introductory to more advanced statistical analyses and SAS output (Table 4). The median confidence level (on a 5-point scale) was never more than 2 prior to their participation in ASIBS, with most participants not having any prior knowledge of SAS, whereas considerable gains ranging from a median of 2 to 4 were made in their ability to conduct and interpret statistical analyses and SAS output. We did not observe improvement with respect to their confidence in conducting bivariate analyses for categorical data, but when asked about their ability to conduct bivariate analyses for categorical data in SAS and interpret their results from these analyses, improvements were observed.
Table 4 Short-term pre-post competencies-related evaluation for the first year of the Applied Statistical Independence in Biological Systems (ASIBS) Short Course
A total of 14 (70%) participants responded to the curriculum-related and quality-related evaluations. Median (IQR) overall satisfaction with ASIBS, on a 1 to 10 scale, was 8 (8–9). In fact, they all indicated that they would recommend ASIBS to their colleagues. They also found the ASIBS Web site to be highly useful with a median (IQR) of 4 (4–5), on a scale of 1 to 5. The majority (56%, n=9) thought that having the 8-week short course take place between January and March was best to ensure maximum engagement, with a quarter suggesting that ASIBS be offered between April and June.
Discussion
The first year of ASIBS was highly successful with regards to the statistical competency-related and SAS proficiency-related gains by participants along with their overall satisfaction with the quality and administration of the short course. Moreover, we were able to implement very effective strategies to ensure a racially/ethnically diverse cohort. This is of particular importance, given our primary goal to reduce the racial/ethnic gap in promotion among faculty in academic medicine. In addition, the fact that the majority of the first cohort was female is especially important since being a URM and female in academic medicine can decrease the chance of receiving NIH funding. Our effort to increase research capacities through statistical training certainly has the potential to improve funding outcomes for these important subpopulations of the clinical and translational investigator workforce.
There are 3 major strengths of the design and implementation of ASIBS. First, we were able to develop a comprehensive curriculum tailored to meet the research needs of early stage clinical investigators, while ensuring that we could successfully meet our diversity-related objectives. Second, to our knowledge, ASIBS is the first federally-funded short course with a mixed online and in-person curriculum directly aimed at increasing the statistical competency of junior faculty and postdoctoral fellows in academic medical centers nationwide. This type of curriculum is ideal for most junior investigators who cannot take long lengths of time away from their clinical responsibilities. Third, and the most important, ASIBS provided the opportunity for cross-disciplinary and cross-institutional collaboration among the participants, therefore serving as an important means for the exchange of ideas and research innovation.
We recognize 2 major areas for quality improvement of ASIBS. First, while we conducted extensive pre- and post-course evaluations, the response rate ranging from 70% to 75% was less than expected. Given that the evaluations provide us with valuable information about the background statistical knowledge of participants, increased knowledge gained as a result of participating in ASIBS, and strengths of the curriculum along with essential areas for improvement, we intend to re-emphasize the importance of these evaluations and highly encourage participants to submit the precourse evaluations upon acceptance to ASIBS and the postcourse evaluations while on-site for the in-person part of the course. Second, while we observed improvements in the statistical competency and statistical computing proficiency of the participants, the gains were more substantial with regards to their confidence in interpreting results than their confidence in conducting statistical analyses independently. To address this limitation, we will encourage future participants to bring de-identified data sets from their current research projects to the in-person session so that they can discuss with the instructors the best analytic strategies to answer their research questions and start conducting appropriate preliminary analyses. Supplementing the in-person curriculum with relevant analytic and statistical computing instruction for participants’ specific research questions and data sets may increase future participants’ confidence with regards to conducting their own analyses.
Conclusions
ASIBS provides a unique educational model to ensure that junior clinical investigators and postdoctoral fellows in academic medicine have sufficient statistical and methodological knowledge to thrive as clinical and translational investigators. This is extremely important, given the overwhelming call for innovative and rigorous, yet reproducible, study designs and analytical strategies in the clinical research community [5]. Although we have presented the findings from the short-term evaluation of the first cohort of participants, future research will evaluate the long-term impact of ASIBS on obtaining research funding, number and quality of publications, and promotion, especially with regards to increasing the opportunities for and decreasing time to promotion of URMs in academic medical centers.
Acknowledgments
Research reported in this publication was supported by the National Institute of General Medical Sciences of the NIH under Award Number R25GM111239. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. The authors would also like to acknowledge (in alphabetical order) Stefano Malerba, Anastasia Sofianou, and Maria Suprun for their assistance with the design, implementation, and administration of ASIBS. This research was first presented in a poster session at the 2016 Translational Science Conference.
Disclosures
The authors have no conflicts of interest to declare.






