Childhood obesity, defined as having a BMI ≥ 95th percentile of the age- and sex-specific US Centers for Disease Control and Prevention BMI growth charts(Reference Koplan, Liverman and Kraak1,Reference Krebs, Himes and Jacobson2) , affects 17 % of 2- to 19-year-olds in the USA(Reference Ogden, Carroll and Lawman3). Although data suggest that in recent years the prevalence of obesity has decreased among children aged 2–5 years and levelled off among children aged 6–11 years, childhood obesity remains a top public health concern(Reference Ogden, Carroll and Lawman3). Children who are obese are at an increased risk of high blood pressure and other adverse cardiometabolic conditions and at an increased risk of chronic diseases such as type 2 diabetes and CVD during adulthood compared with children who are normal weight(Reference Daniels4). Hence there continues to be a need to identify targets for childhood obesity prevention and treatment.
Diet is a well-established modifiable risk factor for obesity(Reference Brown, Halvorson and Cohen5,Reference Waters, de Silva-Sanigorski and Hall6) and targeting snack occasions specifically may be beneficial in children(Reference Hess and Slavin7). Data from the National Health and Nutrition Examination Survey (NHANES) 2013–2014 indicate that over 95 % of 2- to 11-year-old children have at least one self-identified snack occasion daily(8). Further, the foods and beverages consumed during respondents’ self-identified snack occasions account for approximately 25 % of children’s total daily energy intake(9). Defining snack occasions by self-identification is one of many approaches used in the literature. Although this approach promotes inter-individual differences in the definition of snack occasions by relying on participants’ own perceptions of what a snack occasion is, it offers advantages over other definitions. Specifically, this approach accounts for cultural and lifestyle differences in meal times and meal compositions that other definitions of snack occasions may not take into consideration(Reference Johnson and Anderson10,Reference Murakami and Livingstone11) . Thus, for the purpose of the present paper, ‘snack occasion’ refers to an eating occasion specifically designated as such by an individual.
Among studies that use this definition of snack occasion, the association of characteristics of snack occasion (e.g. snack occasion frequency) with diet quality and BMI is unclear(Reference Murakami and Livingstone11–Reference Murakami and Livingstone15). Further, although previous studies have examined how individual foods/beverages are associated with diet quality, no studies have derived dietary patterns based on foods/beverages consumed during respondents’ self-identified snack occasions. Such an approach may provide a better indication of how foods/beverages consumed during snack occasions interact to affect overall diet quality(Reference Hu16). Snack-occasion-specific dietary patterns have been derived using adult populations in the USA and these patterns have been differentially associated with cardiometabolic risk(Reference Nicklas, O’Neil and Fulgoni17,Reference Shin, Song and Krumhar18) and obesity(Reference Nicklas, O’Neil and Fulgoni17). Therefore, deriving these patterns for a child population may provide valuable insight into the intake of children and potentially clarify how intake during snack occasions is associated with diet quality and obesity in this age group.
In the present research we aimed to elucidate whether targeting snack occasions in childhood may be beneficial for future childhood obesity prevention and treatment efforts. We described snacking characteristics (i.e. frequency of snacking, snack energy consumed, snacking companions and screen use while snacking) and snack-occasion-specific dietary patterns in children and examined associations of these characteristics and patterns with diet quality and BMI. We hypothesized that a high snacking frequency, primarily snacking with others and primarily snacking without screen use would be associated with a higher Healthy Eating Index-2010 (HEI-2010) score and lower BMI. Based on the consistency of prior findings reported in the extant literature, we further hypothesized that energy intake during snack occasions would not be predictive of HEI-2010 score and BMI. In addition, we hypothesized that the snack-occasion-specific dietary patterns observed in each study would be associated with HEI-2010 score and BMI.
Methods
Research population
The present research used baseline data from the four Childhood Obesity Prevention and Treatment Research (COPTR) Consortium studies. The COPTR Consortium is comprised of two obesity prevention randomized controlled trials (University of Minnesota, Now Everyone Together for Healthy and Amazing Kids (NET-Works)(Reference Sherwood, French and Veblen-Mortenson19) and Vanderbilt University, Growing Right Onto Wellness (GROW)(Reference Po’e, Heerman and Mistry20)), two obesity treatment randomized controlled trials (Stanford University, GOALS(Reference Robinson, Matheson and Desai21) and Case Western Reserve University, Ideas Moving Parents and Adolescents to Change Together (IMPACT)(Reference Moore, Borawski and Cuttler22)) and a Research Coordinating Unit (University of North Carolina at Chapel Hill)(Reference Pratt, Boyington and Esposito23). All four studies recruited predominantly low-income, racial/ethnic minority populations for randomized controlled trials of three-year multilevel interventions(Reference Sherwood, French and Veblen-Mortenson19–Reference Pratt, Boyington and Esposito23). Participants in each study were recruited over approximately 18 months from 2012 to 2014. By design, each study had different intervention protocols, sample sizes and eligibility criteria. Children of pre-school age were recruited for the NET-Works (n 534, 2- to 4-year-olds with BMI ≥ 50th percentile) and GROW (n 610, 3- to 5-year-olds with BMI ≥ 50th and <95th percentile) studies(Reference Sherwood, French and Veblen-Mortenson19,Reference Po’e, Heerman and Mistry20) . Overweight or obese pre-adolescent and adolescent children were recruited for the GOALS (n 241, 7- to 11-year-olds with BMI ≥ 85th percentile) and IMPACT (n 360, rising 6th graders with BMI ≥ 85th percentile, resulting in recruitment of 10- to 13-year-olds) studies(Reference Robinson, Matheson and Desai21,Reference Moore, Borawski and Cuttler22) . Additional details of the COPTR Consortium and each intervention study have been published previously(Reference Sherwood, French and Veblen-Mortenson19–Reference Pratt, Boyington and Esposito23).
Dietary assessment
Two or three dietary intakes for the index child from each family were measured with 24 h dietary recalls using the Nutrition Database System for Research (NDSR) software (versions 2011–2013) developed by the Nutrition Coordinating Center, University of Minnesota, Minneapolis, MN, USA(Reference Pratt, Boyington and Esposito23,Reference Schakel, Sievert and Buzzard24) . Dietary recalls were collected in person during the initial visit for all studies except GROW, whose initial dietary recall was completed over the telephone. The second and third dietary recalls were completed over the telephone for all studies except NET-Works, whose recalls were primarily conducted in person. Despite these varying protocols, no differences have previously been found in the accuracy of in-person v. telephone dietary recalls in US children(Reference Baxter, Thomspon and Litaker25). All recalls were conducted in English and Spanish, with the aim of collecting data from both weekends and weekdays(Reference Sherwood, French and Veblen-Mortenson19–Reference Moore, Borawski and Cuttler22). In the GOALS and IMPACT studies, the child self-reported his/her dietary intake with parental/guardian assistance as needed(Reference Robinson, Matheson and Desai21,Reference Moore, Borawski and Cuttler22) . For the pre-school-aged children in the NET-Works and GROW studies, a parent/guardian served as a proxy for the child(Reference Sherwood, French and Veblen-Mortenson19,Reference Po’e, Heerman and Mistry20) . Respondents were provided with two-dimensional food portion aids to assist in identifying portion sizes(Reference Sherwood, French and Veblen-Mortenson19–Reference Moore, Borawski and Cuttler22). For children in childcare, food records were given to the childcare provider and the completed form was used by the parent/guardian to report foods the child consumed while in childcare(Reference Sherwood, French and Veblen-Mortenson19,Reference Po’e, Heerman and Mistry20) .
Snack occasions included NDSR self-identified eating occasions labelled ‘snack’ or ‘beverage only’. The two- or three-day means were calculated for all eating occasions combined and for snack occasions only. Average intakes of food groups were calculated based on the average of each child’s dietary recalls. The child or adult proxy also reported who the child was eating with at each eating occasion (alone; with family members only; with non-family members only; with both family and non-family members) and screen use while eating (no screen use; watching television; watching a videotape or movie on a VCR or DVD player; playing video games or playing on a computer) as part of the NDSR protocol(Reference Pratt, Boyington and Esposito23,Reference Schakel, Sievert and Buzzard24) .
Outcome assessment
Diet quality was computed using HEI-2010(Reference Guenther, Casavale and Kirkpatrick26). The HEI-2010 includes nine adequacy components (total fruit; whole fruit; total vegetables; greens and beans; whole grains; dairy; total protein foods; seafood and plant proteins; fatty acids) and three moderation components (refined grains; sodium; empty calories)(Reference Guenther, Casavale and Kirkpatrick26). Participants received a score for the twelve components and the component scores were summed to create the HEI-2010 score(Reference Guenther, Casavale and Kirkpatrick26). For the adequacy components, a higher score indicates higher consumption, and for the moderation components, a higher score indicates lower consumption(Reference Guenther, Casavale and Kirkpatrick26). The HEI-2010 score ranges from 0 to 100, with higher scores indicating better diet quality(Reference Guenther, Casavale and Kirkpatrick26).
Weight and height were measured with the child in light clothing without shoes using a standardized protocol across all studies(Reference Sherwood, French and Veblen-Mortenson19–Reference Moore, Borawski and Cuttler22). Weight was measured to the nearest 0⋅1 kg and height was measured to the nearest 0⋅1 cm(Reference Sherwood, French and Veblen-Mortenson19–Reference Moore, Borawski and Cuttler22). BMI was calculated as weight in kilograms divided by the square of height in metres. Age- and sex-specific BMI percentiles were calculated using the Centers for Disease Control and Prevention’s SAS program(27) to determine site-specific eligibility.
Covariate assessment
Primary caregivers (i.e. parents/guardians) completed questionnaires in their language of choice (English or Spanish) to assess race/ethnicity (non-Hispanic White; non-Hispanic Black; Hispanic; Multiracial; Other), age (date of birth) and sex of the child, employment status (full-time; part-time; not working for pay) of the participating parent/guardian, highest household education (less than high school; high school or equivalent; at least some college) and Supplemental Nutrition Assistance Program (SNAP) participation (yes/no)(Reference Sherwood, French and Veblen-Mortenson19–Reference Moore, Borawski and Cuttler22). Children additionally provided this sociodemographic information in the GOALS and IMPACT studies(Reference Robinson, Matheson and Desai21,Reference Moore, Borawski and Cuttler22) . However, the child-reported information was only used in analyses for the IMPACT study.
Statistical analysis
All statistical analyses were conducted separately by study for children with at least two reliable dietary recalls and no missing data for the exposures, outcomes or covariates of interest. Individuals with only one reliable dietary recall (n 1, GROW) or missing data on SNAP participation (n 1, NET-Works; n 2, GROW; n 1, GOALS) or participating parent/guardian employment (n 1, GROW) were excluded. Final analytic sample sizes for the NET-Works, GROW, GOALS and IMPACT studies were 533, 606, 240 and 360, respectively.
Snack-occasion-specific dietary patterns were derived for each study using exploratory factor analysis. The principal axis factoring approach to estimation was implemented(Reference de Winter and Dodou28), which extracts factors from the original correlation matrix with the ‘1’ values in the diagonal of the correlation matrix replaced with squared multiple correlation coefficients. These coefficients act as the initial communality estimates, but they are replaced during each iteration with new estimates based on factor loadings until the convergence criterion for extraction is satisfied. In order to meet sample size requirements for factor analysis, at least twenty observations per every variable entered in the factor analysis were required(Reference Hair, Anderson and Tatham29). Based on the sample size of the GOALS study and a review of the dietary variables, foods and beverages consumed during snack occasions and entered into analysis were limited to eleven mutually exclusive categories: (i) fruits; (ii) non-starchy vegetables; (iii) starchy vegetables; (iv) dairy foods; (v) meats; (vi) non-meat proteins; (vii) grains; (viii) savoury snacks; (ix) desserts; (x) unsweetened milk; and (xi) sugar-sweetened beverages (SSB; see online supplementary material, Supplemental Table S1 for how NDSR food/beverage groups were collapsed into eleven mutually exclusive categories). Unsweetened beverages, artificially sweetened beverages, fried fruits and fried vegetables were not considered for the factor analysis given their extremely low consumption in each sample and concerns about regrouping these items into the existing eleven categories. Condiments and added fats and sugars were excluded from analysis to avoid derivation of patterns that simply reflected two items commonly being eaten together (e.g. a grains and butter pattern). Additionally, water was omitted due to its lack of contribution to total energy intake.
Intake for each of the eleven food/beverage categories was measured as average number of servings per day consumed during snack occasions. Each category was divided by average daily total energy intake and multiplied by 1000 to adjust for energy intake, then further transformed into a Z-score to account for differences in intake distributions across food/beverage categories. Factors were retained according to the proportion criterion (i.e. until the sum of eigenvalues for the retained factors exceeded 100 % of the common variance). The factor pattern matrix was obtained using an oblique promax rotation. Oblique rotation was used to allow factors to correlate, given it was expected that individuals with a high value for one dietary pattern were likely to have a low value for another. Patterns were named according to those variables with factor loadings ≥|0⋅30|.
Multivariable linear regression models were used to examine associations between each snacking variable and (i) HEI-2010 score and (ii) BMI. Snacking variables were examined as the primary exposure in separate regression models, using either HEI-2010 score or BMI as the outcome. The snacking variables included number of snack occasions (continuous as a percentage of total eating occasions), snacking companion (two categories based on ≥50 % of snack occasions alone), snacking screen use (two categories based on ≥50 % of snack occasions with screen use), total snack occasion energy intake (continuous as a percentage of total daily energy intake) and snack-occasion-specific dietary pattern adherence. Adherence to the snack patterns was examined using quartiles and continuous factor scores. Each individual’s factor scores were computed as the sum of the eleven food/beverage groups’ standardized values for a given factor. The standardized values refer to the product of an individual’s mean intake for a given food/beverage group and the corresponding standardized scoring coefficient for the designated food/beverage group and factor. P-for-trend tests were conducted using the median factor scores for each quartile of snack pattern adherence. All models were adjusted for child’s age (continuous), child’s sex, highest household education, participating parent/guardian employment and SNAP participation. Significance was set at P < 0⋅05 for all analyses. All statistical analyses were performed using the statistical software package SAS version 9.4.
Results
Table 1 presents the characteristics of the analytic sample for each study, with the two obesity prevention studies in young children (NET-Works and GROW) grouped on the left and the two obesity treatment studies in older children (GOALS and IMPACT) on the right. HEI-2010 scores were similar across all studies but IMPACT, with scores being 63⋅7, 64⋅5 and 61⋅7 for NET-Works, GROW and GOALS, respectively, and 47⋅9 for IMPACT. All studies except IMPACT had predominantly Hispanic participants, with those in IMPACT being predominantly non-Hispanic Blacks.
Table 1 Characteristics of the analytic sample for each COPTR Consortium study, USA, 2012–2014

COPTR, Childhood Obesity Prevention and Treatment Research; NET-Works, Now Everyone Together for Healthy and Amazing Kids; GROW, Growing Right Onto Wellness; IMPACT, Ideas Moving Parents and Adolescents to Change Together; GED, General Equivalency Diploma; SNAP, Supplemental Nutrition Assistance Program; HEI-2010, Healthy Eating Index-2010.
Child’s BMI percentile refers to age- and sex-specific BMI percentile calculated using the Centers for Disease Control and Prevention’s SAS program(27).
Table 2 provides an overview of the snacking characteristics and food/beverage group intake during snack occasions by study. On average, younger children (NET-Works and GROW) had twice as many snack occasions and consumed twice as much energy during snack occasions compared with older children (GOALS and IMPACT; ∼2 snack occasions per day v. ∼1 snack occasion per day, respectively; ∼30 % of daily energy intake from snack occasions v. ∼15 % or ∼19 % of daily energy intake from snack occasions, respectively). In all studies except IMPACT, children primarily snacked with others and without screen use. Average intakes in Table 2 are expressed as average servings per day from snack occasions for the eleven food/beverage groups used to derive snack-occasion-specific dietary patterns. Among younger children, the top three contributors to snack occasion intake in terms of number of servings were SSB, fruits and desserts. SSB were also a top contributor to snack intake in older children, with the remaining highest intakes being for fruits and grains in the GOALS study and desserts and savoury snacks in the IMPACT study.
Table 2 Snacking characteristics and snack occasion food/beverage group intake of the analytic sample for each COPTR Consortium study, USA, 2012–2014

COPTR, Childhood Obesity Prevention and Treatment Research; NET-Works, Now Everyone Together for Healthy and Amazing Kids; GROW, Growing Right Onto Wellness; IMPACT, Ideas Moving Parents and Adolescents to Change Together; SSB, sugar-sweetened beverages.
† Adjusted for number of 24 h dietary recalls.
Table 3 shows the food/beverage groups that characterized the two snack-occasion-specific dietary patterns identified in each study. Factors derived for the NET-Works, GROW and GOALS studies were identical and included a lunch/dinner-meal-like pattern, henceforth referred to as the ‘meal-like pattern’, that loaded positively on non-starchy vegetables, meats and grains; and a ‘beverage pattern’ that loaded positively on unsweetened milk and SSB. Two patterns were also derived for the IMPACT study, with the ‘meal-like 2 pattern’ resembling the previously described meal-like pattern (loading positively on non-starchy vegetables and meats but also on starchy vegetables and SSB). The second factor for the IMPACT study was named the ‘dairy/grains pattern’ and loaded positively on dairy foods and grains and negatively on savoury snacks.
Table 3 Factor loadings for snack patterns derived using the analytic sample for each COPTR Consortium study, USA, 2012–2014†

COPTR, Childhood Obesity Prevention and Treatment Research; NET-Works, Now Everyone Together for Healthy and Amazing Kids; GROW, Growing Right Onto Wellness; IMPACT, Ideas Moving Parents and Adolescents to Change Together; SSB, sugar-sweetened beverages.
† Factors selected according to proportion criteria using principal axis factor analysis with promax rotation.
Results of multivariable analyses for associations of snacking companion, screen use and patterns with HEI-2010 score are provided in Table 4. Interpretations of the β coefficients for the exposure of interest are as follows. Snack occasion frequency was positively associated with HEI-2010 among young children (NET-Works and GROW), with every one-percentage-point increase in the number of snack occasions as a percentage of total number of eating occasions being associated with a 0⋅14 (95 % CI 0⋅04, 0⋅23) or 0⋅12 (95 % CI 0⋅02, 0⋅21) increase in HEI-2010 score in the NET-Works and GROW studies, respectively. Energy intake during snack occasions was inversely associated with HEI-2010 score in the IMPACT study, where every one-percentage-point increase in the amount of energy contributed by snacks to total daily energy intake was associated with a 0⋅09 (95 % CI −0⋅18, 0⋅00) decrease in HEI-2010 score.
Table 4 Associations between snacking characteristics and patterns and HEI-2010 score for each COPTR Consortium study, USA, 2012–2014†

HEI-2010, Healthy Eating Index-2010; COPTR, Childhood Obesity Prevention and Treatment Research; NET-Works, Now Everyone Together for Healthy and Amazing Kids; GROW, Growing Right Onto Wellness; IMPACT, Ideas Moving Parents and Adolescents to Change Together; Q, quartile; Ref., reference group; SNAP, Supplemental Nutrition Assistance Program.
* P < 0·05
** P < 0·01.
† All models were adjusted for child’s age, child’s sex, highest household education, participating parent/guardian employment and SNAP participation as covariates. Reference groups: primarily with others, primarily without screen use, Q1.
‡ Linear trend tests performed using median values of each factor’s quartiles.
Regarding snacking companion, a preference to snack alone compared to with others was associated with a 4⋅61-point (95 % CI −7⋅37, −1⋅85) lower HEI-2010 score in the GROW study. A preference to snack while using a screen compared to not using a screen during snack occasions was inversely associated with HEI-2010 score in all studies except IMPACT (NET-Works, −3⋅15 (95 % CI −5⋅37, −0⋅92); GROW, −2⋅44 (95 % CI −4⋅27, −0⋅61); GOALS, −5⋅80 (95 % CI −8⋅74, −2⋅86)). Significant associations between snack pattern adherence, as measured using quartiles of adherence, and HEI-2010 score were primarily limited to the meal-like pattern in younger children. Further examination of these associations using P for trend and continuous factor scores indicated a positive association between meal-like pattern adherence and HEI-2010 score in younger children (NET-Works, P for trend < 0⋅01, 2⋅95 (95 % CI 1⋅42, 4⋅48); GROW, P for trend < 0⋅01, 2⋅58 (95 % CI 1⋅23, 3⋅92)). Significant associations between measures of adherence to the beverage pattern (i.e. quartiles of adherence, P for trend and continuous factor scores) and HEI-2010 score were inconsistent within the NET-Works, GROW and GOALS studies. Associations of all measures of snacking with BMI were almost all null (Table 5), except for a preference to snack alone compared to snacking with others being associated with a 0⋅21 (95 % CI −0⋅40, −0⋅02) lower BMI in the GROW study.
Table 5 Associations between snacking characteristics and patterns and BMI for each COPTR Consortium study, USA, 2012–2014†
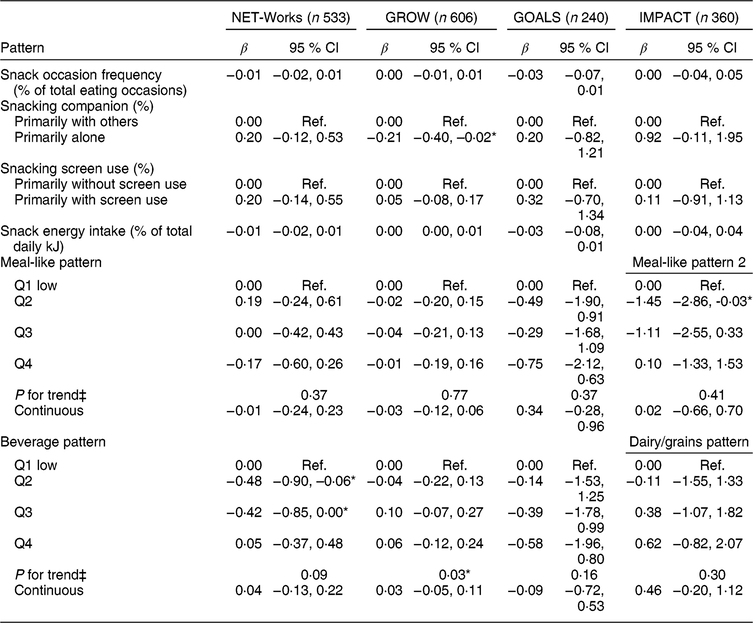
COPTR, Childhood Obesity Prevention and Treatment Research; NET-Works, Now Everyone Together for Healthy and Amazing Kids; GROW, Growing Right Onto Wellness; IMPACT, Ideas Moving Parents and Adolescents to Change Together; Q, quartile; Ref., reference group; SNAP, Supplemental Nutrition Assistance Program.
* P < 0·05, **P < 0·01.
† All models were adjusted for child’s age, child’s sex, highest household education, participating parent/guardian employment and SNAP participation as covariates. Reference groups: primarily with others, primarily without screen use, Q1.
‡ Linear trend tests performed using median values of each factor’s quartiles.
Discussion
We found that two snack-occasion-specific dietary patterns, a meal-like pattern and a beverage pattern, described intake during snack occasions for predominantly low-income, racial/ethnic minority children in each COPTR study except IMPACT. Increased adherence to a meal-like pattern during snack occasions and increased snacking frequency were positively associated with overall diet quality among younger children, while snacking while using a screen was inversely associated with diet quality in all studies except IMPACT. Associations of snacking characteristics and patterns with BMI were almost all null.
To our knowledge, the present study is the first to derive snack-occasion-specific dietary patterns for children. Despite each study being conducted in distinct geographic regions with different recruitment methods and criteria, the same two patterns were independently identified in three of the four studies. These two patterns are not consistent with those derived among adults in NHANES(Reference Nicklas, O’Neil and Fulgoni17,Reference Shin, Song and Krumhar18) , but patterns for the remaining COPTR study (IMPACT) were similar to two of the six patterns derived using NHANES 2007–2008 data(Reference Shin, Song and Krumhar18). The IMPACT study was unique in recruiting the oldest sample of participants in COPTR and being predominantly non-Hispanic Black. It is possible that snack-occasion-specific dietary patterns for IMPACT differed from those derived in the other COPTR studies due to age(Reference Northstone and Emmett30) or racial/ethnic(Reference Ritchie, Spector and Stevens31) differences in study samples.
Previous literature has indicated that overall dietary patterns are relatively stable during early childhood (defined as 3–8 years of age)(Reference Northstone and Emmett30,Reference Knol, Haughton and Fitzhugh32) and differ from those derived among adults(Reference Gubbels, van Assema and Kremers33). However, there appears to be a shift in dietary patterns between the ages of 7 and 9 years(Reference Northstone and Emmett30), after which the modified patterns track through adolescence(Reference Northstone, Smith and Newby34,Reference Mikkilä, Räsänen and Raitakari35) and are similar to those derived for adults(Reference Emmett, Jones and Northstone36). Such findings for overall dietary patterns are similar to those observed in our analyses for snack-occasion-specific dietary patterns, with the three COPTR studies that included children in early childhood having patterns similar to one another but different from the only COPTR study that did not incorporate this age range (IMPACT). However, some extant literature also shows stability in dietary patterns from early childhood through adolescence(Reference Northstone, Smith and Newby34).
Previous studies of US youth have also shown that overall dietary patterns differ by race/ethnicity(Reference Ritchie, Spector and Stevens31). In an exploratory analysis of intake during snack occasions, we observed a lower intake of unsweetened milk among non-Hispanic Blacks compared with Hispanics in all but the GOALS study (which was an almost entirely Hispanic study sample). Thus, a potential explanation as to why the beverage pattern, in which unsweetened milk was a top contributor to intake, was not observed in IMPACT is that it was the only COPTR study comprised predominantly of non-Hispanic Blacks. However, given that IMPACT also examined the oldest age group of children across COPTR studies and that milk consumption has been shown to decrease significantly from early childhood to adolescence(Reference Fiorito, Mitchell and Smiciklas-Wright37,Reference Storey, Forshee and Anderson38) , age may also explain this observation.
Significant associations for adherence to the snack-occasion-specific dietary patterns were primarily limited to increased adherence to the meal-like pattern being associated with improved diet quality among younger children. This may be explained by snack-occasion-specific dietary patterns for this age range capturing a sizeable portion of overall dietary intake (∼30 % of total daily energy intake), likely due to the relatively high number of snack occasions (∼2 snack occasions per day). Thus, by adhering to a meal-like dietary pattern during snack occasions, children were able to obtain a large portion of the components necessary for a high overall HEI-2010 score during their snack occasions.
We further found that snack occasion frequency was positively associated with HEI-2010 score in the NET-Works and GROW studies, which, to our knowledge, is a relationship that has not previously been examined in this age group. In a sample of 6–11-year-olds from NHANES 2003–2012, Murakami and Livingstone(Reference Murakami and Livingstone11) observed a null association between each additional self-identified snack occasion and diet quality. However, Evans et al.(Reference Evans, Jacques and Dallal12) reported that each additional self-identified snack occasion was associated with a 2⋅3-point increase (P < 0⋅02) in HEI-2005 score in 9–11-year-olds and a 2⋅7-point decrease (P < 0⋅01) in HEI-2005 score in 12–15-year-olds. Given these mixed findings in the literature and that we detected a significant association only among younger children, further research should examine whether age moderates the association between snacking frequency and dietary quality.
We also observed an association between snacking activity and HEI-2010 score, with a preference for snacking while using a screen being inversely associated with diet quality in all studies but IMPACT. This is in line with existing findings in children that increased screen use during eating occasions is associated with lower dietary quality(Reference Avery, Anderson and McCullough39). Existing research indicates that eating while using a screen is positively associated with intake of items that are advertised on the screen(Reference Osei-Assibey, Dick and Macdiarmid40–Reference Halford, Boyland and Hughes44), with the majority of food advertisements being for foods that are high in energy density and of low nutritional quality (high in fat, sugar or salt)(Reference Batada, Seitz and Wootan45). It is possible that a tendency to use screens during snack occasions is reflective of habits during other eating occasions, thus explaining why snack-occasion-specific activities are associated with overall dietary quality.
Despite the consistency across studies regarding snack-occasion-specific dietary patterns, snack occasion frequency and snacking screen use, significant associations for energy intake during snack occasions and snacking companion were limited to the IMPACT and GROW studies, respectively. In the IMPACT study, the magnitude of the association between snack energy intake and HEI-2010 score was relatively small and just barely significant (P = 0⋅0495). Further, in the GROW study, a tendency for snacking alone was associated with lower overall diet quality yet a seemingly disparate lower BMI. Null findings for associations of snack energy intake and HEI-2010 score in most studies may be attributable to children consuming a mix of foods and beverages during snack occasions that positively and negatively affected HEI-2010 scores. Only in the IMPACT study were traditional unhealthy snack foods/beverages (e.g. savoury snacks and SSB) the top contributors to snack occasion intake, likely explaining the slight inverse association between snack energy intake and HEI-2010 score.
The disparate findings for the GROW study regarding snacking companion associations may be due to misreporting on the 24 h dietary recall. Children lack the cognitive abilities to self-report dietary intake before the age of 7–8 years and thus parents/guardians in both the GROW and NET-Works studies completed dietary recalls on behalf of their children(Reference Livingstone, Robson and Wallace46). Although parents/guardians can accurately report dietary intake when children are cared for at home, reporting accuracy is far less for eating occasions that occur outside their supervision (e.g. in a childcare setting)(Reference Baranowski, Sprague and Baranowski47). Despite childcare providers completing food records for the parents/guardians to aid in reporting accuracy, it is possible that parents/guardians were unaware of who their child was snacking with and their assumptions regarding snacking companions led to the unexpected findings in the GROW study. Given the nature of the findings for both snack energy intake and snacking companion and that they were isolated to one of the four COPTR studies each, we hesitate to make conclusions regarding these results.
We did not find significant associations with BMI for other snacking characteristics or adherence to any snack patterns. The null findings regarding energy intake during snack occasions and BMI are consistent with existing literature(Reference Huang, Howarth and Lin14,Reference Phillips, Bandini and Naumova48) . However, previous studies using a similar definition of snack occasions and examining the association of snacking frequency and BMI have mixed findings(Reference Nicklas, Yang and Baranowski13–Reference Murakami and Livingstone15), and little to no literature has examined the association of snack patterns, companions and screen use with BMI(Reference Dubois, Farmer and Girard49,Reference Francis, Lee and Birch50) . Low variability in BMI measurements may have contributed to our null findings, particularly among the obesity prevention sites where the variance in BMI was much lower than that of the obesity treatment studies (sd in BMI of 1⋅8 and 0⋅8 kg/m2 for NET-Works and GROW, respectively, v. 4⋅0 and 4⋅9 kg/m2 for GOALS and IMPACT, respectively). Although combining the two obesity prevention and obesity treatment sites may have allowed for greater power to detect associations between the snacking characteristics and patterns and BMI, heterogeneity across the studies in eligibility, recruitment and effect sizes of the snacking associations prevented such pooling.
Social desirability bias in dietary reporting may also have had a role in our null BMI associations, particularly since all participants were enrolled in an obesity prevention or treatment programme and were thus likely aware of the link between diet and weight. Participants or their parents/guardians may have reported healthier snack foods/beverages based on the extent to which they felt the reported diet reflected their own or their child’s weight status(Reference Livingstone, Robson and Wallace46). Further, GOALS and IMPACT limited their sample to overweight and obese children, who are more likely to under-report total energy(Reference Walker, Ardouin and Burrows51), SSB and snack food(Reference Livingstone and Robson52,Reference Rangan, Allman-Farinelli and Donohoe53) intakes compared with normal-weight individuals. Evidence also suggests that parent/guardian obesity status may affect their proxy reports for children, with parents/guardians underestimating food intakes of obese children when the parent/guardian is also obese(Reference McGloin, Livingstone and Greene54). Future research is needed that can examine associations between snack occasions and BMI that accounts for these potential sources of bias before snacking recommendations can be made.
Strengths and limitations
There are numerous strengths to the present research. The four COPTR studies were comprised of low-income, racial/ethnic minority children who were diverse in terms of age and geographic location. Multiple 24 h dietary recalls were used per child in each study, and we used a simple definition of snack occasions and consistent methods to characterize snacking characteristics and patterns that could easily be applied to other studies. Further, the use of a data-driven approach to deriving dietary patterns ensured that snack-occasion-specific patterns reflected actual dietary intake in each study.
Our research is limited by the fact that we used cross-sectional data and thus the associations may not fully reflect the impact of snacking on diet quality and BMI. Also, our findings are comparable only to other studies that used a similar definition of snack occasions, which is highly variable across the literature(Reference Johnson and Anderson10). The COPTR Consortium comprises over 1700 children, but it is possible that we lacked sufficient power to detect associations between snacking characteristics and patterns and BMI when each study was analysed separately. Although it is well known that dietary recalls in general are prone to bias, particularly in children as previously discussed, it is possible that recall error may affect snacking disproportionately compared with traditional meals because snacking often occurs in less structured settings than meals. Such settings may make it difficult to identify snack occasions or to accurately capture snacking screen use or companion.
Conclusions
We found across geographically distinct studies that snack intake among predominantly low-income, racial/ethnic minority children can largely be described with two snack-occasion-specific dietary patterns: a meal-like pattern and a beverage pattern. To our knowledge, we are the first to derive such patterns for children; thus there is a need to determine whether these patterns also describe snack occasion intake in other child populations. Future research may consider deriving dietary intake patterns separately for adolescents and non-Hispanic Blacks, given our findings from the IMPACT study, and may further examine snack patterns, screen use and companions in the context of overall dietary patterns to better understand how snacking relates to diet quality and BMI.
We further found that snack occasion frequency was positively associated with diet quality, but only among younger children, and that screen use was inversely associated with overall dietary quality irrespective of the study’s sociodemographic characteristics. Although future studies should be designed to capture more in-depth detail of the contextual/environmental factors that may affect snacking behaviours, our findings contribute to the literature in suggesting that diets of 2–5-year-old children may benefit from frequent meal-like pattern snack consumption and diets of children of all ages may benefit by decreasing screen use during eating occasions.
Acknowledgements
Financial support: This research was supported by the National Heart, Lung, and Blood Institute and the Eunice Kennedy Shriver National Institute of Child Health and Development and the Office of Behavioral and Social Sciences Research (grant numbers U01 HL103561, U01 HL103620, U01 HL103622, U01 HL103629, U01 HD068890, UL 1RR024989 and NIH DK56350). The content expressed in this paper is solely the responsibility of the authors and does not necessarily represent the official views of the National Heart, Lung, and Blood Institute, the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the National Institutes of Health, or the US Department of Health and Human Services. The National Heart, Lung, and Blood Institute, the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the National Institutes of Health, and the US Department of Health and Human Services had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: M.N.L., K.P.T., D.M.M., T.N.R., J.M.B. and H.L.N. designed the research question; D.M.M., J.M.B. and A.J.T. collected data hands-on; S.M.M., T.N.R. and J.M.B. provided essential data sets; M.N.L. analysed the data; M.N.L. and K.P.T. wrote the manuscript; D.M.M., S.M.K., S.M.M., T.N.R. and J.M.B. substantially edited and critically reviewed the manuscript; M.N.L. had primary responsibility for final content. All authors have read and approved the final manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the Institutional Review Boards at the University of North Carolina at Chapel Hill, University of Minnesota, Vanderbilt University, Stanford University and Case Western Reserve University. Written informed consent was obtained from all subjects.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1368980019000958







