Mexico is in the midst of a nutrition transition(Reference Romieu, Hernandez-Avila and Rivera1, Reference Rivera, Barquera and González-Cossío2). Wasting and stunting among children <5 years of age have declined in recent years(Reference Fernald and Neufeld3–Reference Rivera, Barquera and Campirano7), while rates of obesity have risen steadily(Reference Fernald and Neufeld3, Reference Rivera, Barquera and Campirano7–Reference Sanchez-Castillo, Lara and Villa12). Data from a recent national study in Mexico showed that 20 % of children aged 2–12 years were overweight or obese(Reference Bonvecchio, Safdie and Monterrubio8). For children of pre-school age, rates of obesity were highest in northern Mexico, in urban areas such as Mexico City and among children from higher-resource families(Reference Bonvecchio, Safdie and Monterrubio8, Reference Bacardi-Gascón, Jiménez-Cruz and Jones13, Reference Villa-Caballero, Caballero-Solano and Chavarría-Gamboa14). Childhood obesity is associated with a number of adverse health outcomes that can include type 2 diabetes mellitus(Reference Freedman, Serdula and Srinivasan15, Reference Pinhas-Hamiel, Dolan and Daniels16), hypertension and hyperlipidaemia(Reference Freedman, Serdula and Srinivasan15, Reference Morrison, Sprecher and Barton17, Reference Colín-Ramírez, Castillo-Martínez and Orea-Tejeda18), asthma and sleep apnoea(Reference Leung, Li and Lam19–Reference Taveras, Rifas-Shiman and Camargo21), early maturation(Reference Vignolo, Naselli and Di Battista22, Reference Lee, Appugliese and Kaciroti23) and psychosocial stress(Reference French, Story and Perry24–Reference Puhl, Moss-Racusin and Schwartz26).
Dietary determinants of childhood obesity include excessive intake of sugar-sweetened beverages(Reference Malik, Schulze and Hu27), fruit juice(Reference Dennison, Rockwell and Baker28, Reference Faith, Dennison and Edmunds29) and high-energy foods of low nutritional value, such as chips and cookies(Reference Taveras, Berkey and Rifas-Shiman30–Reference Brownell32). A handful of previous studies have assessed dietary intake in young children in Mexico. In one study of public-school children in Mexico City, researchers found that children consumed insufficient fibre (<25 g/d) and excessive dietary fat (>35 % of daily energy)(Reference Colín-Ramírez, Castillo-Martínez and Orea-Tejeda18). A second study of children 10–19 years of age in Mexico City found that foods provided by schools were of lower nutritional quality than those brought from home(Reference Lozada, Sánchez-Castillo and Cabrera33). A study of children aged 1–4 years showed that those living in Mexico City consumed more dietary fat, carbohydrate and total energy than children in any other region in Mexico(Reference Mundo-Rosas, Rodríguez-Ramírez and Shamah-Levy34). In a national study of beverage consumption, researchers noted a substantial increase in caloric beverage intake over the past decade among pre-school and school-aged children(Reference Barquera S, Bonvecchio and Hernandez-Barrera35). The authors cited full-fat milk and sugar-sweetened fruit juice as the two primary beverages consumed by young children. However, little is known about dietary intake and the nutritional quality of foods and beverages provided to children outside the family home. The purpose of the present study was to assess the nutritional quality of foods and beverages listed on menus serving children in government-sponsored child-care centres throughout Mexico.
Methods
We reviewed and analysed a sample of fifty-four daily menus (including breakfast, lunch and afternoon snack) reflecting foods and beverages served to children attending 142 government-sponsored child-care centres in Mexico, all of whom follow the same menus. The 142 child-care centres provide care to almost 30 000 children from 6 weeks to 6 years of age. We collected menus in the spring of 2009. Menus were still in use in early 2012, but are scheduled to be re-evaluated later that year. Menus were developed by a nutritionist and were used by all government-sponsored child-care centres throughout the country. Menus varied by age, with separate menus for children aged 4–6 months, 7–9 months, 10–12 months, 13–23 months, 24–47 months and 48–72 months. A 1 d sample menu is provided in Fig. 1. We translated menus from Spanish to English prior to nutrient analysis. Since this research was limited to a menu review and did not involve human subjects, we were granted an exemption from the Institutional Review Boards at both Harvard Pilgrim Health Care and Duke University Medical Center.

Fig. 1 Sample of a 1 d menu for children aged 10–23 months attending child-care centres in Mexico, spring 2009
To assess the nutritional value of foods and beverages listed on the menus, we analysed menus using the Nutrition Data System for Research (NDS-R) software version 2005 (Nutrition Coordinating Center, University of Minnesota, Minneapolis, MN, USA). The NDS-R software generated serving sizes based on the 1992 US Department of Agriculture (USDA) Food Guide Pyramid, a national nutrition guideline system in the USA. Menus specified amounts of foods (e.g. 50 g beans) and beverages (e.g. 120 ml fruit juice) for children in each age group. The menus also included detailed ingredients for mixed dishes, which we used in the nutrient analysis. We translated serving sizes into cups and ounces for comparison with national recommendations. Generally, information about the amounts and types of foods was included on the menus. In some cases, the method of preparation, the recipe and the list of ingredients were also included. A small number of traditional Mexican foods were listed on the menus but not included in the NDS-R database. In those cases, we used the closest available substitute based on expert review by one author (e.g. Garibaldi biscuit was substituted with vanilla sponge cake). The NDS-R software does not categorize food into various groups (e.g. fruits); we therefore manually combined data into food group categories. Because NDS-R classified sweetened beverages (e.g. fruit drinks, flavoured waters, sweetened milks) and 100 % fruit juices by their ingredient components, we created a separate category for servings of juice and sugar-sweetened beverages.
We reviewed menu data to determine the amount and type of foods and beverages served to children by age group, averaged over one full day of care. These menus, however, do not reflect foods and beverages served to children at home or outside child care. First, we compared food group values with current USDA MyPlate(36) recommendations by age group. We used MyPlate recommendations because, at the time of the study, Mexico did not have national food group standards for children, with the exception of La Piramide De La Salud, which did not include specific recommendations to allow for comparisons. MyPlate recommendations represent the 2010 Dietary Guidelines for Americans food group serving sizes that replaced the USDA Food Guide Pyramid in 2011. We compared portion sizes of foods and beverages on the menus with daily MyPlate recommendations for each food group (grains, vegetables, fruits, meats and dairy). Next, we computed mean total energy, macronutrients (fat, carbohydrate and protein), fibre and sugar for each menu by age group, and compared these values with the Daily Reference Intake (DRI)(37) standards. Since MyPlate and DRI recommendations begin at age 2 years, with a few exceptions noted, we were not able to make many comparisons for dietary data from infant menus.
Results
Based on a total of fifty-four menus among children aged 24–72 months, for whom MyPlate food group recommendations exist, children in child-care centres were provided with sufficient servings of grains, vegetables, fruits, meats and meat alternatives, and dairy (Table 1). Foods listed contained some wholegrain items, but amounts were below recommendations for children aged 48–72 months. Children received more than the recommended amounts of dark (orange, red, yellow) vegetables, and these vegetables represented ∼50 % of the total vegetables listed on the menus. Moreover, fried vegetables such as French fries and fried potatoes were not listed on any of the 54 d of menus. Nearly half of the meats and meat alternatives on the menus were high-fat or fried, with high-fat beef and eggs being the most common meat items. Fewer than 4 % of total dairy items were reduced-fat and none were 1 % or fat-free. High-sugar and high-salt snack foods were not often listed on the menus.
Table 1 Foods and beverages from fifty-four Mexican child-care centre menus compared with MyPlate recommendations by age*

FDA, Food and Drug Administration.
*MyPlate recommendations start at age 24 months. Age 24–47 months is based on a 5·02 MJ (1200 kcal) diet as recommended by MyPlate (2010 Dietary Guidelines for Americans) for a 3-year-old girl, active 30–60 min/d. Age 48–72 months is based on a 5·86 MJ (1400 kcal) diet as recommended by MyPlate (2010 Dietary Guidelines for Americans) for a 5-year-old girl, active 30–60 min/d.
†Based on amounts recommended weekly by MyPlate (2010 Dietary Guidelines for Americans). Dark vegetable recommendation combines green vegetables and orange vegetables.
‡Sweetened milk is categorized under both the dairy and sweetened beverage categories. Of sweetened beverages, sweetened milk accounts for 27 % (3·6 oz) of the total for age 13–72 months and 0 % for age 10–12 months.
§100 % fruit juice served as a beverage only, not as added in a recipe.
In terms of beverages, menus included some fruit juice for all age groups. Infants were provided a mean of 1·6 (sd 0·2) oz (4–6 months), 4·9 (sd 0·3) oz (7–9 months) and 1·0 (sd 0·0) oz (10–12 months) of 100 % juice daily. Older children received <1 oz/d, on average. Other sugar-sweetened beverages, such as water or milk with added sugar, were more common, with menus listing 6·9 (sd 0·0) oz/d for infants aged 10–12 months and 13·3 (sd 0·1) oz/d for children aged 13–72 months of age. Full-fat milk, including both sweetened and unsweetened, was the most common type of milk served to children of all ages. For children 13–72 months of age, menus listed an average of 1·2 cups of full-fat milk/d, with small amounts of reduced-fat milk. Of all milk served as a beverage (not in recipes), 37 % had added sugars. Children <1 year of age were also served whole cow's milk.
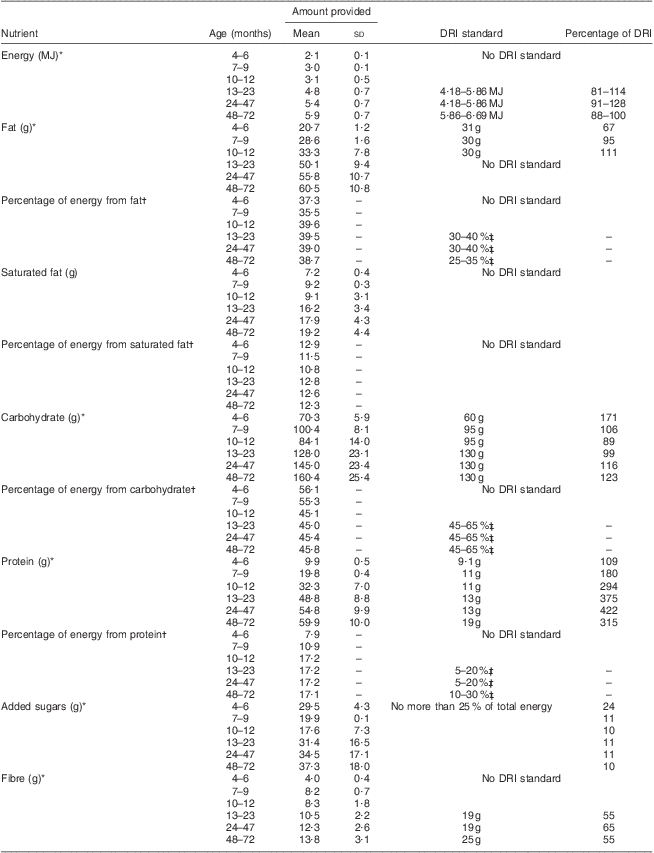
Menus yielded a mean daily energy content of 2·10 (sd 0·09) MJ for infants aged 4–6 months, 3·03 (sd 0·13) MJ for infants aged 7–9 months and 3·14 (sd 0·48) MJ for infants aged 10–12 months. For older children, menus provided 4·77 (sd 0·68) MJ/d for children aged 13–23 months, 5·36 (sd 0·73) MJ/d for children aged 24–47 months and 5·87 (sd 0·70) MJ/d for children aged 48–72 months (Table 2). Menus provided a mean daily fat amount of 20·7 (sd 1·2) g for infants aged 4–6 months, 28·6 (sd 1·6) g for infants aged 7–9 months and 33·3 (sd 7·8) g for infants aged 10–12 months, compared with the DRI of ∼30 g. There is no DRI for grams of fat for toddlers and pre-school children. For children aged 4–6, 7–9, 10–12, 13–23, 24–47 and 48–72 months, menus yielded 70·3 (sd 5·9), 100·4 (sd 8·1), 84·1 (sd 14·0), 128 (sd 23·1), 145 (sd 23·4) and 160·4 (sd 25·4) g carbohydrate/d and 9·9 (sd 0·5), 19·8 (sd 0·4), 32·3 (sd 7·0), 48·8 (sd 8·8), 54·8 (sd 9·9) and 59·9 (sd 10·0) g protein/d, respectively. Generally, the percentage of energy from fat, carbohydrate and protein was in line with DRI standards. However, the percentage of energy from fat was 38·7 % for children 48–72 months, which is slightly above the DRI recommendation of 25–35 %. According to menus, children were provided a mean daily fibre amount of 10·5 (sd 2·2) g (13–23 months), 12·3 (sd 2·6) g (24–47 months) and 13·8 (sd 3·1) g (48–72 months), which approached the DRI recommendation of 19, 19 and 25 g, respectively. Nevertheless, wholegrain foods were low for all age groups. Foods listed on the menu did not include high levels of sugar, except for sugar-sweetened milk and water. In fact, the sugar content of total daily foods was below the recommended level of 25 % for all children.
Table 2 Nutrients from fifty-four Mexican child-care centre menus compared with Dietary Reference Intake (DRI) standards by age*

*Recommended Dietary Intake/Adequate Intake (kcal converted to MJ).
†Averaged by day, not total.
‡Acceptable Micronutrient Distribution Range.
Discussion
Based on dietary data from 54 d of menus used by 142 government-sponsored child-care centres throughout Mexico, children were provided with a high number of megajoules coming from a variety of food groups while in child care. Given that children spend part, but not all of their waking hours in child care, menus listed excessive amounts of most foods, including vegetables, fruits, meats and dairy, compared with MyPlate recommendations. Average total energy and macronutrient levels were quite high for all age groups in which DRI have been established. In particular, menus included excessive grams of protein for nearly all children. Fruit juice, sugar-sweetened beverages and full-fat milk also contributed to excessive total energy.
Several explanations may exist for the excessive amount of energy listed on the menus. Since children spend 8–10 h in full-day care, child-care centres may wish to provide enough energy to meet children's energy needs for an entire day, given that some children may not receive sufficient amounts foods and beverages at home. Additionally, foods listed on the menu may provide more than the recommended amounts of energy and nutrients because child-care centres may assume that children will not eat all foods and beverages served; children may elect to consume a portion of what is offered.
Despite the excess of sugar-sweetened beverages, the total amount of added sugars to foods was just over 10 % of total energy intake for all age groups except infants 4–6 months of age. While this falls well below the liberal DRI recommendation of <25 %, it is just over the WHO recommendation of <10 % of daily energy and is more than double the American Heart Association recommendation of <16 g/d for a 5·86 MJ (1400 kcal) diet(Reference Nishida, Uauy and Kumanyika38–Reference Johnson, Appel and Brands40). This finding was true despite pervasive amounts of sugar-sweetened beverages listed on the menus. Low levels of added sugars may be due to the infrequency of processed foods; nearly all foods listed on the menu were prepared at the child-care centres from scratch, with limited reliance on pre-packaged or processed foods. Nevertheless, grains provided to children aged 48–72 months were slightly inadequate. Interestingly, fibre levels were within recommended amounts, even though wholegrain items were not. This apparent discrepancy may be due to the relatively high levels of fruits and vegetables served. Although beans are a contributor to overall fibre intake and were also listed on the menu, they did not appear frequently.
While menus suggested that the recommended average levels of dairy were served, the majority were full-fat items (for children over the age of 2 years). This finding is similar to results from Ball et al.(Reference Ball, Benjamin and Ward41), who showed that most milk served to pre-school children in US-based child care was full-fat milk. In our sample, beverages were problematic in general, with high quantities of sugar-sweetened beverages served daily. Moreover, 100 % fruit juice was provided to infants <6 months of age, and an average of 5 oz of 100 % fruit juice was served daily to infants aged 7–9 months. Additionally, menus listed cow's milk for infants <12 months of age, which goes against current recommendations to wait until children turn 1 year of age(42).
A handful of studies have assessed the diet quality of foods and beverages served to children in child care in the USA and found that children consumed inadequate amounts of fruits and vegetables, insufficient Fe and fibre, and excessive quantities of full-fat milk(Reference Ball, Benjamin and Ward41, Reference Briley, Buller and Roberts-Gray43–Reference Sigman-Grant, Christiansen and Branen47). Menu data from the present study suggest that the diet quality of foods served to children in child care in Mexico may be higher than in the USA, with greater amounts of fruits and vegetables served, and lower added sugars and processed foods. However, juice and cow's milk were introduced to infants too early, and children were served excessive amounts of full-fat milk, fruit juice and sugar-sweetened beverages. Beverages may be of lower nutritional quality due to the high prevalence of sugar-sweetened beverages. Because beverages contribute to children's overall energy intake, they may be an appropriate target for intervention in this setting.
The few published studies on overall dietary intake suggest that children consume inadequate fibre and excessive amounts of fat in the more urban areas of Mexico(Reference Colín-Ramírez, Castillo-Martínez and Orea-Tejeda18). Children also consume a high percentage of energy from beverages, including full-fat milk and fruit juice(Reference Barquera S, Bonvecchio and Hernandez-Barrera35). Our findings are consistent with this previous research, in that we found menus to provide excessive total energy, insufficient whole grains and a high prevalence of full-fat milk and fruit juice. Menus were also a source of excessive grams of protein, and the contribution from protein made up a large percentage of overall total energy.
The present study has several limitations. First, menus were obtained from government-sponsored child-care centres and may not be representative of other types of child-care programmes in Mexico. While the study population does not represent all children in Mexico, the government-sponsored centres represent roughly one-third of all child-care centres in Mexico. Children who attend organized child care in Mexico come from smaller families with higher household incomes and are more likely to have mothers with higher educational attainment than children cared for at home(Reference Flores Hernández, Reyes Morales and Pérez Cuevas48). Additionally, we analysed the nutrient composition of foods and beverages listed on the menu, not what was actually served to children. Previous data suggest that menus are a reasonably accurate source of information on categories of food (e.g. fruits and vegetables) actually served in child care(Reference Benjamin Neelon, Copeland and Ball49, Reference Fleischhacker, Cason and Achterberg50). Moreover, we did not assess actual dietary intake in children, but our previous study in the USA suggests that children consume 50–100 % of what they are offered in child-care centres(Reference Ball, Benjamin and Ward41). We also compared foods, beverages and portion sizes with US-based recommendations, given the absence of specific national standards in Mexico. We did not assess foods and beverages consumed at home or away from child care, which may provide a more complete and accurate picture of dietary consumption in children <5 years of age.
Conclusions
The present study provides insight into the quantity and nutritional quality of foods and beverages served to young children in child-care centres in Mexico, a country with rapidly rising rates of childhood obesity. Future studies should explore dietary intake to assess what children actually consume in child care and at home throughout Mexico.
Acknowledgements
Sources of funding: This work was carried out with support from a Consejo Nacional de Ciencia y Technologia (CONACyT) grant (#S0008-114027) and CAMBIO – Canada and Mexico Battling Childhood Obesity – which is funded by the Global Health Research Initiative (GHRI), a collaborative research funding partnership of the Canadian Institutes of Health Research, the Canadian International Development Agency, Health Canada, the International Development Research Centre and the Public Health Agency of Canada. M.W.G. was supported, in part, by a National Institutes of Health (NIH) grant (K24 HL068041). The Nutrition Obesity Research Centers (NORC) was supported by an NIH Clinical Nutrition Research Unit grant (DK56350). E.M.T. was supported, in part, by a grant from the National Center on Minority Health and Health Disparities (MD003963). Conflicts of interest: The authors report that they have no financial disclosures or competing interests. Author contributions: S.E.B.N. conceived of the study, coordinated the data analysis and drafted the manuscript. H.R.-M. and J.H. coordinated the exchange of the menus, provided guidance in the design of the study and reviewed and edited the manuscript. E.M.T. and M.W.G. provided scientific guidance on the development of the study and read and approved the manuscript. Acknowledgements: The authors would like to thank Sarah C. Ball for her assistance compiling results for this manuscript, as well as the NORC at the University of North Carolina–Chapel Hill for their assistance with the nutrient analysis.