INTRODUCTION
Managing patients in acute pain is an integral part of the daily reality of emergency department (ED) physicians.Reference Todd, Ducharme and Choiniere 1 Yet, to effectively relieve pain, ED physicians must first be able to quickly and efficiently assess its severity. However, there is no objective measurement for pain, and, because this experience remains entirely subjective, the patient’s verbal report must be accepted as valid.Reference Bromm 2 Intensity is the most frequently evaluated dimension of painReference Carr, Goudas and Lawrence 3 and is usually reported by patients on the widely used 0 - 10 verbal numerical rating scale (NRS)Reference Bijur, Latimer and Gallagher 4 - Reference Hjermstad, Fayers and Haugen 7 or the 0 mm - 100 mm visual analogue scale.Reference Price, McGrath and Rafii 8 The NRS is reliable and valid in clinical research, and, even though it lacks any intrinsic meaning,Reference Farrar, Young and LaMoreaux 9 it is often preferred by patients for its ease of use.Reference Dworkin, Turk and Farrar 10 , Reference Daoust, Beaulieu and Manzini 11 The patient’s pain relief is generally derived from the NRS as a percentage of pain intensity (the difference between the initial pain intensity and the final pain intensity divided by the initial pain intensity multiplied by 100). Current recommendations and provisional benchmarks for interpreting significant changes in pain outcome used the following thresholds: 10% to 20% decrease for minimal pain relief, 30% decrease for moderate relief, and 50% decrease as substantial relief.Reference Dworkin, Turk and Wyrwich 12
Recently, some clinical trials on acute pain have reported the use of a more easily measured variable as an indicator of therapy efficacy and pain relief. These reports are suggesting that simply asking the patients whether they want more pain medication is sufficient to evaluate their level of analgesia.Reference Chang, Bijur and Lupow 13 , Reference Chang, Bijur and Holden 14 It is proposed that the straightforward query “Do you want more pain medication?” better crosses the barrier of communication than analog or numerical scales and may be easier to understand for patients in severe pain.Reference Jensen and Karoly 15 Using this method, it was shown in a recent study that 99% of patients achieved some level of pain control at a given time point during the course of their protocol.Reference Chang, Bijur and Holden 14
To directly evaluate the accuracy that a patient’s refusal for supplemental pain medication can be used as a measure of pain relief, we have conducted a prospective observational study of patients in acute pain presenting to the ED. During this study, patients were asked three different questions – Is your pain relieved?, How would you rate your pain relief?, and Do you want more analgesics? – to determine whether they were relieved or not without having to rely exclusively on pain intensity scoring to do so. It is now relevant, in a patient-partner era, to put a well-informed patient at the centre of his or her therapy decision and adjust analgesic treatment at the patient’s request, regardless of pain scoring.
The main objective of the present study was to validate whether answers to the question: Do you want more pain medication? are sufficient to evaluate patients’ pain relief. To achieve this, we compared the patients’ answers to the question: Do you want more pain medication? with the answers from two other pain relief questions and to the pain intensity difference measurement. As a secondary objective, we have documented the reasons for refusing additional pain medication among non-relieved patients.
METHODS
Study design, setting, and population
We have performed a prospective cohort study in the ED of a tertiary care academic hospital with an approximate annual census of 65,000 (primarily adult) visits. The study population was constructed from a convenience sample of patients ages 16 years and over presenting to the ED from February 2013 to August 2014 and who met the following three criteria: 1) suffered from an acute pain problem with a pain intensity score of 4 or more; 2) received at least one dose of analgesics (opioids and/or non-opioids); and 3) were kept for observation for a minimum of 90 minutes. Patients were identified and recruited during weekdays by two research assistants alerted by the ED computerized information system or by the ED medical staff prior to the patients’ first dose of analgesic administration. Patients who died before pain assessment, pregnant women, and patients suffering from chronic pain were all excluded. For the purpose of this study, chronic pain was defined as pain lasting at least 3 months. This study received approval from our institution’s ethics review board. Patients who met all eligibility criteria were given an explanation of the research protocol and gave their informed consent (or parents in the case of minors). This study did not interfere with the ED usual pain management protocol, and all treatments were left to the discretion of the attending physician. Thus, we did not administer any pain medication, and the patients were monitored by the ED nurses with regards to normal pain follow-ups. The analgesic treatments were completely under the control of the ED physicians with regards to type, route, dose, and time of administration.
Outcome measures
Research assistants documented the following information from the patients’ files: age, gender, pain intensity at triage (recorded by the ED nurse during triage), as well as type, route, dose, and time of analgesic administration. The research assistants asked the patients to score their pain intensity immediately before the first analgesic administration (initial pain intensity assessment), as well as approximately 90 minutes after the initial analgesic administration (final pain intensity assessment). The 90-minute delay was chosen to allow time for the medication to reach its therapeutic window, while also having sufficient time between the last pain medication treatment and the start of the questionnaire. At each of the two pain assessments, the patients were instructed to report their pain on a verbal 11-point NRS ranging from 0 to 10, with the indications that a score of 0 represents “no pain at all,” whereas a score of 10 denotes “the worst pain imaginable.” On the last assessment, the patients were also asked to complete a short pain relief questionnaire to evaluate their level of pain relief. This questionnaire (developed in consensus by JMC, JP, GL, CM, and RD) contained three questionsReference Chauny, Paquet and Lavigne 16 : 1) Overall, which of the following choices better corresponds to your actual pain relief? – I am relieved; I am not relieved, 2) How would you rate your pain relief from the following choices? – not relieved; a little relieved; moderately relieved; very relieved; completely relieved,Reference Farrar, Polomano and Berlin 17 , Reference Jensen, Chen and Brugger 18 and 3) Do you want other medication to treat your pain right now? – yes or no. The order of presentation of the questions was partially counterbalanced to control for a potential order effect (three versions of the questionnaire were used; each question appearing first, second, and third for the same number of times). Patients who refused supplemental pain medication were also queried about the reasons for this refusal using a prepared checklist where multiple answers were possible. Free form text was also an option, and these answers were later classified by the authors by unanimous decision. The percentage decrease of pain intensity level is reported for the entire population as well as for different patient subpopulations. It was calculated as: (initial pain intensity – final pain intensity) ÷ initial pain intensity × 100.
Data analysis and statistics
Percentages and means with standard deviation (SD) are presented for categorical and continuous variables, respectively. To evaluate the concordance between the questions: Do you want more pain medication? and Are you relieved?, the percentage of agreement and the Cohen’s Kappa were performed. Independent t-tests were used to compare the percentage of pain decrease between groups of patients from the questions: Are you relieved? and Do you want more pain medication? All analyses were conducted with SPSS version 23 (IBM, Somers, NY).
RESULTS
A total of 392 patients who met the inclusion criteria were recruited. Fourteen (3.6%) were later excluded because of missing information on either the question: Are you relieved? or the question: Do you want more pain medication? The final cohort was thus composed of 378 acute pain emergency patients. Table 1 contains the characteristics of the included patients: 60% were women, with a mean age of 50.3 years, and an average initial pain score of 7.3 out of 10. Percentage of pain relief from initial to final pain intensity was 36% for all patients. The most common type of medication received by the patients was opioids (72%; choice of agent: morphine 48%, oxycodone 23%, fentanyl 15%, hydromorphone 14%; route of administration: injection 55%, oral 39%, subcutaneous 5%). The majority of subjects (81%) received only one dose of analgesic between initial and final pain intensity measurements, and 63% of all patients were discharged home.
Table 1 Characteristics of the 378 included patients

NRS=numerical rating scale; NSAID=nonsteroidal anti-inflammatory drug; SD=standard deviation.
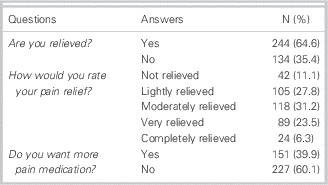
Results of the pain relief questionnaires are presented in Table 2. Almost two-thirds of the patients said that, overall, they were relieved from pain, 61% rated their pain relief as at least moderate to complete, and 60% did not want more pain medication.
Table 2 Results on pain relief questionnaires
To assess the discriminative power of pain relief of the questions: Are you relieved? and Do you want other medication?, we compared the percentage of pain intensity decrease for both questions (Table 3). The difference in the percentage of pain relief between the yes and no answers was significant for both questions (p<0.001), but tended to be higher for the question: Are you relieved? (42%) than for the question: Do you want other medication? (30%).
Table 3 Mean percentage of pain relief for the questions: Are you relieved? and Do you want more pain medication?
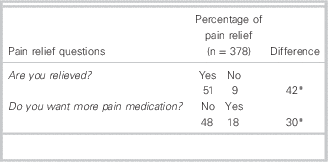
*p<0.001 from t-tests analyses
Table 4 shows the association between the two dichotomous pain relief questions. Interestingly, 68 (28%) of the relieved patients asked for supplemental analgesics, whereas 51 (38%) patients who were not relieved refused to receive further medication. The percentage agreement between the two relief questions is 69%, and the Cohen’s Kappa is 0.33 (95% confidence interval [CI]: 0.23–0.43), which is considered poor agreement.Reference Fleiss 19 Similar results were obtained when we compared the answers from the five-category evaluation: How would you rate your pain relief? to the dichotomous question: Do you want other medication? This analysis demonstrated that 24% of relieved patients (moderately to completely relieved) wanted more analgesics, whereas 35% of unrelieved patients (lightly relieved to not relieved) did not want further pain medication. In this case, the percentage of agreement between the two questions is 71%, and the Cohen’s Kappa is 0.40 (95% CI: 0.31 – 0.49).
Table 4 Association between the questions: Are you relieved? and the Do you want more pain medication? and the number of patients, initial pain intensity, final pain intensity, and percentage of pain relief for each group
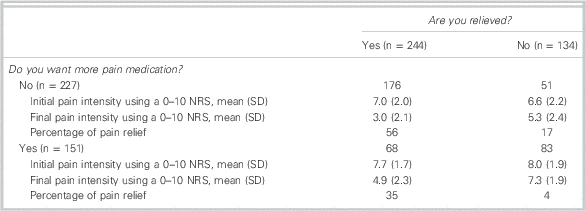
Table 5 presents the justification for refusing supplemental pain medication among the patients who were still in pain (the data were available for 47 patients out of 51). The patients could give multiple answers. The most common reason to refuse more pain medication was to avoid side effects (83%).
Table 5 Justification for refusing medication in patients who were not relieved

* A patient could give multiple reasons for refusal.
DISCUSSION
Approximately 90 minutes after receiving pain medication treatment for an ED acute pain complaint, 65% of the patients responded that they were relieved from pain, and 60% responded that they did not want other medication to relieve their pain. Such similar percentage could indicate that these two questions evaluated pain relief in the same way. However, when patients are classified according to the association between the two dichotomous pain relief questions (Are you relieved? and Do you want other medication?), the agreement among them was poor (Kappa<0.40), suggesting that the two questions did not evaluate the same thing.
We found that a significant proportion of patients (28%) who were adequately relieved from pain asked for more analgesics. We can hypothesize that these patients were not sufficiently relieved from pain, were fearful about their pain coming back, or even experienced a pleasant effect from the drug. However, future studies questioning the patient’s reasons to ask for more pain medication when relieved from pain are required to confirm these hypotheses.
An even bigger proportion of patients who were not relieved from pain refused a supplemental drug (38%). These patients, who were still in pain, had numerous and legitimate reasons (to avoid side effects, felt sufficiently relieved, disliked taking medication or its effects, too short of a delay since last dose, waiting for diagnosis, imminent departure, and fear of addiction) to refuse further pain treatment. Furthermore, the final level of pain intensity in this group of patients was rather high (5.3), accentuating even more the value and the true nature of their personal reason for refusing supplemental pain treatment. Overall, for 31% (119 out of 378) of the patients in our sample, the response to the question: Do you want more medication? was not a reliable indicator of pain relief. Furthermore, ED physicians have to be conscious that almost 40% of unrelieved patients will refuse pain medication treatment when asked about receiving further analgesics.
It is important to note that the patients who were relieved and still wanted more medication had an average decrease of 35% in their NRS pain level. This percentage of pain intensity difference is superior to the 30% decrease benchmark associated with a moderate pain relief, according to the 2008 consensus statement on pain outcome in clinical trials.Reference Dworkin, Turk and Wyrwich 12 However, their final pain level was still quite elevated at 4.9, justifying their desire for more analgesics. This result tends to favor the hypothesis that these patients were not sufficiently relieved from pain. In contrast, the group of patients who were not relieved and refused supplemental medication had experienced only a 20% decrease in their pain level (which is below the 30% decrease threshold for moderate pain relief), and their final pain intensity score was even higher at 5.3. Those results confirm that these patients were not relieved from their pain.
Pain intensity scoring may measure the wrong thing or may not even help improve patient outcome,Reference Green and Krauss 20 but, similarly, associating pain relief with patient refusing analgesics is inadequate. In our report, this assumption would have been inaccurate at least 22% of the time, based on the other two questions that we used to determine pain relief (51 unrelieved patients out of 227 refusing supplemental pain medication). In a recent study, Chang et al. found that 51% of their patients who declined analgesics were still in pain according to their NRS pain score of 5 or greater.Reference Chang, Bijur and Holden 14 , Reference Green and Krauss 20 In our case, 35% of the patients who refused further analgesics had a pain score of 5 or more. Claiming that patients who refuse further analgesics are relieved from pain is an oversimplification. In addition, it is known that patient satisfaction is related not only to pain relief, but also closely linked to the amount of physician attention received during the hospital stay.Reference Kelly 21 , Reference Toma, Triner and McNutt 22 We thus propose that any single query is insufficient to properly assess such a complex phenomenon as pain relief. As usual, the physician’s judgment should prevail, but it ultimately remains the patient’s decision to balance the benefits of pain control versus the potential side effects. It is now well accepted that, in general, the patients should decide for themselves whether they require more pain medication.
One of the main limitations of this study was the use of a convenience patient sample. Our cohort could have a representativeness bias because the recruitment was not conducted on weekends or on a 24-hour basis where more severe cases may happen. Also, pain location and diagnosis were not controlled during the study. However, we aimed for a pragmatic approach with a diversity of patients with acute pain problems typical of an ED’s daily reality. The monocentric nature of this study may also have impacted the results. Another limitation is the possibility that repeated treatments/pain measurements by the ED physician and ED nurse and the noninterventional nature of our study may have influenced the patients’ behaviour during the questionnaire. To complement our pragmatic approach, we believe that to obtain more precise information, future research should look at analgesic refusal in a more controlled setting with fixed times and clearly defined medications. Studies are also required to determine whether the efficacy of the initial treatment may have influenced the patient refusal for supplemental analgesics with additional questions after refusal, such as: Would you have accepted more treatment if the first one would have been more effective?
CONCLUSIONS
In this prospective cohort study of ED patients with acute pain, we found that over a third of patients not relieved from their pain after a first administration of analgesics refused further pain medication. Our study documented numerous legitimate reasons as to why patients would refuse supplemental analgesics. We suggest that the refusal of pain medication alone cannot be used as an indication of pain intensity relief in a clinical setting. However, given the complexity of the pain experience, pain control may involve more than medication-driven pain intensity relief.
CLINICAL IMPLICATIONS
As a result of this new information that patients refusing supplemental pain medication are not necessarily relieved from pain, we feel that an ED physician should not assume that patients are relieved from pain based on a single query nor on simple pain scoring. Multiple approaches and questions must be used to determine the actual state of the patient. ED physicians should inform the patients on the pros and cons of analgesics and, if appropriate, let them decide whether they want further pain treatment.
Acknowledgements: The authors thank the following individuals for their much appreciated efforts: Dominique Petit, PhD, for editing and reviewing the manuscript, and Chantal Lanthier for data collection and study management.
Competing interests: None declared.







