The specific needs of younger people with dementia have tended to be neglected by service providers, only 12 NHS trusts have specialist services (Reference WilliamsWilliams, 1995; Reference BarberBarber 1997; NHS Health Advisory Service, 1997). In 1995 Leeds Community and Mental Health Services NHS Trust, with the City of Leeds Department of Social Services, developed a multi-disciplinary community oriented early onset dementia team. This consists of one whole-time equivalent (w.t.e.) community psychiatric nurse, 0.5 w.t.e. social worker, 0.2 w.t.e. consultant psychiatrist and 0.2 w.t.e. clinical psychologist. There are close links between this team and a day centre specifically for people with early onset dementia, which is run by the Alzheimer's Society.
To help inform future service development a health needs assessment was undertaken in 1997 in order to:
-
(a) compare the prevalence and incidence of early onset dementia in Leeds with the available literature
-
(b) identify the needs of people with early onset dementia and their carers
-
(c) examine existing services and their access by people with early onset dementia and their carers
-
(d) identify gaps and make recommendations to improve the provision of services.
The study
The study consisted of the identification of cases of early onset dementia from health and social care records. In the absence of a central register a comprehensive survey was undertaken of the individuals and organisations likely to be involved in the provision of health and social services. This included consultant psychiatrists (general, old age, liaison, forensic and learning disabilities), neurologists and psychologists in the two Leeds NHS trusts and four neighbouring trusts. In addition, cases were collected from community mental health teams, district nurses, social services, the regional genetic service and local branches of the Alzheimer's, Parkinson's and Huntington's disease societies. Information was also sought from the computerised database by the Leeds Department of Social Services. All potential cases were then investigated by follow-up of health and social care records.
The three entry criteria for cases were:
-
(a) a clinical diagnosis of dementia, made by a consultant psychiatrist or consultant neurologist (for the purpose of the study the diagnosis was taken as the current medical diagnosis according to ICD-10 status (World Health Organization, 1992) recorded in the case notes)
-
(b) being aged under 65
-
(c) residing within Leeds.
Data were collected for the period from 1 June 1994 to 1 December 1997. Those who had died or were no longer residents of Leeds were excluded from the analysis.
The study also consisted of a postal survey of carers and semi-structured interviews with patients, carers and professionals from health and social services and the voluntary sector.
Findings
Epidemiology
One-hundred and thirty-two people were identified as having dementia and aged under 65 years on 1 December 1997. Almost half were aged between 60 and 64 years, 11 cases (8%) were under the age of 45 years and 20 (15%) had a coexisting learning disability. The prevalence rate for early onset dementia in Leeds was 42 per 100 000 aged 30 to 64 years and 78 per 100 000 aged 45 to 64 years. This is based on the 1996 mid-year population of Leeds of just under 320 000 aged 30-64 years. Twenty-nine new cases were identified in the 12 months up to May 1997 and 23 new cases were identified in the previous year. The most frequent cause of dementia was Alzheimer's disease (Table 1). Of the 112 without learning disabilities, 83% lived in their own homes. The majority were being cared for by partners (60%) or their children (14%). Of the 20 who had learning disabilities and dementia, the majority lived in nursing homes or supported group homes.
Table 1. Diagnosis of early onset dementia in Leeds
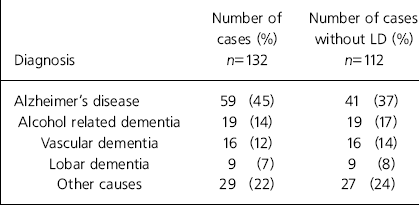
| Diagnosis | Number of cases (%) n=132 | Number of cases without LD (%) n=112 |
|---|---|---|
| Alzheimer's disease | 59 (45) | 41 (37) |
| Alcohol related dementia | 19 (14) | 19 (17) |
| Vascular dementia | 16 (12) | 16 (14) |
| Lobar dementia | 9 (7) | 9 (8) |
| Other causes | 29 (22) | 27 (24) |
There was an uneven geographical distribution of cases, with a concentration in the South and West of the city. There were no obvious explanations for this phenomenon; there was, for example, no link between this geographical distribution and residential placements, age, diagnoses or indices of social deprivation.
The onset of dementia: before diagnosis
The median age of onset for symptoms was 55 years (range 25 to 64 years). Nearly 60% of the main sample (67/112) sought medical help within 12 months of the onset of symptoms. Just under 20% waited for between 1 and 2 years before seeking help and 10% contacted their general practitioner (GP) only after 2-3 years. For most, the forgetfulness, problems with reading and writing, aggression, instability and sleep disturbance were often regarded as temporary exacerbations of character, depression or reactions to stress either at home or work. Most sufferers or their relatives only contacted their GP after a significant event in their lives.
Referral and diagnosis
Four main clinical gateways of referral for specialist investigation were found:
-
(a) to general psychiatry (41/112; 37%)
-
(b) to neurology (31/112; 28%)
-
(c) to psychiatry of old age (12/112; 11%)
-
(d) to liaison psychiatry (12/112; 11%).
From pillar to post
During the period following initial referral many carers and sufferers found themselves to be ‘passed from pillar to post’, between and within psychiatry and neurology. Thirty-eight different pathways of care were identified. Most sufferers had been referred to at least two different consultants and a significant minority had been referred to as many as five different consultants. Very few people were referred directly to the early onset dementia team.
A summary of referral pathways is shown in Table 2. The true picture is much more complex, for example, of the six patients (underlined in Table 2) who were referred onto a second general psychiatrist (general psychiatry B) after initially seeing a general psychiatrist and then a neurologist, four were referred onto and remained patients of the early onset dementia service and two were referred back to the first general psychiatrist (not shown).
Table 2. Referral pathways to care
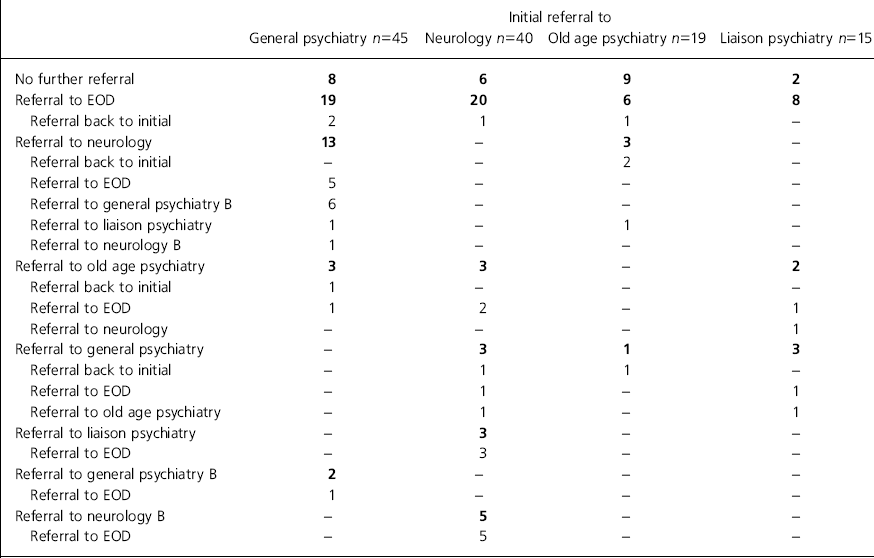
| Initial referral to | ||||
|---|---|---|---|---|
| General psychiatry n=45 | Neurology n=40 | Old age psychiatry n=19 | Liaison psychiatry n=15 | |
| No further referral | 8 | 6 | 9 | 2 |
| Referral to EOD | 19 | 20 | 6 | 8 |
| Referral back to initial | 2 | 1 | 1 | - |
| Referral to neurology | 13 | - | 3 | - |
| Referral back to initial | - | - | 2 | - |
| Referral to EOD | 5 | - | - | - |
| Referral to general psychiatry B | 6 | - | - | - |
| Referral to liaison psychiatry | 1 | - | 1 | - |
| Referral to neurology B | 1 | - | - | - |
| Referral to old age psychiatry | 3 | 3 | - | 2 |
| Referral back to initial | 1 | - | - | - |
| Referral to EOD | 1 | 2 | - | 1 |
| Referral to neurology | - | - | - | 1 |
| Referral to general psychiatry | - | 3 | 1 | 3 |
| Referral back to initial | - | 1 | 1 | - |
| Referral to EOD | - | 1 | - | 1 |
| Referral to old age psychiatry | - | 1 | - | 1 |
| Referral to liaison psychiatry | - | 3 | - | - |
| Referral to EOD | - | 3 | - | - |
| Referral to general psychiatry B | 2 | - | - | - |
| Referral to EOD | 1 | - | - | - |
| Referral to neurology B | - | 5 | - | - |
| Referral to EOD | - | 5 | - | - |
Carers complained about being passed from consultant to consultant. They had not received enough information, practical help, support or counselling. The burden of responsibility for finding out about available help was left with the carers and their families.
Service provision
Almost all of the patients (92%; 103/112) were under the care of a psychiatrist and most were currently with the consultant with a special interest in early onset dementia (78%; 87/112).
Nearly 40% (45/112) of patients had been referred to day care and almost all had been referred to the Alzheimer's Society's day centre for people with early onset dementia. There was evidence that those attending the day centre tended to present with relatively less severe behavioural problems and required relatively less help with activities of daily living than non-attenders who lived at home. Carers who returned the postal questionnaire (response rate 64%; 61/95) indicated that the attenders were less likely to suffer incontinence or display sexual disinhibition, or to be violent regularly or to need help eating meals than non-attenders with early onset dementia who were, also, living at home.
Carers frequently mentioned that their greatest need was a break from caring, and their highest service priority was appropriate respite care. Residential respite care had been provided for 14% of sufferers in a variety of settings - hospital wards for the elderly, general adult psychiatry wards and private sector residential and nursing homes. While such residential respite care was appreciated, there were criticisms of the care being located in inappropriate environments for younger people with dementia. Carers also commented on the difficulties they experienced in finding appropriate homes for permanent care.
Caring and coping with early onset dementia
Patients who were able to take part in the study described their distress at losing their abilities to read, write, converse and take part in everyday life. Just over two-thirds of carers regarded themselves as full-time carers; half were male. A range of behavioural and social problems were reported to be of concern to carers. Two-thirds of carers reported that their emotional well-being was poor or very poor. The longer the length of caring, the worse their emotional well-being. When carers responding to the questionnaire were divided into those that had been caring for less than 3 years (n=16), between 3 and 5 years (n=18) and greater than 5 years (n=15), there was a statistically significant difference between the groups in emotional well-being (analysis of variance, f=6, P<0.01). Post hoc tests (Tukey-HSD) revealed that this difference was accounted for by the fact that the group of carers who had been caring for less than 3 years expressed better emotional well-being than the other two groups.
Discussion
Epidemiology
The findings of this study can be compared with similar case finding research undertaken by Harvey (Reference Harvey1998) and funded by the NHS Executive in two London local authority boroughs, one inner-city and one suburban, with a total population of 193 000 aged 30-64 years.
Table 3 shows the prevalence rates found by Harvey. It should be noted that Harvey included people with learning disabilities within the ‘other’ category and the Leeds figures have been adjusted accordingly for this table.
Table 3. Estimated numbers of early onset dementia, 45-64-year-olds, in Leeds based on Harvey (Reference Harvey1998)
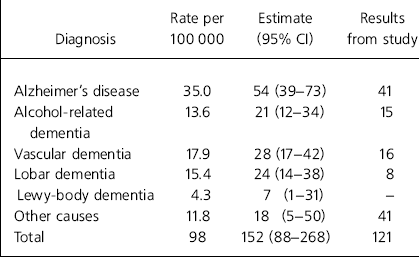
| Diagnosis | Rate per 100 000 | Estimate (95% Cl) | Results from study |
|---|---|---|---|
| Alzheimer's disease | 35.0 | 54 (39-73) | 41 |
| Alcohol-related dementia | 13.6 | 21 (12-34) | 15 |
| Vascular dementia | 17.9 | 28 (17-42) | 16 |
| Lobar dementia | 15.4 | 24 (14-38) | 8 |
| Lewy-body dementia | 4.3 | 7 (1-31) | - |
| Other causes | 11.8 | 18 (5-50) | 41 |
| Total | 98 | 152 (88-268) | 121 |
The numbers (121) found in the Leeds study, aged 45-64 years, were lower than the 152 expected based on Harvey's work, but between the 95% CI (Table 3). The number of people with Alzheimer's disease (41) was at the lower end of the estimates based on Harvey's work, but the rate of 26.5 per 100 000 found in Leeds fell within the Harvey rate of 25-47 per 100 000. Reasons for this lower rate of case identification may include the early onset dementia team being only relatively recently established, coupled with a lack of dedicated continuing care residential services within Leeds, as well as the methodology adopted. The proportion of those found with Alzheimer's disease was 34% (41/121), matching the Harvey estimate of 26% (54/152) or when those with a learning disability are excluded, the proportion with Alzheimer's disease in the 45-64 year age group was 40% in both studies.
The Leeds study identified 20 people with learning disabilities and dementia; much higher than Harvey's work. Reasons for this difference include the presence of a mental handicap hospital in Leeds plus a perceived low level of identification by Harvey (Reference Harvey1998). In addition, the Leeds study, unlike the work of Harvey, was not built around a clinical assessment. Therefore, some of those in the ‘other’ category with a diagnosis of dementia unspecified - are likely to have Lewy body dementia, fronto-temporal dementia, or another specific cause of dementia.
Other epidemiological findings are supported by research elsewhere, namely that about 50% of sufferers were aged between 60 and 64 years, that females with Alzheimer's disease outnumbered males by 2:1 and that there was an uneven geographical distribution of cases (Reference McGonigal, Thomas and McquadeMcGonigal et al, 1993; Reference Whalley, Thomas and McGonigalWhalley et al, 1995; Reference FuhrmannFuhrmann, 1997).
The incidence rate of 23-29 new cases per year is comparable to previous findings, which found an incidence rate of 3.4-7.2 per 100 000 for Alzheimer's dementia (Reference Newens, Forster and KayNewens et al, 1993).
Referral and diagnosis
Once people contacted their GPs they were referred quickly to a consultant psychiatrist or neurologist. This study found, like others undertaken, that there were four main gateways to care (Alzheimer's Disease Society, 1996; Reference FuhrmannFuhrmann, 1997). The establishment and further development of a specialist early onset dementia service offers the opportunity to provide a single gateway through which sufferers and carers can access information, advice, expertise and appropriate care. A multidisciplinary diagnostic service can reduce the length of time from first referral to diagnosis and aftercare.
From pillar to post
In most parts of the country the route to specialist services for younger people with dementia is uncoordinated, with no clear delineation of clinical responsibility and recent research in Brighton found 11 different referral pathways (Reference FuhrmannFuhrmann, 1997). Does the ‘pillar to post’ phenomenon result because of the difficulties in diagnosing or managing these patients, lack of adequate resources or the unwillingness of generalists to take responsibility for this group of people?
Service provision
High levels of satisfaction were expressed by carers in relation to the services provided by the Alzheimer's Society and the specialist early onset dementia team. Carers valued day care very highly, as elsewhere (Alzheimer's Disease Society, 1996). However, as in other studies, carers reported difficulties in accessing appropriate respite, acute and longer-term care for their loved-ones. The provision of dedicated respite care services and designated NHS beds could provide appropriate levels of service for some younger people with dementia and their families.
There is now a lot of practical experience and an adequate evidence base that demonstrates the need for specialist service provision for younger people with dementia. This can then streamline the diagnostic process, build up expertise, clarify clinical responsibility, provide continuity of care and coordinate the delivery of services with other agencies.






eLetters
No eLetters have been published for this article.