Older adults comprise the fastest-growing population group, with WHO projecting a total of 1·2 billion people over the age of 60 years by 2025(1). In 2001, there were approximately 1 million adults aged ≥85 years in England and Wales, with this number projected to increase to 2·5 million (or 4 % of the total population) by 2031(Reference Bray2). In these countries there has been a 14-fold and 23-fold increase in the number of male and female centenarians, respectively, over the past 50 years of the 20th century(Reference Dini and Goldring3). This substantial increase in the number of older adults has important implications for individuals, families and health- and social-care systems, as there is the potential for many people to live a greater number of years in poor health.
Older adults are at greatest risk for lifestyle-related diseases, including type 2 diabetes, CHD, stroke, hypertension and certain cancers. In the UK, 41 % of men and 38 % of women aged 60–74 years suffer from a chronic illness that limits daily activities; this increases to 58 % of men and 62 % of women over the age of 75 years(4). Interventions incorporating healthy eating and regular physical activity are known to be effective in reducing the risks of several chronic diseases(Reference Booth, Chakravarthy and Gordon5, Reference Roberts and Barnard6), emphasising the significant contribution of these lifestyle factors towards maintaining good health throughout an individual's life span.
Malnutrition is estimated to affect >10 % of older adults in the UK(7). Data from the Health Survey for England indicate that 0·9 % of adults aged 65–74 years and 1·6 % of those aged ≥75 years are underweight. Conversely, 76·2 % and 68·9 % of adults in these respective age groups are considered overweight or obese(8). Limited access to affordable healthy foods, difficulties in acquiring, preparing and consuming healthy meals, existing illness, medication use, age-related physiological changes, low levels of physical activity and financial difficulties are important contributors to undernourishment, overweight and obesity in older adults(Reference Brownie9). Currently, there is little published research on the food shopping habits of older adults in the UK and how these habits may be associated with the quality of dietary intake, levels of overweight and physical activity, and overall health.
The ability to care for oneself and remain independent is extremely important to older people(Reference McKie10), with many reporting a strong desire to stay in their own home for as long as possible(Reference Rioux11). Food shopping is not only a necessary activity of daily living but it also contributes to one's sense of independence and can become increasingly difficult for older people as they experience declines in health, mobility and the ability to drive a car. Carrying groceries, limited options for transport and financial constraints all contribute to the challenges experienced by older people when purchasing food(Reference Herne12). Research conducted in North America has shown that food shopping is restricted to the immediate neighbourhood of older adults and proximity to food shops contributes to their well-being(Reference Smith13, Reference Smith and Gauthier14). However, in the UK, an increasing number of local food shops are closing and larger supermarkets located outside local neighbourhoods are appearing more frequently. It is unclear how this change may affect the ability of older adults to purchase healthy foods and maintain adequate nutritional intake, good health and independence.
The primary aims of the present paper are to: (i) describe the food shopping habits of a sample of older adults (aged ≥70 years) living in the UK; and (ii) explore potential associations between food shopping habits and selected health-related indicators, including objectively measured physical activity levels, BMI, physical function and self-reported health status and dietary intake.
Experimental methods
Study design
The present study is part of the Older People and Active Living (OPAL) project, a community-based descriptive observational study that aimed to provide data on physical activity patterns and their determinants among independent older adults living in Bristol, UK. Ethical approval was granted by the Bristol Southmead NHS Research Ethics Committee (Reference no. 06/Q2002/127).
Sampling and recruitment
Complete details of sampling, recruitment and inclusion or exclusion criteria have been published previously(Reference Davis, Fox and Hillsdon15). The aim was to provide a sample that was broadly representative of the city of Bristol in relation to socio-economic position and access to amenities. To achieve this, twelve general medical practices within the city were selected to represent areas of low, medium and high deprivation, as defined by the Index of Multiple Deprivation (IMD) score for each practice(Reference Noble, Wright and Dibben16), and low or high proximity to the nearest store. A total of 1328 individuals aged ≥70 years at the time of recruitment were randomly selected from the twelve practice patient lists, and 1170 individuals who qualified for the study were mailed an invitation, an information pamphlet and a consent form. Response rate to the invitation was 54·6 % (725 of 1170), with 240 participants (47·9 % female) providing written informed consent and completing the study. Sample size was based on detecting a significant difference in the physical activity levels of participants in the three tertiles of IMD(Reference Davis, Fox and Hillsdon15). The results reported in the present paper represent secondary analyses from a study that was primarily designed to detect differences in physical activity; thus, no formal power calculations were carried out to detect differences in food shopping among IMD tertiles. These secondary analyses on food shopping should therefore be considered exploratory.
Measures
Data were collected during 2007–2008 over two home visits (generally 8 d apart) for each participant. The Neighborhood and Quality of Life for Seniors Study Questionnaire(Reference Shigematsu, Sallis and Conway17) included many items such as demographics (age, gender, income, marital status, education, current disease treatment and car ownership) and ‘neighbourhood food environment’ (availability and ease of purchase of fresh fruit, vegetables and low-fat foods). As this questionnaire was developed in the USA, questions were modified, as necessary, for UK delivery. Questions about the perceived distance to the nearest facilities (categorised walking time, min) were originally sourced from the 2002 version of the Neighbourhood Environment Walkability Scale(Reference Saelens, Sallis and Black18), with questions added on the frequency of facility use and normal mode of transport to give richer contextual information.
Household food security, defined as access to enough food by all members at all times for an active, healthy life, was assessed using the US Household Food Security Hunger Survey Module(19). The 12-Item Short-Form Health Survey was used to measure perceptions of general health and functional health status(Reference Ware, Kosinski and Keller20). Dietary intake was measured using the Dietary Assessment for Nutrition Education tool, which has been validated in UK adults and gives a score for low, medium and high dietary intakes of fibre, total fat and unsaturated fat(Reference Roe, Strong and Whiteside21). The low-fat category represents a fat intake of ≤83 g/d, corresponding to 35 % of the energy RDA for an average woman. The high-fat category represents a fat intake >122 g/d, corresponding to 40 % of the energy RDA for an average man. The low-fibre category corresponds to a fibre intake of ≤20 g/d and the high-fibre category corresponds to >30 g/d. The unsaturated fat score is categorised empirically into low, medium and high levels of unsaturated fat contributed by the added fat used for spreads and cooking in the diet. Responses to questions were elicited using large-font prompt cards and recorded by interviewers.
Physical activity (steps/d) was assessed using accelerometry and described previously(Reference Davis, Fox and Hillsdon15). Briefly, participants wore an Actigraph GT1M monitor (Pensacola, FL, USA) on a belt for 7 d and kept a log of daily journeys, including frequency, mode of transport and purpose. GT1M monitors were programmed to record activity in 10 s epochs, producing both activity count and step count data. Physical function was assessed using the Short Physical Performance Battery (SPPB)(Reference Guralnik, Simonsick and Ferrucci22), which measures lower-extremity function in older adults. Height and weight were measured once using a Seca Leicester stadiometer and Seca portable scale, respectively (Northampton, UK); BMI (kg/m2) was calculated from measured height and weight.
Statistical analyses
All statistical analyses were performed using the Statistical Package for the Social Sciences statistical software package version 16·0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics (means, sd, frequencies and proportions) were generated for all variables. Group comparisons were made using independent t tests for continuous data, χ 2 tests for categorical data and Mann–Whitney U tests for ordinal data. Spearman's correlations (ρ) were used to assess the relationships between variables. Significance was set at P < 0·05.
Results
The majority of the 240 participants were white (n 230; 95·8 %), with two (0·8 %), four (1·7 %) and two (0·8 %) reporting race as Black/Afro-Caribbean, Asian and other, respectively. Table 1 includes selected demographic characteristics. Mean age was 78·1 (sd 5·7) years, with 11·7 % of participants aged ≥85 years. Approximately 67 % of OPAL participants were overweight or obese; this compares with 76·2 % of adults aged 65–74 years and 68·9 % of adults aged ≥75 years being overweight or obese nationally(23). Almost 4 % of OPAL participants were underweight. This is slightly higher than the prevalence of 0·9–1·5 % reported in the Health Survey for England(23) for adults aged 65–74 years and ≥75 years, respectively.
Table 1 Demographics of 240 older adults aged ≥70 years living in Bristol, UK
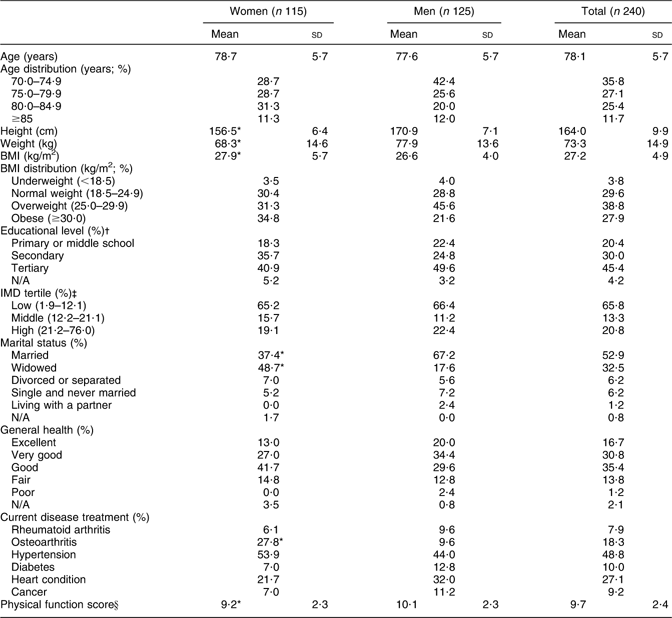
IMD, Index of Multiple Deprivation; N/A, data not available.
*Significant difference between genders.
†Highest level of education achieved. Primary or middle-level education includes those who underwent some amount of schooling, but did not complete secondary school. Tertiary-level education includes college and university education.
‡Scores derived from participants’ postcodes (a high score indicates a high level of deprivation).
§The highest possible score achievable is 12.
The IMD scores for participants’ residence were reasonably representative of the IMD distribution in England, with 22·1 %, 27·9 %, 31·3 % and 18·7 % of the OPAL sample falling into the lowest to highest national quartiles, respectively(Reference Fox, Hillsdon and Sharp24). Almost all participants reported being food secure, with 91·7 % reporting having enough food to eat and 4·6 % reporting having enough food but not always the type of food they would like to eat.
Almost 83 % of OPAL participants self-reported their health as good, very good or excellent. The most commonly reported disease was hypertension (48·8 %), which is less than its overall prevalence in the UK; 52·1 % and 68·4 % of adults aged 65–74 and ≥75 years, respectively, have hypertension(23). In addition, 21·7 % of OPAL women and 32·0 % of men reported having a heart condition; this is comparable to the prevalence of CHD among adults aged ≥75 years in the UK, with 19·3 % of women and 28·6 % of men having CHD(25). The proportion of OPAL participants with osteoarthritis was also similar to its national equivalent(26).
Physical function as measured by the SPPB was relatively high, with a mean score of 9·7 out of a possible 12 points; men had significantly higher physical function scores than women (P = 0·004). Detailed physical activity results are reported elsewhere(Reference Davis, Fox and Hillsdon15). In summary, men were significantly more active than women with a mean of 4714·0 (sd 227·2) v. 4182·9 (sd 233·5) steps/d, although almost none met the current recommendations for physical activity.
Results related to food shopping habits are reported in Table 2. Most participants (80·0 %) conducted their food shopping by themselves or with someone else. Women were more likely than men to shop alone (50·4 % v. 28·8 %, P < 0·001), with men more likely than women to report shopping with their spouse (48·8 % v. 24·3 %, P < 0·001). The most commonly reported main food shopping venue was the nearest supermarket (33·3 %). The main food shopping venues frequented by 115 (86 %) of the 133 participants who reported the name of their main food shop included one of the four largest supermarket chains in the UK (Tesco, Asda, Sainsbury's and Morrisons) or an upmarket national chain (Waitrose).
Table 2 Food shopping habits of 240 older adults aged ≥70 years living in Bristol, UK

N/A, data not available.
*Significant difference between genders.
The perceived walking distance to the main food shopping venue was reported to be at least 31 min in 40·8 % of participants. Over half (53·3 %) reported a frequency of at least once weekly for their main food shopping, with 50·3 % driving to or being driven to their main food shopping venue. Men were more likely than women to drive to their food shopping venue (P < 0·001), with women more likely to be passengers (P < 0·001) or to take the bus (P < 0·001). This finding is consistent with the number of cars reported per household in the present study, with men reporting significantly more cars in their household than women (men: mean = 1·09 cars, range = 0–6; women: mean = 0·73 cars, range = 0–2; P < 0·001).
The majority of participants reported ‘infrequently or never’ using restaurants (78·7 %), fast-food outlets (82·5 %) or pubs (83·3 %), suggesting the predominance of food shopping to procure food. Bakeries were more frequently used, with 13·8 % going to a bakery at least once weekly and 12·5 % going at least once monthly; 60·4 % reported going to a bakery infrequently or never (data not shown).
Table 3 includes the findings related to the ease of purchasing and availability of fruit, vegetables and low-fat food products, and to intakes of fibre, fat and unsaturated fat. The majority of participants somewhat or strongly agreed that it was easy to purchase fresh fruit and vegetables, that they had access to a large selection of them and that they had access to fresh produce of high quality. However, 23·4 %, 31·3 % and 25·0 %, respectively, somewhat or strongly disagreed with these statements. Although more than half also somewhat or strongly agreed that it was easy to purchase low-fat foods and that there was a large selection of low-fat products available, 21·2 % and 26·3 %, respectively, somewhat or strongly disagreed with these statements. Almost 20 % of participants reported a low fibre intake, with 16·2 % reporting a high fat intake. The majority (91·7 %) reported a medium-to-high intake of unsaturated fat. Significantly more women than men reported a low fat intake (P = 0·015), with significantly more men than women reporting a medium fat intake (P = 0·015).
Table 3 Ease of purchasing and availability of fruit, vegetables and low-fat food products and intakes of fibre, fat and unsaturated fat in 240 older adults aged ≥70 years living in Bristol, UK
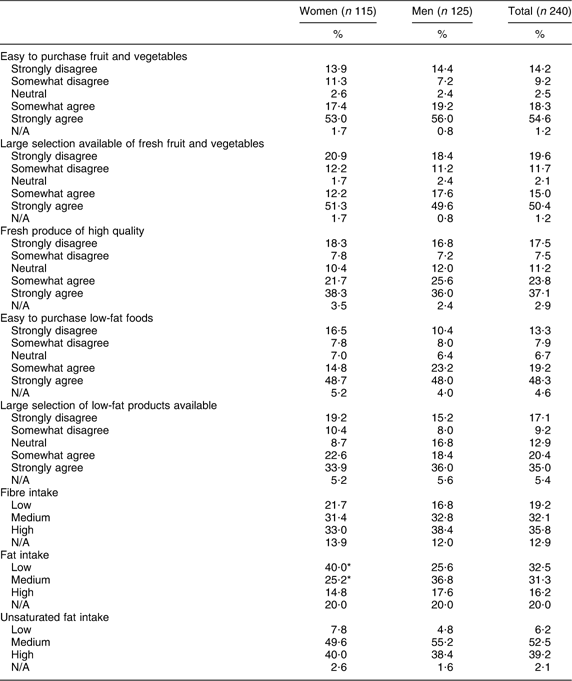
N/A, data not available.
*Significant difference between genders.
Table 4 shows Spearman's rank order correlations (ρ) between BMI, general health, physical function, physical activity levels (steps/d) and selected food shopping variables. There were weak but significant correlations between physical function, general health and physical activity (steps/d), indicating that higher physical function and better self-reported general health were associated with greater levels of physical activity. The ease of purchasing, extent of selection and quality of fresh fruit, vegetables and low-fat products were strongly inter-correlated and weakly but significantly correlated with higher physical function, higher physical activity and better self-reported general health. Participants who reported a stronger disagreement with the ease of purchasing, extent of selection and quality of fruit, vegetables and low-fat products were more likely to report walking a higher number of minutes to their main food shop. Higher levels of physical activity were associated with a higher frequency of use of the main food shopping venue, whereas walking for a higher number of minutes to the main food shop was associated with lower frequency of its use. Taking the bus, walking or cycling to the main food shop was associated with a greater frequency of use of the main food shop compared with using a car (ρ = −0·402, P < 0·001, n 169).
Table 4 Spearman's rank order correlations between BMI, general health, physical function, physical activity levels (steps/d) and food shopping habits among 240 older adults aged ≥70 years living in Bristol, UK
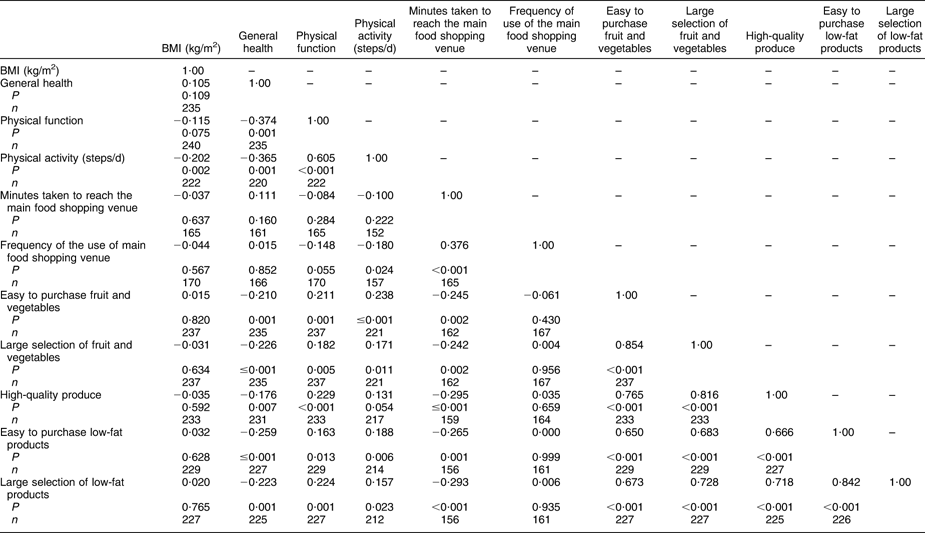
There were very few significant correlations between fibre, fat and unsaturated fat intakes and other shopping and health-related variables (data not shown). Fat intake was weakly correlated with BMI, indicating an association between higher fat intake and lower BMI (ρ = −0·180, P = 0·013, n 192). Fat intake was also weakly correlated with the frequency of use of the main food shopping venue (ρ = 0·185, P = 0·030, n 138), indicating that shopping more often was associated with higher fat intake. Having a spouse or family member shop with/for the participant was also associated with higher fat intake (ρ = −0·265, P < 0·001, n 227). Fibre intake was weakly correlated with IMD score (ρ = −0·162, P = 0·019, n 209), indicating an association between lower fibre intake and a higher level of deprivation. The IMD score was also correlated with the mode of transport to the main food shopping venue (ρ = 0·290, P < 0·001, n 170), indicating that those with a higher level of deprivation were less likely to drive or be driven to their main food shopping venue.
Discussion
The present study makes an important contribution to the limited published literature related to food shopping habits of older adults, particularly of the subgroup aged ≥70 years, and their relationship with selected health-related indicators. The sample included 240 participants from across the socio-economic and amenities-access spectrums in Bristol, UK. The sample is reasonably representative of older adults in the UK in relation to weight status and prevalence of common disease conditions.
Most OPAL participants reported food shopping by themselves or with another person, with men more likely to shop with their spouse and women more likely to shop alone. Supermarkets were the most common shops frequented, with the majority shopping at one of the ‘Big 4’ supermarket chains in the UK or at an upmarket national chain. In addition, the car was the predominant mode of transport to food shops, with men more likely to drive and women more likely to be driven. This pattern of food shopping is consistent with the current location of various food shops in the UK being further away from local neighbourhoods, and suggests a cultural norm towards conducting one large food shop per week. The use of the car is not surprising, as almost half of the participants reported their main food shopping venue to be located at a distance of at least a 30 min walk. Predominance of car use may indicate an ability to maintain independence to do their own shopping, and help older adults avoid the challenges inherent in carrying heavy loads of groceries that those who actively commute experience. Those OPAL participants who tended to actively commute (i.e. by taking the bus, walking or cycling) to their food shopping venue reported a greater frequency of use of their food shop. This probably reflects ease of access and the necessity to limit the weight of purchases to be carried home. Unfortunately it was not possible to link the perceived walking distance to the nearest food shop with the accelerometer data, and thus it is not clear how much food shopping per se may have contributed to daily physical activity levels in this sample.
Approximately 80 % of participants reported ‘infrequently or never’ using restaurants, fast-food outlets or pubs, suggesting that food shopping and cooking at home are critical factors to help older adults meet the needs of their dietary intake. Studies indicate that older adults in Scotland, Sweden and Australia prefer to consume ‘proper’ meals cooked at home on a regular schedule and many expressed a view that convenience foods are unhealthy and only a reasonable option for people with limitations in preparing and cooking food(Reference McKie, MacInnes and Hendry27–Reference Hunter and Worsley29).
Although over half of the participants reported that it was easy to purchase a large selection of fresh fruit, vegetables and low-fat foods of high quality, up to 25 % did not agree. Those who reported a stronger disagreement with the ease of purchasing, extent of selection and quality of fruit, vegetables and low-fat products were more likely to report walking for a higher number of minutes to their main food shop. Morland and Filomena(Reference Morland and Filomena30) found that for every mile travelled to their main food shop, older adults in the USA reported an increase of 0·03 servings of fruit and vegetables/d. These researchers concluded that fruit and vegetables were not locally available and thus those who travelled further were able to access and consume higher amounts of these foods. The OPAL study is cross-sectional; hence, it was not possible to determine causality between distance travelled to the main food shop and purchase and consumption of fruit, vegetables and low-fat products. It is plausible that those who travelled further to their main food shop did so because these food shops carried a larger amount and better quality of fruit, vegetables and low-fat products. Interestingly, in the present study, there were no associations between intake of fibre or fat and type of food shop frequented or the reported ease of purchasing a large selection of high-quality fresh fruit, vegetables and low-fat foods. There were significant associations between higher levels of deprivation, lower fibre intake and reduced use of a car to conduct food shopping. These findings suggest that those with limited resources are less likely to drive or be driven to their main food shopping venue and are less likely to choose higher-fibre foods such as fruit, vegetables and whole grains, possibly because of higher cost and/or challenges related to carrying these food items. The consumption of adequate fruit, vegetables and wholegrain foods is imperative to preventing malnutrition in older adults, as there is growing evidence that the low intakes of micronutrients found in these foods, such as vitamins C and E, carotenoids and folate, are significantly associated with increased risk of frailty in older adults(Reference Bartali, Frongillo and Bandinelli31–Reference Michelon, Blaum and Semba33).
It is of concern that almost 20 % of OPAL participants reported a low fibre intake, as fibre is critical to optimising bowel function and is known to reduce the risk of diverticulitis and perhaps of certain cancers(34). The high fat intake observed in approximately 16 % of participants is also of concern, and combined with the low levels of physical activity in this sample(Reference Davis, Fox and Hillsdon15) could be the contributing factor to the relatively high levels of overweight and obesity in this sample. A higher fat intake was weakly but significantly associated with food shopping more frequently, and with having a spouse or family member shop with or for the participant. Shopping more often could allow for an increased opportunity to buy favourite, higher-fat foods more often. This correlation may be a reflection of the fact that, in this sample, women reported lower fat intakes than men and were more likely to shop alone than with a spouse or family member. There was also a weak association between higher fat intake and lower BMI; this finding suggests an under-reporting of dietary fat in those who are overweight or obese, which has been reported in the literature(Reference Heitmann and Lissner35).
The strong inter-correlations between ease of purchasing, extent of selection and quality of fresh fruit, vegetables and low-fat foods suggest that the main food shopping venues, which tended to be large supermarket chains in the present study, provide a wide variety of high-quality healthy food products. Higher levels of physical function and physical activity and better self-reported general health were significantly but weakly correlated with these food shopping variables. Although these results may suggest that those who were more physically active and healthy were able to maintain their independence, which allowed them to frequent shops with higher food quality and availability, they should be viewed with caution as the relationship may be confounded by other factors such as the IMD score of the neighbourhood or socio-economic status. It is recognised, however, that maintaining independence is paramount in older adults, particularly in relation to food-related activities of daily living, as greater independence in food-related activities such as food shopping and meal preparation has been shown to be significantly associated with fewer health problems, greater physical strength and better food intake in older adults(Reference Keller36).
The present study has a number of limitations. Although the sample fairly represented the national IMD distribution, it was not fully representative of older adults living in the UK in relation to formal education and ethnicity. Participants were more educated than the average adult in this age range in the UK, approximately 20 % of whom have not completed secondary education. It is estimated that >50 % of 70–74-year-old adults in the UK have no formal qualification(37). In addition, this sample was not representative of the black and ethnic minority (BME) groups in Bristol or the UK, as only 3·3 % of our sample reported being from a BME community; the BME population of Bristol is estimated at 8·2 %(38), whereas that of the UK is 7·9 %(39). It is not surprising that we were unable to recruit more people from BME communities, as it has been recognised that using methods of recruitment found to be useful for recruiting white participants into research do not translate into successful recruitment of ethnic minority participants(Reference Areán and Gallagher-Thompson40, Reference Sheikh, Halami and Bhopal41). The strengths of the present study include the collection of a wide array of high-quality data related to food shopping and health-related indicators and the objective assessment of physical activity, physical function and BMI in a relatively large sample of community-dwelling older adults aged ≥70 years.
To conclude, the present study contributes information about food shopping habits and their associations with select health-related indicators among adults ≥70 years of age living in the UK. Results indicate that, in this independent and free-living sample, most shop by themselves or with someone else at large supermarket chains at least once weekly, and the primary mode of transport to food shopping is by car. Although most participants agreed that it was easy to purchase a wide selection of quality fruit, vegetables and low-fat products, a subsample reported low fibre and high fat intakes that were of concern. These results further substantiate the importance of promoting a high-quality diet and regular physical activity in maintaining independence and optimising health in older adults.
Acknowledgements
The present study was supported by the National Prevention Research Initiative (Grant no. G0501312; http://www.npri.org.uk) whose funding partners are the British Heart Foundation; Cancer Research UK; Department of Health; Diabetes UK; Economic and Social Research Council; Medical Research Council; Research and Development Office for the Northern Ireland Health and Social Services; Chief Scientist Office, Scottish Executive Health Department; Welsh Assembly Government; and World Cancer Research Fund. The authors have no conflict of interest to declare. All drafts of the paper were prepared by J.L.T. with inputs from all co-authors. Statistical analyses were executed by J.L.T. All authors have reviewed and approved the final version. The authors thank the participants and general medical practices for giving their time and energy to the study. The authors also acknowledge all the investigators and Project OPAL team members not listed as co-authors.






