Multiple sclerosis (MS) is an immune-mediated disorder of the central nervous system resulting in progressive, and often unpredictable, sensory, physical, and cognitive impairments (Sadovnick, Ebers, Wilson, & Paty, Reference Sadovnick, Ebers, Wilson and Paty1992). Even in their forties, people with MS begin to display slowed motor coordination, comparable with those 30 or more years their senior without MS (Kirkland et al., Reference Kirkland, Downer, Holloway, Wallack, Lockyer and Buckle2017). Although MS reduces life expectancy by 6–10 years, the proportion of people with MS in the later stages of life is growing and is predicted to increase in the coming decades (Bronnum-Hansen, Stenager, Hansen, & Koch-Henriksen, Reference Bronnum-Hansen, Stenager, Hansen and Koch-Henriksen2006; Koch-Henriksen, Laursen, Stenager, & Magyari, Reference Koch-Henriksen, Laursen, Stenager and Magyari2017; Sadovnick et al., Reference Sadovnick, Ebers, Wilson and Paty1992). Older people with MS, like most other seniors, wish to remain in their own homes (Stacom, Reference Stacom2017). Further, older adults with MS in their eighth decade of life (octogenarians with MS), represent an under-studied population about whom there is little information about which factors allow some individuals to remain in the community whereas others require institutional care. Understanding potential protective factors could inform health providers in order to better target appropriate advice and intervention to help older people with neurodegenerative diseases such as MS successfully “age in place”.
Aging in place refers to the ability to live in one’s own home and community regardless of age, income, or disability, which is strongly favored over institutionalization (Cronin & Mandich, Reference Cronin and Mandich2015; Davey, de Joux, Nana, & Arcus, Reference Davey, de Joux, Nana and Arcus2004). Failure to achieve aging in place is significantly predicted by dependence in activities of daily living, depression, impaired cognitive function, difficulties with gait and balance, presence of multiple chronic conditions, and polypharmacy (Stuck et al., Reference Stuck, Minder, Peter-Wuest, Gillmann, Egli and Kesselring2000). These health concerns are typical among persons with MS, so it is not surprising that severity of physical and cognitive dysfunction are also significant predictors of institutionalization among people with MS (Thorpe et al., Reference Thorpe, Knox, Jalbert, Hyun-Ja Lim, Nickel and Hader2015). From the person’s perspective, social support, financial flexibility, resilience, effective and accessible health care, and healthy lifestyle habits are considered to be critical to successful aging at home among people with MS. Because MS is a progressive neurodegenerative disease, it is presumable that very few MS patients in their 80s would continue to live at home. Those who do are likely special in some way that allows them to successfully age in place.
The health of octogenarians with MS as a distinct group has not been examined; however, they have been included in large study cohorts (Ploughman et al., Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014). In these cohorts, people with MS over the age of 55 exhibit healthier lifestyle habits (diet, exercise, drinking alcohol in moderation and abstaining from smoking) than the general population (Ploughman et al., Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014). It is conceivable that octogenarians with MS living at home possess characteristics that protect them against the risk of institutionalization, such as having a milder form of MS with less physical disability or having a greater degree of social support and financial security. Alternatively, these individuals may in fact be living “on the edge” of institutionalization as a result of factors common in the most advanced stages of MS such as high levels of disability, lack of social resources, cognitive impairment, and symptoms of depression.
The overarching aim of the current study was to provide the first description of health, social, and lifestyle factors affecting octogenarians with MS. We employed a two-faceted approach to analyse this unique group by comparing them with a younger sample of people with MS between the ages of 60 and 70 as well as a group of Canadian octogenarians without MS. We hypothesized that octogenarians with MS would have greater disability than their comparators, potentially influencing participation, but would also exhibit protective factors such as high levels of social support, financial stability, and positive lifestyle choices including better diet and exercise practices.
Methods
Participants and Survey Variables
We used the Canadian Survey of Health, Lifestyle, and Aging with Multiple Sclerosis (CSHLA-MS) (Ploughman et al., Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014) to create two MS groups: Octogenarians with MS (80–89 years of age) and a younger group referred to as the “young-old MS group” (60–70 years of age). The CSHLA-MS was a self-report postal survey grounded by qualitative research regarding healthy aging with MS (Ploughman, Austin, Stefanelli, & Godwin, Reference Ploughman, Austin, Stefanelli and Godwin2010; Ploughman et al., Reference Ploughman, Austin, Murdoch, Kearney, Fisk and Godwin2012a, Reference Ploughman, Austin, Murdoch, Kearney, Godwin and Stefanelli2012b). With the assistance of national MS clinics, MS Society chapters, and newspaper advertisements, participants were recruited if they were 55 years of age or older and had had a diagnosis of MS confirmed by a neurologist with MS symptoms for 20 years or more. In total, 921 individuals were contacted, with 743 participants completing and returning the survey. To compare octogenarians with MS with the young-old MS group, we matched each octogenarian with MS randomly to three younger individuals with MS using the following criteria: (1) being between the ages of 60 and 70, and (2) same gender (M/F), (3) similar total years of education (± 2 years), and (4) from the same province. To obtain a comparison group of octogenarians without MS, we used the 2012 Canadian Community Health Survey (CCHS). We compared octogenarians with MS with participants from the 2012 version of the CCHS who were older than 80 years (Canadian octogenarians). Questions from the CCHS were matched by two members of the research team (M.B.D. and E.M.W.) to questions from the CSHLA-MS. As per Ploughman et al. (Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014), the data were extracted through online access using the University of Toronto Data Library service, and were analysed using the Survey Documentation and Analysis software
We compared the three groups (octogenarians with MS, the young-old MS group, and Canadian octogenarians) on four main categories of variables: socio-demographics, health and disability, lifestyle, and participation. With respect to the CSHLA-MS survey, questions were either specifically designed for the survey (including visual analogue scales [VAS]) or were obtained from one of the following sources: the Multiple Sclerosis Impact Scale (MSIS-29) (Hobart, Lamping, Fitzpatrick, Riazi, & Thompson, Reference Hobart, Lamping, Fitzpatrick, Riazi and Thompson2001), the Barthel Index (Mahoney & Barthel, Reference Mahoney and Barthel1965), the Co-Morbidity Questionnaire (Marrie & Horwitz, Reference Marrie and Horwitz2010), Frenchay Activities Index (FAI), the Simple Lifestyle Indicator Questionnaire (SLIQ) (Godwin, Pike, & Bethune, Reference Godwin, Pike and Bethune2013), the Hospital Anxiety and Depression Scale (HADS) (Honarmand & Feinstein, Reference Honarmand and Feinstein2009), the 12-item Resilience Scale (RS-12) (Wagnild & Young, Reference Wagnild and Young1993), and the Personal Resource Questionnaire (PRQ-2000) (Weinert, Reference Weinert1987).
Data and Statistical Analysis
CSHLA-MS data were entered into SPSS (v.21) for analysis. One way analyses of variance (ANOVAs) were used to compare responses on continuous variables, and χ2 tests were performed on categorical variables. Weighted averages in the form of percentages were used to compare the data from CSHLA-MS (MS groups) and the CCHS (Canadian octogenarians).
Results
Demographic Characteristics
There were 23 octogenarians with MS, representing 3.1 per cent of the original CSHLA-MS sample (Table 1). As expected, the octogenarians with MS were significantly older, by about 17 years, than the young-old MS group (mean, 64.6 years [SD = 4.2]). There were no differences in sex (χ2 = .75, p >.05) or level of education (χ2 = 2.14, p > .05) between the two MS groups. In terms of the use of disease-modifying drugs, only one of the MS octogenarians reported currently being prescribed disease-modifying drugs compared with 17 of the young-old MS group. In keeping with prior research on MS (Harbo, Gold, & Tintore, Reference Harbo, Gold and Tintore2013), sex distribution favored females in the MS groups but was more evenly split among Canadian octogenarians (octogenarians with MS were 78.3% female and Canadian octogenarians were 58% female). Octogenarians with MS reported more formal education than Canadian octogenarians, with only 8.7 per cent having less than a high school education compared with 43.4 per cent of Canadian octogenarians (Table 1).
Table 1: Demographic characteristics
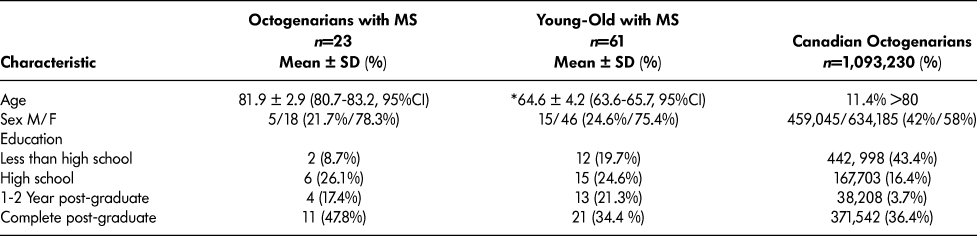
Note. F = 332.56, p < .05.
MS = multiple sclerosis.
Socioeconomics
Despite having been diagnosed with MS a decade earlier, octogenarians with MS reported a slightly higher degree of social support and financial flexibility (although not significantly so) compared with the young-old MS group (Table 2). Concerning living situation, more octogenarians with MS reported living with a partner than did their younger counterparts with MS. Forty-seven per cent of both MS groups reported having private health insurance. Octogenarians with MS reported having to discontinue their employment because of MS half as often as the young-old MS group (Table 2). Socioeconomic data were not available for the Canadian octogenarians sample.
Table 2: Comparing health and lifestyle factors in octogenarians with MS the young-old with MS
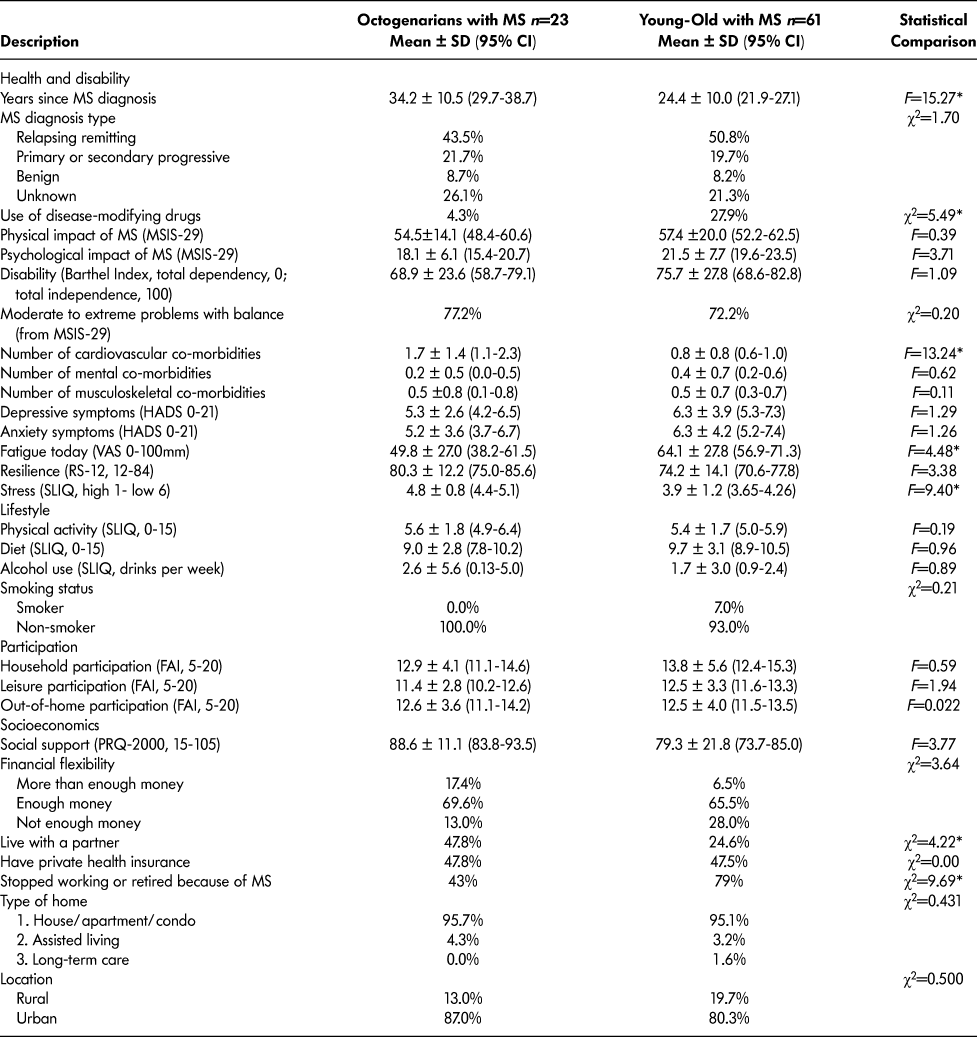
Note. *p < 0.05.
MS = multiple sclerosis , CI = confidence interval, MSIS-29 = Multiple Sclerosis Impact Scale, HADS = Hospital Anxiety and Depression Scale, VAS = visual analogue scale, RS-12 = Resilience Scale-12, SLIQ = Simple Lifestyle Indicator Questionnaire, FAI = Frenchay Activities Index, PRQ-2000 = Personal Resource Questionnaire.
Health and Disability
The majority of both octogenarians with MS and the young-old group were initially diagnosed with the relapsing remitting form of MS (Table 2). There were no differences in the physical and psychological impacts of MS or in the level of disability measured by the Barthel Index (Figure 1). The average Barthel Index scores suggested that most respondents in both groups required assistance with at least some activities of daily living. With respect to mental health, both groups had low levels of anxiety and depressive symptoms as measured by the HADS. The octogenarians with MS reported significantly less stress and less fatigue than the young-old group and reported higher levels of resilience (although not significantly so). Both groups scored on average in the highest quartile on the Resilience Scale. There were no differences between groups concerning mental or musculoskeletal co-morbidities, however octogenarians with MS reported double the number of cardiovascular co-morbidities.
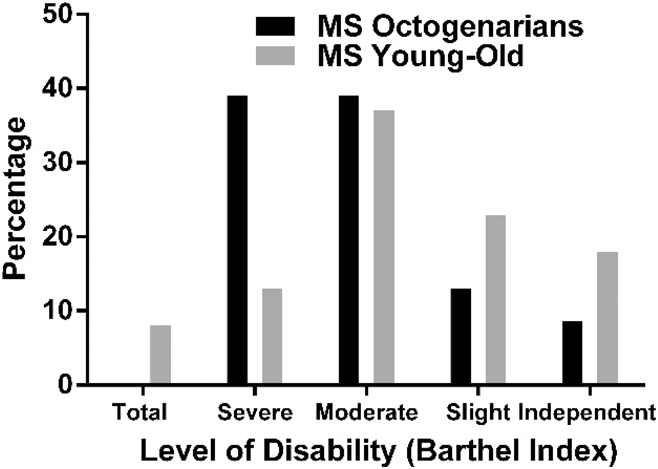
Figure 1: Level of disability measured using the Barthel Index in the octogenarians with multiple sclerosis (MS) and young-old MS groups. Total Dependence is denoted as a total score of 0–20, Severe Dependence is denoted as a total score of 21–60, Moderate Dependence is denoted as a total score of 61–90, Slight Dependence is denoted as a total score of 91–99, and Independent is denoted as a total score of 100, indicating ability to ascend/descend stairs on one’s own and perform activities of daily living without assistance
When comparing the health of octogenarians with MS with that of the Canadian octogenarians (Table 3), octogenarians with MS indicated that they required home or personal care services twice as frequently as other Canadians their age. With respect to mobility, less than half of the octogenarians with MS reported being able to walk independently compared with almost 70 per cent of Canadian octogenarians. Octogenarians with MS reported a higher percentage of mental health and cancer-related comorbidities whereas the Canadian octogenarians more often reported arthritis.
Table 3: Comparing health and lifestyle factors among octogenarians with and without MS
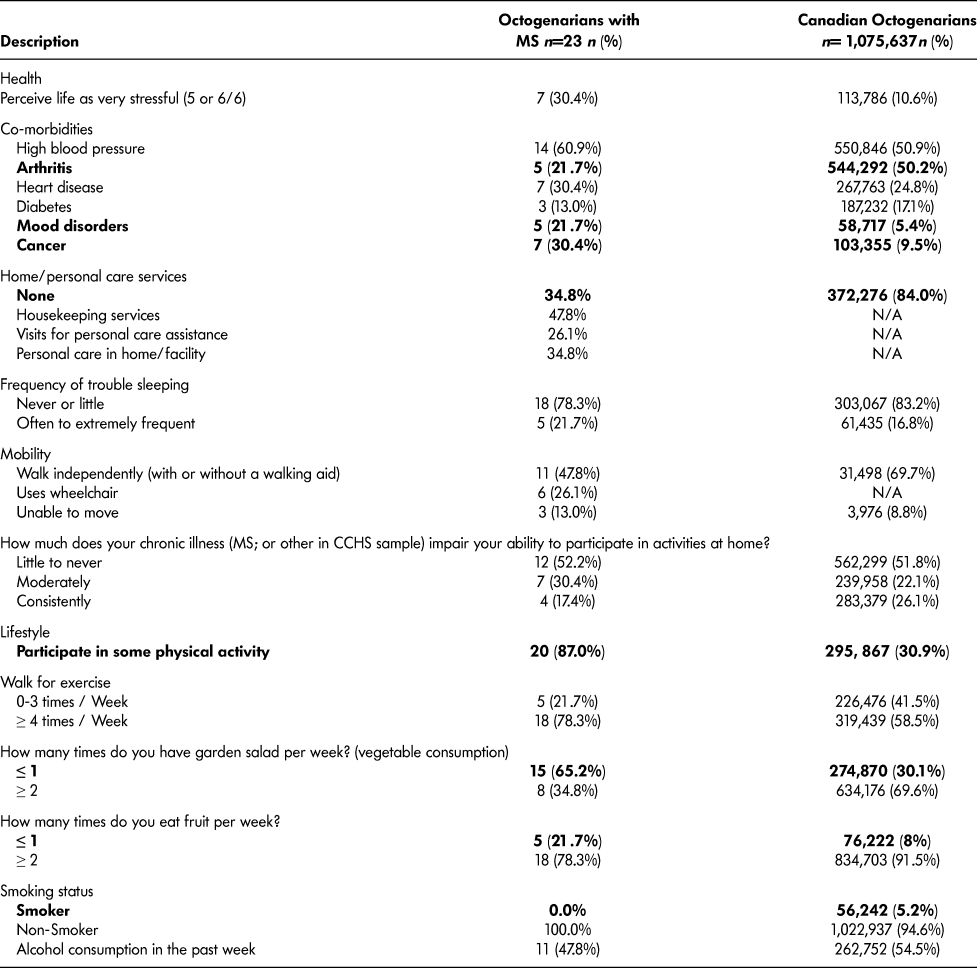
Note. Bold type emphasis indicates variables that are substantially different between groups.
MS = multiple sclerosis, CCHS = 2012 Canadian Community Health Survey.
Lifestyle
We compared scores on the Simple Lifestyle Indicator Questionnaire, which tabulated information about physical activity, diet, alcohol intake, and smoking between the MS groups (Godwin et al., Reference Godwin, Streight, Dyachuk, van den Hooven, Ploemacher and Seguin2008). Both groups reported low to moderate levels of physical activity, a good quality diet, and modest alcohol intake, with no differences between groups. Seven per cent of the young-old MS group were smokers compared with none of the MS octogenarians, although smoking habits were not significantly different between groups (Table 2).
When comparing the octogenarian groups (Table 3), 87 per cent of the MS group reported being physically active compared with only a third of Canadian octogenarians. Seventy-eight per cent of octogenarians with MS walked four or more times per week, compared with 58.5 per cent of Canadian octogenarians (Table 3). With respect to diet, the MS group did not appear to choose fruits and vegetables as often as other Canadians of the same age (Table 3). Of Canadian octogenarians, 69.6 per cent reported vegetable consumption in the form of garden salads more than twice weekly, compared with only 21.7 per cent of octogenarians with MS. The MS group also reported 13 per cent less fruit intake two or more times a week. Finally, the groups did not differ greatly with respect to smoking or alcohol consumption.
Participation
Both the octogenarians with MS and the young-old MS group reported a high degree of household, leisure and out-of-home participation that was not significantly different between groups (Table 2). Octogenarians with MS reported significantly less stress in their lives than the young-old MS respondents (Table 2). More than half of the Canadian and MS octogenarians considered that their chronic health conditions had little or no impact on their participation and ability to function at home (Table 3).
Discussion
Previous research examining successful aging among the general population has identified four key contributors to healthy aging: social connectedness, physical health, intact psycho-cognitive function, and positive lifestyle behaviours (Gray & Arnett, Reference Gray and Arnett2014; Peel, Bartlett, & McClure, Reference Peel, Bartlett and McClure2004). For those living and aging with MS, these contributors to successful aging are often threatened by the progressive nature of the disease itself. We undertook this study to determine potentially protective characteristics within a group of older adults living with MS (octogenarians with MS) who continued to live at home. We compared them with a younger group of older adults with MS 60–70 years of age as well as with members of a national sample of octogenarians in Canada. We expected that octogenarians with MS, who were able to successfully remain at home, would have a milder form of the disease and therefore less disability; however this was not the case. Despite similar levels of disability and a greater number of co-morbid conditions, MS octogenarians reported stable and even slightly higher levels of social support and financial security than their younger counterparts. They maintained moderate levels of physical activity and a high degree of household, leisure, and out-of-home participation despite being more disabled than other Canadians their age. Importantly, they reported significantly less stress and fatigue compared with the young-old MS group. Our findings support that there are five interrelated elements contributing to successful aging among the very oldest people with MS: social support, financial security, attitude, positive lifestyle behaviours (particularly exercise), and participation in life roles. These five factors overlap with some of the elements described in previous qualitative and quantitative studies examining healthy aging with MS, suggesting that these five elements move to higher priority among the oldest old living with MS (Ploughman et al., Reference Ploughman, Austin, Murdoch, Kearney, Fisk and Godwin2012a; Wallack, Wiseman, & Ploughman, Reference Wallack, Wiseman and Ploughman2016).
Our results confirm that social support is central to successful aging in place among people with MS (Foote, Piazza, Holcombe, Paul, & Daffin, Reference Foote, Piazza, Holcombe, Paul and Daffin1990; Ploughman et al., Reference Ploughman, Austin, Murdoch, Kearney, Godwin and Stefanelli2012a; Wallack et al., Reference Wallack, Wiseman and Ploughman2016; Wineman, Reference Wineman1990). The PRQ-2000 survey employed in this study not only measured elements of operational support (physical and emotional assistance) but also attachment to others, social integration, nurturance, and feelings of worth (Weinert, Reference Weinert, Strickland and Dilorio2003), so it provided a comprehensive measure of social connectedness. The scores on the PRQ-2000 in this sample of octogenarians with MS were very high with a mean score of 88.6 out of 105 (10 points higher than the young-old group with MS), suggesting that the octogenarians with MS were socially connected within their families and communities and received assistance as needed. Their average score was higher than that reported among older community-dwelling individuals who scored between 80 and 85 (Tawalbeh & Ahmad, Reference Tawalbeh and Ahmad2013), and higher than those measured among older persons with type 2 diabetes whose scores averaged 80/105 (Bai, Chiou, & Chang, Reference Bai, Chiou and Chang2009; Bai, Chiou, Chang, & Lam, Reference Bai, Chiou, Chang and Lam2008). Further, the octogenarians with MS average PRQ-2000 score exceeded those reported from large samples of younger people with MS (n = 499, n = 450) whose average scores were 82 and 85 (Weinert, Reference Weinert, Strickland and Dilorio2003). Clearly, social support and connectedness should be emphasized by health teams in order to foster aging in place.
The exceptionally high degree of social connectedness in the octogenarians with MS suggests that they were also successful in maintaining co-habitation and marriage. Our data support that, along with high PRQ-2000 scores, they were more likely to live with their partner than were the MS young-old group. This fact is important, because people aging with MS are at great risk of divorce. Pfleger and group reported that the risk of divorce or separation was higher among people with MS (12%) and that risk worsened over 24 years (to 67%) compared with controls (47%) (Pfleger, Flachs, & Koch-Henriksen, Reference Pfleger, Flachs and Koch-Henriksen2010). Among people with dementia, being single carried eight times greater risk of institutionalization compared with being married (Luppa et al., Reference Luppa, Luck, Weyerer, Konig, Brahler and Riedel-Heller2010). Along with the social support provided with marriage, there is likely greater financial security with a potential second income and savings. Our data confirmed that 87 per cent of octogenarians with MS reported that they had enough, or more than enough money to meet their needs. Such security is important, because the estimated out of pocket cost of MS in Canada was $16,800 in 2011 and was predicted to rise in the future (Nana et al., Reference Nana, Ruth, Christina, Rochelle, Douglas and Ron2017). Financial stability, and its inter-relationships with social support and public health, seems to be important to aging in place when living with a chronic disease such as MS. Future research should examine the impact of finances and public health systems on aging in place, particularly comparing practices in other countries.
Despite requiring assistance to perform activities of daily living, octogenarians with MS reported a high degree of participation in household, leisure, and out-of-home activities, similar to levels reported by people with MS who were 10 years their junior. They were also more physically active than other Canadians their age despite reporting greater disability. Notably, over half of respondents in the octogenarians with MS group reported that their chronic condition had little to no impact on their ability to participate. In this unique group of the oldest-old living at home with a neurodegenerative condition, protective factors such as social support and financial stability may foster participation and buffer the deleterious effects of having mobility impairments. For example, 66 per cent of octogenarians with MS reported that they received outside assistance for housekeeping and personal care compared with only 16 per cent of Canadian octogenarians. Such physical care, and the finances to provide such support (because in Canada most services are not covered by the government plan), likely permits octogenarians with MS to successfully age in place. Furthermore, 47 per cent of both MS groups reported having private health insurance, higher than previously reported for Ontario senior citizens (27%) (Allin, Law, & Laporte, Reference Allin, Law and Laporte2013). It is reasonable to think that people with MS should receive counselling early in the disease to establish financial security, as it likely contributes to the ability to afford private health insurance and to obtain paid personal care, factors that synergistically facilitate aging in place.
We found that fewer of the octogenarians with MS in our sample retired or stopped working because of MS (43%) compared with their younger counterparts (79%). Paid work often provides purpose, development of social networks, and financial stability. Work is especially valued among people with MS who express that the non-financial benefits of work are as important as the financial ones (Robinson, Reference Robinson1993). The present findings may suggest that the ability to continue to work while living with MS enhances the capacity to age in place; however, it is worth noting that generational differences between octogenarians with MS and the young-old group may play a role in this difference. From a historical perspective, older generations tended to have women work at home more frequently than more recent generations (Ferrao, Reference Ferrao2010). As most (78.3%) of the octogenarians with MS in our sample were female, it is conceivable that some of these respondents did not work outside of the home and so may have indicated that they had not retired (from presumably paid work). Nevertheless, it is concerning that 79 per cent of the young-old MS group indicated that they had to retire or stop working because of MS. This forced retirement or unemployment can place these individuals at great risk of financial destabilization and social isolation. It was interesting to note that the octogenarians with MS were highly educated, with almost 48 per cent having completed post-graduate education, more than 10 percentage points higher than the young-old and Canadian octogenarians groups. It is also possible that, because of their level of advanced education, the octogenarians with MS were able to continue paid work longer because their work may not have required extensive physical demands. Level of education on its own can be protective. For example, among older people receiving Medicare in the United States, having less than a high school diploma increased odds of deterioration, institutionalization, or death by 24 per cent (Kurichi et al., Reference Kurichi, Streim, Xie, Hennessy, Na and Saliba2017). Furthermore, level of education, advanced occupational attainment, and participation in leisure activities may help to build “cognitive reserve” (Stern, Reference Stern2012) thereby providing some protection against neurodegeneration. Whether unemployment hastens cognitive decline or shrinking of the “cognitive reserve” is not clear; however, work modifications and other methods to maintain employment as mediators of aging in place are worthy of future investigation.
More than 70 per cent of older people with MS report moderate to extreme balance problems (Ploughman, Deshpande, Latimer-Cheung, & Finlayson, Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014) and falls and fear of falling threaten independent living among people aging with a disability (Finlayson & Peterson, Reference Finlayson and Peterson2010; Ploughman et al., Reference Ploughman, Beaulieu, Harris, Hogan, Manning and Alderdice2014). When compared with age-matched controls, Einarsson, Gottberg, Fredrikson, von Koch, & Holmqvist (Reference Einarsson, Gottberg, Fredrikson, von Koch and Holmqvist2006) found that people with MS (mean age 51 ± 12) performed only 35 per cent of the social and lifestyle activities that their peers did (Einarsson et al., Reference Einarsson, Gottberg, Fredrikson, von Koch and Holmqvist2006). Our findings suggest that despite having a greater number of co-morbid conditions, moderate to severe levels of disability (80%) and balance problems, octogenarians with MS participated in valued activities at similar levels as people living with MS who were 17 years their junior, as well as at similar levels as their peers of the same age living without MS. Although we did not examine falls or fear of falling, it seems as though octogenarians with MS are able to overcome the challenges associated with level of disability, higher number of co-morbid conditions, and poor balance in order to maintain exercise levels and household, leisure and out of home activities (Ploughman, Reference Ploughman2017; Ploughman et al., Reference Ploughman, Harris, Wallack, Drodge, Beaulieu and Mayo2015). This result suggests that there is sound rationale for including behavioural therapies that help manage the barriers associated with aging with a chronic disease in a care plan to help people age in place.
Psychological factors such as mood, attitude, and levels of resilience and fatigue likely contribute to participation and to perceived quality of life. Octogenarians with MS reported low levels of depression and anxiety and high levels of resilience and had significantly lower levels of stress and fatigue than the young-old group of people with MS. However, they also had a higher overall prevalence of mood disorders than Canadians their age. High levels of fatigue and low levels of physical activity are part of a vicious cycle, in which one perpetuates the other (Ploughman, Reference Ploughman2017) and attitude is second only to level of disability as a major barrier to participation in physical activity for people with MS (Ploughman, Reference Ploughman2017). There is a large body of evidence to suggest that both anxiety and depression are more common among people with MS than among the general population (Boeschoten et al., Reference Boeschoten, Braamse, Beekman, Cuijpers, van Oppen and Dekker2017). Among 7,757 respondents 65–103 years of age living in 16 European countries, there was a reciprocal relationship between participation in physical activity and positive attitude, despite mobility challenges (Lee, Reference Lee2016) suggesting that psychological health and physical activity are linked. Our results, along with those of others, support that management of depression, anxiety, stress, and fatigue are important for fostering participation in life roles, physical activity, and successful aging with MS.
Our study offers the first description of the prevalence of health and lifestyle factors of octogenarians with MS. However, there are several limitations to the present study. First, the data were derived from self-report and are therefore subjective, and could be subject to recall bias. Second, we were only able to use the CCHS data as reference values, so we were unable to statistically compare the Canadian octogenarians with octogenarians with MS. Because completing questionnaires requires intact cognitive abilities, we were unable to discern whether there were differences in cognition between the groups. Cognitive impairment places older people at greater risk of institutionalization (Thorpe et al., Reference Thorpe, Knox, Jalbert, Hyun-Ja Lim, Nickel and Hader2015), so future studies should examine cognition and institutionalization among older people with MS. The cross-sectional study design is limited in that it cannot infer changes that occur as the same individuals age across time. Future work should address this issue by conducting longitudinal research examining changes in health and lifestyle factors among older people with MS to more closely examine how those aging with MS change across the lifespan. Further, only a small fraction of the CSHLA-MS respondents (n = 23) were octogenarians, possibly representing a small portion of survivors. There is likely sampling bias because people who participate in surveys are more likely to have post-secondary education and are less likely to be from disadvantaged groups (Voigt, Koepsell, & Daling, Reference Voigt, Koepsell and Daling2003). Survey respondents also tend to be healthier overall (Keyes, Rutherford, Popham, Martins, & Gray, Reference Keyes, Rutherford, Popham, Martins and Gray2018). The small sample and potential sampling bias limits generalizability. When comparing with the Canadian cohort, the sample of MS is only 23 compared with more than 1,000,000 respondents in the national survey. Lastly, we could only compare questions from the CSHLA-MS with questions from the CCHS that matched, and in some cases wording was not exactly the same.
Conclusion
Our study offers the first description of the prevalence of health and lifestyle factors in a population of octogenarians with MS. Importantly, five elements including social support, financial security, attitude, positive lifestyle behaviours (particularly exercise), and participation in life roles appear to be integral to aging in place among the very oldest people with MS. When compared with previous work in the field of healthy aging with MS, we suggest that these five elements take on high priority among the oldest old living with MS. Accordingly, these factors should be considered as important targets for early intervention to support young and middle-aged individuals with MS who intend to plan for aging in place.






