Atherosclerosis is associated with several pathologies including hypertension, diabetes and obesity, and it represents a very real public health problem. Thus, further insight into the physiopathology of atherosclerosis and the identification of new therapeutic targets would be extremely useful in the treatment of atherosclerosis.
Atherosclerosis appears to be initiated in response to endothelial dysfunction induced by an accumulation of lipids in the blood vessels (Tedgui & Mallat, Reference Tedgui and Mallat1999). One of the first endothelial dysfunctions observed in hypercholesterolaemia is the attenuation of endothelium-dependent vasodilatation (Singer et al. Reference Singer, Tsao, Wang, Bloch and Cooke1995). These abnormalities may be at least partly due to a reduced availability of NO, which plays an important vasodilator role and is involved in the anti-atherogenic properties of the endothelium (Matthys & Bult, Reference Matthys and Bult1997).
NO is formed from the amino acid arginine, with concomitant formation of citrulline, by endothelial NO synthase (eNOS) in endothelial cells (Cynober et al. Reference Cynober, Le Boucher and Vasson1995). NO production depends on the availability of l-arginine, and supplementation with l-arginine increases NO production in vivo (Cooke et al. Reference Cooke, Singer, Tsao, Zera, Rowan and Billingham1992; Singer et al. Reference Singer, Tsao, Wang, Bloch and Cooke1995; Boger et al. Reference Boger, Bode-Boger, Brandes, Phivthong-ngam, Bohme, Nafe, Mugge and Frolich1997). In rabbit models, l-arginine supplementation (2 % in drinking water, which is sufficient to double plasma levels) has been shown to exert anti-atherogenic effects through the NO pathway: restoration of endothelium-dependent relaxation (Boger et al. Reference Boger, Bode-Boger, Brandes, Phivthong-ngam, Bohme, Nafe, Mugge and Frolich1997), increased urinary nitrate excretion (Boger et al. Reference Boger, Bode-Boger, Szuba, Tsao, Chan, Tangphao, Blaschke and Cooke1998), and inhibition of leucocyte adhesion (Brandes et al. Reference Brandes, Brandes, Boger, Bode-Boger and Mugge2000). Normal plasma arginine levels in man and animals range from 95 to 250 μm depending on nutritional status (Wu & Meininger, Reference Wu and Meininger2000). Human studies in which daily arginine consumption was increased four- to five-fold have also demonstrated the beneficial effects of arginine in improving endothelium-dependent relaxation in hypercholesterolaemic patients (Gornik & Creager, Reference Gornik and Creager2004). These observations suggest that interventions designed to increase NO production may constitute a therapeutic strategy for the treatment and prevention of atherosclerosis. However, a recent study (Vascular Interaction With Age in Myocardial Infarction (VINTAGE MI) randomised clinical trial; Schulman et al. Reference Schulman, Becker and Kass2006) showed that l-arginine supplementation (3 g three times per d) in post-infarction patients did not improve vascular function but may have been associated with higher post-infarction mortality. Hence, based on current data, we cannot draw solid conclusions on l-arginine supplementation for the prevention of atherosclerosis (Loscalzo, Reference Loscalzo2003; Siasos et al. Reference Siasos, Tousoulis, Antoniades, Stefanadi and Stefanadis2007; Yang & Ming, Reference Yang and Ming2006).
Atherosclerosis is currently treated by statins, which are inhibitors of 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase, the rate-limiting enzyme in the biosynthesis of cholesterol (Dujovne, Reference Dujovne1997). Recent large cohort clinical trials (Gresser & Gathof, Reference Gresser and Gathof2004) have demonstrated that statins decrease the incidence of CHD in patients with hypercholesterolaemia and atherosclerosis. Also, statins exert pleiotropic effects (Takemoto & Liao, Reference Takemoto and Liao2001), including inhibition of inflammation and reversal of endothelial dysfunction. At the cellular level, statins increase the bioavailability of NO (by up regulation of eNOS activity) (Laufs et al. Reference Laufs, La Fata, Plutzky and Liao1998), reduce the production of free radicals (Kalinowski et al. Reference Kalinowski, Dobrucki, Brovkovych and Malinski2002) and inhibit the action of many pro-inflammatory mediators (Dichtl et al. Reference Dichtl, Dulak, Frick, Alber, Schwarzacher, Ares, Nilsson, Pachinger and Weidinger2003). Moreover, Feron et al. (Reference Feron, Dessy, Desager and Balligand2001) have demonstrated an atorvastatin-mediated stimulation of NO production in vitro. These results support those from a rabbit study by Thakur et al. (Reference Thakur, Hayashi, Sumi, Kano, Tsunekawa and Iguchi2001) who reported that the administration of simvastatin reduced the total lesion area, stabilised eNOS mRNA levels, increased NO production and functional relaxation, and decreased the production of superoxide anion and peroxynitrite.
Taken together, the data presented suggest that it would be of major interest to combine a therapy that increases eNOS expression (i.e. a statin) with a dietary manipulation that increases the availability of an NO precursor (i.e. l-arginine), with the goal of promoting NO production in order to help the endothelium counteract the atherosclerosis process. Hence, the aim of the present study was to evaluate the combined effects of atorvastatin and dietary l-arginine in the treatment of atherosclerosis in homozygous Watanabe heritable hyperlipidaemic rabbits.
Methods
Chemicals
Unless otherwise stated, all chemicals were purchased from Randox (Montpellier Fréjorgues, France).
Animals and study design
Thirty-four 6-week-old male and female homozygous Watanabe rabbits (Animal Production Centre, Olivet, France) were fed the EXT C15 diet (Dietex, St Gratien, France) throughout the study. This diet contained 16 % crude protein, 3·2 % fat, 49·3 % carbohydrates, 13·6 % fibre and 8·03 MJ gross energy/kg. Arginine content in the diet was 0·98 %. Each animal was housed in an individual cage (at 20°C with a 12 h light–dark cycle) and received a 100–150 g daily food ration. After a 7-d acclimatisation period, the animals were assigned to one of the four treatment groups. Rabbits in the control group (group C; n 9) were fed normal rabbit chow, while rabbits in the l-arginine group (group A; n 9) received chow enriched with 1·5 % l-arginine, i.e. 1 g/kg body weight per d. The l-arginine-enriched chow (EXT C15 diet +1·5 % l-arginine) was prepared by Dietex (St Gratien, France). Rabbits in the statin group (group S; n 8) received 2·5 mg atorvastatin/kg per d (Maeso et al. Reference Maeso, Aragoncillo, Navarro-Cid, Ruilope, Diaz, Hernandez, Lahera and Cachofeiro2000) (Atorvastatin, Tahor® 10 mg; Godeche-Pfizer, Freiburg, Germany) in their drinking water plus normal chow, while rabbits in the statin plus l-arginine group (group SA; n 8) received the l-arginine-enriched chow together with atorvastatin in their drinking water. After one night of water deprivation, the statin was administered in a small quantity of water to ensure that all statin was consumed by the rabbits. The animals then had free access to water during the day. Since the present study involves a pharmacological intervention, we did not consider it useful to render the regimens isonitrogenous.
Food intake was measured daily and the animals were weighed weekly. Blood samples were collected into sodium heparinate (Sanofi, Winthrop Industry, Gentilly, France) and immediately centrifuged at +4°C for 15 min at 4500 g. Samples were taken at the beginning of the treatment (T0) and at 2-week intervals during the dietary intervention period (T2, T4, T6, T8).
After 8 weeks of treatment (T8), blood samples were taken and the animals were anaesthetised with a heparinised sodium pentobarbital solution (40 mg/kg; Sanofi Santé Animale, Libourne, France) before being killed.
Animal care and experimentation complied with the rules of our institution and with Council of Europe Guidelines. Chantal Martin (no. 75–10) and Christophe Moinard (no. 75–522) are licensed to conduct experimental studies on living animals, and we had received approval for the use of animal facilities (agreement no. A75-06-02, Veterinary Service Directorate, Prefecture de Police de Paris, France).
Topography and histological analysis
After being anaesthetised, the animals were laparotomised along the full length of the cervico-thoracic region. An incision was made in the aorta at the iliac bifurcation then taken up to the aortic arch. Excess adventitial tissue was removed in saline. The aorta was fixed for 20 min in a 2 % paraformaldehyde and 2 % glutaraldehyde solution (Clubb et al. Reference Clubb, Cerny, Deferrari, Butler-Aucoin, Willerson and Buja2001). The lumen of the aorta was exposed via a ventral incision along the entire longitudinal length and fixed for 24 h in the same solution. After 24 h, the aorta was rinsed briefly in 70 % alcohol and then stained with Sudan IV (S-8756; Sigma, Aldrich, La Verpillière, France) to identify gross lipid distribution. It was left in the staining solution (at room temperature) for 30 min, and was then differentiated in 80 % alcohol for 20 min and washed in running tap water for 1 h (Clubb et al. Reference Clubb, Cerny, Deferrari, Butler-Aucoin, Willerson and Buja2001). The stained aorta was photographed with a Nikon® 995 digital camera (Tokyo, Japan). The area of lesions was determined using NIH Scion Image Software (Scion, Frederick, MD, USA). The area was measured three times, and the CV averaged 8·9 (se 5·4) %. After evaluation, the aorta was treated for microscopic study.
Optical microscopy was performed using four 2 mm thick fragments of the aorta cut transversely into four segments (aortic arch, thoracic aorta, abdominal aorta and abdominal aorta bifurcation). After dehydration with graded ethanol and paraffin embedding with a suitable orientation, 5 μm sections of each specimen were stained with haematoxylin–eosin–saffron staining.
Biochemical analysis
Plasma total cholesterol was determined by a routine enzymic method (Allain et al. Reference Allain, Poon, Chan, Richmond and Fu1974) on a Hitachi 911 analyser (Roche, Meylan, France).
Plasma l-arginine level was assayed on a JEOL automated amino acid analyser (Tokyo, Japan) using ion-exchange chromatography (Neveux et al. Reference Neveux, David, Cynober and Cynober2004). The results of our participation in the European Quality Control Scheme (ERNDIM) confirm the accuracy of our amino acid determinations.
Since nitrite and nitrate are the products of NO, the concentration of nitrite plus nitrate in plasma was used as an indicator of total NO production. Plasma nitrite levels were measured after enzymic conversion of nitrate to nitrite by nitrate reductase, using a commercial kit (R&D Systems, Lille, France) in a simple two-step process based on the Griess method (Ricart-Jane et al. Reference Ricart-Jane, Llobera and Lopez-Tejero2002). Plasma samples were ultrafiltered using 10 000 molecular weight cut-off filters before analysis to avoid interference with proteins, such as heparin.
Statistics
The experiment was performed in two parts (with animals from all four groups in each part). The two sets of experiments provided similar results which were therefore pooled, with the exception of NOx which showed higher values in the second set of experiments due to improvements in the technique. Therefore, for this parameter, values were expressed as a ratio to controls. All data are expressed as mean values with their standard errors. All biochemical parameters were analysed by two-way ANOVA (variables: treatment and time) followed by Bonferroni post hoc analysis. Area of lesions was analysed using a Kruskal–Wallis non-parametric test (variable: treatment), followed by a Student's t test as post hoc analysis. StatView 5.0 software (SAS Institute, Cary, NC, USA) was used for statistical analysis, and the level of significance was set at P ≤ 0·05.
Results
Food intake
Food consumption over the 8 weeks of the dietary intervention was not significantly different between groups. In arginine-supplemented rabbits, arginine intake from the l-arginine-enriched diet was about two-fold higher than with the normal diet (Table 1).
Table 1 Food consumption and l-arginine consumption* (Mean values with their standard errors)
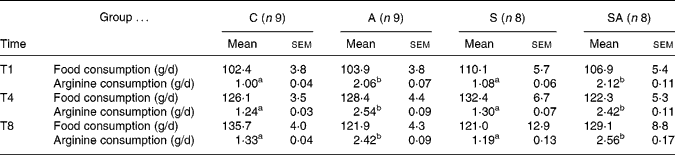
C, control group; A, l-arginine group; S, statin group; SA, statin–l-arginine group; T1, after 1 week of treatment; T4, after 4 weeks of treatment; T8, after 8 weeks of treatment.
a,b Mean values within a row with unlike superscript letters were significantly different (P < 0·05) (one-way ANOVA with Bonferroni post hoc analysis).
* Food consumption and l-arginine consumption were measured daily, and the results are expressed as mean intake over the preceding week (T0–T1, T3–T4 and T7–T8, respectively).
Effect of treatments on plasma cholesterol level
At the beginning of the experiment (T0), the mean plasma cholesterol level of all animals was 21·0 (sem 0·6) mmol/l. Two-way ANOVA analysis revealed both a time effect (P = 0·0023) and a treatment effect (P = 0·0002) as well as interactions between the two (P < 0·001). After 8 weeks of treatment (T8), total plasma cholesterol levels were significantly lower in groups S (P < 0·0001) and SA (P = 0·0011) compared with group A. Cholesterol levels increased continuously from T0 to T8 in groups C and A (Table 2).
Table 2 Effect of treatments on total plasma cholesterol levels*(Mean values with their standard errors)
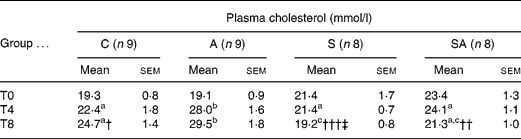
C, control group; A, l-arginine group; S, statin group; SA, statin–l-arginine group; T0, at beginning of experiment; T4, after 4 weeks of treatment; T8, after 8 weeks of treatment.
a,b,c Mean values within a row with unlike superscript letters were significantly different (P < 0·05) (one-way ANOVA with Bonferroni post hoc analysis).
* Two-way ANOVA showed significant time (P = 0·0023) and treatment (P = 0·0002) effects as well as interaction between the two (P < 0·0001).
Mean value at T8 was significantly different from that of the A group: † P = 0·0157, †† P = 0·0011, ††† P < 0·0001.
‡ Mean value at T8 was significantly different from that of the C group (P = 0·0076).
Effects of treatments on atherosclerotic lesions
The mean total area of lesions was lower in animals in group SA (statin plus arginine) and higher in animals in group A compared with controls (group C), but these differences did not reach statistical significance (Table 3).
Table 3 Effect of different treatments on area of lesions after 8 weeks of treatment (T8)† (Mean values with their standard errors)

C, control group; A, l-arginine group; S, statin group; SA, statin–l-arginine group.
* Mean value was significantly different from that of the C and A groups (P ≤ 0·05) (Kruskal-Wallis test followed by a Student's t test).
† Lesion area was estimated using planimetry software (Scion Image Software) showing area of total lesions at T8 expressed as a percentage of total area, and showing area of abdominal lesions measured on the abdominal half-length of the aorta at T8 expressed as a percentage of total area.
There was significantly (P = 0·0320) less lesion area measured on the abdominal aorta (abdominal half-length of the whole aorta) in the SA group compared with the other groups. Moreover, lesion areas were not lower in group S or group A (Table 3).
In all groups, the atherosclerotic plaques observed in the aortic arch were larger and thicker than those observed in the abdominal aorta. Qualitative observations of the aortas showed that that plaques in the SA group showed less spread and lower thickness than those observed in group S. Plaque composition did not correlate with any single treatment. The lesions were more fibrous than cellular (mainly macrophages), and their composition was not different between groups (data not shown).
Effects of treatments on plasma arginine levels and nitric oxide production
Two-way ANOVA analysis revealed both a time effect (P < 0·0001) and a treatment effect (P < 0·0001) as well as an interaction between the two (P < 0·001) on plasma arginine concentrations. After 4 weeks of treatment (T4), plasma arginine levels were significantly (P < 0·0001) higher in the two groups receiving arginine compared with the C group; arginine levels were doubled in group A, whereas group SA showed a slightly lower increase. Of note, arginine levels in groups A and SA were lower than at previous times but nevertheless significant (P = 0·0008) after 8 weeks of treatment compared with values at previous times.
There was no significant effect on plasma nitrite levels after either 4 weeks or 8 weeks of treatment (Table 4).
Table 4 Effect of treatments on plasma nitrite and arginine levelsReference Endres* (Mean values with their standard errors)
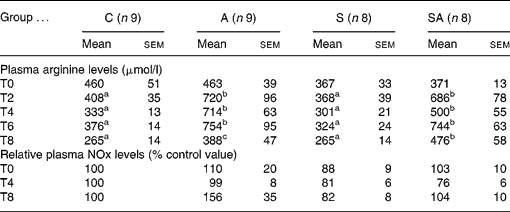
C, control group; A, l-arginine group; S, statin group; SA, statin–l-arginine group; T0, at beginning of experiment; T2, after 2 weeks of treatment; T4, after 4 weeks of treatment; T6, after 6 weeks of treatment; T8, after 8 weeks of treatment.
a,b,c Mean values within a row with unlike superscript letters were significantly different (P < 0·05) (one-way ANOVA with Bonferroni post hoc analysis).
* Two-way ANOVA showed significant time (P = 0·0003) and treatment (P < 0·0001) effects on plasma arginine as well as interaction between the two (P < 0·0001). There was no effect on plasma nitrite levels.
Discussion
The purpose of the present study was to determine the combined effects of l-arginine supplementation and atorvastatin administration in treating atherosclerosis in Watanabe homozygous rabbits. In this model, we showed that the association was more efficient in limiting the area of atherosclerosis lesions than either statin or arginine alone.
To our knowledge, only Pereira et al. (Reference Pereira, Bertolami, Faludi, Salem, Bersch and Abdalla2003) have evaluated the effects of an association of l-arginine and a statin, i.e. simvastatin (20 mg/d), on vasodilation in hypercholesterolaemic subjects. Their study, which was published while the present study was in progress, did not find any positive effects related to the association of l-arginine and statin. The authors explained this by the fact that some of the subjects were only mildly hypertensive, which could have masked improvements in flow-mediated vasodilatation. Also, Pereira et al. (Reference Pereira, Bertolami, Faludi, Salem, Bersch and Abdalla2003) did not evaluate treatment effects on the atherosclerotic plaques.
In the present study, we used homozygous Watanabe rabbits. In contrast with heterozygous Watanabe rabbits or New Zealand White rabbits, homozygous Watanabe animals develop atherosclerosis very early in life and are all atherosclerotic at the age of 5 months (Dowell et al. Reference Dowell, Hamilton, Lindop and Reid1995; Clubb et al. Reference Clubb, Cerny, Deferrari, Butler-Aucoin, Willerson and Buja2001). Moreover, in contrast to New Zealand White rabbits, homozygous Watanabe animals do not need to receive a cholesterol-enriched diet to become hypercholesterolaemic. In the present study, plasma cholesterol levels rose spontaneously as high as 21·0 (se 0·6) mmol/l, which is in strong agreement with previous studies; Clubb et al. (Reference Clubb, Cerny, Deferrari, Butler-Aucoin, Willerson and Buja2001) reported 22 mmol/l, while Dowell et al. (Reference Dowell, Hamilton, Lindop and Reid1995) defined homozygous animals as those exhibiting a cholesterol level greater than 10 mmol/l. Finally, the Watanabe heritable hyperlipidaemic rabbit is considered as a good model of human hereditary hypercholesterolaemia (Aliev & Burnstock, Reference Aliev and Burnstock1998). The higher increase in cholesterol levels in group A after 8 weeks of treatment is coherent with the higher lesion surface area in this group. Leong et al. (Reference Leong, Simkevich, Lesieur-Brooks, Lau, Fugere, Sabo and Thompson2006) showed that arginine might regulate certain cholesterol homeostatic genes; arginine deprivation induced a down regulation of HMG-CoA reductase and LDL receptor expressions. Although further studies are necessary to confirm this hypothesis, we suggest that the arginine supplementation could increase HMG-CoA reductase expression that may result, at least in this rabbit model, in an increase of cholesterolaemia.
The arginine supplementation was sufficient to generate a two-fold increase in plasma arginine, which is in good agreement with the literature (Cooke et al. Reference Cooke, Singer, Tsao, Zera, Rowan and Billingham1992; Singer et al. Reference Singer, Tsao, Wang, Bloch and Cooke1995; Boger et al. Reference Boger, Bode-Boger, Brandes, Phivthong-ngam, Bohme, Nafe, Mugge and Frolich1997). Of note, there was a lower increase in arginine levels at T8. This is probably due to the ‘arginine deficiency syndrome’ (Ochoa et al. Reference Ochoa, Bernard, Mistry, Morris, Figert, Maley, Tsuei, Boulanger and Kearney2000), since the blood was sampled after the laparatomy and Ochoa et al. (Reference Ochoa, Bernard, Mistry, Morris, Figert, Maley, Tsuei, Boulanger and Kearney2000) have shown that a certain amount of haemolysis of erythrocytes occurs immediately after trauma, leading to the release of arginase which in turn decreases plasma arginine levels.
The morphological study of the atherosclerotic plaques showed that there was no effect of treatment with atorvastatin alone, whereas other studies (Vaughan et al. Reference Vaughan, Murphy and Buckley1996; Weber et al. Reference Weber, Erl, Weber and Weber1999; Maeso et al. Reference Maeso, Aragoncillo, Navarro-Cid, Ruilope, Diaz, Hernandez, Lahera and Cachofeiro2000) have reported conflicting results in various animal models. In fact, statins inhibit several mechanisms involved in the formation of atherosclerotic lesions, including infiltration and smooth muscle cell migration and proliferation. Maeso et al. (Reference Maeso, Aragoncillo, Navarro-Cid, Ruilope, Diaz, Hernandez, Lahera and Cachofeiro2000) reported a decrease in area of atherosclerotic lesions in New Zealand White rabbits treated with atorvastatin (2·5 mg/kg per d). Furthermore, Kroon et al. (Reference Kroon, Stalenhoef, Buikema, Demacker, de Wilde, Leijten and van Gilst1993) highlighted a 53–80 % decrease in lesion incidence with pravastatin (40 mg/kg per d) in homozygous Watanabe heritable hyperlipidaemic rabbits. However, that study differed from the present study in that it was performed using 3-month-old animals over a 6-month period and with a significantly higher dose. Furthermore, l-arginine alone appeared to have no effect on lesion area, indicating that the significant decrease observed in the SA group is due to the association of atorvastatin plus l-arginine. We did not investigate the mechanisms by which arginine plus statin decreases the area of lesions in the rabbit aorta, which will require further studies, but there are hypotheses to explain this effect. On one hand, this anti-atherogenic effect of l-arginine may result from the dual action of l-arginine, which increases NO production by competing with the endogenous NOS inhibitor asymmetrical dimethyl l-arginine while at the same time decreasing the rate of oxidative inactivation of NO by superoxide radicals (Boger et al. Reference Boger, Bode-Boger, Brandes, Phivthong-ngam, Bohme, Nafe, Mugge and Frolich1997). A recent study (Hayashi et al. Reference Hayashi, Juliet, Matsui-Hirai, Miyazaki, Fukatsu, Funami, Iguchi and Ignarro2005) also showed that arginine alone was not effective in reducing lesions whereas arginine plus citrulline dramatically decreased lesion area, thus indicating that the lack of substrates might explain the formation of atherosclerotic lesions, as reported by Ozaki et al. (Reference Ozaki, Kawashima, Yamashita, Hirase, Namiki, Inoue, Hirata, Yasui, Sakurai, Yoshida, Masada and Yokoyama2002). On the other hand, even if eNOS is the major NOS isoform expressed in the cardiovascular system, inducible NOS (iNOS) is also expressed in macrophages and vascular smooth muscle cells (Miyoshi et al. Reference Miyoshi, Li, Shih, Wang, Laubach, Matsumoto, Helm, Lusis and Shi2006). In atherothrombotic patients, iNOS is up regulated and its expression and activity can promote atherogenesis (Loscalzo, Reference Loscalzo2003; Napoli et al. Reference Napoli, De Nigris, Williams-Ignarro, Pignalosa, Sica and Ignarro2006). Furthermore, iNOS expression has been reported in advanced atherosclerotic plaques (Miyoshi et al. Reference Miyoshi, Li, Shih, Wang, Laubach, Matsumoto, Helm, Lusis and Shi2006). Another recent study (Hayashi et al. Reference Hayashi, Matsui-Hirai, Fukatsu, Sumi, Kano-Hayashi, Rani and Iguchi2006b) reported that a selective iNOS inhibitor retards the progression of atherosclerosis in rabbits and that the administration of this inhibitor in combination with l-arginine tended to decrease iNOS protein expression in the aorta. Hence, the l-arginine administered would be used by both eNOS and iNOS, but to the best of our knowledge no study has yet shown in what proportion arginine is used by each of these isoforms in atherosclerosis. In light of recent studies showing that statins display anti-inflammatory effects (Endres, Reference Endres2006) and thus blunt iNOS activation, it is possible that the association of arginine with a statin might limit the use of arginine by iNOS and thus favour its use by eNOS. Our histological study gives a first element of response; in group A, the lesions appeared more cellular (mainly macrophages) than fibrous in comparison with groups SA and S (data not shown), indicating iNOS protein in the aortas from groups SA and S, thus confirming the anti-inflammatory effect of statins. Deeper insight into this phenomenon would be gained by using Western blotting to measure treatment-related iNOS changes, and studies should certainly be performed along these lines. Knock-out models could be used to better identify the individual role of each NOS isoform. For example, in a model of endotoxaemia, Soeters et al. (Reference Soeters, Hallemeesch, Bruins, van Eijk and Deutz2002) showed that eNOS and iNOS each contribute to about 50 % of systemic NO production.
We measured plasma nitrite levels to assess arginine conversion into NO (Adams et al. Reference Adams, McCredie, Jessup, Robinson, Sullivan and Celermajer1997; Preli et al. Reference Preli, Klein and Herrington2002). There was no variation in plasma nitrites as in the study of Hayaski et al. (Reference Hayashi, Juliet, Matsui-Hirai, Miyazaki, Fukatsu, Funami, Iguchi and Ignarro2005) in rabbits. Food consumption was controlled daily and was not significantly different between groups, indicating that the absence of variation in NO production was not due to a lack of arginine consumption (which was two-fold higher than with the normal diet). Despite the fact that moderate increases in NO production may be masked by NO storage in Hb (Dejam et al. Reference Dejam, Hunter, Schechter and Gladwin2004), plasma nitrite concentrations nevertheless remain a good indicator of endothelial NO production (Dejam et al. Reference Dejam, Hunter, Schechter and Gladwin2004). Indeed, Kleinbongard et al. (Reference Kleinbongard, Dejam and Lauer2003) using NOS inhibitors showed that 70 % of plasma nitrite was derived from eNOS and that eNOS knock-out triggered an 80 % decrease in plasma nitrite concentrations. Moreover, alterations in eNOS activity induced acute changes in plasma nitrite levels in the forearm vasculature (Dejam et al. Reference Dejam, Hunter, Schechter and Gladwin2004). Therefore, the absence of increase in nitrite in rabbits receiving arginine is more likely due to a lack of increase in plasma NO than an insufficiently sensitive nitrite assay. Given that various studies have given supportive evidence that arginase has a potential role in the regulation of endothelial NO production by competing with eNOS for l-arginine (Yang & Ming, Reference Yang and Ming2006), and that an increase in arginase II activity has been implicated in endothelial dysfunction (Ming et al. Reference Ming, Barandier and Viswambharan2004; Hayashi et al. Reference Hayashi, Esaki, Sumi, Mukherjee, Iguchi and Chaudhuri2006a), it appears likely that an increase in arginase activity in the arterial wall could be responsible for the lack of increase in plasma NO. Hence, it is the balance between NOS and arginase activities that regulates arginine utilisation in the artery wall, and further studies are therefore needed in order to explore the interactions involved. Moreover, it is now accepted that a sufficient NO diffusion gradient between endothelial cells and smooth muscle cells allows local paracrine activity (Dejam et al. Reference Dejam, Hunter, Schechter and Gladwin2004). Therefore, the lack of variation in plasma nitrite levels observed in the SA group could be the result of an optimal NO diffusion from endothelial cells to smooth muscle cells induced by the combination of atorvastatin and arginine. Nieuw Amerongen et al. (Reference Nieuw Amerongen, Vermeer, Negre-Aminou, Lankelma, Emeis and van Hinsbergh2000) showed a protective effect of simvastatin on the endothelial barrier, but they used a high-molecular-weight molecule to evaluate leakage through the endothelial barrier and their experiment was not designed to study the diffusion of low-molecular-weight molecules such as NO.
In conclusion, the present study is the first to demonstrate a significantly more beneficial effect of a treatment associating l-arginine and atorvastatin on the progress of atherosclerosis. The combination of a statin plus arginine as a treatment made it possible to achieve a 21 % decrease in the total area of lesions and a 44 % decrease in the area of abdominal lesions compared with control animals. Further mechanistic studies need to be performed, in particular to study the regulation of the NOS–arginase pathway. Moreover, a dose–response curve should be developed to determine the optimal efficiency of reducing the quantity of drug.






