INTRODUCTION
In March 2003, quarantine was introduced as a means to control the transmission of severe acute respiratory syndrome (SARS). While data to support its effectiveness were unavailable, the lack of such basic information on the causative agent, mode of transmission, period of communicability and incubation period required public health and infectious disease experts to return to first principles of infectious disease control. Containment through isolation of those who had symptoms consistent with SARS and quarantining contacts who might be incubating the disease were the primary community control measures available. The implementation of isolation precautions for persons known or suspected to be infectious remains commonplace for conditions such as tuberculosis, diarrhoeal illness and varicella. Further, mandatory isolation of HIV-positive persons has been used in Cuba during the 1980s and 1990s [Reference Perez-Stable1–Reference Hansen and Groce3]. The use of quarantine for contacts of diseases in modern society has, however, been essentially abandoned for more than a generation.
Quarantine was used for close contacts of SARS cases and has been proposed to control other potential health disasters such as pandemic influenza [4–6]. The impact of quarantine and compliance with restrictions on activities has not been systematically evaluated. Efficiency and effectiveness of SARS transmission in household and community settings has been examined [Reference Ou, Li and Zeng7, Reference Wilson-Clark8]. The experience of those placed under quarantine in terms of compliance, difficulties, emotional response and psychological impact remains under-researched [Reference Hawryluck9, Reference Blenden10]. The one relevant published study was a hypothesis-generating anonymous web-based survey of 129 self-reported quarantined persons [Reference Hawryluck9]. A high prevalence of psychological distress based on the Impact of Event Scale – Revised (IES-R) was reported in this biased sample and served in part as the impetus for this comprehensive study of quarantined individuals. Blenden et al.'s [Reference Blenden10] general population-based telephone survey identified emotional difficulties (11%) and loss of income (10%) as the most frequently reported problems among persons who reported being quarantined or who reported knowing of a family member or friend that was quarantined. Lastly, public health nurses involved in daily follow-up of those under quarantine confirmed concerns about individuals' understanding of quarantine, compliance behaviours, and varying emotional responses.
This study examined a cohort of adults quarantined during the SARS outbreak of 2003 to describe their understanding of the rationale for quarantine, difficulties, compliance and the psychological impact of the quarantine experience.
METHODS
During the 2003 SARS outbreak centred in Toronto, Canada, local public health units were responsible for identifying and quarantining contacts of potential SARS cases. Durham Region, a jurisdiction of 550 000 people immediately east of Toronto, recorded the third highest number of SARS cases in Canada (n=27). From 21 March to 24 June 2003, 4199 people were placed into quarantine. The Durham Region Health Department (DRHD) developed a computerized database to follow all quarantine individuals and recorded demographics, date(s) of exposure, exposure setting (e.g., hospital, travel, workplace), type of exposure (health-care facility worker (HCW), co-worker, patient, visitor, household), quarantine dates and the type of quarantine (i.e. work vs. home). Consistent with other jurisdictions within Canada, all persons placed under quarantine were provided masks, thermometers (if necessary) and instructions about quarantine requirements (Appendix 1). These supplies were delivered to the individual's residence. Quarantined individuals were contacted daily to assess compliance and to monitor for symptom development. While quarantine was initially considered ‘voluntary’ (i.e. a legal order was not issued under public health legislation), any individual who was identified as at risk (i.e. not available or could not be reached on the telephone or appeared as though they were not in their residence, e.g. cell phone) or threatened to breach quarantine received a home visit on behalf of the Health Department (e.g. emergency medical personnel, police, public health inspector, agency volunteer) and/or was issued a legal order.
Two distinct but inter-linked phases of SARS activity occurred, separated by about 3 weeks of unrecognized SARS activity. The two periods, called SARS1 and SARS2, were examined separately owing to knowledge and experience gained as the outbreak progressed. SARS1 is defined as 21 March–20 May 2003 and SARS2 is 21 May–24 June 2003.
All community-living adults aged ⩾18 years who were placed into quarantine, remained well, and were followed for at least two full days by the DRHD were eligible for the study. Institutionalized adults were excluded owing to necessary differences in the implementation of quarantine. In addition, 13 individuals were excluded to whom legal orders were issued owing to known or threatened non-compliance. With these exclusions, 1950 individuals were eligible to participate.
Following the principles of Dillman [Reference Dillman11] a standardized questionnaire was mailed to eligible participants in July 2003, with two reminders sent at 3-week intervals. The questionnaire assessed respondents' understanding of the rationale for quarantine, quarantine behaviours (including difficulties and compliance), as well as socioeconomic and psychological impacts. The complete questionnaire is available at: www.region.durham.on.ca.
Quarantine behaviours included perceived difficulty and actual ability to comply with specific DRHD quarantine requirements, as well as avoidance behaviours after quarantine. During quarantine, behaviours included mask usage, temperature monitoring, and restriction of activities designed to prevent SARS transmission to household members and the community (Appendix 1). Owing to the large number of health-care facilities affected during SARS2, work quarantine, a measure to ensure the short-term sustainability of the health-care system, was implemented. Work quarantine allowed HCW to leave their home to attend their place of work but required a private vehicle for transportation and N95 masks to be used consistently at work (Appendix 1).
Psychological impact examined feelings, fears of developing SARS, stigmatization, and symptoms of post-traumatic stress disorder (PTSD) using the IES-R (Appendix 2) [Reference Weiss, Marmar, Wilson and Keane12]. The IES-R is a self-report measure designed to assess current subjective distress for a specific traumatic life event. Responses to 22 items are scored and summed to a maximum score of 88. The mean on three subscale domains (avoidance, intrusion and hyperarousal) provides an indication of the level of distress experienced. When compared to the diagnostic criteria using DSM-IV, the original IES (without the hyperarousal scale) was found to have a sensitivity of 0·89–1·00 and a specificity of 0·78–0·94 for PTSD depending on cut points used [Reference Wohlfarth13].
Using a unique identifier, the variables date of birth, sex, exposure data (i.e. date, setting, and type) and type of quarantine were abstracted from the DRHD quarantine database and were merged with results of the self-reported study questionnaire.
Results were stratified by type of quarantine, type of exposure (HCW vs. non-HCW), and exposure date (SARS1 vs. SARS2). Data were analysed using SPSS v.12 (SPSS Inc., Chicago, IL, USA). Differences in proportions and means were assessed by χ2 and Student's t test, respectively. Linear regression methods were used to model variables associated with IES-R score.
RESULTS
Questionnaires were mailed to 1950 eligible participants, of which 38 (1·9%) were returned due to a wrong/changed address. Of the remaining 1912 eligible participants, 1057 returned the completed questionnaire for a response rate of 55·3%. Another 85 persons (4·4%) refused to participate and eight persons (0·4%) removed the survey identifier and were excluded from analyses.
The mean age of respondents was significantly higher than non-respondents [49·2 years (s.d.=15·7), and 42·7 years (s.d.=14·1), respectively, P<0·001]. Otherwise, study respondents were comparable to non-respondents with respect to sex, SARS phase, exposure type and type of quarantine (Table 1). Subsequent analysis to examine the independent effects of type of quarantine and HCW status demonstrated that type of quarantine did not provide additional information above HCW status. As a result, no further analysis is presented on type of quarantine.
Table 1. Comparison of SARS quarantine study respondents (n=1057) to non-respondents/refusers (n=855)

* Includes co-workers, household, travel and other.
Study respondents self-reported their duration of quarantine to be significantly longer than that maintained in the DRHD database [8·3 days (s.d.=3·1, range 2–30 days) vs. 5·2 days (s.d.=2·2, range 2–10 days), respectively] (P<0·001).
Most respondents 81·8% [n=819, 95% confidence interval (CI) 79·4–84·2] correctly identified that quarantine had been imposed to protect the community (Table 2). The use of quarantine restrictions to protect members of their household was less understood (48·3%, n=470, 95% CI 45·2–51·4). Less than two-thirds correctly reported that quarantine would not protect themselves (56·6%, n=555, 95% CI 53·5–59·7). A ‘correct rationale’ variable was created to identify respondents who answered correctly to all three questions on reasons for quarantine. Only 21·9% (n=225, 95% CI 19·4–24·4) of respondents correctly identified all rationale-based questions.
Table 2. Understanding the rationale, compliance and difficulties associated with quarantine among SARS study respondents (n=1057)
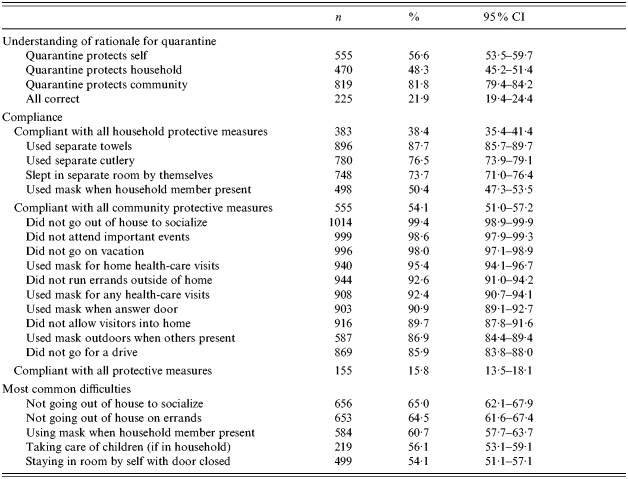
Compliance with quarantine behaviours varied from 50·4% (used mask while household members present) to 99·4% (did not attend social events) (Table 2). The proportion of respondents who reported complying with all household protective measures was 38·4% (n=383, 95% CI 35·4–41·4). Compliance with all community protective measures combined was higher at 54·1% (n=555, 95% CI 51·0–57·2). Combining all behaviours, compliance was reduced to 15·8% (n=155, 95% CI 13·5–18·1).
Grouping ‘quite a bit’ and ‘extremely’ difficult, the most difficult activity for respondents to comply with was not going out of the house to visit friends, family or attend other social activities (65·0%, n=656, 95% CI 62·1–67·9%) (Table 2). For subsequent analysis, the scores for each question were assumed to be ordinal and summed to calculate a ‘mean difficulty score’.
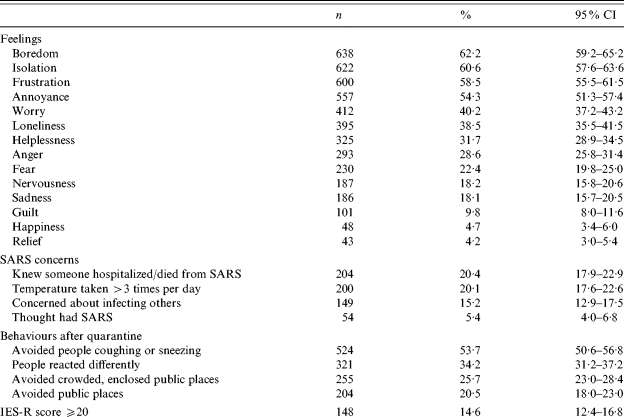
Indicators of the psychological impact associated with quarantine are shown in Table 3. Of the feelings experienced during quarantine, boredom (62·2%, n=638, 95% CI 59·2–65·2), isolation (60·6%, n=622, 95% CI 57·6–63·6), and frustration (58·5%, n=600, 95% CI 55·5–61·5) were most commonly reported. Some respondents expressed other psychological concerns including fears about infecting others, being infected themselves and/or avoidance behaviours people and places after quarantine (Table 3).
Table 3. Psychological impact associated with quarantine among SARS study respondents (n=1057)

IES-R, Impact of Events Scale – Revised.
The mean IES-R score was 8·9 (s.d.=13·7, range=0–82) (Table 3). An IES-R score of at least 20 was found for 14·6% of respondents (n=148, 95% CI 12·4–16·8). This cut-point was used to enable comparison with Hawryluck et al. [Reference Hawryluck9]. For the three domains, respondents reported a mean score of 0·5 for avoidance (95% CI 0·4–0·5), 0·4 for intrusion (95% CI 0·4–0·5) and 0·4 (95% CI 0·3–0·4) for hyperarousal. This corresponds to the response anchors of ‘not at all’ distressing for all domains [Reference Weiss, Marmar, Wilson and Keane12].
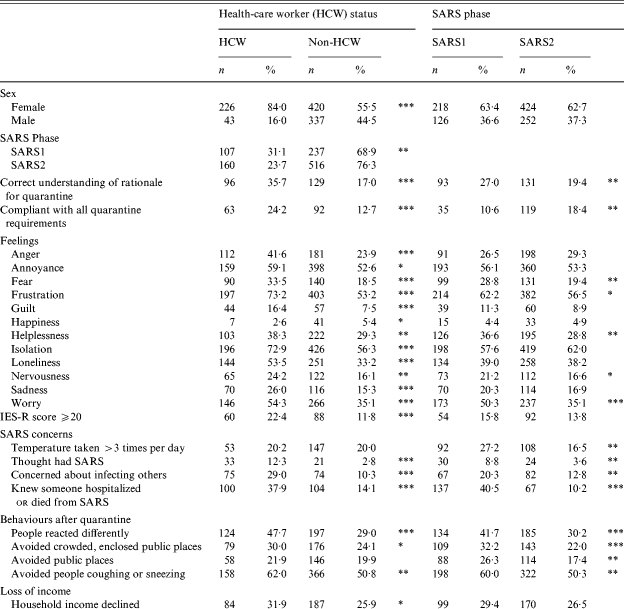
The analyses stratified by HCW status and SARS phase are summarized in Table 4. Only variables that showed a significant difference in either of these strata are shown. In addition, summary variables to indicate overall compliance, correct rationale, and mean difficulty score were used in place of individual questions. Compared with non-HCW, HCW were significantly younger, female, had correct understanding of the rationale for quarantine, were more compliant, felt greater stigmatization (i.e. people reacted differently), exhibited avoidance behaviours, lost income and were consistently more impacted psychologically.
Table 4. Comparison of SARS quarantine study respondents by health-care worker status and SARS phase (n=1057)

IES-R, Impact of Events Scale – Revised.
* P<0·05
** P<0·01
*** P<0·001.
By SARS phase, SARS2 respondents had significantly higher mean number of days in quarantine (self-reported and DRHD quarantine database), were less likely to be HCW, had less understanding of quarantine rationale, improved compliance, less SARS concerns, less stigmatization, less avoidance behaviours and reported less helplessness, nervousness and worry (Table 4). No difference between respondents in SARS1 and SARS2 was observed for IES-R (mean or individual domains).
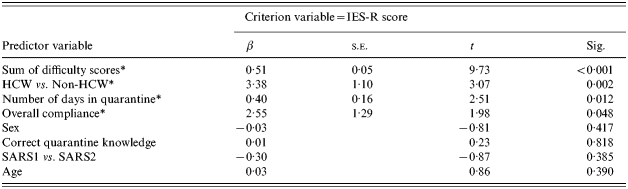
Statistical modelling was conducted to determine the variables offering the best fit for IES-R score. Based on correlation analyses, the following variables were evaluated to determine their contribution to increasing IES-R score: sex, age, correct rationale, HCW status, compliance, SARS phase, number of days in quarantine and difficulty score. Using stepwise linear regression methods, a significant model was produced (F 4,745=35·57, P<0·001 adjusted R 2=0·16) and included increasing difficulty (β=0·51, P<0·001), HCW status (β=3·38, P=0·002), self-reported longer duration of quarantine (β=0·40, P=0·012) and compliance with SARS quarantine requirements (β=2·55, P=0·048) (Table 5).
Table 5. Stepwise multiple linear regression analysis for IES-R score
IES-R, Impact of Events Scale – Revised; HCW, health-care worker.
Reduced model: F 4,745=35·57, P<0·001 adjusted R 2=0·16.
* Variables included in reduced model.
DISCUSSION
The results of this study confirm and expand our limited knowledge about the impact of quarantine [Reference Hawryluck9, Reference Blenden10] and raise important concerns regarding the effectiveness and applicability of quarantine in modern society.
The primary purpose of quarantine is to prevent transmission of an infectious agent from those potentially incubating disease. The quarantine requirements following exposure to SARS were designed to minimize transmission to the community as well as to protect household members. We now know that SARS CoV is transmitted primarily through contact and droplet spread, and rarely via airborne routes, from symptomatic individuals [Reference Booth14]. However, this knowledge was not available during the SARS outbreak, and quarantine was a public health measure imposed to minimize transmission while waiting for the natural history and epidemiology of the disease to be characterized. As evidence mounted that the agent did not transmit until symptom onset, quarantine served the need for early identification of persons with potential symptoms of SARS and the implementation of isolation precautions.
Early in the Toronto-based outbreak, mildly ill SARS cases were known to continue to work and/or circulate in the community, putting others at risk [Reference Svoboda15]. By late March 2003, quarantine became the hallmark of community control for SARS in Ontario. Asymptomatic contacts of potential SARS cases were required to remain quarantined for 10 days after their last exposure, or until SARS had been ruled out for their index case. Daily monitoring for symptoms allowed rapid and safe medical assessment to be initiated. In Toronto and Durham Region, on average 100–160 people were quarantined for each case of SARS, and another 7–8 people were investigated as a result of suspicious symptoms [Reference Svoboda15].
To be effective in preventing transmission to the community and within households, adhering to the SARS quarantine requirements was thought necessary. In a telephone survey of the general public in Toronto, Blenden et al. [Reference Blenden10] found that 97% would agree to quarantine should they be exposed to SARS. The difficulties encountered with the implementation of quarantine as observed here demonstrate the limitations of such hypothetical agreement. Based on self-report, we show that compliance with all requirements was low (15·8%, 95% CI 13·5–18·1), suggesting that quarantine in its current form would be of limited effectiveness in controlling transmission. Household members would be particularly at risk since only 38·4% (95% CI 35·4–41·4) of respondents reported compliance with all household requirements, the least compliant being appropriate mask use. Compliance with quarantine requirements that would be effective in preventing community transmission was significantly higher at 54·1% (95% CI 51·0–57·2) (P<0·001). While compliance with each requirement was high (>85%), overall almost half (45·9%) were non-compliant, potentially putting their communities as risk.
Over 44% of participants thought that they were placed into quarantine in order to protect themselves from developing SARS. Yet, compliance was significantly higher when respondents correctly identified the rationale for quarantine, were HCW, or in SARS2. This suggests that compliance can be improved, probably through improved knowledge about the relevant disease and ensuring a greater understanding of the rationale for quarantine measures. It is possible, however, that the knowledge that quarantine would not protect the quarantined person from SARS could negatively affect compliance. Owing to the high volume of persons on quarantine and the changing knowledge of SARS at the time, the capacity for in-depth education was unavailable. Simple instructions as to the quarantine requirements were developed as shown in Appendix 1 and supported by the daily telephone contacts by public health staff. Other information on SARS, particularly in the media early in SARS1, was limited and sometimes contradictory. By SARS2, more information on SARS (e.g. seriousness, infectiousness) and the need for quarantine were available through the media, websites and the scientific literature and this could have affected participants' decision to comply. Should quarantine measures be found necessary in future, methods to improve the rapid delivery of information, and other methods to improve compliance need to be explored. This could include early and well publicized web-based information, focused messages, surge capacity within public health and health-care responders, early and enhanced involvement of volunteer agencies, and even more coercive measures such as the use of quarantine facilities, compliance hotlines and/or the immediate issuance of legal orders.
Respondents' perceived difficulty with complying with individual requirements of quarantine differed from their reported compliance. For example, not going out of the house to visit others for social reasons was the most commonly cited difficulty; almost every respondent, however, was compliant with this behaviour. Thus, behaviours that quarantined persons may find difficult may not affect actual compliance. While compliance may have been related to concerns about being recognized as breaching quarantine, no placards or other notification was imposed on the individual. Hence, the respondent's quarantine status would only be known if the respondent had informed others of their status.
Beyond the potential community protective effects attributed to quarantine, the risks to the quarantined individual need to be identified. This study demonstrates wide-reaching effects that may be associated with quarantine. Over one-quarter of respondents reported a loss of household income, even though the provincial government sought to offer compensation to eligible persons in quarantine. Loss of income, however, was not significantly associated with overall compliance (P=0·916) and was not a significant predictor of psychological distress as measured by the IES-R regression model.
Overall, perceived increased difficulty, perceived longer time in quarantine, HCW status, and increased compliance were associated with increased PTSD symptoms as measured by higher IES-R scores. Although the response anchors of the three subscales of the IES-R indicated that quarantine was ‘not at all’ distressing, significant differences in IES-R were found within HCW status for all subscales, mean total IES-R score and the ⩾20 cut-point. Compared to Hawryluck et al. [Reference Hawryluck9] who reported 28·9% of respondents scoring at least 20 on the IES-R, we found increased PTSD symptomatology in 14·6% (95% CI 12·4–16·8). These differing results may be attributable to methodological differences and the increased proportion of HCW respondents in the Hawryluck study population. Further, our study included a larger number of respondents, used a cohort approach and may be more representative of all quarantined individuals than the self-selected internet sample used by Hawryluck et al. [Reference Hawryluck9].
The consistency of the psychological impact on HCW is evident and is probably influenced by the higher level of distress experienced by HCW coping with SARS in general [Reference Nickell16]. Here, HCW were more likely than non-HCW to know someone who was hospitalized or died from SARS. Thus, quarantined HCW may have recognized greater personal risk as a result of close contact with SARS patients and/or had more experience/knowledge regarding the severe end of the SARS clinical spectrum. To our knowledge, all exposed HCW were quarantined, thus it is not possible to compare the experiences of quarantined vs. non-quarantined exposed HCW. It should be noted, however, that not all HCW had the same intensity of risk nor familiarity with SARS and these potential confounders were unable to be measured or controlled in the analysis. Overall, therefore, while HCW consistently reported more frequent adverse psychological impacts than non-HCW, their experience was probably influenced by their job-related experiences with SARS and not unique to their HCW status.
Comparable data on the psychological impact of SARS within the non-quarantined general population is limited and incomplete. The Rapid Risk Factor Surveillance System (RRFSS), a monthly random-digit-dial telephone survey of adults aged ⩾18 years conducted by the Institute for Social Research at York University, surveyed 569 Durham Region residents from 23 April to 10 July 2003 [17] on the impact of the SARS outbreak. Excluded were 2·6% respondents who had been quarantined themselves or had another household member hospitalized or quarantined for SARS. A total of 22% (95% CI 18–25%) of RRFSS respondents reported nervousness or worry about SARS. Although methodologies differed between RRFSS and the study reported here, quarantined respondents from our study reported 40·2% (95% CI 37·2–43·2) for worry and 18·2% (95% CI 15·8–20·6) for nervousness. These limited data are suggestive that quarantined individuals experienced greater psychological impacts than the general population.
There are several limitations to this study. Although several strategies were undertaken to optimize survey completion, the response rate was 55% and younger persons were under-represented. For all other variables reviewed here, however, respondents were representative of the population of quarantined residents. Information was not collected on socioeconomic details such as education and household income which would be helpful in planning future educational requirements with respect to quarantine. However, the cohort of eligible quarantined persons was included and, with the exception of age, was representative of the quarantined population based on factors available for analysis. Analysis by the number of quarantined household members and household composition was not possible for this study. Excluded were persons who developed symptoms that were investigated for SARS since their follow-up and experiences would have differed. The study was completed 1–4 months from quarantine to completion of the study questionnaire. Given the rapid changes in knowledge about SARS during these months, recall may have been affected and could impact on reported differences observed between SARS1 and SAR2. Also, data on compliance are self-reported, and validation of self-report was not available. The cover letter and voluntary self-administered mailed questionnaire method attempted to reassure participants that confidentiality would be maintained and alleviate their concerns about responses acknowledging non-compliance. Moreover, a focus on individual behaviours during quarantine was hoped to limit social desirability responses, although there was no way to validate responses. Lastly, the lack of knowledge on the impact of quarantine encouraged an exploration of the multiple impacts that quarantine may have had. As a result, multiple comparisons may increase the likelihood of reporting a type-I alpha error. The consistency and direction of the statistical results, however, support the interpretation that important clinical and significant differences exist.
CONCLUSIONS
Responding to the SARS outbreak using quarantine as a primary community control measure resulted in a significant cost to scarce public health resources [Reference Svoboda15, Reference Schabas18]. The results of this study suggest that the implementation of quarantine requires evaluation. Should the health system be faced with the re-emergence of SARS or another novel transmissible infectious disease and quarantine measures are being contemplated, several considerations as identified in this study should be addressed. These include providing a clear rationale to quarantined individuals, minimizing the duration of quarantine, and paying special attention to high risk groups (e.g. HCW and persons immediately affected by the disease). In addition, quarantine, in its present form, requires further research as to its utility for arresting transmission in the community and household settings, particularly for disease that could be transmitted prior to symptom onset. Revised requirements and improved preparation/education of those placed into quarantine may better limit the psychological impact of the quarantine experience.
APPENDIX 1. Home and work quarantine requirements, SARS outbreak, 2003
A. Home quarantine
(i) Wear a mask when you are in contact with any family member(s).
(ii) Take temperature twice a day. Please record your temperatures. We will phone daily.
(iii) Sleep in a separate room.
(iv) Use a separate bathroom, if available.
(v) Use separate towels and utensils. Clean as per usual.
(vi) Do not have any visitors to your home.
(vii) Do not go to community activities (functions, shopping, etc.).
(viii) If need to walk your dog, use your backyard only. It is not necessary to wear mask if you are alone in your backyard but have a mask with you to put on if someone comes into your yard.
(ix) If you develop any symptoms contact: ‘the Durham Region Health Department’.
B. Work quarantine
Work quarantine was only available for health-care workers and health-care facility workers during SARS2 and required approval by the Durham Region Health Department:
(i) You can continue to work at the hospital that you were exposed in as long as you remain well. You will be screened with a symptom check and have your temperature checked before beginning work.
(ii) When driving to work, you should be alone in a private vehicle.
(iii) While at work, you must wear a mask at all times and practice diligent hand hygiene. You must eat in a separate room from everyone else if at all possible. If not possible, stay at least 2 metres away from others while eating.
(iv) Do not enter another hospital site except as authorized by the Medical Director or administrator of the second site.
(v) If you have an office in the community and are in quarantine, and if absolutely necessary, essential patients can be seen in your office; defer all non-essential patients. All office staff, including the exposed person, must wear a mask at all times and practice diligent hand hygiene.
(vi) When not at work, you must follow home quarantine requirements.
(vii) If you develop any symptoms contact: ‘the Durham Region Health Department’.
APPENDIX 2. Impact of Events Score – Revised (IES-R) [Reference Weiss, Marmar, Wilson and Keane12] to assess the SARS quarantine experience
Respondents were asked to score their responses to the following questions on a scale of 0–5 where:
0=Not at all
1=A little bit
2=Moderately
3=Quite a bit
4=Extremely.
Below is a list of difficulties people sometimes have after stressful life events. Please read each item, and then indicate how distressing each difficulty has been for you during the past seven days with respect to your SARS quarantine experience. How much were you distressed or bothered by these difficulties?
1. Any reminder brought back feelings about it.
2. I had trouble staying asleep.
3. Other things kept making me think about it.
4. I felt irritable and angry.
5. I avoided letting myself get upset when I thought about it or was reminded of it.
6. I thought about it when I didn't mean to.
7. I felt as if it hadn't happened or wasn't real.
8. I stayed away from reminders of it.
9. Pictures about it popped into my mind.
10. I was jumpy and easily startled.
11. I tried not to think about it.
12. I was aware that I still had a lot of feelings about it, but I didn't deal with them.
13. My feelings about it were kind of numb.
14. I found myself acting or feeling like I was back at that time.
15. I had trouble falling asleep.
16. I had waves of strong feelings about it.
17. I tried to remove it from my memory.
18. I had trouble concentrating.
19. Reminders of it caused me to have physical reactions, such as sweating, trouble breathing, nausea, or a pounding heart.
20. I had dreams about it.
21. I felt watchful and on-guard.
22. I tried not to talk about it.
The Intrusion subscale was calculated based on the mean item response of items 1, 2, 3, 6, 9, 14, 16, 20. The Avoidance subscale was the mean item response of items 5, 7, 8, 11, 12, 13, 17, 22. The Hyperarousal subscale was the mean item response of items 4, 10, 15, 18, 19, 21.
DECLARATION OF INTEREST
None.







