Background
Social isolation is considered to be a foundational aspect of life course processes of aging and which reflects the absence of social engagement and social connectedness within family, friendship, and community social networks. It is commonly defined as being of a low quantity and quality of contact with others, and considers the number, types, and quality of social network contacts, feelings of belonging, a sense of engagement with others, and related attributes (Courtin & Knapp, 2015; National Seniors Council, 2014a; 2014b; Nicholson, Reference Nicholson2009; Toepoel, Reference Toepoel2013).
These multifaceted social dimensions have gained attention in the gerontological literature, given serious public health concerns arising from connections between social isolation and several components of health-related quality of life. These include increasing risk of mortality as well as a range of physical and mental health morbidities, including psychological well-being and quality of life (Courtin & Knapp, 2015; Harasemiw, Newall, Shooshtari, Mackenzie, & Menec, 2017; Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; National Seniors Council, 2016; Wister et al., Reference Wister, Coatta, Schuurman, Lear, Rosin and MacKey2016). Furthermore, social isolation has been linked to lower access to, and less effective, health care utilization in older age (Newall, McArthur, & Menec, Reference Newall, McArthur and Menec2015). Although researchers have used a number of measures to estimate social isolation, there is a lack of conceptual and methodological clarity and consistency of their use and interpretation in the literature, especially between social isolation and loneliness (see Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Valtorta, Kanaan, Gilbody, & Hanratty, Reference Valtorta, Kanaan, Gilbody and Hanratty2016). Based on a multidimensional conceptual model that integrates social isolation and loneliness, our study sought to develop a composite social isolation index using available measures in the Canadian Longitudinal Study on Aging (CLSA).
Estimates of the prevalence of social isolation and loneliness have been characterized as having significant variation, depending on the population under study, measures, and survey type. According to the 2008/2009 Canadian Community Health Survey, approximately 16 per cent of seniors have felt isolated from others often or some of the time (Statistics Canada, 2010). Reported loneliness appears to be higher among older individuals, especially the very old, and older women. For instance, 24.7 per cent of women aged 65–74, and 30.8 per cent of those aged 75 and older (compared to 17.9% of men aged 65-74, and 19.4% of men aged 75 and older), felt lonely some or all of the time (using the CES-D single loneliness item), based on analyses of the 2010–2013 baseline CLSA data (Wister & Menec, Reference Wister, Menec, Raina, Wolfson, Kirkland and Griffith2018). However, the prevalence of persons who are chronically isolated and/or chronically lonely is considerably lower, approximately 10 per cent reporting being directly affected by high levels of social isolation (Kirkland et al., Reference Kirkland, Griffith, Menec, Wister, Payette, Wolfson and Raina2015; Kobus-Matthews at al., 2010; National Seniors Council, 2014b). Chronically isolated or lonely individuals have an increased risk of experiencing the deleterious effects of these conditions.
Specifically, social isolation has often been broadly divided into objective structural elements of one’s social network, such as number of contacts, size, and density, as well as functional elements pertaining to more qualitative aspects of social interactions, such as the types and amount of social support experienced and their qualitative assessment (Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016). Early definitions of social isolation also differentiated it from loneliness (Weldrick & Grenier, Reference Weldrick and Grenier2018). Whereas social isolation pertains to the objective social contacts in an individual’s social network, loneliness is the subjective perceptions and reactions that individuals have to their environment and relationships, and the perception that intimated social needs are not being met (Newall & Menec, Reference Newall and Menec2017). Thus, social isolation and loneliness are not interchangeable. For example, a person with moderate social connections may feel lonely; conversely, an individual who is socially isolated may not feel lonely because they prefer this arrangement. This is consistent with research showing a weak-moderate association (r = .21) between social isolation and loneliness measures in an older population (Coyle & Dugan, Reference Coyle and Dugan2012).
However, this objective versus subjective distinction has been challenged over recent years, in part because subjective feelings often accompany an absence of social interaction (Pettigrew, Donovan, Boldy, & Newton, Reference Pettigrew, Donovan, Boldy and Newton2014; Weldrick & Grenier, Reference Weldrick and Grenier2018; Zavaleta, Samuel, & Mills, Reference Zavaleta, Samuel and Mills2017). Indeed, Weldrick and Grenier, (2018, p. 78) state that, “definitions began to move away from defining social isolation as entirely objective or subjective, and towards the development of multi-pronged definitions that included objective and subjective dimensions.” Thus, objective and subjective dimensions of social isolation (including social network and loneliness components) are intertwined (Pettigrew et al., Reference Pettigrew, Donovan, Boldy and Newton2014), do not necessarily completely overlap (Nicholson, Reference Nicholson2009), and may be well-suited for inclusion within a composite index.
Another reason why the perception of loneliness can be conceptually connected to social isolation is that loneliness and isolation share many precursors and outcomes (Alspach, Reference Alspach2013; Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016; Wister & Menec, Reference Wister, Menec, Raina, Wolfson, Kirkland and Griffith2018). For instance, both are important correlates of health and well-being in middle and later life, albeit to different degrees, including mental health, frailty and chronic illnesses, and mortality, as well as life satisfaction and happiness (Courtin & Knapp, 2015; Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; Holt-Lunstad, Smith, Baker, Harris, & Stephenson, Reference Holt-Lunstad, Smith, Baker, Harris and Stephenson2015; de Jong Gierveld, Keating, & Fast, Reference de Jong Gierveld, Keating and Fast2015; National Seniors Council, 2016; Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Wister & Menec, Reference Wister, Menec, Raina, Wolfson, Kirkland and Griffith2018). Thus, whereas both social isolation and loneliness have been linked to health and well-being among older adults, it is unclear which aspect is most important, hence the need for tools that take both into account as well as separately.
Research into the predictors and outcomes of social isolation and loneliness has been challenged not only by conceptual and measurement complexity, but also by contextual factors. For instance, there is a higher likelihood of chronic social isolation and/or chronic loneliness among the most vulnerable older adults, who are typically not examined or not well-represented in surveys. With respect to correlates and outcomes, there is evidence that social isolation and loneliness are associated with several socio-demographic factors: advanced age; widowhood; living alone; low education, income, or poverty; and not having children. In addition, persons experiencing isolation over long periods include those with episodic or lifelong physical and mental health issues (including seniors with Alzheimer’s disease or other related dementias, frailty, sensory loss, or multiple chronic illnesses); those older adults having immigrant and/or ethnic status, or seniors who are lesbian, gay, bisexual, or transgendered; caregivers with heavy burden; and those living in rural or remote areas and who often experience challenges relating to technology (costs, literacy, comfort) including telephone systems, computers, and social media (de Jong Gierveld et al. Reference de Jong Gierveld, Keating and Fast2015; Kirkland et al., Reference Kirkland, Griffith, Menec, Wister, Payette, Wolfson and Raina2015; National Seniors Council, 2014a, 2014b, 2016). Thus, contexts under which social isolation or loneliness is associated with risk and protective factors are multifaceted, and may be elucidated through the use of new measures of social isolation (Zavaleta et al., Reference Zavaleta, Samuel and Mills2017).
Although individual measures of social isolation and loneliness may be appropriate for certain research questions, other research may be enhanced by using a multi-level composite social isolation measure that combines both subjective and objective dimensions.
Conceptual Framework for a Social Isolation Composite Measure
Valtorta et al. (Reference Valtorta, Kanaan, Gilbody and Hanratty2016) have developed a framework for assessing social isolation and loneliness measurement tools. In a systematic review of measures, the authors identified 54 instruments (see Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016: Table 1, pp. 4–5). Individual items of all measures were assessed and mapped according to two dimensions: structure versus function (vertical axis), and degree of subjectivity of the questions in the scale (horizontal). Structural social isolation refers to objective elements, such as the social network linkages (marital status, number and type of people with whom one interacts, size and density of social network, etc.). Functional elements refer to the qualitative and behavioural beneficial components that are the result of interactions between people and which are shaped by the quality, quantity, and type of social support given or received (emotional help, instrumental or tangible assistance, companionship) (Harasemiw et al., 2017; Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016).
Table 1: Descriptive statistics and mapping scores for social isolation index variables, outcomes, and co-variates (n = 21,491)

Equations to Calculate CLSA Social Isolation Index
Structural Objective (SO) Equation:
Community Participation Items (a + b + c + d + e + f + g + h) / 8 = A
Social Network Items (i + j + k + l + m + n + o + p) / 8 = B
Last Time Visited Items (q + r + s + t + u) / 5 = C
Living Alone (v) = D
Marital Status (w) = E
(A + B + C + D + E) / 5 = SO
Functional Objective (FO) Equation: (x + y + z + ∞) / 4 = FO
Functional Subjective (FS) Equation: (α + Ω) / 2 = FS
CLSA-SII Social Isolation Total Scale: (SO + FO + FS) / 3
The second dimension is the degree to which items are objective or subjective. Questions asking about the number of family or friends that they see over a period of time is on the objective end of the spectrum. Subjective questions ask about the availability, adequacy, and feelings associated with the social relationships, in that order. Overall, most instruments with primarily structural social isolation items tend to be more objective; those that are more functional range between objective and subjective. This results in three primary combinations of these two dimensions; however, some instruments capture multiple domains along these continuums. Examples of commonly used instruments that fall within the three primary domains include these four: (a) structural, objective: the Berkman-Syme Social Network Index (Berkman & Breslow, Reference Berkman and Breslow1983); (b) functional, objective and subjective items: Medical Outcomes Study (MOS) Scale (Sherbourne & Stewart, Reference Sherbourne and Stewart1991); (c) functional, subjective: 11-item de Jong Gierveld Loneliness Scale (de Jong Gierveld et al., Reference de Jong Gierveld, Keating and Fast2015); and (d) both structural and functional, objective and subjective items: 11-item DUKE-UNC Functional Support Inventory (Powers, Goodger, & Byles, Reference Powers, Goodger and Byles2004).
The positioning of commonly used social isolation, loneliness, or social support scales according to these two dimensions can help to identify key content areas for a composite social isolation index. Most surveys typically provide other indicators, such as individual items embedded in other scales, or other indicators/variables, that capture the three primary domains located along these two dimensions. Given the breadth and potential of the Canadian Longitudinal Study on Aging (CLSA), the present study provides a rationale for a composite index of social isolation based on CLSA measures that cover three of the four primary domains in the Valtorta et al. (Reference Valtorta, Kanaan, Gilbody and Hanratty2016) conceptualization framework. These include (a) structural social isolation with objective measurement; (b) functional social isolation with objective measurement; and (c) functional social isolation with subjective measurement. There is no scale covering both structural and functional objective and subjective domains together; therefore, we did not include this domain.
Methods
Design and Sample
This research utilized a subset of the baseline wave of the CLSA data set. Launched in 2010, this 20-year panel study of persons aged 45 to 85 has been funded primarily by the Canadian Institutes for Health Research (CIHR), Canada’s federal granting agency for health research. Data collected at baseline included biological, clinical, psychosocial, and societal information that influence disease, health, and well-being (Raina et al., Reference Raina, Wolfson, Kirkland, Griffith, Oremus, Patterson and Brazil2009). The CLSA participants were randomly selected and invited to participate from the population aged 45 to 85 (excluding those living in institutional full-time military, persons living on federal First Nations reserves, and the three northern territories), resulting in a total sample of 51,338. The sampling method is the same as that used by Statistics Canada for its Canadian Community Health Survey (CCHS) – Healthy Aging 2008/2009 survey, and included participants from that study in its recruitment, supplemented with Provincial Health Registries, telephone sampling using random digit dialling, and the Quebec Longitudinal Study on Nutrition and Aging. The sample contains weights to adjust for sampling error and to produce a sample that is representative of the targeted Canadian population (Raina et al., Reference Raina, Wolfson, Kirkland, Griffith, Oremus, Patterson and Brazil2009).
The present research used all persons aged 65 and older (n = 21,491; mean age 72.87, 53.5% women) drawn from the CLSA full baseline data (n = 51,338), since follow-up data were not available. The full CLSA sample included a tracking cohort and comprehensive cohort. The tracking cohort received telephone interviews from one of four computer-assisted telephone interview sites across Canada. Comprehensive participants were randomly selected within age/sex strata from within 25 km of dense population data sites, or within 50 km of data collection sites in areas with a lower population density. Participants for this cross-sectional data set initially completed a face-to-face interview at home with a data collector who utilized a laptop-computer-assisted interviewing instrument. After this home interview, participants would visit their local data collection site in order to undergo additional computer-assisted interviews and clinical assessments. The 11 data collection sites for the CLSA were located in Victoria, BC; Vancouver, BC; Surrey, BC; Calgary, AB; Winnipeg, MB; Hamilton, ON; Ottawa, ON; Montreal, QC; Sherbrooke, QC; Halifax, NS; and St. John’s, NFLD.
Sample weights were used to correct for sampling error by age, gender, and geographic location for the combined data set. The independent and dependent variables had minimal (under 3%) missing cases. Missing data for these variables were list-wise deleted in the analyses.
Measures
Social Isolation Index Measures and Standard Scoring
A number of measures were available to develop the Social Isolation Index using the Canadian Longitudinal Study on Aging (CLSA-SII), representing combinations of structural-functional and objective-subjective dimensions of social isolation and loneliness. Frequencies and descriptive statistics are shown in Table 1.
Structural, Objective Variables
Several different structural areas of the social network have been included in prior measures and research among older adults. Research has established that engagement in a diverse social network that entails not only the structural elements of the number and frequency of seeing family and friends, living arrangement, and marital status, but also connections to the wider community environment, affects health and well-being as people age (Harasemiw et al., 2017; Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Zavaleta et al., Reference Zavaleta, Samuel and Mills2017). We selected five domains of variables (numbered 1 to 5 in the list below) from the CLSA that fall within the structural, objective dimension. These are presented beginning with the broader network structure (community participation, network size, and frequency of contact) and moving to the narrower network structural elements (living arrangement and marital status).
(1) Domain 1: Eight separate variables measuring Frequency of Community/Social Participation were included, using frequency of participation in each over the past 12 months. The eight activities reported in the CLSA data set include those identified as sport; religious, volunteer or charity work, clubs or fraternal, educational or cultural, neighbourhood associations, other recreational, and family/friends outside of the home. The response set included at least once a day, at least once a week, at least once a month, at least once a year and never.
(2) Domain 2: Number of network members (counts) in eight separate network nodes were included in this domain (number of close friends, number of neighbours, number of people known through other activities, number of people known through community involvement, number through work or school, number of living biological and step children, number of siblings, and number of relatives).
(3) Domain 3: Network member visits included responses to the last time that the participant saw people outside of the household from the following five network groupings: children, siblings, other relatives, friends, and neighbours. The response set included those within the last day or two, within the last week or two, within the past month, within the past 6 months, within the past year, and more than 1 year ago.
(4) Domain 4: Living arrangement was dichotomized into alone/not living alone, given the importance of living on one’s own for social isolation.
(5) Domain 5: In this domain, marital status was dichotomized from “single, never married or never lived with a partner”, “married/living with a partner in a common-law relationship”, “widowed”, “divorced”, and “separated” into a binary variable with “married/common-law” and “non-married/non-common-law” categories.
Functional, Objective Scale with Four Subscales.
A number of social support scales have been developed to tap into the functions that different types of social support performs for individuals in the areas of health and well-being, especially as individuals age (Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; Holt-Lunstad et al., Reference Holt-Lunstad, Smith, Baker, Harris and Stephenson2015; National Seniors Council, 2016). It is well-established in the social support literature that the frequency of contact or other structural network characteristics do not directly measure the quality of contact or relationships, since some contact can be negative. Therefore, measures that reflect functional aspects of support are also needed, and may indeed interact with, or perhaps be more important, than structure alone (Fuller-Iglesias, Reference Fuller-Iglesias2015). It is also recognized that social support is multidimensional and ranges from affective to instrumental types (Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016).
The Medical Outcome Study (MOS) Social Support Survey Scale (Sherbourne & Stewart, Reference Sherbourne and Stewart1991) is an objectively measured scale with four subscales that was used to capture this domain in the CLSA. This measure is one of the most commonly used instruments that falls in the functional domain using items that fall more closely into objective types. The MOS consists of 19 items measuring social support along four internal subscales: emotional/informational support, affectionate support, tangible support, and positive social interaction. Emotional/informational items ask whether a person has someone to listen and to advise them in crisis situations. Affectionate support items ask whether a person has someone to love and/or who loves them. Tangible support items ask a respondent about whether they have someone who can help them if sick, and/or to help with daily chores such as preparing meals. Positive social isolation items ask whether the respondent has someone with whom they can have fun, and engage in enjoyable leisure activities. Each question in the scale (items shown in Table 1) ranges from 1 (none of the time) to 5 (all of the time), where higher scores indicate greater levels of social support. We used the four separate subscales in order to measure each of these functional social support types on the composite social isolation index (see scoring below).
Functional, Subjective Measures.
Loneliness scales have been used to capture a functional, subjective domain of social isolation and social support. Perceptions of loneliness have been shown to lower health-related quality of life, health status, and health care utilization among older adults (Courtin and Knapp, 2015; Coyle and Dugan, Reference Coyle and Dugan2012; de Jong Gierveld et al., Reference de Jong Gierveld, Keating and Fast2015; Kobus-Matthews et al., Reference Kobus-Matthews, Barr, Jackson, Ziegenspeck, Jiwani, Easlick and Lok Chow2010; Valtorta et al., Reference Valtorta, Kanaan, Gilbody and Hanratty2016). The only available loneliness measure in the CLSA was based on a single item from the Center for Epidemiological Studies Depression Scale (CES-D) (Radloff, Reference Radloff1977) that assessed how often a participant felt lonely over the past week. The response set ranged from “all of the time, 5–7 days”, “occasionally, 3–4 days”, and “some of the time, 1–2 days” to “rarely or never, less than 1 day”. Participants were also asked a functional, subjective question if they wanted to participate in more activities, allowing for a second measure tapping into this domain. Finally, another functional, subjective measure, Desire to Participate in More Activities, was a constructed with a yes, no response set.
In order to standardize different types and distributions of social isolation measures, we employed a mapping system (converting all measures into scores between 0 and 10), which has been used as a normalization procedure for a multimorbidity resilience composite measure (Wister et al., Reference Wister, Lear, Schrumann, MacKey, Mitchell, Cosco and Fyffe2018) and the development of a successful aging index (Cosco, Stephan, & Brayne, Reference Cosco, Stephan and Brayne2015). As detailed in Table 1 (see mapping values), we converted ordinal measures by dividing the number of responses into 10 proportionately. For example, a 5-point Likert ordinal scale (1 to 5) would be converted to 0, 2.5, 5, 7.5, and 10, from low social isolation to high. We used the same method for the 19 individual Likert response items contained in the four MOS subscales, but divided by 19 to retain a 10-point range. Continuous measures (number of network members in each type) were divided by a divisor that converted the lowest value into 10 (highest social isolation) and highest to 0 (lowest social isolation) consistent with the index. Note that there were different maximum values for each of the different membership numbers (children 0–20, siblings 0–50, relatives 0–100, friends 0–90, and neighbours 0–90), which required different divisors as shown in Table 1. The dichotomous variable (desire to participate in more activities) was coded as 0 and 10, where some desire was coded as 10 and no desire as 0, again resulting in a score of 0–10.
In order to standardize the three social isolation dimensions, the scores for all sub-index variables were summed and divided by the total to convert into a 0–10 scale. Equations showing calculations for the sub-indices as well as the total CLSA-SII appear at the bottom of Table 1. Thus, for the four domains in the structural, objective dimension, we added the individual converted scores and divided by the total number (resulting in an average with a range of 0–10). This weighted each of the four domains equally within the functional objective dimension. The domains were then added and divided by four to create a single 0–10 score for the structural, objective dimension. Similarly, after combining the converted individual item MOS subscale scores into their respective subscales (emotional/informational support, affection support, tangible support, and positive social interaction), we added and divided these by four resulting in a 0–10 score. Finally, we added the two dichotomous converted scores for the functional, subjective dimension (loneliness and desire for more activities) and divided by two in order to produce a 0–10 score. Finally, these three-dimension scores were added and divided by three to create the single CLSA-SII composite score (0–10). Higher scores indicated greater social isolation levels for all variables.
Concurrent Validity Outcome Measures
We assessed the concurrent validity of the CLSA-SII with the following four measures: life satisfaction, depression score, perceived health, and perceived mental health (see Table 2). We selected these on the basis of extensive literature establishing their association with social isolation (Courtin & Knapp, 2015; de Jong Gierveld et al., Reference de Jong Gierveld, Keating and Fast2015; Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; Stringhini et al., Reference Stringhini, Berkman, Dugravot, Ferrie, Marmot, Kivimaki and Singh-Manoux2012; Zavaleta et al., Reference Zavaleta, Samuel and Mills2017). The Diener Satisfaction with Life Scale (Diener, Emmons, Larsen, & Griffin, Reference Diener, Emmons, Larsen and Griffin1985) ranges from 5 to 35 with higher scores indicating greater life satisfaction. Individual questions range from 1 (strongly disagree) to 7 (strongly agree). We measured depression using the CES-D Scale. It ranges from 0–30 and contains 10 questions on specific depression symptoms such as hopefulness, appetite, loneliness, concentration, and so on. Each question has possible answers from 0 (rarely or none of the time, less than 1 day) to 3 (most or all of the time, 5–7 days). Since loneliness is included in the CLSA-SII, and is one of the 10 items in the CES-D, we removed it, resulting in a scale comprising the 9 remaining items.
Table 2: Descriptive statistics for outcome variables and co-variates (n = 21,491)
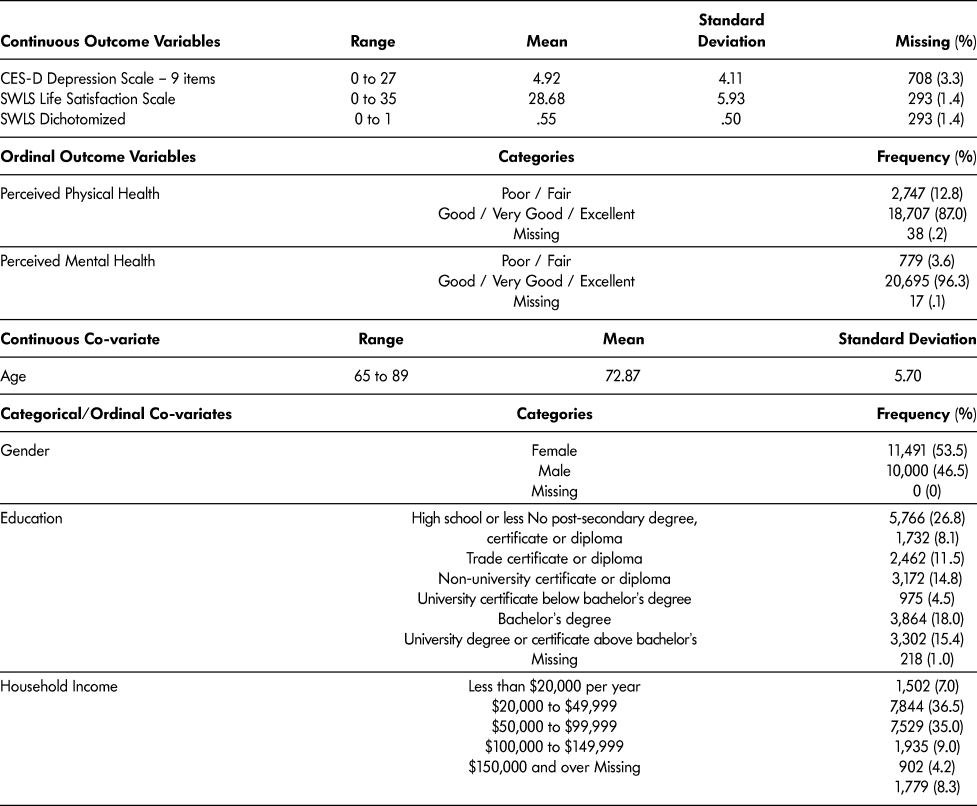
This measurement strategy has been used in other research on social isolation using the revised CES-D scale (Cacioppo, Hawkley, & Thisted, Reference Cacioppo, Hawkley and Thisted2010). The removal of a single item in the CES-D scale has been shown to have a minimal effect, although comparisons to research using the original CES-D should be made with caution. Perceived health was based on the single item question “how would you rate you your health?” We dichotomized answers for this question into fair/poor (0) and good/very good/excellent (1) for the logistic regression analysis. Similarly, perceived mental health was based on the single item question “how would you rate you your mental health?” This was also split into fair/poor (0) and good/very good/excellent (1).
Co-variates
Given the importance of several socio-demographic correlates of social isolation, we adjusted for the effects of age, gender, education level, and total household income in logistic and linear regression analyses. As shown in Table 2, the age variable ranged from 65 to 86. Gender was a dichotomous variable. The education level variable was assessed as to the highest degree, certificate, or diploma the participant had obtained. Because of the small number of categories, we dummy-coded this variable with the level “no-post-secondary degree, certificate or diploma” as the reference category. The other categories included “education below bachelor’s: trade certificate or diploma”, “bachelor’s degree”, and “university degree or certificate above bachelor’s degree” included as well. Total household income was also dummy coded with the level “less than $20,000” as the reference category, with “$20,000 to $49,999”, “$50,000 to $99,999”, “$100,000 to $149,999”, and “$150,000 or above”. Frequencies and descriptive statistics are presented for the outcome variables and co-variates in Table 2.
Data Analyses
Initial examination of the continuous life satisfaction variable indicated that it was heavily skewed beyond the point of reasonable transformation, and the structure of the residual/fitted values violate assumptions for ordinary least squares regression. We therefore converted the Life Satisfaction Scale into a dichotomous variable based on the categorization as originally recommended by Diener et al. (Reference Diener, Emmons, Larsen and Griffin1985). The higher value measured higher levels of life satisfaction. We performed logistic regression analyses for the Life Satisfaction Scale as well as the dichotomized Likert scale outcome measures (perceived health and perceived mental health), in order to assess associations with the CLSA-SII, adjusting for the socio-demographic variables. We used linear regression techniques for the CES-D scale. Odds ratios (OR) (with 95% confidence intervals), and significance levels are presented for the logistic regression analyses, with both unadjusted and adjusted models. Unstandardized beta coefficients (with 95% confidence intervals), standardized beta coefficients, and significance levels (unadjusted and adjusted) are reported for the linear regression.
Results
CLSA Social Isolation Index Patterns
The descriptive statistics for the CLSA-SII for the full sample resulted in a mean of 2.86 and standard deviation of 1.55. Social isolation, as measured by the CLSA-SII, was found to be higher among older males than older females (M = 3.10, SD = 1.57; and 2.60 and 1.48 respectively). In addition, the CLSA-SII was higher among the very old. Among those aged 65–74, the mean was 2.74, with a standard deviation of 1.53; among those aged 75 and over, the mean was 3.06, with a standard deviation of 1.56. These patterns are similar to those found in other studies based on selected individual measures of social isolation and loneliness using the CLSA (Wister & Menec, Reference Wister, Menec, Raina, Wolfson, Kirkland and Griffith2018).
Regression Analyses of Social Isolation Index
Table 3 shows a moderate inverse association (OR = .61±.01, p < .001) between the CLSA-SII and life satisfaction, both for the unadjusted model and adjusting for the effects of age, gender, education level, and total household income. Given that this association is inverse, the odds ratio represents a .61 (OR) factor decrease in the probability of reporting high levels of life satisfaction compared to low levels for each unit change in the CLSA-SII, with odds ratios falling between unity (1) and zero for negative coefficients (not shown here). In order to make comparisons with additional outcome measures in other studies that may entail positive associations (e.g., depression, stress, etc.), it is useful to also represent our results as odds ratios based on equivalent coefficients, but positive in direction. The inverse odds ratio (.61) is equivalent to a 1.64 OR (rounded) when converted into a positive association, indicating that the likelihood of reporting low levels of life satisfaction compared to high levels (reversed) is increased by 1.64 for each unit change in the CLSA-SII.
Table 3: Logistic and linear regression for CLSA-SII on life satisfaction and health outcomes, adjusting for age, gender, education, and income (n = 17,769)
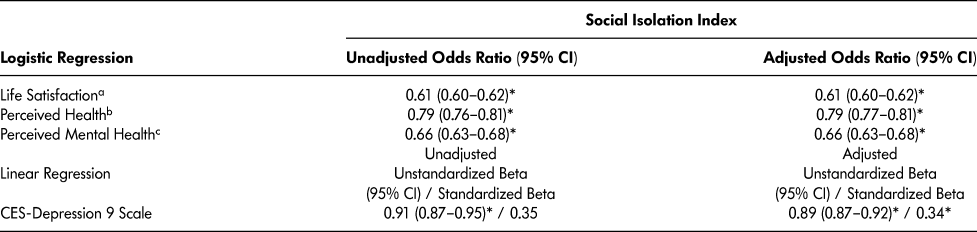
* p < .001.
a Categorized as per Diener et al. (Reference Diener, Emmons, Larsen and Griffin1985), with higher values indicating greater levels of life satisfaction.
b Grouped into fair/poor (0) and good/very good/excellent (1).
c Grouped into fair/poor (0) and good/very good/excellent (1).
CI = Confidence interval.
We also observed an inverse moderate association between the CLSA-SII and perceived health (OR = .81±.03, p < .001), in both unadjusted and adjusted models. The probability of reporting good-excellent perceived health, compared to poor-fair, is decreased by a factor of .81 for each unit change in the CLSA-SII. When converted to a positive association, this is equivalent to an odds ratio of 1.23.
A similar association emerged for CLSA-SII and perceived mental health (OR = .66±.03, p < .001), again for unadjusted and adjusted conditions. The likelihood of reporting good-excellent perceived mental health, compared to poor-fair, is decreased by a factor of .66 for each unit change in the CLSA-SII. This odds ratio based on an inverse association can be represented in positive form, which equates to 1.50 odds ratio factor change.
Turning to the linear regression results of the nine-item CES-D depression scale (loneliness item removed), we found a moderate association for the unadjusted model with the CLSA-SII (standardized beta = .35, p < .001), as well as the adjusted model (standardized beta = .34, p < .001). The unstandardized coefficients and 95 per cent confidence intervals are reported in Table 3.
Overall, these results show good concurrent validity of the CLSA-SII. It should be noted that odds ratios (for life satisfaction, perceived health, and perceived mental health outcome variables) of this magnitude for the CLSA-SII, which we scaled with an interval range of 10, are very strong, since they reflect unit change in the dichotomous-dependent variable. Similarly, the beta coefficients associated with the depression measure are also moderate in strength. In addition, the replication of these results in both the unadjusted and adjusted models indicates that the index is not affected by socio-demographic conditions.
Discussion
The topic of social isolation has received increasing attention in the gerontological literature, given rapid population aging and growing public health concerns arising from identified associations between its various measures and mortality and morbidity (Courtin & Knapp, 2015; Harasemiw et al., 2017; Leigh-Hunt et al., Reference Leigh-Hunt, Bagguley, Turner, Turnbull, Valtorta and Caan2017; National Seniors Council, 2016). However, research has been limited by the highly variable conceptualization and measurement of this concept, which limits comparability. Research has established that social isolation is a multifaceted concept that captures the quantity and quality of social contact and interactions with others, including structural aspects of one’s social network, functional social support components, and subjective feelings of loneliness and the desire to have greater social connections.
In an effort to develop a composite index of social isolation, specifically based on the CLSA, we employed Valtorta et al.’s (Reference Valtorta, Kanaan, Gilbody and Hanratty2016) unique two-dimensional framework for assessing social isolation and loneliness measurement instruments. The two dimensions entail structural-function and objective-subjective continuums. The 24 measures used for the CLSA-SII were selected to represent three of the four measurement domains falling along the two axes of the framework. Given the different measurement, and unequal number of measures in each domain, we employed a mapping method of standardization used in other composite index development (Cosco et al., Reference Cosco, Stephan and Brayne2015; Wister et al., Reference Wister, Lear, Schrumann, MacKey, Mitchell, Cosco and Fyffe2018), and weighted these equally.
The CLSA-SII was regressed on four key outcome variables: (a) life satisfaction scale, (b) a nine-item version of the 10-item CES-D depression scale (omitting the loneliness item), (c) perceived mental health and perceived health, and (d) the adjusted key socio-demographic factors of age, sex, education, and household income. The logistic and linear regression results supported moderate statistically significant associations in the expected directions. Although the available literature focusing specifically on social isolation and/or loneliness and similar outcome variables among older adults is sparse, there are some useful comparative studies.
Based on 5-year cross-lagged data from the United States’ Chicago Health, Aging and Social Relations Study (ages 50–68 at starting period), Cacioppo et al. (Reference Cacioppo, Hawkley and Thisted2010) found a weak-moderate inverse association (r = –.17, p < .05) between social network size and the CES-D 20-item scale (loneliness item removed) at baseline. The authors uncovered a similar strength association (positive) between loneliness and depression, after adjusting for co-variates. In comparison, the CLSA-SII was shown to have a stronger association with the CES-D (loneliness removed) (standardized beta = .34, p < .001).
In a study of older adults using the U.S. National Social Life, Health, and Aging Project of community-based older adults, Cornwell and Waite (Reference Cornwell and Waite2009) examined the effects of social disconnectedness and perceived isolation on both self-rated physical and mental health. Social disconnectedness was measured using a scale of eight items capturing the number and lack of connectedness to a variety of social network members; loneliness was measured using a nine-item scale including perceptions of loneliness and perceived lack of social support. Social disconnectedness and loneliness demonstrated independent weak-moderate associations with dichotomized measures of self-rated physical and mental health, net of socio-demographic co-variates. The odds ratios for social disconnectedness were .72 and .83 for self-rated physical and mental health respectively (controlling for age, gender, education, race, partner status, co-morbidities, and loneliness) (Cornwell & Waite, Reference Cornwell and Waite2009). These are very similar to the magnitude of the odds ratios (.81 and .66 respectively) in our study using the CLSA-SII on self-rated physical and mental health, using identical dichotomous categories, after adjusting for socio-demographic co-variates. Cornwell and Waite (Reference Cornwell and Waite2009) also found a similar weak-moderate association for their loneliness measure on self-rated physical health, but a stronger one for self-rated mental health than uncovered for their disconnectedness measure.
Taken together, this research suggests that the CLSA-SII can be used with confidence in future studies, which is important since the number and variation of social isolation indicators pose methodological challenges to researchers, such as over-specification of models and collinearity among independent variables. The development of the CLSA-SII allows for additional research into social isolation that can be used in the CLSA. Furthermore, the CLSA-SII provides an easily replicated comprehensive measure with proven outcome concurrent validity and does not appear to be influenced significantly after adjusting for key socio-demographic variables, indicating psychometric properties that can be directly compared across studies. For example, approximately 75 per cent of the measures used in the CLSA-SII were identified in the well-known U.S. Health and Retirement Study, which include variables that represent the same three social isolation dimensions used in our study.
A number of limitations of this research can be identified. First, the CLSA-SII is constrained by the available measures of social isolation available in the data set. While the index is comprehensive, there may be other potential measures and conceptual framing of the index. Second, the development of similar measures in other surveys may not have an identical set of measures, thus limiting its reproducibility as we have discussed. Third, the assessment of concurrent validity focuses on four outcome variables and can be extended to others. Finally, the use of baseline CLSA data restricted the testing and interpretation of our results based on the CLSA-SII.
Future research needs to examine the usefulness of this measure in comparative research, such as similar index development using other major surveys. Another issue is the need to employ longitudinal data to address the bidirectionality of social isolation and its protective, risk, and outcome factors. For example, social isolation can attenuate well-being and quality of life in old age and heighten levels of depression, resulting from the separation of individuals from their informal social networks, community supports, and health care systems. Alternatively, persons experiencing poor psychological health can separate themselves from important support networks and associated supports which, if harnessed, could actually alleviate these conditions. In addition, longitudinal data would allow for examination of changes in trajectories of social isolation and those associated with significant health transitions in old age (e.g., multimorbidity, mental health, and well-being, as well as health care utilizations) (Wister, Levasseur, Griffiths, & Fyffe, Reference Wister, Levasseur, Griffiths and Fyffe2015). It is hoped that the CLSA-SII will generate new research in the growing and timely field of social isolation among older adults.





