INTRODUCTION
Hepatitis A is a viral disease which has a worldwide distribution. It has an incubation period of, on average, 28 days (range 15–50 days) [Reference Koff1]. Hepatitis A virus (HAV) infection is usually asymptomatic in young children [Reference Hazarika2]. Most outbreaks of hepatitis A have been linked to consumption of uncooked contaminated foods, or contaminated water [Reference Wheeler3–Reference Bloch7].
Improved sanitation in many parts of the world, including in China, has left a growing proportion of school-aged children and young adults susceptible to HAV, and these are the age groups that are most typically affected by HAV outbreaks in middle-income countries [Reference Heymann8]. As a result of this increase in susceptibility, hepatitis A vaccination in children has been conducted in China since the 1990s. In parallel with this the risk of HAV infection has been in sharp decline [Reference Xu9].
On 29 May 2011, the Center for Disease Control and Prevention of county M in Anhui province, China, found on an increased number of pupils with hepatitis A at an elementary school in a rural township with 86 000 residents. This was a day school with 42 teachers and 698 pupils. After preliminary investigations, it was confirmed as an outbreak and reported through China's Public Health Emergency Response Information System (PHERIS). Anhui province introduced HAV vaccine in routine childhood immunization in 2006; however, all of the cases in this outbreak were children born before 2006 who had not received the free vaccination. Based on data from the notifiable diseases reporting system in China, there were only five (sporadic) cases of hepatitis A reported in the township during 2004–2010; and all cases had been adults aged >25 years. The cluster hepatitis A symptomatic cases in children therefore received considerable public attention.
A social network in an outbreak is a set of actors (that ‘play a role’ in the transmission of an infectious agent, such as persons, places and other ‘objects’ such as an animal reservoir) together with the links that connect them in an infectious disease outbreak. The links are epidemiologically relevant interactions between the persons, places and any other actors involved [Reference Klovdahl10]. By the use of social network diagrams we were able to reconstruct an outbreak network and quantify the relative importance of the different actors that played a role in the outbreak. In community outbreaks, especially in rural areas where isolating and identifying pathogens is difficult, the use of social networks may help both to determine epidemiological links between cases and to identify the possible source of the infectious disease outbreak. The network method was used in this study to map possible sources and routes of transmission in affected children.
METHODS
Case definition and case identification
A clinical case of HAV infection was defined as a pupil or staff member with onset of jaundice or debility between 7 May and 6 June 2011 with elevated alanine aminotransferase (ALT) of more than double the normal upper limit. A confirmed case of hepatitis A was defined as an acute illness with clinical symptoms compatible with a clinical case plus the presence of IgM antibody to HAV. Cases were identified on the basis of reports from laboratories and physicians.
A comprehensive questionnaire was administered to all class teachers in the school and general practitioners of township hospitals in order to identify additional cases. Historical reports of HAV in this county were also investigated.
Epidemiological investigation
General investigation
A standardized questionnaire was developed for information collection. The children with symptoms of hepatitis were interviewed by members of the investigation team. For younger children who might not be able to answer the questions accurately on their own, the children's mothers (or guardians) were interviewed alongside the children. Questions focused on: (1) general information: sex, age, school grade, classroom, home village; (2) clinical information: onset and duration of illness, symptoms, date of hospitalization; (3) potential risk factors: sources of water consumed, school activities, food consumption, personal hygiene habits and contact with other symptomatic individuals. These contacts (cases) were defined as having an epidemiological link to another case, for which a detailed investigation was conducted through the contact and social network investigation.
Contact and social network investigation
A hepatitis A case was considered to have an epidemiological link if there was known contact with another case or if the case was a member of the identified social network. Face-to-face interviews of available cases (or with help from their guardians) were conducted to establish links. The epidemiological link was defined as a close relative or friend/classmate. Particular attention was paid to contacts who lived together, shared food or used the same tableware between cases and contacts. Contact tracing records were reviewed to discover if there was a common source.
Case-control study
An unmatched case-control study was conducted at the elementary school. All pupils who met the clinical case definition were included and controls were selected using stratified random sampling from all classes of the school. Controls were excluded if they had a history of hepatitis A or had received hepatitis A vaccine. Serum samples of controls were subjected to the serum antibody test and those who were positive for HAV IgM or IgG were also excluded. The same questionnaire, with the exception of clinical information, was used for interviewing controls. All participants gave informed consent to participate in this study.
Environmental investigation
Further investigation also included the school's water supply system (potable water and well water) and possible problems during the month prior to the epidemic. Potable water and well water specimens and snacks sold in grocery stores near the school were sampled for HAV detection using reverse transcription–polymerase chain reaction (RT–PCR) [Reference Nainan11].
Statistical analysis
Epi Info v. 3.5.4 (CDC, USA) was used to record data and R v. 2.15.3 (R Foundation, Austria) for statistical analysis. We described the distribution of cases by age, sex, school grade, classroom, and village. The χ 2 test was used to analyse the outcomes. The package ‘igraph’ of R was used to draw the social network diagrams.
Each individual case and control was shown as a node in the network, connected to other nodes via a line which depicted the status of their links, i.e. relative or close friend/classmate, without directionality. Univariate analysis was performed calculating odds ratios (OR) and 95% confidence intervals (CI) for individual exposures in the case-control study. Variables statistically significant at P < 0·1 in univariate analysis were included in a multiple logistic regression model. In the latter model, an association was considered statistically significant when P < 0·05.
RESULTS
Clinical and epidemiological characteristics of the patients
A total of 28 cases which occurred between 7 May and 6 June 2011 met the clinical case definition and were confirmed by serological testing. Symptoms of the 28 patients were typical for HAV infection (see Table 1). All cases were pupils aged 7–13 years. The attack rate was 4·0% (28/698). Male pupils had a higher attack rate (5·8%) than female pupils (1·3%). Cases were found in all grades, distribution of cases did not cluster within grades (χ 2 = 10·266, P > 0·05, see Table 2). Grades 1–3 had a statistically significant higher attack rate than grades 4–6 (6·2% vs. 1·5%, P = 0·002). Nine out of 14 classes had hepatitis A cases with a median attack rate of 3·7% (range 1·9–16%). Compared to the baseline of hepatitis A in county M (Table 3), this cluster was confirmed as an outbreak.
Table 1. Symptoms of hepatitis A for cases, Anhui province, China, 2011
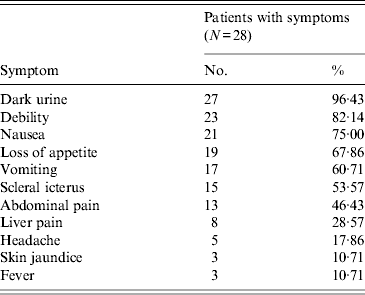
Table 2. Attack rate by grade, class and sex in hepatitis A outbreak, Anhui province, China, 2011
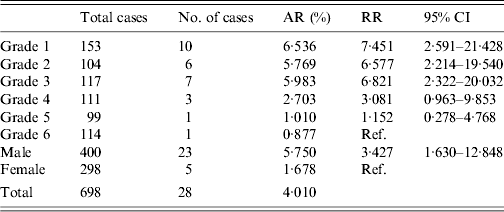
AR, Attack rate; RR, risk ratio; CI, confidence interval.
Table 3. Case numbers and incidence rate of hepatitis A in county M (1991–2010)
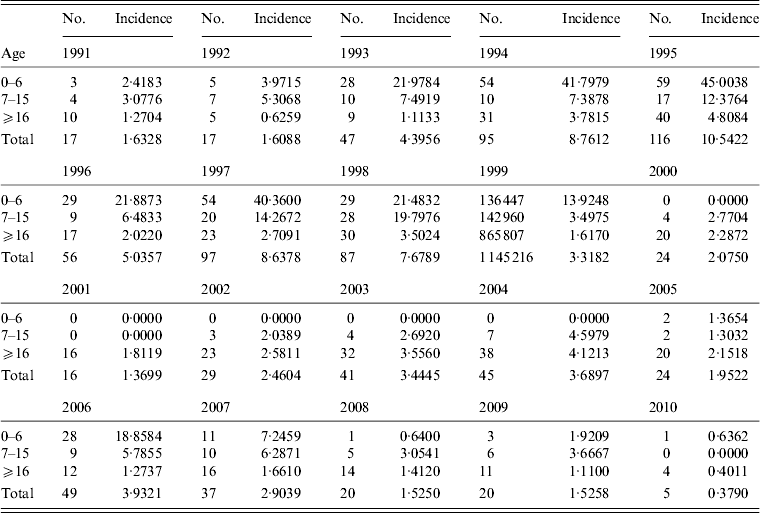
Social network analysis to identify a source patient
Contact tracing and network investigation was used in the outbreak for purposes of source-case determination. Based on the network derived from interviews of cases in the outbreak, a cluster of three pupils (CA01, CA02, and CA03, with previous clinical cases onset on 23, 30 March and 10 April, respectively) were found to connect to all but three cases through direct contact or a shared social setting (Fig. 1). These included two girls (cousins, CA01 and CA03) living together and one boy (CA02) who was their neighbour. Further interview of the three cases linked them to another 4-year-old boy (boy A, onset on 13 March). Boy A's family had rented an apartment from the cousins' family to run a noodle restaurant from November 2010, and moved away after the boy had developed symptoms of hepatitis. Neither boy A nor his family were able to be found for interview. Social network analysis had identified boy A as the most probable source case. The evidence from the social network diagram enhanced the growing confidence that this hepatitis A outbreak in the elementary school was a typical human-to-human transmission.

Fig. 1. Network diagram of hepatitis A outbreak in an elementary school, Anhui province. Different-sized circles indicate (from large to small) boy A (red), the three primary cases before the outbreak (yellow), the outbreak cases (purple), controls (grey) and close contacts of the cases (green), respectively. Numbers in the circles indicate the number of days since onset of symptoms for boy A. The large pink arrow indicates the most likely source case suggested by the network structure. Heavy lines indicate links between clinical cases; light lines connect cases and their close contacts, e.g. family members, classmates or friends.
Adding the previous cases into the epidemic curve, the shape of the epidemic curve appears compatible with a propagated spread, especially when the curve was drawn by individual class. It showed that the three cases disseminated HAV to the other pupils who subsequently developed symptoms (Fig. 2). Five of nine first cases in each class in this outbreak were all close contacts of the three initial cases. They were family members, neighbours, friends playing together, or classmates sharing the same desk. As the virus spread, cases started to increase and reached its peak in the week of 26 May.

Fig. 2. Date of illness onset for hepatitis A cases (n = 32), in an elementary school, Anhui province, March–June 2011. The red bar indicates boy A, who had symptom onset on 10 March; green bars indicate the three primary cases that were found by the network investigation; the blue bars indicate cases identified during the outbreak. The dates are the onset dates of the four previous cases.
Risk factors of the hepatitis A outbreak indentified by the case-control study
The case-control study included 28 cases and 56 controls. The classmate controls had a similar age distribution (mean age 9·51 years, s.d. = 1·56) compared to cases (mean age 9·40 years, s.d. = 1·45, t = 0·3117; P = 0·7561 for t test). Males accounted for 73·2% (41/56) and 82·1% (23/28) of total controls and cases, respectively. Sex distribution was not significantly different in either group (P = 0·365).
During the 50 days (longest incubation period) before onset, 61% of cases were in close contact with other persons who had hepatitis symptoms compared to 16% of controls (OR 8·071, 95% CI 2·850–22·857). A well located near a toilet, containing non-potable water was also identified as a potential vehicle for transmission. Well water was consumed by 36% of cases compared to 14% of controls (OR 3·194, 95% CI 1·087–9·384). Living in villages Z or C was associated with increased risk for HAV infection (OR 3·059, P < 0·05). The risk for pupils who washed their hands before eating was significantly lower than that of pupils who did not (OR 0·289, 95% CI 0·111–0·753). Results of univariate and multivariate analysis are shown in Tables 4 and 5.
Table 4. Results of the univariate analysis (n = 84)
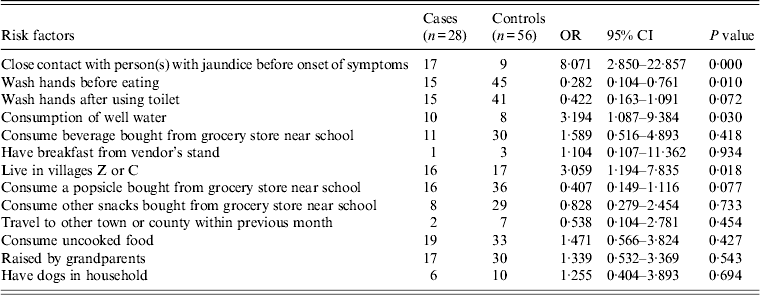
OR, Odds ratio; CI, confidence interval.
Table 5. Results of the multivariate analysis (n = 84)
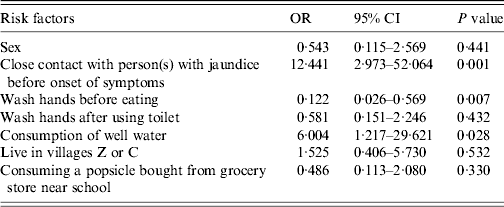
OR, Odds ratio; CI, confidence interval.
Of the six variables qualifying for inclusion in the multivariate analysis (see Table 5) three factors were significantly associated with hepatitis A infection. The strongest association was close contact with a person with jaundice (OR 12·44, 95% CI 2·97–52·06), followed by consumption of well water (OR 6·00, 95% CI 1·22–29·62). Washing hands before eating was associated with a low risk of hepatitis A infection (OR 0·122, 95% CI 0·026–0·569).
Environmental evidence and public health action taken
The purpose of the well near the toilet facility was for flushing the toilet and cleaning. Although being informed of the risks of drinking raw water several times, some students reported drinking well water occasionally. The well water was sampled on 30 May and returned a negative result by RT–PCR for HAV with no detectable total or faecal coliforms/100 ml. We suspected that the well water might be as a potential source; however, we were unable to obtain reliable environmental and laboratory evidences to support this. The water samples were tested about 2 months after the initial case became infected. The viability of HAV in water is probably considerably shorter than that length of time.
To prevent continuing infection, all the affected patients were isolated in the town hospital. Members of these cases' families and other close contacts were placed under medical observation at home. It was also recommended that pupils should take basic hygiene measures, with emphasis on washing hands before eating, especially when having snacks at school. No additional cases were reported that year following the interventions described above. As a precautionary measure, hepatitis A vaccine was administered to students aged 7–13 years in the surrounding villages.
DISCUSSION
Network analysis, as an appropriate approach to explore and understand structural and relational aspects of health, has been used primarily to study disease transmission, particularly sexually transmitted diseases [Reference Klovdahl10, Reference Krugman, Ward and Giles12]. In an outbreak investigation, social network analysis may visually illustrate links to explain secondary transmission and identify the pattern of spread. It played an essential role in identifying transmission patterns and possible source cases, especially where laboratory evidence was insufficient. In this outbreak social network mapping was used as a tool for an acute infectious disease outbreak investigation and to help target control measures. The result of the network analysis was confirmed by the case-control study and verified the propagating epidemic. It was a good example of using social network diagrams in the management of an outbreak.
Hepatitis A outbreaks occur worldwide, with most linked to contaminated food and water [Reference Lassen13–Reference Petrignani15]; however, there are limited published studies about outbreaks propagated through close contact [Reference Lim, Choi and Lee16]. Increasingly, school-aged children and young adults are susceptible for hepatitis A due to improved sanitation [Reference Heymann8]. The annual national incidence rate of hepatitis A in China was in sharp decline in the preceding decades [Reference Xu9]. Surveillance data suggested that the incidence rate of hepatitis A over the past two decades in county M shifted from intermediate to low endemic and has fallen to 5/100 000 since 2010. Only five adult sporadic cases of hepatitis A occurred in this township during 2004–2010, although it is suspected that infected children may be asymptomatic. In this outbreak of hepatitis A virus infection, all the victims were children aged 7–13 years. Younger children had a higher attack rate than older ones. This may be due to two reasons:
-
(1) Older children were more likely than younger children to have had prior infection. The sampling IgG-positive rate in asymptomatic children of grades 4–6 was slightly higher than that in children of grades 1–3, but the difference was not statistically significant (63% vs. 51%, P = 0·31). The attack rate may have been underestimated as non-susceptible children (IgG positive) were included. The real attack rate in older children might have been higher in the susceptible children without IgM than the attack rate found in younger children.
-
(2) We compared the hand-washing habits between younger and older students. It was showed that older students had better hygienic habits than younger students. Younger school-aged children, with less scrupulous hygiene, may have served as a source of infection and caused the cluster of cases of hepatitis A in grades 1–3 to be greater in grades 4–6.
The network mapping and elevated ORs suggest that the virus could be transmitted through close contact with an infectious person. From 2006, Anhui province introduced HAV vaccine in routine childhood immunization. In this outbreak, victims were born after 2006 (age range 7–13 years, median 9 years) and so were not under the Expanded Programme on Immunization (EPI) of China; moreover, few of them had received commercial vaccine. These individuals would be at high-risk of infection especially where poor sanitary conditions existed [17]; this created the possibility of an outbreak. Nearly 40% of cases did not recall close contact with jaundiced person(s). This may have been due to asymptomatic HAV infection in young children. Of the 144 selected pupils 53·5% had a positive IgG test result. While none of the children had received the HAV vaccination before, there was an indication that asymptomatic infection was common in the school children.
HAV is transmitted primarily by the faecal–oral route [Reference Krugman, Ward and Giles12]. Washing hands with safe water may reduce the spread of hepatitis A. Results from this case-control study re-confirmed this fact. Previous studies identified that HAV can remain infectious on the hands for more than 4 h and can be easily transferred from contaminated surfaces. The risk of illness was greater for people who did not routinely wash their hands when taking care of infants or people with disabilities [Reference Schwarz14, Reference Lim, Choi and Lee16, Reference Watson18]. A programme of health education targeted at primary students will help this group form good personal hygiene habits such as washing hands and should provide benefit beyond the current outbreak.
The epidemic curve reached a peak in the week of 26 May. The sudden, increasing of cases late in the outbreak may indicate a link to other sources. The case-control study also revealed that consumption of well water had a statistically significant association with hepatitis A in this outbreak. We suspected that the water may have been contaminated by cases early in this outbreak which led to a larger peak in cases later on. However, no laboratory evidence was found in the environmental investigation of the well water to support this association. The absence of laboratory evidence may be due to the viability of HAV in water. Confirmation of well-water sources through identification of HAV from the water has been reported previously [Reference Guthmann6, Reference De19]. In laboratory studies, >90% of HAV survived for >12 weeks in ground water or waste water at 5°C [Reference Sobsey20]. Nevertheless, in field epidemiological investigations, it is difficult to sample positive water. In our investigation, the well-water samples were tested about 2 months after the initial case onset. By this time the local CDC had already disinfected the well water to reduce the likelihood of future infections. Failure to sample the well water for HAV prior to it being disinfected was a limitation of our study. There was other evidence from the investigation that pupils who washed their hands more frequently had a lower risk of infection. This may rebut the speculation regarding water contamination, because as well water was the only source for washing, if it was contaminated those who used the water to wash their hands had the chance of becoming infected. The increased risk may also be confounded with other behaviours rather than well water itself. In addition, the three early cases were not confirmed cases since they had recovered before the outbreak was detected and this was a limitation of our investigation.
This outbreak could have been prevented if the three early cases of hepatitis A had been reported and isolated promptly. Those children who were in close contact with these cases could have received immunoglobulin soon after exposure, which might have prevented their illness as well as the subsequent transmission of HAV to others. Hepatitis A vaccine should also have been considered for the pupils of this school when the first three cases became sick, as this could have prevented the further spread of disease. However, the opportunity of vaccination to control this outbreak of hepatitis A. was missed, and because of the high positive rate of IgG we estimated, vaccination was not conducted in this school.
ACKNOWLEDGEMENTS
This study was supported by Avian and Human Influenza (AHI) Facility Grant No. TF012401 Capacity Building for Emerging Infectious Disease Preparedness and Response in China Project, which is administrated by the World Bank. The authors are most grateful to the staff of Anhui CDC and the trainees of CFETP for their contributions to this investigation. We acknowledge the EpiCentre of Massey University, especially Professor Mark Stevenson and Lachlan McIntyre, for their outstanding technical expertise and review. We thank Caroline Fyfe from the Centre for Public Health Research, Massey University, for her useful comments and language editing which has greatly improved the manuscript.
DECLARATION OF INTEREST
None.









