1 Introduction
Until recently, little attention has been paid to the treatment of child patients in eighteenth-century hospitals. Patient-focused studies have explored case records and others have investigated hospital admission records, but the primary focus has been on adult inpatients.Footnote 1 More recent work concerning children in eighteenth-century English provincial hospitals clearly demonstrates the presence of children in these charitable institutions.Footnote 2 These works articulate the common themes found in medical history and childhood studies, and how these fields, when examined together, can help demystify the interactions of poor child patients with the medical institutions of the eighteenth century.
Poverty was not static or absolute during the long eighteenth century and poor individuals might require varied forms of formal and informal social welfare during the course of their lives. In fact, individuals were likely to change financial status throughout their lives.Footnote 3 This life-cycle poverty has been addressed in the rich historiography of the poor law, revealing key points in individuals’ lives when the risk of financial crisis was highest, namely childhood, young parenthood, and old age.Footnote 4 Sickness or an accident could ‘[propel] people into poverty’ due to the combined effects of reducing their ability to work and requiring the immediate outlay of resources.Footnote 5 When faced with sickness, the poor had a variety of options available, including paying out of pocket for a practitioner’s expertise, consulting kin and neighbours, calling upon the membership of a Friendly Society for aid, applying to the parish for poor relief, or seeking admittance to a voluntary infirmary.Footnote 6 The question, according to Mary Fissell, is ‘why and how certain groups came to rely upon institutions to provide health care’, considering the variety of resources available.Footnote 7 Indeed, the voluntary hospitals did not operate in isolation; they stood against a complex backdrop of potential sources of medical advice and care. Parish relief under the Old Poor Law, spending on which grew steadily between 1696 and 1803, was ‘neither ineffective nor ungenerous’Footnote 8 and could provide money for births, medical practitioners’ services and burials.Footnote 9
Studies of poverty have been criticised for being ‘rarely concerned with the poor as subjects of their own stories’Footnote 10 and there is an increasing desire to bring attention to ‘the experiences of, responses to, and realities of their lives as individuals’Footnote 11 through a history-from-below approach. Institutional records for a delimited population, such as the hospital admittance records under scrutiny, capture individuals who represent a specific subgroup of London’s populace. Poor children’s dealings with the medical marketplace have previously been obscured since they were generally not the ones making primary decisions concerning their medical care and their reactions to their health care were not often recorded. This article is among the first to quantitatively investigate the hospital admission of children of the working poor in London, contributing insight into their interaction with the medical marketplace through a study of children admitted to the London Hospital.
This research probes a series of admission records from the London Hospital, a voluntary hospital in London, UK founded in 1740. These records provide a dataset with which to compare the child inpatient results described by Levene and colleagues, drawn from eighteenth-century English towns.Footnote 12 This article seeks to explore the following questions. First, for what medical or surgical conditions were children most commonly being admitted to the London Hospital? Second, on average how long were child inpatients spending in hospital? Third, what was the result of their inpatient stay? The admission records affirm the contemporary reputation of the London Hospital as a destination for trauma cases and illustrate the myriad risks to children’s health in eighteenth-century London, particularly the effects of traumatic injury.
2 General Hospitals in London
The eighteenth century saw the rise of the general hospital movement in England; this period has been nicknamed the Age of Hospitals.Footnote 13 London boasted seven general institutions, which provided approximately two thousand beds for the poor.Footnote 14 Four of these hospitals, the Westminster, St George’s, the London and the Middlesex, depended upon public donations and subscriptions to provide charitable care. The others, St Bartholomew’s, St Thomas’s and Guy’s, were independently endowed and could therefore survive without appealing to the public for donations.Footnote 15 These institutions were designed to treat the working poor, wage-labouring individuals who could not afford to pay for private medical care; they were expected to return to work following treatment.
Admittance criteria to these seven institutions were strict, and dictated that only individuals deemed ‘deserving’ or ‘worthy objects of charity’ could be treated.Footnote 16 In essence, the hospitals sought to treat those who could otherwise work in order to ‘[recover] future wealth potentially lost to the nation’.Footnote 17 Individuals seeking hospital admittance could only gain access if they were recommended by a hospital governor or subscriber (an individual who donated money to the hospital in exchange for the right to recommend annually a certain number of patients for treatment), unless they had suffered an accident.Footnote 18 Hospitals focused on the care of curable injuries and illnesses, discouraging the admittance of chronic cases or those deemed incurable; these would take up beds that could otherwise be used by patients suffering from acute maladies. The London Hospital, in its 1762 instructions to those recommending patients for admittance, explained clearly that
‘no woman big with child, no children under seven years of age (except in cases of compound fractures, amputations, or cutting for the stone [i.e., lithotomy procedure to remove bladder stones]) no persons disordered in their senses, or suspected to have Smallpox, Itch, or other infectious distempers, or who are judged to be in a consumptive, asthmatic, or dying condition’
were to be admitted.Footnote 19 The exclusion of children is critical, because juvenile individuals were certainly being accepted at English voluntary hospitals, all of which had similar strict admittance policies.Footnote 20
Specialist medical care for children in London was limited. The London Foundling Hospital, an orphanage, was established in 1739 and a dispensary for the infant poor was founded in 1769, but until the founding of the Great Ormond Street Hospital for Children in 1852, there were no institutions that specifically catered for children’s inpatient medical care.Footnote 21 Workhouses sometimes accepted pauper children with medical issues, including the infectious and chronic conditions frowned upon by voluntary hospitals, such as smallpox and fever diseases.Footnote 22
Children in London’s voluntary general hospitals have received insufficient attention by researchers, due to the fact that age was almost never recorded for inpatients. Intermittent admission and discharge records have survived for St Thomas’s Hospital with some admitted individuals labelled as ‘child’ or ‘infant’; from 1773 to 1796 children make up less than five per cent of all admissions and reasons for admission were rarely recorded.Footnote 23 Apothecary reports from the Middlesex Hospital (1760–4, 1771–8) record scattered cases of child inpatients admitted for fractures, burns, and scalds.Footnote 24 Further, there is evidence that some child patients received outpatient care and clinical consultation at St Bartholomew’s Hospital.Footnote 25 Inconsistently recorded reasons for admission limit the comparability of these records to those from the London Hospital, but they emphasise that children were on occasion being accepted at London’s voluntary general hospitals.
3 Child Patients at the London Hospital
The London Hospital, founded in 1740, was built facing Whitechapel Road, in east London. The hospital received its Royal designation in 1990 on its 250th anniversary. The hospital’s house committee admitted patients (excluding acute cases who could be admitted at any time) who arrived at the hospital with a governor’s letter of recommendation.Footnote 26 The London did not charge a burial deposit or ‘caution money’, a deposit paid upon admittance to cover the costs in the case of a patient’s death, probably making it a particularly attractive institution at which to seek medical care.Footnote 27
This research examined the surviving admission and discharge registers of the London Hospital. Registers from 1760, 1791, 1792, and the latter half of 1805 are extant and available for consultation.Footnote 28 The records for 1805 did not record the ages of the inpatients and were thus excluded. The London Hospital records provide information on the patient’s name, parish of abode, occupation, age, reason for admission, result of hospital stay and date of discharge. The three full years available allow for comparison within this institution. No case descriptions are available for the London Hospital, but casebooks from St George’s Hospital and death records from St Bartholomew’s Hospital covering the early nineteenth century were consulted and are used to illustrate some roughly contemporary experiences of children admitted to the London Hospital.
The total number of patients admitted to the London Hospital in the three years under investigation was divided into two groups: children thirteen and under, and those seven and under, following the framework used by Levene and colleagues in their study of provincial voluntary hospitals to allow for inter-hospital comparisons.Footnote 29 The average age of apprenticeship in children of the working poor was thirteen and this age is thus chosen as the terminus of childhood, though it is acknowledged that the differentiation between children and adults is a social categorisation that has changed through time.Footnote 30 The age of seven is important since the London Hospital specifically prohibited the admittance of children under this age.Footnote 31
Table 1: Number of child patients admitted to the London Hospital, 1760, 1791 and 1792.

Table 1 displays the total number of individuals, adults and children, admitted to the London Hospital in each year. Overall, the proportion of inpatients under the age of thirteen was low, ranging from 3.7 to 5.3 per cent; those under the age of seven constituted between 1.0 and 1.1 per cent of the inpatient population. These results are uniformly lower than those described by Levene and colleagues, despite the fact that the average inpatient cohort in this investigation was higher at 1192, compared with 928.Footnote 32 Anne Borsay’s study of the admission records from the infirmary at Bath between 1742 and 1752, where inpatient ages were recorded, also demonstrated a higher percentage of admitted children, with 8.72 per cent of all inpatients falling between the ages of 0 and 14.Footnote 33 The London Hospital results potentially reflect a stricter adherence to the hospital admittance guidelines in addition to the wide variety of medical options available to the parents of ill children in London: other voluntary general hospitals, dispensaries and alternative medical practitioners. Borsay and Mary Fissell, in her study of the Bristol Infirmary, compare the inpatient age groups with age structure data for England as whole, from Wrigley and Schofield’s population reconstruction of England.Footnote 34 They note that children are underrepresented in both the Bath and Bristol Infirmaries, a result also found at the London Hospital. Although there are inherent limitations present when attempting to apply broad population data as a comparative source to a geographically limited sample, it is interesting to note that between 1756 and 1796 (years chosen to encompass the available London Hospital admission records) an estimated 33.1–36.8 per cent of the residents of England were between the ages of 0 and 14 while only an average of 4.4 per cent of child inpatients at the London Hospital were between the ages of 0 and 13.Footnote 35 The Medical Register, compiled in 1783, indicates that in London alone there were 968 registered surgeons, apothecaries and physicians, though this total does not include the many alternative and fringe medicinal practitioners such as quacks, bone-setters and wise women.Footnote 36 In 1783 the English provinces had the ratio of one medical practitioner to 2224 people; London’s ratio was about three times better.Footnote 37 Outpatient care was provided by the dispensaries on a charitable basis; by 1800 there were twenty-one dispensaries in London alone, with a further twenty-two located in the rest of Britain.Footnote 38 Beyond hospitals, dispensaries and alternative practitioners, the independence of ill individuals was heightened by the publication of self-help tomes such as John Wesley’s Primitive Physick, which championed natural holism and cold water therapy, and William Buchan’s Domestic Medicine, which proposed a philosophy of health based upon hygiene and temperance and included descriptions of specific care for children.Footnote 39 These volumes, published in English rather than Latin to appeal to a literate lay medical audience, went through many editions, indicating the popularity of self-help. There was clearly a range of choice in London’s medical marketplace outside individuals’ family and community networks, in which the voluntary hospitals were only one option, if parents sought to seek health care for their children outside the home.
Table 2: Classification of diseases among child patients admitted to the London Hospital, 1760, 1791 and 1792.
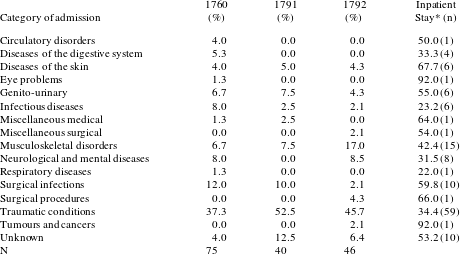
* Inpatient stay is the average number of days spent in hospital by those children who were eventually discharged as ‘cured’ or ‘relieved’ (recorded as n). Those who died, returned, or were removed from hospital before official discharge were not included in the average.
Table 3: Result of inpatient stay.
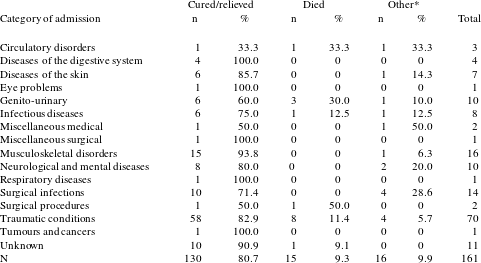
* Results in the ‘Other’ category included children who were removed from the hospital early, those labelled ‘went away with leave’, those who ‘won’t stay’ and those whose fate was labelled as ‘unknown’.
Table 2 summarises the reasons for children’s admission and the average inpatient stay at the London Hospital following the categories set out by Risse’s study of the admission records of the Royal Infirmary of Edinburgh, subsequently used by Levene and colleagues; the results of these inpatient stays are recorded in Table 3.Footnote 40 Traumatic conditions were the most common reason for admission each year and further detail is provided concerning this category in Table 4. Boys were consistently admitted more frequently than girls; boy inpatients made up an average of 63.4 per cent of the annual admissions for children. Levene and colleagues similarly noted that boys were more commonly admitted as surgical patients than girls, citing that potentially ‘boys and girls experienced different risks of injury and accident in their daily work and play; that they were treated differently by hospital authorities; or that parents distinguished between sons and daughters when seeking medical assistance’.Footnote 41 Previous studies have found more adult male than female inpatients, demonstrating the valuing of male labour and occupational hazards facing males during the long eighteenth century.Footnote 42 Further, removing women from their households was discouraged as a potential cause of familial instability, with eighteenth-century dispensary founders warning that their hospitalisation could lead to ‘dangerous consequences’.Footnote 43
Table 4: Details of traumatic condition category.

* Percentages may not total exactly 100% due to rounding.
The treatment of children, especially those explicitly prohibited, suggests that they were valued for their future labour potential.Footnote 44 This mercantilist view, that medical care for children through a paternalist hospital was an investment in future labour, is echoed in John Bellers’ 1714 treatise, stating that the early death of an adult labourer ‘may be accounted two hundred pounds loss to the kingdom’.Footnote 45 Children between the age of five, when they ‘achieved a degree of physical independence’, and apprenticeship were of particular concern; if they were to become disabled or otherwise unable to work during this time they were unlikely to achieve an apprenticeship and become viable workers.Footnote 46 It was therefore in the best interests of the hospitals, and by extension the nation, to accept children who arrived with conditions deemed treatable. This is not to suggest that parents did not feel concern and love for their children, a point that has been well established in the literature.Footnote 47 A sick child represented both a source of stress and a risk to his or her family’s financial situation. Wider social provisions for children in the form of parish poor relief – such as pensions, clothing, shoes and tools – and apprenticeships clearly ‘illustrate the perceived social value of the health of children’.Footnote 48 Emotional and economic investments were therefore both key factors in seeking medical care for a child. The goals of the hospital echoed those of the Old Poor Law – to ensure that the able-bodied were restored to their ability to work. Sickness and injury have been identified by scholars of the Old Poor Law as major drivers in the determination of poor relief.Footnote 49 Both the overseers of the Poor Law and the voluntary hospitals recognised that upfront costs for medical treatment represented long term investments in individuals who would, if restored to health, be less likely to require chronic care.Footnote 50
The vast majority of the child patients accepted at the London Hospital were registered as inhabitants of the eastern districts of London, such as Whitechapel, St George in the East, Spitalfields, Shoreditch, and Bethnal Green. This suggests that proximity to the hospital was a major factor in deciding to seek admission to the London Hospital. There are some interesting exceptions, however, where children were brought to the hospital from areas further afield. John Phipps, a thirteen-year-old boy from Datchworth, north of London, was admitted to the London with a diseased nose, and stayed as an inpatient for 113 days before being discharged as cured. Two children were admitted a day apart, 20 December and 21 December 1791, for the stone. This was an admittance allowed by the hospital’s policies, but it is interesting to note that these children, a labourer’s child and a farmer’s son, resided in Purleigh, Essex, located nearly forty miles north-east of the hospital. Clearly the desire for surgical intervention motivated the parents to bring the children to hospital, suggesting that the hospital may have been perceived as more trustworthy or professional than locally available practitioners. The boys’ ultimate fates differed drastically; one was cured and discharged fifty days after admittance, the other died eleven days following his admission. There is no information recorded as to whether or not the boys were ultimately cut for the stone, leaving tantalising, but unanswered questions about the medical care experienced by these children.
The range of illnesses and conditions affecting child inpatients was vast. Several admission classifications had low intake in all three years under study: the circulatory disorder group (comprising mostly dropsy cases), digestive system disorders (those with bloody flux – diarrhoeal disease – and worms), skin diseases (mainly scurvy and skin eruptions), eye problems, respiratory diseases, tumours and cancers, and miscellaneous categories. The majority of children in the genito-urinary category were admitted for the stone; musculoskeletal disorders included diseased and inflamed joints; and the majority of the surgical infections category comprised abscesses. Surgical procedures included two cases of amputation, one of which was successful and resulted in John Douglass, an eight-year-old boy from St George in the East, being discharged as cured after a stay of sixty-six days. The other case resulted in the death of seven-year-old William Messer, also of St George, after a stay of 102 days. Overall, categories with the highest intake mostly represent conditions that could be treated with medical or surgical interventions, similar to the results described by Levene and peers.Footnote 51 Interestingly, children were admitted with infectious disease (eight cases diagnosed as ‘fever’ or ‘ague’), though the average proportion of total cases (4.2%) is lower than in five of the six cohorts studied by Levene and colleagues.Footnote 52 The neurological category is, on average (5.5%), higher than in five of the six provincial cohorts, and this diagnosis included one case of palsy, two of paralysis, and four of epilepsy, one concussion, and two cases of St Vitus’s Dance. These results demonstrate that despite the clear guidelines for admissions there were still young patients being admitted with either infectious or chronic conditions. These cases, since they were not acute accidents, would have required a letter of recommendation from a hospital governor, indicating ‘the value placed both on the treatment and on the child’s good health by the subscriber as well as by the parents’.Footnote 53
The inpatient results summarised in Table 3 reveal that 80.7 per cent of child patients were discharged as ‘cured’. Hospital governors and sponsors knew that rapid patient turnover and the discharge of many ‘cured’ individuals were beneficial to the reputations of the voluntary hospitals.Footnote 54 This liberality appears to play a role in the London Hospital records. Two boys, a labourer’s son and a shoemaker’s son, were admitted to the London Hospital with fractured skulls and were discharged at four and nine days respectively as ‘cured’. This short period of time is insufficient for any substantial healing to have taken place and reminds the contemporary researcher that ‘cured’ might have more complex meanings than at first assumed. Williams and Sharma noted a similar conundrum in their study of children admitted to hospital with neurological conditions such as epilepsy; many were described as ‘cured’, despite the fact that their conditions are clinically defined as incurable.Footnote 55 Similarly, in the present investigation, eighty per cent of children with neurological conditions were discharged as ‘cured’.
The application of the term ‘cured’ probably also applied to those who were making excellent progress in their recovery. Thomas Stevenson, a boy ‘seven or eight years of age’ was thrown from a cart and suffered a fracture of the elbow ‘1½ inch above the condyles, & extending downwards into the joint, so that the condyles might be drawn from one another’ as well as two superficial wounds to the elbow.Footnote 56 His arm was splinted and bandaged at St George’s Hospital and he was discharged cured two weeks after his admittance once it was noted that ‘the union appears [reasonably] firm’.Footnote 57 According to modern clinical studies, fractures take approximately six weeks for substantial healing to occur, thus Thomas was discharged without a fully healed and remodelled injury, but was on the route to recovery.Footnote 58
Traumatic conditions were the most common reason for admittance to the London Hospital for all three years under investigation. This result aligns with the hospital’s policy of accepting acute accident cases outside regular patient admittance days. Early modern medical writers identified broken bones, as well as dislocations, hernias and wounds, as conditions that were generally easier to treat in children than adults.Footnote 59 Surgical conditions, such as broken bones, were more likely to be treated in a hospital than by dispensaries, which catered more to medical issues.Footnote 60 Table 4 displays the traumatic condition diagnostic label divided into subcategories. Boys were more commonly admitted to the London as trauma patients than girls; on average seventy-seven per cent of trauma cases were male children. Prognosis appears to have been mostly positive for those admitted with fractures. Only one of the thirty-two fractures was recorded as fatal; William Bettes, age thirteen, was admitted on 22 November 1792 for a compound fracture of the leg and died on 27 January 1793.
Table 5 displays the anatomical areas fractured by children at the London Hospital. Children admitted with fractures who were discharged as ‘cured’ stayed in hospital for between four and sixty days; the average inpatient stay was thirty-five days. As mentioned above, two cases of skull fracture were discharged too early for substantial healing to take place. It is possible that some children were admitted with dramatic looking wounds that revealed themselves to be lacerations or severe sprains rather than fractures once they were cleaned. The length of stay for arm fractures is less than for those of the thigh and lower leg; it was in the hospital’s best interest to discharge patients as soon as they were able and fractures that did not affect an individual’s ability to walk clearly required less time as an inpatient. The childhood fracture most frequently treated at the London Hospital was the thigh or femoral fracture, a common childhood injury in modern clinical studies.Footnote 61 These fractures are most commonly caused by accidents such as falls, sports, and collisions with vehicles. An individual presenting with a fractured thigh would most commonly be splinted: so that
Table 5: Body areas fractured.
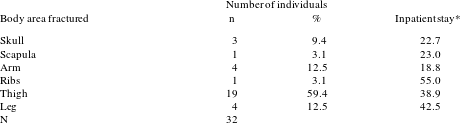
* Inpatient stay is the average number of days spent in hospital by those children who were eventually discharged as ‘cured’ or ‘relieved’ (recorded as n). The individual who died was not included in the average.
‘the limb may be kept permanently extended by splints being applied to it, while the trunk is attached to the head of the bedstead, & the foot to the opposite end, by means of proper bandages…permanent extension may be effected without considerable difficulty.’Footnote 62
The average inpatient stay for thigh fractures, 38.9 days, is approximately sufficient time for the injury to heal in a clinical sense; femoral fractures take at least six weeks for significant healing to occur.Footnote 63 The immobilisation and bed rest would allow sufficient healing to have occurred to allow the child to regain some mobility.
4 Broken Bodies: Accidents, Injuries and Risks
Simple fractures appear to have been treated as quotidian challenges by eighteenth-century surgeons; they were generally reduced, bound and splinted, and allowed time to heal. Compound injuries, in which the fractured bone pierces the skin and communicates with the air, were greatly feared due to the risk of infection; however, the injuries were not universally fatal. In previous research, it was found that of the adult individuals admitted to the London and Middlesex hospitals for compound fractures, only 28.6 per cent of males and 35.3 per cent of females died as inpatients, suggesting that the majority of individuals who suffered compound fractures were not dying in hospital, though their prognosis following discharge is unknown.Footnote 64
Two compound fractures experienced by children and recorded in contemporary physicians’ notes resulted in dramatically different outcomes. Henry Davis, age nine, was struck by a falling chimney brick. Two hours after the accident he was brought to St George’s by his mother. During the journey,
‘he conversed cheerfully and rationally with her …On his admission there was a wound on the right parietal bone 2 ½ inches in length, and on inserting the finger into it a deep depression of bone was felt, and small portions of Cerebrum were found mixed with coagulated blood. He is perfectly sensible and told the Nurse cheerfully that his head did not acke [sic].’Footnote 65
Two months later Henry is to be discharged as an outpatient, but it is noted that
‘there is, however, a large piece of bone to exfoliate. This morning a piece of brick came away from the wound about the size of the top of my little finger which no doubt had been lodged since the injury between the fractured portions of the cranium’.Footnote 66
This example provides a window into the child’s personality and also reveals a case in which an extreme injury was survived. The hospital records do not, of course, provide information on long-term health outcomes.
Edward [Quinton], a fifteen-year-old male who was admitted to St George’s after falling from the top of a tree, was eventually a fatal case. His injuries were clearly severe, as:
‘On his admission into the Hospital, a crepitus was discovered in some of the cervical vertebrae; the right clavicle, and one or two ribs were also fractured. The femur was broken about 3 inches about the knee, the bone had penetrated the skin making a large wound, and had also passed through the boy’s trousers. He lay for some hours motionless, excepting his head which he occasionally moved. His extremities were cold, and pulse scarcely perceptible; and he occasionally uttered long…cries expressive of the most horrible pain. It was a long time before the heat of the body returned, even with the assistance of bottles filled with hot water &c-.’Footnote 67
These examples are important, not only because they exemplify opposite medical outcomes; they provide a view into the qualitative patient experiences of poor children, which were rarely recorded.Footnote 68
Most fractures occur due to accidental traumatic injury. Seeking to access and reconstruct the context of historical fractures requires examination of the proximate (mechanical) and ultimate (cultural) causes of fractures. Clearly, without specific contextual evidence the cause of a fracture is simply speculative, but modern clinical data provide a framework in which to consider historical evidence. According to clinical data for the United States, vehicular trauma is the leading mechanism of injury, with falls as the second most common cause of injury.Footnote 69 Falls onto an outstretched hand, for example, may be the clear mechanism of injury, but the falls themselves may be caused by accidents or intentional pushes.Footnote 70 Many factors influencing the risk of fracture due to falls have been investigated in the clinical literature, including age, health status, prescription medications, footwear, time of day, handedness, location and the type of fall.Footnote 71 Studies specifically focused on children have identified playing, sports and vehicles as major contributing risk factors to children’s fractures.Footnote 72 These risks – particularly childhood play and the presence of vehicles – transcend time.
Eighteenth-century London was fraught with hazards. The health of a child born in eighteenth-century London was under pressure from birth, due to beliefs surrounding infant feeding and weaning. Newborns were often prevented from drinking nutrient-rich colostrum, the first milk produced by a new mother; the substance was deemed dangerous, probably due to its differing consistency and colour from later breast milk.Footnote 73 In addition, in Britain the median age at weaning dropped from 18 months in the early sixteenth century to 7.25 months by the end of the eighteenth century, in part due to an increase in artificial feeding.Footnote 74 Early weaning and the lack of colostrum robbed infants of the maternal antibodies in breast milk that aid in the support of the infant’s immune system.Footnote 75 Further, artificial feeding introduced nutritional challenges for infants which could lead to vitamin deficiencies such as scurvy, as weaning foods such as pap were generally of low quality, consisting of breadcrumbs or flour in milk or water.Footnote 76 Rickets, caused by a lack of vitamin D, was present in children in rapidly industrialising English cities such as London and Birmingham due to inadequate access to sunlight.Footnote 77 Urban overcrowding, pollution, inadequate sewage disposal and poor public hygiene led to epidemic outbreaks of diseases such as dysentery, typhoid, diphtheria and typhus.Footnote 78 Tuberculosis was common, spread by respiratory vectors and infected milk.Footnote 79 Contemporary physicians recognised that these epidemic diseases tended to spread in the overcrowded ‘narrow courts and alleys’ of the city, reflecting an awareness of the socially differentiated levels of risk present across London.Footnote 80
Table 6: Total number of child inpatients admitted per month ling number of inpatients with traumatic conditions.
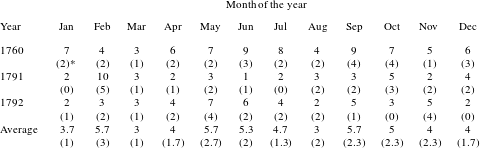
* Each cell displays the total number of child inpatients admitted with the number of child inpatients admitted for traumatic conditions in parentheses.
The London Hospital registers allow for a basic investigation of seasonality and its relationship to hospital admissions. Table 6 displays the number of child inpatients admitted by month and the number of child patients admitted into the most populous category, traumatic conditions. These data are represented graphically in Figure 1, in which the average number of child admissions per month and the average number of child admittances in the traumatic conditions category are displayed. There are three clear peaks in admittance: February, May–June, and September–October. The datasets chart a similar pattern, with the traumatic admissions clearly driving the admission peaks of February and May. These patterns may be artefacts of the small sample size, but there is value in comparing the data to studies of the relationship between accidental deaths recorded in the Bills of Mortality and seasonality. The winter months (November to February) were found to have higher than average incidence of burns and an increased number of scalds, posited to be related to the increased use of fires and preparation of hot foods indoors.Footnote 81 In February there were two admissions for scalds and four for burns; two other burns were admitted in November. The Bills of Mortality reveal that the summer months and beginning of fall (May–October) yielded the highest number of fatal falls, construction accidents, deaths due to animals, and vehicle-related accidents.Footnote 82 May, August, and October demonstrated the highest number of admissions for fractures and wounded body parts at the London Hospital, potentially reflecting the effects of children spending more time outdoors in the milder weather, thereby putting themselves at an increased risk for accidental injuries.
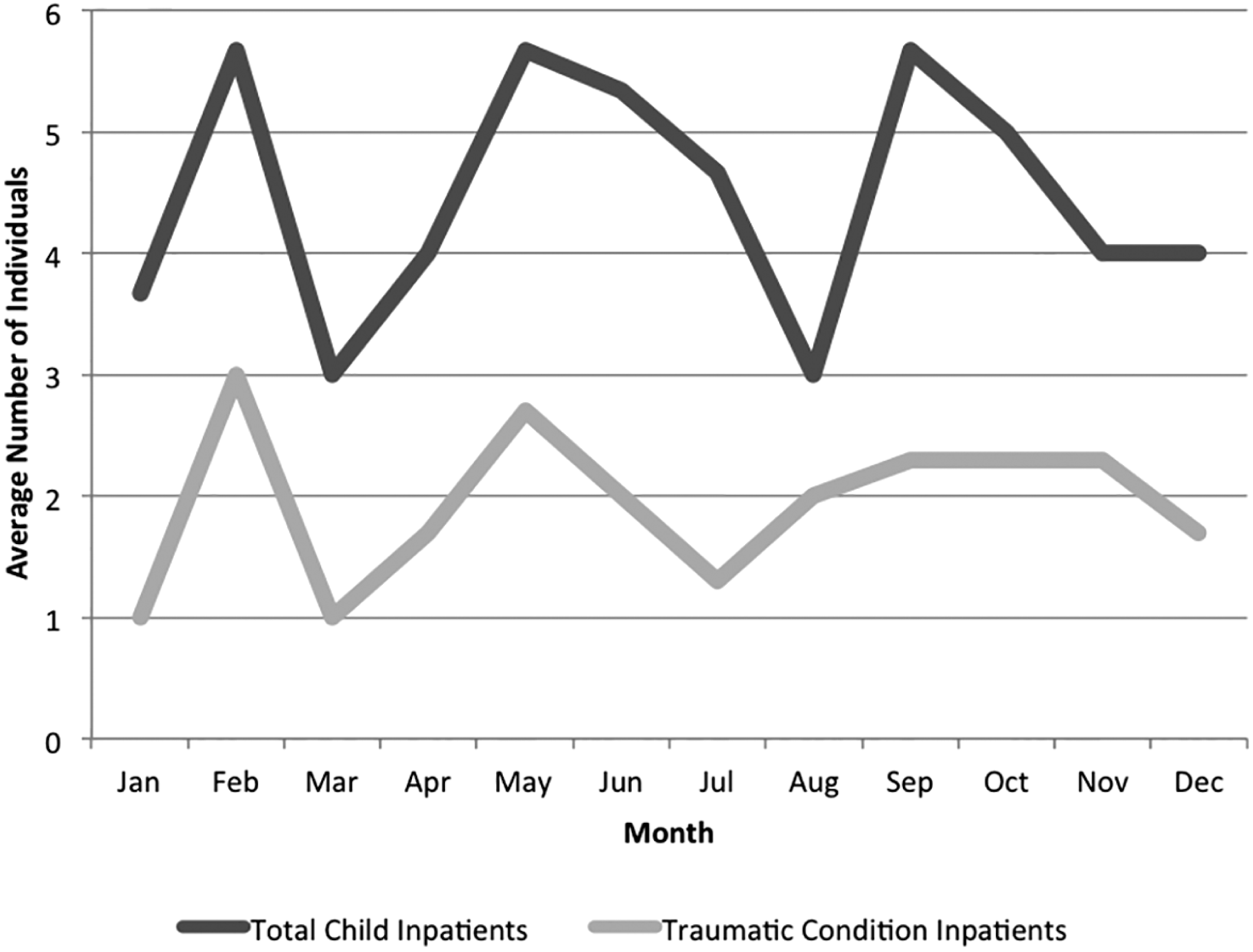
Figure 1: Average number of child admissions for traumatic conditions per month, compared with average total number of child admissions per month.
Using the London Bills of Mortality, Spence investigated the accidents and violent deaths that befell citizens of early modern London.Footnote 83 Though drowning was the most commonly recorded reason for accidental death between 1654 and 1735, falls were in second place, forming 11.8 per cent of the total recorded cases.Footnote 84 Vehicular accidents and being struck by various objects make up 5.4 per cent and 5.8 per cent of the total, respectively. Though children are not the primary focus of the work, Spence notes that children’s ‘limited abilities in judging distance and speed’ increased their risk of suffering accidental trauma involving carts and horses.Footnote 85 Many cases of accidents resulting in fractures probably never made it to the hospital; for example, John Cowley accidentally ran over three-year-old Edith Isham’s head with his coach and was eventually charged with manslaughter.Footnote 86 Many children were reported to have died due to accidental defenestration. For example, a two-and-a-half-year-old girl was admitted to St George’s hospital, having fallen fourteen feet out of a window. It was noted upon her admittance that ‘a considerable effusion of blood was found over the right parietal bone. Owing to this effusion it could not be ascertained whether there was any depression of bone or not’.Footnote 87 It was only upon dissection after her death that the diagnosis of fracture could be confirmed.
Other reasons for urban children’s injuries are equally likely to befall children living in more rural areas. Burns were often recorded in the Bills of Mortality due to the use of fire for cooking, lighting and heating.Footnote 88 Children with epilepsy were apparently at risk of falling into fires; billowing clothing catching fire is cited on several occasions in the death records from St Bartholomew’s Hospital as the reason for a child’s death.Footnote 89 The Bills of Mortality record fifty cases of children drowning; these were often domestic accidents involving water drawn for cooking or laundry or cases of children wandering too close to bodies of water.Footnote 90 A previous study of historic childhood injury notes that children were often injured whilst enjoying leisure activities, such as ‘playing ball or tag, running races, [and] attempting to be dare devils’, demonstrating the difficulty in narrowing down specific proximate causes for the injuries detailed in the London Hospital records.Footnote 91
Work undertaken by children may have put individuals at risk of injury. From an early age children were expected to take on tasks to assist their families. The range of activities depended upon the environment and age of the child; children in rural settings would probably have undertaken more varied tasks than those in cities and towns.Footnote 92 It was, however, common for children to be involved in household and agrarian tasks such as cleaning, collecting water, herding livestock, tending gardens and fields, preparing meals and minding siblings.Footnote 93 Some children in the London Hospital admission records have an occupation listed. Most of these are children in the eleven-to-thirteen-age range, when work outside the home would have been the increasing focus of their lives.Footnote 94 Apprenticeships, as noted above, generally started about age thirteen; those beginning apprenticeships were immediately put at greater risk of suffering accidents, catching epidemic diseases (for example, typhus, smallpox, tuberculosis), or ending up with occupational diseases.Footnote 95 The occupational health and accidents of young workers, as recorded in coroners’ records, has been investigated, though the focus is on the late medieval period.Footnote 96 In the present investigation, six female seamstresses (ages eleven to thirteen) were admitted with complaints ranging from fevers to an inflamed foot to two neurological cases (paralysis and St Vitus’s Dance). John Jenkins, a twelve-year-old errand boy from Whitechapel was admitted with a carious thumb, while a collection of servants and young labourers arrived at the London Hospital with various wounds, abscesses and contusions. Two fractured thigh cases, John French of Shoreditch and Richard Jones of Stepney, were listed as servants, but without further details it cannot be assumed their occupation was necessarily connected with their injury.
The proportion of admissions due to traumatic conditions is higher at the London Hospital than in any of the provincial cohorts studied by Levene and colleagues, particularly Chester and Manchester.Footnote 97 Though in four of the six cohorts examined by Levene and colleagues traumatic conditions were the most common reason for admission, the higher proportions evident in the London results is striking. The authors caution that ‘local industry, epidemiology or environment clearly cannot give us the whole story’.Footnote 98 These disparate results may suggest that London itself is a special case, and certainly the bustling urban environment of the metropolis posed higher risks of traumatic injury (particularly vehicular collisions and failures of infrastructure) for children than the provinces, though further records will need to be located and investigated to shed further light upon this characterisation. Certainly London ‘afforded the best possible response to traumatic injury with regard to the availability of medical personnel’.Footnote 99 It is possible that in smaller settlements, with less robust medical infrastructure, more children were being treated for traumatic injuries at home, by itinerant medical providers, or by provincial surgeons whose records may have not survived or have yet to be discovered. Probing further into the character of the London Hospital, however, proves fruitful since the ‘experience of hospitals was different’ across London.Footnote 100 The London Hospital was located ‘in the centre of one of the densest and poorest districts, and in close proximity to the Docks’, and was known in particular for its accident intake.Footnote 101 In fact, the hospital itself recorded that ‘the admission which is at all times freely given by night and by day to cases of accident and extreme urgency is one of the most important benefits conferred by the London Hospital’.Footnote 102 This echoes the finding that the Manchester Infirmary admitted many children with ‘sore eyes’ complaints, suggesting a known specialty of the hospital.Footnote 103
5 Conclusion
Examining the history of children in hospitals allows a more nuanced view into the broader history of accessing medical relief. A working poor family with a sick or injured child was tasked with navigating the medical marketplace to determine the best course of action. Despite a lack of specialised care for children in the eighteenth century and hospital rules dictating against accepting such patients, children were treated in eighteenth-century voluntary hospitals, including the London Hospital, for a variety of ailments. Children were admitted for reasons in direct violation of the hospital’s admittance procedures, demonstrating that case-by-case evaluation sometimes resulted in lenient and solicitous decisions. Indeed, children were viewed as a future source of labour – natural resource – thus treatment of conditions deemed curable was a worthwhile investment.
Overall, a lower proportion of children were admitted to the London Hospital than the provincial hospitals, but the proportion of traumatic cases accepted at the London is higher than any of the provincial cohorts studied by Levene and colleagues. This key finding potentially reflects the greater hazards to children present in the capital, where crowding and vehicular accidents were more likely to occur, but equally supports the London Hospital’s contemporary reputation as an accident centre. Traumatic conditions were the most common reason for admission to the London Hospital and the in-hospital mortality rates for these conditions were low.
The vast majority of child patients were discharged from the hospital as ‘cured’. Despite the seemingly liberal use of the term, most children admitted with fractures appear to have spent enough time as inpatients for substantial healing to have occurred. Exceptions do exist; however, it is likely that children who were clearly on the mend were candidates for early discharge in order to free up beds for patients with acute concerns. It is difficult to locate information on post-discharge patient prognosis, but contemporary clinical writings indicate that both closed and compound fractures were common sights to eighteenth-century medical practitioners and were often treated successfully.
The results of this study provide an intriguing view into the morbidity of children during the long eighteenth century. Further quantitative studies will provide a more detailed context in which to understand the risks to children’s health in London. The major limitations to such investigations are the inconsistent recording practices employed in the voluntary general hospitals across England, most of which did not include patient age, and the limited survival of extant patient admission records. It is hoped that further records will be unearthed and examined to further amplify the voices of the historical child inpatient. In the meantime, existing studies of children’s inpatient experiences will serve as critical historical context for bioarchaeological and palaeopathological studies of the skeletons of infants and children, a rapidly developing area of study.Footnote 104 Bioarchaeological studies provide invaluable insight into the lives of individuals in the past. The marks left on bones by fractures, as well as chronic infectious and metabolic diseases, provide a tangible record of lived disease and injury experience that can be further contextualised by historical evidence such as that gleaned from hospital records.
Like their modern counterparts, children in the past fell ill and suffered accidents. Clearly parents could not always keep a watchful eye on their children, but a popular eighteenth-century nursery rhyme, adapted from a seventeenth-century ballad, contains the following admonishment:
The frequency of children being admitted for traumatic injuries suggests that they were a common occurrence, potentially an expected part of childhood. Working poor parents whose children did not readily stay ‘safe at home’ faced a complex nexus of choices regarding health care. It is to the modern observer’s benefit that some chose to seek care at the voluntary general hospitals, leaving their marks and allowing a glimpse of the risks facing London’s youngest residents.









