Autism as a concept has developed over the past 50 years since Kanner first described it in 1943 (Reference KannerKanner, 1943). The concept of a classic triad of symptoms has developed into the present model of a continuum of related disorders referred to as pervasive developmental disorders, with classic Kannerian autism lying at one extreme. Prevalence rates for autism using the initial diagnostic criteria showed rates of about 4-6/10 000 (Reference LotterLotter, 1966; Reference Wing, Yeates and BrierlyWing et al, 1976), but the prevalence rates increased as the concept of autism expanded. Wing & Gould (Reference Wing and Gould1979) quoted the prevalence rate of autism as 21/10 000; of these, 4.9/10 000 have a strict diagnosis with all the criteria and 2/10 000 have the classic Kannerian autism.
Separate to the issue of changing diagnostic criteria, it appears that the prevalence rate of autism over the past 10 years may be increasing. Fombonne (Reference Fombonne1999) in his meta-analysis showed a median rate for autism of 5.2/ 10 000, but studies over the past 10 years showed a median rate of 7.2/10 000. It is not known whether this increased rate is due to a true increase in incidence or increased awareness of autism and related disorders.
Previous research into autism appears to concentrate on children, but autism is a lifelong condition with improvement tending to be the best outcome. This study identifies autistic-type disorders in an adult population with learning disabilities and, in particular, establishes a prevalence rate.
Obtaining accurate prevalence rates for autism in adults is important because it allows for planning and funding of specialist services. Treatment of autism in children is based mainly upon empirical evidence, suggesting benefits on long- and short-term functioning. Positive outcomes have been suggested also for treatment starting in adult life (Reference Jorden, Powell and MorganJorden & Powell, 1996). Services, therefore, are needed for this client group in order to maximise their individual potential.
There is an established association between learning disability and autism, learning disability being present in four out of five cases of autism (Reference Wing and GouldWing & Gould, 1979). Two major issues need to be taken into consideration in diagnosing autism in people with learning disabilities. The first is the separation of the deficits caused by autism from the deficits secondary to a learning disability. The second is the recognition that the presentation of psychiatric symptoms and signs is transformed by the presence of learning disabilities. The literature also shows a trend of increasing rates of autism with increasing severity of learning disability. Wing (Reference Wing1996) has suggested that 50-60% of those with severe learning disabilities have the autistic triad, compared with 0.2-0.4% of those with mild or no learning disability.
As a step in planning comprehensive services for adults with learning disabilities, the prevalence of autistic disorders needs to be established to allow effective planning.
Method
The Pervasive Developmental Disorder — Mental Retardation Scale (PDD-MRS; Reference KraijerKraijer, 1997) has been standardised on people with all degrees of learning disabilities, for use between the ages of 2 and 55 years (with reduced validity up to 81 years of age). As suggested from its name, it screens for pervasive developmental disorder. This screening tool has 12 items and looks at behaviour in the past 2-6 months as rated by a parent or carer. The PDD-MRS has been validated in adults with all levels of learning disability, and takes only 20-30 minutes to complete per individual.
The PDD-MRS consists of four categories. There are 12 individual items and some items have more than one stem. Each stem is scored individually and some stems are weighted so that they score more than other stems. The four categories are as follows: social interaction with adults (one item with three stems; a maximum score of six); social interaction with peers (one item with two stems; a maximum score of four); language and speech (three items, with a maximum score of four); and other behaviour (seven items, with a maximum score of 10). The maximum score is 19; a score of 10-19 gives a positive result but a score of 7-9 gives a doubtful result. Validity is stated as 94% against the diagnoses of ‘experienced psychological and medical experts’; internal consistency has an α coefficient of 0.8, specificity is 93%, interrater reliability is 0.83 and the scale was validated on 1052 individuals.
The PDD-MRS (Reference KraijerKraijer, 1997) was selected as the screening tool for this study. The diagnosis of an autistic disorder was a two-stage procedure. In the first stage a target group of people was identified by a definite or doubtful diagnosis with the PDD-MRS screening test. At the second stage a consultant psychiatrist confirmed the diagnosis of a pervasive developmental disorder clinically using the ICD-10 (World Health Organization, 1992) criteria; this clinical diagnosis consisted of a review of the individual's notes supplemented by personal knowledge of him/her. Because most people identified by the screening had complex care needs, most were under psychiatric out-patient care, the process of confirmation of a diagnosis of autism was simplified.
Population
The sample screened were adults with learning disability living in a clearly defined metropolitan borough in the West Midlands, our sample area having one responsible health authority and one co-terminous social services department. The total adult population for the area from census information was 230 000. Individuals were identified if they were in contact with any service for people with a learning disability or living in any residential placement for people with learning disabilities. Information was obtained from purchasers of both health and social services about any day services or residential placements funded or known; this was supplemented by local knowledge of any voluntary services from the community learning disability services and social services. The services screened varied from an individual residential placement to a social services day centre with 120 users. There were no traditional long-stay hospitals in this borough.
Results
In total, 571 people were screened over the period 1998-1999. No parents or carers declined to participate in the screening, the majority of the screening information being obtained from professional carers. Information on the sample screened was limited compared with the sample identified with autism. This was because not all of these individuals were under psychiatric care and hence there were no medical assessments to obtain information such as the level of learning disability.
Twenty-seven people fell into the doubtful category in the PDD-MRS, and of these 18 were diagnosed clinically as having autism and nine as not having autism. All of the individuals with a category of PDD in the screening test were confirmed clinically to have autism, which is surprising but may be due to the high threshold of the screening test.
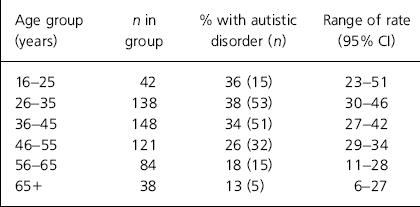
A total of 171 people were identified as having an autistic disorder clinically, which is a rate of 30% in those screened and an overall point prevalence rate of 7.7 per 10 000, taking into account the estimate of 230 000 adults in the defined population area. Unfortunately the demographic information available for the adult population did not give a breakdown of adults in specific age groups, which prevented further analysis of age-specific prevalence rates. The proportion of individuals in our sample with autistic disorder is shown in 10-year age bands in Table 1; this shows a marked decrease in proportions after the age of 55 years, a possible cause being a decreased longevity in learning disabled populations selectively affecting those with more complex needs. The clinical diagnosis of our identified sample was either infantile autism (F84.0; ICD-10) or atypical autism (F84.1; ICD-10). No other cases of developmental disorders, such as Rett's syndrome or childhood disintegrative disorder, were identified in our sample.
Table 1. Prevalence rates of autism in 10-year age bands
| Age group (years) | n in group | % with autistic disorder (n) | Range of rate (95% Cl) |
|---|---|---|---|
| 16-25 | 42 | 36 (15) | 23-51 |
| 26-35 | 138 | 38 (53) | 30-46 |
| 36-45 | 148 | 34 (51) | 27-42 |
| 46-55 | 121 | 26 (32) | 29-34 |
| 56-65 | 84 | 18 (15) | 11-28 |
| 65+ | 38 | 13 (5) | 6-27 |
The overall gender ratio was 1.25:1 male to female. Of the group identified, 57% had severe learning disability, 31% had moderate learning disability and 12% had mild learning disability. The level of learning disability was obtained from the medical notes. Owing to the complex needs of the identified people, most of these were obtained from formal IQ testing.
The care resources of those identified with an autistic disorder were also examined. The prevalence of an autistic disorder in various service settings varied, the social day care setting having a prevalence rate of only 7% compared with 58% in specialist day care. Nursing homes with people with significant needs had a higher rate of 64%, compared with social care centred residential homes (45%).
Discussion
Population studies in the field of learning disabilities commonly have difficulties in case identification. Most of the UK does not have comprehensive case registers and it is inevitable that some individuals with learning disabilities are missed. This study attempted to minimise this problem by using information from health services, social services and the voluntary sector in identifying individuals, although it is accepted that some people may have been missed. Groups that the study would have missed would be people with mild learning disability who functioned independently, those living with carers who totally supported them and those whose needs were so specialist that they were provided for out of district. Statistically, 2.27% of a population have an IQ of less than 70, suggesting that just over 5000 individuals in our sample area would have a learning disability; clearly our population of 500 is not a comprehensive community survey. However, our sample population will include the majority of people with learning disability with medical and social needs and this study needs to be interpreted with this in mind.
The Autistic Diagnostic Interview (ADI; Reference Lord, Rutter and LecoutierLord et al, 1994) is widely used as the most comprehensive diagnostic tool for autism, but it has the disadvantage of being very time consuming, taking up to 2 hours per person. It is also designed primarily for use in children. In our study it was decided that we needed a screening test to allow sufficient numbers of people to be screened. It was important that this screening test was designed and validated specifically for adults with learning disabilities.
In selecting the PDD-MRS (Reference KraijerKraijer, 1997) two major issues were considered. First, most screening tools and diagnostic interviews for use in autism are standardised on populations of children or adolescents. It has been reported that symptoms of autism may change over time, thus potentially confounding the use of childhood screening tests on adults. Social deficits and ritualistic behaviours improve (Reference RutterRutter, 1970), communication difficulties improve (Reference Ando and YoshimuraAndo & Yoshimura, 1979) and long-term institutionalisation and deprivation may mimic some of the obsessional features (Reference Rutter, Anderson-Wood and BeckettRutter et al, 1999). Second, many of the screening tests are not standardised over the spectrum of learning disabilities, with small numbers of people with learning disability being used or one degree of learning disability being overrepresented.
Our results showed a 30% overall prevalence rate of autistic disorders for people accessing learning disability services. This study gives a general population prevalence rate of 7.7 per 10 000 for autistic disorders, which is marginally high compared with the median rate of 7.2/ 10 000 from the meta-analysis by Fombonne (Reference Fombonne1999), taking into account that Fombonne's rate also included 20% of individuals with autism but without a learning disability. No studies identifying autism in adults only were identified in the literature; this lack of similar studies was confirmed in Fombonne's (Reference Fombonne1999) meta-analysis. It was not possible to obtain absolute prevalence rates of autism for each level of learning disability but the results showed that a disproportionate number of those diagnosed with an autistic disorder had severe learning disabilities (57%). This appears to confirm a positive association between increasing prevalence of autism and increasing severity of learning disability (Reference WingWing, 1996).
This survey also shows a high prevalence of autistic disorder in people living in 24-hour care placements. This may reflect the complex needs of people with an autistic disorder or the association of more severe learning disability with increasing rates of autism. Both of these increased needs could make care of the individual in a family setting more challenging.
The variation of prevalence rates of autistic disorders in various care settings suggests that people with an autistic disorder have more complex and difficult needs. This observation may be important, because staff can perceive some of the individuals' difficulties being due to challenging behaviour rather than the perceptual, language and behavioural phenotype associated with autistic disorders. This distinction is focal, because different approaches to problem behaviour are needed if someone has a diagnosis of an autistic disorder.
Conclusion
This study shows that autistic disorders are common: a point prevalence of 30% in the adult learning disability population, with higher prevalence rates in more intensive care settings. It also illustrates the graduation of people with childhood autistic disorders into the adult learning disability services. These individuals tend to aggregate in areas that cater for the needs of more challenging individuals, but they have different treatment needs to adults without autistic disorders. Service provisions should take this into account and also make available more specific intervention strategies focused on skills deficits associated with autistic disorders.




eLetters
No eLetters have been published for this article.