Introduction
Developmental psychopathology explores illness trajectories from a life-course perspective, and as such it may be especially helpful for understanding the emergence of mental disorders in youth (Scott et al. Reference Scott, Leboyer, Hickie, Berk, Kapczinski, Frank, Kupfer and McGorry2013). In young people, a particular challenge is to identify deviations in basic psychological and/or biological processes that can explain why the initial clinical presentation may demonstrate concurrent mental, physical, and alcohol/substance misuse disorders and/or the longitudinal phenomenology may show heterotypic continuity over time (McGorry et al. Reference McGorry, Hickie, Yung, Pantelis and Jackson2006; Hickie et al. Reference Hickie, Naismith, Robillard, Scott and Hermens2013; Scott et al. Reference Scott, Leboyer, Hickie, Berk, Kapczinski, Frank, Kupfer and McGorry2013).
Attempts to understand evolving patterns of signs and symptoms have increasingly focused on the application of dimensional approaches such as clinical staging and the Research Domain Criteria (RDoC) initiative (Insel et al. Reference Insel, Cuthbert, Garvey, Heinssen, Pine, Quinn, Sanislow and Wang2010; Sanislow et al. Reference Sanislow, Pine, Quinn, Kozak, Garvey, Heinssen, Wang and Cuthbert2010; Hickie et al. Reference Hickie, Naismith, Robillard, Scott and Hermens2013; McGorry et al. Reference McGorry, Keshavan, Goldstone, Amminger, Allott, Berk, Lavoie, Pantelis, Yung, Wood and Hickie2014). Both approaches highlight the need to consider psychopathology on a continuum (from normal experiences through to established clinical disorders) and emphasize that our understanding of liability and co-morbidity is more likely to be improved by examining putative underlying mechanisms that cut across current heterogeneous disorder categories (Baskin-Sommers & Foti, Reference Baskin-Sommers and Foti2015). Implicit in these frameworks is the notion that identifying trans-diagnostic processes that translate into ‘modifiable factors’ is a critical step in the development of precision or personalized medicine for mental disorders (Insel et al. Reference Insel, Cuthbert, Garvey, Heinssen, Pine, Quinn, Sanislow and Wang2010; McGorry et al. Reference McGorry, Keshavan, Goldstone, Amminger, Allott, Berk, Lavoie, Pantelis, Yung, Wood and Hickie2014), and moreover, that clinical advances will only really be achieved by greater integration of behavioural neuroscience into the study of psychopathology (Sanislow et al. Reference Sanislow, Pine, Quinn, Kozak, Garvey, Heinssen, Wang and Cuthbert2010). However, research to date has predominantly focused on ‘biomarkers’ (measurable biological characteristics) and/or neurocognition (‘cold circuits’) (McGorry et al. Reference McGorry, Keshavan, Goldstone, Amminger, Allott, Berk, Lavoie, Pantelis, Yung, Wood and Hickie2014). There have been fewer reviews that synthesize data on ‘hot cognitions’ (Simon et al. Reference Simon, Stenstrom and Read2015), such as cognitive processing styles involved in emotional regulation.
Given the lack of reviews that focus on cognitive-emotional processes that may act as a trans-diagnostic risk factor in young people with emerging severe mental disorders, we explore whether a particular ‘coping style’, namely rumination (and particularly ‘toxic’ brooding), can be considered as a specific age- and stage-related mechanism for psychopathology in youth. Whilst rumination has been studied extensively, we particularly focus on its evolution and its role in shaping emotional responses to stress in childhood, adolescence and early adulthood, including the peak age of onset period for psychosis, mood disorders and alcohol/substance misuse (between the ages of about 15 and 25 years) (Kessler et al. Reference Kessler, Chiu, Demler and Walters2005; Jones, Reference Jones2013) and whether rumination is a mechanism that can also help explain why many disorders in young people show heterotypic continuity over time and related phenomena such as multi-finality and pluri-potentiality (Ehring & Watkins, Reference Ehring and Watkins2008).
The paper begins by briefly discussing cognitive-emotional regulation and the concept of coping response style, and then reviews rumination from the perspective of theories about its evolution, its normal developmental trajectory and its role in the evolution of high prevalence disorders (such as anxiety and depression) that are often the early stage clinical phenotypes that co-occur with severe mental disorders in adolescence and early adulthood. Next, the paper explores the emerging evidence for links between rumination and alcohol and substance misuse, and bipolar and psychotic disorders. Finally, we briefly highlight the neurobiological underpinnings of rumination and how its putative role in physiological responses to stress may offer insights into the high prevalence of physical and mental co-morbidities in young people.
Brief overview of cognitive-emotional regulation and rumination
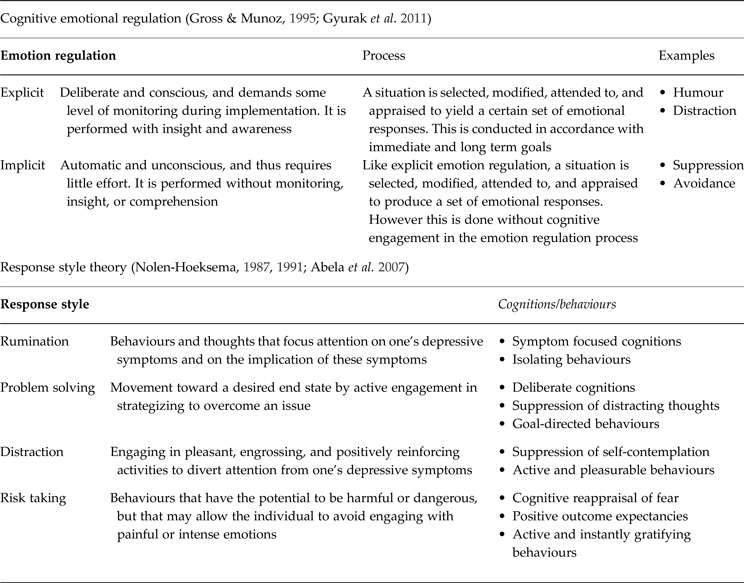
Cognitive-emotional regulation (CER) encompasses any attempt to understand and shape the emotions experienced and how these are expressed (Gross & Munoz, Reference Gross and Munoz1995). This regulation can be implicit (automatic, unconscious) or explicit (deliberate, requiring conscious effort) (Gyurak et al. Reference Gyurak, Gross and Etkin2011). Conscious, effortful cognitive processes can be adaptive or maladaptive and include strategies such as reappraisal and rumination (Garnefski & Kraaij, Reference Garnefski and Kraaij2007).
The most widely researched example of CER is the Response Styles Theory (RST; Nolen-Hoeksema, Reference Nolen-Hoeksema1987). RST focuses on individual styles of processing emotion that emerge in reaction to stressors and identifies four main coping responses: distraction, problem solving, risk taking, and rumination (see Table 1). Problem solving and distraction are considered to be adaptive response styles as they can positively impact on outcomes and provide opportunities for positive reinforcement, which increases future positive emotions and decreases negative affect (Abela et al. Reference Abela, Aydin and Auerbach2007). Risk-taking is considered maladaptive as, although it may temporarily offer distraction from or avoidance of difficult situations or feelings, the ‘downstream’ effects are more often negative (Nolen-Hoeksema, Reference Nolen-Hoeksema1987; Nolen-Hoeksema et al. Reference Nolen-Hoeksema, Wisco and Lyubomirsky2008).
Table 1. Key elements of cognitive emotion regulation and response styles theory
Rumination can be viewed as a stable individual trait (Smith & Alloy, Reference Smith and Alloy2009) characterized by ‘the tendency to repetitively analyse one's problems, concerns and feelings of distress without taking actions to make positive changes’ (Nolen-Hoeksema, Reference Nolen-Hoeksema1991, p. 569). Rumination appears to be a multifaceted construct, having adaptive and maladaptive components, often referred to as ‘reflective pondering’ and ‘toxic brooding’, respectively (Treynor et al. Reference Treynor, Gonzalez and Nolen-Hoeksema2003). Treynor et al. (Reference Treynor, Gonzalez and Nolen-Hoeksema2003) define reflection as a purposeful turning inward to engage in cognitive problem solving to alleviate one's distress whilst brooding is defined as ‘passive comparison of one's current situation with some unachieved standard. Brooding is associated with the maintenance and exacerbation of negative mood states such as depression and dysphoria (Verhaeghan et al. Reference Verhaeghen, Joormann and Aikman2014), and negative cognitive biases such as attentional engagement with negatively valanced stimuli (Joormann, Reference Joormann2004).
Several models of rumination confirm that it acts to amplify and prolong a prevailing mood state (see Smith & Alloy, Reference Smith and Alloy2009), increasing the likelihood that dysphoria will progress to depression, and can increase anxiety in individuals faced with threatening situations (Nolen-Hoeksema & Watkins, Reference Nolen-Hoeksema and Watkins2011). Negative cycles of rumination and dysphoria make it increasingly likely that an individual will focus on prior negative thoughts and experiences, which further impairs instrumental behaviour and effective problem solving (Brosschot et al. Reference Brosschot, Gerin and Thayer2006; Nolen-Hoeksema & Watkins, Reference Nolen-Hoeksema and Watkins2011). In contrast, there is emerging evidence that positive self-focused attention (positive reflection or ‘basking’) can be associated with lower levels of anxiety or negative affect (Segerstrom et al. Reference Segerstrom, Stanton, Alden and Shortridge2003; Feldman et al. Reference Feldman, Joormann and Johnson2008; Raes et al. Reference Raes, Smets, Nelis and Schoofs2012; Hou & Ng, Reference Hou and Ng2014).
How ruminative thought processes, such as toxic brooding, emerge and the underpinning mechanisms have been addressed by several research groups. The most prominent models of rumination, like RST, propose that rumination emerges in reaction to emotions such as negative affect and sadness, and that it is the styles of processing and reacting to emotions that lead to adverse psychological and physical health consequences (Nolen-Hoeksema, Reference Nolen-Hoeksema1991; Conway et al. Reference Conway, Csank, Holm and Blake2000). Other models, such as the ‘goal progress theory’ or ‘goal conflict theory’ propose that rumination is a response to behavioural inhibition and failure to progress satisfactorily towards a goal, or inaction and increased negative cognitive rehearsal associated with conflictual strivings, rather than a reaction to mood state per se (Emmons & King, Reference Emmons and King1988; Martin et al. Reference Martin, Tesser, McIntosh, Wegner and Pennybaker1993). It is suggested that failure to progress toward a goal and act on competing desires inaugurate ruminative thinking, which then leads to aversive psychological consequences such as mental disorders (Jones et al. Reference Jones, Papadakis, Hogan and Strauman2009; Einstein, Reference Einstein2014). There is evidence that individuals who fail to progress toward goal states have lower wellbeing (Emmons & King, Reference Emmons and King1988), that high levels of goal failure combined with maladaptive rumination (brooding) are associated with more depressive symptoms (Jones et al. Reference Jones, Papadakis, Hogan and Strauman2009), and that rumination mediates the link between goal attainment and positive affect (McIntosh et al. Reference McIntosh, Harlow and Martin1995).
Intolerance of uncertainty (IU), defined as a cognitive bias that affects how a person interprets and responds to uncertain situations (Dugas et al. Reference Dugas, Schwartz and Francis2004) is another mechanism proposed to underpin ruminative thinking (de Jong-Meyeret al. Reference de Jong-Meyer, Beck and Riede2009; Yook et al. Reference Yook, Kim, Suh and Lee2010; Einstein, Reference Einstein2014). It is suggested that individuals with IU are more sensitive to stress and use maladaptive coping strategies, such as dysfunctional cognitive processes or safety behaviours such as rumination, in order to reduce uncertainty, which may amplify affective states (McIntosh & Martin, Reference McIntosh and Martin1992). Studies of IU and rumination demonstrate that rumination completely mediates the relationship between IU and depression (Yook et al. Reference Yook, Kim, Suh and Lee2010; Liao & Wei, Reference Liao and Wei2011), but other cognitive biases such as worry did not show a mediation effect (Yook et al. Reference Yook, Kim, Suh and Lee2010).
Developmental trajectory of rumination
This section briefly examines evidence for the development of rumination over the life span, selecting three key topics to discuss: age, gender and early environment (including exposure to adversity).
Age and gender
Rumination involves a process of cognitive appraisal and so requires some capacity for basic abstract thinking and formal operational thought, which usually become apparent during the transition from mid-childhood to early adolescence (Piaget, Reference Piaget, Overton and Gallagher1977; Cole et al. Reference Cole, Nolen-Hoeksema, Girgus and Paul2006). Population-based studies confirm that children and pre-adolescents show significantly lower levels of rumination than adolescents (Hampel & Petermann, Reference Hampel and Petermann2005; Thompson et al. Reference Thompson, Mata, Jaeggi, Buschkuehl, Jonides and Gotlib2010). Interestingly, Sütterlin et al. (Reference Sütterlin, Paap, Babic, Kübler and Vögele2012) showed a decline in rumination from early adulthood onwards, where the highest levels of ‘brooding’ occurred in individuals aged <25 years. Explanations of the age trajectory of rumination concentrate on the potential long-term impact of childhood coping skills development and experiences. For example, some investigators have suggested that a peak in toxic brooding during adolescence is linked to difficulties in coping with increased levels of normative stressors that occur in this age range especially in those who failed to acquire sufficient adaptive problem-solving skills at an earlier age (Compas, Reference Compas1987).
Gender differences in rumination also emerge during adolescence, with levels increasing in a linear fashion for girls from 12 to 15 years of age onwards, but with limited increases in rumination in males during the post-pubertal period (Tamres Janicki & Helgeson, Reference Tamres, Janicki and Helgeson2002; Jose & Ratcliffe, Reference Jose and Ratcliffe2004; Jose & Brown, Reference Jose and Brown2008). There are a number of theories as to why females may ruminate more than males, including gender-stereotyped coping style (Cox et al. Reference Cox, Mezulis and Hyde2010) and differences in self-perceptions of emotionality and the stressfulness of the environment (Rudolph & Hammen, Reference Rudolph and Hammen1999; Gohm, Reference Gohm2003; Hyde et al. Reference Hyde, Mezulis and Abramson2008; Nolen-Hoeksema, Reference Nolen-Hoeksema2012). Against the latter, a meta-analysis by Tamres et al. (Reference Tamres, Janicki and Helgeson2002) found that gender differences in rumination were independent of the appraisal of stressors. Interestingly, work on ‘pubertal timing’ suggests that early puberty predicted higher levels of interpersonal dependent events and enhanced the risk of dysphoric symptoms in boys and girls who had a more negative cognitive style and a lower level of emotional clarity (Hamilton et al. Reference Hamilton, Hamlat, Stange, Abramson and Alloy2014a , Reference Hamilton, Stange, Kleiman, Hamlat, Abramson and Alloy b ).
Early environment
Some research indicates that future risk of becoming a ‘ruminator’ may be associated with early adversity, and rumination can be a learnt response style developed via parent modelling and communication (Hankin et al. Reference Hankin, Oppenheimer, Jenness, Barrocas, Shapero and Goldband2009; Cox et al. Reference Cox, Mezulis and Hyde2010). Nolen-Hoeksema (Reference Nolen-Hoeksema1998) proposed that children who have little perceived control over their environment might be especially prone to becoming ruminators in adolescence. For example, pre-school exposure to ‘negative-submissive family expressivity’ has been shown to predict rumination in adolescence (Hilt et al. Reference Hilt, Armstrong and Essex2012), whilst exposure to ‘over-controlling’ parenting can undermine the child's sense of self-efficacy or mastery and contribute to the development of maladaptive coping strategies (Parker, Reference Parker1983; Blatt & Homann, Reference Blatt and Homann1992) and a greater tendency to ruminate (Spasojevic & Alloy, Reference Spasojevic and Alloy2002; Manfredi et al. Reference Manfredi, Caselli, Rovetto, Rebecchi, Ruggiero, Sassaroli and Spada2011).
Neglect or abuse in childhood may shape a child's response to their environment, e.g. being vigilant to signs of threat and becoming passive to avoid aggravation in such situations, paying greater attention to negative stimuli, etc. (Macleod et al. Reference MacLeod, Rutherford, Campbell, Ebsworthy and Holker2002). In such circumstances, a child who feels helpless and socially and emotionally isolated may show reduced reliance on externally-oriented problem solving and an increased likelihood of engaging in solitary coping styles such as rumination (Browne & Finkelhor, Reference Browne and Finkelhor1986; Nolen-Hoeksema et al. Reference Nolen-Hoeksema, Parker and Larson1994). Moreover, Pearson et al. suggested that childhood abuse increases the development of anxious attachments, which have been found to prospectively predict rumination (Pearson et al. Reference Pearson, Watkins and Mullan2011).
Several studies offer support for the association between early adversity and rumination. For example, in non-clinical samples of college students, individuals with a history of childhood sexual abuse showed higher levels of rumination about sadness and dysphoria than those without such a history (Conway et al. Reference Conway, Mendelson, Giannopoulos, Csank and Holm2004). Likewise, clinical studies confirm an association between childhood sexual and emotional abuse and adult ruminative response style (e.g. Spasojevic & Alloy, Reference Spasojevic and Alloy2002); however, trends were statistically significant for females but not males (although the latter might be due to limited statistical power). A recent study by O'Mahen et al. (Reference O'Mahen, Karl, Moberly and Fedock2015) examined different experiences of childhood maltreatment in depressed and non-depressed pregnant women and suggested that childhood emotional neglect was related to behavioural avoidance whilst childhood emotional abuse was associated with rumination. Importantly, repeated assessment of nearly 1000 adolescents demonstrated that emotional abuse by parents or peers was an antecedent of negative coping and cognitive styles, and, as elaborated below, brooding mediated the association between abuse and future depressive symptoms (Padilla & Calvete, Reference Padilla Paredes and Calvete2014).
It is important to note that all these adverse experiences may be linked by an overarching issue, namely that they reduce the capacity of a child or adolescent to engage in effective and balanced control of their multiple needs; this in turn may exacerbate feelings of hopelessness, especially if they are living in unsupportive environments (Mansell & Carey, Reference Mansell, Carey, Kennedy, Kennerley and Pearson2013). Furthermore, these elements may increase the long-term risk of developing psychological problems and mental disorders in the future (Powers, Reference Powers1973).
Rumination and psychopathology
The increased interest in early intervention in youth with severe mental disorders has led to greater awareness of illness trajectories, in particular that preschool temperament or personality traits can be risk markers for psychopathology such as internalizing or anxiety problems in childhood, which may precede the onset of depressive symptoms or disorders and be the antecedents of later psychopathology (see Fig. 1). Not all individuals show progression from high prevalence disorders (e.g. anxiety, depression) to the lower prevalence disorders (e.g. psychosis, bipolar disorders), which is a developmental pattern that mimics a clinical staging model (McGorry et al. Reference McGorry, Hickie, Yung, Pantelis and Jackson2006). Clinical staging involves a detailed assessment of where an individual exists on a continuum of disorder progression from stage 0 (an at-risk but asymptomatic state) through to stage IV (late or end-stage disease) (McGorry et al. Reference McGorry, Hickie, Yung, Pantelis and Jackson2006; Hickie et al. Reference Hickie, Naismith, Robillard, Scott and Hermens2013; McGorry et al. Reference McGorry, Keshavan, Goldstone, Amminger, Allott, Berk, Lavoie, Pantelis, Yung, Wood and Hickie2014), and it is used routinely to describe disease progression in general medicine, e.g. for heart disease or diabetes. If this is a plausible approach for mental disorders, then trans-diagnostic mechanisms should be identifiable across stages and over time both within and between individuals.

Fig. 1. Representation of clinical stages of mental disorders beginning with early childhood temperament through to anxiety, depression, and then severe mental disorders (with peak age of onset in late adolescence/early adulthood).
Temperament, rumination and future psychopathology
Temperament can be broadly defined as biologically based, relatively stable individual differences in emotions, behaviours, and cognitions (Rothbart & Bates, Reference Rothbart, Bates, Eisenberg, Damon and Richard2006). Negative emotionality (NE) is an infant temperamental style that is widely associated with psychopathology in adolescence, with high NE individuals experiencing negative emotions more frequently and intensely than their peers (Belsky et al. Reference Belsky, Hsieh and Crnic1996), and are more likely to exhibit depression (Mezulis et al. Reference Mezulis, Priess and Hyde2011), anxiety (Hudson & Rapee, Reference Hudson, Rapee, Heimberg, Turk and Mennin2004), and/or substance abuse (Allen & Gabbay, Reference Allen and Gabbay2013).
A prospective longitudinal study from birth to adolescence, found that rumination significantly mediated the association between NE in infancy and depressive symptoms at age 15 years (Mezulis et al. Reference Mezulis, Priess and Hyde2011). Consistent with other studies (e.g. Verstraeten et al. Reference Verstraeten, Vasey, Raes and Bijttebier2009), Mezulis et al. (Reference Mezulis, Priess and Hyde2011) noted that the association was stronger among adolescent girls, although a further study by the same group highlighted that high levels of depressive symptoms at age 11 were associated with both early puberty and high levels of NE in boys (Mezulis et al. Reference Mezulis, Salk, Hyde, Priess-Groben and Simonson2014).
Neuroticism is a similar but narrower construct than NE (Eysenck & Eysenck, Reference Eysenck and Eysenck1985). Like NE, ruminative response style has been shown to fully or partially mediate the association between neuroticism and anxiety and depression in adolescents and young adults (Muris et al. Reference Muris, Meesters and Diederen2005; Kuyken et al. Reference Kuyken, Watkins, Holden and Cook2006; Roelofs et al. Reference Roelofs, Huibers, Peeters and Arntz2008).
Anxiety and depression
About 50% of individuals with anxiety disorders experience their first symptoms by the age of 11 (Kessler et al. Reference Kessler, Chiu, Demler and Walters2005). A number of studies demonstrate that childhood anxiety and/or internalizing symptoms may predict adolescent depressive symptoms/episodes (Last et al. Reference Last, Hansen and Franco1997; Horn & Wuyek, Reference Horn and Wuyek2010), whilst anxiety disorders in early adolescence significantly predict first onset of a major depressive episode (MDE; Bittner et al. Reference Bittner, Goodwin, Wittchen, Beesdo, Höfler and Lieb2004). Rates of depressive disorders increase markedly during mid to late adolescence with about 20% of adolescents experiencing a MDE (Lewinsohn et al. Reference Lewinsohn, Rohde and Seeley1998), and concurrent depression and anxiety occurs significantly more frequently in adolescence compared to childhood (Lamers et al. Reference Lamers, van Oppen, Comijs, Smit, Spinhoven, Van Balkom and Penninx2011).
Studies suggest that there is a robust relationship between rumination and the development of internalizing problems (such as withdrawal, anxiety and depression) but not externalizing problems (such as aggression, hyperactivity, etc.) in childhood (Garnefski et al. Reference Garnefski, Kraaij and van Etten2005). Rumination is also significantly associated with the development and maintenance of anxiety symptoms in adolescents (e.g. Garnefski et al. Reference Garnefski, Kraaij and Spinhoven2001, Reference Garnefski, Legerstee, Kraaij, Van Den Kommer and Teerds2002; Tan et al. Reference Tan, Forbes, Dahl, Ryan, Siegle, Ladouceur and Silk2012; Jose et al. Reference Jose, Wilkins and Spendelow2012; Jose & Weir, Reference Jose and Weir2013), and increases the risk of developing anxiety problems in early adolescence (Tan et al. Reference Tan, Forbes, Dahl, Ryan, Siegle, Ladouceur and Silk2012). Furthermore, in a mid-teen sample, social anxiety (a recognized antecedent of severe mental disorders) directly predicted higher levels of rumination over time, especially in females (Jose et al. Reference Jose, Wilkins and Spendelow2012).
Stressful life events and experiences such as bullying are potent risk factors for the development of internalizing symptoms (e.g. McLaughlin et al. Reference McLaughlin, Hatzenbuehler and Hilt2009). In cross-sectional and prospective studies, McLaughlin and colleagues (e.g. McLaughlin & Hatzenbuehler, Reference McLaughlin and Hatzenbuehler2009; McLaughlin & Nolen-Hoeksema, Reference McLaughlin and Nolen-Hoeksema2012) demonstrated that rumination fully mediated the relationship between stressful life events and anxiety and depression among adolescents, but only partially mediated the association in adults. A large-scale study by Michl et al. (Reference Michl, McLaughlin, Shepherd and Nolen-Hoeksema2013) confirmed that rumination is a key mediator between stress and anxiety and depressive phenomena in adolescents.
Independently for depression, there is a vast literature that indicates that rumination is significantly associated with depression onset, maintenance, and relapse, especially during adolescence (e.g. Wood et al. Reference Wood, Saltzberg, Neale, Stone and Rachmiel1990; Nolen-Hoeksema, Reference Nolen-Hoeksema2000; Michalak et al. Reference Michalak, Hole, Livingston, Murray, Parikh, Lapsley and McBride2012). A meta-analysis demonstrated that the higher levels of rumination in females compared to males significantly mediated the increased rates of depression that becomes apparent post-puberty (Aldao & Nolen-Hoeksema, Reference Aldao and Nolen-Hoeksema2012). Broderick (Reference Broderick1998) suggests that adolescents use rumination to deal with family, academic, and peer group problems, which become increasingly more stressful and prominent during the adolescent period. However, as ruminative response style exacerbates rather than reduces the negative outcomes of stressful life events, it increases the likelihood of depressive outcomes (Schwartz & Koenig, Reference Schwartz and Koenig1996; Broderick, Reference Broderick1998; Kraaij et al. Reference Kraaij, Garnefski, de Wilde, Dijkstra, Gebhardt, Maes and ter Doest2003). Furthermore, a study of an ethnically diverse sample of over 1000 college students demonstrated that individuals who brood in response to negative life events may be vulnerable to thinking about suicide, and that whilst level of suicidal ideation was partly explained by severity of symptoms of depression, it was also directly related to brooding itself (Chan et al. Reference Chan, Miranda and Surrence2009).
Alcohol and substance misuse
The prevalence of alcohol use disorders (AUD) and substance use disorders (SUD) in adolescents range from about 5–10% (Merikangas et al. Reference Merikangas, He, Burstein, Swanson, Avenevoli, Cui, Benjet, Georgiades and Swendsen2010; Merikangas & McClair, Reference Merikangas and McClair2012). Approximately 40% of individuals with an AUD and just below 50% of those with SUD experienced their first symptoms of harmful use before 19 years (Helzer et al. Reference Helzer, Burnam, McEvoy, Robins and Regier1991; Dennis et al. Reference Dennis, Babor, Roebuck and Donaldson2002).
In clinical settings, 70–80% of adolescents with AUD and SUD have a co-morbid mental disorder (Ḳaminer & Bukstein, Reference Ḳaminer and Bukstein2008), including anxiety, depression, psychosis or bipolar disorders. Studies indicate that rumination increases the risk for harmful alcohol and/or substance use (e.g. Nolen-Hoeksema & Harrell, Reference Nolen-Hoeksema and Harrell2002; Caselli et al. Reference Caselli, Bortolai, Leoni, Rovetto and Spada2008; Caselli et al. Reference Caselli, Ferretti, Leoni, Rebecchi, Rovetto and Spada2010), particularly in female adolescents where rumination predicted the onset of substance abuse (and of bulimia), and predicted a future increase in substance abuse symptoms over a 4-year period (Nolen-Hoeksema et al. Reference Nolen-Hoeksema, Stice, Wade and Bohon2007).
The association between rumination and alcohol and substance misuse may be direct or indirect. For example, some studies of adolescents suggest that depression increases rumination, which in turn leads to increased substance use, as demonstrated by the association between brooding and marijuana use (Adrian et al. Reference Adrian, McCarty, King, McCauley and Vander Stoep2014). Skitch & Abela (Reference Skitch and Abela2008) showed that ruminative brooding predicted substance abuse for up to 18 weeks following negative events, and that this effect was exacerbated in older adolescents with an existing MDE. Other research supports a direct association (e.g. Willem et al. Reference Willem, Bijttebier, Claes and Raes2011), reporting that, independent of depression, adolescents with lower reflective pondering demonstrated higher drug consumption whilst higher brooding was associated with more problematic substance use.
Bipolar disorders (BD)
The peak age of onset for BD is late adolescence and early adulthood, although most individuals experience one or more MDE, brief hypomania or sub-threshold mania before syndromal episodes of hypomania or mania occur (Duffy et al. Reference Duffy, Alda, Hajek and Grof2009; Douglas & Scott, Reference Douglas and Scott2014). Those individuals with depression who may be at highest risk of transition to BD often show cyclothymic or hypomanic personality traits or have a family history of bipolar disorders (Duffy et al. Reference Duffy, Alda, Hajek and Grof2009; Geoffroy et al. Reference Geoffroy, Leboyer and Scott2013; Bechdolf et al. Reference Bechdolf, Ratheesh, Cotton, Nelson, Chanen, Betts, Bingmann, Yung, Berk and McGorry2014).
There is limited research on rumination and mania in adolescents and young adults, but studies in middle-aged adults or mixed samples of younger and older adults show that rumination is present in both the depressed and (hypo)manic phases of BD, is increased in unaffected first degree relatives compared to healthy controls, and that increased rumination predicts relapse and/or worse course of illness (Johnson et al. Reference Johnson, McKenzie and McMurrich2008; Van der Gucht et al. Reference Van der Gucht, Morriss, Lancaster, Kinderman and Bentall2009; Green et al. Reference Green, Lino, Hwang, Sparks, James and Mitchell2011; Ghaznavi & Deckersbach, Reference Ghaznavi and Deckersbach2012).
A study of university students (mean age 22 years) (Thomas & Bentall, Reference Thomas and Bentall2002), reported that ruminative response style was positively correlated with scores on the Hypomanic Personality Scale (Eckblad & Chapman, Reference Eckblad and Chapman1986). A second study of undergraduate students (mean age 19 years) by the same group found that rumination was independently associated with both depression and hypomania symptom scores (Knowles et al. Reference Knowles, Tai, Christensen and Bentall2005), and that risk-taking behaviours were also increased in association with rumination, especially in males. Knowles et al. (Reference Knowles, Tai, Christensen and Bentall2005) hypothesized that rumination may exacerbate depressive symptoms whilst some individuals make active attempts to avoid negative or intense mood states by engaging in high-risk activities, which may be linked to hypomanic or manic symptoms (Van der Gucht et al. Reference Van der Gucht, Morriss, Lancaster, Kinderman and Bentall2009; Weiss et al. Reference Weiss, Sullivan and Tull2015).
Studies of individuals at high risk of BD or the offspring of BD parents demonstrate early evidence of deficits in CER (e.g. Nijjar et al. Reference Nijjar, Ellenbogen and Hodgins2014; Van Rheene et al. Reference Van Rheenen, Murray and Rossell2015). In a study of response styles, Jones et al. (Reference Jones, Tai, Evershed, Knowles and Bentall2006) found that offspring with current or past evidence of psychopathology (affected offspring) and unaffected offspring had higher levels of rumination than age- and gender-matched controls. Pavlickova et al. (Reference Pavlickova, Turnbull and Bentall2014) demonstrated that, compared to offspring of healthy parents, affected offspring of bipolar parents showed significantly increased levels of rumination and of hypomanic cognitions compared to unaffected offspring or healthy controls. An experiential sampling study by the same group examined the inter-relationships between mood, self-esteem and response styles over 6 days (Pavlickova et al. Reference Pavlickova, Turnbull, Myin-Germeys and Bentall2015). Interestingly, increased negative as well as positive mood resulted in greater rumination in offspring and controls, and low self-esteem triggered greater risk-taking in the bipolar offspring group, while negative affect instigated increased active coping in the control group. Additionally, as in studies of depression, CER impairments such as increased ruminative response style are associated with suicidal ideation in young people with emerging bipolar disorders (Stange et al. Reference Stange, Hamilton, Burke, Kleiman, O'Garro-Moore, Seligman, Abramson and Alloy2015).
Psychosis
The typical age of onset for psychotic disorders is late adolescence or early twenties, being slightly later in females than males (Hafner et al. Reference Hafner, Maurer, Löffler and Fatkenheuer1994; Gogtay et al. Reference Gogtay, Vyas, Testa, Wood and Pantelis2011). Several studies report that anxiety or depression in childhood or adolescence may precede the onset of psychosis (Baynes et al. Reference Baynes, Mulholland, Cooper, Montgomery, MacFlynn, Lynch, Kelly and King2000; Mulholland & Cooper, Reference Mulholland and Cooper2000; Maggini & Raballo, Reference Maggini and Raballo2006). Research in groups at high risk of psychosis indicate that transition is common in those who have experienced brief periods of psychosis or psychotic-like symptoms (Yung et al. Reference Yung, Stanford, Cosgrave, Killackey, Phillips, Nelson and McGorry2006), whilst the presence of depression and/or anxiety is associated with increased suicidality, self-harm, disorganized behaviour, disorganized speech, and anhedonia (Fusar-Poli et al. Reference Fusar-Poli, Nelson, Valmaggia, Yung and McGuire2014).
Rumination has been shown to be associated with hallucination-proneness and a range of mild anomalous experiences including feelings of unreality, perceptual alterations, and temporal disintegration (Jones & Fernyhough, Reference Jones and Fernyhough2009; Freeman et al. Reference Freeman, Startup, Dunn, Černis, Wingham, Pugh, Cordwell and Kingdon2013). Experiential sampling in young adults with psychosis demonstrates that antecedent rumination and worry predict persecutory delusions and auditory hallucinations, and that rumination predicted the level of distress associated with these psychotic experiences (Hartley et al. Reference Hartley, Haddock, Vasconcelos e Sa, Emsley and Barrowclough2014). Also, Halari et al. (Reference Halari, Premkumar, Farquharson, Fannon, Kuipers and Kumari2009) demonstrated that rumination can be associated with negative symptoms such as stereotyped thinking and emotional withdrawal.
As ruminative response style overlaps with perseverative thinking, it could indicate that rumination in psychosis is associated with underlying psychotic or dysphoric (anxiety/depressive) dimensions (Cernis et al. Reference Cernis, Dunn, Startup, Kingdon, Wingham, Evans, Lister, Pugh, Cordwell, Mander and Freeman2015). Theoretically, rumination might also help explain why some young people who experience psychotic symptoms become distressed and seek help, whilst others do not (Van Nierop et al. Reference Van Nierop, van Os, Gunther, Myin-Germeys, de Graaf, ten Have, van Dorsselaer, Bak and van Winkel2012; Rapado-Castro et al. Reference Rapado-Castro, McGorry, Yung, Calvo and Nelson2015).
Lastly, in a cross-sectional study of psychotic inpatients with and without suicidality (n = 2383; mean age at onset 25 years), ruminative thinking, social withdrawal, and lack of activity were all associated with increased suicidality (Ahrens & Linden, Reference Ahrens and Linden1996).
Neurobiological underpinnings of rumination
Neurobiological factors play a key role in the activation and maintenance of cognitive-emotional processes. This section briefly examines a selection of the developing research on the associations between rumination in young people and genetics, neuropsychology, physiology, sleep and physical health.
Genes
There are reasons to consider the role of genetics in the development of rumination. As noted, rumination may mediate the association between temperamental styles that are heritable (e.g. NE, neuroticism) and depression. Furthermore, children at high risk of depression (e.g. offspring of mothers with a history of MDE) show higher levels of rumination than controls (Gibb et al. Reference Gibb, Grassia, Stone, Uhrlass and McGeary2012). A small number of twin studies have examined genetic and environmental influences (shared and non-shared elements) on rumination, brooding and mood disorders. In a Chinese study of adolescent twins, the heritability of depression (30–42%) was modest, but genetic effects accounted for 24% of the variation in adolescent rumination, and genetics mediated the relationship between rumination and depression (Chen & Li, Reference Chen and Li2013). In a US study of adolescent twins aged 12–14 years, heritability accounted for 21% of the variation in adolescent brooding, highlighting again that although the heritable influences were modest, they accounted for the majority of the relationship between brooding and depression (h2 = 0.62) (Moore et al. Reference Moore, Salk, Van Hulle, Abramson, Hyde, Lemery-Chalfant and Goldsmith2013). Preliminary data from a UK study of BD in twins and siblings showed that ruminative response style had a low to moderate heritability with 23% of the total variance accounted for by additive genetic effects (Beards et al. Reference Beards, Georgiades, Sharma, Kane, Kalidindi, Schulze, Walshe, Scott, Murray, Rijsdijk and Kraviriti2012).
Certain polymorphisms of the BDNF gene (a protein involved in the growth of new and existing neurons and synapses) have also been found to be linked to rumination (Beevers et al. Reference Beevers, Wells and McGeary2009). Results suggest that individuals with the Val66Met BDNF gene polymorphism are significantly more likely to ruminate than individuals without the gene. This is consistent with recent research that has found an association between the BDNF gene Val66Met polymorphism, rumination, and depression (Hilt et al. Reference Hilt, Sander, Nolen-Hoeksema and Simen2007), where analyses suggested that rumination mediated the relationship between the BDNF polymorphism and depressive symptoms.
Neuropsychology
A number of cognitive processes are activated when engaging in rumination, in particular attention, memory, and self-referential processing (Lyubomirsky et al. Reference Lyubomirsky, Caldwell and Nolen-Hoeksema1998). Investigators have reported that rumination generates difficulties in controlling the entry of irrelevant information into working memory (WM) and short-term memory (STM) (Joormann, Reference Joormann2004; Goeleven et al. Reference Goeleven, De Raedt, Baert and Koster2006; Joormann et al. Reference Joormann, Nee, Berman, Jonides and Gotlib2010), or the removal of negative self-relevant information from WM and STM storage (Joormann & Gotlib, Reference Joormann and Gotlib2008). Ruminators also show general deficits in the ability to shift attention from unhelpful to helpful strategies (Davis & Nolen-Hoeksema, Reference Davis and Nolen-Hoeksema2000). Futhermore, a study of over 200 adolescents demonstrated that engaging in ruminative thoughts consumes cognitive resources that would otherwise be allocated towards difficult tests of executive functioning (the resource allocation hypothesis). In contrast, no evidence was found to support the notion that lower levels of executive functioning at baseline predicted levels of rumination or depressive symptoms at follow-up (Connolly et al. Reference Connolly, Wagner, Shapero, Pendergast, Abramson and Alloy2014).
Functional magnetic resonance imaging (fMRI) shows that rumination is positively correlated with an increased activation of the medial prefrontal cortex and amygdala (Ray et al. Reference Ray, Ochsner, Cooper, Robertson, Gabrieli and Gross2005), and adults who ruminate regularly (e.g. dysphoric or depressed patients) show high connectivity between these structures (Gotlib & Hamilton, Reference Gotlib and Hamilton2008). Ruminators also engage in higher rates of self-referential processing compared to their non-ruminative counterparts (Gotlib & Joormann, Reference Gotlib and Joormann2010); a process that can be examined via neuroimaging of the default mode network (DMN) (Ochsner & Gross, Reference Ochsner and Gross2005; Schmitz & Johnson, Reference Schmitz and Johnson2006). In non-ruminators, activation of DMN brain regions is reduced after performing non-self-referential (i.e. goal-directed) activities during off-task or rest periods, suggesting an ability to lose one's self in the work (Sheline et al. Reference Sheline, Barch, Price, Rundle, Vaishnavi, Snyder, Mintun, Wang, Coalson and Raichle2009). In contrast, high ruminators show high connectivity between DMN regions during these rest periods, reflecting an inability to suppress self-referential thoughts during off-task times. Berman et al. (Reference Berman, Peltier, Nee, Kross, Deldin and Jonides2011b ) noted that in young adults (mean age 22 years) these connectivities were only found when participants engaged in brooding and not reflective pondering.
Marchetti et al. (Reference Marchetti, Koster, Sonuga-Barke and De Raedt2012) propose that an imbalance in the task positive (TP) and task negative (TN) elements of the DMN is the overarching neural mechanism involved in rumination. Studies of rumination in youth (Berman et al. Reference Berman, Nee, Casement, Kim, Deldin, Kross, Gonzalez, Demiralp, Gotlib, Hamilton, Joormann, Waugh and Jonides2011a ) and of adult depressed cases v. controls (Hamilton et al. Reference Hamilton, Furman, Chang, Thomason, Dennis and Gotlib2011) support the proposal that a TN-TP imbalance is associated with a failure to attenuate TN activity in the transition from rest to task periods and with toxic brooding.
A recent fMRI study compared healthy controls with unmedicated adolescents in remission from MDE (Jacobs et al. Reference Jacobs, Jenkins, Gabriel, Barba, Ryan, Weisenbach, Verges, Baker, Peters, Crane, Gotlib, Zubieta, Phan, Langenecker and Welsh2014) and showed that the remitted MDE adolescents exhibited hyper-connectivities within the DMN and between the DMN and salience networks (posterior cingulate cortex, subgenual anterior cingulate, and amygdala) and regions of the cognitive control network, which were related to rumination and sustained attention. However, it was not possible to conclude that the hyper-connectivities represented brain-based markers of traits (e.g. rumination), as it is plausible that the hyper-connectivities represent compensatory mechanisms in individuals with emerging mood disorders. Fewer studies examine CER in individuals aged 15–25 years with emerging bipolar disorders, although in mixed samples of younger and older adults it has been shown that individuals at increased risk of developing bipolar disorders are less successful at down-regulating amygdala activity and demonstrate inefficient use of reappraisal and distraction strategies (e.g. Heissler et al. Reference Heissler, Kanske, Schonfelder and Wessa2014).
Hypothalamic-pituitary-adrenal (HPA) axis and physiological studies
Several physiological studies have examined the relationship between rumination and heart rate variability. Key et al. (Reference Key, Campbell, Bacon and Gerin2008) demonstrated that heart rate variability in response to stress is more strongly associated with trait rather than state rumination in female college students.
A review of the relationship between rumination and cortisol identified that 13 of 17 studies were undertaken in children, students or young adults (Zoccola & Dickerson, Reference Zoccola and Dickerson2012). Whilst higher levels of state rumination were consistently linked to increased cortisol concentrations, findings were less consistent for the physiological effects of stressors (basal cortisol levels or cortisol awakening response to naturally occurring or laboratory-induced stress). However, those studies that utilized social-evaluative stressor tasks generally showed that rumination predicted greater cortisol reactivity or delayed recovery. These findings are supported by a study using pupillary response to perceived rejection in depressed adolescents (Stone et al. Reference Stone, Silk, Siegle, Lee, Stroud, Nelson, Dahl and Jones2016).
Gianferante et al. (Reference Gianferante, Thoma, Hanlin, Chen, Breines, Zoccola and Rohleder2014) also showed that rumination in response to repeated stress predicted non-habituation of the HPA axis, which the authors suggest may offer a pathway linking rumination to negative health outcomes. Interestingly, this association may be bidirectional or attenuated by baseline physical status (Puterman et al. Reference Puterman, O'Donovan, Adler, Tomiyama, Kemeny, Wolkowitz and Epel2011). For example, Puterman et al. (Reference Puterman, O'Donovan, Adler, Tomiyama, Kemeny, Wolkowitz and Epel2011) demonstrated that although ruminators experienced a more rapid initial increase in cortisol levels, greater HPA axis reactivity, and slower HPA axis recovery from stress, this profile was only significant in sedentary participants. In active participants, cortisol trajectories were equivalent in high and low ruminators. These findings are noteworthy given the evidence of increased sedentary lifestyles and lower physical activity in youth with mental disorders (even when medication-free) compared to their peers (Gehue et al. Reference Gehue, Scott, Hermens, Scott and Hickie2015; Vallarino et al. Reference Vallarino, Henry, Etain, Gehue, Macneil, Scott, Barbato, Conus, Hlastala, Fristad, Miklowitz and Scott2015).
Sleep and circadian rhythms
Rumination may indirectly influence circadian rhythms through its association with increased cortisol production (Rea et al. Reference Rea, Smith, Bierman and Figueiro2010) and alterations in cortisol secretion patterns (for a review see Chan & Debono, Reference Chan and Debono2010). Furthermore, studies of sleep in adolescents show rumination to be directly associated with poorer general sleep quality, longer time to fall asleep and more awakenings after sleep onset (Thomsen et al. Reference Thomsen, Yung Mehlsen, Christensen and Zachariae2003). Dysregulated sleep is associated with increased rumination compared to good sleepers with evidence that brooding is associated with fatigue, poor concentration and low mood (Carney et al. Reference Carney, Edinger, Meyer, Lindman and Istre2006). Zoccola et al. (Reference Zoccola, Dickerson and Lam2009) found that ruminating about a past stressor before bedtime predicted longer sleep onset latencies. This suggestion that post-stressor ruminative thought may predict delayed sleep onset is of particular interest as delayed sleep phase syndrome is a recognized marker of circadian disturbance that occurs more often in young compared to older adults (Robillard et al. Reference Robillard, Naismith, Smith, Rogers, White, Terpening, Ip, Hermens, Whitwell, Scott and Hickie2014; Alloy et al. Reference Alloy, Nusslock and Boland2015; Steinan et al. Reference Steinan, Lagerberg, Melle, Andersson, Morken and Scott2015). Batterham et al. (Reference Batterham, Glozier and Christensen2012) found that rumination and neuroticism mediated the relationship between self-reported sleep disturbance and new onset depressions in younger adults, but not the onset of generalized anxiety of panic disorders.
The above studies mainly relied on self-ratings rather than objective recordings of sleep. An exception is the study of university students (mean age about 20 years) by Pillai et al. (Reference Pillai, Steenburg, Ciesla, Roth and Drake2014), which showed that nightly variations in pre-sleep rumination were predictive of significantly longer sleep onset latency (SOL) as recorded by actigraphy and by a self-report diary. It was estimated that, after controlling for baseline sleep disturbance and depressive symptoms, a one standard deviation increase on the pre-sleep rumination scale was associated with an approximately 7-min increase in actigraphy-based SOL.
Physical health and immune system
Rumination has been found to be negatively associated with self-reported physical health, including higher levels of somatic complaints and lower general health (Lok & Bishop, Reference Lok and Bishop1999; Rector & Roger, Reference Rector and Roger1996). In a longitudinal study of younger compared to older adults, Thomsen et al. (Reference Thomsen, Mehlsen, Hokland, Viidik, Olesen, Avlund, Munk and Zachariae2004a ) demonstrated that higher levels of rumination predicted poorer self-reported physical health and more somatic complaints in those aged 20–35 years only. High levels of rumination have been linked with immune functioning, but to date these associations have only been reported for some of the immune markers measured (numbers of leucocytes, lymphocytes, and polyclonal activation), and the findings were significant in older but not younger adults (Thomsen et al. Reference Thomsen, Mehlsen, Olesen, Hokland, Viidik, Avlund and Zachariae2004b ).
Brosschot (Reference Brosschot2010) suggests that sustained cognitive representations of events (namely rumination and worry) can cause prolonged physiological activity, which may lead to intermediate pathogenic states (such as increased allostatic load) and finally to somatic disease. Glynn et al. (Reference Glynn, Christenfeld and Gerin2002) found that ruminating about an emotional task resulted in increased blood pressure and delayed blood pressure recovery, which parallel findings reported in students with high levels of rumination and in adults (Bermúdez & Perez-Garcia, Reference Bermúdez and Perez-Garcia1996; Neumann et al. Reference Neumann, Waldstein, Sollers, Thayer and Sorkin2001). Finally, although the co-morbidity between mood disorders and cardiovascular disease reported in young adults may be linked to medications or lifestyle factors (Goldstein et al. Reference Goldstein, Carnethon, Matthews, McIntyre, Miller, Raghuveer, Stoney, Wasiak and McCrindle2015), it is hypothesized that trait rumination may delay physiological recovery from acute stress and could act as a mechanism (Larsen & Christenfeld, Reference Larsen and Christenfeld2009) (Fig. 2).
Conclusions
This paper highlights several key aspects of rumination. First, we note that, of the two core components of rumination, it is the maladaptive (brooding) rather than the adaptive element (reflection or positive basking) that is consistently associated with the development of psychopathology. Also, the normative pattern of development of rumination parallels age and gender profiles associated with the typical evolution of internalizing disorders. Importantly, we highlight the association between the development of a ruminative response style and traumatic and abusive experiences in childhood, which are risk factors linked to a range of psychological problems in adolescence including mood and psychotic disorders. The evidence suggests that rumination is an underlying mechanism that contributes to a significant proportion of the explained variance between early adversity and later mental health problems. We do not claim that rumination is the only explanatory model, as other cognitive structures (e.g. beliefs and schemata) and processes have been implicated in the links between early trauma, CER and the development of psychopathology and acts of self-harm. Several studies demonstrate that these models and constructs may overlap and that there are links between early maladaptive schema, rumination and future symptoms of anxiety and depression in adolescents (Orue et al. Reference Orue, Calvete and Padilla2014; Black & Pössel, Reference Black and Pössel2015) or between early childhood trauma, over-general memory and high levels of ruminative thinking (Watkins & Teasdale, Reference Watkins and Teasdale2001; Williams et al. Reference Williams, Barnhofer, Crane, Herman, Raes, Watkins and Dalgleish2007). However, more research is needed to clarify the interactions between these different CER elements.
As reported in reviews of older adult populations, we confirm the importance of rumination in the evolution and maintenance of depression and highlight that in adolescence (but not always older adults) rumination may fully or partially mediate the relationship between childhood temperament and/or stressful events and the later onset of anxiety disorders. This sequence offers support for the notion of rumination being important in the longitudinal trajectory of the development of mental disorders and the notion that rumination plays a role in the transition between clinical stages. Our review differs from many previous reviews of rumination as a trans-diagnostic process operating across age groups and populations (Harvey et al. Reference Harvey, Watkins, Mansell and Shafran2004; Ehring & Watkins, Reference Ehring and Watkins2008; Watkins, Reference Watkins2009; Watkins & Nolen-Hoeksema, Reference Watkins and Nolen-Hoeksema2014), as we also examine the possible role of rumination in evolution of a problem from its sub-threshold phenomenology through to levels of harmful alcohol and substance use, bipolar and psychotic disorders that lead to help-seeking in an individual. Furthermore, we explore its putative influence on the trajectories of illness observed in this younger population and how similar processes may operate across physical and mental disorders. There is emerging evidence that rumination can be directly linked to the onset or maintenance of these problems in young adults, as well as existing evidence of indirect associations, with rumination exacerbating levels of anxiety or depressive symptoms, which in turn increase the distress that accompanies the symptoms or impede the ability to cope with those symptoms. It was also notable that rumination is frequently associated with suicidal ideation in depression, bipolar and psychotic disorders. We suggest that this is an important area for research, as the role of rumination in amplifying mood states and reducing flexibility in thinking styles and CER is under-explored in the age groups at the highest risk for onset of severe mental disorders or deliberate self-harm.
Evidence of the heritability of and neuropsychological pathways implicated in rumination is important as, for example, changes in the neural networks associated with CER may precede behavioural manifestations in unaffected high risk populations (Heissler et al. Reference Heissler, Kanske, Schonfelder and Wessa2014). Critically, this review suggests ruminative response style is a putative shared mechanism for the development of sleep and physiological dysregulation and health problems in young adults with evolving mental disorders. This is relevant as attempts to explain physical and mental co-morbidities on the basis of factors such as the adverse physical effects of treatment or reduced daytime activity (post-onset of mental disorder) have proven to be overly simplistic and fail to take into account findings of the high levels of physical and mental co-morbidity in untreated, early stage cases. It appears that a ruminative response style may be associated with circadian and HPA disruptions, and its relationship to physical disease is not driven by greater reactivity in systems, but instead through extending activation and increasing allostatic load, which may increase the risks for cardiovascular or other damage (Larsen & Christenfeld, Reference Larsen and Christenfeld2009). Indeed, Ottaviani et al. (Reference Ottaviani, Shapiro, Davydov, Goldstein and Mills2009) suggest that rumination represents an ‘autonomic phenotype’ because the associated autonomic dysregulation plays a role in the relationships between temperament, anxiety, depression and cardiovascular health.
In conclusion, this selective review of the association between rumination and the early clinical stages of mental disorders suggests that it is an important underlying trans-diagnostic process that operates in adolescents and young adults. Further, rumination shows a predictable developmental trajectory that is both detectable and modifiable. From the perspective of primary or early secondary prevention, modifying the maladaptive ‘toxic brooding’ component of rumination and substituting a more flexible response style that engenders a greater sense of self-control has the potential to reduce the onset or maintenance of problems such as depression and anxiety (Cook & Watkins, Reference Cook and Watkins2016), and may reduce the distress or severity of other disorders, such as psychosis and bipolar disorders (Vallarino et al. Reference Vallarino, Henry, Etain, Gehue, Macneil, Scott, Barbato, Conus, Hlastala, Fristad, Miklowitz and Scott2015; Scott, Reference Scott and Vieta2016). This review indicates that examination of rumination and other CER is an important, underexplored issue in trans-diagnostic and dimensional approaches to mental disorders, which is especially important given the apparent links to physical and well as mental health, and the prospects for modification of this risk factor.

Fig. 2. Model of rumination as a trans-diagnostic process impacting psychopathology and physical health, underpinned by genes and neural networks, age, gender, and temperament, and early environment. AUD, Alcohol use disorder; HPA, hypothalamic-pituitary-adrenal; SUD, substance use disorder.
Acknowledgements
A.G. has received grant funding from the National Health and Medical Research Council in Australia. I.B.H. is a Commissioner in Australia's National Mental Health Commission; a Member of the Medical Advisory Panel for Medibank; a Board Member of Psychosis Australia Trust. He has received honoraria for presentations of his own work at educational seminars supported by a number of non-government organizations and by the pharmaceutical industry (including Servier, Pfizer, AstraZeneca, and Eli Lilly) and funding from Servier for a study of major depression and sleep disturbance in primary-care settings. Other relevant funding for Professor Ian Hickie is in relation to this study includes ‘Testing and delivering early interventions for young people with depression’ (APP ID: 1046899). S.N. has received grant funding from the National Health and Medical Research Council including for research on sleep and actigraphy. J.S. is a visiting professor at the Brain & Mind Centre at The University of Sydney. J.S. has received UK grant funding from the Medical Research Council (including for projects on actigraphy and bipolar disorders) and from the Research for Patient Benefit programme (PB-PG-0609-16166: Early identification and intervention in young people at risk of mood disorders).
Declaration of Interest
None.





