Type 2 diabetes is a highly prevalent disease among the elderlyReference Papazoglou, Manes, Chatzimitrofanous, Papadeli, Tzounas, Scaragas, Kontogiannis and Alexiades1–Reference Castell, Tresserras, Serra, Goday, Lloveras and Salleras4 and the incidence of clinical diabetic complications in this population has been associated with glycaemiaReference Stratton, Adler, Neil, Matthews, Manley, Cull, Hadden, Turner and Holman5. Although the impact of diabetes control is less well known in the elderly population, it can be postulated that, like younger subjects, older diabetics could benefit from efficient control of their diabetes. Diet is the cornerstone of diabetes management. In type 2 diabetes, diet without additional anti-diabetic durgs is recommended as long as patients are meeting treatment goals, that is to say an glycosylated hemoglobin A1c (HbA1c) inferior to 7 %6. In a recent study in the UK, approximately one-third of patients with type 2 diabetes were managed by diet aloneReference Hippisley-Cox and Pringle7. This proportion could be even greater in the elderly population.
One of the objectives of diet is to assure an adequate ratio between carbohydrates and lipids, which contributes to improve insulin sensitivity, a major factor in type 2 diabetes care. Diet also has to ensure an adequate and sufficient energy intake, which is of paramount importance in elderly people. Even when anti-diabetic drugs are required, diet is still a major contributor to glycaemic control. Thus, analysis of diet among elderly diabetic subjects is of particular interest since increasing our knowledge of the nutritional behaviour of the elderly diabetic population should make it possible to adapt the nutritional advice given to this population.
Some studies have evaluated to what extent diabetic persons in the population follow dietary recommendationsReference Shimakawa, Herrera-Acena, Colditz, Manson, Stampfer, Willett and Stamper8–Reference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13. However, although most studies considered both insulin-dependent and non-insulin-dependent diabetesReference Shimakawa, Herrera-Acena, Colditz, Manson, Stampfer, Willett and Stamper8, Reference Parker, McPhillips, Lapane, Lasater and Carleton9, Reference Virtanen, Feskens, Rasanen, Fidanza, Tuomilehto, Giampaoli, Nissinen and Kromhout11–Reference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13, very few focused on the elderly populationReference Virtanen, Feskens, Rasanen, Fidanza, Tuomilehto, Giampaoli, Nissinen and Kromhout11, Reference Cruz and Calle-Pascual12 and study samples were often quite small. Moreover, to our knowledge, previous studies have compared the diets of diabetic subjects with those of non-diabetic subjects. However, only one previous study has investigated the discrepancy between diet and nutritional recommendations in diabeticsReference Cruz and Calle-Pascual12.
We hypothesised that diet of elderly diabetic subjects differs from that of non-diabetic ones but is not totally in line with nutritional recommendations for diabetic subjects. To test this hypothesis, we compared nutritional behaviours of diabetic subjects, first with non-diabetic subjects and then with nutritional recommendations for diabetics within the Three City (3C) Study, a French population-based cohort study of subjects aged 65 years and over designed to study the main vascular and neurodegenerative pathologies related to ageing.
Materials and methods
Design of the study
The present study was part of the 3C Study, a collaborative research programme based on a longitudinal cohort of 9294 subjects aged 65 years and over. The main objective of this cohort is to estimate the risk of dementia and cognitive impairment attributable to vascular factors and to define target groups for future preventive strategies14.
Participants were recruited between March 1999 and March 2001 in three French cities: Bordeaux (2104 participants included), Dijon (4931) and Montpellier (2259). Details of the 3C Study are reported elsewhere14. To be eligible, people had: (1) to be aged 65 years or over, (2) to be living in one of the selected districts of the three cities and registered on the electoral rolls, and (3) not to be institutionalised. The study protocol was approved by the Ethical Committee of the Kremlin-Bicêtre University Hospital. Data collection included measurements and examinations common to the three centres, principally related to the central objective of the 3C Study. Additional data have been collected for centre-specific ancillary studies.
Population
The present paper is based on the data of the Bordeaux centre collected at the 2-year follow-up of the cohort. At this time, the Bordeaux centre had planned specific dietary objectives and had collected additional data on nutritional habits. Among the 2104 subjects initially included in the Bordeaux centre, 1761 (83·7 %) were visited in 2001–2. A total of 1661 (94·3 %) of them had a nutritional evaluation during this follow-up. After exclusion of three subjects with extremely low energy intake (less than 2092 kJ (500 kcal)) on the 24 h recall, 1658 subjects were included in the present study.
Data collection
Data were collected during a face-to-face interview using a standardised questionnaire administered by trained psychologists. Data collection included sociodemographic variables, habits, personal medical history, current symptoms and diseases including diabetes, an inventory of all drugs used daily or regularly during the preceding month and anthropometric data (including height and weight). A fasting blood sampling, including fasting glucose level, was performed at the inclusion of the cohort but not repeated at this follow-up. Dietary information was collected by a specifically trained dietitian who administered a FFQ and a 24 h dietary recall. The FFQ was adapted from the questionnaire used for inclusion in the SU.VI.MAX (SUpplémentation en VItamines et Mineraux AntioXydants) randomised controlled studyReference Hercberg, Preziosi, Briancon, Galan, Triol, Malvy, Roussel and Favier15. The FFQ asked for the usual frequency of consumption of broad categories of food and beverages at each meal and in intervals. During the 24 h recall, the dietitian registered all the meals and beverages consumed at any time during the previous day. Portion sizes were estimated by a picture booklet16 edited for the SU.VI.MAX studyReference Hercberg, Preziosi, Briancon, Galan, Triol, Malvy, Roussel and Favier15. Then estimation of the daily nutrient intake of each participant was obtained using BILNUT software© (release 4.0, SCDA Nutrisoft, Cerelles, France) which includes food composition tables for FranceReference Favier, Ireland-Ripert, Toque and Feinberg17. At the end of the interview, the dietitian evaluated the reliability of the information provided by the subject based on the global coherence of the record and the cognitive abilities of the respondent. We excluded subjects for whom the report was judged as unreliable. For the same reason, we excluded demented participants from the sample. The validity of dietary questionnaires has been previously assessed by evaluating the association between total fat intake estimated from the 24 h recall and TAG assessed at baselineReference Feart, Jutand, Larrieu, Letenneur, Delcourt, Combe and Barberger-Gateau18. In addition, fish consumption frequency evaluated by the FFQ was also linked to the estimated EPA and DHA intakeReference Feart, Jutand, Larrieu, Letenneur, Delcourt, Combe and Barberger-Gateau18.
Diabetes diagnostic procedure
The presence of diabetes was evaluated on a self-reported diagnosis of diabetes and/or a consumption of insulin or oral hypoglycaemic agents. In order to ensure that the non-diabetic group did not include any diabetic subjects, results of the fasting glucose level obtained at the baseline phase of the cohort were also taken into account. Thus, subjects who did not report diabetes but were classified as hyperglycaemic (fasting glucose level between 6·1 (included) and 7 (excluded) mmol/l) or diabetic (fasting glucose level equal or over 7 mmol/l) on the blood sample at baseline were excludedReference Alberti and Zimmet19; in addition, subjects who did not report diabetes and had no blood sample at baseline were also excluded.
Other variables
Age, sex, marital status (married or living together, widowed, never married, and divorced or separated) and living conditions (alone or not) were considered. Educational level was evaluated on two levels, at least primary school level validated by a diploma, versus no diploma (low level). BMI was calculated (weight/size2) in kg/m2.
Data analysis
The Statistical Analysis Systems statistical software package version 8.2 (SAS Institute, Cary, NC, USA) was used. Student's t test (for quantitative data) and χ2 test (for qualitative data) were used to compare socio-demographic characteristics and food consumption by groups. Nutrient intake has been presented in absolute values and nutrient densities for diabetic and non-diabetic subjects. Because of differences in diet between men and women, at least in total energy intake, most of the results are presented separately for men and women.
To compare nutrient intake between diabetic and non-diabetic subjects, linear regression models adjusted for age and educational level have been performed. Because of a significant interaction between gender and nutrient intake, these models have been performed separately for each sex. Statistical assumptions for these models have been verified graphically.
To evaluate the discrepancy between nutritional behaviours and nutritional recommendations in diabetic subjects, indicators of consumption were created for the three nutrient densities (carbohydrates, fats and protein), saturated fats and cholesterol. In France, nutritional recommendations for diabetic subjects in 2000 mention that consumption of carbohydrates should be between 45 and 50 % of total energy intake, total fats between 25 and 35 % and protein between 10 and 20 %20. As data in the 3C Study were collected in 2001–2, we chose to refer to these recommendations rather than more recent ones. At first, only consumption of carbohydrates was considered. Then, consumption of less than 300 mg cholesterol and less than 10 % of daily energy intake was also evaluated. As French recommendations differed slightly from American and European recommendations21, 22, we also evaluated the proportion of subjects for whom consumption was not in compliance with those recommendations which advise more than 60 % of daily energy intake as carbohydrates and monounsaturated fats.
Results
The initial sample consisted of 1658 subjects who underwent nutritional evaluation at the 2-year follow-up of our cohort. Among them, we excluded 107 subjects for whom dietary information was judged to be unreliable, due to a diagnosis of dementia (n 75), or based on the judgement of the dietitian (n 32). In order to avoid misclassification, we excluded 195 subjects who declared they were non-diabetic at this follow-up: 140 of them because they did not provide a blood sample at the baseline examination and fifty-five who had nevertheless hyperglycaemia in their blood sample at baseline. Finally, twenty subjects who were diagnosed as diabetic at the baseline phase of the study but who did not report diabetes at this follow-up were also excluded. Our final working sample therefore consisted of 149 diabetic participants and 1187 non-diabetic participants.
Characteristics of the diabetic and the non-diabetic sample according to gender are described in Table 1. Diabetic subjects were more often men (54·4 % of men among diabetics compared to 35·9 % among non-diabetics, P < 0·0001), but did not differ by age (76·0 years for diabetics and 75·9 for non-diabetics, P = 0·73). Diabetic women had a lower level of education than non-diabetic women. As expected, BMI was greater among diabetic than non-diabetic subjects, especially for women, with a BMI 3·9 higher for diabetic women than for non-diabetic ones (P < 0·0001).
Table 1 Principal characteristics according to sex and the diagnosis of diabetes, Three City Study, 2001–3
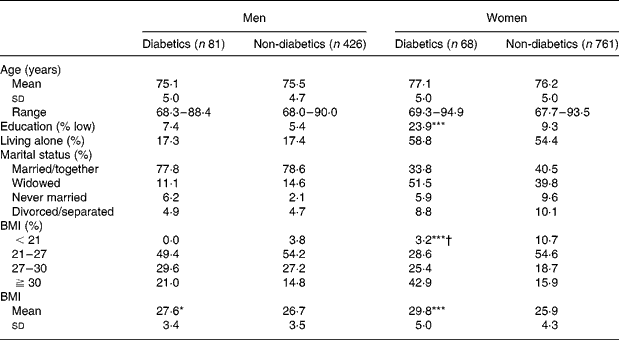
Values were significantly different from those of the non-diabetic subjects for each sex (Student's t test for quantitative variables and χ2 test for qualitative variables): *P < 0·05; ***P < 0·001.
† Global P value for the BMI categories.
Food consumption
Six non-diabetic subjects did not answer the FFQ and the results for food consumption are thus based on 1330 subjects. The number of meals per day, including snacks, was lower for diabetic women compared to non-diabetic women, whereas no difference was observed in men (Table 2). Only two diabetic subjects declared having only two main meals instead of three (breakfast, lunch and dinner). In men, fruit consumption per week was slightly more frequent among diabetic than among non-diabetic subjects as well as meat consumption. However, in women, no differences in consumption of fruit, vegetable, meat, pork-meat and fish were observed between diabetic and non-diabetics. On average, 87·3 % of the diabetic subjects ate at least one piece of fruit a day and diabetic subjects ate about three vegetables a day. Non-diabetic subjects ate sweet foods more often than diabetic subjects, particularly for breakfast and also as snacks between meals for men. About 36 % of non-diabetic subjects reported nibbling sweets between meals regularly (i.e. at least five times a week), compared to 21·5 % of diabetic subjects (P < 0·0003). The use of artificial sweeteners was more frequent for diabetic subjects with more than half of them (51·0 %) adding an artificial sweetener to their drink regularly at breakfast, compared to 13·0 % of the non-diabetic subjects.
Table 2 Food frequency consumption according to sex and the diagnosis of diabetes, Three City Study, 2001–3
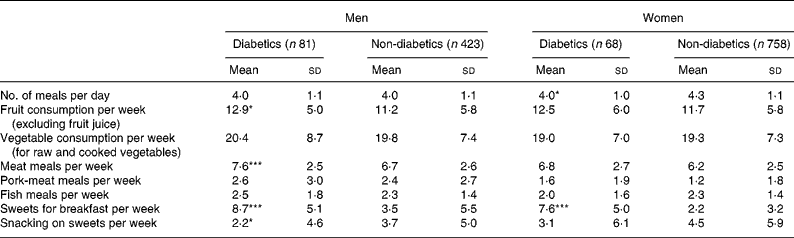
Mean values were significantly different from those of the non-diabetic subjects for each sex (Student's t test): *P < 0·05; ***P < 0·001.
Energy and nutrient intake
Table 3 shows the absolute values of nutrient intake, assessed with the 24 h recall, for both sexes according to diabetic status. Comparisons between diabetic and non-diabetic subjects have been performed using linear regression models, separately for each sex. Adjusted for age and educational level, energy intake the day before significantly differed between diabetic and non-diabetic subjects only for women, with a lower energy intake for diabetic women.
Table 3 Nutrient intake in absolute values assessed with the 24 h recall among diabetic and non-diabetic subjects according to sex, Three City Study, 2001–3

Mean values were significantly different from those of the non-diabetic subjects for each sex (linear regression models adjusted for age and educational level): *P < 0·05; **P < 0·01; ***P < 0·001.
Compared to non-diabetic men, diabetic men had a lower intake of carbohydrates, essentially due to a lower intake of mono- and disaccharides, and a higher intake of protein (Table 3). Fibre intake was also higher in diabetic men. As for men, intake of carbohydrates was also lower for diabetic women, but not accompanied by an increase in another nutrient, with thus a lower energy intake overall. The lower intake of carbohydrates in diabetic women was essentially due to a lower intake of mono- and disaccharides. Regarding intake of polysaccharides, there was no significant difference between diabetics and non-diabetics, neither for women nor for men. Alcohol intake was also lower in diabetic women.
Similarly, the comparison of nutrient densities evidenced a lower carbohydrate intake for diabetic subjects, and notably a lower mono- and disaccharide intake whatever the sex (Table 4). This reduction in carbohydrate intake was done simultaneously with a slightly higher intake of protein and fats. However, distribution of subtypes of fats (saturated, monounsaturated and polyunsaturated) was similar for diabetic and non-diabetic subjects for both sexes.
Table 4 Nutrient intake in nutrient densities (%) assessed with the 24 h recall between diabetic and non-diabetic subjects according to sex and comparisons with dietary recommendations, Three City Study, 2001–3

Mean values were significantly different from those of the non-diabetic subjects for each sex (linear regression models adjusted for age and educational level): *P < 0·05; **P < 0·01; ***P < 0·001.
† Agence Nationale d'Accréditation et d'Evaluation en Santé20.
Comparison with nutritional recommendations
Proportions for nutrient densities for diabetic men and women are displayed in Table 4. About 84 % of the diabetic subjects did not consume between 45 and 50 % of their daily energy intake as carbohydrates as recommended, with about two-thirds (63·8 %) consuming less than 45 %. Even with less restrictive criteria, 43·0 % of our diabetic subjects consumed less than 40 % of their daily energy intake as carbohydrates. In addition, although 61·1 % of the diabetic subjects consumed less than 300 mg cholesterol, only 20·8 % consumed less than 10 % of daily energy intake as saturated fats. When all the criteria were combined, only one diabetic subject was totally in compliance with the nutritional recommendations. In addition, regarding the American and European recommendations, 77·2 % of the diabetic subjects consumed less than 60 % of daily energy intake as carbohydrates and monounsaturated fats.
Discussion
The present study on the food habits of elderly subjects showed that food behaviour differed between diabetic and non-diabetic subjects, particularly with a lower intake of carbohydrates, essentially due to a lower intake of mono- and disaccharides. However, food behaviours of diabetic subjects did not seem to be appropriate since consumption of carbohydrates was too low in these elderly diabetic subjects and about two-thirds of them were not in line with the recommendations and consumed less than 45 % of daily energy intake as carbohydrates. Moreover, protein intake was high in diabetic men.
Compared to nutritional recommendations, total energy intake appears to be relatively low in the present results, particularly among women. However, total energy intake reported in the present study was similarReference Virtanen, Feskens, Rasanen, Fidanza, Tuomilehto, Giampaoli, Nissinen and Kromhout11, Reference Koehler, Hunt and Garry23, Reference Bamia, Orfanos and Ferrari24 or only slightly lowerReference Shimakawa, Herrera-Acena, Colditz, Manson, Stampfer, Willett and Stamper8, Reference Cruz and Calle-Pascual12, Reference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13, Reference Haveman-Nies, Tucker, de Groot, Wilson and van Staveren25 compared to previous evaluations in diabetic subjects or healthy elderly. When lower, these differences could be partly explained by the fact that our population was older. Although the present results were comparable to previous ones, under-reporting of intake cannot totally be ruled out. Indeed, in the present population, although total energy intake appears to be relatively low, BMI is high among diabetic subjects. Even if nutritional assessment was performed in the same way in diabetic and non-diabetic subjects and was part of an epidemiological study whose primary objective was not nutrition, a selective under-reporting of restricted foods among diabetic subjects cannot be ruled out. However, previous studies with similar reports of energy intake consistently found a high BMI among diabetic subjectsReference Shimakawa, Herrera-Acena, Colditz, Manson, Stampfer, Willett and Stamper8, Reference Parker, McPhillips, Lapane, Lasater and Carleton9, Reference Virtanen, Feskens, Rasanen, Fidanza, Tuomilehto, Giampaoli, Nissinen and Kromhout11–Reference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13.
The present results were based only on one 24 h recall of food consumption. Thus, for an individual, it does not reflect his/her regular food habits, since diet varies from day to day. However, it represents mean values for the groups of diabetic and non-diabetic subjectsReference Willett and Willett26. One limitation in this method is that the within-person variation is such that the median tends to be correct, but the variance is increasedReference Beaton, Milner and Corey27, Reference Beaton, Milner, McGuire, Feather and Little28. In the present study, the 24 h recall was assessed using food photographs which generally have a positive influence on the relative validity for absolute food group intakeReference Fraser29. In addition, although validity has not been evaluated for each nutrient, dietary assessment methods have been previously validated for fat intakeReference Feart, Jutand, Larrieu, Letenneur, Delcourt, Combe and Barberger-Gateau18, Reference Willett, Stampfer, Chu, Spiegelman, Holmes and Rimm30 and the mean energy intake was positively associated with the intensity of physical activity in the present studyReference Feart, Jutand, Larrieu, Letenneur, Delcourt, Combe and Barberger-Gateau18.
Nevertheless, the present results are very close to previous results in a younger French populationReference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13. This replication of results, in a similar population but of different age, limits the risk of methodological bias. For many diabetic subjects in the present population, nutritional behaviour appears to be different to the French nutritional recommendations for diabetic persons. Indeed, many diabetic subjects in the present population consumed fewer carbohydrates than recommended. Yet, this population has a modified diet compared to the non-diabetic population. The decrease of mono-/disaccharide consumption, of alcohol consumption for women and the increase of artificial sweetener consumption bear witness to these modifications, but they seem partly inadequate. This is probably due to the fact that the current belief for diabetes is that people need to avoid sugar and many diabetic people are not aware of the necessity of high carbohydrate consumption and an adequate carbohydrate/lipid ratio. Thus, nutritional information should clearly underline the main messages.
In France, dietary recommendations directed towards subjects with type 2 diabetes do not specifically include the consumption of monounsaturated fats, except for subjects with abdominal obesity, hypertriglycaeridemy, and low HDL-cholesterol20. These cases apart, the main recommendation is that carbohydrates should provide about half the total energy intake21. When considering this recommendation, only one-third of the diabetic subjects consumed enough carbohydrates. Moreover, because of increased within-person variation due to use of the 24 h recall, the actual percentage of people who habitually eat less than 45 % of energy from carbohydrates is probably greater than the estimated value. The proportion of subjects in line with nutritional recommendations has rarely been provided directly in previous published data. Even if results cannot be compared directly since recommendations differ across countries, the present result appear to be in contradiction with previous data in a Spanish population, where more than 80 % of the patients complied with the recommendation of consuming more than 60 % of daily energy intake as carbohydrates and monounsaturated fatsReference Cruz and Calle-Pascual12. However, consumption of carbohydrates was relatively low in this Spanish population, about 38 % of total energy; the high compliance with recommendations was explained by a very high consumption of fats (almost 40 %, including about 56 % of monounsaturated fats), which appears to be a common nutritional habit in Spain rather than respect of nutritional recommendations in this diabetic population. In other studies, the mean consumption of carbohydrates and monounsaturated fats was lower than 60 % in two of the three countries in the Seven Countries StudyReference Virtanen, Feskens, Rasanen, Fidanza, Tuomilehto, Giampaoli, Nissinen and Kromhout11 and also in FranceReference Gauthier-Chelle, Mennen, Arnault, Rigalleau, Hercberg and Gin13.
The low intake of carbohydrates in the present diabetic population leads to an imbalance between carbohydrates and lipids, which hampers the action of insulin. Thus, this nutritional behaviour of reducing carbohydrate intake is deleterious for the management of these diabetic patients, making it more difficult to obtain glycaemic control and probably increasing the vascular risk associated with diabetes.
Beyond the low intake of carbohydrates in the present diabetic population, the difference between diabetic men and women in nutritional behaviour is of particular interest. Indeed, diabetic women decrease their nutritional intake whereas diabetic men increase their protein consumption. Both of these are risk behaviours. The decrease in energy intake can lead to malnutrition in women. Thus, although high BMI is problematic, nutritional recommendations for this population should be cautious and not too restrictive. In men, the high intake of protein constitutes a risk for renal function, particularly in the case of nephropathy, which may be frequent in this population.
For non-diabetics, in comparison with the French recommendations for the elderly, protein intake was slightly higher and mean carbohydrate intake was lower. However, despite a mean increase of protein intake, a previous paper on the same population evidenced that 44 % of the elderly consumed lower than 1 g protein/kg per d, suggesting that some protein-energy malnutrition occurs in the elderly, putting them at higher risk of sarcopaeniaReference Feart, Jutand, Larrieu, Letenneur, Delcourt, Combe and Barberger-Gateau18. Despite an adequate intake of total fat, non-diabetics had an excessive intake of saturated fat compared to the current French recommendations, concomitant to a low monounsaturated fat intake. This latter result confirms that the French diet is not perfect despite a relatively low incidence of heart diseases.
The present results offer several clues on how to improve nutritional recommendations for the elderly population. Although the diet of diabetic subjects differs from that of non-diabetic subjects, it is not totally in line with nutritional recommendations. The message is probably poorly understood or distorted. Thus, nutritional advice should focus on the main messages such as the need for a large quantity of carbohydrates and moderate protein consumption, as well as the need to avoid malnutrition in the diabetic population.
Acknowledgements
The 3C Study is conducted under a partnership agreement between the Institut National de la Santé et de la Recherche Médicale (INSERM), Victor Segalen Bordeaux 2 University and the Sanofi-Synthélabo Company. The Fondation pour la Recherche Médicale funded the preparation and initiation of the study. The 3C Study is also supported by the Caisse Nationale Maladie des Travailleurs Salariés, Agence Française de Sécurité Sanitaire des Produits de Santé, Direction Générale de la Santé, Conseils Régionaux of Aquitaine and Bourgogne, Fondation de France, Ministry of Research-INSERM Programme ‘Cohortes et collections de données biologiques’. The present study was supported by a grant from the Association Internationale pour la Recherche sur la Maladie d'Alzheimer (AIRMA).






