INTRODUCTION
Along with funding and leadership, governance has an important impact on the performance of an academic department, division, or section of emergency medicine (EM). Governance structures and processes are a means to an end. They are not an end unto themselves. The purpose of an EM academic structure is to facilitate and enable excellence in the mission of academic medicine, including research, education, and, ultimately, patient care.Reference Brimacombe 1 Different academic units of EM will put different emphasis on each element of the mission. (For the purposes of this article, departments, divisions, and sections of EM will be referred to collectively as academic units of EM.) Good governance facilitates meeting the strategic goals and fiduciary responsibilities of the academic units of EM, and creating the ability to respond to system challenges and opportunitiesReference Chalt, Ryan and Taylor 2 in an era of rapid change in academic medicine and health system reform.Reference Daschle 3
While there is an established matrix of governing bodies, institutions, and regulations with which an academic unit of EM must align and integrate, this paper will focus on two practical levels of governance: 1) the relationship between individual emergency physicians and their academic unit of EM; and 2) the relationship between the academic unit of EM and its parent faculty of medicine or academic health centre. Given that there is a significant cause-and-effect relationship between funding streams, local politics, and health systems organization, it is no surprise that there is a wide variation of governance structures in academic EM.
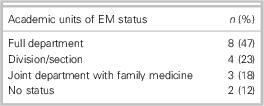
This paper aims to make sense of the strengths and challenges of the current governance structures, and make recommendations on principles and general approaches that may guide improvements in governance at both levels. Specific how-to steps will require significant context-dependent analysis, consultation, and understanding of specific university (or health authority models), and are beyond the scope of these recommendations. It is clear that no one size will fit all (Table 1).
Table 1 Status of the 17 academic units of EM within the Canadian faculties of medicine
METHODOLOGY
Expert panel and literature review on governance
Eight established medical leaders from across Canada were identified for their contributions to the EM community and were asked to form a governance panel. The panel met by teleconference four times and was supported by the Academic Section of the Canadian Association of Emergency Physicians (CAEP). All members reviewed the governance literature and discussed individual experiences to identify 1) the elements of governance; 2) the relationships between emergency physicians and academic units of EM, and between the academic unit of EM and faculty of medicine; 3) current status of governance in Canadian academic units of EM; and 4) essential elements of good governance. This discussion culminated into six recommendations around three themes: 1) the importance of good governance; 2) the purposes of an academic unit of EM; and 3) essential elements for better governance for academic units of EM. The panel presented the findings at the CAEP Academic SymposiumReference Sherbino, Van Melle and Bandiera 4 - Reference Vaillancourt, Rowe and Artz 10 held in Edmonton, Alberta, on May 30, 2015, to about 80 attendees, who were predominately emergency physicians with interests in governance, administration, and leadership. Their feedback, as well as comments gathered subsequent to the electronic distribution of the recommendations to the CAEP Academic Section, were discussed by the panel, and the recommendations were updated by panel consensus.
What is governance? How does it relate to funding and leadership in academic EM?
As soon as there are more than two people making a decision, especially if there is money involved, then there is a governance challenge. While the Institute on Governance (http://www.iog.ca) acknowledges that the complexity of governance is difficult to capture in a simple definition, they did stipulate that “governance determines who has power, who makes decisions, how other players make their voices heard, and how account is rendered.” 11 In the context of academic EM, the academic unit becomes essential in organizational decision-making and accountability. Although effective governance models contribute to organizational performance, often “we don’t think about or debate governing; we just do it.” Reference Chalt, Ryan and Taylor 2 In its simplest concept, the purpose of governance in academic units is to facilitate engagement (in the academic mission) and trust (in the decision-making by leadership) within the faculty.
The mission of academic medicine is supported by three foundational pillars: governance, leadership, and funding. For the purpose of this analysis and accompanying recommendations, governance has been differentiated from leadership development and funding, with respect to its influence on the academic unit’s performance and effectiveness. In practice, it is difficult to separate these interdependent relationships. For example, local traditional funding streams have likely had a significant impact on an academic unit’s decision-making around resource allocations, while institutional leadership precedence has shaped the evolution of governance structures and processes. Nonetheless, the three elements together provide the wherewithal to optimally improve the performance of the academic unit of EM.
Two separate, but interdependent levels of governance
For these recommendations, two levels of governance were considered. The first level governs the relationship between individual physicians and the academic unit of EM. The second governs the relationship between the academic unit of EM and the faculty of medicine. It is important to recognize that good governance of internal affairs (i.e., decision-making around the academic unit structures and processes) does not require independent academic departmental status at the university level. Conversely, full academic departmental status does not guarantee good governance over the practical day-to-day performance and decision-making of the department. Excellence in academic performance may be achieved by an academic unit of EM operating from any position (Figure 1). The obstacles to achieving full independent academic departmental status may differ from those that affect internal performance regardless of the academic unit governance model.

Figure 1 The levels of governance and their influence on full EM departments or divisions/sections/units of EM.
As individual academic units of EM evaluate their own status (see Appendix 1: Self-evaluation questions) and identify in which quadrant they fit (see Appendix 2: Key aspects list for good internal governance), more customized strategies and advice can be generated to improve governance in service of academic excellence. The how-to steps from C→A will be different from D→B, which, in turn, will be different from B→A (see Figure 1).
Governance theme 1: Governance is important to the academic units of EM
Governance is important because it determines who makes what decision, and how these decisions are made. 11 In an effort to give governance some practical relevance, it has been reframed as an aspect of leadership.Reference Chalt, Ryan and Taylor 2 This framework should be kept in mind as this question is asked: Do the structures and processes of the governance of academic EM support the ability of the academic unit of EM to make fiduciary, strategic, and generative (adaptive) decisions in the service of the academic mission?
Fiduciary decision-making is the stewardship of tangible assets in alignment with financial and legal obligations, accountability to senior organizations (i.e., payers, partners, stakeholders), and accountability to individual members and constituent interests. Strategic decision-making involves setting the academic units’ course and priorities (i.e., mission, vision, values), and deploying resources appropriately. Generative (or adaptive) decision-making refers to the role of framing problems and making sense of ambiguous situations, as well as ensuring that academic units can evolve, adapt, and respond to uncertainty and changing environments.Reference Chalt, Ryan and Taylor 2
As with the codification of corporate memory, group values, and organizational culture, the governance structure and policies become the user’s manual for the chair (or chief) of the academic units of EM, and its other leaders. If this user’s manual is well thought out and robustly structured, this can create the conditions of trust and engagement necessary for the academic unit. If this is not the case, the chair (with or without a leadership team) must create or improve those aspects of internal governance that do not align with the mission and values.
In a recent article entitled, “Predictors of Workplace Satisfaction for U.S. Medical School Faculty in an Era of Change and Challenge,”Reference Bunton, Corrice and Pollart 12 it was found that departmental (and medical school) organization, governance, and transparency were highly consistent predictors of faculty satisfaction across all surveyed schools and models. The authors suggested “that a culture characterized by open communication, consistency in decision-making, and opportunities for faculty input contributes to faculty perceptions of their worth to their institution and of institutional equity, all of which foster satisfaction.”Reference Bunton, Corrice and Pollart 12
Along with leadership and funding, governance can have an important impact on the academic unit of EM policy development, decision-making, and effectiveness. Governance must not be taken for granted.
Recommendation 1: There should be a deliberate approach to defining, implementing, and reviewing governance structures, processes, and desired outcomes.
Governance theme 2: The purpose of the academic unit of EM
Because governance is a means to an end, the goals of an academic unit of EM must be defined before clear recommendations can be made around the best governance model to achieve the desired outcomes. For the sake of this discussion, the vision of the CAEP Academic Section of EM will be used to articulate that purpose. The vision of the Academic Section is to promote high-quality emergency patient care by conducting world-leading education and research in EM (caep.ca/AcademicSectionOverview). By extension and for the development of recommendations, the raison d’être of any given academic unit of EM is to improve patient outcomes through better education and impactful research (Figure 2). This aligns with the arguments made by the “One future, three missions” white paper on the future of Academic Health Science Networks in Canada.Reference Brimacombe 1 As academic units within those academic health science networks, EM must have aligned roles and responsibilities.

Figure 2 The relationship between the tripartite mission of academic medicine (outlined in black) and its leadership, governance, and funding.
That is not to say that all academic units of EM across the country will, or should, put equal emphasis on the three missions (see Figure 2). In some medical schools, the chair of the academic unit of EM is separated from any direct patient care oversight or responsibility, whereas, in others, the health authority (or university by-laws) has intentionally combined the roles in a joint appointment, albeit with site chief positions responsible for day-to-day clinical operations. Even in settings focused solely on academic leadership, the ultimate goal will always be to improve patient care. It is understood that different universities will put more or less emphasis on the elements of the academic mission and have different governing by-laws. There is no standard formula for governance structures in academic EM. This limits the ability to make specific recommendations about what governance structure will work best for academic EM.
Further preventing such recommendations is that academic units of EM are evolving in an era of accelerating change in academic medicine and health care reform.Reference Daschle 3 , Reference Borden, Mushlin and Gordon 13 - Reference Ferris, Singer and Naylor 17 The expectations of an academic unit of EM now exceed the traditional scholarship of education and research roles.Reference Boyer 18 This is having a significant effect on the imperative to acquire novel leadership skills and must be considered when designing resilient and adaptive governance models.Reference Kastor 19 - Reference Thoma, Poitras and Penciner 23 Elner et al. in a recent article entitled, “Health Systems Innovations at Academic Centers: Leading in a New Era of Health Care Delivery,” argued that with the increasing imperative to improve patient experience, population outcomes, and reduce or stabilize system costs, academic health care centres have an opportunity “to create new approaches to service delivery and to nurture leaders of transformation.” They argued that an increasingly important role of academic medicine is to foster health systems innovation (as distinguished from biomedical research and continuous quality improvement), and that this should be recognized through more inclusive promotions criteria, valued through more robust funding opportunities, and embedded in new curricula for trainees.Reference Ellner 14
The implications of this are twofold: 1) Because EM is now seen as an active partner and positive catalyst for change, a strong and mature voice at the decision-making and problem-solving tables will be required, and 2) the traditional differentiation between the strategic priorities of the clinical department and the academic department will require more integrated and synergistic governance structures.
The current calls for leadership and structures to support the new opportunities for academic medicineReference Wartman 24 were entirely predicted (and likely influenced) by Boyer’s report on “Scholarship Reconsidered.”Reference Boyer 18 In many ways, academic EM has been a leader in moving towards these more integrative and less traditional forms of scholarship. Boyer defined scholarship as more than just-publish-or-perish research, and more than just teaching and curriculum development for education. He emphasized the importance of the scholarship of integration (i.e., giving meaning to isolated facts, putting them in perspective, making connections across disciplines, placing the specialties in a larger context, illuminating data in a revealing way) and the scholarship of application (i.e., applying knowledge to consequential problems to help individuals and institutions, problems themselves become the scholarly agenda).Reference Boyer 18
Given the previous, the academic unit may not be easily separated in purpose (and therefore governance structure) from the clinical unit. Whether the health authority and university by-laws formally recognize this, the practical implications that this will have on the future academic unit of EM organization and decision-making must be considered.
Recommendation 2: No two academic units of EM are the same. The ideal governance structure for any given academic unit of EM should be aligned with the local institutional by-laws, organizational cultures, and relative emphasis that the academic unit of EM puts on the interdependent missions of academic EM (patient care/health system innovation, research, and education).
Current governance models in Canadian academic units of EM
During 2014 and 2015, a survey of the chairs of EM in the 17 medical schools was conducted. A structured 84-question survey was followed up by clarifying questions and probes to determine various aspects of each academic unit of EM’s governance status and management structure. A full report on the results of this survey is being preparedReference Stiell, Artz and Lang 25 and forms the background context of these recommendations. The data were informative with respect to administrative structures (e.g., program leadership positions and funding) to describe how various academic units of EM are organized across the country. As the academic chairs/heads evolve their collaboration in the near future, there may be more opportunities to share and publish information about how each academic unit of EM determines who has power, who makes what decisions, how other players make their voice heard, and how account is rendered. 11 Along with Figure 1, other highlights about Canadian academic units of EM from the CAEP environmental scan include the number of directors in education and research (Table 2) and the listing of division and selection affiliations (Table 3).
Table 2 Number of education and research directors at 17 academic units of EM across Canada
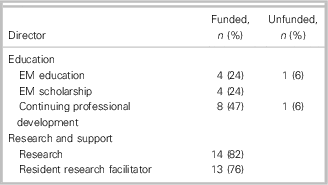
Table 3 The affiliations for the divisions and sections of EM (n=4) (X having multiple affiliations)
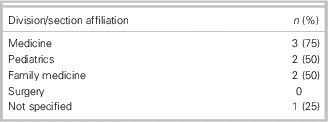
The three pathways to credentialing in the discipline of EM (FRCP, CCFP[EM], and FRCP PedsEM) must be considered as EM academics move towards better governance models. These distinct pathways have contributed to some of the fragmentation of the academic mission in EM at various medical schools. They have also contributed to the complicated matrix of reporting to parent departments that some academic units of EM are still navigating (see Table 3). As EM works towards better clinical care, innovative systems of EM, and better research and education, the governance model of academic EM can be used as a catalyst to integrate the academic mission, vision, and values of EM under one umbrella. Ideally, this would not be seen as a threat to any one group, but rather as an opportunity for integration and collaboration.
Governance theme 3: Essential elements of good governance
In general, there are five elements of good governance (legitimacy and voice, strategic direction, performance, equity and fairness, transparency and accountability),Reference Sheng 26 which can be adapted to the academic unit of EM. Appendix 1 illustrates practical examples of these five principles and what they might mean at the two levels of academic unit of EM governance (with a sixth category of general [and other] questions of governance to consider).
Better governance at both levels for academic units of EM
Revisiting Figure 1, it is important for academic units of EM leadership and faculty to reflect upon where they may sit in the 2×2 table in order to best improve their governance. With regards to internal governance, consideration should be given to the key aspects list of governance principles that may come into play at this level (see Appendix 2).
Recommendation 3: Internal governance structures govern the relationship between the academic unit of EM and the constituent academic programs, and the individual physicians. The academic unit of EM should consider implementing the key aspects of good internal governance in their design (while modifying to local contexts).
When it comes to the question of whether a division or section of EM should become a full academic department (see Appendix 3), there are several considerations.Reference Hamilton, Nelson and Scalea 27 The overarching prerequisite is knowledge of the local context and culture of the university and faculty of medicine. Several questionsReference Hamilton, Nelson and Scalea 27 must be asked:
-
1) Would the academic unit of EM have advantages as a full department? Is the performance of research and education, as well as the likelihood of future academic opportunities, likely to improve by establishing this formal structure?
-
2) How effective are current resources and influence with parent departments(s)? Will they be improved as a department, or is there too much political or fiscal risk?
-
3) Is the current unit sufficiently mature to meet the criteria for a department? Does the academic unit of EM have a good track record? Does the academic unit of EM’s research and education output need to improve first? Would the current chief qualify as a chair or would a new search and survey be required?
-
4) Is the internal governance organization optimized to ensure academic excellence with the current funding streams and leadership?
-
5) Is now a good time, or are there political or fiscal realities that make this a risk or too large of an endeavor (at this time)? If not now, when?
If the reasons to become a department (see Appendix 3) are felt to be compelling,Reference Hamilton, Nelson and Scalea 27 , Reference Derlet 28 and the initial questions do not dissuade, then the hard work starts. There is no algorithm for how to become a full academic department, but there are some strategiesReference Hamilton, Nelson and Scalea 27 to create the conditions for the emergence of an EM department.
-
1) Build the respect for, and reputation of EM over time, especially in research and education, but also in clinical care, one patient at a time.
-
2) Articulate a vision of improved patient care, population outcomes, and innovative system design fostered by excellence in EM education and research.
-
3) Become a student of the culture at the university faculty of medicine and health science centre.
-
4) Know the criteria and process of your application to the university.
-
5) Understand the priorities and values of the dean and the CEO of the health science centre(s), and frame the prospective department’s priorities with these.
-
6) Build coalitions (especially with the chairs of surgery, medicine, family medicine, and pediatrics) that emphasize mutual advantages of departmental status.
Recommendation 4: Divisions and sections of EM should seek to become academic departments as a means to develop, sustain, and grow strong academic programs (provided that careful analysis supports mutual benefits to EM and the mission of the faculty of medicine and health sciences centre).
Recommendation 5: The CAEP Academic Section should organize and support a consultation service to provide experience, analysis, and advice to chairs, because there is no established blueprint for an academic unit of EM to construct, implement, and improve their governance.
Recommendation 6: Many of the leadership, governance, and funding issues as well as challenges facing academic emergency medicine have similar patterns and drivers (even if contexts and details may differ between universities). The academic chair should establish a formal and regular forum for meeting and sharing experiences and approaches to common issues.
NEXT STEPS
The governance of academic EM is relatively complex, although the goal of good governance is straight forward: constantly improving academic performance. It is essential that governance structures and processes (along with leadership and funding) are iteratively improved over time in service of the education and research mission of academic EM, better patient care, and optimal population health outcomes. Given the significant variation in starting points and contexts across the country, there is no simple guide that all academic units of EM can use. These recommendations on the governance of the academic units of EM aim to support the evolution of academic EM and complement the recommendations provided by the funding and leadership panels.Reference Lang, Artz and Wilkie 29 , Reference Sinclair, Worthington and Joubert 30 The Leadership Working Group of the CAEP Academic Section will be addressing each recommendation and will present an update at its next Academic Leadership Symposium to be held in 2018.
Acknowledgements: The authors thank Kelly Wyatt and Kathleen White for their administrative support throughout the development of these recommendations.
Competing interests: None declared.
Supplementary Material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/cem.2016.22







