INTRODUCTION
Residency training has been shown to have a negative impact on physical, emotional, and social well-being. 1 Residents experience high rates of burnout,Reference West, Shanafelt and Kolars 2 , Reference Martini, Arfken, Churchill and Balon 3 depression,Reference Dyrbye, West and Satele 4 emotional exhaustion,Reference Kimo Takayesu, Ramoska and Clark 5 and social strain.Reference Landrigan, Rothschild and Cronin 6 Shift work for emergency medicine (EM) residents also poses long-term risks, including metabolic syndromeReference De Bacquer, Van Risseghem and Clays 7 , Reference Karlsson, Knutsson and Lindahl 8 and cardiovascular disease.Reference Bøggild and Knutsson 9 Moreover, learning environments include intimidation 1 and personal safety concerns.Reference Anglin, Kyriacou and Hutson 10
Accredited Canadian EM training includes two streams: those leading to a certification through either the Royal College of Physicians and Surgeons of Canada (RCPSC) or the College of Family Physicians of Canada (CFPC). Neither EM stream wellness experience has been well characterized. Given the negative effects of residency training and the paucity of information on EM resident wellness experiences, we conducted a national cross-sectional study to characterize the current landscape of Canadian EM resident wellness.
METHODS
This was a cross-sectional study of Canadian EM residents. A Canadian Association of Emergency Physicians Resident Section (CAEP RS) wellness working group composed of four senior residents (AT, AH, ZP, ND) created a list of survey questions based on a CAEP wellness position statementReference Taher, Crawford and Koczerginski 11 and Resident Doctors of Canada (RDoC) survey 1 topics. Survey questions were chosen by a working group member consensus. Several questions were discarded due to ambiguity after consultation with a survey methodologist (Appendix).
An anonymous survey link, along with study information, was sent to chief residents (CRs) of Canadian EM residency programs by email, with two follow-up emails over a 4-month period. Francophone programs received all information and the survey in French. CRs were then asked to forward the information to their residents. Total resident numbers were calculated from program websites, the Canadian residency matching service (CaRMS), 12 and confirmation with programs. The study period was from January to May 2017. Two programs with the highest response rates were awarded $250. A full list of survey questions is illustrated in the online Appendix. No program information was collected to maintain anonymity. Approval was obtained from the Research Ethics Board of Sunnybrook Health Sciences Centre.
RESULTS
A total of 511 Canadian EM residents were included, 31 EM programs were contacted (14 RCPSC and 17 CFPC), and a 42% (n=216) response rate was obtained. A full list of responses and demographics is illustrated in the online Appendix. RCPSC residents comprised 25% (n=128), with most in their first 3 years of training. Forty-four respondents (8.6%) did not specify their year.
EM residency experiences are illustrated in Tables 1 and 2. During residency training, 20% (n=103) reported falling asleep while driving post-night shift, or after a 24-hour call shift, and 3.5% (n=18) were involved in a motor vehicle collision (MVC) post-night or during a call shift. Verbal, physical, and sexual harassment and assault occurred at varying levels by patients, accompanying persons, other residents, or faculty. During residency, 35% (n=178) reported low mood, and 4.3% (n=22) reported suicidal ideation. Six percent (n=14) reported social isolation. Overall, residents reported gaps in wellness instruction, with 34% (n=173) welcoming dedicated program wellness time and 31% (n=160) for resilience training.
Table 1 EM residency training experience survey responses
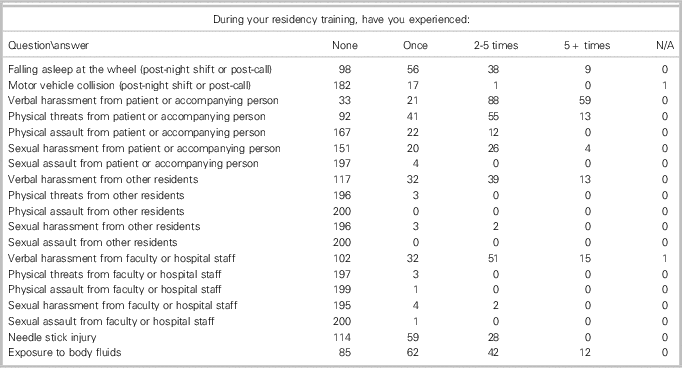
Table 2 EM residency survey responses for frequency of experiences
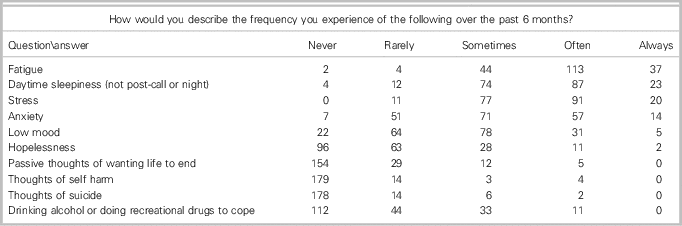
DISCUSSION
In this survey of Canadian EM residents, we identified a multitude of significant wellness challenges and important opportunities for improvement. Burnout, mental health struggles, and concerns for safety such as MVCs were notable. These experiences support previously reported rates of burnout and decreased quality of life.Reference West, Shanafelt and Kolars 2 - Reference Dyrbye, West and Satele 4 Moreover, our rate of suicidal ideation is in keeping with previously reported rates in medical trainees of 4.4% to 14%.Reference Dyrbye, Thomas and Massie 13 - Reference Tyssen, Vaglum, Grønvold and Ekeberg 15
Responses suggest actionable areas for further investigation and mitigation. Resiliency training has previously shown positive effects on quality of life for staff physiciansReference Sood, Prasad, Schroeder and Varkey 16 and residents.Reference Howe, Smajdor and Stöckl 17 However, the need for more training needs to be reconciled with program curricula time limitations. The transition to Competence by Design (CBD) may provide an opportunity for this (a national working group of stakeholders should form to address this need).
Secondly, there is a low reported rate of seeking wellness resources, with some dissatisfaction when accessed. It would be important to determine whether this is due to a lack of knowledge of their existence or whether accessibility barriers exist. RCPSC and CFPC accreditation standards govern EM residency programs, 18 which programs may be meeting, but there remains a deficit in EM residents accessing these resources. Therefore, residents need to be involved as stakeholders to inform future mitigation.
Several limitations were identified. The survey questions were not pilot tested on an independent sample of potential respondents but rather among the consensus committee. An external survey methodologist was also consulted. Although the questions seemed to have face validity, some improved clarity could have been achieved. We cannot determine any program-related patterns or biases due to the confidentiality inherent in our model. Low response rates were received from francophone (n=19) and CFPC training programs (n=44), as well as RCPSC senior residents; 8.6% of respondents did not answer the demographics section. Moreover, one program was not contacted (Saint John, New Brunswick) due to the inability to locate it on the CaRMS website. Although the overall response rate was 42%, these limitations may impede national generalizations and the ability to make associations between subgroups.
CONCLUSION
Our exploratory survey suggested that Canadian EM residents are facing psychosocial and physical wellness challenges. These present opportunities to further investigate resident wellness with validated tools, engage stakeholders, and advance the EM resident wellness agenda.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/cem.2018.416
Acknowledgements: We would like to acknowledge the assistance of the CAEP head office with the survey collection and analysis, and the University of Toronto Postgraduate Medical Education office for providing a survey methodologist.
Competing interests: The Canadian Association of Emergency Physicians (CAEP) head office supported this study, and two authors (AT, AH) were part of the CAEP wellness position statement working group.




