Violent behaviour in persons with psychiatric disorder causes great public concern and is recognised by mental health clinicians as a significant problem associated with illness relapse, hospital recidivism and poor outcomes in community-based treatment (Reference Monahan and SteadmanMonahan & Steadman, 1994; Reference MullenMullen, 1997). Involuntary out-patient commitment (OPC) is a legal intervention designed to benefit individuals with severe mental illness (SMI) who need ongoing psychiatric care and support to prevent dangerous relapse, but who are reluctant or unable to follow through with community-based treatment. Proponents of OPC assert that it may improve treatment adherence and may also act as a lever on a mental health service system: mobilising supportive services and motivating clinical vigilance. This paper addresses the question of whether OPC can help to prevent violent behaviour in psychiatric populations with a history of ‘revolving-door’ hospital admissions often associated with dangerousness. Findings are presented from the first randomised study of the effectiveness of OPC combined with case management (Reference Swartz, Swanson and WagnerSwartz et al, 1999).
Background
Serious violent acts committed by individuals with mental illnesses are statistically rare events (Reference MonahanMonahan, 1992). Still, the potential for violence in a proportion of persons with severe, persistent and often untreated psychiatric disorders stimulates public fear, prevents general acceptance and inclusion of persons with psychiatric disabilities and limits normalisation and effectiveness of community-based mental health services. The risk of violence creates dilemmas in the clinical realm by interrupting community tenure and continuity of care, in the legal realm by increasing concerns about professional liability, and in the public realm by heightening fear and stigma associated with mental illness (Reference Link, Cullen and FrankLink et al, 1987; Reference Angermeyer and MatschingerAngermeyer & Matschinger, 1996; Reference Borum, Swartz and SwansonBorum et al, 1996; Reference SimonSimon, 1998).
With the advent of managed care in both public and private mental health systems, and with clinicians increasingly held liable for the behaviour of patients inadequately treated, concerns about the risk of violence have increased (Reference CuffelCuffel, 1997; Reference SimonSimon, 1998). Individuals suffering from SMI with a history of violence are disproportionately high users of the most expensive mental health services in the most restrictive settings (e.g. involuntary in-patient treatment) (Reference Borum, Swartz and SwansonBorum et al, 1996). However, clinicians' efforts to prevent violence through conventional out-patient treatment are impeded: patients at risk often do not adhere to medication regimens or keep scheduled appointments, they may misuse substances and they tend to live in impoverished, dangerous environments with inadequate social support (Reference Swartz, Swanson and HidaySwartz et al, 1998b ; Reference Silver, Mulvey and MonahanSilver et al, 1999). Some studies have reported increased violent behaviour among mentally ill persons suffering from psychotic symptoms that involve perceived threat and override of internal cognitive controls (threat/control-override: TCO) (Reference Link, Stueve and PhelanLink et al, 1998), and particularly among those with TCO symptoms and substance misuse who have not had recent contact with a community mental health provider (Reference Swanson, Estroff and SwartzSwanson et al, 1997a ).
Involuntary OPC is a promising legal intervention that may significantly reduce violent behaviour associated with these particular problems by improving compliance with medications that mitigate high-risk psychotic symptoms; by improving access to substance misuse treatment for persons with dual diagnoses; by increasing clinical surveillance; and by augmenting case management intensity, thus leveraging scarce resources in community care systems (Reference Swanson, Swartz and GeorgeSwanson et al, 1997b ).
Out-patient commitment statutes exist in 35 states and the District of Columbia (Reference Torrey and KaplanTorrey & Kaplan, 1995). In North Carolina, where the present study was conducted, OPC statutes require compliance with recommended treatment, excluding forced medication in the out-patient setting. Under OPC, the responsible clinician may request that law officers escort the non-adherent patient to a community mental health centre for examination and hopeful persuasion to accept treatment. Evidence from naturalistic studies (Reference Fernandez and NygardFernandez & Nygard, 1990; Reference Geller, Grudzinskas and McDermeitGeller et al, 1998), as well as the current randomised study (Reference Swartz, Swanson and WagnerSwartz et al, 1999), suggests that OPC may decrease hospital readmission rates and total days hospitalised. However, OPC is strongly opposed by some mental health consumers and mental health law advocates, who argue that coerced out-patient treatment infringes on civil liberties, extends unwarranted social control into the community and may actually drive people away from needed treatment (Reference Mulvey, Geller and RothMulvey et al, 1987; Reference StefanStefan, 1987).
The potential of OPC to prevent violent behaviour warrants empirical investigation. The present study addresses the question of whether and how OPC reduces the risk of violence among people with SMI, using prospective longitudinal data from a sample of 262 people with psychotic or major mood disorders who were placed on OPC combined with case management in the Piedmont region of North Carolina.
METHOD
Study design and sample
Selection criteria
Subjects were screened sequentially from a population of involuntarily hospitalised patients who had been ordered to undergo a period of OPC upon discharge. Eligibility criteria for the study were: age 18 years or older; diagnosis of schizophrenia, schizo-affective disorder, other psychotic disorder or major affective disorder; duration of disorder of one year or more; significant functional impairment in activities of daily living; intensive treatment within the past two years; resident of one of nine counties participating in the study; and awaiting a period of court-ordered OPC. Legal criteria for OPC in North Carolina include SMI diagnosis and mental status limiting a person's ability to seek or comply voluntarily with treatment, and the likelihood that without treatment the person would predictably decompensate to a point of dangerousness or grave disability.
Study group assignment
By special arrangement with the court, subjects randomly assigned to a control group were released from OPC. Subjects in the experimental group, by law, received an initial period of OPC no longer than 90 days. Thereafter, the commitment order could be renewed for up to 180 days if a psychiatrist and the court determined that the subject continued to meet the legal criteria for OPC. However, subjects in the control group received immunity from any OPC during the year of the study. All subjects received case management and other out-patient treatment at one of four participating area mental health programmes representing nine contiguous urban and rural counties. An exception to the randomisation procedure was necessary in the case of subjects with a history of serious assault involving weapon use or physical injury to another person within the preceding year. These subjects (the seriously violent group) were required to undergo at least the initial period of OPC as ordered. Renewals were left to the discretion of the clinician and court.
Refusal, attrition, and differences in length of time on OPC
Of the identified eligible patients, 12% refused consent to participate. Rates of refusal did not vary significantly by gender, race or diagnosis. Subjects over age 45 years were more likely to refuse than those under 45 years (14% v. 7%). The baseline sample consisted of 331 subjects. At the 12-month follow-up, 69 subjects (20.9%) had withdrawn or were lost to follow-up, with 262 remaining: 114 controls, 102 in the OPC group and 46 in the OPC violent group. Attrition did not differ significantly by group. There was no evidence of sample bias in renewal of OPC orders, except that subjects with a baseline history of medication non-compliance were somewhat more likely to receive extended OPC (renewed court orders); 40.0% v. 18.75%. (The potential implications of this difference for interpretation of the results will be discussed below.) Approximately one-third of subjects in both the OPC and violent OPC groups received overall more than 180 days of court-ordered treatment.
Data collection
At baseline, structured interviews were conducted with each subject and with a family member or other informant who knew the respondent well. Hospital records were reviewed for additional information regarding clinical history. Follow-up interviews were conducted every four months with the subjects, case manager and collateral informant. Out-patient service records and hospital admissions were recorded as well.
Measurement
Violence
Incidence of violence was assessed from three data sources. Subjects were asked every four months whether they had been picked up by police or arrested for physical assault on another person, had been in fights involving physical contact or had threatened someone with a weapon. Family members and case managers were asked comparable questions about the subject's behaviour. A composite index was constructed measuring whether at least one violent act was reported by any source during the year of the study (Reference Swanson, Borum and SwartzSwanson et al, 1999).
Psychiatric symptoms
Psychiatric symptoms were assessed using the Brief Symptom Inventory (BSI; Reference Derogatis and MelisaratosDerogatis & Melisaratos, 1983). The BSI total score and a sub-scale for paranoid symptoms were used in the present analysis. An additional sub-scale was constructed from BSI items measuring TCO symptoms (Reference Link, Stueve and PhelanLink et al, 1998).
Functional impairment
Functional impairment was assessed using the Global Assessment of Functioning scale (GAF), which is a measure of functional status and severity of psychiatric disturbance rated on a continuum of 0-100 from most to least impaired (Reference Endicott, Spitzer and FleissEndicott et al, 1976).
Insight
Insight was measured by the Insight and Treatment Attitudes Questionnaire (ITAQ; Reference McEvoy, Apperson and ApplebaumMcEvoy et al, 1989). The ITAQ assesses the ability of subjects with SMI to recognise their need for treatment.
Social support
Social support was assessed using a sub-scale of the Duke Social Support Scale (Reference George, Blazer and HughesGeorge et al, 1989), measuring respondents' subjective perception of their status and value in a social network, whether the network would provide help if needed and satisfaction with the quantity and quality of received support.
Substance use and misuse
Substance use and misuse were assessed by combining interview data from three sources and (at baseline) the hospital record. Substance use was defined as drinking alcohol or using illicit drugs once to several times per month or more frequently. Substance misuse was defined as the occurrence of any problems related to alcohol or drug use: problems with family, friends, job, police, physical health or any recorded diagnosis of psychoactive substance use disorder (Reference Swartz, Swanson and HidaySwartz et al, 1998a ).
Medication adherence
Medication adherence was measured from three interview sources: subject, case manager and collateral informant. Respondents were defined as non-adherent if they were prescribed psychotropic medications but reportedly never took them or only sometimes took them as prescribed (Reference Swartz, Swanson and HidaySwartz et al, 1998b ).
Out-patient services utilisation
Out-patient services utilisation was obtained from service records in the information systems of participating community mental health centers. All service encounters for case management, medication, psychotherapy and other out-patient services were summed in a single index. Regular treatment was defined as three or more out-patient service encounters per month in the community (the median amount). This rate was adjusted for time spent hospitalised. For those receiving regular treatment according to this definition, the median number of out-patient service events per month was seven. For those not receiving regular treatment, the median number of events was one per month.
Analysis
Logistic regression analysis was used to examine the relative impact of sustained OPC and out-patient services utilisation on the incidence of violent behaviour, controlling for baseline violence history and relevant covariates. Odds ratios produced by this technique estimate the average change in the odds of a predicted event (any violence) associated with the presence of a risk factor. For independent variables measured on a continuous scale or ranking, the odds ratio indicates the change in event likelihood per unit change in the predictor.
Sample description
Demographic characteristics
As noted in Table 1, sample members were predominantly young to middle-aged adults of lower educational status and mostly not married and not cohabiting. The racial distribution of the sample was 66% African American, 33% non-Hispanic White and 1% other. Although the majority were city residents, a substantial proportion of the sample lived in rural areas and small towns. This sample was representative of the population of patients admitted to state mental hospitals in North Carolina.
Table 1 One-year incidence of violent behaviour by sample characteristics

| Baseline risk factors | n | % Violent | |
|---|---|---|---|
| Age | 18-39 years | 138 | 48.55*** |
| 40-65 years | 124 | 26.61 | |
| Gender | Male | 140 | 40.71 |
| Female | 122 | 35.25 | |
| Race | African American | 172 | 42.44† |
| White/other | 90 | 30.00 | |
| Marital status | Single | 208 | 41.35* |
| Married | 54 | 25.93 | |
| Duke Social Support Scale (perceived social support) | Median or below | 144 | 47.22*** |
| Above median | 118 | 27.12 | |
| Education | High school graduate | 165 | 38.79 |
| No High School | 97 | 37.11 | |
| Annual income | $6000 or less | 137 | 40.15 |
| Above $6000 | 125 | 36.00 | |
| Community of residence | Rural | 108 | 30.56* |
| Urban | 154 | 43.51 | |
| Homeless at some time in preceding four months | No | 208 | 33.17*** |
| Yes | 54 | 57.41 | |
| Victim of crime during preceding four months | No | 194 | 35.05† |
| Yes | 68 | 47.06 | |
| Primary discharge diagnosis | Schizophrenia | 100 | 35.00 |
| Schizoaffective | 58 | 41.38 | |
| Other psychotic | 21 | 33.33 | |
| Bipolar disorder | 72 | 41.67 | |
| Major depression | 11 | 36.36 | |
| Personality disorder (Axis 2 diagnosis) | No | 228 | 35.09** |
| Yes | 34 | 58.82 | |
| Global Assessment of Functioning (GAF) | Median or below | 131 | 45.80* |
| Above median | 131 | 30.53 | |
| Brief Symptom Inventory (BSI) | Median or below | 135 | 33.33 |
| Above median | 127 | 43.31 | |
| Paranoid symptoms (BSI sub-scale) | Median or below | 137 | 29.93** |
| Above median | 125 | 47.20 | |
| Threat/control-override (TCO) symptoms | Median or below | 134 | 31.34* |
| Above median | 128 | 45.31 | |
| Insight and Treatment Attitudes Questionnaire (ITAQ) | Median or below | 135 | 42.96 |
| Above median | 127 | 33.07 | |
| Psychiatric hospitalisations in the preceding year | Less than two | 163 | 33.13* |
| Two or more | 99 | 46.46 | |
| Substance use | No use | 112 | 26.79*** |
| Occasional use | 60 | 36.67 | |
| Problems | 90 | 53.33 | |
| Medication-adherent in preceding four months | No | 190 | 37.89 |
| Yes | 72 | 38.89 |
Clinical characteristics, substance misuse, and history of violence at baseline
The majority of the sample (68%) had diagnoses of psychotic disorders, whereas 28% had bipolar disorder and 4% had recurrent major depression. Thirteen per cent had a co-occurring diagnosis of a personality disorder. The majority of the sample had moderate functional impairment (GAF median score=47). Alcohol and drug use (57%), medication non-compliance (73%) and violent behaviour (51%) were common in the four months prior to hospitalisation. More than one-third (39%) had experienced two or more psychiatric hospital admissions during the preceding year. For a more extensive presentation of the sample and the characteristics of violent events preceding hospitalisation, see Swanson et al (Reference Swanson, Borum and Swartz1999).
RESULTS
Predictors of violence
Table 1 presents bivariate associations of baseline risk factors with any violent behaviour during the one-year follow-up. The risk of violence was significantly higher among subjects who were: young (under age 40 years); single; with low social support; residents of urban areas; those recently homeless; with greater functional impairment (GAF score <47); substance misusers; those with paranoid symptoms; TCO symptoms; and those with more than two hospital admissions in the prior year.
Key correlates of violent behaviour during the follow-up year included ongoing substance misuse problems and non-adherence with prescribed psychotropic medications. Fifty per cent of substance misusers were violent v. 26.5% of those who did not misuse substances (Fisher's exact test, two-tailed, P<0.001); and 41.6% of those who did not adhere to prescribed medication regimens were violent v. 25.5% of those who took medications as prescribed (Fisher's exact test, two-tailed, P<0.05).
Out-patient commitment and violence
Considering this study strictly as a randomised controlled trial, subjects with a baseline history of serious violence must be excluded from analysis and all experimental subjects must be considered as a single group (without regard to the length of exposure to OPC). On this basis alone, the study found no significant difference in the prospective rate of violence between the two randomly assigned groups: 32.3% in the OPC group v. 36.8% in the control group (Fisher's exact test, one-tailed: P=0.292; two-tailed: P=0.567).
However, a problem with this test is that it excludes a key risk group to which OPC policy may be targeted specifically (the seriously violent group), and constricts the dependent variable by eliminating a substantial number of violent events from the analysis. Moreover, the test as specified cannot take into account varying amounts of exposure to the intervention (i.e. length of time actually spent under court-ordered treatment). Time on OPC varied considerably; it was not subject to experimental control, but depended on clinician's discretion in applying the legal criteria for renewal of expiring OPC orders. As mentioned earlier, this may have selected into the long-term OPC group a greater proportion of clients with a history of non-adherence to medication; this was indirectly associated with a higher baseline risk of violence. Clearly, however, insofar as this created a bias, its effect was conservative, that is, it would work against finding a positive effect for extended OPC in reducing violence risk.
Alternatively, when subjects with a history of serious violence were included in the analysis and the OPC intervention was redefined as receiving at least six months of court-ordered treatment, the results were striking. The extended OPC group had a significantly lower incidence of violence during the year: 26.7% v. 41.6% (Fisher's exact test, one-tailed: P=0.049; two-tailed: P=0.025).
The six-month cut-off point for categorising extended OPC is somewhat arbitrary. However, there were good reasons for dichotomising this variable. The distribution of total OPC days was highly skewed, with all members of the control group receiving zero days of OPC. The majority of the randomised experimental and violent group subjects received less than six months of OPC, whereas a large cluster remained on OPC for the entire year of the study, giving the variable a bimodal distribution. Specifically, for those with less than six months of court-ordered treatment the mean number of days on OPC was 76, whereas for those receiving extended OPC the mean number of days was 330. Using a dichotomous version of the intervention variable, a significant association was found between extended OPC and incidence of violence; this effect remained significant in multivariate analysis, as will be shown below.
We also re-analysed the data for high and low exposure to OPC separately for the randomised subjects and the non-randomised violent group. In the randomised study groups, control subjects did not differ significantly in their risk of violence from those with brief, discontinued OPC (36.8% v. 39.7%). However, the incidence of violence was significantly less (22.7%) among randomised OPC subjects who received extended court-ordered treatment (Fisher's exact test, one-tailed: P=0.043; two-tailed: P=0.076). Among the subjects who were violent at baseline, the effect of extended OPC was also seen at a level approaching statistical significance: among violent subjects with brief, discontinued OPC, 63.3% repeated their violent behaviour during the year of the study; of those receiving extended OPC, only 37.5% were violent (Fisher's exact test, one-tailed: P=0.086; two-tailed: P=0.126).
Multivariate analysis
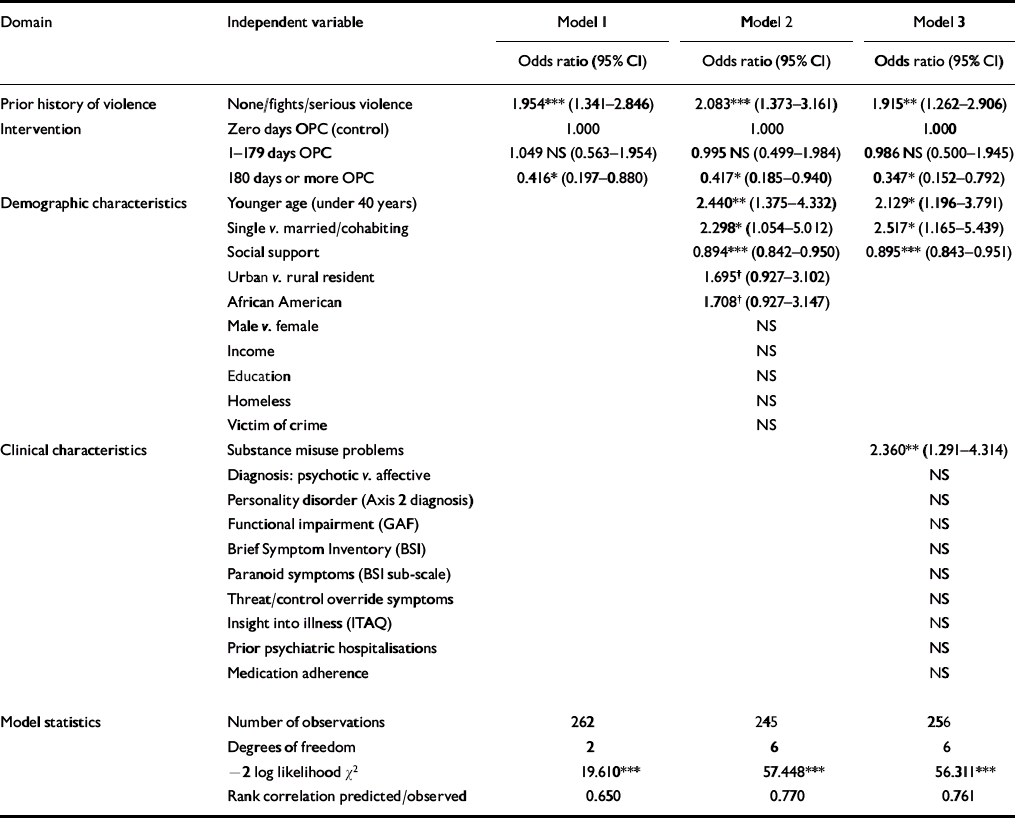
Staged logistic regression analysis with stepwise inclusion was conducted to test the effect of OPC on reduced violence in the context of relevant covariates. A control variable was included to hold constant the effect of baseline history of violence and initial assignment to the violent OPC group. An initial model (see Table 2, Model 1) showed that extended OPC was associated with significantly lower odds of any violent behaviour during the year of the study, controlling for baseline history of violence (odds ratio=0.42; P<0.05). In Model 2, being young, single, and having a low degree of perceived social support were identified as significant demographic risk factors. In Model 3, among the clinical variables substance misuse was a significant predictor of violence. Controlling for the significant demographic variables and substance misuse, respondents who received more than 180 days of OPC were only about one-third as likely to commit a violent act during the year as their counterparts in the control group (odds ratio=0.35; P<0.01). Those receiving 1-179 days of OPC did not differ from the control group with respect to risk of violence.
Table 2 Predictors of violent behaviour during the year after hospital discharge: effects of sustained out-patient commitment (OPC) controlling for baseline risk factors
| Domain | Independent variable | Model 1 | Model 2 | Model 3 |
|---|---|---|---|---|
| Odds ratio (95% Cl) | Odds ratio (95% Cl) | Odds ratio (95% Cl) | ||
| Prior history of violence | None/fights/serious violence | 1.954*** (1.341-2.846) | 2.083*** (1.373-3.161) | 1.915** (1.262-2.906) |
| Intervention | Zero days OPC (control) | 1.000 | 1.000 | 1.000 |
| 1-179 days OPC | 1.049 NS (0.563-1.954) | 0.995 NS (0.499-1.984) | 0.986 NS (0.500-1.945) | |
| 180 days or more OPC | 0.416* (0.197-0.880) | 0.417* (0.185-0.940) | 0.347* (0.152-0.792) | |
| Demographic characteristics | Younger age (under 40 years) | 2.440** (1.375-4.332) | 2.129* (1.196-3.791) | |
| Single v. married/cohabiting | 2.298* (1.054-5.012) | 2.517* (1.165-5.439) | ||
| Social support | 0.894*** (0.842-0.950) | 0.895*** (0.843-0.951) | ||
| Urban v. rural resident | 1.695† (0.927-3.102) | |||
| African American | 1.708† (0.927-3.147) | |||
| Male v. female | NS | |||
| Income | NS | |||
| Education | NS | |||
| Homeless | NS | |||
| Victim of crime | NS | |||
| Clinical characteristics | Substance misuse problems | 2.360** (1.291-4.314) | ||
| Diagnosis: psychotic v. affective | NS | |||
| Personality disorder (Axis 2 diagnosis) | NS | |||
| Functional impairment (GAF) | NS | |||
| Brief Symptom Inventory (BSI) | NS | |||
| Paranoid symptoms (BSI sub-scale) | NS | |||
| Threat/control override symptoms | NS | |||
| Insight into illness (ITAQ) | NS | |||
| Prior psychiatric hospitalisations | NS | |||
| Medication adherence | NS | |||
| Model statistics | Number of observations | 262 | 245 | 256 |
| Degrees of freedom | 2 | 6 | 6 | |
| -2 log likelihood χ2 | 19.610*** | 57.448*** | 56.311*** | |
| Rank correlation predicted/observed | 0.650 | 0.770 | 0.761 |
A cross-sectional analysis of baseline data from this same study showed a significant association between history of violence and history of medication non-adherence combined with substance misuse (Reference Swartz, Swanson and HidaySwartz et al, 1998b ). This finding was replicated with the longitudinal follow-up data controlling for extended OPC and significant covariates. Risk of violence was found to be three times greater among subjects who misused substances and did not take medications as prescribed during follow-up (odds ratio=3.19; P<0.01); however, risk was not significantly elevated among respondents with only one of these problems alone.
Based on this finding of an interaction effect of substance misuse and non-compliance, two composite variables were coded for subsequent analysis: clinical risk status at baseline, and change in clinical risk status at follow-up. Subjects whose status on both substance misuse and medication adherence improved from baseline received the highest change scores, whereas those who deteriorated or maintained a poor status received lower scores accordingly. Change scores ranged from ‒3 to +4 (mean=1.2, s.d.=1.7). In bivariate analysis, subjects who received extended OPC achieved significantly better mean scores on the index (1.8 v. 1.1; mean square=14.2; F=4.79; P<0.05). Subjects who remained free of violent behaviour also were found to have significantly better scores (1.53 v. 0.76; mean square=36.7; F=12.76; P<0.01).
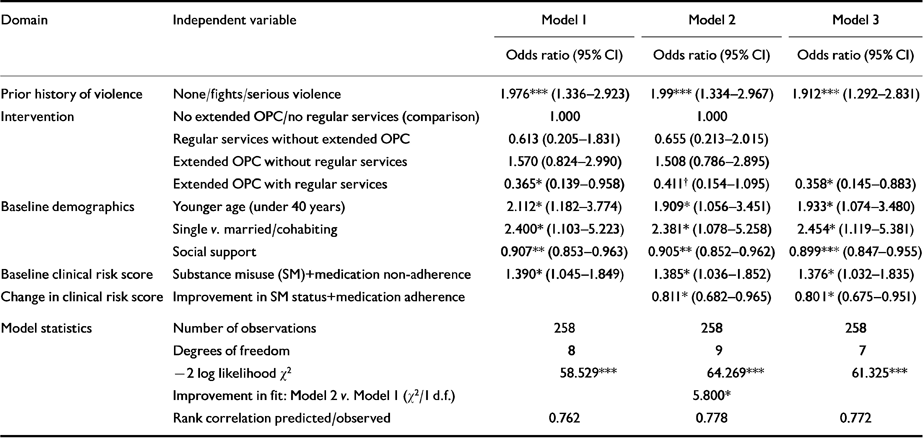
The staged multivariate analysis shown in Table 3 examines whether OPC interacts with the provision of out-patient services to reduce the risk of violent behaviour and, if so, whether OPC prevents violence indirectly by means of reducing substance misuse and improving medication adherence. Model 1 shows that extended OPC alone did not significantly reduce risk. Similarly, receiving frequent services alone was not associated with less violence. Rather, the combination of both variables — at least 180 days of OPC with an average of three or more out-patient visits per month in the community — showed a significant effect in reducing violence (odds ratio=0.37; P<0.05). In this model, the predicted probability of any violent behaviour was cut in half from 48% to 24%, attributable to extended OPC and regular out-patient services provision.
Table 3 Predictors of behaviour during the year after hospital discharge: effects of sustained out-patient commitment (OPC) and regular services controlling for baseline characteristics and improvement in combined clinical risk factors (substance misuse and medication adherence)
| Domain | Independent variable | Model 1 | Model 2 | Model 3 |
|---|---|---|---|---|
| Odds ratio (95% Cl) | Odds ratio (95% Cl) | Odds ratio (95% Cl) | ||
| Prior history of violence | None/fights/serious violence | 1.976*** (1.336-2.923) | 1.99*** (1.334-2.967) | 1.912*** (1.292-2.831) |
| Intervention | No extended OPC/no regular services (comparison) | 1.000 | 1.000 | |
| Regular services without extended OPC | 0.613 (0.205-1.831) | 0.655 (0.213-2.015) | ||
| Extended OPC without regular services | 1.570 (0.824-2.990) | 1.508 (0.786-2.895) | ||
| Extended OPC with regular services | 0.365* (0.139-0.958) | 0.411† (0.154-1.095) | 0.358* (0.145-0.883) | |
| Baseline demographics | Younger age (under 40 years) | 2.112* (1.182-3.774) | 1.909* (1.056-3.451) | 1.933* (1.074-3.480) |
| Single v. married/cohabiting | 2.400* (1.103-5.223) | 2.381* (1.078-5.258) | 2.454* (1.119-5.381) | |
| Social support | 0.907** (0.853-0.963) | 0.905** (0.852-0.962) | 0.899*** (0.847-0.955) | |
| Baseline clinical risk score | Substance misuse (SM)+medication non-adherence | 1.390* (1.045-1.849) | 1.385* (1.036-1.852) | 1.376* (1.032-1.835) |
| Change in clinical risk score | Improvement in SM status+medication adherence | 0.811* (0.682-0.965) | 0.801* (0.675-0.951) | |
| Model statistics | Number of observations | 258 | 258 | 258 |
| Degrees of freedom | 8 | 9 | 7 | |
| -2 log likelihood χ2 | 58.529*** | 64.269*** | 61.325*** | |
| Improvement in fit: Model 2 v. Model 1 (χ2/1 d.f.) | 5.800* | |||
| Rank correlation predicted/observed | 0.762 | 0.778 | 0.772 |
Model 2 in Table 3 shows that combined improvement in medication adherence and substance use/misuse status was a significant predictor of reduced violent behaviour: about 20% reduction with each unit improvement in clinical risk (odds ratio=0.81; P<0.05). This model provides evidence of an indirect effect of the intervention, as mentioned above. With the clinical risk change score in the equation, the direct effect of OPC and services was suppressed from an odds ratio of 0.36 (P<0.05) in Model 1 to an odds ratio of 0.41 (P<0.10) in Model 2, and the fit of the model improved significantly.
Finally, Model 3 specifies a reduced set of predictors using stepwise selection of variables. Based on this model, subjects who received the high intervention (sustained OPC and regular services), who concurrently remained free of substance misuse and who took medications as prescribed during the year of the study had the lowest likelihood of any violence (13% predicted probability). In contrast, those who did not receive the high intervention, who continued to misuse substances and who stopped taking their medications had a 53% predicted probability of violent behaviour during the year.
DISCUSSION
This study examined jointly the effectiveness of OPC and the impact of key risk factors associated with violent behaviour among persons with psychotic or major mood disorders. In a multivariate model that tested a range of socio-demographic and clinical characteristics, a small set of baseline risk factors — being young (under age 40 years), single, having low social support, and misusing substances — were identified prospectively as significant predictors of violent behaviour in the ensuing year. Consistent with prior analysis (Reference Swartz, Swanson and HidaySwartz et al, 1998b ), the study also found that the combination of co-occurring substance misuse and non-adherence with medications was strongly associated with violence.
Sustained OPC combined with regular community-based service
The key finding is that extended OPC (more than six months) combined with regular out-patient services utilisation (three or more events per month) produced a significant decrease in the incidence of violence. Neither the court order nor services alone was effective in reducing violence. However, with regular service use, the presence of extended OPC reduced the probability of violence from 48% to 24%.
Improved medication adherence and diminished substance misuse
The study provides evidence for an important mechanism by which OPC may exert its effect in preventing violent behaviour. Respondents who received extended OPC with regular out-patient services achieved, on average, the highest positive (improved) change scores on medication adherence and substance use. In turn, those with high change scores in both of these risk factors combined had a significantly reduced incidence of violent behaviour during the year of follow-up. A multivariate model suggests that the benefit of OPC as described is at least partly an indirect effect attributable to change in these intervening clinical risk factors.
Deviation from randomised design
The study design deviates in two ways from a strict randomised controlled trial. First, the sample included a subgroup of subjects with a recent history of serious violent behaviour who could not be assigned randomly to the initial control group (outright release from OPC). To exclude these subjects altogether would have meant that the study findings could not be generalised to a crucially important sub-population to which OPC policy may be targeted. However, random assignment was not feasible for these subjects; the Institutional Review Board, the District Court judges and the hospital psychiatrists overseeing these patients' care and research participation would not authorise rescinding their OPC orders at baseline — citing practice liability and other concerns. Nevertheless, over half of these subjects did not remain on OPC, and thus were unexposed to court-ordered treatment during a large proportion of the period of observation. Hence, the non-renewal of many of these orders allowed an informative comparison of rates of violent recidivism between those remaining under OPC for more than six months (average 330 days) and those receiving less than six months of OPC (average 76 days).
This leads to a second necessary deviation from a strict randomised controlled design. Amount of time on OPC was not random or controlled experimentally, but varied as clinicians applied the legal criteria for renewal of OPC orders. Potentially, this could have lead to a biased conclusion (i.e. attributing a positive intervention effect to subjects who might have been less violent anyway because of pre-existing lower risk). However, this could only be a problem if higher-risk subjects were less likely to get renewal of their court order. In fact, the legal criteria for OPC work in the opposite direction.
Possible conservative bias favouring not finding an effect of OPC on reducing violence
Renewal of the court order required a second determination (by a psychiatrist and the court) that the respondent would predictably become dangerous (or ‘gravely disabled’) without treatment and predictably would not comply with treatment. At the end of the initial OPC period (up to 90 days), each case was re-evaluated systematically. Prompting notices were sent to clinicians, reminding them that a subject's OPC order was about to expire and summarising the OPC criteria for easy reference. If at that point the psychiatrist and the court concluded that the respondent was no longer likely to become dangerous without treatment or, even if so, would comply voluntarily with treatment, then the legal criteria for OPC were not satisfied and the order could not be renewed. (Beyond the legal criteria, common sense suggests that clinicians would not cull out clients assessed to be at highest risk of violence and selectively not renew their OPC orders.)
Anecdotally, when clinicians were asked by research staff members to state their reasons for not renewing an OPC order, the most typical answer was that the patient had been compliant with treatment and was doing reasonably well at that time; hence, continuing a court order was not seen as legally justifiable. Empirically, respondents who had been mostly compliant with medications in the four months prior to hospitalisation were significantly less likely to receive extended OPC after their initial court order expired; and medication compliance was indirectly associated with lower risk of violence in these data (Reference Swartz, Swanson and HidaySwartz et al, 1998b ). In summary, if bias existed in the selection of subjects for longer periods of OPC, then such a bias would seem to work against finding that extended OPC lowers the risk of violence. Thus, our results may understate the true impact of OPC in preventing violent behaviour.
Responsibility of mental health service systems using OPC
These results show that OPC may be an effective strategy for reducing community violence among people with SMI. However, if service systems intend to use OPC to this end, they must be prepared to monitor clients for sustained periods. Most importantly, they must make available adequate services to address the complex needs of persons with SMI and (often) substance misuse comorbidity, who lack adequate social resources and experience persistent difficulties in complying with out-patient treatment on their own. With such provisos, OPC may assist mental health agencies in reducing violent behaviour and costly institutional recidivism, and may significantly improve the lives of persons suffering from severe and persistent mental illness.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ An extended period of involuntary out-patient commitment (six months or more) may significantly reduce the risk of violent behaviour in persons with severe mental illness.
-
▪ Involuntary out-patient commitment must be supported by frequent mental health service visits (three or more monthly visits on average) in order to have a significant effect in managing violence risk.
-
▪ Out-patient commitment reduces violence risk at least in part by improving medication adherence while diminishing substance misuse; hence, treatment planning for out-patient-committed persons with a history of violence should focus on these intervening clinical issues.
LIMITATIONS
-
▪ Length of time on out-patient commitment was a key variable in the intervention, but could not be randomly assigned. Legal criteria for renewal of out-patient commitment would seem to prevent selection of lower-risk subjects for longer exposure to court-ordered treatment. Still, unknown selection factors may have affected duration of out-patient commitment.
-
▪ Persons with a documented history of serious violent behaviour upon entry into the study could not be assigned to control group (released from out-patient commitment outright); hence, analysis of the effectiveness of out-patient commitment in this group is limited to comparisons between those with shorter v. longer periods of court-ordered treatment in the community.
-
▪ Out-patient service intensity was not controlled by the study, but varied according to clinical need and unknown factors. Perceived risk may have stimulated service provision, just as treatment may have prevented violence; causation is difficult to establish.
ACKNOWLEDGEMENTS
The research presented here was supported by two grants from the National Institute of Mental Health: Effectiveness of Involuntary Outpatient Commitment (R01-MH48103-05); and Program on Services Research for People with Severe Mental Disorders (P50-MH51410-02). The authors gratefully acknowledge the support and cooperation of many state mental health personnel, judges, clinicians, administrative staff and law officers from Durham, Vance, Franklin, Granville, Warren, Orange, Person, Chatham and Guilford counties in North Carolina and Linda George, PhD, who helped design and participated in this study.






eLetters
No eLetters have been published for this article.