Comorbidity of mental illness and substance misuse (comorbidity) has been associated with increased psychiatric admission (Reference Hunt, Bergen and BashirHunt et al, 2002), violence (Reference Scott, Johnson and MenezesScott et al, 1998), suicidal behaviour (Reference Appleby, Shaw and AmosAppleby et al, 1999), excess service costs (Reference Hoff and RosenheckHoff & Rosenheck, 1999) and poor treatment outcome in both psychiatric (Reference Hunt, Bergen and BashirHunt et al, 2002) and substance misuse treatment populations (Reference Carey, Carey and MeislerCarey et al, 1991). Improved management of comorbidity is now a priority of the National Health Service (NHS) in the UK (Reference Banerjee, Clancy and CromeBanerjee et al, 2002) and options for service development have been widely discussed (Reference Hall and FarrellHall & Farrell, 1997; Reference JohnsonJohnson, 1997; Reference Weaver, Renton and StimsonWeaver et al, 1999). However, the absence of comparable multi-centre prevalence data from UK substance misuse and community mental health team (CMHT) treatment populations, and limited evidence about the current capacity of these services to manage comorbidity, has hampered the identification of appropriate service delivery models.
METHOD
Study aims
Our study aims were to measure the prevalence of comorbidity among patients of CMHTs and substance misuse services in four inner-city treatment centres, to assess whether there were differences in the prevalence between centres, and to measure the potential for joint management by CMHT and substance misuse services where patients with comorbidity were identified.
Design and setting
We conducted a cross-sectional prevalence survey between January 2001 and February 2002 in four urban UK centres. These were two neighbouring inner-London boroughs (Brent, and Hammersmith and Fulham) and services in inner-city areas of Nottingham and Sheffield. At all four centres the CMHTs were consultant-led, multi-disciplinary teams serving geographically defined catchment areas. Each had access to designated in-patient beds, operated according to contemporary care programme approach (CPA) guidelines and gave priority (in terms of the allocation of case-load places) to patients with severe and enduring mental illness. The drug and alcohol teams were statutory providers. They offered separate structured, appointment-based services through keyworkers within nurse-led clinics. All clients were allocated a personal keyworker and assigned to the case-load of a psychiatrist or responsible medical officer (RMO). All drug services had a strong emphasis upon the management of opiate dependency. Independent drug services were available in some areas (including services for stimulant users), but not in others. These latter agencies were not investigated. In each population, we completed a case-load census to identify the sampling frame and a patient interview survey with case-note audit in a random sample.
Participants
All patients of the drug and alcohol teams who were allocated to the case-load of a keyworker and psychiatrist/RMO on the census date were included in the substance misuse case-load census population. The only current patients excluded were a small proportion who had not completed an assessment. The sample sizes were proportionate to the size of the total treatment populations in each centre. To be included in the CMHT case-load census population, patients had to be allocated to the case-load of a care coordinator and psychiatrist/RMO on the census date, be aged 16–64 years and be included on the local CPA register. Only a small proportion of current CMHT patients were excluded because they had not completed an assessment, or exceeded the age range. Interview samples of 400 CMHT and 353 substance misuse patients were selected from these census populations at the coordinating centre (Imperial College) using Statistical Package for the Social Sciences (SPSS) random case selection procedures (SPSS, 1999).
Data collection
Data collection procedures were agreed with local research ethics committees. Services identified eligible patients, who were allocated anonymous case numbers used in all data collection. Care coordinators and keyworkers completed census questionnaires (one per patient), gave patients sampled for interview an information sheet, and invited them to meet a trained fieldworker. All interviewed patients gave written informed consent. Non-consenting patients were regarded as non-respondents and not substituted.
Assessments
Case-load census
Care coordinators and keyworkers were asked to report demographic details, ICD–10 psychiatric diagnoses (World Health Organization, 1992) established or confirmed by psychiatric assessment in the past year, and any psychiatric and substance misuse interventions provided in the past month. Care coordinators for CMHT patients were asked to identify people using any illicit or non-prescribed drug in the past year, and to apply diagnostic criteria (reproduced on the census form) to this group to identify those misusing drugs (American Psychiatric Association, 1994). Care coordinators applied the same criteria to all patients to identify those misusing alcohol.
Interview survey
Mental health status was assessed using the Quick Personality Assessment Schedule (Reference Tyrer and TyrerTyrer, 2000), the Comprehensive Psychopathological Rating Scale (CPRS; Reference Åsberg, Perris and SchallingÅsberg et al, 1978) and its sub-scales for rating depression (Montgomery–Åsberg Depression Rating Scale; Reference Montgomery and AsbergMontgomery & Åsberg, 1979) and anxiety disorders (Brief Scale for Anxiety; Reference Tyrer, Owen and CicchettiTyrer et al, 1984). All of the above assessments were applied to participants from both CMHT and substance misuse patient populations. Research psychiatrists assessed patients in the substance misuse group for psychosis using the Operational Checklist for Psychiatric Disorders (OPCRIT; Reference McGuffin, Farmer and HarveyMcGuffin et al, 1991) based on a case-note review. A specificity analysis was completed using information from the patient interview to ensure conservative rating of psychosis.
We used service-defined diagnoses to identify CMHT patients with psychosis. We completed OPCRIT assessments in a subsample of cases, enabling a specificity analysis to be completed; this showed that service-defined diagnosis was acceptable and reliable in identifying people with psychotic disorders (sensitivity 95%, specificity 81%). In our analysis the diagnostic category ‘psychosis’ included schizophrenia (F20.0–F20.9); schizotypal, schizoaffective, delusional and other unspecified psychotic disorders (F21–F29); manic episode with psychotic symptoms (F30.2); bipolar affective disorder (F31); severe depression with psychotic disorder (F32.3); and recurrent severe depression with psychotic symptoms (F33.3). The Alcohol Use Disorders Identification Test (AUDIT; Reference Saunders, Aasland and BaborSaunders et al, 1993) identified harmful (score ≥8) and severe (score ≥15) alcohol-related problems. A structured interview checklist identified drug types used (ever, past year, past month) and whether associated problems were present (economic, domestic, social, legal or interpersonal). Problem drug use was defined as self-reported presence of one or more of the above drug-related problems or care coordinator assessment of misuse. The Severity of Dependence Scale (Reference Gossop, Darke and GriffithsGossop et al, 1995) assessed drug dependency. These assessments were implemented in each treatment population.
To assess the reliability of self-reported drug use in CMHT patients we tested hair and urine samples, obtained from a random subsample of participants, by means of chromatography (Reference Paterson, Cordero and McCullochPaterson et al, 2000) and mass spectrometry analysis (Reference Paterson, McLachlan-Troup and CorderoPaterson et al, 2001). Samples were obtained contemporaneously with self-report data. However, consent for hair and urine testing was obtained separately after each interview assessment.
Analysis
All analysis presented in this paper was undertaken with the interview samples achieved in each treatment population (Fig. 1). The primary analysis calculated the proportions of each sample with comorbid conditions and the size of sub-populations defined in terms of psychiatric diagnosis and pattern of substance misuse. We then measured the proportions of comorbid cases that had been identified by keyworkers. By measuring the severity and types of comorbid disorder we identified approximate thresholds for access to each service. We used these data to assess the proportions of each treatment population with high or low potential for cross-referral and who had documented contact with both psychiatric and substance misuse services. All prevalence estimates are reported with exact binomial 95% confidence intervals. The statistical significance of observed differences in proportions was assessed using Pearson chi-squared or Fisher's exact tests. These analyses were completed using SPSS (SPSS, 1999).

Fig. 1 Size of eligible community mental health team, drug service and alcohol service study populations at case-load census, interview sample sizes and response rates achieved.
We then completed an extended quantitative analysis in relation to comorbid and non-comorbid sample groups in each treatment population. Multiple logistic regression was undertaken using cases with complete data on age, gender, ethnicity and diagnosis to investigate factors independently associated with comorbidity in the London centres v. the aggregated Nottingham and Sheffield centres. Adjusted odds ratios with 95% confidence intervals were obtained and compared with the odds ratios from the univariate analysis. All variables were entered as categorical variables. Interactions between age group, gender, ethnicity, case-mix variables and location were investigated. The coding for ethnicity and age group was predetermined. The statistical package Stata 6.0 (StataCorp, 1999) was used for these latter analyses.
RESULTS
Number and characteristics of participants
We obtained data on 2528 of 2567 CMHT patients (98.5%) meeting census eligibility criteria (Fig. 1). Interviews were completed in 282 of 400 cases (70.5%) randomly sampled from this population. Sixty-eight of the patients interviewed were randomly pre-sampled for subsequent hair and urine testing, and 50 provided a sample (73.5%). Keyworkers provided data about 1645 of 1674 substance misuse service patients (98.3%) meeting census eligibility criteria. Complete interview and case-note data were obtained in 278 of 353 randomly selected cases (78.8%) (216 drug service patients, 62 alcohol service patients).
Treatment populations were predominantly male (57–67%). Men in contact with drug services and CMHTs had similar median ages (35 years and 36 years respectively) and age group distributions. Patients misusing alcohol were typically older (median age 42 years). In contrast, women in contact with drug services had a younger median age (32 years) than women in contact with alcohol services (39 years) or CMHTs (43 years). There were marked differences in ethnicity between patients comprising the drug and alcohol case-loads (>90% White) and those of CMHTs (68.8% White, 23.8% Black).
Of the CMHT sample, three-quarters (n=216) had a psychotic disorder and 41 had a primary diagnosis of severe depression. Additional ‘complex care needs’, which tend to qualify patients for enhanced CPA management, were present in 80% (n=226): these were previous psychiatric admission, suicidal behaviour, self-neglect/harm, risk of exploitation or secondary psychiatric disorder. Most of the drug service patients reported lifetime opiate use (92.6%, n=200), and 78% (n=158) reported lifetime injected drug use. Some alcohol service patients reported controlled drinking in the past year, but 79% (n=49) recorded AUDIT scores indicative of severe alcohol misuse.
Prevalence of comorbidity in CMHT patients
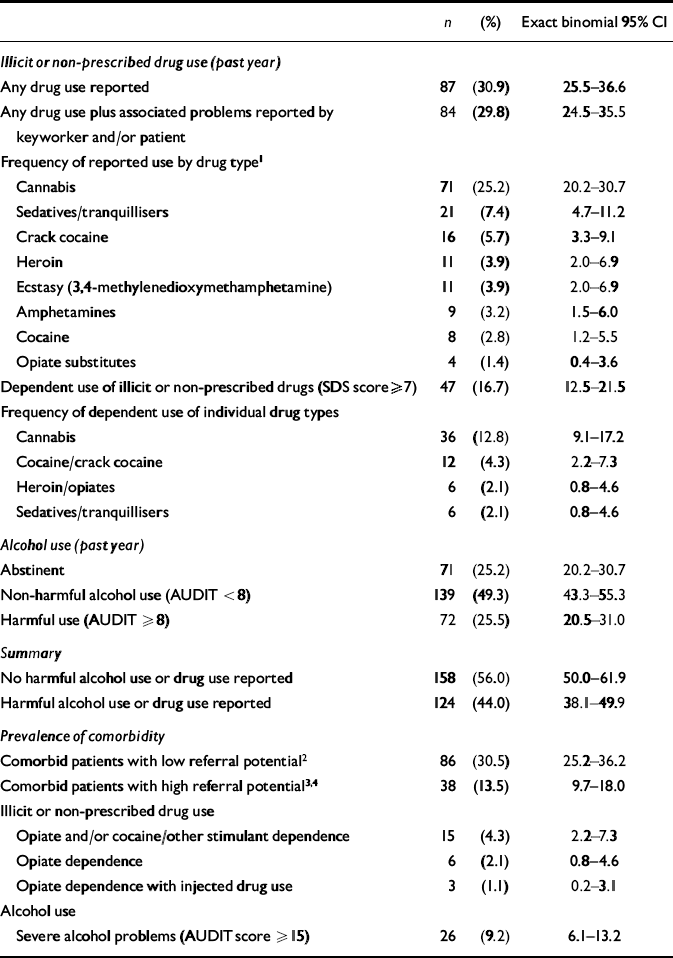
Among CMHT patients, 124 (44%) self-reported drug use and/or harmful alcohol use (Table 1). Harmful alcohol use (defined by the AUDIT criteria) was reported by about a quarter of patients (n=72) and about a tenth (n=26) reported severe alcohol misuse. Illicit or non-prescribed drug use in the past year was reported by 87 (30.9%) patients; most met our criteria for problem drug use: n=64 (29.8%). Drug dependency was identified in 47 (16.7%). The most frequently reported drugs were cannabis (25.2%, n=71), sedatives/tranquillisers (7.4%, n=21) and crack cocaine (5.7%, n=16). Heroin, ecstasy (3,4-methylenedioxymethamphetamine), amphetamines and cocaine powder were all reported by less than 4% (Table 1). Harmful alcohol use was strongly associated with problem drug use. Of the patients who did not report drug use, 19% had harmful levels of alcohol use. The prevalence of harmful alcohol use was double this rate in patients reporting any problem drug use: 40.2% (χ2=13.7, d.f.=1, P<0.001).
Table 1 Community mental health team study population (n=282): prevalence of self-reported harmful alcohol use, problem drug use and dependent drug use in the past year, and proportion of patients with substance misuse problems meeting referral thresholds for substance misuse services
| n | (%) | Exact binomial 95% CI | |
|---|---|---|---|
| Illicit or non-prescribed drug use (past year) | |||
| Any drug use reported | 87 | (30.9) | 25.5-36.6 |
| Any drug use plus associated problems reported by keyworker and/or patient | 84 | (29.8) | 24.5-35.5 |
| Frequency of reported use by drug type1 | |||
| Cannabis | 71 | (25.2) | 20.2-30.7 |
| Sedatives/tranquillisers | 21 | (7.4) | 4.7-11.2 |
| Crack cocaine | 16 | (5.7) | 3.3-9.1 |
| Heroin | 11 | (3.9) | 2.0-6.9 |
| Ecstasy (3,4-methylenedioxymethamphetamine) | 11 | (3.9) | 2.0-6.9 |
| Amphetamines | 9 | (3.2) | 1.5-6.0 |
| Cocaine | 8 | (2.8) | 1.2-5.5 |
| Opiate substitutes | 4 | (1.4) | 0.4-3.6 |
| Dependent use of illicit or non-prescribed drugs (SDS score ≥ 7) | 47 | (16.7) | 12.5-21.5 |
| Frequency of dependent use of individual drug types | |||
| Cannabis | 36 | (12.8) | 9.1-17.2 |
| Cocaine/crack cocaine | 12 | (4.3) | 2.2-7.3 |
| Heroin/opiates | 6 | (2.1) | 0.8-4.6 |
| Sedatives/tranquillisers | 6 | (2.1) | 0.8-4.6 |
| Alcohol use (past year) | |||
| Abstinent | 71 | (25.2) | 20.2-30.7 |
| Non-harmful alcohol use (AUDIT < 8) | 139 | (49.3) | 43.3-55.3 |
| Harmful use (AUDIT ≥ 8) | 72 | (25.5) | 20.5-31.0 |
| Summary | |||
| No harmful alcohol use or drug use reported | 158 | (56.0) | 50.0-61.9 |
| Harmful alcohol use or drug use reported | 124 | (44.0) | 38.1-49.9 |
| Prevalence of comorbidity | |||
| Comorbid patients with low referral potential2 | 86 | (30.5) | 25.2-36.2 |
| Comorbid patients with high referral potential3,4 | 38 | (13.5) | 9.7-18.0 |
| Illicit or non-prescribed drug use | |||
| Opiate and/or cocaine/other stimulant dependence | 15 | (4.3) | 2.2-7.3 |
| Opiate dependence | 6 | (2.1) | 0.8-4.6 |
| Opiate dependence with injected drug use | 3 | (1.1) | 0.2-3.1 |
| Alcohol use | |||
| Severe alcohol problems (AUDIT score ≥ 15) | 26 | (9.2) | 6.1-13.2 |
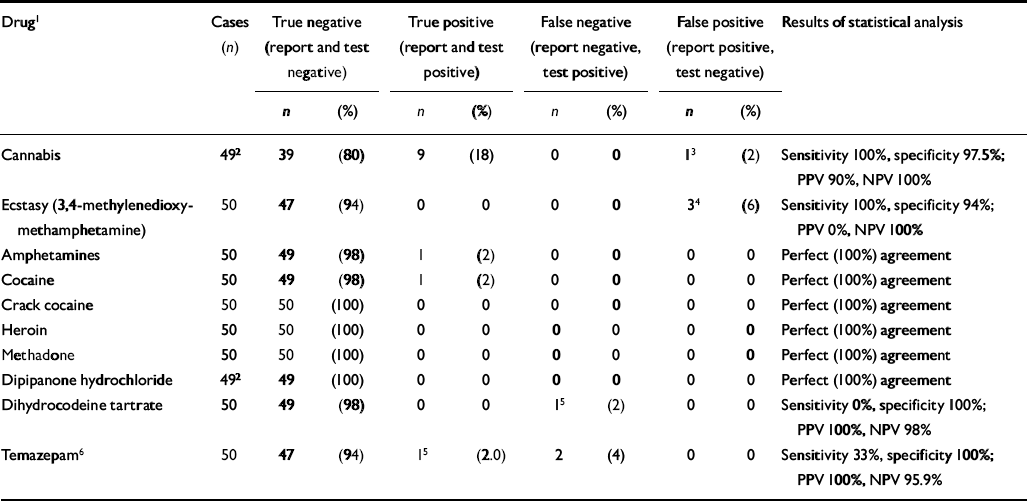
Table 2 presents the findings of the comparison between self-reported ‘pastmonth’ drug use and the hair and urine analysis. This shows that virtually no unreported drug use was detected by hair and urine analysis. Although 18 respondents refused to provide samples, 4 of these reported drug use and there was no case in which care coordinators reported drug use that the patient denied.
Table 2 Validity assessment of self-reported drug use in community mental health team patients: comparison in matched subsample of 50 cases between self-reported drug use (past month) and use as detected by analysis of hair and urine samples
| Drug1 | Cases (n) | True negative (report and test negative) | True positive (report and test positive) | False negative (report negative, test positive) | False positive (report positive, test negative) | Results of statistical analysis | ||||
|---|---|---|---|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | n | (%) | |||
| Cannabis | 492 | 39 | (80) | 9 | (18) | 0 | 0 | 13 | (2) | Sensitivity 100%, specificity 97.5%; PPV 90%, NPV 100% |
| Ecstasy (3,4-methylenedioxy-methamphetamine) | 50 | 47 | (94) | 0 | 0 | 0 | 0 | 34 | (6) | Sensitivity 100%, specificity 94%; PPV 0%, NPV 100% |
| Amphetamines | 50 | 49 | (98) | 1 | (2) | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Cocaine | 50 | 49 | (98) | 1 | (2) | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Crack cocaine | 50 | 50 | (100) | 0 | 0 | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Heroin | 50 | 50 | (100) | 0 | 0 | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Methadone | 50 | 50 | (100) | 0 | 0 | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Dipipanone hydrochloride | 492 | 49 | (100) | 0 | 0 | 0 | 0 | 0 | 0 | Perfect (100%) agreement |
| Dihydrocodeine tartrate | 50 | 49 | (98) | 0 | 0 | 15 | (2) | 0 | 0 | Sensitivity 0%, specificity 100%; PPV 100%, NPV 98% |
| Temazepam6 | 50 | 47 | (94) | 15 | (2.0) | 2 | (4) | 0 | 0 | Sensitivity 33%, specificity 100%; PPV 100%, NPV 95.9% |
Prevalence of comorbidity in drug and alcohol services
Three-quarters of drug service patients (n=161) rated positive for at least one psychiatric disorder (Table 3). A psychotic disorder was present in 17 patients (8%), personality disorder in 80 (37%) and severe depression in 58 (27%). The prevalence of all psychiatric disorders was markedly higher among alcohol service patients, although the small sample size means that the 95% confidence intervals for prevalence estimates are wide (Table 3).
Table 3 Drug and alcohol service patients: prevalence rates of psychiatric disorder and of non-referable and referable comorbidity

| Drug service patients (n=216) | Alcohol service patients (n=62) | |||||
|---|---|---|---|---|---|---|
| n | (%) | Exact binomial 95% CI | n | (%) | Exact binomial 95% CI | |
| Non-substance-induced psychotic disorders | 17 | (8) | 4.7-12.3 | 12 | (19) | 10.4-31.4 |
| Schizophrenia | 6 | (3) | 1.0-5.9 | 2 | (3) | 0.4-11.2 |
| Bipolar affective disorder | 1 | (1) | 0.01-2.6 | 3 | (5) | 1.0-13.5 |
| Non-specific psychosis | 10 | (5) | 2.2-8.3 | 7 | (11) | 4.7-21.9 |
| Personality disorder | 80 | (37) | 30.6-43.9 | 33 | (53) | 40.1-66.0 |
| Affective and/or anxiety disorder | 146 | (68) | 60.9-73.8 | 50 | (81) | 68.6-89.6 |
| Severe depression | 58 | (27) | 21.1-33.3 | 21 | (34) | 22.3-47.0 |
| Mild depression | 87 | (40) | 33.7-47.1 | 29 | (47) | 34.0-59.9 |
| Severe anxiety | 41 | (19) | 14.0-24.9 | 20 | (32) | 20.9-45.3 |
| Summary | ||||||
| No disorder | 55 | (25) | 19.8-31.8 | 9 | (15) | 6.9-25.8 |
| Psychiatric disorder present | 161 | (75) | 68.2-80.2 | 53 | (85) | 74.2-93.1 |
| Prevalence of comorbidity | ||||||
| No comorbid psychiatric disorder | 55 | (26) | 19.8-31.8 | 9 | (15) | 6.9-25.8 |
| Low potential for referral (disorder present, but no additional vulnerability criteria) | 122 | (57) | 49.6-63.2 | 33 | (53) | 40.1-66.0 |
| High potential for referral1 | 39 | (18) | 13.2-23.8 | 20 | (32) | 20.9-45.3 |
| Severe depression plus vulnerability criteria | 22 | (10) | 6.5-15.0 | 8 | (13) | 5.7-23.9 |
| Psychosis plus vulnerability criteria | 17 | (8) | 4.7-12.3 | 12 | (19) | 10.4-31.4) |
Comparison of prevalence rates between centres
CMHT populations
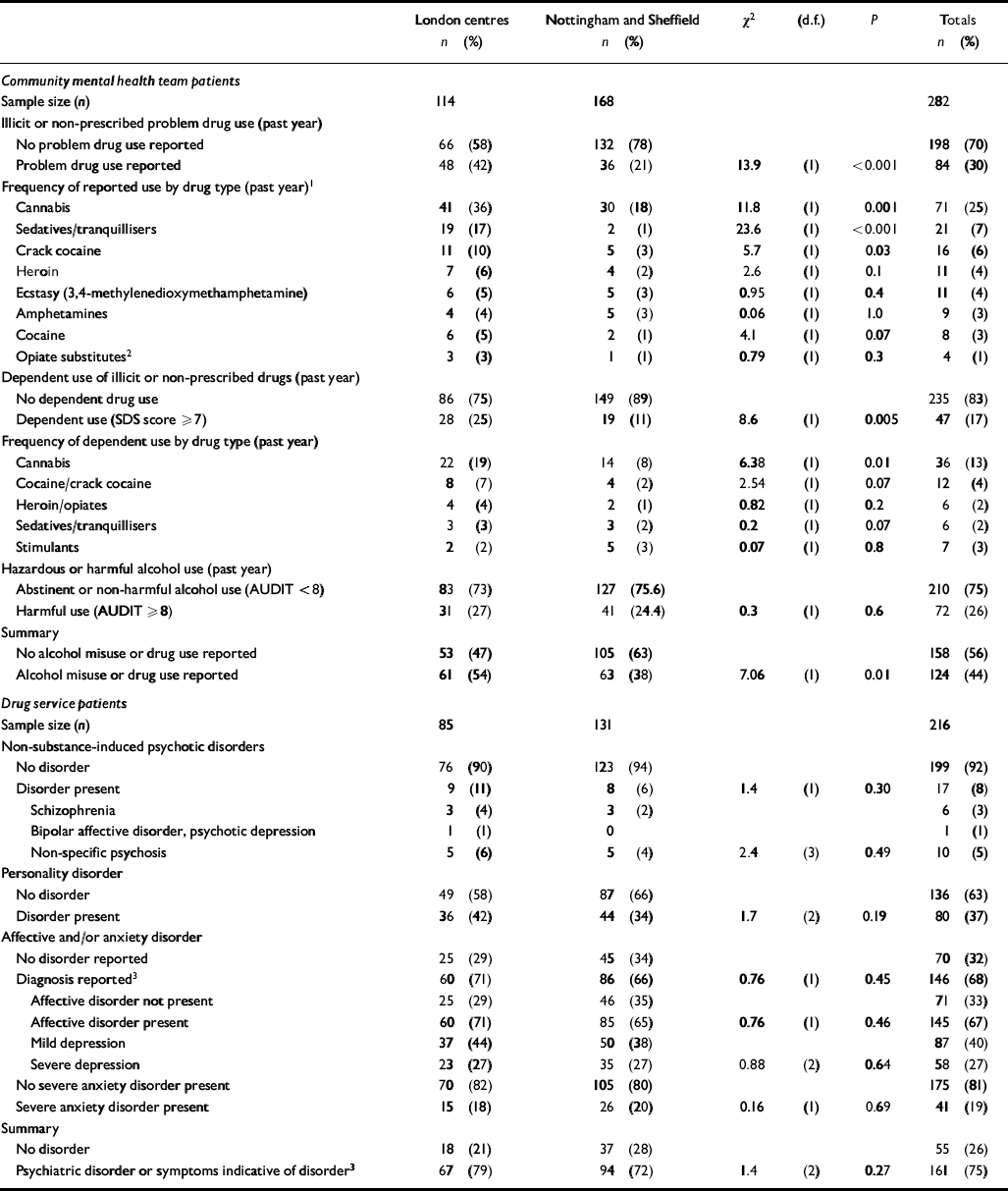
Table 4 shows that a significantly higher proportion of CMHT patients from London centres reported problem drug use than those from Nottingham and Sheffield (42% v. 21, χ2=13.9, d.f.=1, P<0.001). Patients reporting problem drug use in London centres (n=48) also reported pastyear use of a higher number of drug types (mean=2.38) than drug-using patients in Nottingham and Sheffield (n=36; mean= 1.65). Cannabis, sedatives/tranquillisers and crack cocaine use were all reported by a significantly higher proportion of patients in London centres than in Nottingham and Sheffield. The prevalence of any drug dependency was also significantly higher in patients from the London centres (25% v. 11; χ2=8.6, d.f.=1, P=0.005).
Table 4 Comparison between London centres and Nottingham/Sheffield in the prevalence of comorbidity: prevalence of self-reported problem drug use and harmful alcohol use in the past year in community mental health team patients, and prevalence of psychiatric disorders (psychosis, personality disorder, affective/anxiety disorder) in drug service patients
| London centres | Nottingham and Sheffield | χ2 | (d.f.) | P | Totals | ||||
|---|---|---|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | ||||
| Community mental health team patients | |||||||||
| Sample size (n) | 114 | 168 | 282 | ||||||
| Illicit or non-prescribed problem drug use (past year) | |||||||||
| No problem drug use reported | 66 | (58) | 132 | (78) | 198 | (70) | |||
| Problem drug use reported | 48 | (42) | 36 | (21) | 13.9 | (1) | <0.001 | 84 | (30) |
| Frequency of reported use by drug type (past year)1 | |||||||||
| Cannabis | 41 | (36) | 30 | (18) | 11.8 | (1) | 0.001 | 71 | (25) |
| Sedatives/tranquillisers | 19 | (17) | 2 | (1) | 23.6 | (1) | <0.001 | 21 | (7) |
| Crack cocaine | 11 | (10) | 5 | (3) | 5.7 | (1) | 0.03 | 16 | (6) |
| Heroin | 7 | (6) | 4 | (2) | 2.6 | (1) | 0.1 | 11 | (4) |
| Ecstasy (3,4-methylenedioxymethamphetamine) | 6 | (5) | 5 | (3) | 0.95 | (1) | 0.4 | 11 | (4) |
| Amphetamines | 4 | (4) | 5 | (3) | 0.06 | (1) | 1.0 | 9 | (3) |
| Cocaine | 6 | (5) | 2 | (1) | 4.1 | (1) | 0.07 | 8 | (3) |
| Opiate substitutes2 | 3 | (3) | 1 | (1) | 0.79 | (1) | 0.3 | 4 | (1) |
| Dependent use of illicit or non-prescribed drugs (past year) | |||||||||
| No dependent drug use | 86 | (75) | 149 | (89) | 235 | (83) | |||
| Dependent use (SDS score ≥7) | 28 | (25) | 19 | (11) | 8.6 | (1) | 0.005 | 47 | (17) |
| Frequency of dependent use by drug type (past year) | |||||||||
| Cannabis | 22 | (19) | 14 | (8) | 6.38 | (1) | 0.01 | 36 | (13) |
| Cocaine/crack cocaine | 8 | (7) | 4 | (2) | 2.54 | (1) | 0.07 | 12 | (4) |
| Heroin/opiates | 4 | (4) | 2 | (1) | 0.82 | (1) | 0.2 | 6 | (2) |
| Sedatives/tranquillisers | 3 | (3) | 3 | (2) | 0.2 | (1) | 0.07 | 6 | (2) |
| Stimulants | 2 | (2) | 5 | (3) | 0.07 | (1) | 0.8 | 7 | (3) |
| Hazardous or harmful alcohol use (past year) | |||||||||
| Abstinent or non-harmful alcohol use (AUDIT <8) | 83 | (73) | 127 | (75.6) | 210 | (75) | |||
| Harmful use (AUDIT ≥8) | 31 | (27) | 41 | (24.4) | 0.3 | (1) | 0.6 | 72 | (26) |
| Summary | |||||||||
| No alcohol misuse or drug use reported | 53 | (47) | 105 | (63) | 158 | (56) | |||
| Alcohol misuse or drug use reported | 61 | (54) | 63 | (38) | 7.06 | (1) | 0.01 | 124 | (44) |
| Drug service patients | |||||||||
| Sample size (n) | 85 | 131 | 216 | ||||||
| Non-substance-induced psychotic disorders | |||||||||
| No disorder | 76 | (90) | 123 | (94) | 199 | (92) | |||
| Disorder present | 9 | (11) | 8 | (6) | 1.4 | (1) | 0.30 | 17 | (8) |
| Schizophrenia | 3 | (4) | 3 | (2) | 6 | (3) | |||
| Bipolar affective disorder, psychotic depression | 1 | (1) | 0 | 1 | (1) | ||||
| Non-specific psychosis | 5 | (6) | 5 | (4) | 2.4 | (3) | 0.49 | 10 | (5) |
| Personality disorder | |||||||||
| No disorder | 49 | (58) | 87 | (66) | 136 | (63) | |||
| Disorder present | 36 | (42) | 44 | (34) | 1.7 | (2) | 0.19 | 80 | (37) |
| Affective and/or anxiety disorder | |||||||||
| No disorder reported | 25 | (29) | 45 | (34) | 70 | (32) | |||
| Diagnosis reported3 | 60 | (71) | 86 | (66) | 0.76 | (1) | 0.45 | 146 | (68) |
| Affective disorder not present | 25 | (29) | 46 | (35) | 71 | (33) | |||
| Affective disorder present | 60 | (71) | 85 | (65) | 0.76 | (1) | 0.46 | 145 | (67) |
| Mild depression | 37 | (44) | 50 | (38) | 87 | (40) | |||
| Severe depression | 23 | (27) | 35 | (27) | 0.88 | (2) | 0.64 | 58 | (27) |
| No severe anxiety disorder present | 70 | (82) | 105 | (80) | 175 | (81) | |||
| Severe anxiety disorder present | 15 | (18) | 26 | (20) | 0.16 | (1) | 0.69 | 41 | (19) |
| Summary | |||||||||
| No disorder | 18 | (21) | 37 | (28) | 55 | (26) | |||
| Psychiatric disorder or symptoms indicative of disorder3 | 67 | (79) | 94 | (72) | 1.4 | (2) | 0.27 | 161 | (75) |
Overall, there was a marked and statistically significant difference in proportions of patients reporting problem drug use and/or harmful alcohol use between London centres and Nottingham/Sheffield. This difference was mainly attributable to the higher reported prevalence of problem drug use in London, as there was no significant difference in the prevalence of harmful alcohol use between London centres and Nottingham/Sheffield.
We completed an extended multivariate analysis to investigate whether the observed differences in prevalence of drug use was explicable in terms of demographic variables (gender, ethnicity, age) and case-mix variables (presence of harmful alcohol use, psychiatric case-mix). This analysis revealed that the univariate odds ratio of problem drug use for patients on a London service case-load was 2.86 compared with Nottingham/Sheffield (95% CI 1.67–4.90). When the above variables were included in the multiple regression model we found that the adjusted odds ratio (AOR) of problem drug use in London centres over Nottingham/Sheffield was marginally reduced, but a large and statistically significant difference remained (AOR=2.52, 95% CI 1.31–4.85). Hence, a significant excess in problem drug use exists in the London centres compared with Nottingham and Sheffield which cannot be explained by controlling for the above variables.
We repeated this analysis to assess the association between reported harmful alcohol use in the past year using the same demographic (gender, ethnicity, age) and psychiatric case-mix variables but substituting ‘presence of drug use’ for ‘presence of harmful alcohol use’. The univariate odds ratio of harmful alcohol use for London CMHT patients was 1.18 compared with Nottingham and Sheffield (95% CI 0.68–2.04). However, as indicated by the confidence interval, the difference in odds is not statistically significant. When the above variables are included in the multiple regression model the adjusted odds ratio of alcohol misuse in London centres over Nottingham and Sheffield is reduced to a marginal level (AOR=1.05, 95% CI 0.52–2.11). Hence, this series of adjusted analyses showed statistically significant difference in prevalence of drug use between centres after adjustment for the selected case-mix variables. This contributes to a statistically significant difference in comorbidity (problem drug and/or harmful alcohol use). However, there is no evidence of a difference in the prevalence of harmful alcohol use between centres.
Drug and alcohol services
Table 4 compares the observed prevalence rates of psychiatric disorder in drug service patients between London centres and Nottingham/Sheffield. Despite a consistent pattern of marginally higher prevalence in London centres across the spectrum of disorders, there is no statistically significant difference in the proportions assessed to have one or more disorder, or a disorder within any of the three main subgroups assessed (psychosis, personality disorder, affective and anxiety disorder). We implemented an extended multivariate analysis to assess whether there was any difference in the odds of comorbidity between the London and Nottingham/Sheffield samples after adjustment for demographic (gender, ethnicity, age) and case-mix (presence of alcohol misuse, drug use profile) variables.
This analysis revealed that the univariate odds ratio of any psychiatric disorder for patients on a London service case-load was 1.47 (95% CI 0.77–2.80) compared with Nottingham/Sheffield. However, as indicated by the confidence interval, the difference in odds is not statistically significant. When the above variables are included in the multiple regression model the adjusted odds ratio of psychiatric disorder in London centres over Nottingham/Sheffield is marginally reduced (AOR=1.24, 95% CI 0.57–2.70). Hence, no significant unexplained excess in psychiatric disorder among drug service patients exists in London centres over Nottingham/Sheffield. We repeated the analysis using the presence of psychotic disorder as our outcome variable, with similar results.
Potential for cross-referral of patients
CMHT patients
Just six of the CMHT patients were opiate-dependent and had a high referral potential for statutory opiate-based drug treatment services. An additional nine patients reported crack cocaine or other stimulant dependence and would potentially qualify for brief intervention or referral to stimulant clinics (if available). Although significant additional numbers were cannabis-dependent, these patients are unlikely to meet referral criteria applied by routinely available drug services. (No drug service patient was dependent solely on cannabis in our sample.) The potential for referral to alcohol services appears to be greater, given that almost a tenth of patients (n=26) reported severe alcohol misuse (i.e. AUDIT score >15; Table 1).
Substance misuse service patients
Non-substance-related psychotic disorder was identified in 17 drug service patients and 12 alcohol service patients. All exhibited ‘complex care needs’ and recorded high CPRS scores (median for drug service patients 22, range 0–42; median for alcohol service patients 32, range 13–54) relative to psychiatric service patients with a psychotic disorder (median 8, range 0–38). Hence they were likely to have high referral potential to CMHTs for enhanced CPA management. A further 10–13% in each population had severe depression and ‘complex care needs’, which might have made them candidates for CMHT management. Thus, in total, 39 drug service patients (18%) and 20 alcohol service patients (32%) appeared to have a high potential for CMHT referral (see Table 3).
Identification and management of comorbidity
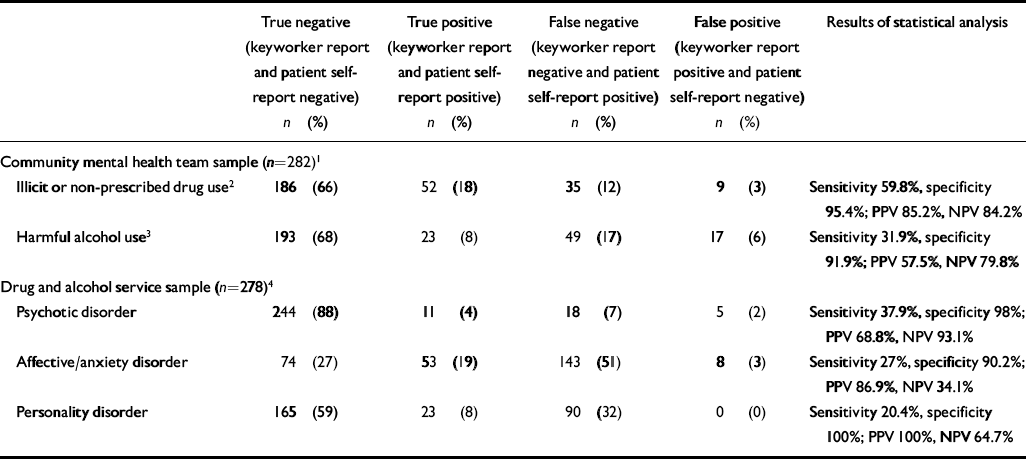
We compared comorbidity reported by care coordinators and keyworkers with the relevant reference assessments obtained at interview. Patients without comorbidity were generally correctly identified as such by services (specificity >90%). However, substance misuse service patients with psychiatric disorders and CMHT patients reporting harmful alcohol use were mostly unrecognised (sensitivity 20–38%). Only in relation to CMHT patients reporting (any) drug use did care coordinators achieve moderately good sensitivity (60%) (Table 5).
Table 5 Matched case comparison between keyworker or care coordinator reports of comorbidity and reference assessments obtained at interview
| True negative (keyworker report and patient self-report negative) | True positive (keyworker report and patient self-report positive) | False negative (keyworker report negative and patient self-report positive) | False positive (keyworker report positive and patient self-report negative) | Results of statistical analysis | |||||
|---|---|---|---|---|---|---|---|---|---|
| n | (%) | n | (%) | n | (%) | n | (%) | ||
| Community mental health team sample (n=282)1 | |||||||||
| Illicit or non-prescribed drug use2 | 186 | (66) | 52 | (18) | 35 | (12) | 9 | (3) | Sensitivity 59.8%, specificity 95.4%; PPV 85.2%, NPV 84.2% |
| Harmful alcohol use3 | 193 | (68) | 23 | (8) | 49 | (17) | 17 | (6) | Sensitivity 31.9%, specificity 91.9%; PPV 57.5%, NPV 79.8% |
| Drug and alcohol service sample (n=278)4 | |||||||||
| Psychotic disorder | 244 | (88) | 11 | (4) | 18 | (7) | 5 | (2) | Sensitivity 37.9%, specificity 98%; PPV 68.8%, NPV 93.1% |
| Affective/anxiety disorder | 74 | (27) | 53 | (19) | 143 | (51) | 8 | (3) | Sensitivity 27%, specificity 90.2%; PPV 86.9%, NPV 34.1% |
| Personality disorder | 165 | (59) | 23 | (8) | 90 | (32) | 0 | (0) | Sensitivity 20.4%, specificity 100%; PPV 100%, NPV 64.7% |
Small minorities of CMHT patients with comorbidity had received alcohol- or drug-related interventions in the month prior to assessment – 15 of 72 reporting harmful alcohol use (21%) and 14 of 84 reporting problem drug use (17%) – mostly counselling provided through the CMHT. Seven patients had contact with specialist drug or alcohol services. More patients with high referral potential (as defined above) received substance misuse interventions, but interventions were more likely to be provided to patients with either high or low referral potential if a care coordinator identified the comorbidity problem. For example, 11 of 14 CMHT patients with identified severe alcohol problems received interventions compared with 1 of the 12 whose severe problems were undetected.
More than a fifth of drug and alcohol services patients with comorbidity (48 of 214) had contact with psychiatric services, of whom 26 (12%) were allocated to CMHT management during the previous month. Patients with ‘high’ referral potential were significantly more likely to have contact with psychiatric services than those rated ‘low’ (35/59, 59% v. 13/155, 8%; χ2=60.8, d.f.=1, P<0.001). Some patients with comorbidity reported consultations with a psychiatrist in the substance misuse service (n=41, 19%) or with a general practitioner (n=57, 27%) about their mental health problems, but 32% (n=68) received no intervention. Most of the latter were patients with undetected, ‘low referral potential’ problems (48/68, 71%).
DISCUSSION
Study limitations
Certain study limitations should be acknowledged. First, we assessed comorbidity within current treatment populations, which tend to include more complex cases; therefore, findings are not generalisable to the same diagnostically defined groups within the general population. Second, given our sample sizes, some prevalence estimates lack precision. Third, the study compares the prevalence of comorbidity in samples drawn from two urban centres in London and from Nottingham and Sheffield. Although the study represents an advance on previous singlecentre studies and highlights the potential for variability in prevalence, we need to exercise caution in our interpretation of these findings. We make no claim that Nottingham and Sheffield are representative of urban areas outside London. Similarly, it is important to note that the London centres were both inner-city ones and not representative of London as a whole. People in inner London with severe mental illness have rates of geographical mobility that are twice as high as those for outer London. This may help account for higher psychiatric morbidity (Reference Lamont, Ukoumunne and TyrerLamont et al, 2000). Further investigation in more regions would be required before any definitive picture emerges about regional variation in prevalence.
Despite these limitations, the study provides strong evidence that comorbidity is highly prevalent in CMHT, drug and alcohol treatment populations. Our findings relating to the profile and management of comorbidity also have major implications for service development.
Prevalence and pattern of comorbidity
Overall, 44% of CMHT patients reported past-year problem drug use and/or harmful alcohol use. This is higher than previously observed in comparable UK populations using similar assessment methods (33–36%) and is largely accounted for by a higher level of drug use than previously reported (Reference Menezes, Johnson and ThornicroftMenezes et al, 1996; Reference Wright, Gournay and GlorneyWright et al, 2000; Reference Duke, Pantelis and McPhillipsDuke et al, 2001). Hair and urine analysis revealed no significant covert drug use and suggested that these self-reported drug use data provide a reliable and valid basis for prevalence estimation. Given that consent for obtaining hair and urine samples was separate from and subsequent to interviews, we can exclude the possibility that patients were more accurate in reporting drug use because they knew they were to be tested. The prevalence of harmful alcohol use among CMHT patients (26%) is consistent with previous estimates (20–32%) using self-reported measures (Reference Menezes, Johnson and ThornicroftMenezes et al, 1996; Reference Wright, Gournay and GlorneyWright et al, 2000; Reference Duke, Pantelis and McPhillipsDuke et al, 2001).
Findings in relation to the validity of prevalence estimates of comorbidity reported by keyworkers at the case-load census have important implications for service development, the interpretation of previously published research and the design of future studies. Studies that have estimated prevalence on the basis of assessments provided by keyworker informants may underestimate prevalence (e.g. Reference Graham, Maslin and CopelloGraham et al, 2001; Reference Weaver, Rutter and MaddenWeaver et al, 2001).
Our findings confirm that comorbidity of severe mental illness and substance misuse is highly prevalent in urban UK mental health settings. However, findings in relation to the level of problem drug use are even more striking when the differences between centres are considered. In the London centres, 42% of CMHT patients reported problem drug use and 25% were assessed as drug dependent. Overall, more than half of London CMHT patients reported substance misuse problems in the past year. We stress the importance of cautious interpretation of these findings, but nevertheless this does appear to confirm the view that patients with such comorbidity may represent the core client group of CMHTs in certain inner-city areas, where the prevalence may be dramatically high (Reference Banerjee, Clancy and CromeBanerjee et al, 2002).
Large majorities of patients treated for drug and alcohol misuse experience psychiatric disorder, although there was no suggestion that these rates differed significantly between centres in our study. Our estimates for the prevalence of severe depression and personality disorder are consistent with other studies of comparable populations (Reference Regier, Farmer and RaeRegier et al, 1990; Reference VerheulVerheul, 2001). However, the prevalence of psychosis (drug service patients 8%, alcohol service patients 19%) was significantly higher than previously reported (Reference Regier, Farmer and RaeRegier et al, 1990) and was 10 times (drug) and 24 times (alcohol) the prevalence rate for psychosis in the urban UK population (0.8%; Reference Jenkins, Bebbington and BrughaJenkins et al, 1998).
Implications for management
In each population studied, comorbid presentations were heterogeneous. Responding to the level and range of need will be challenging given associated clinical management problems (Reference Scott, Johnson and MenezesScott et al, 1998; Reference Hunt, Bergen and BashirHunt et al, 2002), the current configuration and orientation of services (Reference JohnsonJohnson, 1997; Reference Weaver, Renton and StimsonWeaver et al, 1999) and the difficulty both services have in reliably identifying patients with comorbid problems. Most drug-using CMHT patients exhibit patterns of use unlikely to make them eligible for generally available drug treatment programmes. Even among patients with a high referral potential, a minority had contact with drug services. Larger proportions of drug and alcohol services patients with high referral potential had contact with mental health services, but there was still extensive unmet need for referral and intervention.
Implications for service development and future research
It is evident that ‘parallel’ or ‘serial’ treatment by independent and substance misuse services and CMHTs (as currently configured) cannot meet the level and range of need presented by comorbid populations. Integrated treatment teams – favoured in the USA to provide treatment for both types of disorders without cross-referral (Reference Drake, Noordsy, Ackerson, Lehman and DixonDrake et al, 1995) – lack a strong evidence base (Reference Ley, Jeffery and McLarenLey et al, 1999) and may not be appropriate or replicable in UK settings (Reference Hall and FarrellHall & Farrell, 1997; Reference JohnsonJohnson, 1997; Reference Weaver, Renton and StimsonWeaver et al, 1999). Moreover, there is a danger that the development of integrated teams could result in drug and alcohol services remaining underresourced and narrowly focused (i.e. upon opiate use, in the case of drug services). Instead, we support current efforts to develop the capacity and competency of ‘mainstream’ services (Reference Banerjee, Clancy and CromeBanerjee et al, 2002).
Drug and alcohol treatment services already provide mental health interventions (both pharmacological and psychotherapeutic) to significant numbers of their patients with mental health problems. However, there were equally large numbers of patients with comorbidity whose needs were unmet or unidentified. Resources need to be deployed enabling substance misuse services to offer evidence-based treatments to a much higher proportion of these patients (Reference Hall and FarrellHall & Farrell, 1997). Models of collaborative working with local general practitioners and psychotherapy services (in addition to general adult psychiatry) should be developed and evaluated. In relation to CMHTs, our findings suggest that mainstream staff need to be able to implement at least basic management of comorbidity. To achieve this, staff are likely to need enhanced training in the assessment of drug and alcohol problems (and in the use of appropriate evaluation tools), as well as motivational techniques to improve patient engagement with substance misuse treatment and achieve harm minimisation goals. Interventions to address these skill deficits require urgent evaluation.
Although enhanced training has rightly been identified as a key component of our response to comorbidity (Reference Banerjee, Clancy and CromeBanerjee et al, 2002), there is also a need to resource, develop and evaluate new service-based assessment, treatment and management approaches, which can support psychiatric and substance misuse services in offering evidence-based treatments to much higher proportions of their patients with problems of comorbidity.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Comorbidity of psychiatric disorders and substance misuse is highly prevalent in those receiving treatment for one of these conditions.
-
▪ Psychiatric teams and substance misuse services fail to identify significant proportions of patients with such comorbidity on their case-loads. Most patients with substance misuse problems on psychiatric case-loads receive no substance misuse interventions, and a third of substance misuse patients with mental health problems do not receive any mental health interventions.
-
▪ Comorbidity cannot be adequately managed by cross-referral between psychiatric and substance misuse services as currently configured and resourced. A new approach is needed to enable psychiatric and substance misuse services to offer evidence-based treatment of comorbid conditions to a much higher proportion of their patients.
LIMITATIONS
-
▪ Because comorbidity was assessed within treatment populations, findings are not generalisable to the same diagnostically defined groups within the general population.
-
▪ Some prevalence estimates lack precision owing to small sample sizes.
-
▪ We found significant differences in the prevalence of drug use among psychiatric patients in different centres, but evidence from more centres is required before firm conclusions about regional differences in prevalence are made.
Acknowledgements
The authors of this work received funding under the Department of. Health's Drug Misuse Research Initiative. The views expressed in this. publication are those of the authors and not necessarily those of the. sponsors. The authors express their gratitude to the funders for supporting. this work. The Centre for Research on Drugs and Health Behaviour is core. funded by the London Regional Office of the National Health Service. Executive.
The COSMIC study group consists of the following members: Imperial College, London: Tim Weaver, Vikki Charles, Zenobia Carnwath, Peter Madden, Adrian. Renton, Gerry Stimson, Peter Tyrer, Thomas Barnes, Chris Bench and Susan. Paterson; Turning Point, Brent: Chris Ford; Central and North West London. Mental Health NHS Trust: Jonathon Greenside, Owen Bowden Jones and William. Shanahan; Community Health Sheffield NHS Trust: Helen Bourne, Muhammad Z. Iqbal and Nicholas Seivewright; Nottingham Healthcare NHS Trust: Sylvia. Cooper, Katina Anagostakis, Hugh Middleton and Neil Wright.









eLetters
No eLetters have been published for this article.