Introduction
Traditionally only a small proportion of the work force was engaged in shift work. In recent times, working patterns have adapted in response to changes in economic pressures and greater consumer demand for services that operate on a ‘24 hour a day’ basis, resulting in an increase in shift work. The term ‘shift work’ often covers a wide variety of working arrangements. The Council Directive 93/104/EC of 23 November 1993 defines shift work as ‘any method of organising work in shifts whereby workers succeed each other at the same work stations according to a certain pattern, including a rotating pattern, and which may be continuous or discontinuous, entailing the need for workers to work at different times over a given period of days or weeks’(1, 2). However, there is no consensus definition of the term among the published scientific literature. In simple terms, shift work is often referred to as working primarily outside of normal daytime working hours or on a schedule other than the standard working week. Shift patterns vary depending on the timing of the shift (early morning, afternoon, evening, night), the rotation cycle (number of days between two identical sequences), the direction of rotation (forward or backward rotating) and the stability of the time slots planned (permanent shifts v. rotating shifts)(Reference Esquirol, Perret and Ruidavets3). In Europe approximately 17 % of the workforce is engaged in this type of work schedule(4).
There are many economic advantages to an increase in shift work, namely the creation of employment, increased provision of services to customers and improved trade opportunities. Unfortunately, shift work has been reported to have a negative impact on the health of workers and is accompanied by greater incidence of non-communicable diseases such as cancer(5), CVD(Reference Tuchsen, Hannerz and Burr6), metabolic(Reference De Bacquer, Van Risseghem and Clays7), gastrointestinal(Reference Knutsson and Boggild8) and sleep disorders(Reference Rajaratnam, Howard and Grunstein9). Many of the risk factors for non-communicable diseases, including poor diet, lack of physical activity, deleterious lifestyle behaviours such as excess alcohol and smoking, insufficient sleep and being overweight, are frequently reported among shift workers. The aim of the present review is to evaluate the current status of the evidence on the diet and lifestyle habits of shift workers, and the subsequent health risk compared with non-shift workers. In addition, the evidence for barriers and opportunities for improving the health and lifestyle of this group will also be explored, which extends the scope of previous reviews in this area.
Methodology
This is a narrative review which aimed to summarise the effects of shift work on workers’ lifestyle and health risk, and to address the barriers to and opportunities for shift workers to lead a healthier lifestyle. An extensive literature search for relevant peer-reviewed scientific articles and reports was conducted, using targeted Internet searches, for example, Medline and Web of Knowledge. Key words searches were conducted using the terms ‘shiftwork’ or ‘shift work’. Articles were considered if they were available in full text, were in English and were conducted among human subjects. The relevance and strength of each article are dealt with throughout the text, with critical comments on the factors which made for higher- and lower-quality publications.
Shift work and lifestyle habits
Dietary intakes
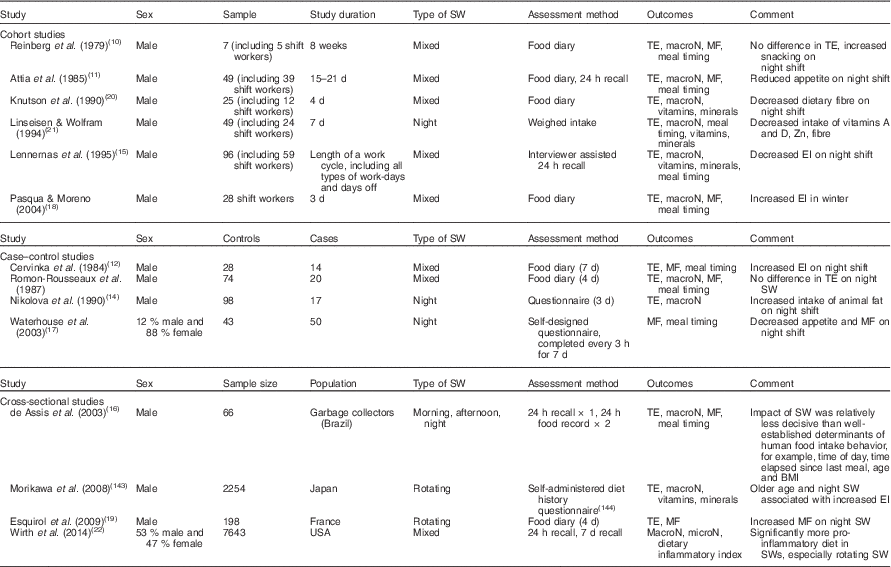
Table 1 summarises the results of studies investigating dietary intakes among shift workers. Earlier studies in the area showed that, overall, total energy intake of shift workers is similar to that of day workers(Reference Reinberg, Migraine and Apfelbaum10–Reference Nikolova, Handjiev and Angelova14), with this being confirmed by more recent findings(Reference Lennernas, Hambraeus and Akerstedt15–Reference Esquirol, Bongard and Mabile19). However, methodological issues existed in many of these studies, with small sample sizes(Reference Reinberg, Migraine and Apfelbaum10, Reference Pasqua and Moreno18, Reference Knutson, Andersson and Berglund20), reliance on self-reported food diaries(Reference Attia, Mustafa and Khogali11, Reference Pasqua and Moreno18–Reference Knutson, Andersson and Berglund20) and failure to compare dietary intakes with non-shift worker controls(Reference de Assis, Kupek and Nahas16, Reference Pasqua and Moreno18) apparent. Due to these limitations in study design and to variability in defining shift work and assessing dietary intake, results between studies are difficult to compare.
Table 1 Summary of studies on dietary intake in shift workers (SWs)Footnote *

SW, shift work; TE, total energy; macroN, macronutrients; MF, meal frequency; EI, energy intake; microN, micronutrients.
* Table adapted from Lowden et al. (Reference Lowden, Moreno and Holmbäck137).
While total energy intake does not appear to be affected, shift work may make an impact on diet quality. Alterations in macronutrient intakes have been observed, such as increased intake of saturated fat(Reference Nikolova, Handjiev and Angelova14, Reference Esquirol, Bongard and Mabile19) and decreased intake of polyunsaturated fat(Reference Linseisen and Wolfram21) and dietary fibre after commencing shift work(Reference Knutson, Andersson and Berglund20). In addition, decreased intake of a number of essential micronutrients, such as vitamins A, D and E, and Zn is documented among shift workers, relative to day workers(Reference Linseisen and Wolfram21). Furthermore, one study reported that the diets of shift workers, and in particular rotating shift workers, were significantly more pro-inflammatory than day workers(Reference Wirth, Burch and Shivappa22), but the biological significance of this in terms of dietary inflammatory load remains unclear. Along with alterations in dietary quality, much of the recent evidence has collectively shown that shift workers differ from day workers with respect to the distribution of their energy intake over 24 h(Reference Reinberg, Migraine and Apfelbaum10, Reference Lennernas, Hambraeus and Akerstedt15, Reference de Assis, Kupek and Nahas16, Reference Pasqua and Moreno18, Reference Esquirol, Bongard and Mabile19). Erratic meal patterns, increased consumption of energy later in the day and increased snacking were common, with multiple snacks being consumed during the night shift in place of a full meal. The significance of these altered dietary habits must be considered. There is convincing evidence that night time eating can cause disruptions to endogenous circadian rhythms, compared with day time eating(Reference Pasqua and Moreno18, Reference Morgan, Hampton and Gibbs23–Reference Simon, Weibel and Brandenberger27), which can result in significantly elevated postprandial TAG levels and plasma glucose levels on the night shift, as compared with the day shift. This may have negative implications for health, particularly in relation to risk of insulin resistance, type 2 diabetes mellitus (T2DM) and the metabolic syndrome (MetS). It has therefore been suggested that restricting fat intake at night time in workers who are not adapted to night shift work may be beneficial(Reference Al-Naimi, Hampton and Richard26).
Physical activity
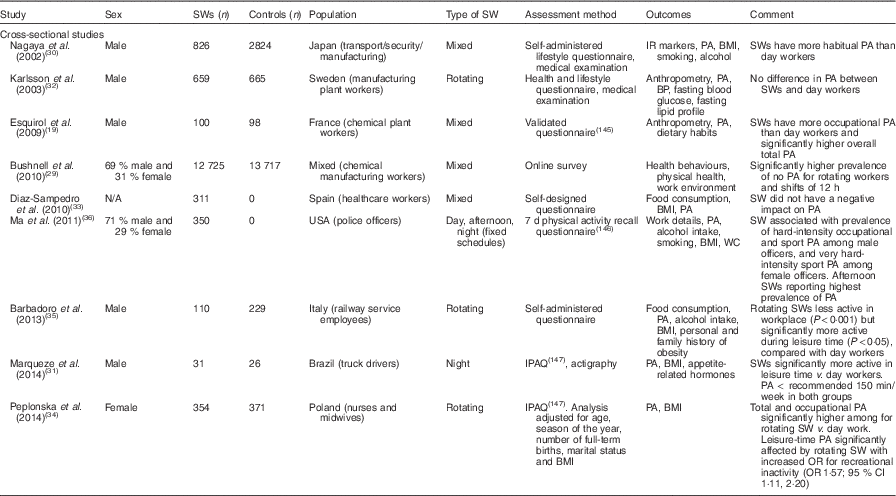
The evidence of the impact of shift work on physical activity presents a mixed picture (Table 2). Studies have reported negative(Reference Siedlecka28, Reference Bushnell, Colombi and Caruso29), positive(Reference Esquirol, Bongard and Mabile19, Reference Nagaya, Yoshida and Takahashi30, Reference Marqueze, Ulhoa and Castro Moreno31) or no effects(Reference Karlsson, Knutsson and Lindahl32, Reference Diaz-Sampedro, Lopez-Maza and Gonzalez-Puente33) on levels of physical activity in shift workers compared with day workers. However, the definitions of physical activity used may, at least in part, contribute to these equivocal results. Different measures used include leisure-time activity, habitual activity, total activity and/or occupational activity. Even when studies have analysed both occupational and leisure-related activity, differences in results have been observed. Some have reported that shift workers had significantly higher occupational activity compared with day workers, resulting in significantly higher overall total activity(Reference Esquirol, Bongard and Mabile19, Reference Peplonska, Bukowska and Sobala34), while others have reported that shift workers had lower occupational activity but higher leisure-related activity(Reference Barbadoro, Santarelli and Croce35). One factor potentially contributing to these inconclusive results is the occupational heterogeneity of subjects in these studies. Broadly speaking, subjects were recruited from manufacturing(Reference Esquirol, Bongard and Mabile19, Reference Bushnell, Colombi and Caruso29, Reference Nagaya, Yoshida and Takahashi30, Reference Karlsson, Knutsson and Lindahl32), transport(Reference Nagaya, Yoshida and Takahashi30, Reference Marqueze, Ulhoa and Castro Moreno31, Reference Barbadoro, Santarelli and Croce35), security(Reference Nagaya, Yoshida and Takahashi30, Reference Ma, Burchfiel and Fekedulegn36) or healthcare(Reference Diaz-Sampedro, Lopez-Maza and Gonzalez-Puente33, Reference Peplonska, Bukowska and Sobala34) sectors, with roles potentially varying widely in terms of occupational activity. Another limitation is that much of the evidence is cross-sectional in nature and relied on self-reported data, with just one study(Reference Marqueze, Ulhoa and Castro Moreno31) using actigraphy to compare activity levels between day workers and shift workers. Objective measures such as this would provide more reliable data. Unfortunately, despite the number of studies in this area, the discrepancies in study design mean that no definitive conclusions can be currently drawn on the effects of shift work on physical activity.
Table 2 Summary of studies on physical activity (PA) in shift workers (SWs)

SW, shift work; IR, insulin resistance; BP, blood pressure; N/A, not available; WC, waist circumference; IPAQ, International Physical Activity Questionnaire.
Despite the lack of conclusive evidence, barriers to engagement in regular physical activity among this group have been explored. Shift workers may have difficulty in implementing and maintaining an active lifestyle(Reference Kaliterna, Prizmic and Zganec37), with reasons such as fatigue due to a demanding schedule, difficulty engaging in social forms of exercise or team sports, possible increased perceived exertion and fatigue during exercise performed at night or in the early morning(Reference Atkinson, Fullick and Grindey38) all cited. A lack of facilities available at times convenient to shift workers may also be an issue. The health implications of an inactive lifestyle are large, with indisputable evidence for the effectiveness of regular exercise in the prevention of chronic non-communicable diseases and premature death(Reference Warburton, Nicol and Bredin39). Where it occurs, physical inactivity therefore may exacerbate the risk of chronic disease among shift workers.
Smoking
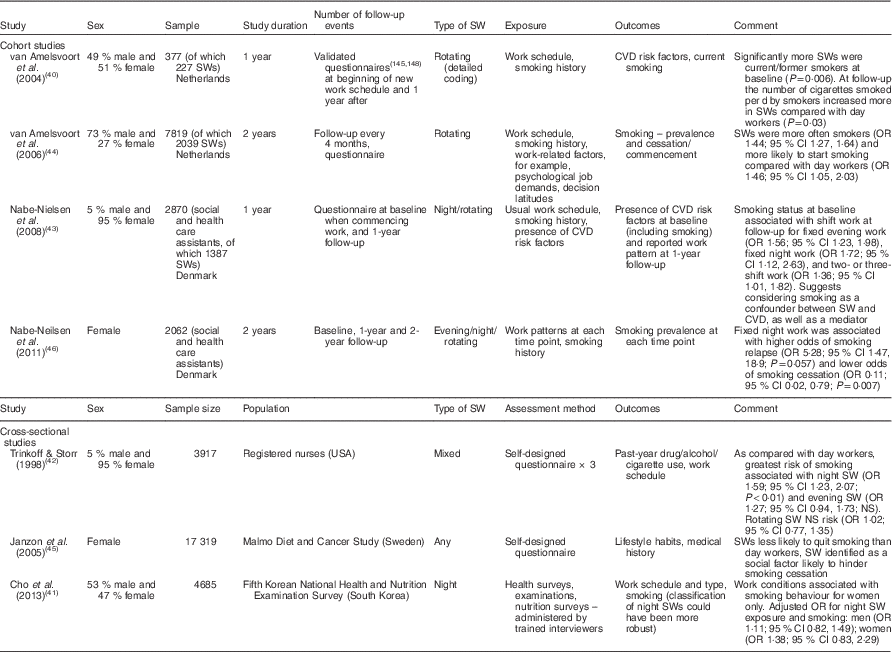
The results of cross-sectional data and cohort studies exploring smoking habits among shift workers are presented in Table 3. Engaging in shift work(Reference van Amelsvoort, Schouten and Kok40, Reference Cho, Kim and Myong41) and, in particular, night shift work(Reference Trinkoff and Storr42, Reference Nabe-Nielsen, Garde and Tuchsen43) was shown to be associated with a higher prevalence of smoking(Reference Cho, Kim and Myong41–Reference Nabe-Nielsen, Garde and Tuchsen43) or increased number of cigarettes smoked per person(Reference van Amelsvoort, Schouten and Kok40). Longer working hours appear to affect rates of smoking also, with working shifts >8 h in length(Reference Trinkoff and Storr42) or working 49–60 h per week(Reference Cho, Kim and Myong41) associated with higher rates of smoking. Shift workers have also been shown to be more likely to take up smoking once engaged in shift work(Reference van Amelsvoort, Jansen and Kant44). Furthermore, it has been reported that shift workers are less likely to quit smoking(Reference Janzon, Engstrom and Lindstrom45, Reference Nabe-Nielsen, Quist and Garde46) and have higher odds of smoking relapse(Reference Nabe-Nielsen, Quist and Garde46) compared with day workers.
Table 3 Summary of studies on smoking in shift workers (SWs)

SW, shift work.
Alcohol
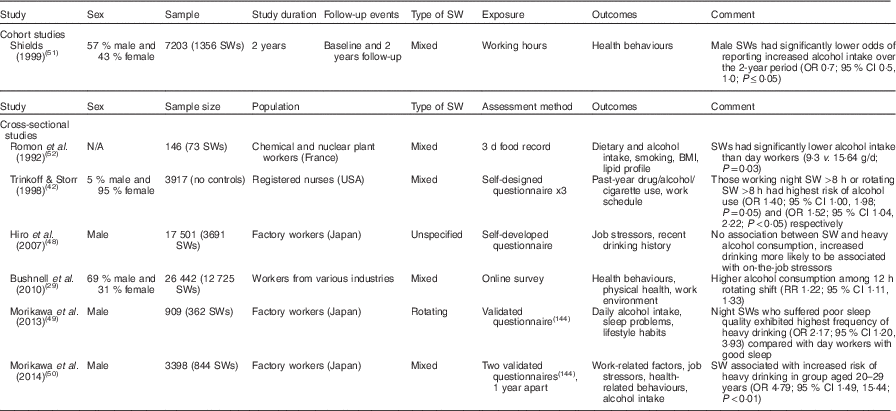
The results of observational studies of alcohol consumption among shift workers are presented in Table 4, with mixed reports observed. Shift workers may use alcohol in an attempt to overcome difficulties sleeping(47), or to ease the stresses associated with their work pattern(Reference Bushnell, Colombi and Caruso29). In the included studies, ‘heavy drinking’ was typically defined as >40–60 g of alcohol per d(Reference Hiro, Kawakami and Tanaka48–Reference Morikawa, Nakamura and Sakurai50), ≥5 drinks on one occasion(Reference Trinkoff and Storr42), or increased consumption on previous measurements of consumption(Reference Shields51). A modestly increased risk of heavy drinking was associated with shift work by some, and this was typically related to younger age(Reference Morikawa, Nakamura and Sakurai50), night shift(Reference Trinkoff and Storr42, Reference Morikawa, Sakurai and Nakamura49) or rotating shift(Reference Bushnell, Colombi and Caruso29, Reference Trinkoff and Storr42) of greater than 8 h in length. However, in some cases, this relationship was mediated by shift work-related sleep issues(Reference Morikawa, Sakurai and Nakamura49). In contrast, other studies have found no association(Reference Hiro, Kawakami and Tanaka48) or an inverse association(Reference Shields51, Reference Romon, Nuttens and Fievet52) between shift work and alcohol consumption. As shift work often interferes with family time and social activities, there may be reduced opportunities for social alcohol consumption among this group. In summary, while shift work may increase the likelihood of increased alcohol consumption, available data are merely observational in nature and various factors such as age, sex and shift type or length may potentially influence this.
Table 4 Summary of studies on alcohol consumption in shift workers (SWs)

SW, shift work; N/A, not available; RR, relative risk.
Sleep patterns
Shift workers report more sleep problems compared with the general public, and it has been estimated that 10–30 % of shift workers suffer from shift work disorder(Reference Gumenyuk, Roth and Drake53), a circadian rhythm sleep disorder characterised by insomnia and excessive sleepiness(Reference Dagan54). Some of the most problematic symptoms reported are difficulty falling asleep, shortened sleep duration and somnolence during working hours that persists during days off(Reference Akerstedt55). Levels of sleep disturbance have been compared with clinical insomnia(Reference Akerstedt56).
Shift patterns, shift lengths, direction of rotation, and length of recovery time between shifts have been examined, with respect to their impact on sleep patterns. Those working night shifts, rotating night shifts and early morning shifts have been reported to have the shortest average sleep duration or the most disturbances in sleep–wake patterns(Reference Akerstedt55–Reference Pilcher, Lambert and Huffcutt58). Forward rotating shift schedules are considered to be more beneficial to workers in terms of health and sleep disturbances, along with moving from slow- to fast-rotating shifts(Reference Driscoll, Grunstein and Rogers59–Reference Sallinen and Kecklund61). Elsewhere, others have suggested that a slowly rotating shift pattern had the least negative impact on sleep length for schedules that include a night shift(Reference Pilcher, Lambert and Huffcutt58). The effect of shift duration has also been investigated, with little difference noted in the effect of 8 h v. 12 h shifts on sleep patterns(Reference Sallinen and Kecklund61, Reference Smith, Folkard and Tucker62).
A lack of controlled intervention studies in the area makes it difficult to determine the true impact of different shift schedules on sleep patterns. In addition, there is evidence to suggest that there is high inter-individual variability in the ability of workers to tolerate disruption to circadian rhythm caused by shift work, adding further difficulty to the interpretation of the studies published(Reference Costa63, Reference Nachreiner64). Despite this, the evidence indicates that both good physical fitness and sleep hygiene (i.e. habits and practices that are conducive to sleeping well on a regular basis) can be effective in improving tolerance to shift work, by increasing overall efficiency and reducing fatigue. In terms of health risk, disrupted sleep patterns may have metabolic effects that predispose to weight gain. Short sleep duration is generally defined as ≤5–6 h sleep per 24 h, and has been associated with increased BMI(Reference Moreno, Louzada and Teixeira65–Reference Cappuccio, Taggart and Kandala69). While addressing the area of sleep duration and BMI is beyond the scope of this review, short sleep duration may potentially mediate a relationship between shift work and obesity.
Summary on the effects of shift work on lifestyle habits
Although not inevitable, shift work can result in altered lifestyle habits. Dietary habits appear to be affected, with more frequent eating occasions, poorer-quality diets and irregular distribution of energy intake over the course of 24 h. It is unclear whether shift work has an impact on physical activity patterns, with mixed results reported. Mixed reports are also observed for alcohol consumption with various factors such as age, sex and shift type affecting study conclusions. In addition increased rates of smoking are reported, with shift workers also less likely to quit smoking compared with day workers, while poor quality and quantity of sleep are also described in the literature. Socio-economic status is known to have a negative impact on dietary and lifestyle habits and on health risk(Reference Pampel, Krueger and Denney70). However, the current review found no evidence to indicate that a social class gradient exists among shift worker groups which might influence health behaviours or health risk, or account in part for some of the differences observed in dietary and lifestyle behaviours. What is clear, however, is that the lifestyle habits described, in conjunction with disruption to circadian rhythms, may create a metabolic environment which can facilitate the development and progression of chronic disease.
Shift work and health risks
As the body has a roughly 24 h circadian rhythm, we are programmed to eat during the day and to sleep at night. The circadian system also regulates the timing of daily variations in numerous behavioural, endocrine and neurophysiological processes(Reference Zhang, Dube and Esser71), for example, sleep–wake cycles, body temperature, blood pressure and the release of hormones. This 24 h rhythm is generated by the suprachiasmatic nucleus, which is located in the anterior hypothalamus of the brain(Reference Schibler and Sassone-Corsi72). Almost all body functions, from those at cellular level to large physiological systems, have a circadian rhythm, and thus disruptions to these rhythms have systemic implications throughout the body. The physiological effects of both circadian rhythm disruption, and the behavioural and psychological effects of shift work exposure may interact, with potential consequences for disease risk as summarised in Fig. 1.

Fig. 1 Circadian disruption and shift work exposure – the potential pathways to disease.
Cancer
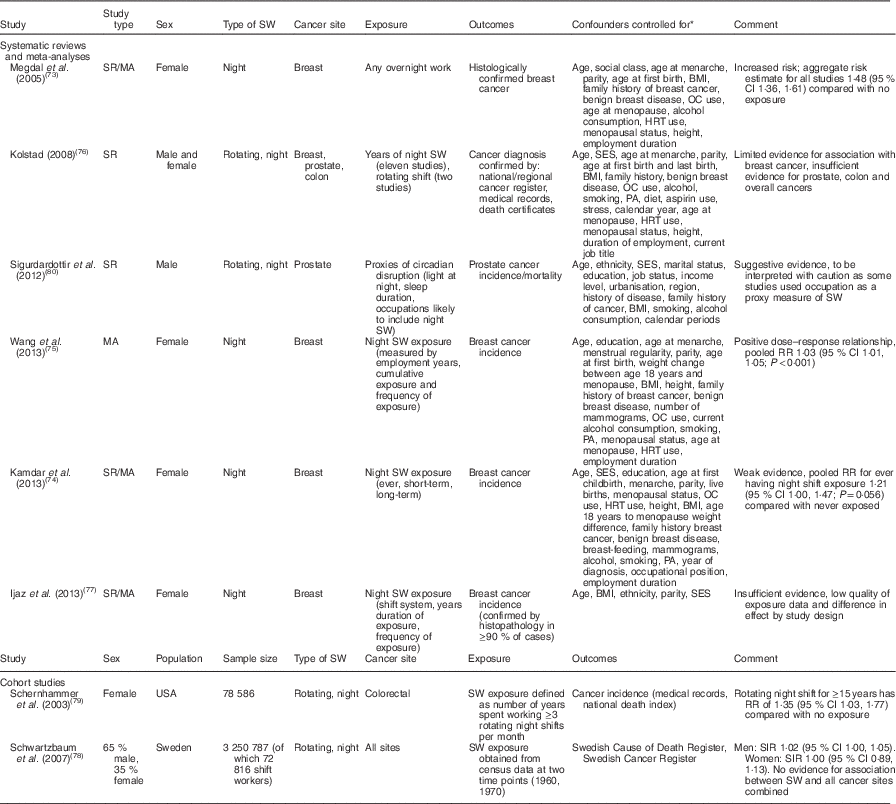
A 2007 report by the International Agency for Research on Cancer(5) classified shift work that involves disruption of the circadian rhythm as a probable human carcinogen. The hypothesis for a potential causal link is based on experimental evidence that melatonin, which is highest at night time, is protective against cancer development, and that exposure to night shift work reduces melatonin levels via increased exposure to light at night. Although extensive observational and cross-sectional data have been published on the relationship between shift work and cancer, inclusion of these studies is beyond the scope of the present review. However, a number of systematic reviews and meta-analyses based on observational data have been conducted, and are summarised in Table 5.
Table 5 Summary of studies on cancer risk in shift workers

SW, shift work; SR, systematic review; MA, meta-analysis; OC, oral contraceptive; HRT, hormone replacement therapy; SES, socio-economic status; PA, physical activity; RR, relative risk; SIR, standardised incidence ratio.
* For systematic reviews/meta-analyses all confounders controlled for are included. All may not be included in each individual original study.
A large proportion of the research into shift work and cancer risk has specifically addressed breast cancer, mainly owing to early interest in breast cancer risk among nurses and flight attendants. Many of these early observational studies showed weak to moderate evidence for an association between breast cancer and shift work; however, these studies had their limitations. Several of the systematic reviews and meta-analyses have since reported moderately increased breast cancer risk due to shift work(Reference Megdal, Kroenke and Laden73, Reference Kamdar, Tergas and Mateen74) and a positive dose–response relationship between shift work exposure and incidence of breast cancer(Reference Wang, Yeung and Chan75). Others have, however, reported limited evidence to support the association between the two(Reference Kolstad76) and have highlighted study limitations such as immeasurable confounding and substantial between study heterogeneity as issues in their analyses. Nonetheless, only one of the systematic reviews/meta-analyses reported insufficient evidence for a causal link(Reference Ijaz, Verbeek and Seidler77), citing the low quality of the exposure data as problematic in providing conclusive evidence. Currently we can only state that while there appears to be some associated increased risk of breast cancer for those engaging in shift work, further work is required to reach a consensus.
Evidence for an association between other forms of cancer and shift work is not particularly strong, with weak or conflicting data reported. This may be, at least in part, owing to a lack of high-quality research in this area. Both the risk of individual cancer types and overall cancer risk have been assessed among shift workers. Those studies addressing all-site cancer risk found insufficient evidence for increased risk among shift workers(Reference Kolstad76, Reference Schwartzbaum, Ahlbom and Feychting78). The association between shift work and colon cancer and colorectal cancer has been explored. With regard to the risk of colorectal cancer among shift workers, reports from the Nurses’ Health Study showed an increased risk of colorectal cancer among those with long-term exposure (≥15 years) to shift work(Reference Schernhammer, Laden and Speizer79); however, elsewhere a critical review found there was insufficient evidence to support an association between shift work and risk of colon cancer, due to the low number of studies in the area(Reference Kolstad76). Prostate cancer risk has also been investigated among this group. Again, as with studies on other cancer types, conflicting results are reported, with insufficient evidence to support an association in one study(Reference Kolstad76), and another reporting suggestive evidence for an association(Reference Sigurdardottir, Valdimarsdottir and Fall80). Overall, evidence for an effect of shift work on cancer risk appears inconclusive, with much variability in study methodologies, including the methods to define shift work and shift work exposure, and the control for confounding factors frequently unclear.
Obesity
Obesity has been identified as another health risk associated with shift work. Studies in the area are presented in Table 6. Epidemiological data suggest that shift workers appear to be heavier, or gain weight more often than day workers(Reference Di Lorenzo, De Pergola and Zocchetti81–Reference Nakamura, Shimai and Kikuchi85). It has also been demonstrated that obesity risk increases according to the duration of shift work exposure(Reference van Amelsvoort, Schouten and Kok83, Reference Ha and Park86, Reference Parkes87). Studies which reported on the longitudinal trends in BMI and shift worker status found that maintaining or changing shift work status can make an impact on BMI(Reference Morikawa, Nakagawa and Miura82, Reference Zhao, Bogossian and Turner84). Those who maintained shift work patterns, or who changed from regular daytime hours to shift work, had a significant increase in BMI. These associations remained after adjusting for confounding variables. While BMI is a useful tool in estimating body fat, waist circumference and waist:hip ratio are useful for estimating central adiposity which is associated with increased health risk. Studies assessing central adiposity revealed a significant association between shift work and increased waist:hip ratio(Reference Nakamura, Shimai and Kikuchi85, Reference Ha and Park86), yet these studies revealed no significant associations between BMI and shift work. This suggests that while shift work may not necessarily increase overall body weight it may detrimentally influence body fat distribution with a tendency towards central adiposity, which may have potential implications for the metabolic and cardiovascular health of shift workers.
Table 6 Summary of studies on obesity risk in shift workers

SW, shift work; SR, systematic review; MA, meta-analysis; WHR, waist:hip ratio; PA, physical activity; BP, blood pressure; HbA1c, glycosylated Hb; WC, waist circumference.
* For systematic reviews/meta-analyses all confounders controlled for are included. All may not be included in each individual original study.
As with other studies in this area, the methodological problems noted previously apply in many of these studies. One systematic review found strong evidence for a crude relationship between shift work exposure and weight gain; however, this evidence was considered insufficient once adjustments for confounding factors were made(Reference van Drongelen, Boot and Merkus88). Another review article on obesity and shift work showed that while there was considerable epidemiological evidence that shift work was associated with an increased risk of metabolic disturbances, such as obesity, many articles included in the review were potentially biased due to lack of protocols to control for confounding factors when anthropometric measures such as height and weight were self-reported(Reference Antunes, Levandovski and Dantas89). While the majority of these studies showed a tendency towards a positive association between shift work and being overweight or obese, the methodological issues recognised highlight that future studies need to address these in order to identify the true impact of shift work on body weight.
Metabolic syndrome
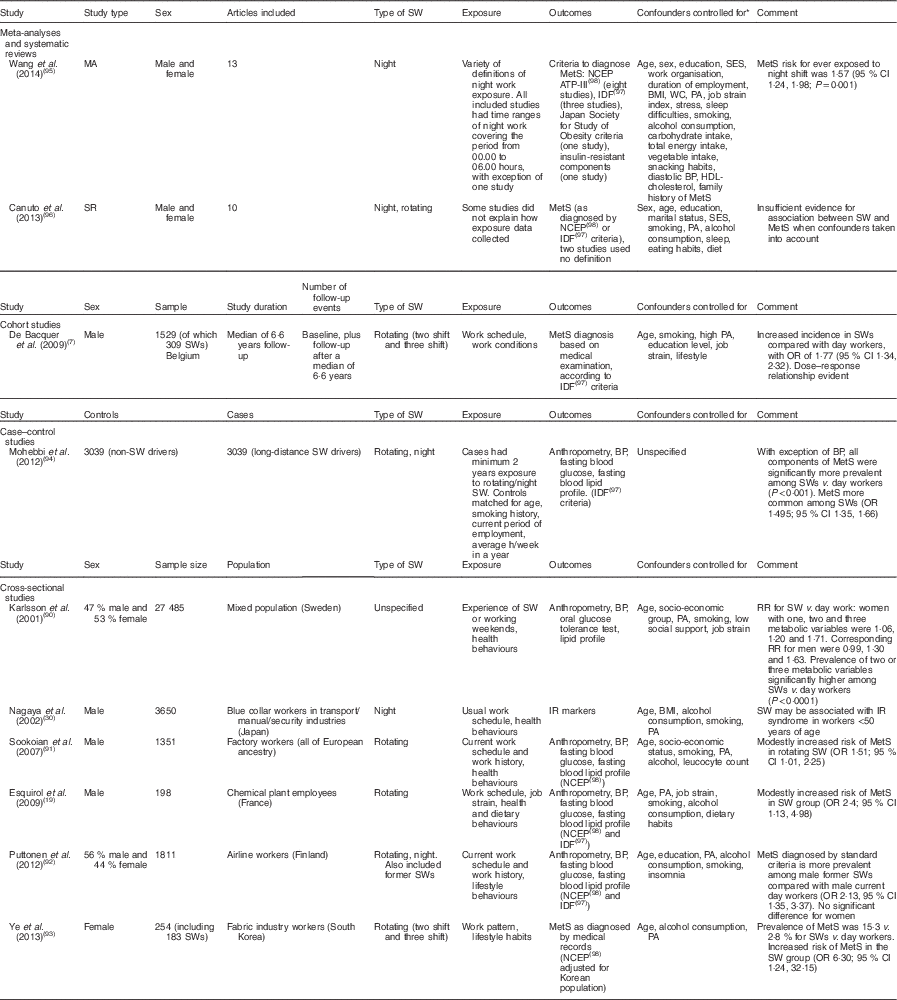
Circadian rhythm disruption can create metabolic disturbances such as lipid and glucose intolerances, with levels shown to be significantly elevated throughout the night shift compared with the day shift(Reference Al-Naimi, Hampton and Richard26). This may potentially contribute towards the risk of the MetS among shift workers. The results of studies addressing shift work and the MetS are presented in Table 7.
Table 7 Summary of studies on metabolic syndrome (MetS) risk in shift workers (SWs)

SW, shift work; MA, meta-analysis; NCEP ATP-III, National Cholesterol Education Program Adult Treatment Panel III; IDF, International Diabetes Foundation; SES, socio-economic status; WC, waist circumference; PA, physical activity; BP, blood pressure; SR, systematic review; RR, relative risk; IR, insulin resistance.
* For systematic reviews/meta-analyses all confounders controlled for are included. All may not be included in each individual original study.
The earliest of these studies noted that obesity, elevated blood TAG and low concentrations of HDL-cholesterol appeared to cluster together more often in shift workers than in day workers, indicating a potential association between shift work and components of the MetS(Reference Karlsson, Knutsson and Lindahl90). Since then, further studies have assessed the risk of the MetS among shift workers, with cross-sectional data indicating a modestly increased risk of the MetS among this group(Reference Esquirol, Bongard and Mabile19, Reference Sookoian, Gemma and Fernandez Gianotti91–Reference Ye, Jeong and Jeon93). In addition to this, case–control data have shown that all components of the MetS, with the exception of hypertension, are significantly more prevalent among shift workers(Reference Mohebbi, Shateri and Seyedmohammadzad94). As with obesity, a dose–response relationship has been observed, with increasing risk of the MetS with increased exposure to shift work(Reference De Bacquer, Van Risseghem and Clays7, Reference Wang, Zhang and Zhang95). Furthermore, the impact of previous shift work on health may persist even after disengaging from shift work, with data suggesting that the MetS may be more prevalent among former shift workers compared with current day workers(Reference Puttonen, Viitasalo and Harma92).
However, difficulties have been identified when attempting to determine the association between the MetS and shift work among higher-quality studies. The results of one meta-analysis suggest a positive association between the MetS and having ever been exposed to night shift work, with higher risk indicated with longer exposure to night shift work(Reference Wang, Zhang and Zhang95). However, in contrast, a recent systematic review, while finding that the majority of studies reported a positive association between the MetS and shift work, concluded that the evidence was insufficient to support an association once confounders were accounted for(Reference Canuto, Garcez and Olinto96). As well as a lack of control for confounders, issues with variability in defining both shift work and the MetS across studies were apparent. Among the included studies, different criteria have been used to define the MetS, with some studies using the International Diabetes Federation (IDF) criteria(Reference Alberti, Eckel and Grundy97) and others using the updated National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP-III) criteria(Reference Grundy, Cleeman and Daniels98). While the IDF includes the same general criteria as the NCEP ATP-III, the presence of central obesity is required to fulfil the definition of the MetS, with ethnic-specific values for waist circumference thresholds. Use of different criteria can make it difficult to compare studies, and it has been previously shown that use of NCEP ATP-III and IDF criteria for determining the MetS among shift workers can yield different results, with the IDF criteria finding a greater prevalence of the MetS compared with the NCEP ATP-III criteria(Reference Copertaro, Bracci, Barbaresi and Santarelli99).
Type 2 diabetes mellitus
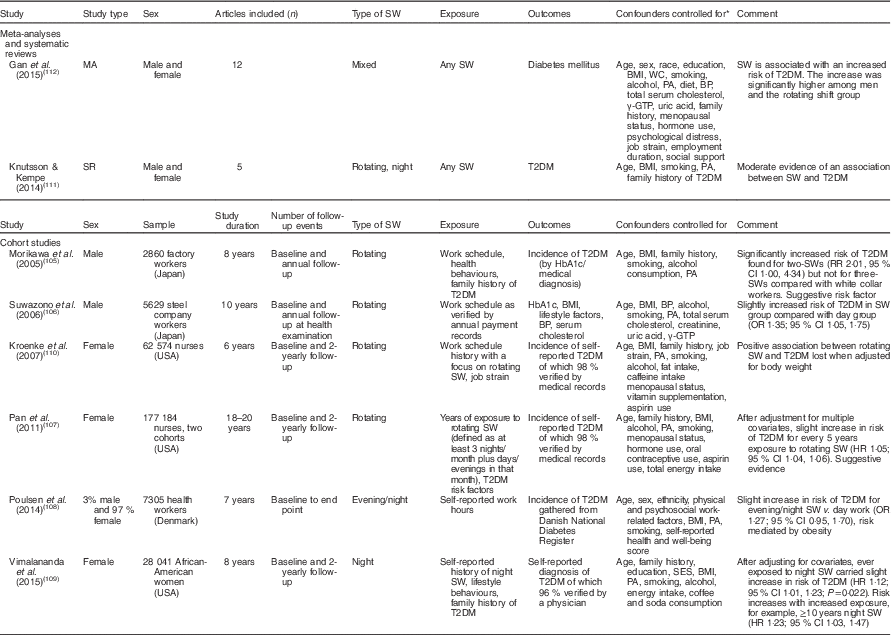
The results of studies addressing shift work and risk of T2DM are presented in Table 8. Findings on disturbed postprandial glucose and lipid profiles among shift workers(Reference Ribeiro, Hampton and Morgan24–Reference Al-Naimi, Hampton and Richard26, Reference Boggild and Knutsson100) suggest that shift work may induce insulin resistance, increasing the risk of T2DM. The regulation of glucose homeostasis is under circadian control, thus highlighting a potential link between chronic circadian misalignment and incidence of T2DM. Clinical studies have demonstrated that acute circadian misalignment (as little as 1–3 weeks) either alone or in conjunction with sleep restriction can cause the dysregulation of glucose homeostasis and postprandial impaired glucose tolerance(Reference Spiegel, Leproult and Van Cauter101–Reference Buxton, Pavlova and Reid104). Therefore, it could be assumed that continued or long-term disruption to circadian rhythms may increase the risk of T2DM.
Table 8 Summary of studies on type 2 diabetes mellitus (T2DM) risk in shift workers (SWs)

SW, shift work; MA, meta-analysis; WC, waist circumference; PA, physical activity; BP, blood pressure; γ-GTP, γ-glutamyl transpeptidase; SR, systematic review; HbA1c, glycosylated Hb; RR, relative risk; HR, hazard ratio; SES, socio-economic status.
* For systematic reviews/meta-analyses all confounders controlled for are included. All may not be included in each individual original study.
Based on evidence from cohort studies, shift work appears to be a suggestive risk factor for T2DM, with slightly increased risk with shift work exposure after adjusting for confounders(Reference Morikawa, Nakagawa and Miura105–Reference Vimalananda, Palmer and Gerlovin109), particularly for rotating shift work(Reference Morikawa, Nakagawa and Miura105–Reference Pan, Schernhammer and Sun107). In some cases, the association was mediated by body weight, with association between T2DM and shift work lost once adjusted for body weight(Reference Kroenke, Spiegelman and Manson110). Duration of exposure to shift work appears to be particularly important with regard to increasing risk(Reference Pan, Schernhammer and Sun107, Reference Vimalananda, Palmer and Gerlovin109). Looking at higher-quality evidence, a systematic review of cohort studies reported moderate evidence for a positive association between shift work and T2DM; however, the low methodological quality of original studies was highlighted as a limitation(Reference Knutsson and Kempe111). Meanwhile, a meta-analysis of observational studies in the area found a modest increase in risk of T2DM for those ever exposed to shift work, and subgroup analyses found higher risk among men and those engaged in rotating shift work(Reference Gan, Yang and Tong112). As before, methodological issues were highlighted, with heterogeneity across many of the original studies due to poor definitions of shift work and variability in shift work exposure. In addition there were inconsistent methods for defining diagnosis of T2DM as the outcome with varying diagnostic criteria used, or with some studies relying on self-reported T2DM diagnosis.
CVD
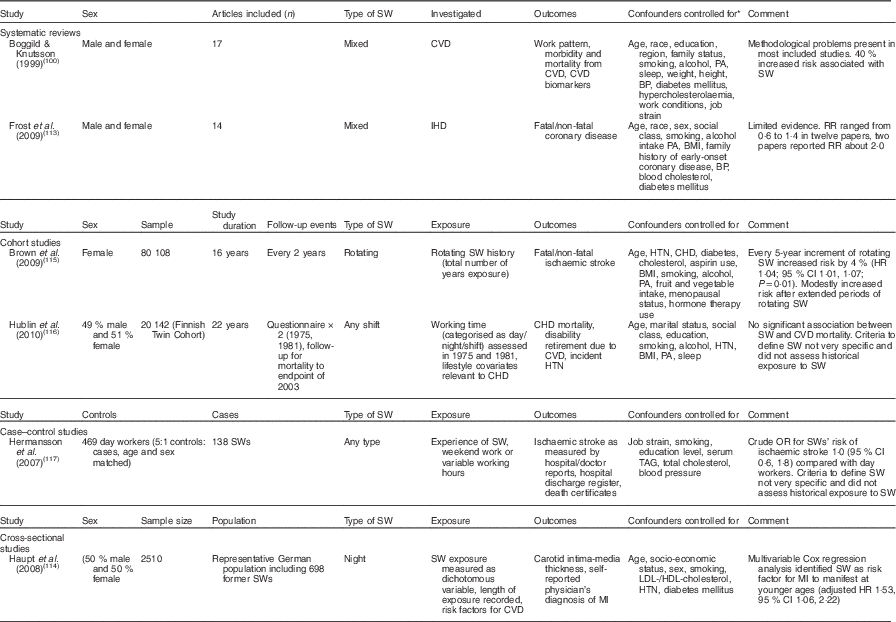
Occupational factors such as sleep duration and shift work have been suspected to be related to risk of CVD. The results from studies in the area are presented in Table 9. The hypothesis for a potential causal link proposes that metabolic changes, psychosocial stress and adverse health behaviours among shift workers may lead to increased CVD risk(Reference Frost, Kolstad and Bonde113). Although studies published over the past two decades suggest an impact of shift work on CVD risk factors, the data are not conclusive.
Table 9 Summary of studies on CVD risk in shift workers (SWs)

SW, shift work; PA, physical activity; BP, blood pressure; RR, relative risk; HTN, hypertension; HR, hazard ratio; MI, myocardial infarction.
* For systematic reviews/meta-analyses all confounders controlled for are included. All may not be included in each individual original study.
Observational evidence shows mixed results for an association between shift work and CVD. Modestly increased risk or suggestive evidence has been observed by some(Reference Haupt, Alte and Dorr114, Reference Brown, Feskanich and Sanchez115), with onset at younger ages among shift workers(Reference Haupt, Alte and Dorr114), or cumulative risk with extended periods of exposure(Reference Brown, Feskanich and Sanchez115). In contrast, other studies indicate no evidence of an association between shift work and CVD(Reference Hublin, Partinen and Koskenvuo116) or increased risk compared with day workers(Reference Hermansson, Gillander Gadin and Karlsson117), and the higher-quality studies have been unable to conclusively confirm an association. Two systematic reviews have indicated that data in the area suggest a modestly increased risk of CVD(Reference Boggild and Knutsson100) or limited evidence for an association(Reference Frost, Kolstad and Bonde113). Both studies highlighted methodological issues in most of the included studies, such as selection bias, exposure and outcome classifications, controlling for confounders and inappropriate comparison groups. Overall, there appears to be suggestive but not conclusive evidence for a relationship between shift work and adverse CVD outcomes.
Gastrointestinal disorders
As early as the 1950s peptic ulcer disease was acknowledged as ‘the occupational disease of shift workers’(Reference Thiis-Evensen118). There is evidence that circadian disruption affects the brain–gut axis, contributing to the pathogenesis of diseases and disorders of the gastrointestinal tract(Reference Hoogerwerf119). Important core functions of the gastrointestinal tract such as motility, maintenance and replacement of the protective barrier, and production of digestive enzymes may be disrupted, and such disruptions have been associated with gastrointestinal symptoms such as abdominal pain, constipation and diarrhoea(Reference Konturek, Brzozowski and Konturek120). Higher-quality data are lacking in this area. The only existing systematic review observed an increased risk of gastrointestinal symptoms, peptic ulcer disease and functional gastrointestinal disease among those engaged in shift work(Reference Knutsson and Boggild8); however, issues were noted with the original studies, with many being of poor quality or inadequately adjusting for confounders such as age, social class and exposure to known gastrointestinal irritants such as non-steroidal anti-inflammatory drugs. In addition only a small number of studies have addressed gastro-oesophageal reflux disease, inflammatory bowel disease and gastrointestinal cancers, all with inconclusive results.
Mental health and cognitive function
While the effect of shift work on physical health has been explored extensively, much less is published on its relationship with mental health. Shift workers may be more susceptible to depressive symptoms for a number of reasons, including disruption to the sleep–wake cycle, poor work–life balance, social desynchronisation, a demanding work environment with low control, and low levels of support at work. Social support from family and friends is also integral to preventing or reducing the impact of depressive disorders, and the social implications of shift work may weaken this crucial support network. In addition, the effect of light at night on mood has been a suggested hypothesis linking circadian disruption to major depression and other mood disorders(Reference Bedrosian and Nelson121).
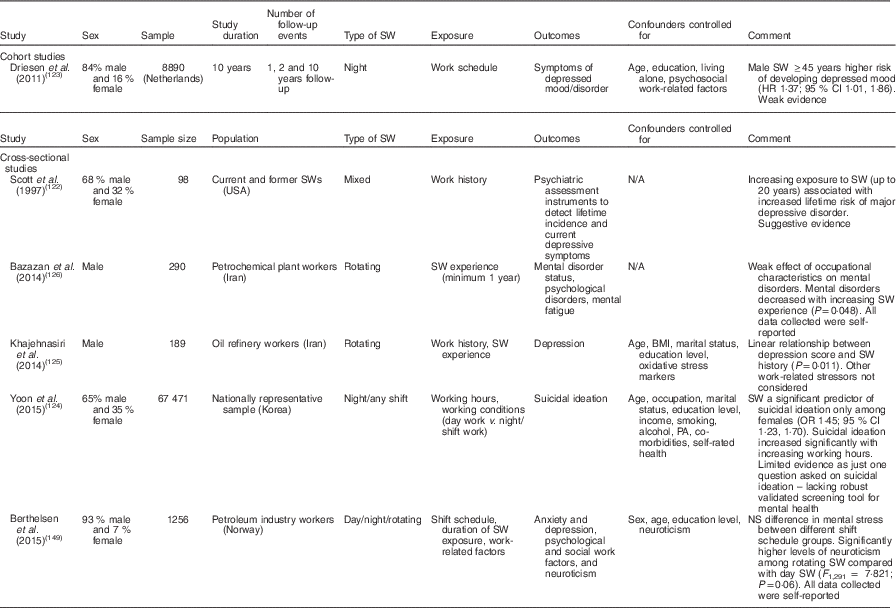
Results of studies on depressive disorders and shift work are presented in Table 10. An association has been reported; however, the evidence is not particularly convincing(Reference Scott, Monk and Brink122, Reference Driesen, Jansen and van Amelsvoort123). Male shift workers over 45 years of age were identified as having the highest risk of developing depressed mood(Reference Driesen, Jansen and van Amelsvoort123), while shift work was a predictor of suicidal ideation among female workers(Reference Yoon, Bae and Kang124). Duration of exposure to shift work is reported to increase risk for depressive disorders(Reference Scott, Monk and Brink122, Reference Khajehnasiri, Akhondzadeh and Mortazavi125); however, elsewhere mental disorders reportedly decreased with increasing shift work experience(Reference Bazazan, Rasoulzadeh and Dianat126). Exploration of mental health among shift workers is very much in the preliminary stages, and many of the available studies lack the use of a robust screening tool or fail to control for possible confounders.
Table 10 Summary of studies on mental health risk in shift workers (SWs)

SW, shift work; HR, hazard ratio; N/A, not available; PA, physical activity.
The effect of shift work on cognitive performance has also been explored, with a theory of bidirectional interactions between circadian processes and cognitive performance suggested(Reference Gritton, Kantorowski and Sarter127). Investigations into the long-term consequences of chronic sleep deprivation showed male shift workers had lower cognitive performance than workers never exposed to shift work, with memory performance decreasing with increasing shift work duration(Reference Rouch, Wild and Ansiau128). A possible reversal of these effects was observed more than 4 years after cessation of shift work. However, more recent data from this ongoing longitudinal cohort study showed that shift work chronically impairs cognition, with a strong association for exposure duration exceeding 10 years. Again, it was shown that recovery of cognitive performance can occur 5 years after cessation of shift work(Reference Marquie, Tucker and Folkard129). The evidence is not conclusive, however, as another longitudinal study demonstrated no association between midlife shift work and long-term cognitive effects in older adults(Reference Devore, Grodstein and Schernhammer130). Reasons for the discrepancies in study results may relate to difficulties in assessing the true impact of shift work on brain function and cognition, due to problems distinguishing this impact from the influence of other related factors such as ageing and altered lifestyle behaviours. Unfortunately, clinical studies in this area are sparse.
Summary of the impact of shift work on health
Overall, it appears that shift work may have a negative impact on health, and the studies included in the present review more often than not showed a tendency towards increased health risk. Common also among many studies was the linear association between the duration of exposure to shift work and increased health risk. However, methodological issues were present in many of the studies, including the use of different measures of risk which increases the difficulty in interpreting and comparing results. To assess the true risk of these conditions for those engaging in shift work, it is necessary to standardise the definition of shift work, shift schedules and study outcome measures in order to provide high-quality evidence for associations between shift work and health risk.
Improving the lifestyle habits and health of shift workers
While other reviews have addressed lifestyle habits and health risks among shift workers(Reference Esquirol, Bongard and Mabile19, Reference Puttonen, Harma and Hublin131, Reference Wang, Armstrong and Cairns132), the present review goes beyond the range of those previously published, by exploring the barriers to improving lifestyle behaviours and the opportunities to promote health and reduce health risk among this group.
Barriers to a healthy lifestyle
The identification of existing barriers to change is necessary if the lifestyle habits of shift workers are to be improved. Data on this topic are sparse, with occupational sectors outside healthcare poorly represented. A number of studies have addressed barriers to healthy eating among occupations that typically involve shift work, such as medical and nursing staff(Reference Winston, Johnson and Wilson133–Reference Phiri, Draper and Lambert136). The most commonly cited perceived barriers across studies were a lack of breaks, shift patterns, poor food selection, inadequate canteen opening times, lack of time and tiredness due to long working hours. Many shift workers are not provided with suitable meal options, sufficient time or appropriately spaced breaks in which to eat their meals in a relaxed environment. It has previously been shown that meal timing and content are constrained by task demands in the work place(Reference Lowden, Moreno and Holmbäck137) and there is also evidence to show that eating on the night shift is driven more by scheduling constraints than by actual hunger(Reference Waterhouse, Buckley and Edwards17). Few workers felt that their employer was supportive of healthy eating(Reference Winston, Johnson and Wilson133–Reference Faugier, Lancaster and Pickles135), which again identifies the workplace as a key area for change in order to facilitate healthier lifestyle behaviours. The studies in this area highlight the need for workplace interventions that encourage well-designed work schedules and regular meal breaks, improved availability of healthy dining options and access to canteens at evenings and weekends. In addition, for some shift workers lack of nutritional knowledge may be a further barrier to healthy eating(Reference Faugier, Lancaster and Pickles134, Reference Faugier, Lancaster and Pickles135), presenting an opportunity for the provision of nutrition education tailored to shift work.
Meals outside the workplace should also be considered. Shift workers often experience a mismatch between their own routine and that of family and friends(Reference Lowden, Moreno and Holmbäck137). This may result in a variety of scenarios – dining with family in the evening and eating again later in work resulting in over eating, or choosing not to dine with family resulting in meals that are self-prepared and eaten alone, which can result in poorer-quality meals(Reference Waterhouse, Bailey and Tomlinson138). Disruption between work and home life routines may be particularly significant for women with children, who have a high off-job workload due to domestic duties, and often find themselves preparing family meals at times that are at odds with their own sleep pattern and appetite(Reference Atkinson, Fullick and Grindey38).
Opportunities for a healthier lifestyle
Workplace initiatives and careful management of shift work by employers can help minimise the deleterious effects of shift work on health and promote workers’ wellbeing. Employers stand to gain from investing in the health of their employees, with costs minimised by reduced sickness and absence, reduced staff turnover, lower numbers of errors and accidents and their associated costs, and increased productivity(47). As most adults spend approximately 60 % of their waking hours at work, worksites provide many opportunities to promote dietary and physical activity programmes and also have the opportunity to reach large populations(Reference Morgan, Collins and Plotnikoff139). Systematic reviews of studies involving workplace initiatives for promoting health among employees generally report short-term consistent modest reduction in weight, as a result of such interventions(Reference Anderson, Quinn and Glanz140, Reference Benedict and Arterburn141). However, they also identify a lack of data on long-term health and economic outcomes and the dearth of good-quality research in this area, with many of the published studies limited by weak methodologies and difficulties with subject recruitment and retention.
Specifically in shift workers, Morgan et al. (Reference Morgan, Collins and Plotnikoff139) conducted a prospective randomised controlled trial for a workplace-based weight loss programme targeting overweight and obese male shift workers. The intervention group had significant reductions in weight, waist circumference, BMI, systolic blood pressure and resting heart rate, and a significant increase in physical activity. This programme was successful despite a low level of face-to-face contact. Online support meant that participants could access support and information at their convenience, a feature which may be particularly appealing to shift workers. Further opportunities to improve health, such as health screening, may also be beneficial to the shift work population. Viitasalo et al. (Reference Viitasalo, Lindstrom and Hemio142) showed that screening for T2DM and CVD among airline employees effectively identified employees with an increased risk who would benefit from lifestyle intervention. However, the benefits of regular health screening of shift workers for markers of chronic diseases requires further exploration before recommendations can be made.
Conclusion
A recurrent theme in the literature is the lack of a standardised definition for shift work and the variability in shift patterns. This, along with inter-study variability in methods to define shift work exposures and outcomes, and poor control for confounding factors, impairs the ability to clearly demonstrate associations between shift work and lifestyle or health risks. Nonetheless, a trend towards shift work being associated with negative outcomes for lifestyle behaviours and health risks is apparent. It is evident that there is a lack of information on the barriers to health and the opportunities for effective health improvement and promotion among this group. This warrants investigation, in order to help those engaging in shift work to overcome associated occupational hazards and lead a healthier lifestyle. The current prevalence of non-communicable diseases and mental health disorders in society, coupled with a workforce where shift work is increasingly prevalent, means that addressing the associated health risks is important in terms of both public and occupational health, and economic and personal cost. Identifying the barriers and opportunities for improving health will help to direct health promotion to this group, enabling the implementation of effective interventions such as nutrition and lifestyle education and workplace health-promotion programmes, which will serve towards making the healthier choice more accessible to all employees.
Acknowledgements
The present study was supported by safefood, the Food Safety Promotion Board, under grant no. 10-2013.
F. N. conducted the majority of the literature review, drafted the original manuscript and compiled the tables. J. K., B. L., K. P. and C. C. critically reviewed and revised the manuscript, and F. N. prepared the manuscript for submission in its final form. All authors read and approved the final version of the manuscript before submission.
There are no conflicts of interest.