Involuntary admissions to psychiatric hospitals are practised throughout the world. There has been much debate on the ethical justification, Reference Hoyer1–Reference Lidz and Hoge3 appropriate legislation and best practice of involuntary admissions, but limited empirical research. Reference Katsakou and Priebe4 Involuntary patients are more likely to be readmitted compulsorily after their index hospitalisation than voluntary patients. Reference Houston and Mariotto5–Reference McEvoy, Applebaum, Apperson, Geller and Freter8 Although involuntarily hospitalised patients tend to improve clinically Reference McEvoy, Applebaum, Apperson, Geller and Freter8–Reference Kjellin, Anderson, Candefjord, Palmstierna and Wallsten10 their views on the justification and the overall evaluation of their admission vary widely. Reference Katsakou and Priebe11,Reference Farnham and James12 Between 33% and 81% of patients have been found to retrospectively regard their treatment as justified and/or beneficial. Reference Katsakou and Priebe4 There are, however, no sufficiently powered published studies to identify factors associated with more or less favourable outcomes. Reference Katsakou and Priebe4 Such evidence is vital to understand the processes leading to different outcomes in order to improve practice.
The present study assessed two important outcomes of involuntary hospital admissions in the largest national study to date: (a) as an objective outcome criterion we selected involuntary hospital readmissions within 1 year after the index admission (involuntary admissions are unequivocally a negative outcome, whereas voluntary readmissions might sometimes be a positive sign of therapeutic collaboration); and (b) as a patient-rated outcome we examined whether patients retrospectively assessed their involuntary index admission as justified. Within medicine, admissions against the wishes of patients are specific to psychiatry, and this is based on the assumption that their current illness makes it difficult for patients to accept treatment. Reference Wertheimer13,Reference Beck and Golowka14 Thus, effective care may be expected to be associated with patients seeing the admission as justified in retrospect, at a stage when the acute phase has been overcome.
We assessed these outcomes 1 year after the index admission. We investigated conventional socio-demographic and clinical data as well as patients' perception of treatment and coercion at baseline as possible explanatory variables for outcome.
Method
Design
We conducted an observational prospective study with a 1-year follow-up. Involuntarily admitted patients were recruited in 22 hospitals provided by 8 mental health National Health Service (NHS) trusts in England. Hospitals were purposively chosen to cover geographically spread urban and rural areas. Baseline variables and readmission data at 1 year were collected for the total sample. A consenting sample was interviewed at baseline and at 4 weeks, 3 months and 1 year.
Participants
Consecutive patients between 18 and 65 years, living in the catchment area of the participating hospitals, admitted under Sections 2, 3 and 4 of the Mental Health Act 1983 or voluntarily admitted but subsequently detained under these sections within 7 days of admission were included. Section 4 allows emergency detention of a patient for up to 72 h, Section 2 allows involuntary admission for assessment for up to 28 days and Section 3 involuntary admission and treatment for up to 6 months.
Eligible patients were identified through Mental Health Act administrators or staff in the wards between July 2003 and July 2005. On receipt of information on new admissions, researchers asked the ward staff for consent to contact patients. The researchers then approached the eligible patients and invited them to participate in the study. A range of questionnaires were subsequently administered to those who gave written informed consent to participate. The follow-up interviews were usually completed either in the hospital or in the interviewees' home, and rarely, over the telephone (between 2% and 8%).
Procedures and measures
The study design as presented above was approved by the multicentre research ethics committee. The acquisition of data for those who did not take part in the interviews was approved by the Patient Information Advisory Group.
Data collected for the whole sample included: age, gender, ethnicity (census categories), diagnosis (ICD–10), 15 legal status and length of index admission and readmissions (involuntary or otherwise) from medical records in each hospital.
For those who gave informed consent to be interviewed, the following extra data were collected within the first week after admission: past use of services; perceived coercion rated by patients at admission on the MacArthur Perceived Coercion Scale; Reference Gardner, Hoge, Bennet, Roth, Lidz and Monahan16 perceived risk to self and others rated by patients before admission on one closed question each (score 0=no, 1=yes); and patients' satisfaction with treatment on the Client's Assessment of Treatment Scale, Reference Priebe, Gruyters, Heinze, Hoffmann and Jakel17 which consists of 7 items on different aspects of hospital treatment (general assessment, psychiatrist, other staff, medication, other treatment components, personal respect, perceived help, each rated on a scale from 0 to 10 with 10 being the most positive response; mean score used) and has been widely used to assess patients' views of in-patient care. Reference Kallert, Priebe, McCabe, Kiejna, Rymaszewska and Nawka18,Reference Priebe, Jones, McCabe, Briscoe, Wright and Sleed19 The Cronbach's alpha for a total score on this scale was 0.90. Functioning on the Global Assessment of Functioning 20 (GAF; ranging 0–100 with 100 being the most positive score) and symptom levels on the 24-item version of the Brief Psychiatric Rating Scale Reference Lukoff, Nuechterlien and Ventura21 (with 168 being the highest symptom level) were assessed by researchers, whereas the other instruments were self-rated. Documented reasons for the index involuntary admission were obtained from medical records.
At follow-up interviewed patients were asked whether they thought their involuntary admission (or their subsequent detention within 7 days after admission for those admitted voluntarily) was justified. This was rated on a Likert-type scale ranging from 0 (‘entirely wrong’) to 10 (‘entirely right’). The ratings were later dichotomised as less than or equal to, or greater than the neutral middle point of 5, so that patients were classified into those with neutral/negative views and those with positive views. Although we established readmissions in the whole sample, retrospective justification of involuntary admission rates could only be assessed in those patients who were interviewed at follow-up. All researchers on the study were trained in the assessments and achieved an interrater reliability of Cohen's kappa=0.90 on the Brief Psychiatric Rating Scale.
Statistical analysis
Patients interviewed and not interviewed at baseline and, out of those interviewed at baseline, patients re-interviewed and not re-interviewed at 1 year, were compared on socio-demographic characteristics, diagnostic group, legal status of admission and length of index hospitalisation. Overall rates of involuntary readmissions and proportions of those who felt their original admission to be justified were estimated. Explanatory variables for these outcomes were investigated using multivariable regression models.
The dichotomised variable reflecting perceived justification was analysed using logistic regression, and involuntary readmission using Poisson regression, first with data for the total sample and second including additional variables from interviews. Time at risk for readmission was computed as total follow-up time minus time in hospital; in 45 cases this was missing and was replaced by the mean time at risk for the rest of the sample. Three patients were still in hospital after a year and were excluded from the analysis of readmissions.
Age, gender and ethnic group were included for both models. Other baseline variables that were individually significant at P=0.1 were then considered. Variables that became non-significant at P=0.05 in the multivariable model were excluded one by one and the model refitted. The final models were refitted as sensitivity analyses (a) including the provider organisations (i.e. NHS trusts) as random effects, (b) replacing any missing covariates by the centre mean (continuous variables) or centre mode (categorical variables) and (c) reconsidering excluded variables at each stage (first, socio-demographics; second, self-reported evaluation of admission, treatment and perceived risk; third, clinical status data). Stata version 9 for Windows was used for the analysis (commands logistic, xtlogit, poisson, xtpoisson).
Results
Description of the sample
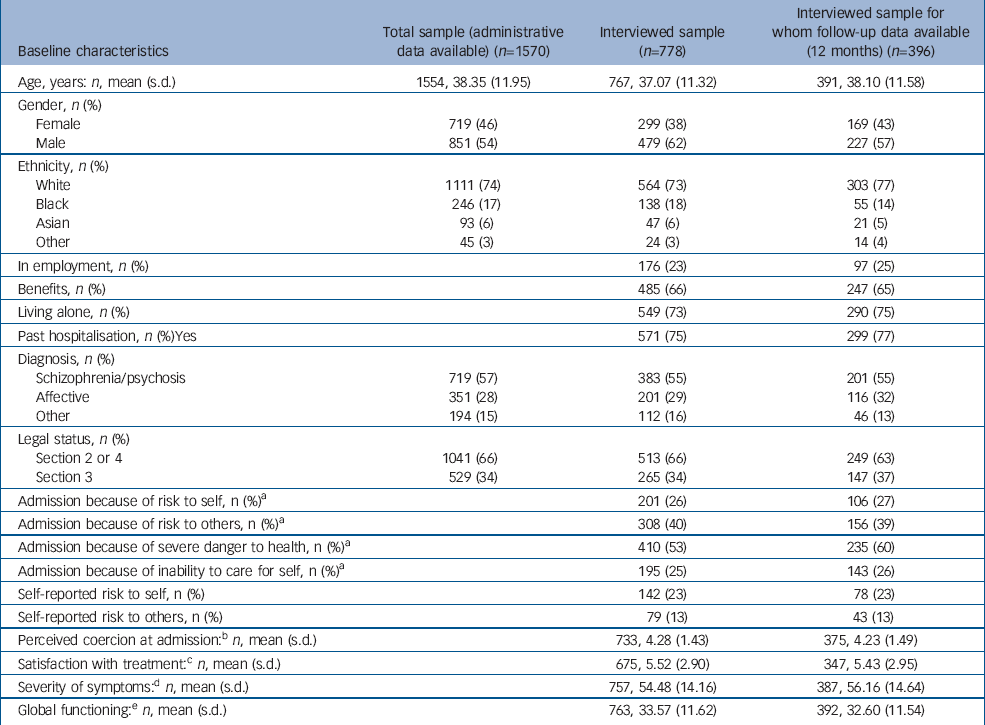
During the recruitment period, 1570 eligible patients were identified. Of these, 167 (11%) were initially admitted voluntarily and then detained within the first week. Out of the total sample, 778 (50%) consented to be interviewed at baseline. Of these, 396 (51%) were re-interviewed at 1 year. Table 1 shows the baseline characteristics for the total sample and for the samples that were interviewed at baseline and at 1 year.
Table 1 Baseline characteristics for samples recruited, interviewed and analysed
| Baseline characteristics | Total sample (administrative data available) (n=1570) | Interviewed sample (n=778) | Interviewed sample for whom follow-up data available (12 months) (n=396) |
|---|---|---|---|
| Age, years: n, mean (s.d.) | 1554, 38.35 (11.95) | 767, 37.07 (11.32) | 391, 38.10 (11.58) |
| Gender, n (%) | |||
| Female | 719 (46) | 299 (38) | 169 (43) |
| Male | 851 (54) | 479 (62) | 227 (57) |
| Ethnicity, n (%) | |||
| White | 1111 (74) | 564 (73) | 303 (77) |
| Black | 246 (17) | 138 (18) | 55 (14) |
| Asian | 93 (6) | 47 (6) | 21 (5) |
| Other | 45 (3) | 24 (3) | 14 (4) |
| In employment, n (%) | 176 (23) | 97 (25) | |
| Benefits, n (%) | 485 (66) | 247 (65) | |
| Living alone, n (%) | 549 (73) | 290 (75) | |
| Past hospitalisation, n (%)Yes | 571 (75) | 299 (77) | |
| Diagnosis, n (%) | |||
| Schizophrenia/psychosis | 719 (57) | 383 (55) | 201 (55) |
| Affective | 351 (28) | 201 (29) | 116 (32) |
| Other | 194 (15) | 112 (16) | 46 (13) |
| Legal status, n (%) | |||
| Section 2 or 4 | 1041 (66) | 513 (66) | 249 (63) |
| Section 3 | 529 (34) | 265 (34) | 147 (37) |
| Admission because of risk to self, n (%)a | 201 (26) | 106 (27) | |
| Admission because of risk to others, n (%)a | 308 (40) | 156 (39) | |
| Admission because of severe danger to health, n (%)a | 410 (53) | 235 (60) | |
| Admission because of inability to care for self, n (%)a | 195 (25) | 143 (26) | |
| Self-reported risk to self, n (%) | 142 (23) | 78 (23) | |
| Self-reported risk to others, n (%) | 79 (13) | 43 (13) | |
| Perceived coercion at admission:b n, mean (s.d.) | 733, 4.28 (1.43) | 375, 4.23 (1.49) | |
| Satisfaction with treatment:c n, mean (s.d.) | 675, 5.52 (2.90) | 347, 5.43 (2.95) | |
| Severity of symptoms:d n, mean (s.d.) | 757, 54.48 (14.16) | 387, 56.16 (14.64) | |
| Global functioning:e n, mean (s.d.) | 763, 33.57 (11.62) | 392, 32.60 (11.54) |
The patients interviewed at baseline were younger (37.0 years v. 39.5 years, P<0.001) and more likely to be male (62% v. 47%, P<0.001) than those who were not interviewed. There were no other significant differences between these two groups.
Some significant differences were found between those who were interviewed at 1 year and those who dropped out between baseline and follow-up. Those re-interviewed at 1 year were older (mean 38.1 years v. 35.9 years, P=0.01) and more likely to be female (43% v. 34%, P=0.013) and White (77% v. 69%, P=0.028) than the patients not re-interviewed. There were no other significant differences.
The reasons for non-participation or dropping out of interviews at 1-year follow-up are shown in Fig. 1.

Fig. 1 Recruitment and follow-up flowchart.
Outcomes of involuntary admission
Within the 1-year follow-up period after the index episode 234 patients (15% of the total sample) were involuntarily readmitted. The average time at risk was 286 days (total 1230 person-years) and the rate per person-year was 0.190 (95% CI 0.166–0.216). An additional 169 patients (11%) were admitted voluntarily within the same period. Of the re-interviewed sample, 40% felt that their index admission was justified at 1 year.
Patients who were voluntary at admission, and subsequently detained, had very similar outcomes to patients who were involuntary at admission (42% v. 40% justified their involuntary admission and/or detention, P=0.702; 16% v. 15% were involuntarily readmitted within 1 year, P=0.799). Consequently, the analysis of factors associated with outcome was conducted for the total sample, including those who were detained within the first week of admission.
Factors associated with involuntary readmissions in the follow-up period
The only factor that was significantly associated with involuntary readmissions in the total sample was ethnic group. Patients of Black African or Black African–Caribbean origin were more likely to be involuntarily readmitted within a year after the index admission than their White counterparts. The rates of involuntary readmission were 0.184, 0.251 and 0.181 per person-year for White, Black and Asian patients respectively, with a rate ratio (RR) of 1.37 (95% CI 0.99–1.89, P=0.051) comparing Black patients with White patients.
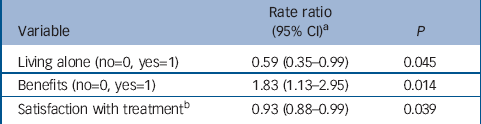
Univariate associations among the interviewed sample that were significant at P=0.1 (adjusted for age, gender and ethnic group) were for being in receipt of welfare benefits (RR=2.07, 95% CI 1.32–3.26), living alone (RR=0.58, 95% CI 0.36–0.93), past hospitalisation (RR=0.53, 95% CI 0.32–0.87), perceived coercion (RR=1.16, 95% CI 0.98–1.36) and satisfaction with treatment (RR=0.94, 95% CI 0.88–0.99). In the multivariable model (Table 2) patients receiving welfare benefits, those less satisfied with their treatment at baseline and those living with others were more likely to be readmitted involuntarily.
Table 2 Multivariable associations with rates of involuntary readmission within the 1-year follow-up period (n=624)
| Variable | Rate ratio (95% CI)a | P |
|---|---|---|
| Living alone (no=0, yes=1) | 0.59 (0.35-0.99) | 0.045 |
| Benefits (no=0, yes=1) | 1.83 (1.13-2.95) | 0.014 |
| Satisfaction with treatmentb | 0.93 (0.88-0.99) | 0.039 |
Factors associated with perceived justification of involuntary admission
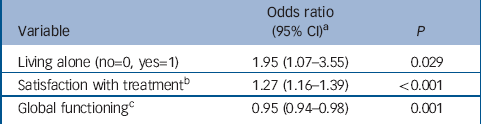
In univariate analyses, the following variables were associated with patients' perceived justification of the index admission (or the subsequent detention within 7 days after admission) at a significance level of P=0.1: living alone (OR=1.62, 95% CI 0.97–2.72), legal status (Sections 2 or 4 v. 3; OR=1.79, 95% CI 1.14–2.82), self-reported risk to self (OR=1.72. 95% CI 1.00–2.96), self-reported risk to others (OR=3.15, 95% CI 1.57–6.32), perceived coercion (OR=0.87, 95% CI 0.75–1.00), satisfaction with treatment (OR=1.24, 95% CI 1.14–1.35), and global functioning (OR=0.97, 95% CI 0.95–0.99). In the multivariable model (Table 3) living alone, initial treatment satisfaction and global functioning remained significant. Those with higher levels of functioning were less likely to view their involuntary admission as justified, whereas those who were living alone or more satisfied with treatment were more likely to consider it justified.
Table 3 Multivariable associations with perceived justification of involuntary admission (n=323)
| Variable | Odds ratio (95% CI)a | P |
|---|---|---|
| Living alone (no=0, yes=1) | 1.95 (1.07-3.55) | 0.029 |
| Satisfaction with treatmentb | 1.27 (1.16-1.39) | <0.001 |
| Global functioningc | 0.95 (0.94-0.98) | 0.001 |
The results of the sensitivity analyses did not alter the conclusions. They are available from the authors on request.
Discussion
Main findings
The most striking finding of this large national study of involuntary admissions is that initial satisfaction with treatment is associated with both objective and patient-rated outcomes 1 year after the index admission. Patients who express a lower satisfaction with hospital care within the first week of involuntary admission are more likely to be involuntarily readmitted within 1 year. They also are less likely to feel that the index admission was justified. Although initial patient views were associated with outcome, conventional clinical variables such as diagnostic group and symptom levels were not.
Patients on benefits, an indicator of poor socio-economic status, and those living with other people have higher involuntary readmission rates. A similar trend was observed in the total sample for patients from an African or African–Caribbean background. The latter adds to existing extensive evidence that African–Caribbean patients are more likely to be involuntarily admitted in England. Reference Singh and Burns22–Reference Bhui, Stansfeld, Hull, Priebe, Mole and Feder25
Poor global functioning at the time of the admission was associated with a more positive assessment of the involuntary admission later. Remembering a severe impact of the acute illness on functioning might foster the view that the admission was justified. Living alone is linked with lower involuntary readmission rates and a more positive retrospective judgement of the index admission. Living with other people may make relapses more likely to be noticed and lead to more conflicts at the time of relapses. At the same time, people living alone are more likely to consider their original admission justified, possibly because they particularly value the company and social support during and after hospital care and, subsequently, have a more positive view of that experience.
Strengths and limitations
This is the largest national prospective study of involuntary hospitalisation to date, and all admission and treatment procedures were regulated by the same jurisdiction. Socio-demographic baseline variables and objective outcome at 1 year were collected on all eligible consecutive patients. Half the patients were interviewed to provide more detailed information, including patient ratings of care and coercion, which reaches the quality standard for these types of studies. Reference Katsakou and Priebe4 Of those interviewed at baseline, more than 50% were re-interviewed at 1 year, which is a high proportion in this often uncooperative and highly mobile group of patients. Reference Priebe, Jones, McCabe, Briscoe, Wright and Sleed19 A further strength is that we brought together socio-demographic, clinical, administrative and patient-rated factors in the same study.
A limitation of the study is that we found a few differences between patients interviewed and not interviewed at baseline, and between patients followed up and not followed up. Although these differences were controlled for in the analysis, there could have been other unmeasured sources of bias. As this is an observational study no conclusions can be drawn on the causality of associations.
Implications
Only 40% of patients felt in retrospect that their original involuntary admission was justified, and this percentage might have been even smaller if all patients had been re-interviewed. Most previous studies found higher percentages. Reference Katsakou and Priebe4 The findings are, however, difficult to compare since previous studies had different response rates and used shorter follow-up periods. Improving the percentage of patients stating that the admission was justified might be a sensible aim for both policy and clinical practice.
The association of being on welfare benefits with higher readmission rates may underline the importance of social inclusion programmes that help patients with mental disorders to discontinue benefits and enter employment. Such programmes should include patients with severe mental illness who experienced involuntary hospital admission. Social inclusion programmes are often proposed because of their benefits to patients' quality of life. If successful, they may have broader benefits in reducing such adverse consequences as involuntary readmissions. Yet, many of the patients in this study were severely disabled and unlikely to achieve regular employment through rehabilitation, job coaching or other inclusion programmes.
Initial patient ratings of treatment have been found to predict outcome of antipsychotic medication, Reference Van Putten, May, Marder and Wittmann26,Reference Van Putten, May and Marder27 psychotherapy, Reference Horvarth and Symonds28,Reference Luborsky, McLellan, Woody, O'Brien and Auerbach29 and voluntary day-hospital Reference Priebe and Gruyters30 and in-patient care. Reference Bröker, Röhricht and Priebe31 Our study shows that it also applies to involuntary admissions. What patients think about their care within the first week is an important prognostic indicator in the long term, i.e. at 1 year. It should be considered even when symptom levels are often still high and when many patients hold particularly negative views. In fact, involuntarily admitted patients in this study expressed a much less favourable view of treatment in the first week than has been found for voluntary patients. Reference Kallert, Priebe, McCabe, Kiejna, Rymaszewska and Nawka18,Reference Priebe, Jones, McCabe, Briscoe, Wright and Sleed19,Reference Bröker, Röhricht and Priebe31 It is understandable in the context of a compulsory admission that clinicians might think that immediate patient satisfaction is not that relevant. However, our data suggest that attention paid to this goes beyond simple humanity and may have important implications for the subsequent course of treatment and use of scarce resources.
Clinical practice may focus on better procedures and communication beginning immediately after admission to improve both patients' initial satisfaction with care and long-term outcomes. There is, however, only limited evidence on what specific procedures and interventions may help patients develop a more positive view of a hospital treatment which was compulsorily imposed on them. Observational studies suggest that procedural fairness, comprehensive information, respect, empathy and involving patients in treatment decisions are associated with a more positive view of treatment. Reference Monahan, Hoge, Lidz, Roth, Bennett and Gardner32 Experimental studies have been conducted with day-hospital and hospital patients, and provide some evidence that engaging patients in treatment planning and accommodating their preferences in treatment decisions can improve treatment satisfaction. Reference Priebe and Gruyters33,Reference Sorgaard34 Nevertheless, involving involuntary patients in treatment decisions may be particularly challenging and require structured, flexible and skilful therapeutic input.
Conclusions
Clinicians should proactively elicit patients' views about hospital treatment at an early stage and take the answers seriously. Future research should explore the processes behind patients' initial views of treatment and consider these views as an important early outcome in modelling and testing new interventions.
Acknowledgements
This study was funded by a grant from the Policy Research Programme of the Department of Health, UK (Commission no. 0230072). This work was undertaken and coordinated by the Unit for Social and Community Psychiatry, Barts and the London School of Medicine and Dentistry, Queen Mary University of London, who received funding from the Department of Health. The views expressed in the publication are those of the authors and not necessarily those of the Department of Health. This study was supported by the NIHR UK Mental Health Research Network. We are grateful to all interviewed patients and staff of participating trusts. We also thank Olive Bennewith, Louisa Bolt, Simon Clarke, Susan Collinson, Suzi Curtis, Rosemary Davies, Rebekka Evans, Sarah Grant, Dannielle Oliver, Felicitas Rost, Rebecca Read, Rajinder Sidhu, Emma Williams and Jessica Zetteler for their contribution to the study.







eLetters
No eLetters have been published for this article.