Deliberate self-harm is a major public health problem. It is estimated that 140 000 cases presented to accident and emergency departments in England and Wales in 1996 (Reference Hawton, Fagg and SimkinsHawton et al, 1997). In the South-West of England it is the third most frequent cause of admission to a general medical bed after myocardial infarction and congestive cardiac failure (Reference Gunnell, Brooks and PetersGunnell et al, 1996). The incidence in the general population is likely to be greater because many do not seek medical attention following deliberate self-harm (Reference Patton Harris, Carlin and HibbertPatton Harris et al, 1997). Deliberate self-harm is a high risk factor for future suicide because individuals who have deliberately self-harmed have a 100-fold increased risk of suicide compared to the general population (Reference Hawton and FaggHawton & Fagg, 1988). Some 1% of those who deliberately self-harm will die by suicide within 1 year of an attempt (Reference Hawton and FaggHawton & Fagg, 1988) and this may be as high as 10% at longer follow-up (Reference Nordentoft, Breum and MunckNordentoft et al, 1993). The population attributable fraction for deliberate self-harm has been calculated at between 6% and 20% and it has been estimated that reducing suicide rates in this high risk group by 25% would reduce overall suicide rates by up to 5.8% (Reference Lewis, Hawton and JonesLewis et al, 1997). Services for deliberate self-harm therefore have an important role in suicide prevention. A reduction in the suicide rate was made a priority in the Health of the Nation document (Department of Health, 1992) and remains so for Our Healthier Nation (Department of Health, 1998).
It is proposed that national standards for service provision within the NHS will be implemented through the National Service Framework for Mental Health (Department of Health, 1999) and the National Institute for Clinical Excellence (Department of Health, 1997). Guidelines on the health service management of deliberate self-harm were published by the Department of Health and Social Security in 1984 and a national survey in the late 1980s suggested these guidelines were being largely ignored (Reference Butterworth and O'GradyButterworth & O'Grady, 1989). In 1994 the Royal College of Psychiatrists produced a more detailed consensus statement on standards of service provision for the general hospital management of adult deliberate self-harm (Royal College of Psychiatrists, 1994). The aim of this study was to find out if services for those admitted to an in-patient bed following deliberate self-harm of any sort have improved, and to compare existing services with those recommended in the consensus statement. Those discharged directly from the accident and emergency department were not included.
Overview of existing guidelines
The Department of Health and Social Security (1984) guideline key points were that:
-
(a) everyone presenting following deliberate self-harm should have a psycho-social assessment;
-
(b) each hospital should have a clearly laid down policy for dealing with deliberate self-harm;
-
(c) there is a need for adequate training of all staff undertaking assessments;
-
(d) All hospitals should have one or two wards to which the majority of deliberate self-harm cases are admitted, and these wards should have nursing staff with psychiatric experience.
The Royal College of Psychiatrists (1994) consensus statement extends the recommendations outlined in the Department of Health and Social Security guidelines by including the following recommendations:
-
(a) Service provision. A deliberate self-harm team is desirable for each hospital. Staff should have scheduled time to undertake assessments, which should be carried out within 24 hours of referral, in a private room. It should be clear whether responsibility for discharge lies with the specialist psychiatric team or the general hospital team. Likewise it should be clear who communicates with the general practitioners. Follow-up, if needed, should normally occur within 7 days.
-
(b) Training. A senior psychiatrist should be responsible for staff training. All those new to assessments following deliberate self-harm should undertake at least five observed assessments and should receive detailed supervision in every case for the first 6 months. Junior psychiatrists should have a brief discussion for each case.
-
(c) Planning. Each hospital should have a self-harm planning group to oversee the service provided, including the adequate training of staff.
The study
A questionnaire was designed to measure whether each of the service standards given in the Royal College of Psychiatrists consensus statement (1994) were being met and included data on the number of referrals seen. Trusts in England were identified from a list obtained from the Department of Health. Of the 402 trusts, 51 were excluded because they obviously did not provide secondary mental health services (e.g. ambulance trusts). The remaining 351 trusts were then contacted by telephone in order to determine whether or not they provided secondary mental health services and if so, to identify the clinical director of psychiatry.
After piloting, a postal questionnaire was sent and those not responding after 6 weeks were sent a repeat questionnaire.
Findings
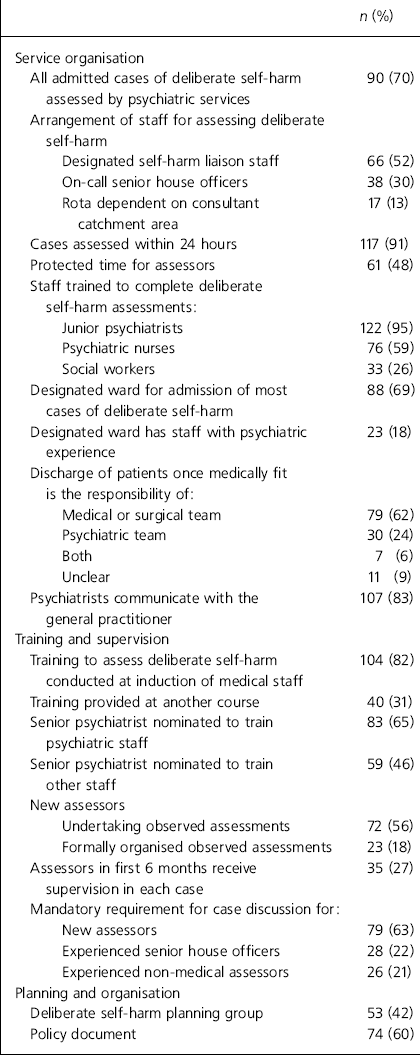
Questionnaires were distributed to 208 trusts. Nine replies were returned from trusts that did not have a general deliberate self-harm service. Of the remaining 197 trusts 129 replied, giving a response rate of 65%. The main results are given in Table 1.
Table 1. Main results from postal questionnaire responses
| n(%) | |
|---|---|
| Service organisation | |
| All admitted cases of deliberate self-harm assessed by psychiatric services | 90 (70) |
| Arrangement of staff for assessing deliberate self-harm | |
| Designated self-harm liaison staff | 66 (52) |
| On-call senior house officers | 38 (30) |
| Rota dependent on consultant catchment area | 17 (13) |
| Cases assessed within 24 hours | 117 (91) |
| Protected time for assessors | 61 (48) |
| Staff trained to complete deliberate self-harm assessments: | |
| Junior psychiatrists | 122 (95) |
| Psychiatric nurses | 76 (59) |
| Social workers | 33 (26) |
| Designated ward for admission of most cases of deliberate self-harm | 88 (69) |
| Designated ward has staff with psychiatric experience | 23 (18) |
| Discharge of patients once medically fit is the responsibility of: | |
| Medical or surgical team | 79 (62) |
| Psychiatric team | 30 (24) |
| Both | 7 (6) |
| Unclear | 11 (9) |
| Psychiatrists communicate with the general practitioner | 107 (83) |
| Training and supervision | |
| Training to assess deliberate self-harm conducted at induction of medical staff | 104 (82) |
| Training provided at another course | 40 (31) |
| Senior psychiatrist nominated to train psychiatric staff | 83 (65) |
| Senior psychiatrist nominated to train other staff | 59 (46) |
| New assessors | |
| Undertaking observed assessments | 72 (56) |
| Formally organised observed assessments | 23 (18) |
| Assessors in first 6 months receive supervision in each case | 35 (27) |
| Mandatory requirement for case discussion for: | |
| New assessors | 79 (63) |
| Experienced senior house officers | 28 (22) |
| Experienced non-medical assessors | 26 (21) |
| Planning and organisation | |
| Deliberate self-harm planning group | 53 (42) |
| Policy document | 74 (60) |
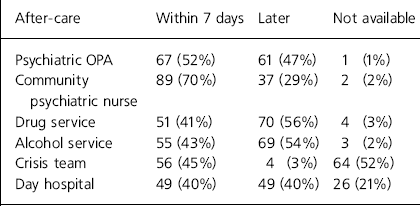
The after-care that was considered to be routinely available within the trust for those who require it following deliberate self-harm varied widely between trusts. An appointment with a community psychiatric nurse was the most common service to be available within 7 days (Table 2).
Table 2. Services available following psycho-social assessment after deliberate self-harm
| After-care | Within 7 days | Later | Not available |
|---|---|---|---|
| Psychiatric OPA | 67 (52%) | 61 (47%) | 1 (1%) |
| Community psychiatric nurse | 89 (70%) | 37 (29%) | 2 (2%) |
| Drug service | 51 (41%) | 70 (56%) | 4 (3%) |
| Alcohol service | 55 (43%) | 69 (54%) | 3 (2%) |
| Crisis team | 56 (45%) | 4 (3%) | 64 (52%) |
| Day hospital | 49 (40%) | 49 (40%) | 26 (21%) |
Discussion
The study achieved its aim of comparing actual services with the standards set out in the consensus statement of the Royal College of Psychiatrists (1994). No data were available from trusts that did not respond, therefore, some caution is needed in generalising from the 65% responding to this questionnaire. However, we have no reason to believe that service provision would be any better from those trusts not responding to the questionnaire. The results show that generally the current provision of deliberate self-harm service training and planning falls substantially below those suggested in both the Department of Health and Social Security (1984) guidelines and the Royal College of Psychiatrists consensus statement (1994).
The principle that each hospital should have a ‘clearly laid down policy’ for the service, provided to those presenting following deliberate self-harm, was stated in the Department of Health and Social Security document over 15 years ago. This study has shown that 40% of trusts do not appear to have such a policy document. The ‘most fundamental recommendation’ of the Royal College of Psychiatrists consensus statement was the need for a deliberate self-harm services planning group. The tasks of such a planning group include establishing policy in cases where non-psychiatric or non-medical staff may undertake assessments and to ensure adequate training of all staff. The group should also decide whether the psychiatric or medical team are responsible for both discharge and contact with the general practitioner. Only 42% of trusts have a self-harm planning group, although it is unclear from this study whether these responsibilities are undertaken by other groups. However, it is reasonable to suppose, given the absence of a policy document or a planning group in at least 40% of cases, that standards of planning fall significantly below those recommended.
Although the minority of individuals admitted following deliberate self-harm have a serious mental illness (Reference Urwin and GibbonsUrwin & Gibbons, 1979), it is concerning that 30% of trusts do not routinely refer all cases for a specialist psycho-social assessment. An important issue for trusts to address is that few wards that regularly admit patients following deliberate self-harm employ staff with psychiatric experience. In 31% of trusts that do not have a designated ward for the admission of these patients, such developments are unlikely.
Recommendations for the training of junior psychiatrists in deliberate self-harm assessment are outlined in detail. The results of a previous smaller study (Reference TaylorTaylor, 1998) suggest that training and supervision fall well below recommended standards.
The guidelines were derived by expert consensus, and are not evidence-based. Furthermore, there is little evidence for the efficacy of any intervention in deliberate self-harm (Reference Hawton, Arensman and TownsendHawton et al, 1998), although, so far, trials have been of inadequate size to detect clinically important effects. Hence, there is an urgent need for further trials of promising interventions, such as emergency card provision or problem solving therapy (Reference Hawton, Arensman and TownsendHawton et al, 1998). In the absence of proven effective interventions, the consensus statement provides the best available guidance on service provision, planning and training. Meeting these standards would provide a sound basis for further service development, if effective interventions are found.
Given the enormous gap between national recommendations and current service provision it may be wise to set modest but achievable goals, in the review of the Royal College of Psychiatrists consensus statement due this year and in standards for a deliberate self-harm service that may be set by the National Service Framework.





eLetters
No eLetters have been published for this article.