Electroconvulsive therapy (ECT) is one of the most empirically-based interventions but is, nevertheless, one of the most controversial in the public domain (Reference FinkFink, 2001). A recent ECT audit in England and Wales noticed an improvement in ECT practice (Reference Duffett and LelliottDuffett & Lelliott, 1998). However, two-thirds of ECT clinics still fell short of the most recent College standards and the report raised a concern whether an accreditation system of ECT clinics and practitioners might be needed. We conducted a territory-wide survey on the practice and utilisation of ECT in Hong Kong and report our major findings here.
Method
The study was conducted between October 1999 and August 2000, during which eight of 13 public in-patient psychiatric units in Hong Kong had ECT treatment facilities. The ECT consultants of all eight units consented to the study. There were no public out-patient clinics or day hospitals providing ECT. Letters inviting participation in the study were also sent to all private psychiatrists. Thirty-two of the 35 private psychiatrists replied (91%), of whom four reported that they had performed ECT in the last 3 years, and all agreed to participate. The survey had two components; a postal questionnaire and a site visit. The questionnaire primarily consisted of multiple-choice questions and covered all major areas of ECT practice and policy. The authors (K.F.C. and Y.K.N.) visited all public ECT units to observe the ECT facilities and treatment, to interview psychiatric, anaesthetic and nursing staff who attended ECT treatment on the day of visit and to inspect ECT records. Administration of ECT was infrequent in the private clinics and visits were not arranged. We compared the standards of ECT practice in Hong Kong against checklists for good practice in ECT (Royal College of Psychiatrists, 1995). The rate of ECT use was tabulated as the number of ECT courses per year and per 10 000 population.
Results
Table 1 presents the territory-wide compliance rates of the ECT practice areas compared with College guidelines.
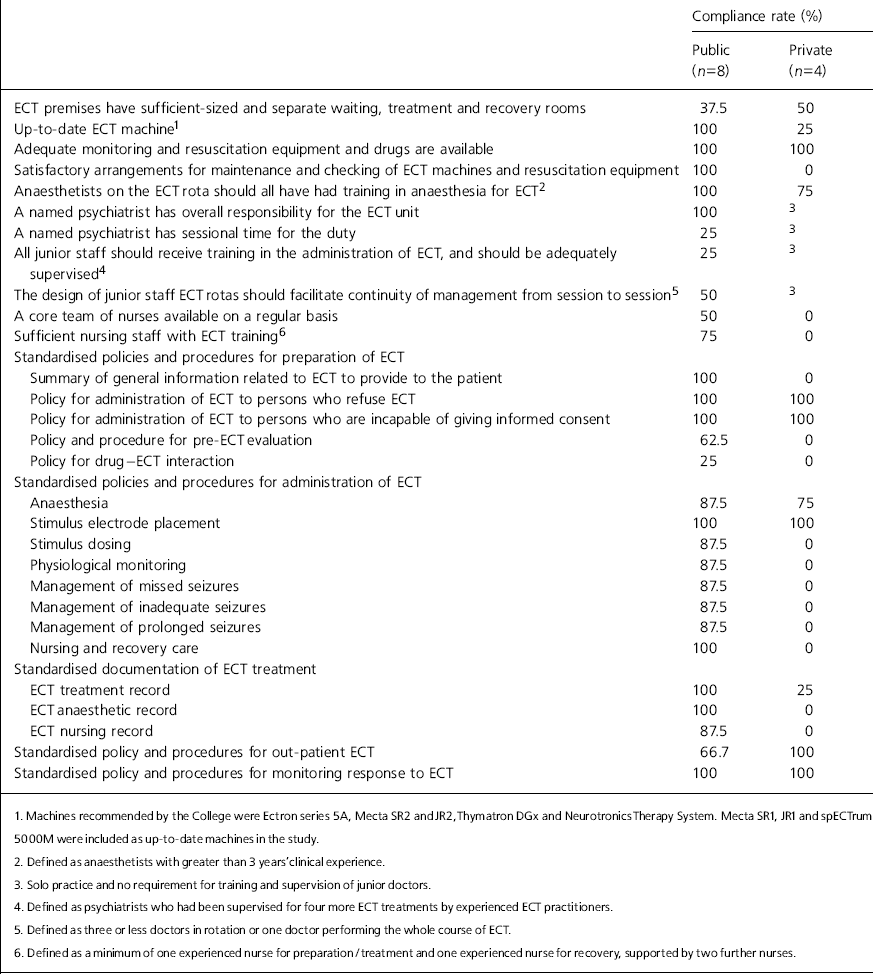
Table 1. Compliance rates of ECT practice in Hong Kong against checklists for good practice in ECT (Royal College of Psychiatrists, 1995)
| Compliance rate (%) | ||
|---|---|---|
| Public (n=8) | Private (n=4) | |
| ECT premises have sufficient-sized and separate waiting, treatment and recovery rooms | 37.5 | 50 |
| Up-to-date ECT machine1 | 100 | 25 |
| Adequate monitoring and resuscitation equipment and drugs are available | 100 | 100 |
| Satisfactory arrangements for maintenance and checking of ECT machines and resuscitation equipment | 100 | 0 |
| Anaesthetists on the ECT rota should all have had training in anaesthesia for ECT2 | 100 | 75 |
| A named psychiatrist has overall responsibility for the ECT unit | 100 | 3 |
| A named psychiatrist has sessional time for the duty | 25 | 3 |
| All junior staff should receive training in the administration of ECT, and should be adequately supervised4 | 25 | 3 |
| The design of junior staff ECT rotas should facilitate continuity of management from session to session5 | 50 | 3 |
| A core team of nurses available on a regular basis | 50 | 0 |
| Sufficient nursing staff with ECT training6 | 75 | 0 |
| Standardised policies and procedures for preparation of ECT | ||
| Summary of general information related to ECT to provide to the patient | 100 | 0 |
| Policy for administration of ECT to persons who refuse ECT | 100 | 100 |
| Policy for administration of ECT to persons who are incapable of giving informed consent | 100 | 100 |
| Policy and procedure for pre-ECT evaluation | 62.5 | 0 |
| Policy for drug—ECT interaction | 25 | 0 |
| Standardised policies and procedures for administration of ECT | ||
| Anaesthesia | 87.5 | 75 |
| Stimulus electrode placement | 100 | 100 |
| Stimulus dosing | 87.5 | 0 |
| Physiological monitoring | 87.5 | 0 |
| Management of missed seizures | 87.5 | 0 |
| Management of inadequate seizures | 87.5 | 0 |
| Management of prolonged seizures | 87.5 | 0 |
| Nursing and recovery care | 100 | 0 |
| Standardised documentation of ECT treatment | ||
| ECT treatment record | 100 | 25 |
| ECT anaesthetic record | 100 | 0 |
| ECT nursing record | 87.5 | 0 |
| Standardised policy and procedures for out-patient ECT | 66.7 | 100 |
| Standardised policy and procedures for monitoring response to ECT | 100 | 100 |
ECT premises, ECT machines and other equipment
Only three of the eight ECT premises in public hospitals met College guidelines. Treatment and recovery rooms at four units were separated only by wooden or plastic partitions and one unit did not have a waiting area. ECT in the private sector was mostly carried out in a single or shared room in hospital or in a room in a clinic. All eight public units had installed up-to-date ECT equipment. Seven units were using a Mecta US domestic version SR1 and one had recently installed a Mecta spECTrum 5000M. However, three of the four private ECT practitioners were still using Ectron Mark 4 models. For back-up, the public units had installed either Ectron series 5 or Mecta SR1 machines. No back-up machine was available in the private sector. ECT machines and resuscitation equipment in the public sector were serviced every 3 to 12 months by qualified personnel, whereas in the private sector the machines were not regularly checked.
Supervision and training of psychiatric personnel
At all centres, junior doctors were given an informal briefing on ECT and had at least one supervised ECT administration before giving treatment on their own. The average number of supervised patient treatments was four (range=1-15). Doctors at four of the eight public ECT units performed blocks of treatment sessions and their periods on duty varied from 1 week to 3 months. The ECT sessions at the remaining four public units were attended by three to 20 doctors in rotation. All the private ECT practitioners were experienced psychiatrists. However, they performed treatments infrequently and their last ECT administrations were from one to 20 months prior to the survey. The audit team observed that the training at only two centres had covered the back-up ECT machine.
Administration, documentation and response monitoring of ECT
The most commonly used anaesthetic agents and muscle relaxants in Hong Kong were thiopentone and suxamethonium, respectively. In addition, bilateral electrode placement was usually performed. The pre-selected dosage method was the most commonly used dosing procedure among the public ECT units (63%). The remaining three hospitals employed the dose titration method. In the private sector, there was no standardisation of ECT stimulus dosing policy. Most of the public units (88%) monitored both electroencephalographic and motor seizure duration. Only two of the eight hospitals used the Hamilton cuff technique. In the private sector, two of the four ECT practitioners did not measure seizure duration during treatments. Most of the public units (88%) had standardised records, but no standardised documentation was used in the private sector. Only one private practitioner had recorded seizure duration during ECT treatment. All public ECT units required doctors to assess their patients every one or two treatments, but only one unit had a procedure in place to enforce this practice. Private ECT practitioners usually assessed their patients before each treatment.
Observed treatment sessions
In most units, patient preparation and delivery of treatment was consistent with College recommendations. On one occasion, we observed the use of the ‘impedance override’ on the Mecta SR1 after repeated checking of cable connections and electrode contact because of a ‘self-test’ failure. Seizure was not produced in the session. On the same occasion, the back-up ECT machine was found not to be ready for use. Another important observation during hospital visits was that, although hospital policy required patients to be assessed every one to two treatments during a course of ECT, the policy was only practised in four of the nine patients we observed. The last written entry of clinical information for one patient was 8 days before the session we observed.
Utilisation
The eight public units completed 221 courses of ECT in the calendar year of 1998. The use of ECT varied widely between the units. Three units (37%) performed less than 20 courses of ECT in the 12-month period and the number of ECT courses per 100 acute hospital beds ranged from 0 to 83.8. Five courses of ECT were completed in the private sector in 1998. With a total population in Hong Kong of 6 645 600 by mid 1998 (Census & Statistics Department, 2001), the number of ECT courses per 10 000 population was 0.34.
Discussion
The survey provided an almost complete picture of ECT practice in Hong Kong. The response rate was 100% for the public ECT units and 91% among the private psychiatric service. We obtained our data by postal questionnaire and site visit. The latter was particularly important as it revealed the actual ECT practice. Our findings highlighted the importance of training and supervision in ECT administration. Previous ECT surveys rarely examined back-up ECT machines (Reference PippardPippard, 1992; Reference Duffett and LelliottDuffett & Lelliott, 1998). We suggest that back-up machines need to be included in ECT surveys and training on its use is necessary. We found that most of the public ECT services in Hong Kong had standardised policies but doctors might not strictly follow guidelines in administration and response monitoring of ECT. One public service in Hong Kong had adopted a policy that required mandatory recording of the patient's response to ECT every week before the treatment was continued and this helped the practical implementation of the guideline.
In previous studies, the estimated number of patients treated with ECT per year per 10 000 population varied from 0.8 to 4.9 (Reference Duffett, Siegert and LelliottDuffett et al, 1999; Reference Glen and ScottGlen & Scott, 1999; Reference Hermann, Dorwart and HooverHermann et al, 1995; Reference KramerKramer, 1999), which is higher than the annual rate of use in Kong Kong. ECT usage varied widely between the psychiatric units in Hong Kong and at some public ECT units and among the private practitioners, the usage was so small as to raise concerns about maintaining the service.
The study has several limitations. We only examined ECT practice in Hong Kong, and a study that covered ECT treatment in mainland China and other Asia-Pacific countries would be useful. Our analysis of ECT utilisation was based on a postal questionnaire, which did not examine usage in terms of the number of individual treatments per year. Factors that might influence the utilisation rate, such as age and gender of the patients, were also omitted. A replication study on ECT utilisation and factors that influence the rate of ECT use will contribute to the literature on ECT use worldwide.
We found that most practice areas in Hong Kong's public ECT services complied with College recommendations. Although the private ECT practitioners accounted for a very small proportion of ECT treatments in Hong Kong, their practice was not in line with the most recent ECT guidelines. The results of the study have been disseminated to the units involved so that they may consider ways of improving their services. A second audit cycle is planned in due course.




eLetters
No eLetters have been published for this article.