INTRODUCTION
Emergency department (ED) overcrowding is a significant problem affecting both children and adults and has been linked to adverse patient outcomes.Reference Hostetler, Mace and Brown 1 , Reference Timm, Ho and Luria 2 A conceptual model of ED overcrowding proposed by Asplin et al. identified three determinants of overcrowding: input factors, throughput factors, and output factors.Reference Asplin, Magid and Rhodes 3 Output constraints (e.g., boarding of admitted patients in the ED) are the major contributor to overcrowding of general EDs.Reference Asplin, Magid and Rhodes 3 , Reference Stang, McGillivray and Bhatt 4 In contrast, overcrowding in pediatric emergency departments (PEDs) has generally been attributed to input and throughput factors, with relatively less contribution of output constraints.Reference Asplin, Magid and Rhodes 3 Of particular importance is the idea of the reciprocal impact that return visits to the emergency department (RTED) and overcrowding may have on one another. The busiest time in the PED is in the evening, when peak patient volumes coincide with reduced access to health care providers in the community. Children initially seen during these times have a higher rate of return visits than those seen at other times.Reference Goldman, Ong and Macperson 5 Concurrently, as many as two-thirds of unscheduled return visits occur during these same busy hours, further increasing patient volume.Reference Alessandrini, Lavelle and Grenfell 6
An RTED is generally defined in the literature as an unscheduled ED visit for a similar or related complaint within 48 hours to 7 days of the index visit, and is a frequent occurrence.Reference Goldman, Ong and Macperson 5 - Reference Calder, Pozgay and Riff 15 Previous studies suggest that the rate of RTED within PEDs ranges from 2.7% to 8.1% in the United States, Canada, and the UK.Reference Goldman, Ong and Macperson 5 - Reference Goldman, Kapoor and Mehta 7 , Reference Ali, Place and Howell 9 - Reference Pham, Kirsch and Hill 16 The variable definition of what constitutes an RTED (within 2-7 days) likely accounts for this variability in rates of RTED. Although the majority (85%) of all ED visits by children occur in community EDs,Reference Hostetler, Mace and Brown 1 , Reference Cho, Shapiro and Cabana 11 most studies of pediatric RTED have been conducted in PEDs only, and those occurring in general EDs do not report pediatric outcomes separately. The few large studies examining multiple centres have either focused on multiple individual tertiary PEDs or do not specify the direction of RTED to and from the PED versus from the PED to a community ED.Reference O’Loughlin, Hacking and Simmons 10 - Reference Sung, Liu and Chen 18
The aim of this study is to measure the incidence and describe the directional pattern of RTED for children discharged from a major tertiary care PED to any ED (pediatric and general) in a large catchment area within 7 days of the index visit and to characterize operational measures (waiting time [WT] and length of stay [LOS]) as well as outcome measures (discharge disposition) for these subsequent visits. More accurately characterizing the regional RTED rate in this way will help better estimate the burden of RTED associated with the care at a PED.
METHODS
Design and study population
We conducted a retrospective cohort study of all patients less than 17 years of age who presented initially to British Columbia Children’s Hospital (BCCH) over a 1-year period from August 1, 2012, to August 8, 2013, using the PED administrative database. The 53rd week period was included to account for only any RTED that may have been triggered by the 52nd week included in our study period. BCCH is a tertiary children’s hospital in metropolitan Vancouver, is the only pediatric referral centre in British Columbia, and receives just over 40,000 visits per year, serving children up until their 17th birthday. We also reviewed data for pediatric visits from all 17 community/general EDs that see both children and adults in Vancouver Lower Mainland. Together, the 18 EDs included in the study provide care for a population of over 2.5 million people, or nearly 60% of the province. In addition to these 18 EDs, children in this area may also access medical care through walk-in urgent care clinics and family physicians, through the British Columbia universal health care coverage.
Linkage and database preparation
A data custodian merged pediatric visits from all study sites, taking care to identify the visit sites. Once merged, study subjects’ personal health numbers were replaced with a unique study number, allowing us to link multiple ED visits to any of the study sites by the same subject. We included only visits for which the chronologically earlier visit occurred at the study PED. We took this visit to be the incident or “index” visit. To be considered an RTED, linked ED visits had to fulfill the following criteria: 1) The time-lapse between visits was ≤7 days, and 2) the subsequent visit was for the same clinical condition as the index visit. To determine whether initial and RTED clinical conditions were related, we examined both their National Ambulatory Care Reporting System (NACRS)Reference Unger, Afilalo and Boivin 19 codes for chief complaint and discharge diagnosis. NACRS codes are the standard reporting codes for ED visits in Canada. Discharge diagnosis and chief complaint codes are presented with a letter and a number, where the letter represents a category of diseases and the number corresponds with a specific diagnosis or complaint. If the paired visits shared the same disease category, the visits were considered to be related, otherwise, the visits were further evaluated by two reviewers, where the final decision was made by the senior reviewer. Where discharge diagnosis was not available due to a disposition of left without being seen (LWBS), the chief complaint was used to determine whether the visits were related. In cases where there was more than one RTED, we applied the same criteria to determine whether additional visits were related. The data available did not enable us to differentiate between planned and unplanned RTED.
We extracted the following demographic and visit characteristics from the administrative databases for each visit: age, sex, visit site, triage acuity level using the Canadian Triage and Acuity Scale (CTAS), reason for visit, date and time of initial contact (triage or registration, whichever occurred chronologically earlier), date and time initially seen by the physician, date and time of disposition, discharge diagnosis, discharge disposition (transferred, admitted, discharged, death, LWBS, or left against medical advice [LAMA]). The institutional ethics boards for participating sites reviewed and approved this study. Given the low risk to patient confidentiality of this retrospective administrative database design, a waiver of consent was approved.
Study objectives and outcome measures
Our primary objective was to determine the proportion of children initially presenting to a tertiary PED with an RTED (PED or general ED) both within 72 hours and within 7 days of the incident visit to compare the rate of return visits using both the upper and lower limits for RTEDs reported in the current literature. Our secondary objective was to describe and compare measures of ED flow (WT and LOS) and disposition between a) the index visit and the first RTED against all visits to the PED, to highlight the difference in utilization characteristics of children who come back to the ED and those who do not; b) the index visit compared to the first RTED; and c) RTED occurring at the PED against RTED at a general ED. The outcome measures included ED LOS, WT to physician assessment, proportion of visits being admitted to an inpatient ward, and proportion of LWBS.
Analyses
We used descriptive statistics to report all outcomes. We presented continuous variables (LOS, WT) using medians and interquartile range (IQR). We used proportions to present bivariate variables (rates of return visits, rate of admissions). We used the Mann-Whitney U test to evaluate the difference between unpaired continuous outcome measures (LOS and WT between index and overall PED visits) and the Wilcoxon signed ranks test to evaluate the difference between paired outcome measures (LOS and WT between index and their RTED). We used the chi-square test to compare binary outcomes such as 1) rate of admission between index visits and RTED, 2) CTAS distribution between children with and without return visits to the PED, 3) CTAS distribution between index and repeat visits to the ED, and 4) CTAS distribution on the index visit between children who were admitted and those who were discharged on the RTED.
RESULTS
Rates of return visits
During the study period, the PED received 43,596 visits, of which 3,311 (7.6%) had an RTED within 7 days, including 2,540 (5.8%) for which the RTED was within 72 hours. Our review also identified 88 index visits with return presentations deemed unrelated to the original visit diagnosis and were excluded from further analyses. Of all RTED within 7 days, 2,866 (87%) returned to the PED, and 426 (13%) returned to another facility. Among children with repeat visits to the ED, 80.0% had one repeat visit only; for those with more than one RTED, the average number of return visits was 2.4 (standard deviation 0.7, range 1-6).
Characteristics of subjects with and without return visits
Table 1 describes the demographic details of the study population. Compared to all other PED visits, the group of children who had a subsequent RTED had a higher triage acuity at their index visit (CTAS-1 0.2%, CTAS-2 15.6%, CTAS-3 42%, CTAS-4 40.5%, CTAS-5 1.6% v. CTAS-1 0.5%, CTAS-2 13.7%, CTAS-3 37.1%, CTAS-4 45.5%, CTAS-5 3.2%, p<0.01). Measures of flow and disposition for visits at the PED are shown in Table 2. The LWBS proportion was higher among index visits of children with a subsequent RTED than among the overall PED visit population (6.5% compared to 3.9%, p<0.001). ED LOS was longer for patients with a subsequent RTED than the overall PED population (210 minutes v. 185 minutes p<0.001). On the index visit, infectious diseases accounted for>40% of diagnoses resulting in an RTED. The five most common diagnoses at the index visit associated with an RTED are listed in Table 3.
Table 1 Demographic characteristics comparing all PED visits to those with RTED within 7 days
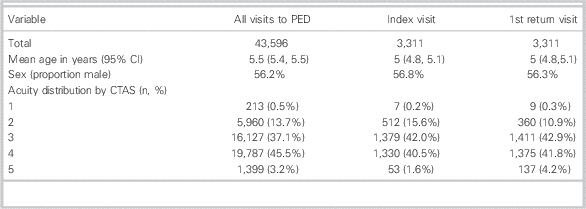
CTAS=Canadian Triage and Acuity Scale; PED=pediatric emergency department; RTED=return to emergency department.
Table 2 Measures of ED flow and disposition comparing all PED visits and the index and first RTED
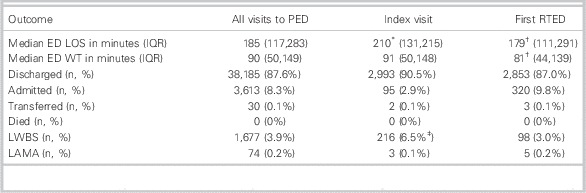
ED=emergency department; LAMA=left against medical advice; LOS=length of stay; LWBS=left without being seen; PED=pediatric emergency department; RTED=return to emergency department; WT=waiting time.
* p<0.001 (index visit v. all PED visits).
† p<0.001 (first RTED compared to index visit).
‡ p<0.01 (index visit v. all PED visits).
Note that the admission rate of 2.9% on the first visit to the emergency department indicates that 2.9% of patients with a return visit to the emergency department for the same clinical complaint were admitted, subsequently discharged, and returned to the ED within 7 days of their initial visit.
Table 3 Top five most common discharge diagnoses of children with an associated RTED

Characteristics of return visits
At the RTED, the distribution of triage acuity was lower on the return visit compared to the index visit (CTAS-1 0.3 %, CTAS-2 10.9%, CTAS-3 42.9%, CTAS-4 41.8%, CTAS-5 4.2% v. CTAS-1 0.2%, CTAS-2 15.6%, CTAS-3 42.0%, CTAS-4 40.5%, CTAS-5 1.63%, p<0.01). The rate of hospital admission was slightly higher on the first RTED than that found in the overall PED population (9.8% v. 8.3%, p<0.01). Of note, among children with one or more RTED, 95/3,311 (2.9%) were admitted on their index visit, discharged from the in-patient ward, and subsequently returned to the ED for the same complaint within 7 days of their index PED visit, despite their initial hospital admission.
Although the proportion of LWBS was higher among subjects with an RTED than the overall PED population during their index visit, the proportion of LWBS during RTED was similar to the overall PED population at 3.0%. Median ED LOS was longer on the index visit than on the first RTED (210 minutes v. 179 minutes, p<0.001).
Return visits to the PED versus general ED
Children returning to the PED had a much higher rate of admission than those returning to a general ED (10.6% v. 3.7%, p<0.01). Both median ED LOS and WT were longer on the first RTED when it occurred in the PED compared to a general ED (186 minutes v. 132 minutes, p<0.001 and 88 minutes v. 44 minutes, p<0.001, respectively). A comparison of demographic information and outcomes between RTED at the PED versus a general ED is shown in Table 4.
Table 4 Comparison of patient characteristics, measures of ED flow, and disposition on the first RTED stratified by return visit site (PED v. community ED)
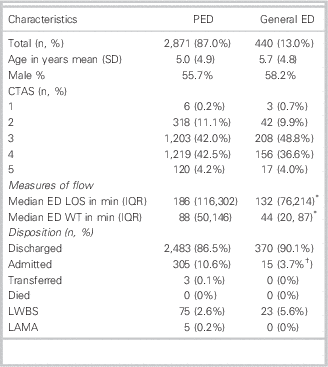
* p<0.001.
† p<0.01.
CTAS=Canadian Triage and Acuity Scale; ED=emergency department; LAMA=left against medical advice; LOS=length of stay; LWBS=left without being seen; PED=pediatric emergency department; RTED=return to emergency department; SD=standard deviation; WT=waiting time.
Missing data
With the exception of WT, where the data were missing for about 20% of all subjects, the proportion of subjects with missing values on all other variables was trivial. Triage CTAS category was missing for 110/43,596 in the overall PED population, 30/3,311 patients on the index visit with an RTED, and 19/3,311 patients on their first RTED (possibly because they left prior to triage and CTAS assignment). LOS data were missing for 6/43,596 in the overall PED population, 1/3,311 patients at the index visit, and 1/3,311 patients on their first RTED. Information on disposition was missing for 17/43,596 patients in the overall PED population, 2/3,311 patients at the index visit, and 32/3,311 patients on their first RTED.
DISCUSSION
This study of RTED from a PED includes those children who returned to any of the 17 community/general EDs in addition to the tertiary PED at which the index visit occurred, thereby providing a more complete measure of RTED within a large metropolitan catchment area. As expected, the proportion of children with a return visit, when including return visits to community EDs (7.6%), is on the high end of the range reported in the current literature (2.7% to 8.1%).Reference Goldman, Ong and Macperson 5 - Reference Goldman, Kapoor and Mehta 7 , Reference Ali, Place and Howell 9 - Reference Montalbano, Rodean and Kangas 14 , Reference Pham, Kirsch and Hill 16 RTED to only the original PED significantly underestimates the burden of return visits in this study by approximately 15% (6.6% v. 7.6%).
Only a few previous large studies have examined pediatric RTED to multiple sites.Reference Cho, Shapiro and Cabana 11 - Reference Sung, Liu and Chen 18 Three of these multicentre studies included patients of all ages, including adults.Reference Calder, Pozgay and Riff 15 - Reference Ko, Lee and Chen 17 Two large studies reported low rates of RTED: Akenroye et al. described a 3.3% RTED to and from PEDs but did not capture returns to general EDs and focused their study on identifying factors associated with admission upon RTED.Reference Akenroye, Thurm and Neuman 12 Cho et al. reported a 2.7% RTED rate using a large administrative database from the National Ambulatory Care Hospital Survey, but only visits to and from the same ED were examined, and the ED type was not reported.Reference Cho, Shapiro and Cabana 11 At the high end of the range, Saunders et al. reported a pediatric RTED rate of 7.5% among a multicentre cohort in Ontario,Reference Saunders, To and Parkin 13 and Montalbano et al. reported the highest published pediatric RTED rate of 8.1% among a sample of children with Medicaid in the United States.Reference Montalbano, Rodean and Kangas 14 The Saunders study focused specifically on the impact of family immigration status on return visits or adverse outcomes and did not report RTED according to site or type of ED. Although the Montalbano study described pediatric patients who returned for care to urgent care or office clinic settings following an ED visit, these comprised a small proportion of return visits, and the type of ED and directionality of RTED were not reported among their RTED cohort. Therefore, our study contributes to a further understanding of how children treated in a PED who return for care related to their index visit impact not only the PED but also other community EDs as well, and may offer a more accurate estimation of the true incidence of RTED resulting from visits to a PED, particularly within the context of the Canadian universal health care system where patients are not restricted to specific networks of care within the context of individual insurance plans.
Previous research on return visits has used variable definitions, with a time frame from 48 hours to 7 days following the index visit. We found that including revisits up to 7 days after the index visit captured an additional 30% (5.8% v. 7.6%) of children who sought care for the same complaint compared to a window of 72 hours, suggesting that shorter definitions of RTED may underestimate the true burden. Moreover, published reports with lower proportions of RTED often exclude index visits with a disposition of LWBS, LAMA, or admission to the hospital.Reference O’Loughlin, Hacking and Simmons 10 We found that these index visits represent a significant number of patients who ultimately return to an ED for evaluation of the same complaint, thereby adding to ED input factors that contribute to further ED crowding and should therefore be included to provide a more accurate assessment of the overall burden of RTED on ED resources.
Controversy exists over whether RTED are an indicator of ED safety/quality or reflect a larger systems failure that might be preventable.Reference Timm, Ho and Luria 2 , Reference Pham, Kirsch and Hill 16 Previous studies have shown that parents of children who had an RTED were generally satisfied with the care they received on their initial visit (94% satisfaction rate), but a significant majority cited lack of access to a family physician as a primary reason for their return visit.Reference Ali, Place and Howell 9 On the other hand, a study by Easter and Bachur (2012) found that among children who returned to the ED and required admission to the hospital, 13% had received medical care/counselling that was deemed deficient by an independent reviewer, suggesting that the RTED may be a marker of poor quality of care.Reference Easter and Bachur 8
Numerous studies have found specific demographic variables associated with an RTED (i.e., chronic disease, higher acuity on presentation, younger age, underlying diagnosis, time of arrival to the PED, lack of access to primary care and a disposition of LWBS on the index visit).Reference Goldman, Ong and Macperson 5 - Reference Saunders, To and Parkin 13 With the exception of LWBS, these risk factors are not modifiable in the ED. In addition, studies examining the impact of RTED have generally used disposition outcomes (i.e., proportion admitted) to evaluate the impact of RTED on resource utilization, while we chose to also focus on measures of emergency ED flow (WT and LOS). Our study found that children with an RTED had several markers of increased disease severity or health care utilization on their index visit (increased acuity, longer LOS, and higher rates of admission on RTED), suggesting that follow-up, unscheduled or scheduled, may have been appropriate, in some cases. However, triage acuity overall decreased between the index and RTED, suggesting that it is possible or even likely that a non-ED follow-up setting may have been appropriate for some.
We also noted a higher admission rate if the RTED occurred at the PED than at a general ED (10.6% v. 3.7%, p<0.01). This is despite the observation that the triage acuity level of RTED was generally lower at the PED than at general EDs (see Table 4). Whether this reflects systematic variability in triage acuity assignment between a PED and ED triaging, or self-selection by families with regard to which ED to return to, is unclear. Large multicentre observational studies have validated the use of the pediatric CTAS for children in the PED, demonstrating both high inter-rater reliability and its robust ability to predict health services utilization, but these studies have not yet included the pediatric population receiving care in a non-PED institution.Reference Gravel, Gouin and Goldman 20 - Reference Gravel, Gouin and Manzano 23 Although we have not found any study exploring families’ preferences for ED sites when returning for further emergency care, one study did document significant differences in both patient characteristics (younger) and clinical outcomes (more frequently hospitalized) in children assessed at PEDs compared to general EDs that would support the notion that children brought back to a PED rather than to a general ED may follow a similar pattern.Reference Nelson, Walsh and Fleisher 24 In Canada, it is common for a single tertiary care referral centre to service a large geographic area; therefore, preference for a return visit site may simply reflect proximity. Future studies are planned to characterize the bi-directional nature of pediatric RTED, including those with an index visit in the community to better understand the complex pattern of ED utilization among children.
Limitations of our study include those inherent to all retrospective administrative databases. Information related to the hospital course for children admitted at the index visit was not available, therefore limiting our ability to comment on reasons for return visits following hospitalization, which are expectedly very different from those who were discharged; also, we were unable to distinguish between an RTED that was scheduled (i.e., told to return for re-evaluation) and unscheduled. Recognizing that root cause analyses of potentially modifiable factors associated with RTED (whether discharged or hospitalized at the index visit) are important but would require a different approach (detailed medical chart review) and would not be feasible with the size of this study’s population and the number of sites where charts would have to be pulled from, we have initiated a separate study with a reduced study population scope.
Similarly, completeness of data available was inconsistent, in that, although data on LOS were available for nearly all children presenting to the PED, just under 80% had documented WTs, making this estimation less reliable. Moreover, it is possible that families who first sought care for their child at the BCCH PED had an RTED beyond the 18 included centres in our study. This would imply that they either reside within the studied catchment area but opted to drive out of their way to seek further emergency care or reside outside of the catchment area and, upon repeat ED visits, chose to seek care locally. Although we cannot capture the magnitude of the frequency of the first scenario proposed, our previously published study on the trend of PED utilization found that only less than 3.5% of our PED users reside outside of the BCCH and Lower Vancouver Mainland area, which are covered by our study EDs.Reference Doan, Genuis and Yu 25
An additional limitation of this cohort study is that the discharge diagnosis NACRS codes were assigned by individual clinicians (nurses and physicians) or unit clerks using diagnostic terms written by the clinicians depending on the site. We did not review individual ED charts, thereby relying on the diagnostic categorization of individual practitioners.
Finally, data summaries and the interpretation we offer here relate to an environment where there is only one referral PED centre in a large geographic area and where most emergency care to children is provided in a general or community hospital with mixed adult-pediatric EDs, and thus may not be generalizable to other health care models.
Strengths of this study include our large data set and geographic area covered, likely capturing all RTED resulting from visits originating at our PED, regardless of the choice of site at the RTED. Future research might further explore the directional pattern and magnitude of the burden of pediatric RTED, where the index visit occurred in a general ED in the community.
CONCLUSION
This study found that the incidence of RTED associated with visits to a PED is higher than most previous estimates, when return visits to any of the community EDs within a large catchment area are considered, with an additional 15% of RTED occurring at EDs other than at the index PED. Furthermore, we found important differences in resource utilization related to a return visit (i.e., WT, LOS, admission rate) between those that occurred in a PED and those in a general ED.
Acknowledgements: The Michael Smith Foundation for Health Research Scholars supported this research.
Competing interests: None declared.






