INTRODUCTION
Measles remains a leading cause of vaccine-preventable death worldwide with more than 30 000 cases reported in the European region in 2011 [1]. Although substantial progress has been made by many Member States over the past few years, the World Health Organization (WHO) target date of 2015 for the elimination of measles and rubella in Europe has passed [2]. A strategy in Ireland for eliminating measles, and rubella and preventing congenital rubella infection was published in 2007 [3].
In Ireland the measles-mumps-rubella (MMR) vaccine is given to babies at age 12 months. A second dose is given at age 4–5 years. About 95% of individuals develop immunity to measles after one dose, and two doses gives protection in about 99% of people [4].
A measles outbreak occurred in a school in a small town in the South East of Ireland in September–November 2013. The town has a population of almost 10 000. It is a dormer town of a neighbouring city which has a population of almost 47 000. There is considerable commuting to the city for employment, education and childcare facilities. MMR uptake at 24 months in the geographical region of the outbreak from 2009 to 2012 was between 85% and 94% annually [5]. In the region the second MMR dose is given by the school immunization team.
There are three primary schools in the town. The index school of this outbreak, school Q, is one of the three town primary schools. Junior Infants is the first year of primary school, which children start at age 4–5 years, in Ireland. The index school had three junior infant classes, classes E, F and G. This outbreak occurred mainly in class E in school Q. The school is in a new building and has almost 700 pupils.
METHODS
Recognition of the outbreak and initial actions
The Consultant in Public Health Medicine [CPHM, Medical Officer of Health (MOH)] on duty in the Department of Public Health in the South East was informed, on 9 October 2013, of five children in the junior infant classes absent with rash illness from school Q. Another child had been ill a couple of weeks previously, reportedly with measles.
All six children's General Practitioners (GPs) were contacted that day and it was established that all cases were thought clinically to have measles. The first date of onset of illness was on 14 September. All six children had received one MMR dose.
The parents of the six suspected cases were contacted to obtain enhanced surveillance information, provide control advice, and to organize salivary swabs for measles virus.
By 10 October the Department of Public Health was aware of eight clinical cases of measles in the index school. All of these cases had received one MMR dose. On this date it was decided to bring forward the planned second dose of MMR for all junior infants. A planned catch-up MMR programme in the three town schools would also be brought forward and completed within 2 weeks.
The first laboratory confirmation of a measles case was on 14 October and an Outbreak Control Team (OCT) meeting was convened on 15 October by the MOH.
Case-finding, enhanced surveillance and case management
School Q, other primary schools, GPs, childcare facilities and asylum-seeker residential centres in the town were contacted to advise of the cluster, to request reporting of suspect cases and to provide advice.
Each reported case was followed up to determine whether they fitted the case definition, to advise on sampling and to provide public health advice (see below).
Enhanced surveillance information was collected on cases and a case-management system was set-up.
Case definition and classification
The case classification is as defined in Case Definitions for Notifiable Diseases, HPSC, 2012 [6]. If a case was recently vaccinated or did not meet the case definition clinical criteria (i.e. no cough, conjunctivitis or coryza), the CPHM in consultation with National Virus Reference Laboratory (NVRL) staff interpreted the laboratory results and clinical symptoms to classify these cases.
Attack rate and vaccine effectiveness
The attack rate and vaccine effectiveness were calculated for the three junior infant classes and for the Junior Infant year in school Q. It was not possible to calculate vaccine effectiveness for the outbreak (due to the very low number of unvaccinated children). Therefore, it was calculated assuming an attack rate of 90% in the unvaccinated population [7].
Microbiology
The WHO measles eradication programme recommends that all suspected measles cases be laboratory investigated [8]. Salivary swabs were taken for all clinical cases reported during the outbreak. The NVRL performed Immunoglobulin M (IgM) and/or PCR testing on swabs, as indicated, depending on the timing of the sample in relation to rash onset. Genotyping of the measles virus identified was performed by the NVRL on a number of samples.
RESULTS
Descriptive epidemiology of the outbreak
There were 33 notifications of suspected measles cases from the town and its county between 9 October 2013 and 11 November 2013. All notified cases were investigated and none of those notified from the neighbouring city or other areas of the county was deemed a case. A total of 20 notifications were deemed confirmed (17) or probable (3) cases and associated with the outbreak.
Of the 20 cases 15 attended school Q and five were pre-school-age children, four of whom attended local childcare facilities. The age range of cases was 1·8–5·8 years (mean 4·5 years); 12 cases were female.
The attack rate in vaccinated children in class E was 36% and in all three junior infant classes it was 14%. Vaccine effectiveness was 60% in class E, 97% in classes F and G and 84% for all three junior infant classes.
Figure 1 illustrates the number of confirmed and probable cases in the outbreak by date of onset. Fifteen cases were in school Q, 14 of whom were in Junior Infants (Table 1). The other five cases were pre-school-age children, four of whom attended three different childcare facilities. Three of the preschool cases attending childcare were siblings of cases in Junior Infants. All three attended different childcare facilities. The fourth childcare case attended the same childcare facility as one of these children. There was no clear epidemiological link identified for the last pre-school-aged child to any of the other cases. Three cases (siblings) were unvaccinated.

Fig. 1. Confirmed and probable measles cases by date of symptom onset, South East Ireland, September–November 2013.
Table 1. Case onset dates, epidemiological links, case classification and genotype, measles outbreak, South East Ireland, September to November 2013 (n = 20)
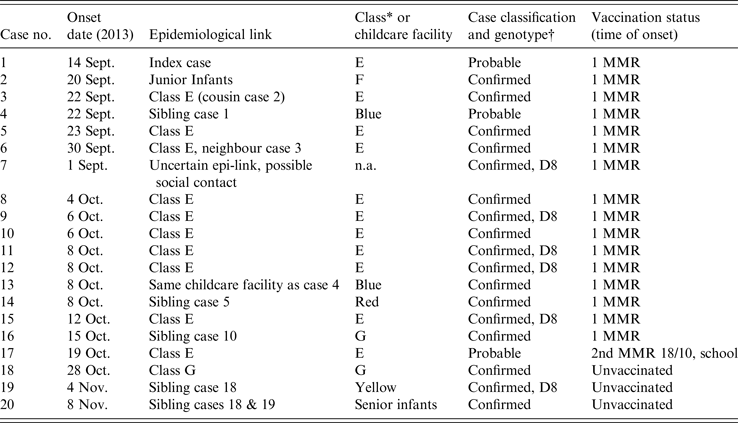
* Classes E, F and G are junior infants in school Q.
† Where not given, genotyping not done.
A complementary figure to Table 1 (Fig. 2), illustrates the chain of transmission and generations of measles in the outbreak. Six generations (incubation period 6–15 days) of measles cases were identified in the outbreak. The six generations include the index case (progenitor) and also the first to fifth generations, as illustrated. Three generations of measles infection occurred prior to notification of the outbreak (the index case and two subsequent generations). The fourth generation was a single case, the unvaccinated child in Junior Infants, and the fifth generation two unvaccinated siblings of this case. MMR vaccination was refused by the parents of these three children but they were excluded from all social settings prior to becoming infectious, thereby halting transmission.

Fig. 2. Chain of transmission by generation, class and date of onset, measles outbreak, South East Ireland, September to November 2013 (n = 20).
It can be seen, from Figure 2 and Table 1 that the main epidemiological link in this outbreak was between cases in class E in school Q.
The clinical illness in all cases was mild with only one case hospitalized and one case with a complication (otitis media).
Seventeen measles cases were confirmed on salivary swab as measles infection by either IgM or RNA. Genotyping of six cases identified the measles virus as a D8 genotype, Taunton.
Site visit
A site visit to school Q was conducted by the CPHM after the end of the outbreak. A walkabout was conducted with the school Principal, all three junior infant classes visited, and teachers interviewed. It is a new school, with almost 700 pupils. All three junior infant classes are in similar classrooms, large and well-ventilated, built to Department of Education standards. It had previously been established that the teacher in class E did not have measles.
In addition, all absences of children in Junior Infants from the school in September and October were reviewed with the Principal and the teachers to ensure that all possible cases had been identified.
Outbreak control measures
Outbreak control measures included measures implemented for cases and contacts, measures at school Q and vaccination measures (Table 2). All appropriate actions were taken on probable cases prior to obtaining results of laboratory investigation.
Table 2. Outbreak control measures: cases and contacts; school Q; MMR, South East Ireland, September–November 2013
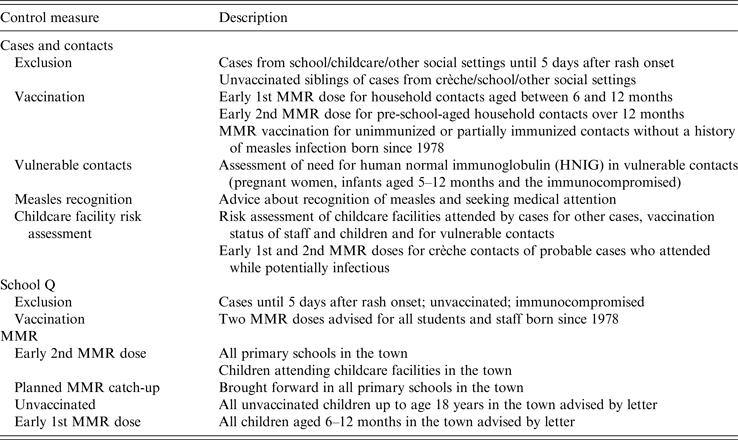
The outbreak was declared over on 14 December 2013, two incubation periods (36 days) after the onset of the last case.
Communications
The CPHM leading the investigation maintained ongoing contact with the Principal of school Q during the outbreak, providing advice and obtaining updates. In addition, other primary schools in the area were contacted to give public health advice.
The school immunization team liaised directly with school Q and surrounding schools to provide MMR vaccination.
The Department of Public Health proactively communicated with parents of children during the course of the outbreak. Letters were sent to primary schools and to childcare facilities, for distribution to all parents, advising of the outbreak and the need for appropriate vaccination. The Child Health Information system was used to identify unvaccinated children and letters were sent to parents/guardians, to advise vaccination. Parents of unvaccinated children who attended the index school were telephoned directly, and written to, to give advice about vaccination and exclusion from school. The Department of Public Health and the local Child Health Office also dealt with many calls from parents throughout the outbreak.
Local clinicians, GPs, paediatricians, obstetricians and emergency-room consultants were informed of the outbreak at the outset and an outbreak update was provided, approximately weekly, to local GPs.
The appropriate health service managers were informed of the outbreak at the outset, and then kept abreast of significant events, in particular vaccination advice.
All childcare facilities and the two local direct provision centres for asylum seekers were contacted to advise of the outbreak, and to provide public health advice.
All vaccinated cases were reported to the Irish Medicines Board (now the Health Products Regulatory Authority) and to the vaccine manufacturers.
A press release was prepared for release in the event of media queries. It was deemed unnecessary to release it proactively as there was otherwise a very active communication campaign being conducted and the feedback received was positive. All unvaccinated children were being proactively identified and written to. In addition, there was concern that press coverage might create anxiety, with false positive clinical diagnoses, and potentially unnecessary actions.
DISCUSSION
This was a well-circumscribed outbreak of measles, largely occurring in one junior infant class of a primary school, with associated cases in pre-school-age children. A number of early cases were seen by GPs and CareDoc (out-of-hours family doctor service) and correctly diagnosed clinically as measles. However, as the cases were not notified by the clinicians and the school did not make contact with the Department of Public Health, notification of the outbreak occurred late. It was notified by a Community Senior Medical Officer (SMO) during a coincidental visit to the school by the school immunization team. Three generations of measles infection had occurred by the time the outbreak came to the attention of the Department of Public Heath. However, we believe that due to the prompt action of the multidisciplinary team involved, this outbreak was brought quickly under control.
Bonačić Marinović et al. reported that it is possible to reduce the number of cases during a measles outbreak in a school by applying a school-wide vaccination strategy within a realistic time-frame [Reference Bonačić Marinović9]. As is seen in Figure 1, any new cases that occurred after notification of the outbreak were either already incubating infection at that stage or were children whose parents refused vaccination. Therefore, no avoidable cases of measles occurred following notification of the outbreak. An overriding concern of the OCT was the potential for spread to the neighbouring city, with the potential for a much bigger and more drawn-out outbreak. This did not occur.
The origin of the outbreak is unclear. The genotype, D8, is associated with South East Asia [Reference Mulders10] but has also previously been associated with outbreaks in Europe [Reference Fitzpatrick11, Reference Rota12]. It is possible that the first case in this outbreak was associated with travel to Europe but this was not proven.
Working relationships and communication during this outbreak were good and contributed to effective outbreak management. As the initial outbreak was identified by an SMO on the school immunization team this illustrates one of the benefits of the team, i.e. visiting schools and liaising with the school community. In addition, the prompt and effective management of the outbreak was made possible by the responsiveness and flexibility of the school immunization team.
In this outbreak, a new approach was taken in identifying unvaccinated children by targeting them with individualized letters advising vaccination. This would not have been possible without the Child Health Information System that has been used over many years in the South East.
The exclusion of cases from school and other social settings is known to be an effective control measure [Reference Pegorie13–Reference Batzing-Feigenbaum16]. During this outbreak exclusion of unvaccinated children proved invaluable in terminating the outbreak. It is a measure that requires careful consideration as children can potentially be excluded for a long time. However, if they opt to be vaccinated an earlier return to school is possible. Unvaccinated children in the school were identified and targeted letters sent to their homes. There were very few unvaccinated children in the school and some disregarded the advice. However, an unvaccinated child in Junior Infants was excluded from school before they subsequently became a case and infectious. The child and two unvaccinated siblings were advised to stay out of school, childcare facilities and other social settings. All three contracted measles but did not transmit the illness to anyone outside their family. This terminated the outbreak.
This was an unusual outbreak of measles in Ireland, in that it occurred in a well-vaccinated population (the three unvaccinated cases occurred late). This may be a reflection of improving MMR immunization uptake rates in Ireland, and, therefore, of changing the measles outbreak epidemiology. That is, when measles is introduced into a well-vaccinated population the cases will be vaccinated individuals.
However, the attack rate in vaccinated children in class E (36%) and in Junior Infants (14%) was considerably greater than the percentage that would be expected due to vaccine failure [7]. Therefore, it may have been due to other factors, e.g. human or vaccine factors. MMR vaccine must be kept refrigerated at +2 °C to +8 °C and protected from light. It should be used within 1 h of reconstitution. Failure to adhere to these recommendations can result in loss of vaccine potency and diminished effectiveness [3]. Two other investigations were undertaken during the outbreak: a cohort study into factors associated with illness in vaccinated children and a detailed study of vaccine management and administration. Neither of these conclusively identified the reason for an outbreak in this vaccinated population. However, in Ireland there is no contractually required tool for use by GPs to ensure correct within-practice vaccine storage and handling. It is important to note that both vaccine manufacturers involved identified no quality deficiencies with the relevant batches of MMR vaccine. Furthermore, if one studies the vaccine effectiveness in this vaccinated population, while it was only 60% in class E and 84% in the junior infant cohort, it was 97% in both classes F and G. It may be that prolonged and intense exposure among children in class E to the measles virus prior to notification of the outbreak resulted in more cases in that class than elsewhere.
CONCLUSIONS
In conclusion, this was a well-circumscribed outbreak of 20 cases of measles occurring, unusually, in a well-vaccinated population. It came late to the attention of the Department of Public Health, delaying intervention. Clinician reporting of suspect measles cases is of great importance in preventing outbreaks. Once notified prompt action by the multidisciplinary team involved, and institution of control measures resulted in quick termination of the outbreak and prevention of cases in the neighbouring city.
Great reliance is placed on clinicians’ diagnostic ability in managing measles cases from a public health perspective, as the time to receiving laboratory results can be many days. In this outbreak the clinical illness was mild possibly indicating some vaccine protection [Reference Rosen17, Reference Ramsay and Brown18], but also illustrating the diagnostic dilemmas that clinicians may face.
Bringing forward the routine, planned second MMR dose in the schools in the town was a big logistical challenge for the child immunization team which was carried out effectively and efficiently.
Exclusion of unvaccinated children from school, childcare facilities and other social settings was an effective control measure, dependent on support from parents and the school. Close cooperation with the Information Communications and Technology (ICT) team resulted in the OCT being able to send targeted letters to the homes of children who had defaulted on MMR vaccination and to children aged between 6 and 12 months, to advise early first MMR dose. Close working with the National Immunization Office was essential in investigating and endorsing MMR vaccination early in the outbreak and, also, in organizing the required extra vaccine deliveries.
The reason for intense measles activity in class E in the index school was not established.
Recommendations
Following the outbreak the OCT made a number of recommendations in the outbreak report, some of which are outlined here.
All suspect cases of measles to be notified promptly by clinicians to the Department of Public Health and continued intensive investigation of all clinically notified cases of measles, including sampling, to facilitate progress towards elimination of measles from Ireland.
Exclusion of children from school may be necessary to prevent a larger outbreak, with its consequences. This requires serious consideration if children are to be deprived of their right to education for the time of exclusion.
An audit tool for cold chain and vaccine stock management in general practice should be developed. This would facilitate regular audit within general practice. There should be consideration of inclusion of audit of cold chain practice and vaccine stock management by GPs in the immunization contract.
ACKNOWLEDGEMENTS
The authors thank all the members of the outbreak and incident control teams, the Child Health Office, Consultant Microbiologists, General Practitioners, HSE South East Information and Communications Technology Department, the schools, National Immunization Office, National Virus Reference Laboratory, and the Health Protection Surveillance Centre.
DECLARATION OF INTEREST
None.







