Drug-induced aseptic meningitis (DIAM) is a rare adverse effect (AE), most commonly associated with nonsteroidal anti-inflammatory drugs (NSAIDs), intravenous immunoglobulin (IVIG), monoclonal antibodies, vaccines, and antibiotics. Amoxicillin-induced aseptic meningitis (AIAM) has been reported, but to our knowledge only 13 cases exist in the literature. Amoxicillin-induced aseptic meningitis is not currently listed as a potential AE on amoxicillin’s product monograph. We present a 14th case of AIAM and suggest that AIAM be added to the list of amoxicillin’s potential AEs.
A 73-year-old male with no known allergies presented with 2 days of confusion, headache, nausea, and fever. Four days prior, he developed symptoms of otitis media. Two days later, he was prescribed amoxicillin 500 mg PO BID and had taken four doses before presentation. He did not take any NSAIDs. He denied sick contacts or recent travel. His past medical history included another episode of aseptic meningitis, multiple vascular risk factors, chronic obstructive pulmonary disorder, and chronic kidney disease. These were being treated appropriately, with no new or recently adjusted medications.
On examination, he had a low-grade fever. His vital signs were otherwise stable. He was alert but disoriented and confused. Passive neck flexion was painful, but there was no objective nuchal rigidity, Kernig’s sign, or Brudzinski’s sign. The remainder of his examination was normal.
A lumbar puncture was performed, then empiric treatment with vancomycin, ceftriaxone, and acyclovir was started. Amoxicillin was discontinued immediately. CSF analysis revealed mild lymphocytosis, elevated protein, and normal glucose (Table 1). Gram stain, cultures, and viral polymerase chain reaction were negative. CT of his head was normal. He improved to baseline within 3 days. Antibiotics were discontinued after 1 week.
Table 1 Results of CSF analysis and microbiology during our patient’s two admissions for aseptic meningoencephalitis
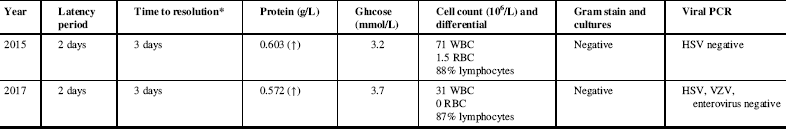
* Of symptoms after discontinuation of amoxicillin.
CSF= cerebrospinal fluid; HSV=herpes simplex virus; PCR=polymerase chain reaction; RBC=red blood cells; VZV=varicella zoster virus; WBC=white blood cells.
A review of his pharmacy records revealed that he had taken four doses of amoxicillin 500 mg PO BID for an upper respiratory tract infection two days before his first episode of aseptic meningitis. He had similar symptoms, including headache, nausea, and confusion. CSF analysis showed lymphocytosis, elevated protein, and normal glucose (Table 1). A CT head and electroencephalography were normal. Amoxicillin was discontinued on admission and he was treated empirically with vancomycin, ceftriaxone, and acyclovir after the lumbar puncture. His symptoms resolved within 3 days. He had not taken any amoxicillin in between these two episodes.
Further workup including HIV and syphilis screening, autoimmune serology, thyroid function tests, and MRI of the brain were normal or negative. Given the temporal relationship of his symptoms with amoxicillin, CSF analysis, and negative infectious, autoimmune, and imaging investigations, he was diagnosed with AIAM and advised to avoid amoxicillin in the future.
Drug-induced aseptic meningitis is an uncommon adverse reaction characterized by meningeal inflammation with negative microbiology. Causative drugs include NSAIDs, IVIG, monoclonal antibodies, vaccinations, and antibiotics. Of the antibiotics, common culprits are trimethoprim-sulfamethoxazole, ciprofloxacin, cephalexin, metronidazole, penicillin, and isoniazid.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 – Reference Shahien, Vieksler and Bowirrat 3 AIAM is extremely rare, and have been previously reported only 13 times.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 As with most cases of DIAM, AIAM is a diagnosis of exclusion. The first episode is not usually attributed to amoxicillin, and many cases likely go undiagnosed. All of the published cases of AIAM, including our own, document a positive re-challenge with amoxicillin.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1
The pathogenesis of DIAM remains elusive. Theories suggest an immune-mediated hypersensitivity reaction or direct meningeal irritation.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 The former has been supported by the detection of serum immune complexes in the CSF of some patients with DIAM caused by drugs other than amoxicillin. However, one report of AIAM tested serum and CSF for immunoglobulin E to amoxicillin and immune complexes interacting with C1q and did not provide any evidence supporting a type 1 or 3 hypersensitivity reaction.Reference Kastenbauer, Pfister and Wick 4 No other cases and similar studies of AIAM have been reported. Further investigations are required to understand its underlying mechanisms.
The clinical manifestations of AIAM are typical for meningoencephalitis, including fever, headache, neck stiffness with or without objective meningismus, cognitive changes, and related neurological signs.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 , Reference Prieto-González, Escoda, Coloma and Grau 2 Our patient’s presentation was therefore similar to previous reports. Given the nonspecific signs and symptoms, the differential diagnosis for recurrent meningitis is broad. The most common infectious cause is herpes simplex virus-2; however, other viruses, fungi, and parasites may be culprits. For instance, an unusual case of spinal neurocysticercosis presenting with recurrent aseptic meningitis after a prolonged incubation period has been reported.Reference Rosenberg and Galen 5 , Reference Boulos, Aviv and Lee 6 Autoimmune diseases such as systemic lupus erythematosus, Behçet’s disease, and sarcoidosis are infrequently complicated by recurrent aseptic meningitis. Malignancy should be ruled out. Rarely, patients with benign tumors or intracerebral cystic abnormalities have developed recurrent meningitis.Reference Boulos, Aviv and Lee 6
In our patient, autoimmune serology and neuroimaging were normal or negative. His CSF was typical for DIAM, as it usually shows mononuclear, often lymphocyte-predominant, pleocytosis, elevated protein, and normal glucose. These are also found in viral or partially treated bacterial meningitis; however, microbiological testing was negative.
Ultimately, AIAM is suggested if the symptoms occur only after exposure to amoxicillin, typically within hours to days, and resolve within 24-72 hours after it is discontinued. With repeated exposure and occurrences of AIAM, patients tend to experience shorter incubation times and more severe clinical presentations.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 However, our patient had the same 48-hour incubation time, a similar clinical presentation, and less CSF pleocytosis and protein elevation with the second episode.
Treatment of any DIAM is withdrawal of the drug and symptomatic measures.Reference Turk, Šimić, Makar-Aušperger and Radačić-Aumiler 1 Our patient received antibiotics on admission with the presumption that his presentation may have been infectious. Although it is possible that these are an unidentified infectious agent, the temporal relationship of his symptoms with amoxicillin use and discontinuation and negative serology, CSF microbiology, and neuroimaging support a diagnosis of AIAM instead.
In conclusion, aseptic meningitis is a reversible but rare complication of amoxicillin use and is not currently listed as a potential AE on the product monograph. Given that our case represents the 14th incidence of AIAM and that amoxicillin is prescribed globally for numerous reasons, health care professionals should be aware of this potential AE. Whether or not other related drugs or β-lactams should also be avoided in patients with AIAM has yet to be investigated.
Acknowledgments
None.
Disclosures
LC and ME have nothing to disclose.
Statement of Authorship
Study concept and design: Laura Chu and Marsha Eustace; data acquisition: Laura Chu; drafting of manuscript: Laura Chu; revising for content: Marsha Eustace; study supervision: Marsha Eustace.



