The anaemia caused by Fe deficiency is considered the most common nutritional disorder worldwide, and affects children, pregnant women and women of childbearing age. Pregnancy is an important phase of risk for the development of Fe-deficiency anaemia, which is a public health problem due to its associated increased risks of perinatal morbidity and mortality( Reference Dal Pizzol, Giugliani and Mengue 1 ).
Approximately 40 % of all maternal deaths during the perinatal period are related to anaemia. Unfavourable pregnancy outcomes occur 30–40 % more frequently among women with anaemia than among non-anaemic women and their babies get less than 50 % of the required Fe reserve, presenting higher risks of developing anaemia during their first year of life( Reference Batista Filho, Souza and Bresani 2 ).
The global prevalence of anaemia in pregnant women is estimated at 41·8 %; in the Americas alone, this prevalence reaches 24 %. In Brazil, the prevalence of anaemia in pregnant women is about 29 %( 3 ).
One of the strategies recommended for the control of anaemia is nutritional education, with promotion of diversity in food consumption among at-risk populations, along with actions for supplementation and fortification of foods with Fe( 3 ). Food fortification constitutes a low-cost intervention measure, with high efficacy and flexibility; besides, it is socially accepted since it does not interfere with the eating pattern of the population and uses everyday foods. Overall, as the doses of supplements added to the foods are low, the risks of side-effects and toxicity are minimal( 3 ).
Several countries have implemented food fortification strategies to meet Fe needs. In Brazil, the fortification of all flours of wheat and corn with Fe became mandatory in December 2002, being fully implemented in July 2004. The level of fortification is 4·2 mg/100 g flour. The compounds approved for fortification are: ferrous sulfate dehydrated (dry); ferrous fumarate; reduced Fe – 325 mesh Tyler; electrolytic Fe – 325 mesh Tyler; NaFeEDTA; and Fe bis-glycine chelate( 4 ).
Recently, some studies that evaluated the effect of the fortification of wheat and corn flours with Fe on maternal health in Brazil were published. In an assessment of the Hb concentrations of 228 pregnant women attending a public maternity facility in Brazil before and after the implementation of flour fortification, Côrtes( Reference Côrtes 5 ) described that anaemia was more prevalent before (29 %) as compared with after the implementation of fortification (8 %; P < 0·001). Fujimori et al. ( Reference Fujimori, Sato and Szarfarc 6 ) analysed data from 12 119 medical records of pregnant women attending public prenatal services in five Brazilian geographical regions and found that the prevalence of anaemia fell from 25 % to 20 % in the group before and after the fortification of flour with Fe (P < 0·001).
In contrast, a study with 750 pregnant women in São Paulo found no significant differences in the prevalence of anaemia or Hb concentration before and after implementation of the national food fortification( Reference Sato, Fujimori and Szarfarc 7 ). Therefore, besides being scarce, it is verified that the results in these studies are contradictory, rendering no conclusions about the fortification of flours with Fe and its effects on maternal health.
The objective of the current study was to estimate the frequency of anaemia in pregnant women before and after the mandatory fortification of wheat and corn flours with Fe.
Experimental methods
Study design
The present study is a retrospective cross-sectional analysis developed from secondary data. It is part of a multicentre research project on the impact of fortification of flours with Fe on Hb concentration of pregnant women attending health centres in Brazil, developed in urban centres from five regions of the country. The data analysed in the present study relate to data obtained in the city of Rio de Janeiro, located in the Southeast region of Brazil.
Two groups were studied: (i) Group 1 (G1) pre-fortification, comprising pregnant women who attended prenatal care and whose parturition happened before June 2004, when flour fortification was effectively implemented in the country; and (ii) Group 2 (G2) post-fortification, comprising pregnant women whose last menstrual period happened after June 2005, when the fortification programme had already completed 1 year of implementation, until 2007.
The minimum size of the sample for each group of pregnant women was calculated based on the desired precision to estimate the proportion of women with anaemia: ![]() , in which p is the proportion of women in an adequate situation; q is the proportion of women with anaemia (
, in which p is the proportion of women in an adequate situation; q is the proportion of women with anaemia (![]() ); z is the percentage of normal distribution; and d is the maximum error in the absolute value. Considering p = 0·50 (which means the highest relationship between p and q) and d = 5 % to a confidence interval z of 95 %, results in
); z is the percentage of normal distribution; and d is the maximum error in the absolute value. Considering p = 0·50 (which means the highest relationship between p and q) and d = 5 % to a confidence interval z of 95 %, results in ![]() (
Reference Fujimori, Sato and Szarfarc
6
).
(
Reference Fujimori, Sato and Szarfarc
6
).
To reach the expected sample size, pregnant women attending two public maternity hospitals in Rio de Janeiro were included in the study from 1999 to 2007. The medical records did not show the same format, but contained the same type of information required, because they are teaching hospitals. Initially the investigation involved a sample of 500 medical records of pregnant women per group. This was done because losses were expected owing to data inconsistency, although the institutions were teaching hospitals. After the exclusion criteria were established (we excluded the medical records of pregnant women who did not have Hb concentration registered during gestation, who presented twin pregnancy or who had HIV infection and other chronic diseases), 778 medical records of pregnant women attending at these hospitals were selected, of which 391 were from G1 and 387 were from G2.
The data in the medical records were collected by a trained and supervised team, following a field manual for data collection that ensured the standardization of procedures.
Both hospitals are located in Rio de Janeiro and give free medical appointments to local pregnant women, as per demand. Through analysis of the patients’ sociodemographic and anthropometric characteristics in both units, similarities were verified among the treated pregnant women in both health establishments.
Blood Hb concentration and anthropometry
The Hb cut-off point adopted for anaemia diagnosis was <11·0 g/dl( 8 ). When more than one Hb measurement was recorded in a gestational trimester, the mean of the values was considered.
Measures of pre-pregnancy weight, pre-birth weight or weight at the last prenatal care visit and stature were obtained. The adequacy of gestational weight gain in the pregnant adult women and adolescents was evaluated considering the ranges of weight gain for each category of pre-gestational/initial BMI( 8 , Reference Padilha, Accioly and Veiga 9 ). The assessment of pre-gestational nutrition status among adolescents was based on cut-offs of pre-gestational BMI that were adopted for each age in years and months( Reference Saunders, Accioly and Costa 10 ).
Newborn characteristics
Weight, length and gestational age data of the newborns were collected at birth. Newborns were classified as ‘low weight’ when the weight at birth was <2500 g and as ‘macrosomic’ when the birth weight was ≥4000 g. The babies were considered ‘preterm’ when the gestational age at birth, according to the last menstrual period, was <37 weeks and as ‘post-term’ when the gestational age was ≥42 weeks( Reference Fescina, De Mucio and Martínez 11 ).
Socio-economic characteristics
The following variables were obtained: maternal age (≤19 years old, ≥20 years old) and schooling (≤8 years of schooling, >8 years of schooling).
Characteristics of clinical and prenatal care
The following variables were obtained: number of prenatal appointments with a doctor (≤5, ≥6); number of prenatal appointments with a nutritionist (≤3, ≥4); and obstetric precedents such as number of gestations (0, 1–3, ≥4), number of abortions (0, 1, ≥2), weight gain during pregnancy (adequate, inadequate), pre-pregnancy BMI (underweight, normal weight, overweight, obese), type of parturition (natural, Caesarean), newborn's weight at birth (<2500 g, ≥2500 g) and gestational age (<37 weeks, ≥37 weeks)( Reference Fescina, De Mucio and Martínez 11 ).
Analysis and processing of data
For the comparison of categorical variables between G1 and G2, the χ 2 test was employed and P < 0·05 was used to indicate statistical significance. Differences in Hb concentration and frequency of anaemia between groups, adjusted for possible confounding variables, were evaluated by linear regression (for Hb concentration) and logistic regression (for frequency of anaemia). The enter/stepwise method was applied in order to insert variables into the models. The variables inserted into the models as confounders were the ones that showed significant differences in the comparison between G1 and G2. Two linear regression models were elaborated: one for the second gestational trimester, the other for the third gestational trimester. For logistic regression, three models were elaborated: one for each of these two moments and another for the whole gestational period. The values of β and their respective 95 % confidence intervals are presented. The variables with P < 0·05 were retained in the models. Data analysis was conducted using the SPSS statistical software package version 16·0.
Ethical/legal aspects
The project was approved by the Ethics in Research Committee of Escola de Enfermagem da Universidade de São Paulo (process no. 521/2006/CEP-EEUSP) and by the Ethics in Research Committee of Maternidade Escola da Universidade Federal do Rio de Janeiro (May 23rd, 2007). The data collection was initiated only after formal approval of the managers of the institutions involved. The research coordinator was responsible for confidentiality of the information collected, considering that, owing to the characteristics of secondary data collection, was not possible to obtain the consent of the pregnant women.
Results
In the analysis, the medical records of 778 pregnant women were included: 391 referred to as the pre-fortification group (G1) and 387 referred to as the post-fortification group (G2). In both G1 and G2, the proportion of pregnant adult women was higher than the proportion of pregnant adolescents (73·2 % v. 26·8 % in G1 and 87·1 % v. 12·9 % in G2), although there was a higher proportion of adolescents in G1 than in G2 (P < 0·001). A higher proportion (P < 0·001) of pregnant women in G1 had up to 8 years of schooling. There was no significant difference between the groups according to maternal anthropometric characteristics, pre-gestational BMI or adequacy of total weight gain (Table 1).
Table 1 Anthropometric and socio-economic characteristics of the study population: pregnant women attending two public maternity hospitals in Rio de Janeiro, Brazil, 1999 to 2007
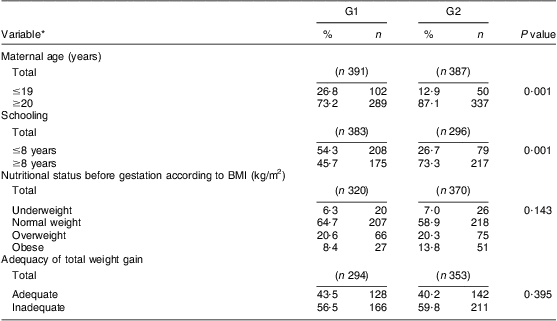
G1, pre-fortification group, those who attended prenatal care and whose parturition happened before June 2004, when fortification of flours with Fe was implemented in the country; G2, post-fortification group, those whose last menstrual period happened after June 2005, when the fortification had already completed 1 year of implementation, until 2007.
*The total n was variable depending on the amount of information available in medical records.
When we compared the groups with respect to prenatal care characteristics and obstetric history, it was verified that women in G2 had higher numbers of previous gestations (P = 0·005), prenatal visits (P = 0·001) and appointments with a nutritionist (P = 0·022) than women in G1 (Table 2).
Table 2 Prenatal care, obstetric history and birth condition characteristics of the study population: pregnant women attending two public maternity hospitals in Rio de Janeiro, Brazil, 1999 to 2007
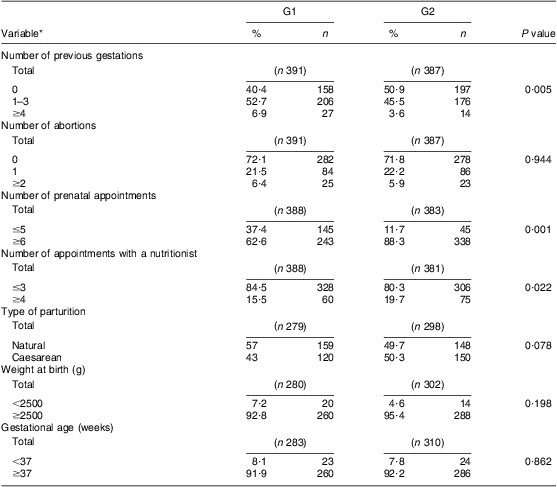
G1, pre-fortification group, those who attended prenatal care and whose parturition happened before June 2004, when fortification of flours with Fe was implemented in the country; G2, post-fortification group, those whose last menstrual period happened after June 2005, when the fortification had already completed 1 year of implementation, until 2007.
*The total n was variable depending on the amount of information available in medical records.
The prevalence of anaemia varied in accordance with the trimester of pregnancy, with lower values for G2 in the second trimester (25·6 % v. 33·2 %, P = 0·033), in the third trimester (25·4 % v. 39·7 %, P = 0·001) and when considering anaemia during any period of pregnancy (28·8 % v. 40·3 %, P = 0·001) compared with G1 (Table 3). Hb concentrations were significantly higher in G2, when compared with G1, in the second and third trimesters (P = 0·001 for both; Table 3).
Table 3 Anaemia prevalence and Hb concentration by trimester of pregnancy among the study population: pregnant women attending two public maternity hospitals in Rio de Janeiro, Brazil, 1999 to 2007
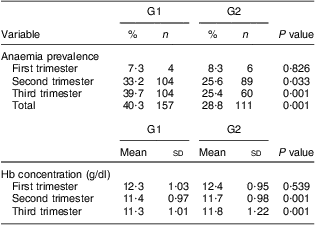
G1, pre-fortification group, those who attended prenatal care and whose parturition happened before June 2004, when fortification of flours with Fe was implemented in the country; G2, post-fortification group, those whose last menstrual period happened after June 2005, when the fortification had already completed 1 year of implementation, until 2007.
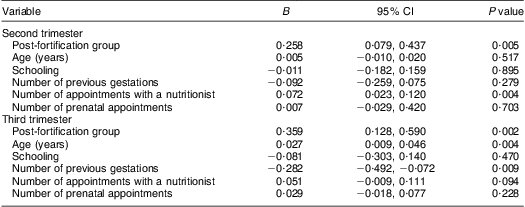
The predictor variables in the model for Hb concentration during the second trimester of pregnancy were (i) being a member of the post-fortification group G2 and (ii) number of appointments with a nutritionist. During the third trimester they were (i) being a member of G2, (ii) maternal age and (iii) number of previous gestations. The women in G2 presented Hb concentration 0·26 g/dl and 0·36 g/dl higher in the second and third trimesters, respectively, in comparison to the women in the pre-fortification group G1, independent of sociodemographic, obstetric and prenatal care variables. An increase of 0·072 g/dl in Hb concentration of pregnant women for every appointment they had with a nutritionist was also observed in the second trimester (Table 4).
Table 4 Results of linear regression models for predictor variables of Hb concentration in the second and third trimesters of pregnancy
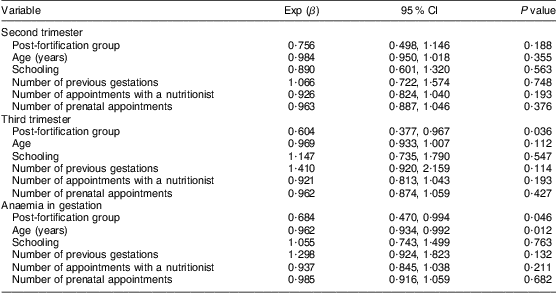
Being a member of the post-fortification group G2 was observed as being protective against anaemia in the third trimester in the logistic regression analysis of predictor variables in the model for anaemia presence, although such a fact was not observed in the second trimester (Table 5). In other words, the women in G2 had approximately 40 % less chance to have anaemia in the third trimester, when compared with the women in pre-fortification group G1, independent of the effect of confounding variables. When the presence of anaemia was considered in any gestational trimester, it was observed that being a member of G2 was a protective factor against anaemia. So, the women in G2 had 32 % less chance of developing anaemia during gestation, compared with G1. In this analysis the age of the pregnant woman was also found to be associated with anaemia; for each year of increase in age, the chance to have anaemia decreased by 4 % (Table 5).
Table 5 Result of logistic regression models for predictor variables of anaemia prevalence in the second and third trimesters of pregnancy and anaemia in gestation
Discussion
Nowadays there are countries that fortify foods with Fe and, according to data researched by the Flour Fortification Initiative( 12 ), the percentage of wheat flour that gets fortified worldwide increased from 18 % in 2004 to 27 % in 2007. However, studies that evaluate the impact of this measure on the health of pregnant women are still scarce.
Sadighi et al. ( Reference Sadighi, Sheikholeslam and Mohammad 13 ) evaluated the efficacy of the programme of food fortification with Fe in Iran among women aged 15–49 years, and observed a lower prevalence of low ferritin levels in the intervention group, concluding that the programme had a positive effect on the prevalence of low ferritin levels.
Hotz et al. ( Reference Hotz, Porcayo and Onofre 14 ) conducted a randomized controlled intervention study in Mexico, among non-pregnant women aged 18 to 49 years, to test the efficacy of ingesting rice fortified with micronized and encapsulated ferric pyrophosphate in the improvement of serum Fe concentration. A reduction of 10·3 % in anaemia was observed.
In contrast, in a similar study Sato et al.( Reference Sato, Fujimori and Szarfarc 7 ) did not observe any significant difference in the prevalence of anaemia between pregnant women in São Paulo in the periods before and after the implementation of mandatory fortification of flours with Fe. On the other hand, Côrtes( Reference Côrtes 5 ) evaluated the effect of this measure on pregnant women attending prenatal services in Brasília/DF, before and after implementation of the law, and observed a significant difference (P < 0·001) with anaemia being more prevalent in the group before fortification, a fact also observed in our study. Similar findings are described by Fujimori et al.( Reference Fujimori, Sato and Szarfarc 6 ) in a study among pregnant women from all regions of Brazil. Therefore, it has been found that the prevalence of anaemia decreased after fortification, but remains high in some regions (North and Northeast) in Brazil.
Similar results were observed by Mackerrras et al.( Reference Mackerras, Powers and Boorman 15 ) in a longitudinal study in 2003 where Australian pregnant and lactating mothers used bread as a vehicle to consume iodine; a positive impact of ingestion of this micronutrient among the population was noticed.
Anaemia is harmful to the mother–child pair, being associated with higher risks of morbidity and mortality( 3 ). Food fortification is proposed as an important strategy for anaemia reduction caused by Fe deficiency, since it is economically attractive and presents the possibility to be employed on a large scale( Reference Sato, Fujimori and Szarfarc 7 ).
The higher prevalence of anaemia in the second and third gestational trimesters can be explained by increased Fe needs throughout pregnancy, in addition to the increased need for Fe by the fetus at the end of gestation. Similar Hb levels to those found in the present study have been described in pregnant women in the North region of Brazil and from all regions of Brazil( Reference Fujimori, Sato and Szarfarc 6 ). The findings of the reduction in anaemia prevalence in G2 in the second and third trimesters of pregnancy were confirmed by the increased Hb concentrations in G2 compared with G1 in the same periods, suggesting the protective effect of flour fortification in the pregnant women studied.
In relation to the number of prenatal appointments, it was observed that 62·6 % of G1 and 88·3 % of G2 attended six or more prenatal appointments. The results found in our study are similar to those seen in the National Demographic and Health Survey – PNDS for the Southeast region of Brazil (84·7 %)( 16 ).
It has been noted that women's adherence to prenatal care is related to the quality of care provided by such services and health professionals( 8 ). The higher proportion of women in G2 receiving six or more prenatal appointments, compared with G1, could have influenced the lower prevalence of anaemia in G2. However, in multivariate analysis the effect of membership of G2 on anaemia did not change after adjusting for the effect of variable number of prenatal appointments.
In the identification of sociodemographic variables that influenced mean Hb concentrations in the third trimester, it was verified that each additional year of age increased Hb concentration by 0·027 g/dl in the pregnant women. Through this, the vulnerability of pregnant adolescents to develop anaemia is observed, as reported by some authors( Reference Vitolo, Boscaini and Bortolini 17 , Reference Dias, Lessa and Telarolli 18 ). In fact, the effect of age on Hb concentration in the third trimester and on anaemia during pregnancy remained in the multivariate analysis, and did not alter the effect of fortification on these outcomes.
Pregnancy among adolescents is still regarded as a public health problem at present and is attracting more attention, since the number of adolescent mothers is increasing day by day. Nutritional deficiencies in adolescents that reflect the quantity and quality of food consumption are related to factors such as cultural aspects concerning the standard of beauty, psychological problems and economic constraints( Reference Saunders, Accioly and Costa 10 ).
As for the number of previous gestations, an association between this obstetric variable and a reduction of 0·282 g/dl in Hb concentration for each gestation was observed in our study. Multiparity as well as reduced inter-gestational intervals complicate the reconstitution of women's nutritional reserves and thus can initiate gestational anaemia( Reference Torres, Sato and Yara 19 ). In a study conducted in São Leopoldo/RS among 197 pregnant women, Vitolo et al. ( Reference Vitolo, Boscaini and Bortolini 17 ) observed a tendency of association between anaemia and gestation number higher than three.
It was verified in the present study that the number of appointments with a nutritionist influenced Hb concentration, which increased in value by 0·072 g/dl for each appointment with this professional, in the second trimester. It is worth saying that appointments with a nutritionist, in which the nutritional care is based on educational practice and prophylactic measures that aim to prevent and treat nutritional disorders during gestation, is a positive factor to improve maternal and infant nutritional status. Among the measures employed, guidance towards eating plant-based sources of Fe is emphasized( Reference Lacerda 20 ).
The difference in anaemia prevalence between the groups studied was observed in the second and third trimesters, and in the variable anaemia during gestation (that refers to anaemia in any gestational trimester), therefore suggesting a high protective effect of food fortification with Fe.
The current study evaluated the prevalence of anaemia in pregnant women at two moments: the first was before the mandatory fortification of flours and the second happened at least 1 year after effective implementation of mandatory flour fortification in Brazil. One limitation of the present study is that it was not possible to obtain information about adherence to the Fe+folic acid supplementation prescribed during the prenatal period to all pregnant women beginning in the 20th gestational week( 8 ). This information was not available in the medical records from which the data were abstracted. Furthermore, because the study is a retrospective one that uses secondary data, it was not possible to obtain this information through interviews with the pregnant women.
Besides, by aiming at programme evaluation, the current study presents other limitations with regard to the unknown processes involved in the implementation of mandatory flour fortification with Fe, such as the availability of fortified flours after 2004 and their Fe content. The access of pregnant women to these products and the level of implementation of the fortification in Rio de Janeiro could not be conveniently evaluated. However, based on the National Food Survey, the average daily consumption of bread and pasta, major food sources of wheat flour in Brazil, is about 87 g/d. Where wheat flour is the main component of these products (100 %), one can estimate that the additional Fe intake from fortification is about 3·7 g/d( 16 ).
Despite their limitations, the results of the current study point to a possible protective effect caused by the programme of flour fortification with Fe implemented in the country, because the reduction of anaemia prevalence during gestation was verified after the implementation of mandatory fortification, thus contributing to the prevention and control of this nutritional deficiency that represents the most prevalent gestational occurrence among pregnant Brazilian women.
Acknowledgements
This work was supported by the Conselho Nacional de Pesquisa e Desenvolvimento Científico e Tecnológico (CNPq; process no. 402295/2005-6). The authors declare no conflict of interest. The authors’ contributions were as follows: C.L.d.S., coordination of field work, data collection, analysis of results, drafting the article; C.S. and G.V.d.V., definition of the study design, data analysis, drafting and approval of the final version of the article; E.F. and S.C.S., coordination of the study, approval of the final version of the article.







