The incidence of a single umbilical artery (SUA) approximates 0.5% in singleton pregnancies (Granese et al., Reference Granese, Coco and Jeanty2007; Hua et al., Reference Hua, Odibo, Macones, Roehl, Crane and Cahill2010). Such a finding may be associated with fetal aneuploidy (Dagklis et al., Reference Dagklis, Defigueiredo, Staboulidou, Casagrandi and Nicolaides2010) or malformations (most commonly cardiac or renal; Hua et al., Reference Hua, Odibo, Macones, Roehl, Crane and Cahill2010; Thummala et al., Reference Thummala, Raju and Langenberg1998), but an isolated finding can present clinicians with a pregnancy challenge. While some studies have reported an increased incidence of fetal growth restriction and adverse outcome (Burchstein et al., Reference Burchstein, Levy, Holcberg, Zlotnik and Sheiner2011; Hua et al., Reference Hua, Odibo, Macones, Roehl, Crane and Cahill2010), other studies have reported no difference in fetal growth restriction when compared with a normal three-vessel cord (Bombrys et al., Reference Bombrys, Neiger, Hawkins, Sonek, Croom, McKenna and Sibai2008; Wiegand et al., Reference Wiegand, McKenna, Croom, Ventolini, Sonek and Neiger2008).
An isolated SUA in twin pregnancies can present an even greater challenge than management in singleton pregnancies. Discordance with the co-twin, issues of chorionicity, and the inherent risks of any twin pregnancy all require consideration. An early review of autopsy cases found that a SUA was more prevalent in twin pregnancies than singletons and that most are discordant (Heifetz, Reference Heifetz1984).
More recent studies have found significantly lower birth weights in a twin with a SUA compared to a co-twin with a normal three-vessel cord (Byers et al., Reference Byers, Saade and Harirah2013; Klatt et al., Reference Klatt, Kuhn, Baumann and Raio2012). When compared with a cohort of twins both with three-vessel cords, the outcomes of a twin pregnancy with a SUA include increased risks of growth discordance (Klatt et al., Reference Klatt, Kuhn, Baumann and Raio2012), small for gestational age (SGA; Klatt et al., Reference Klatt, Kuhn, Baumann and Raio2012; Stout et al., Reference Stout, Obido, Longman, Shanks and Cahill2013), and preterm delivery before 28 weeks (Stout et al., Reference Stout, Obido, Longman, Shanks and Cahill2013).
As no current study has compared cases of isolated SUA in twin pregnancies with individually matched consecutive controls, and given the apparent controversy in the management of an isolated SUA in singleton pregnancies, we have aimed to investigate the outcomes further.
Patients and Methods
All patients who had a twin pregnancy and a second trimester morphology ultrasound at the Royal Women's Hospital, Melbourne, over a period of 7.5 years were considered for inclusion. Patients were identified through the hospital's Picture Archiving System (PACS; Viewpoint, GE Healthcare, Buckinghamshire, United Kingdom), with the start point of the study defined as the introduction of the computerized PACS in our hospital.
All patients were scanned at a tertiary obstetric hospital by consultant obstetricians with particular expertise in obstetric ultrasound. Color Doppler was used to visualize the umbilical arteries, both adjacent to the fetal bladder and in a section of a free loop of cord. Twin pregnancies diagnosed with a SUA in one or both twins were identified.
Placental histopathology was performed by experienced perinatal pathologists, and those cases in which a three-vessel cord was identified were excluded. If placental histopathology was not performed, the ultrasound images were reviewed by one of the authors (FDSC).
For those cases in which the finding was isolated, three controls were selected (cases with a major coexistent anomaly or aneuploidy were excluded from analysis). These were defined as the next three consecutive twin pregnancies undergoing a second trimester ultrasound at our hospital, with neither twin being diagnosed with any congenital anomaly. Controls were matched for chorionicity and maternal age (within 5 years). Background and outcome data were collected for the mother and both twins for cases and controls.
Primary outcomes were preterm delivery in less than 34 weeks, SGA (birth weight < -2 SD relative to the British Growth (Cole et al., Reference Cole, Freeman and Preece1998)), and perinatal death. Other outcomes were mode of delivery, twin-twin transfusion syndrome (for monochorionic twins), oligohydramnios, growth restriction or abnormal umbilical Doppler studies, and neonatal intensive care (NICU) or special care nursery (SCN) admission.
Data were analyzed using Stata version 13.1 (StataCorp, 2013). Differences between groups for continuous variables were assessed using Student's t test, both paired and unpaired, where appropriate, and mean differences with 95% CIs were calculated. Dichotomous variables were analyzed with either chi-square or Fisher's exact test if sample sizes were small, and odds ratios (ORs) and 95% CIs were calculated. To adjust for confounding variables, continuous variables were analyzed by linear regression and dichotomous variables by logistic regression. Models were fitted using generalizing estimating equations to account for clustering of twins for fetal/infant outcomes, where necessary.
This study was approved as an audit by the hospital's Human Research Ethics Committee.
Results
Initially, 34 multiple pregnancies were identified as a ‘SUA’ or ‘two-vessel cord’ on the hospital software over the specified period (7.5 years). Four cases were excluded when placental histopathology revealed a three-vessel cord. In seven cases, no placental histopathology was performed and ultrasound images were not available for review: these cases were also excluded.
Of the remaining 23 cases, three were triplet pregnancies, one was a conjoined twin and nine had co-existing anomalies and were excluded. One case was a fetal death in utero in the early second trimester and was also excluded.
Of the 10 cases with coexistent anomalies, three had cardiac anomalies (two coarctations of the aorta and one right-sided aortic arch with enlarged pulmonary trunk), two were cases of trisomy 18, two had multiple serious anomalies, one had an absent lung, and one had severe ventriculomegaly.
This left a total of nine cases of isolated SUA out of 1,243 twin pregnancies over the same period (0.72%). All were discordant for SUA. The exclusions are summarized in Figure 1.
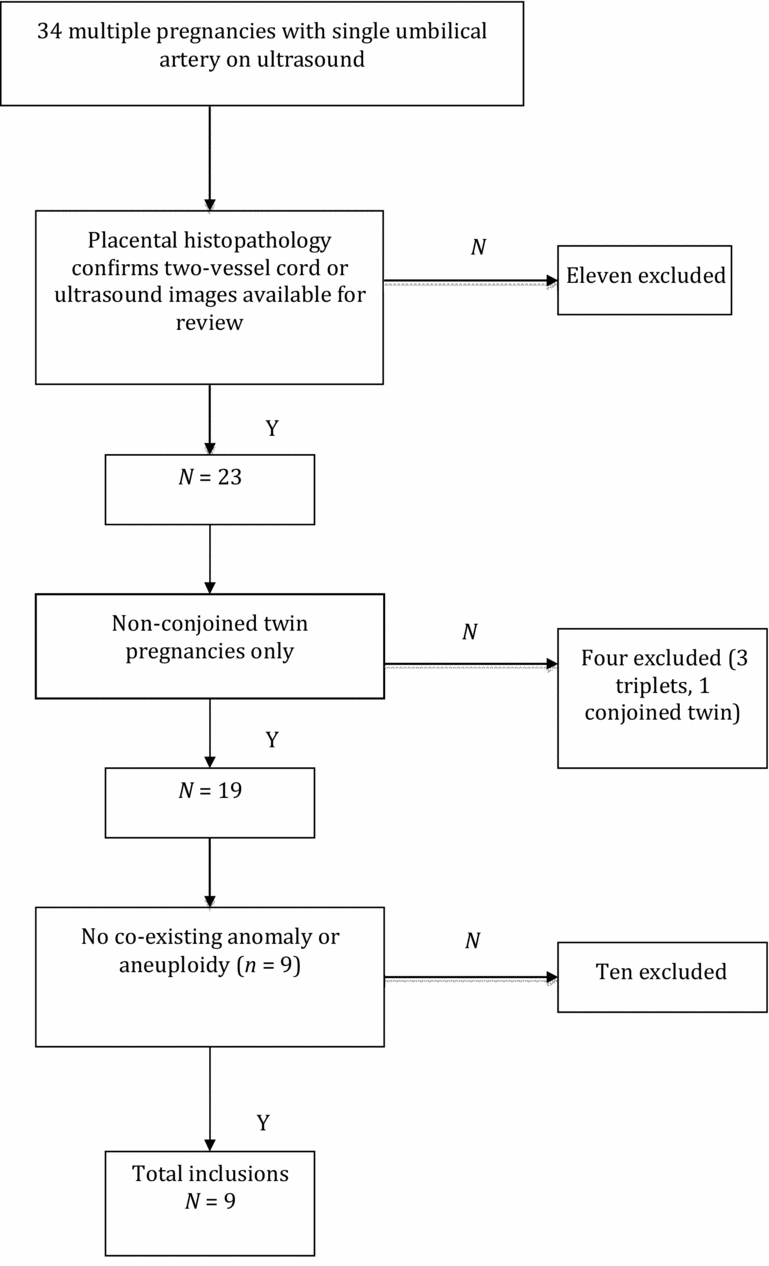
FIGURE 1. Inclusions and exclusions.
There were no differences between cases and controls in background or antenatal variables (Table 1). There was an increased chance of delivery before 34 weeks but no difference in the mode of delivery. There was also no statistically significant increase in growth restriction on antenatal ultrasound.
TABLE 1 Maternal Data

Primary outcomes in bold type.
DCDA = dichorionic, diamniotic; IUGR = intrauterine growth restriction; TTTS = twin-twin transfusion syndrome; GA = gestational age; OR = odds ratio; CI = confidence interval.
*mean difference (95% CI).
Although there was a significantly lower mean birth weight there was not a significantly lower incidence of SGA (Table 2). Within the cases, there was no difference in birth weight SD score between the fetus with and without the SUA (mean (SD): with SUA -0.7 (1.5); without SUA -1.4 (1.0); mean difference = 0.6; 95% CI = -0.2, 1.4; p = .11). In fact, the twin with the SUA tended to be the larger one.
TABLE 2 Fetal Data

Primary outcomes in bold type.
BW = birthweight; NICU = neonatal intensive care nursery; SCN = special care nursery; FDIU = fetal death in utero; OR = odds ratio; CI = confidence interval; NA = not available.
*Adjusted for clustering of multiples; †mean difference (95% CI, adjusted for clustering of multiples); ‡Fisher's Exact Test.
There was a statistically significant increase in any perinatal death in the cases (OR = 10.6, 95% CI = 1.03–109, p = .046) but not after adjusting for clustering of multiples (Table 2). Any perinatal death was strongly related to gestational age: odds of mortality fell by 0.66 (95% CI = 0.48–0.91) for each week's increase in gestational age. Of the three cases of perinatal death, two were in an unaffected infant and one was in an infant with SUA. When adjusted for clustering of multiples and for gestational age, the odds of perinatal death became non-significant (OR = 1.26; 95% CI = 0.27–5.8; p = .77).
Of the other variables, there was a significantly higher chance of admission to NICU or SCN in the cases (Table 2). Admission to NICU was strongly associated with diminishing gestational age. The association with admission to NICU in the cases became non-significant after adjusting for gestational age (OR = 1.56; 95% CI = 0.24, 10.2; p = .64). Admission to either the SCN or the NICU was strongly associated with diminishing gestational age at birth; however, it was not possible to assess the effect of adjusting for gestational age on the odds of being admitted to SCN or NICU.
Discussion
The literature on isolated SUA in twin pregnancies is scarce, with concerns generally focusing on preterm birth, intrauterine growth restriction, or SGA. In the largest and most recent series, Stout et al. (Reference Stout, Obido, Longman, Shanks and Cahill2013) examined 40 twin pregnancies and reported an incidence of 1.7% and a slight increase in preterm birth rates and moderate increase in SGA. Our series of nine patients represents a lower rate of 0.72%, possibly because we mandated a histopathological diagnosis of SUA in the placenta postnatally or review of ultrasound images by a single experienced operator. We cannot calculate an accurate incidence because not all twin pregnancies have had the same scrutiny of ultrasound and histopathology as the cases with SUA.
Our series confirms an increased risk of preterm delivery at <34 weeks; however, there was no increase in antenatal intrauterine growth restriction, nor of postnatal SGA. Indeed, within the cases, the infant with the SUA was slightly larger at birth than the other twin. On reviewing the cases, most preterm deliveries were spontaneous at the onset and not iatrogenic. The only iatrogenic case was due to severe pre-eclampsia related to pre-existing maternal renal disease.
We also showed a statistically significant increase in the risk of perinatal death before adjustment for confounders. Interestingly, of the three cases of perinatal death in pregnancies with a SUA, one was in the infant with the SUA and two were in the unaffected co-twin. This raises the question whether the presence of SUA is an adverse predictor for the twin pregnancy as a whole, or if the increase in perinatal death was due to the earlier gestation at delivery. As controlling for gestational age reduced the odds of perinatal death, the latter is more likely.
The case-control methodology with strict inclusion criteria for individually matched, consecutive controls is a strength of our study. Another is the requirement for all patients to have been scanned at our tertiary referral center and histopathological confirmation of the diagnosis or expert review of the antenatal images. While these factors contribute to a more robust methodology, we are also limited by the small sample size. The relatively low rate of isolated SUA, even in a large tertiary referral center such as The Royal Women's Hospital, makes it difficult to undertake properly designed prospective studies without multicenter collaboration.
Our series thus has quite different findings to others that have commented on an increase in SGA for isolated SUA in twin pregnancies (Byers et al., Reference Byers, Saade and Harirah2013; Stout et al., Reference Stout, Obido, Longman, Shanks and Cahill2013). Klatt et al. in their series in 2012 commented on the trend to increased SGA, but this did not reach statistical significance. It is unclear why our findings are different; however, the strict methodology we have employed for both case and control identification and inclusion (as detailed above) may be one factor. The significantly increased risk of preterm birth in the cases in our study may also suggest that growth restriction occurs at a later gestation in these pregnancies; however, more data is required to definitively support such a hypothesis.
We conclude that isolated SUA increases the risk of preterm delivery <34 weeks but no other significant obstetric outcome, thus adding a degree of risk to an already high-risk pregnancy.
Acknowledgment
Funding from the Centre of Research Excellence Grant in Neonatal Medicine (National Health and Medical Research Council of Australia).





