Over the past 25 years there has been a significant change in the provision of services for people with intellectual disabilities. Large institutions have either closed or become much smaller in the UK, USA and other countries. Reference Anderson, Prouty and Lakin1 Many people with intellectual disabilities and mental health needs and/or challenging behaviour now live in their family home or in a variety of supported living options and psychiatric services are increasingly provided in the community. However, the most recent White Paper in England for people with intellectual disabilities 2 continues to recognise that at times an in-patient admission for the purposes of assessment and treatment may be necessary with a view to being discharged to their own homes once the symptoms have remitted.
The Health of the Nation Outcome Scales (HoNOS) were developed by the Royal College of Psychiatrists' Research Unit to measure the health and social functioning of people with severe mental illness, aiming to provide a means of recording progress towards the Health of the Nation target ‘to improve significantly the health and social functioning of mentally ill people’. Reference Wing, Curtis and Beevor3 Since their development in adults of working age they have been successfully adapted and validated for a number of psychiatric subspecialties, including psychiatry of old age (HoNOS-65+), forensic (HoNOS-Secure), children and adolescents (HoNOS-CA) and learning disabilities (HoNOS-LD). Reference Roy, Matthews, Clifford, Fowler and Martin4
The HONOS-LD has previously been used to evaluate a model for in-patient care of people with intellectual disabilities. Reference Hall, Parkes, Samuels and Hassiotis5 We have subsequently collected HoNOS-LD data on all service users admitted for assessment and/or management of mental disorders as a clinical outcomes indicator and in line with current National Health Service (NHS) policy for service quality monitoring. We report the results of analyses carried out and the issues that arose for clinical practice.
Method
HoNOS-LD scoring
The HoNOS-LD instrument can be used to detect changes (either improvement or deterioration) across periods of 4 or more weeks, with a maximum score of 88 accrued over 18 items. A minimum of 4 weeks duration of in-patient stay is required because the HoNOS-LD score is based on the previous 4 weeks' parameters. The HoNOS-LD glossary provides details on the ratings for each item, where scores range from 0 to 4, indicating no problem to a severe problem. Reference Roy, Matthews, Clifford, Fowler and Martin6
Inclusion and exclusion criteria
For a 19-month period, between July 2006 and February 2008, the HoNOS-LD was completed at admission and discharge for all in-patients with intellectual disabilities if the admission lasted more than 4 weeks. Eligible admissions lacking both an admission and discharge assessment were excluded. Assessments were performed only by clinicians attached to the specialist learning disabilities teams, who had received instruction by consultant trainers and with regular multidisciplinary team review of ratings to ensure reliability. High interrater reliability has been previously demonstrated. Reference Roy, Matthews, Clifford, Fowler and Martin4
Data collection
Total HoNOS-LD scores were recorded, and also specific clusters of scoring items were identified within the tool. Seven specific ‘clusters’ were identified within the HoNOS-LD through consensus opinion between clinicians based on the nature of the items being assessed. These clusters were:
-
• behavioural problems, items 1-3
-
• cognition, items 4 and 5
-
• communication, items 6 and 7
-
• mental state, items 8-11
-
• physical problems, items 12 and 13
-
• activities of daily living, items 14-16
-
• social functioning, items 17 and 18.
These were used for a further data analysis to identify changes in these specific areas.
Additional demographic and clinical data not included in the HoNOS-LD were also collected such as diagnosis, duration of stay, and status under the Mental Health Act.
Data analysis
Data were analysed using Wilcoxon's signed rank test for non-parametric paired data with SPSS version 16 on Windows. This was both for change in overall HoNOS-LD score and change in score of individual clusters. Raw data were used for analysis of change in total HoNOS scores, and for analysis of change within clusters. For graphic representation of the seven clusters, an adjustment to the data was made in order to allow the proportion of the overall HoNOS score that each cluster represented, for the following reasons: first, some clusters contained more individual items than others as can be seen; and second, question 3 is subdivided into five different parts (‘A-E’) and therefore has a higher total maximum score than the other items. The formula used for the standardisation of scores between clusters is as follows:
The significance level was set at 0.01 for more conservative estimates.
Results
Demographic data
At the time of analysis, the data included details on 33 admissions for 24 service users. Their length of admission varied from 3 to 505 days, with a median of 92 days and an average duration of 80 days. Only two admissions were of service users not previously known to the service. Of the 33 admissions, 13 were for a period of less than 28 days and were excluded. Of the remainder, five did not have paired HoNOS-LD scores due to missing data and were also excluded. Data from 15 individuals with paired HoNOS-LD scores were included in the analyses. The mean age of individuals was 37 years (range 24-65). Demographic information for admissions meeting inclusion criteria is shown in Table 1.
Table 1 Demographic and clinical data for admissions meeting inclusion criteria

| Admissions n (%) | |
|---|---|
| Gender | |
| Female | 9 (60) |
| Male | 6 (40) |
| Accommodation on admission | |
| Independent | 5 (33.3) |
| Family home | 5 (33.3) |
| Supported | 3 (20) |
| Unrecorded | 2 (13.3) |
| Degree of intellectual disability | |
| Mild | 13 (86.7) |
| Moderate | 2 (13.3) |
| Severe and profound | 0 (0) |
| Diagnosis | |
| Psychotic disorders | 6 (40) |
| Affective disorders | 4 (26.7) |
| Other (substance misuse/organic/unclear) | 5 (33.3) |
| Mental Health Act status during admission | |
| Informal | 3 (20) |
| Detained under Section 2 | 2 (13.3) |
| Detained under Section 3 | 10 (66.7) |
Total HoNOS-LD scores
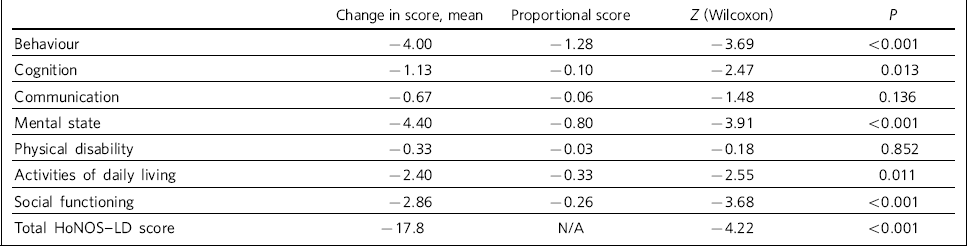
The mean of total HoNOS-LD scores was 28.8 on admission (range 10-44) and 11 on discharge (range 4-31). The mean change in score was −17.8 (range −6 to −28). For all data-sets there was a significant improvement in HoNOS-LD score at the time of discharge (P<0.001) (Table 2).
Table 2 Health of the Nation Outcome Scales for People with Learning Disabilities (HoNOS–LD) scores data analysis
| Change in score, mean | Proportional score | Z (Wilcoxon) | P | |
|---|---|---|---|---|
| Behaviour | −4.00 | −1.28 | −3.69 | <0.001 |
| Cognition | −1.13 | −0.10 | −2.47 | 0.013 |
| Communication | −0.67 | −0.06 | −1.48 | 0.136 |
| Mental state | −4.40 | −0.80 | −3.91 | <0.001 |
| Physical disability | −0.33 | −0.03 | −0.18 | 0.852 |
| Activities of daily living | −2.40 | −0.33 | −2.55 | 0.011 |
| Social functioning | −2.86 | −0.26 | −3.68 | <0.001 |
| Total HoNOS–LD score | −17.8 | N/A | −4.22 | <0.001 |
HoNOS-LD cluster scores
All 15 cases with recorded HoNOS-LD scores for admission and discharge contained item-specific scores and paired data were analysed using the cluster method with adjustment as described above (Table 2). All clusters showed improvements following admission. These are represented graphically in Fig. 1. Significant improvements were observed in behaviour, mental state and social functioning domains. Trends towards improvement were also seen in the activities of daily living and cognition domains.

Fig 1 Proportional change in adjusted mean scores of the Health of the Nation Outcome Scales for People with Learning Disabilities clusters. ADL, activities of daily living.
Discussion
Following changes in the way in which individuals with intellectual disability are cared for by mental health services, there has been little evidence-based guidance to quantify the ways in which in-patient admission may be of benefit. Reference Bouras and Holt7 In this outcomes analysis we have been able to show initial findings that suggest that certain domains of function may respond well to in-patient admission. Although our data are based on a small sample of admissions, the similarity of trends in results between each data-set suggests that these were not chance findings. The service is representative of psychiatric morbidity in two inner London boroughs with a combined population of over 300 000.
The HoNOS-LD has been designed and validated as a suitable tool to monitor response to treatment in individuals with intellectual disability. Reference Roy, Matthews, Clifford, Fowler and Martin4 Its use as a quality-outcome indicator has been advocated elsewhere Reference Campbell8 and there is a growing body of published data where it has been used either in part Reference Prakash, Andrews and Porter9 or in its entirety. Reference Banerjee, Morgan, Lewis, Rowe and White10-Reference Webb and Reid12 We present data that provide further support for its use to monitor outcomes during in-patient admissions. The HoNOS has also been extensively and successfully validated in other psychiatric subspecialties, including old age, children and adolescents, adults of working age, adults with brain injury and forensic settings. Reference Hallam, Beecham, Knapp, Carpenter, Cambridge and Forrester-Jones13 Further, it has high interrater reliability and measures a broad range of clinical outcome indicators. Domains of clinical function were identified by consensus to allow broad areas of change to be identified and to enable the data to be analysed.
It has previously been demonstrated that although psychiatric morbidity is similar in both individuals in the community and those who are in-patients, significantly higher risks are associated with in-patient populations. Reference Hall, Parkes, Samuels and Hassiotis5 In our analysis a number of statistically significant outcomes have been clearly identified in several relevant domains, demonstrating that in-patient stay is associated with significant improvements in behaviour, mental state and social functioning. These factors are interdependent, and should be the focus of treatment for mental illness. Such improvements are likely to be a consequence of interventions that occur more intensively in an in-patient setting such as support by trained staff, occupational therapy, psychological therapies and medication. In addition, the HONOS-LD is able to clearly and effectively demonstrate change in these factors in response to treatment, and thus can be used to monitor the response and outcomes of people with intellectual disabilities admitted to mental health units.
We also saw trends towards improvement in activities of daily living and cognition. Improvements in activities of daily living may be attributable to a number of factors. First, prevailing mental state would have an impact on these activities and therefore improve concurrently. Second, the more intensive therapeutic interventions as described above during in-patient episodes may also explain improvements in this domain. The trend in the cognition domain may be the result of improvements in cognition secondary to treatment of the mental illness (e.g. reduction of depressive symptoms) or improvement in psychosis related to non-convulsive status epilepticus. However, the cognition domain in HoNOS-LD is a very blunt instrument and further investigation of this would be required through formal cognitive testing, which was beyond the scope of the present work.
The most recent Mansell Report emphasises the importance of commissioning appropriate services for people with intellectual disabilities who present with challenging behaviour. Reference Pirkis, Burgess, Kirk, Dodson, Coombs and Williamson14 Our results indicate that behavioural disturbance associated with mental disorders shows significant improvements following a period of in-patient treatment. Treatment in a hospital setting therefore appears to be an appropriate, cost-effective short-term intervention for adults with intellectual disabilities with challenging behaviour associated with acute mental disorders. The availability of specialist learning disability in-patient beds therefore need to be part of commissioning strategies for people with intellectual disabilities who present with challenging behaviour.
The systematic use of HoNOS-LD may be a solution to the potential problems of applying payment-by-results to the intellectual disabilities services through providing a potential currency. Arguably, the complexity of psychiatric presentation, interplay of physical and mental health and other comorbidities in people with intellectual disabilities can complicate the recording of information as well as compromising the accuracy of the data on each patient episode. 15 Therefore, a tool that can be useful in the assessment and identification of clinical change in people with intellectual disabilities both in community and in-patient settings is of great importance. Our results have indicated domains of ‘dynamic’ and ‘static’ function in relation to at least in-patient admission. The scores of particular clusters may be of use in guiding treatment during admissions as well as for treatment in the community. Other professionals may also be able to use the HoNOS-LD if trained and thus improve monitoring of the mental state as well as ensuring recognition and rating of mental health-related needs with increased precision.
We would like to emphasise its ease of use and its value in the identification of relevant areas of clinical function, and would encourage other teams working with service users with intellectual disabilities to use it.
Acknowledgements
We acknowledge the assistance of Dr Adrian Lambourne with statistical analysis (Information Manager, Hertfordshire Primary Care Trusts).






eLetters
No eLetters have been published for this article.