People with severe personality disorders do not easily find their way into treatment. Reference Bateman and Tyrer1 Many may go unnoticed owing to limited detection by health providers, Reference Links, Boiago, Allnut and Links2 resulting in patients not receiving specialised therapy. Reference Andrews3–Reference Stone5 Even when such increasingly effective therapies are indicated, Reference Adshead6–Reference Leichsenring and Leibing7 not all patients profit from them because of limited availability or suitability. Apart from notable differences in their implementation, our own experience with referral to and working in these specialised therapies is that in many cases the therapies are not indicated or the patients fail to enter treatment, drop out or fail to improve. Some patients have limited motivation or capacities, have an abundance of social problems that prevent therapy taking place properly, behave in an overly disruptive manner or lack the stability to attend sessions regularly. In a large group of patients with severe personality disorders, those of lower socioeconomic status and with more impaired psychosocial functioning were more likely to receive residential, day and psychopharmacological treatment than intensive individual, couple or group psychotherapy. Reference Binks, Fenton, McCarthy, Lee, Adams and Duggan8
A general form of treatment may then be offered to these patients: community mental healthcare (CMHC). This is a community-based, long-term treatment within a supportive atmosphere aimed at stability rather than change. Although referred to as ‘good clinical care’, Reference Andrews3,Reference Zanarini, Frankenburg, Hennen and Silk9 it is largely unclear if CMHC is ‘good’. On the contrary, in daily practice it is often associated with long-term care lacking clear aims and therapeutic ambitions, Reference Dowson and Grounds10 possibly resulting in unnecessary dependency. In addition, negative professional attitudes towards patients with personality disorders have been reported frequently, Reference Craddock, Antebi, Attenburrow, Bailey, Carson and Cowen11–Reference Lewis and Appleby13 possibly resulting in an ineffective patient–professional interaction, especially in long-term supportive care. Therefore, we aim to answer the following questions in this review: what, exactly, is CMHC for severe personality disorder; who provides it; how does it compare with other forms of treatment for this disorder; what are its empirical and theoretical underpinnings; and what are its strengths and limitations?
Method
The search strategy consisted of three successive phases, owing to limited findings in the previous phases. First, a systematic search of general databases was conducted. Second, control conditions of experimental treatments of personality disorder treatments were searched. Third, textbooks and cross-references were used to obtain a broader scope.
A search of the Medline and PsycINFO databases was conducted for publications in English between 1980 (when Axis II was introduced in the DSM–III) and May 2006. Owing to the lack of a clear search term for CMHC, a broad search strategy was designed. The MeSH headings ‘personality disorders’ AND (‘community mental health service’ OR ‘counseling’ OR ‘ambulatory care’ OR ‘nursing care’ OR ‘long-term care’ OR ‘case management’ OR ‘social work’ OR ‘psychiatric social work’ OR ‘day care’ OR ‘rehabilitation’ OR ‘supportive therapy’ [the last as a title word]) were used. The main inclusion criteria were that the article had to have a psychosocial treatment of personality disorders as its main subject and be written in English. Exclusion criteria were descriptions or evaluations of manualised specialised psychotherapy for personality disorder; interventions with juveniles (under 18 years old) or those over 65 years of age; and interventions in a non-psychiatric setting (e.g. a general hospital). Although over a thousand references were retrieved, only 20 met these criteria. For this reason, an additional search strategy was designed. A meta-analysis of psychotherapy outcomes for personality disorders and a recent Cochrane systematic review of psychotherapies for borderline personality disorder were analysed to detect studies that possibly described CMHC as the control condition. Reference Bateman and Tyrer1,Reference Links, Boiago, Allnut and Links2 No other more recent meta-analyses or Cochrane reviews of this field were available at the time this search took place.
Of the total 26 studies analysed, 7 described the control condition (‘treatment as usual’) in enough detail to be of use. The remaining 19 studies did not aim at severe personality disorder, did not have a control condition, described a second psychotherapeutic treatment as the control condition or described the control condition only vaguely. Since these control conditions were only described and not explained in detail, we hand-searched recent textbooks on personality disorders – retrieved on the internet by combining ‘personality disorders’ with ‘management’ and (‘handbook’ or ‘textbook’ or ‘guide’ or ‘manual’) – for chapters or texts on non-psychotherapeutic treatments. Additionally, we used cross-references to extend findings and broaden our understanding of the subject.
Results
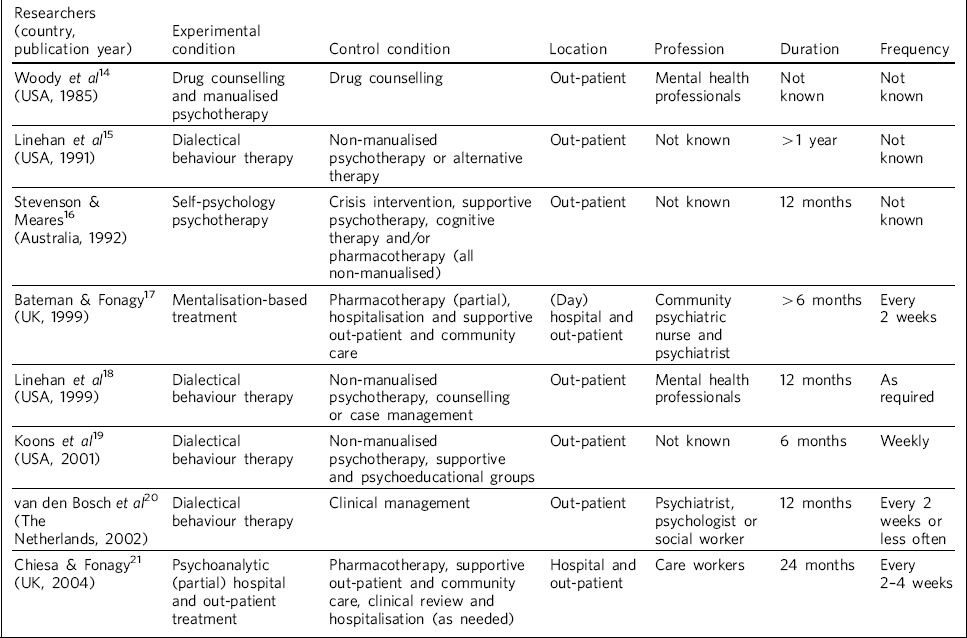
In the search conducted, no single paper was devoted to the description of what might be considered as standard community care for severe personality disorder. Our additional search strategy yielded eight descriptions of ‘treatment as usual’ (Table 1), Reference Deans and Meocevic14–Reference Koons, Robins, Tweed, Lynch, Gonzalez and Morse21 based on which we draw some tentative conclusions. Community mental healthcare is most often offered on an out-patient basis, every 2 weeks on average, lasting 6–24 months. It is not formalised or manualised but consists of an eclectic mix of different modalities. It has a supportive character that seems more closely linked to care and psychosocial support than to psychotherapy. It is most often offered by general mental health professionals (not psychotherapists). Formal goals of CMHC are not acknowledged in the literature retrieved, yet they seem to be centred around not making things worse, offering a certain holding to the patient and keeping things under control. Reference Zanarini, Frankenburg, Hennen and Silk9 It appears relatively universal across Western psychiatry, since studies originated from different parts of the world (Australia, Europe and North America).
Table 1 Control conditions describing community mental healthcare (‘treatment as usual’)
| Researchers (country, publication year) | Experimental condition | Control condition | Location | Profession | Duration | Frequency |
|---|---|---|---|---|---|---|
| Woody et al Reference Deans and Meocevic14 (USA, 1985) | Drug counselling and manualised psychotherapy | Drug counselling | Out-patient | Mental health professionals | Not known | Not known |
| Linehan et al Reference Newton-Howes, Weaver and Tyrer15 (USA, 1991) | Dialectical behaviour therapy | Non-manualised psychotherapy or alternative therapy | Out-patient | Not known | >1 year | Not known |
| Stevenson & Meares Reference Woody, McLellan, Luborsky and O'Brien16 (Australia, 1992) | Self-psychology psychotherapy | Crisis intervention, supportive psychotherapy, cognitive therapy and/or pharmacotherapy (all non-manualised) | Out-patient | Not known | 12 months | Not known |
| Bateman & Fonagy Reference Linehan, Armstrong, Suarez, Allmon and Heard17 (UK, 1999) | Mentalisation-based treatment | Pharmacotherapy (partial), hospitalisation and supportive out-patient and community care | (Day) hospital and out-patient | Community psychiatric nurse and psychiatrist | >6 months | Every 2 weeks |
| Linehan et al Reference Stevenson and Meares18 (USA, 1999) | Dialectical behaviour therapy | Non-manualised psychotherapy, counselling or case management | Out-patient | Mental health professionals | 12 months | As required |
| Koons et al Reference Bateman and Fonagy19 (USA, 2001) | Dialectical behaviour therapy | Non-manualised psychotherapy, supportive and psychoeducational groups | Out-patient | Not known | 6 months | Weekly |
| van den Bosch et al Reference Linehan, Schmidt, Dimeff, Craft, Kanter and Comtois20 (The Netherlands, 2002) | Dialectical behaviour therapy | Clinical management | Out-patient | Psychiatrist, psychologist or social worker | 12 months | Every 2 weeks or less often |
| Chiesa & Fonagy Reference Koons, Robins, Tweed, Lynch, Gonzalez and Morse21 (UK, 2004) | Psychoanalytic (partial) hospital and out-patient treatment | Pharmacotherapy, supportive out-patient and community care, clinical review and hospitalisation (as needed) | Hospital and out-patient | Care workers | 24 months | Every 2-4 weeks |
Professionals providing community mental healthcare
From a number of studies we may tentatively conclude that mental health professionals from different backgrounds, without formal psychotherapeutic training, offer CMHC. Reference Deans and Meocevic14–Reference Koons, Robins, Tweed, Lynch, Gonzalez and Morse21 This would be consistent with daily practice noticed in different countries, where care is offered from busy non-specialised mental health centres. Reference Andrews3,Reference van den Bosch, Verheul, Schippers and van den Brink22 From an English study it was concluded that the case-loads of community psychiatric nurses and occupational therapists in community mental health teams contained far more patients with personality disorders (67%) than did those of psychiatrists and psychologists (35%). Reference Chiesa, Fonagy, Holmes and Drahorad23 In a comparable study, it was social workers and again occupational therapists who treated most people with personality disorder. Reference Burns, Sampson, McCubbin and Tyrer24 A possible explanation is that patients with severe personality disorders are treated by the professionals with the lowest threshold for inclusion in their case-load (i.e. non-psychotherapists). Support for this hypothesis is offered by the large percentage of patients with severe personality disorders among the case-loads of community psychiatric nurses and occupational therapists: twice as many as among psychiatrists and psychologists (31% v. 15%). Reference Chiesa, Fonagy, Holmes and Drahorad23 Although these professions may be the principal providers of CMHC, they are virtually absent from the literature on severe personality disorders (e.g. in a guide on personality disorders and community mental health teams, they did not author a single chapter). Reference Keown, Holloway and Kuipers25
Relation to other treatments
We conclude from the above that CMHC is an eclectic treatment, combining elements of different therapeutic approaches (especially cognitive–behavioural and supportive therapy), crisis management and pharmacotherapy. It resembles the ‘psychiatric management’ described in the American Psychiatric Association's guideline on borderline personality disorder. Reference Greenwood, Chisholm, Burns and Harvey26 Its principles are:
-
• responding to crises and monitoring safety;
-
• establishing and maintaining a therapeutic framework and alliance;
-
• providing education about the disorder and its treatment;
-
• coordinating the treatment effort;
-
• monitoring and reassessing the patient's clinical status and treatment plan.
However structured this may look, no treatment form is described as such and in daily practice decisions may be made on a much more ad hoc basis.
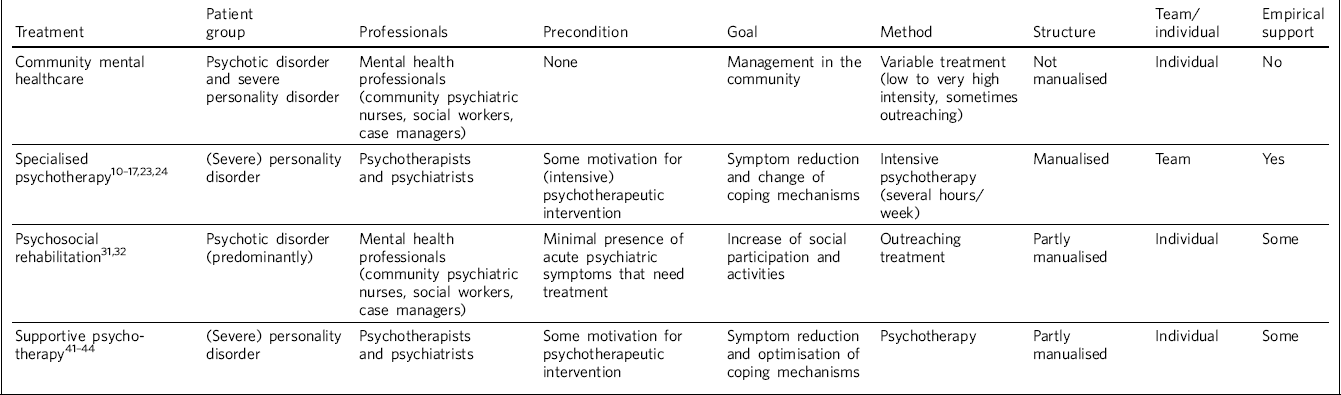
Community mental healthcare differs from psychotherapy and psychosocial rehabilitation in several ways (Table 2). The distinct empirically supported psychotherapies focus on internal psychological processes such as increased emotion regulation (dialectical behaviour therapy), Reference Newton-Howes, Weaver and Tyrer15 change of maladaptive schemas (schema-focused therapy), Reference Sampson, McCubbin and Tyrer27 increased mentalisation (mentalisation-based therapy), Reference Linehan, Armstrong, Suarez, Allmon and Heard17 or integration of internal mental representations (transference-focused therapy). 28 If CMHC is carefully and successfully carried out, patients may move on to one of these programmes, if available. Reference Giesen-Bloo, van Dyck, Spinhoven, van Tilburg, Dirksen and van Asselt29 Psychosocial rehabilitation programmes, on the other hand, focus more on social functioning and aim at increased social participation and activities. Originally designed for people with psychotic disorders, rehabilitative approaches are described increasingly frequently in cases of personality disorder. From different international perspectives, a professional attitude of acceptance of, and coping with, chronic problems is described. Reference Clarkin, Levy, Lenzenweger and Kernberg30–Reference Paris34 The extension of psychosocial rehabilitation to this group of patients is not without trouble, however. Many professionals do not know how to work well with these patients: they find the working alliance with patients with personality disorders more complex than with patients with psychosis (who mostly receive psychosocial rehabilitation). Reference Paris34 Likewise, people with (severe) personality disorder as a primary diagnosis are rarely represented in psychosocial rehabilitation or assertive community treatment programmes, Reference Links35–Reference Krawitz and Watson37 or are more likely to drop out. Reference Nehls38
Table 2 Treatment modalities associated with (severe) personality disorder
| Treatment | Patient group | Professionals | Precondition | Goal | Method | Structure | Team/individual | Empirical support |
|---|---|---|---|---|---|---|---|---|
| Community mental healthcare | Psychotic disorder and severe personality disorder | Mental health professionals (community psychiatric nurses, social workers, case managers) | None | Management in the community | Variable treatment (low to very high intensity, sometimes outreaching) | Not manualised | Individual | No |
| Specialised psychotherapy Reference Dowson and Grounds10-Reference Linehan, Armstrong, Suarez, Allmon and Heard17,Reference Chiesa, Fonagy, Holmes and Drahorad23,Reference Burns, Sampson, McCubbin and Tyrer24 | (Severe) personality disorder | Psychotherapists and psychiatrists | Some motivation for (intensive) psychotherapeutic intervention | Symptom reduction and change of coping mechanisms | Intensive psychotherapy (several hours/week) | Manualised | Team | Yes |
| Psychosocial rehabilitation Reference Gunderson, Gratz, Neuhaus, Smith, Oldham, Skodol and Bender31,Reference Livesley32 | Psychotic disorder (predominantly) | Mental health professionals (community psychiatric nurses, social workers, case managers) | Minimal presence of acute psychiatric symptoms that need treatment | Increase of social participation and activities | Outreaching treatment | Partly manualised | Individual | Some |
| Supportive psychotherapy Reference Ranger, Methuen, Rutter, Rao and Tyrer41-Reference Hoffman, Fruzetti, Oldham, Skodol and Bender44 | (Severe) personality disorder | Psychotherapists and psychiatrists | Some motivation for psychotherapeutic intervention | Symptom reduction and optimisation of coping mechanisms | Psychotherapy | Partly manualised | Individual | Some |
In textbooks on personality disorders, some treatment elements (although not CMHC in general) are described in more detail: psychoeducational approaches, Reference Barton39,Reference Twamley, Jeste and Lehman40 supportive therapy, Reference Ranger, Methuen, Rutter, Rao and Tyrer41,Reference Cohen, Edstrom and Smith-Papke42 and general treatment considerations. Reference Ruiz-Sancho, Smith, Gunderson and Livesley43,Reference Hoffman, Fruzetti, Oldham, Skodol and Bender44 Supportive psychotherapy, which aims at adaptation (a concept discussed below in more detail) is the most researched of these. Reference Winston, Rosenthal, Muran and Livesley45–Reference Livesley47 Some empirical support exists for it in general, Reference Dawson and Links48,Reference Aviram, Hellerstein, Gerson and Stanley49 and for cluster B and C personality disorders in particular. Reference Appelbaum, Oldham, Skodol and Bender46,Reference Livesley47 Some authors suggest that supportive therapy might be the treatment of choice with patients with severe personality disorders. Reference Ranger, Methuen, Rutter, Rao and Tyrer41,Reference Winston, Rosenthal, Muran and Livesley45,Reference Appelbaum, Oldham, Skodol and Bender46 Other studies emphasise the adaptive element in the treatment of severe personality disorder and offer some instructions on specific areas: adjusting environmental factors, Reference Hellerstein, Rosenthal, Pinsker, Samstag, Muran and Winston50,Reference Piper, Joyce, McCallum and Azim51 offering vocational training, Reference Rockland52 and installing supportive milieus. Reference Holmes53 Practical matters such as the optimal frequency of appointments, managing ‘no-show’ and indication criteria for hospitalisation are not addressed in either approach.
Theoretical and empirical base of community mental healthcare
The aforementioned issues may be resolved through the use of a theoretical framework, yet none of the articles retrieved contained any data about theoretical or empirical support for CMHC. Although the supportive therapy mentioned above differs significantly from CMHC in that it is more formalised and strict (e.g. weekly appointments for a given number of weeks) and requires at least some motivation for a change-oriented treatment, its theoretical concept may apply to CMHC as well. The theoretical base of supportive therapy lies in an adaptive concept: the therapist ensures the safety of the patient by being non-judgemental, by supporting effective defence mechanisms, by focusing on the real relationship instead of on transference phenomena, and by reframing negative experiences into more positive meanings. Transference is then analysed only when it obstructs treatment. This description, although not derived from the CMHC literature, fits in with our previous general description of CMHC, as well as with aforementioned adaptive approaches. Community mental healthcare offers a supportive rather than a confrontational atmosphere and also focuses on the ‘here and now’. The difference lies in its final aim, which in supportive therapy is individual change, whereas in CMHC it is management in the community and preservation of a certain quality of life.
Strengths and limitations of community mental healthcare
Community mental healthcare may be regarded as a highly humane form of help for particularly vulnerable individuals, as expressed through the term ‘good clinical care’. Reference Andrews3,Reference Zanarini, Frankenburg, Hennen and Silk9 For example, patients who are frequently (para)suicidal are usually not welcome in other branches of social or mental healthcare, thus CMHC may be the only service that supports these patients. It may be argued that if these patients could not seek some refuge in mental healthcare they would become marginalised even further. The validity of this argument is somewhat undermined by recent data on the natural course of borderline personality disorder. This research, showing diminishing symptoms over a 10-year period, Reference Tyrer54 suggests that intrusive interventions by mental health professionals may not always be indicated. Also, rapid remissions that could not be completely related to treatment gains have been seen in some patients with borderline personality disorder. Reference Tyrer, Sensky and Mitchard55 However, in neither of these studies could the positive (or negative) attributions of therapy to remission be assessed empirically. Although treatment is obviously helpful in most cases, it cannot be concluded that treatment is always necessary or better than no treatment.
Discussion
First of all, we must state that this review has some limitations: we are not sure to what extent the indirect information about CMHC is reliable. It may be that CMHC is very different from setting to setting and even from professional to professional. Another limitation is the lack of differentiation between the accessibility of different systems of psychiatric care across Western countries. Because of local funding principles, CMHC may be quite inclusive in some regions and virtually absent in others. Although we know from personal experience and inter-collegiate contacts that these differences exist, we could not trace them in the literature. Owing to the limited literature and even more limited research, the conclusions of this review must be considered as preliminary.
From our results we conclude that CMHC lacks a clear description and both solid empirical and theoretical grounds. The lack of evidence does in itself not mean that CMHC has no relevance or quality, but does make it susceptible to debate. Since CMHC has only served as a control condition in research thus far, it has not been established for whom and when it may work. The studies reviewed here show different outcomes: both positive and negative as well as undecided or hard to interpret. As such, we cannot be definitive about CMHC apart from the observation that a treatment that appears to be harmful in some cases needs to be indicated carefully. Once indicated, we believe CMHC would profit from meeting some basic requirements.
Iatrogenic damage
The main argument to consider carefully when assessing the suitability of CMHC for patients with severe personality disorder is the risk of iatrogenic damage, opposed to the chance of (sometimes spontaneous) remission. Current opinion is that people with the single most prominent personality disorder (borderline) do not always profit more from bad care than from no care at all. Reference Rockland52–Reference Tyrer54 Community mental healthcare, which could potentially be provided ‘several times a week’ (Dowson & Grounds: Reference Zanarini, Frankenburg, Hennen and Silk9 p. 276) ‘on an indefinite basis’ (ibid: p. 278) may foster unnecessary dependence on psychiatric care in the patient. Reference Zanarini, Frankenburg, Hennen and Silk9 Iatrogenic damage may also consist of serious (physical) damage from multiple or lengthy hospitalisations aimed at preventing suicide, yet paradoxically exacerbating it. Reference Hennessey and McReynolds59 Such damage is observed more often in CMHC than in specialised care. Reference Appelbaum and Munich60 With regard to other personality disorders, equal doubts about the need for support and the risk of dependency have been expressed. Reference van den Bosch, Verheul, Schippers and van den Brink22,Reference Hoffman, Fruzetti, Oldham, Skodol and Bender44 If some patients actually become worse through CMHC, its indication for any patient should be carefully considered. Moreover, owing to the often turbulent course of treatment and the difficulties of the patients involved, interpersonal problems between patients and professionals easily arise in CMHC. As staff members are not always specifically trained in the management of such (counter)transference, and community mental health centres tend to be busy and somewhat overburdened institutions, Reference Keown, Holloway and Kuipers25,Reference Zanarini, Frankenburg, Hennen, Reich and Silk61–Reference Gunderson, Bender, Sanislow, Yen, Rettew and Dolan-Sewell63 adverse reactions are likely. In particular, staff who primarily work with major Axis I disorders (e.g. psychotic disorders, in which interpersonal issues are of a different kind) may be unpleasantly surprised by the impact of working with people with severe personality disorder. Reference Appelbaum and Munich60 The centre's structure and culture may not be prepared for intensive supervision or consultation with regard to these patients.
Possible improvements
Community mental healthcare would, in our view, greatly benefit from some alterations. First, it should have a solid structure. The current practice of intermittent reinforcement of intensive crisis intervention, combined with relatively little or no care during calmer periods, may be the very perpetuator of the dependency loathed by many (e.g. British psychiatrists who recently stated that patients may expect more than just ‘non-specific psychosocial support’). Reference Dowson and Grounds10 Improvement of the structure and predictability (including, for instance, mutual goal-setting, treatment contracting and limit-setting) of CMHC might prevent this. Second, from two highly researched psychotherapies for severe borderline personality disorder (dialectical behaviour therapy and mentalisation-based therapy) it may be concluded that a team approach is preferable to an individual one. In such a cooperative framework, it is highly important that professionals working with patients with severe personality disorders are in some way able to express their feelings about patient contacts. Although hardly surprising, and obviously relevant for any form of treatment for personality disorders, this is often overlooked in CMHC. Professionals providing CMHC are often not psychotherapeutically trained and may lack the routine of looking at their own role in the therapeutic encounter. Reference Fonagy and Bateman65 Therefore, supervision should be provided within the (treatment) structure of the team. Reference Dawson and Macmillan66 Third, not every individual is suited to work with people with severe personality disorder. Gunderson et al concluded, having studied 752 clinicians, that ‘some psychiatrists, many social workers and most nurses’ consider themselves incompetent with patients with borderline disorder (p. 248). Reference Giesen-Bloo, van Dyck, Spinhoven, van Tilburg, Dirksen and van Asselt29 Considering that CMHC is often provided by social workers and community psychiatric nurses, assigning patients with severe personality disorder at random to a community mental health professional may be unwise. Awareness of each team member's abilities and limitations may help in such cases. Furthermore, research shows that training may be effective in improving both professionals' knowledge of these patients and their attitudes towards them. Reference Gunderson67,Reference Paris68
Implications for research and practice
Although our results are limited in both quantity and quality, we may draw some preliminary conclusions from this review. Community mental healthcare may profit from more structure than it currently has. It should not ignore social problems, while maintaining a working alliance that fosters clients' independence and responsibility. A team approach that enables mutual support and supervision and matches patients to professionals might further improve quality, just as focused training might do. An integration of useful elements of specialised psychotherapy and psychosocial rehabilitation might serve CMHC well. Such an integrative programme should combine the specific elements of the former (e.g. management of patient–professional interaction, explanatory model of personality disorders) with those of the latter (e.g. long-term goal-setting, strategies to enhance social participation).
Funding
This study was made possible by financial support from ZonMw (Geestkracht program, grant 100-002-031), Altrecht Mental Health Care, De Gelderse Roos Mental Health Care and Inholland University, Amsterdam, The Netherlands.





eLetters
No eLetters have been published for this article.