Introduction
Common mental health conditions such as depression and anxiety disorders affect approximately one in six people in the UK at any one time, causing substantial personal and economic burden (Kessler et al., Reference Kessler, Chiu, Demler and Walters2005; Office for National Statistics, 2009). Although effective treatment for common mental health conditions exists, gaining access to treatment may be problematic (Office for National Statistics, 2009). Despite efforts to train more therapists, and make treatment more accessible, demand for psychological therapies by far outstrips supply (Andersson, Reference Andersson2016). One-to-one therapy is labour intensive, costly, and inherently limited in terms of the number of patients that can be seen at any one time (Lovell and Richards, Reference Lovell and Richards2000; Stallard et al., Reference Stallard, Richardson and Velleman2010). Given that access to the internet is becoming nearly ubiquitous in the UK, with almost 80% of individuals aged over 18 years now accessing the internet daily (Office for National Statistics, 2015), offering computerized CBT via the internet has been proposed as an innovative way to begin meeting the demand for evidence-based psychological therapies in the population.
What is computerized CBT (cCBT and eCBT/iCBT)?
Computerised CBT (cCBT) refers to any CBT intervention delivered via a computer programme. CBT's structured approach has already been adapted for manualized self-help interventions which require minimal therapist contact, and so seems suitable for internet-delivered therapy (Perle et al., Reference Perle, Langsam, Randel, Lutchman, Levine, Odland and Marker2013). Clients typically log in to a web portal and work through a set of interactive modules that may include videos, written exercises and quizzes. Although there are packages that are designed to be delivered without any therapist support, high attrition limits the use of this format in clinical settings (Richards and Richardson, Reference Richards and Richardson2012). Therefore, most packages now include therapist support in the form of asynchronous messaging (i.e. written feedback on exercises, progress reviews and problem-solving), or telephone support (Andersson, Reference Andersson2016). This approach has been termed ‘eCBT’ or ‘iCBT’ in the literature. It still allows a far greater number of patients to receive treatment than would be possible in face-to-face or ‘online’ therapy (CBT over Skype or synchronous chat), while attempting to mitigate the issue of client drop-out (Richards and Richardson, Reference Richards and Richardson2012).
SilverCloud
One specific eCBT package used in several IAPT services is SilverCloud (Sharry et al., Reference Sharry, Davidson, McLoughlin and Doherty2013). Clients are sent log-in details by their allocated Psychological Wellbeing Practitioner (PWP) and encouraged to work through a set of 8–10 online modules that are matched to address their difficulties, at their own pace. Currently, treatment programmes are available for depression, anxiety and depression, generalized anxiety, panic, health anxiety, phobia, social anxiety and obsessive compulsive disorder (OCD). In addition, there is the option to ‘add on’ more general modules, for example a module on sleep or stress. Programmes can also be individualized based on a client's needs (Sharry et al., Reference Sharry, Davidson, McLoughlin and Doherty2013).
Each module takes about 40 minutes to complete. Content is based on CBT, and includes psychoeducation on understanding the link between thoughts, feelings and behaviours; exercises including thought challenging; and behavioural experiments. Modules are intended to be accessed in order, and clients are encouraged to complete one module weekly to allow space for homework and practice. However, modules can also be accessed in any order and within any timeframe, which has been shown to maintain motivation and engagement (Sharry et al., Reference Sharry, Davidson, McLoughlin and Doherty2013). Clients have access to the programme for one year after completion, which may help with relapse prevention (Richards and Suckling, Reference Richards and Suckling2009).
Therapists support clients by logging into the programme and reviewing clients’ progress, providing personalized encouragement and support. In addition, clients complete weekly standardized symptom measures of depression and anxiety routinely collected in IAPT services.
What is the evidence base for eCBT?
A recent systematic review and meta-analysis of 13 studies (N = 1053) compared eCBT with face-to-face CBT (either individual, n = 6 studies or group format, n = 7 studies; Andersson et al., Reference Andersson, Cuijpers, Carlbring, Riper and Hedman2014). Studies covered a range of conditions, including social anxiety disorder, panic disorder, depression, specific phobias, body dissatisfaction, tinnitus, and male sexual dysfunction. Results indicated that effect sizes of eCBT were comparable to those of face-to-face interventions, with eCBT for social anxiety even slightly outperforming face-to-face interventions. Client acceptability was high, and effects were maintained after adjusting for participant drop-out. Although samples in all studies included in this meta-analysis were self-selected, and may therefore not be entirely reflective of clinical populations, clients embarking on eCBT in everyday clinical settings will still have agreed to this treatment modality. Trials were small, yet of high quality and with low risk of bias, which also gives more confidence in the current findings. Results from this meta-analysis are also in line with those from earlier reviews (Cuijpers et al. Reference Cuijpers, Donker, van Straten, Li and Andersson2010; Newman et al. Reference Newman, Szkodny, Llera and Przeworski2011), comparing guided self-help interventions (including eCBT) with face-to-face interventions, which suggested that CBT can be delivered successfully with minimal therapist contact over the internet. Overall, evidence to date thus suggests that eCBT can be acceptable to clients and have efficacy comparable to face-to-face ‘high-intensity’ CBT for clients who have chosen to engage with this type of therapy. There are, however, limitations to this body of research which prevent drawing firmer conclusions. For example, individual studies are often underpowered to detect differences; the most recent meta-analysis falls one study short of its own power calculation; CBT control conditions include group, not just individual, therapy; and differences in treatment content (between different online programmes) and patient characteristics are not controlled for nor taken into account (Andersson et al., Reference Andersson, Cuijpers, Carlbring, Riper and Hedman2014). Nonetheless, there is good enough evidence such that eCBT has been recommended by NICE as a treatment modality for common mental health conditions (National Collaborating Centre for Mental Health (Great Britain) and Royal College of Psychiatrists, 2011).
What is the current uptake of eCBT?
However, despite a relatively strong emerging evidence base for the efficacy, cost-effectiveness and client acceptability of eCBT, uptake in clinical settings can be slow (Andersson, Reference Andersson2016). Although IAPT services are now encouraged to offer internet-based interventions to a substantial proportion of their clients, this can prove difficult to achieve. An internal audit of the IAPT service in which this study was carried out showed that only 12% of clients had tried SilverCloud, whereas the service model encourages a target closer to 30%. This is problematic if it results in resources being used inefficiently and delays patients receiving an evidence-based treatment (as waiting lists for face-to-face CBT are typically longer than the immediately accessible eCBT).
One barrier to implementation may be negative therapist attitudes to eCBT which may affect whether they offer it as a treatment modality to clients, but little research has explored this topic. Previous research on therapist attitudes has been conducted on cCBT (computerized CBT without clinician support). There is some evidence to suggest that mental health workers’ knowledge of cCBT is often poor, and misinformation is common (Wells et al., Reference Wells, Mitchell, Finkelhor and Becker-Blease2007; Du et al., Reference Du, Quayle and Macleod2013). Stallard et al. (Reference Stallard, Richardson and Velleman2010) found cautious, yet positive attitudes of clinicians towards the use of cCBT with children and adolescents. The authors identified the perceived lack of a therapeutic relationship and associated support as the biggest barrier to offering cCBT to clients. Donovan et al. (Reference Donovan, Poole, Boyes, Redgate and March2015) found that health workers’ higher knowledge and higher belief in the efficacy of cCBT was associated with higher intentions to use cCBT with clients. These results on cCBT indicate that discovering and addressing negative attitudes of therapists towards eCBT could play a part in improving its acceptance as an effective treatment modality. Most previous research has been conducted on cCBT (computerized CBT with no/minimal clinician support). One published paper (Kivi et al., Reference Kivi, Eriksson, Hange, Petersson, Bjorkelund and Johansson2015) refers to therapist attitudes towards what they term iCBT (computerized CBT with regular, limited, asynchronous online clinician support). However, this research took place in Sweden, the therapists interviewed were part of the research team investigating as well as implementing iCBT, and the findings focus mostly on organizational factors, and include only two broad themes that indicate generally positive attitudes towards iCBT. Therefore, detailed research into the attitudes of practising clinicians towards offering eCBT in the UK context is still required.
Aims of the current study
The aim of the current study was therefore to investigate therapists’ beliefs about, and attitudes to, offering eCBT in an inner-city UK IAPT service, as part of exploring potential barriers to referring clients to SilverCloud (the eCBT programme offered in that service).
Method
Survey development
The survey was based on published literature about perceived benefits of, and barriers to, using cCBT (Stallard et al., Reference Stallard, Richardson and Velleman2010; Donovan et al., Reference Donovan, Poole, Boyes, Redgate and March2015). In addition, questions were drawn from topics raised in informal discussions at four service meetings. The final survey included a brief description of eCBT used in the IAPT service to ensure that all participants were answering about the eCBT programme offered in the service. This was followed by 14 closed questions and statements, broadly encompassing perceived benefits and barriers of eCBT, perceived effectiveness of eCBT, and perceived training needs within the service. Questions and statements were rated on Likert scales. Participants were also asked to rank what would be most helpful to them for referring more clients to eCBT from 1 to 6, with 6 being the most helpful. After each section, an open question about any additional thoughts allowed respondents to add any reflections not covered in the closed questions. The survey was revised in an iterative fashion within the team, and piloted with two trainee clinical psychologists not involved in the survey to ensure readability and low participant burden.
Participants
The survey was sent to all therapists practising within the IAPT service (n = 73). The invitation to take part in the online survey was sent by email which contained a link to the survey. Two reminders were sent out; one after 2 weeks, and one after 4 weeks. Thirty-three therapists responded (response rate = 46%). The majority were PWPs (33%, n = 11), 24% (n = 8) were clinical psychologists, 21% (n = 7) were high intensity CBT therapists, 9% (n = 3) were counsellors, 6% (n = 2) were counselling psychologists, and 6% (n = 2) were assistant psychologists or trainee clinical psychologists. The PWPs supported patients with SilverCloud; all other participants could offer patients SilverCloud as a treatment option following initial screening and assessment.
Data analysis
Data were analysed using descriptive statistics. Likert scale responses were categorized into ‘strongly disagree/disagree’, ‘neither agree nor disagree’ and ‘agree/strongly agree’ because individual categories were small. Content of open questions was analysed using thematic analysis (Braun and Clarke, Reference Braun and Clarke2006).
Results
The percentage of cases reportedly offered eCBT by respondents in the week preceding the survey ranged from 0 to 70%, with a mean of 50%, and a median of 10%. High intensity therapists and clinical psychologists had on average stated that they allocated a larger percentage of their cases to eCBT than other therapist groups (26.7 vs 5.6%, respectively, allocated more than 25% of their cases to eCBT), but the difference was not significant (chi-squared (2) = 3.03, p = 0.219).
Perceived knowledge about eCBT
As shown in Fig. 1, almost all participants (97%) reported that they ‘know what eCBT involves’. Most (65%) were ‘comfortable with the technical aspects of eCBT’, and slightly fewer (62%) were ‘confident to offer eCBT to clients’. About one-quarter of participants (23%) thought that ‘eCBT is preferable to other forms of self-help’, with over half of the sample (56%) neither agreeing nor disagreeing with this statement. Only about 10% of participants ‘agreed’ or ‘strongly agreed’ that ‘there is a strong evidence base to support the use of eCBT’.
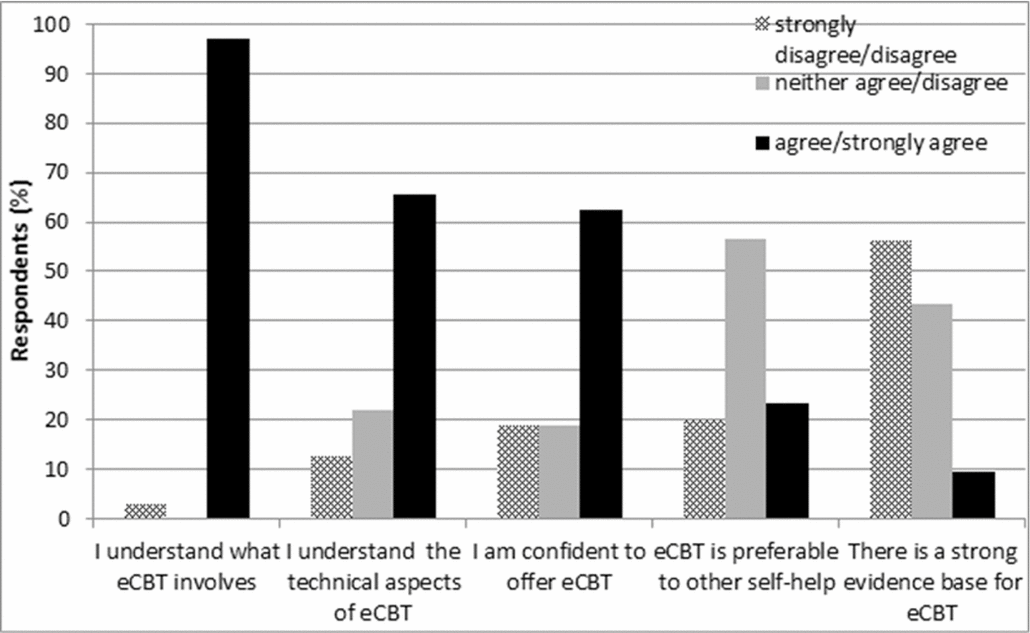
Figure 1. Therapists’ perceived knowledge about eCBT
Beliefs about effectiveness of eCBT
About two-thirds of participants (62%) ‘agreed’ or ‘strongly agreed’ that eCBT could be effective for ‘mild and moderate mental health difficulties’, while only 3% ‘agreed’ or ‘strongly agreed’ that it could be effective for ‘severe mental health difficulties’.
Overall, participants believed that eCBT would compare ‘worse’ or ‘much worse’ with face-to-face interventions across most mental health conditions. As shown in Fig. 2, in comparison with face-to-face interventions, 80% of participants believed that eCBT would perform ‘worse’ or ‘much worse’ for social anxiety, 77% believed that it would perform ‘worse’ or ‘much worse’ for OCD, 72% believed that it would perform ‘worse’ or ‘much worse’ for comorbid depression and anxiety, and 63% believed that it would perform ‘worse’ or ‘much worse’ for depression. Respondents were slightly more optimistic for generalized anxiety disorder (GAD), with just over half (52%) believing that eCBT would perform ‘the same’ as face-to-face interventions. Two-thirds of participants (60%) also believed that eCBT would perform ‘the same’ as face-to-face interventions for symptoms of stress.

Figure 2. Beliefs about the effectiveness of eCBT in comparison with face-to-face interventions
Perceived advantages of eCBT
As shown in Fig. 3, all participants (100%) ‘agreed’ or ‘strongly agreed’ that one advantage of eCBT is that it is available 24/7. Almost all participants (93%) also agreed that it ‘could be easily used at home’, with slightly fewer (87%) endorsing that eCBT would provide ‘easy access to evidence-based treatment’, and a similar proportion (86%) agreeing that it ‘is easy to include outcome measures’. Most participants (77%) also endorsed that eCBT could help ‘reduce the stigma associated with seeking help for mental health conditions’, and over half of the sample (57%) agreed that it would be ‘easy for clients to share problems using eCBT’. Participants were somewhat more sceptical about how easy it would be to adapt CBT for online use, with only one-third (30%) endorsing that ‘CBT can be easily adapted to be used online’.

Figure 3. Perceived advantages of eCBT
Perceived barriers to offering clients eCBT
As shown in Fig. 4, most therapists (77%) agreed or strongly agreed that ‘eCBT will not meet clients’ expectations about therapy’, and an equal percentage thought that ‘the lack of therapist contact will be perceived negatively by clients’. Over half (57%) thought that ‘the lack of the therapeutic relationship will lead to worse treatment outcomes’, and 50% of the sample thought that ‘clients will be unhappy being offered eCBT’.

Figure 4. Perceived barriers to offering eCBT to clients
Over half of the sample (53%) agreed or strongly agreed that ‘clients will not complete exercises when using eCBT’, and 43% thought that ‘clients will drop out’. Although relatively few participants (16%) thought that ‘clients would have difficulty understanding the exercises when using eCBT’, 43% thought that it would be difficult to tailor homework to the client. The sample was divided over whether it would be difficult to ‘pitch’ materials when using eCBT with one-third (33%) each agreeing, neither agreeing nor disagreeing, or disagreeing with this statement.
Few therapists (6%) thought that computer access would constitute a problem for clients, or that clients would not be computer literate, with only 3% endorsing this statement. Only 6% of participants expected clients to be concerned about privacy when using eCBT.
Two-thirds of participants (60%) thought that supporting a client using eCBT ‘requires skill’, but only 13% agreed that the ‘therapist's work is valued when supporting clients using eCBT’. Just over one-third of the sample (37%) agreed that eCBT ‘saves time for therapists’, and less than a quarter (20%) of the sample ‘agreed’ or ‘strongly agreed’ that eCBT could ‘be a solution to the lack of qualified therapists’.
Solutions to help therapists refer more people to eCBT
As shown in Fig. 5, providing training for therapists who allocate clients to different treatment modalities to help them become more familiar with eCBT was endorsed as the most helpful potential solution, followed by receiving training on the evidence base for eCBT. Offering eCBT earlier in the assessment and allocation process was also deemed as important, as was the provision of telephone support to help maintain rapport. Raising more awareness about eCBT among GPs and ensuring that supervisors are familiar with eCBT were both seen as important, albeit less urgent.

Figure 5. Perceived training needs/service changes to help offering eCBT to clients
Qualitative responses
Open-text responses highlighted several other areas for concern or potential barriers to offering eCBT. Participants saw guidance on managing risk as crucial (‘It is difficult to assess and manage risk, which can lead to negative perceptions of therapy and reduce further help-seeking in future’). There was also concern that working with eCBT would be less person-centred (‘It can be difficult to hold information about different clients in mind when only communicating online, potentially resulting in treatment feeling less person-centred and tailored to the individual’). The same participant also pointed out that reviews could become time-consuming (‘Clients can write a lot in their responses, particularly in journal entries, which make reviews time consuming’).
Participants were eager to point out that eCBT should ‘not be seen as panacea which can be offered to everyone’, although they acknowledged that it could be effective ‘for a select group of clients who are motivated and not very complex’, for participants ‘who are housebound or cannot travel’, and for ‘busy people such as parents’.
One participant suggested that ‘it would be helpful for clients to have one face to face session where eCBT could be explained thoroughly, to help clients identify what they would like support/help with, also to make clear boundaries around expectations and commitment, to plan when they will use the programme, and offer telephone reviews weekly or bi-weekly’.
Discussion
This survey study investigated attitudes to offering eCBT in an inner-city London IAPT service. Results indicate that therapists are confident that they know what eCBT involves. However, therapists are less confident in the evidence base for eCBT, and believe that, whilst it may be effective for mild to moderate problems, outcomes would be ‘worse’ or ‘much worse’ for eCBT than for face-to-face interventions. Although most participants acknowledged the potential advantages of eCBT, such as increasing access to therapy, and reduction in stigma, there was also an assumption that eCBT would ‘not meet clients’ expectation of what therapy involves’, and that ‘the lack of a therapeutic relationship will lead to worse outcomes’. Also, many therapists did not see eCBT as preferable to or different from self-help. As a result of these beliefs, perhaps, only a small majority of respondents felt confident in referring clients to eCBT.
Findings from this survey mirror those for similar surveys for computerized CBT without therapist support (Whitfield and Williams, Reference Whitfield and Williams2004; Stallard et al., Reference Stallard, Richardson and Velleman2010; Newton and Sundin, Reference Newton and Sundin2016). It is interesting to observe that general attitudes towards the effectiveness of eCBT appear to have been little influenced by technological advances, or the growing evidence base for eCBT demonstrating comparable outcomes to face-to-face interventions (Cuijpers et al., Reference Cuijpers, Donker, van Straten, Li and Andersson2010; Andersson et al., Reference Andersson, Cuijpers, Carlbring, Riper and Hedman2014). Furthermore, concerns about the lack of a therapeutic relationship in cCBT seem to persist about eCBT, despite its incorporation of therapist support. This conflicts with studies to date, which indicate that acceptability of internet-based interventions is high (Botella et al., Reference Botella, Gallego and García-Palacios2008; Andrews et al., Reference Andrews, Cuijpers, Craske, McEvoy and Titov2010; Wootton et al., Reference Wootton, Titov, Dear, Spence and Kemp2011), and that clients can form a good therapeutic alliance using internet-based technologies (Andersson et al., Reference Andersson, Paxling, Wiwe, Vernmark, Felix, Lundborg and Carlbring2012; Kiluk et al., Reference Kiluk, Serafini, Frankforter, Nich and Carroll2014; Bengtsson et al., Reference Bengtsson, Nordin and Carlbring2015). Also pertinent is the debate surrounding the importance of the therapeutic alliance for therapy success in general (Wampold, Reference Wampold2015). Research on the therapeutic alliance specifically in CBT has shown that it is necessary, but not sufficient to bring about symptomatic change (Turner et al., Reference Turner, Bryant-Waugh and Marshall2015). Instead, evidence suggests that change in symptoms early in therapy is a marker for improved outcomes (DeRubeis and Feeley, Reference DeRubeis and Feeley1990), which then drives strengthening of the therapeutic alliance. Further conflicting with therapist attitudes identified in this survey is the fact that eCBT also differs from pure guided self-help in that the materials are more engaging and interactive, and it incorporates regular support in the form of reviews by a PWP.
This study therefore suggests a discrepancy between what eCBT offers (in terms of features, effectiveness and patient experience) and how clinicians within this service perceive it. A qualitative study of client experience of eCBT within the same service found that clients found eCBT to be beneficial, and that they could form a therapeutic relationship online (R.P. Perera-Delcourt and G. Sharkey, unpublished data). Although patients did express a preference for face-to-face therapy, they were generally willing to try eCBT, particularly because it offers help immediately (as there is no waiting list). The difference of eCBT from pure self-help was also positively commented on by participants. This suggests that therapists’ beliefs about eCBT's appeal, and how important a face-to-face therapeutic relationship is, may not be entirely shared by patients, which could be a barrier to patients receiving effective help more quickly (if clinicians do not refer them for eCBT and instead place them on a waiting list for CBT). This discrepancy between staff and patient attitudes has also been found with regard to the use of eHealth interventions (web-based aftercare) by physical health professionals (Hennemann et al., Reference Hennemann, Beutel and Zwerenz2017).
Given the discrepancy between clinician attitudes and the evidence base, the current findings therefore highlight the importance of providing adequate education about eCBT to practising clinicians to ensure that clinical practice is based on the best available evidence. The need for training on the evidence base for eCBT was also identified as a priority by clinicians participating in the current study, which again echoes findings for other forms of web-based intervention (Perle et al., Reference Perle, Langsam, Randel, Lutchman, Levine, Odland and Marker2013). In addition to this, informal reviews of therapist attitudes to eCBT in team meetings and supervision (group and individual) is likely to be necessary, as provision of facts alone is unlikely to change views and practice by itself. A previous study has shown that a short presentation (5 minutes, 13 PowerPoint slides) can increase clinician knowledge about cCBT and its advantages, but not necessarily significantly increase their intention to use it, and calls for a more ‘sophisticated’ intervention to be developed (Donovan et al., Reference Donovan, Poole, Boyes, Redgate and March2015). Future research could develop such an intervention to address the staff attitudes identified, and examine the effect on the uptake of eCBT.
Based on the current evidence base for interventions addressing staff attitudes towards cCBT, training to address clinicians’ beliefs which affect them offering patients eCBT can be brief. Presenting factual information about the efficacy, comparable outcomes to face-to-face CBT, acceptability, advantages and data security of cCBT has been shown to increase clinicians’ intention to use it (Donovan et al., Reference Donovan, Poole, Boyes, Redgate and March2015; Hennemann et al., Reference Hennemann, Beutel and Zwerenz2016). This has also been shown to increase the intention to use cCBT by adolescents (Mitchell and Gordon, Reference Mitchell and Gordon2007) and parents of children with mental health difficulties (Sweeney et al., Reference Sweeney, Donovan, March and Laurenson2017). For professionals, it may be beneficial to improve their general IT literacy, make use of social norms, i.e. provide information about how much eCBT is used, and present research that shows that healthcare professionals typically view eCBT less positively than patients (Hennemann et al., Reference Hennemann, Beutel and Zwerenz2017). An interactive or video demonstration of the specific eCBT programme on offer, perhaps by a clinician who supports patients with it, with text or speech overlay, can make presentations more effective, and address misconceptions such as about the (perceived lack of) differences between eCBT and written self-help (Mitchell and Gordon, Reference Mitchell and Gordon2007; Donovan et al., Reference Donovan, Poole, Boyes, Redgate and March2015; Hennemann et al., Reference Hennemann, Beutel and Zwerenz2016). In addition to offering this training to clinicians within their IAPT services, service managers may wish to run the presentations for GPs, other referrers and other stakeholders (such as service user groups), given that these groups will influence patients’ expectations, and thus uptake, of eCBT (Hennemann et al., Reference Hennemann, Beutel and Zwerenz2016). Table 1 outlines suggestions for specific aspects of training tailored to the findings from the present study.
Table 1. Suggestions for training content

As well as addressing the attitudes of staff offering eCBT as a treatment option following assessment, this survey (and subsequent discussion within the service) highlighted that the beliefs of PWPs delivering eCBT interventions also appeared to be significant. Staff identified that they do not feel valued in their work, and struggle to manage the length of their replies and remain person-centred, when delivering these interventions. Further evidence-based training and supervision could ameliorate this. There has been some exploratory research in this area, which identified therapist behaviours correlating positively and negatively with eCBT engagement and outcome (Paxling et al., Reference Paxling, Lundgren, Norman, Almov, Carlbring, Cuijpers and Andersson2013; Schneider et al., Reference Schneider, Hadjistravopoulos and Faller2016). However, as the research is correlational and with mixed results, it is not possible yet to draw firm conclusions about what constitutes evidence-based practice for clinicians supporting patients with eCBT (for example, how flexible to be about task deadlines, and what kind of statements or questions to use in messages).
This study also highlighted a valid concern about the suitability of patients for eCBT. As described in the Introduction, eCBT has been developed as a way of managing resources. This is necessary in the current economic climate (Bower and Gilbody, Reference Bower and Gilbody2005). However, clinicians were understandably concerned about not offering eCBT to patients for whom it might be harmful (e.g. those at high risk of suicide). Clearer guidelines about for whom eCBT is suitable would be helpful, to prevent clients being offered it in order to meet targets at their detriment. Further research could investigate factors predictive of suitability for eCBT.
One major limitation of this study is that it used a sample from a single service. Findings may therefore not generalize to other services. Also, the survey used provided brief information about eCBT, which could have inflated answers to one question about perceived knowledge about eCBT. However, the attitudes to eCBT in the current study match those identified in earlier studies of cCBT with larger samples, which gives some confidence in the current findings. Nonetheless, future research could use a larger sample from multiple services to gain more conclusive findings. Another limitation of the current study is that all data are purely descriptive. Future research could identify predictors of attitudes to eCBT to get a better understanding of the drivers of a negative attitude towards the introduction of novel technologies in healthcare.
Conclusion
This study suggests that, despite awareness of some beneficial features of eCBT, staff in an inner-London IAPT service hold negative views conflicting with the evidence base for its effectiveness, and early evidence about the patient experience, and are unsure on how to best support clients using eCBT. While therapist concerns about suitability seem valid (as we are not suggesting that the use of eCBT should exceed its evidence base), and attitudes towards offering therapy in modalities other than ‘traditional face-to-face interventions’ are always likely to persist to some extent, it seems important to address these attitudes and perceived lack of skills as much as possible, through training and supervision, in order to allow clients to access evidence-based treatments in a resource-efficient, clinically appropriate, and timely manner.
Main points
(1) The majority of therapists in the service studied held a number of negative beliefs about eCBT which may be barriers to offering this therapy modality.
(2) Education on the evidence base of eCBT and client experiences of this therapy modality may help challenge therapist beliefs about eCBT that do not fit with the evidence base.
(3) Further research can examine whether addressing specific attitudes identified about eCBT could increase access for more patients to this quickly accessible evidence-based treatment.
(4) Clear guidelines about who may benefit from eCBT could be helpful (when research can tell us what these should contain).
(5) Staff delivering eCBT may benefit from further training and modality-specific supervision, to improve skills and confidence in using this approach.
Acknowledgements
The authors would like to thank Drs Janet Wingrove, Katharine Rimes and David Hambrook, and Gemma Sharkey for their contributions to and support of this project, as well as the clinicians who took part.
Ethical standards
The study was approved by the South London and Maudsley Clinical Governance Audit Committee. The authors have abided by the British Psychological Society's Code of Human Research Ethics.
Conflicts of interest
The authors have no conflicts of interest with respect to this publication.
Financial support
This study represents independent research part-funded by the National Institute for Health Research (NIHR) Biomedical Research Centre at South London and Maudsley NHS Foundation Trust and King's College London. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health.
Learning objectives
After reading this article the reader should be able to:
(1) Be aware that supported computerized CBT (eCBT) is an innovative way to meet demand for psychological therapies which has an emerging evidence base, but which services have been slow to adopt.
(2) Understand the nature and prevalence of therapist beliefs about eCBT that may contribute to its slow uptake.
(3) Consider the implications of the findings for the provision of training and supervision on this area within services.









Comments
No Comments have been published for this article.