Psychiatric disorders are common in learning disability (Reference Rutter, Tizard and WhitmoreRutter et al, 1970), although implications for mental health across the life course in this group are not fully known. Maughan et al (Reference Maughan, Collishaw and Pickles1999) studied 100 males and females with mild learning disability from the National Child Development Study (NCDS). At age 33 years these individuals suffered poorer social circumstances, greater potential stressors and were at higher risk of affective disorder than the remainder of the cohort. Childhood family and social disadvantage accounted for approximately 20-30% of this variation. The British 1946 birth cohort provides an opportunity to replicate and extend these findings. Our aims were to compare measures of affective disorder at ages 36 and 43 years in those meeting the criteria for learning disability and the remainder of the cohort, and to investigate the extent to which any group difference was accounted for by adverse social or material circumstances.
METHOD
The 1946 birth cohort
Participants were drawn from the Medical Research Council's National Survey of Health and Development (NSHD), also known as the British 1946 birth cohort, and initially consisting of 5362 children of non-manual and agricultural workers and a random sample of one in four of manual workers selected from all births that occurred in England, Scotland and Wales during one week in March 1946 (Reference WadsworthWadsworth, 1991). Information about socio-demographic factors and medical, cognitive and psychological function has been obtained repeatedly by interview and examination, most recently in 1989 at age 43 years, when sample size was 3262. This can be regarded as a representative sample of the UK population legitimately and singly born in the immediate postwar era (Reference Wadsworth, Mann and RodgersWadsworth et al, 1992).
Learning disability status
In line with ICD-10 criteria for mild learning disability (F70) (World Health Organization, 1992), participants were classified as having mild learning disability if they scored 2-3.33 s.d. units below the mean on the general ability score of the Group Ability Test AH4 (Reference HeimHeim, 1955), equivalent to an IQ score range of 50-69. The AH4 is a 130-item timed test with separate verbal and non-verbal sections that are summed to yield the general ability score, administered at age 15 years (Reference Pigeon, Douglas, Ross and SimpsonPigeon, 1968). The verbal items consist of analogies, comprehension and numerical reasoning, whereas the non-verbal items consist of matching, spatial analysis and non-verbal reasoning. An adequate measure to assess whether participants met the ICD-10 criterion of impaired adaptive behaviour was not available.
Psychiatric outcomes
Two principal psychiatric outcome measures were used. The first was a shortened version of the Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974) at age 36 years. This is a structured interview to elicit symptoms primarily of depression and anxiety. PSE caseness was determined by the index of definition (Reference Wing and SturtWing & Sturt, 1978), using the cut-off for threshold disorder or above. The second was the Psychiatric Symptom Frequency (PSF) scale (Reference RodgersRodgers, 1994) — an interview-based scale for symptoms of anxiety and depression. A total symptom score was obtained and a cut-score of 31 for classifying caseness in terms of psychiatric disturbance gave an identical prevalence rate to that obtained using the PSE (Reference Paykel, Hayhurst and AbbottPaykel et al, 2001). This also allowed a measure of chronicity, where survey members were classified as meeting case criteria for neither outcome (PSE and PSF), either outcome or both outcomes. Neuroticism at age 26 years, measured by the Maudsley Personality Inventory (MPI; Reference EysenckEysenck, 1958), provided an earlier indication of anxiety-proneness. Scores for all participants who self-completed this instrument were included in the analysis. For descriptive purposes, school teachers' behavioural ratings (disobedience, discipline difficulties, restlessness in class, aggression and difficulty in making friends) at age 15 also are reported.
Early background variables
The following variables were chosen to represent early social background and early adversity:
(a) Paternal occupational social class, assigned using the father's occupation, classified according to the UK Registrar General's system (Office of Population Censuses and Surveys, 1970) when the participant was aged 11 years or, if this was unknown, occupation at 4 or 15 years.
(b) Maternal education, classified into those with primary or secondary education only with no formal qualifications, and those with formal qualifications or any further education.
(c) Family size (≤4 v. >4 children).
(d) Overcrowding at age 15 years (>4 persons to a room).
(e) Parental divorce by age 15 years or parental death by age 26 years.
(f) Any illness requiring hospitalisation of 3 weeks or more up to age 5 years.
For descriptive purposes, birthweight and age at reaching motor developmental mile-stones (age at first sitting up, standing and walking) also are reported.
Circumstances at age 36 years
The following variables were chosen to represent social, material and other potential adverse circumstances at age 36 years:
(a) Socio-economic status (occupational social class of the head of household using categories similar to those for father's social class).
(b) Educational attainment (highest educational or training qualifications achieved by 26 years).
(c) Family circumstances (any of the following: divorced or separated, living on own or no children).
(d) Employment status (yes/no).
(e) Financial hardship.
(f) Poor material home conditions (any of the following: shared kitchen, shared bathroom, no indoor lavatory, no hot running water).
(g) Medical complaints over the past 12 months.
(h) Adverse life events in the past 12 months.
Statistics
Logistic regression was used to determine the unadjusted association between each early background variable (see above) and learning disability. The association between learning disability and the principal psychiatric outcomes (PSE at age 36 years and PSF at 43 years) also was investigated using logistic regression. To examine the extent to which any association between learning disability and adverse psychiatric outcome was accounted for by early disadvantage, these associations were adjusted for the early background variables. The extent to which any association was specific to midlife was examined by adding MPI Neuroticism at 26 years to the models for ages 36 and 43 years (the influence of learning disability thus being assessed in relation to early adulthood to these ages) and by adding the PSE at 36 years to the model for PSF at 43 years (for similar reasons). Finally, to test whether any association between learning disability and the PSE was accounted for by current adverse circumstances, adjustment was made, in turn, for each variable representing circumstances at age 36 years (see above).
RESULTS
Sample selection
A total of 4017 participants (74.9% of the original cohort) had AH4 data available at age 15 years. Of these, 143 (3.6%) fell within the learning disability range according to the above cognitive criteria, and 3866 (96.4%) provided a comparison group. This was reduced to 41 and 2119, respectively, when selected for non-missing values on the psychiatric outcomes, the early background variables and MPI Neuroticism at 26 years. Those with missing values for any of these variables were more likely to be classified as having learning disability than those with non-missing values for all variables in the model (χ2=37.92, P<0.001).
Early background variables
Table 1 shows that although there was no gender difference in the likelihood of being classified as having learning disability, those with learning disability were significantly more likely than the comparison group to have had a manual social class background, a mother with no educational qualifications, to be part of a large family and to have experienced overcrowding at 15 years. There was no association at the 5% level between parental divorce or death and learning disability, or hospitalisation for at least 3 weeks by age 5 years and learning disability (no participant with learning disability had been hospitalised during childhood or adolescence for diseases of the central or peripheral nervous system).
Table 1 Odds ratios and 95% confidence intervals for the effect of the early life variables on learning disability

| Variable | Comparison group | Learning disability group | OR | (95% Cl) | P |
|---|---|---|---|---|---|
| n | 2119 | 41 | — | — | — |
| Gender (% female) | 50.6 | 48.8 | 0.93 | (0.50-1.72) | 0.81 |
| Father's social class (% manual) | 57.6 | 90.2 | 6.80 | (2.41-19.11) | <0.001 |
| Mother's education (% no qualifications) | 61.9 | 95.1 | 11.97 | (2.88-49.40) | <0.001 |
| Family size (% >4) | 16.2 | 41.5 | 3.66 | (1.94-6.89) | <0.001 |
| Overcrowding (% >4/room, at age 15) | 1.2 | 7.3 | 6.36 | (1.84-21.98) | 0.003 |
| Parental death or divorce (%) | 22.2 | 29.3 | 1.45 | (0.73-2.86) | 0.29 |
| Illness, up to age 5 years (%)1 | 4.3 | 9.8 | 2.38 | (0.84-6.82) | 0.11 |
| Low birth weight (%) | 2.6 | 14.6 | 6.30 | (2.56-15.64) | <0.001 |
| Age at sitting (months) | — | — | 1.12 | (0.91-1.36)2 | 0.28 |
| Age at standing (months) | — | — | 1.03 | (0.89-1.18)2 | 0.70 |
| Age at walking (months) | — | — | 0.97 | (0.84-1.10)2 | 0.63 |
Those with learning disability were significantly more likely to have had low birth weight (<2.5 kg). However, there was no difference at the 5% level between those with learning disability and the comparison group in time to reach the motor developmental milestones of sitting, standing or walking.
Behavioural and psychiatric variables
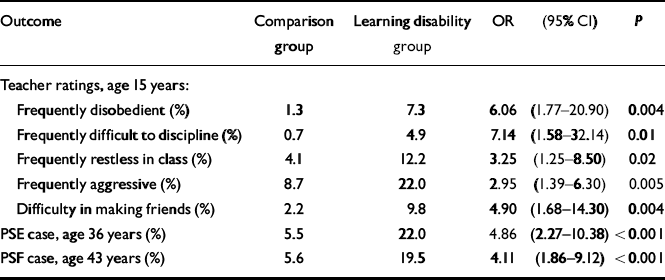
There was clear evidence of mental disturbance in adolescence and middle adult life in those with learning disability (Table 2). Thus, they were significantly more likely than the comparison group to be rated by teachers as showing behavioural disturbances at 15 years, and were significantly more likely to meet PSE and PSF case criteria at 36 and 43 years, respectively. Indeed, joint risk of behavioural disturbance (defined as scoring at least one of the five teacher ratings in Table 2) and PSE caseness was significantly greater in the group with learning disability than in the comparison group (χ2=43.86,P<0.001). Of the psychiatric measures, only MPI Neuroticism at 26 years (not shown) did not distinguish between the two groups (regression coefficient=0.54 (95% CI −0.65 to 1.72), P=0.38).
Table 2 Odds ratios and 95% confidence intervals for the effect of learning disability on the mental health outcomes
| Outcome | Comparison group | Learning disability group | OR | (95% CI) | P |
|---|---|---|---|---|---|
| Teacher ratings, age 15 years: | |||||
| Frequently disobedient (%) | 1.3 | 7.3 | 6.06 | (1.77-20.90) | 0.004 |
| Frequently difficult to discipline (%) | 0.7 | 4.9 | 7.14 | (1.58-32.14) | 0.01 |
| Frequently restless in class (%) | 4.1 | 12.2 | 3.25 | (1.25-8.50) | 0.02 |
| Frequently aggressive (%) | 8.7 | 22.0 | 2.95 | (1.39-6.30) | 0.005 |
| Difficulty in making friends (%) | 2.2 | 9.8 | 4.90 | (1.68-14.30) | 0.004 |
| PSE case, age 36 years (%) | 5.5 | 22.0 | 4.86 | (2.27-10.38) | <0.001 |
| PSF case, age 43 years (%) | 5.6 | 19.5 | 4.11 | (1.86-9.12) | <0.001 |
Table 3 shows that the associations between learning disability and the two principal psychiatric outcomes were not attenuated by adjustment for gender, early background variables and MPI Neuroticism. Indeed, coefficients for the PSE were strengthened by the inclusion of these variables. Nor were they attenuated by the addition of birth weight into the model (not shown). However, the association between learning disability and the PSF total score at age 43 years fell below the 5% level after adjusting for the PSE at age 36 years, suggesting no significant increase in cases of affective disorder after age 36 years.
Table 3 Odds ratios and 95% confidence intervals for the effect of learning disability on Present State Examination (PSE) and Psychiatric Symptom Frequency (PSF) scale outcomes, progressively adjusting for background variables

| PSE case | PSF case | |||||
|---|---|---|---|---|---|---|
| OR | (95% CI) | P | OR | (95% CI) | P | |
| Learning disability (unadjusted) | 4.86 | (2.27-10.38) | <0.001 | 4.11 | (1.86-9.12) | <0.001 |
| +Gender | 5.11 | (2.36-11.13) | <0.001 | 4.26 | (1.90-9.49) | <0.001 |
| +Early background1 | 5.50 | (2.46-12.30) | <0.001 | 3.63 | (1.58-8.33) | 0.002 |
| +Neuroticism, age 26 years | 5.51 | (2.41-12.55) | <0.001 | 3.58 | (1.54-8.33) | 0.003 |
| +PSE | — | — | — | 2.40 | (0.96-5.99) | 0.06 |
Because those with learning disability were more likely to have a father of manual social class, these analyses were repeated after weighting to allow for the stratified social class sampling used to select this cohort. The pattern of results was similar to that of the unweighted ones presented.
To test whether the association between learning disability and the PSE was accounted for by current adverse circumstances (i.e. at age 36 years), the variables representing these circumstances (see Method) were added in turn to the model, already adjusted for gender, the early background variables and MPI Neuroticism. Only financial hardship attenuated the association to any notable degree, although the coefficient remained significant at the <0.001 level, as it did after adjusting for each of these variables in turn.
Finally, in terms of chronicity, those with learning disability were significantly more likely than the comparison group to meet the case criteria for both psychiatric measures (χ2=28.45, P<0.001). For meeting the criteria on neither measure, proportions were 67.5% and 90.4%, for meeting the criteria on either measure they were 22.5% and 8.1% and for meeting the criteria on both measures they were 10.0% and 1.5% in the group with learning disability and the comparison group, respectively.
DISCUSSION
In a large population-based prospective study we found that individuals who met the cognitive criteria for learning disability at age 15 years were at high risk of affective disorder, persisting at least into mid-life. In particular, these individuals were significantly more likely than those in a comparison group to be rated by a teacher as having behavioural problems, and over four times more likely to be at risk of affective disorder in mid-life, as determined by the PSE at age 36 years and the PSF at age 43 years. These results confirm those of Maughan et al (Reference Maughan, Collishaw and Pickles1999) from the NCDS. They indeed strengthen them in two respects. First, the PSE and PSF are interview-based instruments and therefore less vulnerable to potential bias from poor reading skills than a self-completion instrument such as the Malaise Inventory used in the NCDS. Second, risk of affective disorder in learning disability was observable in two measures 7 years apart and therefore was sustained in mid-life.
These results also build on those of van Os et al (Reference van Os, Jones and Lewis1997), who initially reported an association between low cognitive ability and affective disturbance in this cohort by showing that this association was not accounted for by adverse social or material circumstances in childhood or adulthood.
There are several potential limitations of this study. First, the number of learning disability cases was relatively small in this birth cohort, which limits the ability to perform stratified analyses, such as examination of gender differences. Second, two different instruments were used at different times to measure psychiatric disturbance. Both measure a similar spectrum of symptoms of milder disorder, and a PSF cut-score was employed to give similar case rates for the PSE index of definition (Reference Paykel, Hayhurst and AbbottPaykel et al, 2001). However, there are significant methodological differences between the two instruments, and the validity of adjusting the PSF cut-score in this way depends on the assumption (for which there is some support) of constant prevalence over the 7 years separating the measures (Reference Paykel, Hayhurst and AbbottPaykel et al, 2001). Third, the PSE and PSF were designed for the general population, and are not specifically validated for use in learning disability. Although standard diagnostic criteria may become less appropriate in the general population the more severe the learning disability (Royal College of Psychiatrists, 2001), we have sought to minimise this potential bias by excluding those with moderate, severe and profound learning disability.
Conversely, the Psychiatric Assessment Schedule for Adults with a Developmental Disability (PAS-ADD), an instrument specifically designed to diagnose and measure degree of psychiatric illness in learning disability (Reference Moss, Patel and ProsserMoss et al, 1993), would not have been suitable for use in the general population. However, because this instrument is based in part on the PSE, the latter, although less likely to be valid for learning disability than the PAS-ADD, should have some degree of face validity in this population. Similarly, the PSF was relatively brief and administered by lay interviewers, and should not have presented an undue challenge to those with mild learning disability.
Potential reasons for affective disorder in learning disability
In summarising potential reasons for the high risk of affective disorder in learning disability, Scott (Reference Scott, Rutter, Taylor and Hersov1995) identified four basic factors: medical, including general conditions such as a brain disorder; environmental neglect or inconsistency; an effect of learning disability regardless of cause; and reverse causality (i.e. psychiatric disorder leading to impaired intellectual performance). Of these, Scott notes that the last is the least likely, because low intelligence usually predates the psychiatric disorder. Regarding medical conditions, those with learning disability in this study were no more likely to have been hospitalised in early life than the comparison group, and there were no participants with learning disability in the analysis who had been hospitalised at this time for central or peripheral nervous system conditions. As with Maughan et al (Reference Maughan, Collishaw and Pickles1999), those with learning disability had significantly lower birth weight than controls. This is consistent with evidence that birth weight is associated directly with cognitive development (Reference BreslauBreslau, 1995; Reference Richards, Hardy and KuhRichards et al, 2001) and with susceptibility to stress (Reference Nilsson, Nyberg and OstergrenNilsson et al, 2001). Again, however, risk of affective disorder in learning disability was maintained even after adjusting for low birth weight. Furthermore, there was no evidence of delayed motor milestones in this group, a phenomenon linked to risk of schizophrenia (Reference Jones, Rodgers and MurrayJones et al, 1994) and affective disorder (Reference van Os, Jones and Lewisvan Os et al, 1997) in this cohort. The lack of clear involvement of neurological disease or a neurodevelopmental syndrome is consistent with the group in this study representing mild learning disability.
The second factor identified by Scott (Reference Scott, Rutter, Taylor and Hersov1995) involves environmental neglect or inconsistency. As already noted, however, we did not find that adverse circumstances in childhood accounted for the increased risk of affective disorder in learning disability. Indeed, as Scott notes, “ Being reared in adverse conditions does not explain the increased incidence of those disorders which have not been shown to be strongly related to any specific environmental influences, for example most emotional disorders” (p. 631). Maughan et al found that early social adversity played a more significant role in the NCDS. One possible discrepancy is that these authors included behaviour problems as an explanatory variable in this respect, whereas we treated these as outcomes.
The third factor identified by Scott (Reference Scott, Rutter, Taylor and Hersov1995) is psychiatric disorder as an effect of learning disability regardless of cause. Adverse circumstances in adulthood did not account for risk of affective disorder in learning disability in the present analysis, just as adverse circumstances in early life did not. However, there may be more subtle factors that were not taken into account, such as coping capacity and self-worth (Reference Scott, Rutter, Taylor and HersovScott, 1995).
Implications for later life
What are the implications for risk of affective disorder in later life among those with learning disability? In a clinic-based study, Cooper (Reference Cooper1997) found higher rates of anxiety and depression in those with learning disability aged 65 years and older than in a younger group with this disability. The present results suggest high risk of affective disorder, which, although not increasing over time, is at least persistent in mid-life. If high risk of affective disorder is confirmed in older people with learning disability at the population level, then the strategic planning in the health and social services for older people with learning disability (Reference HollandHolland, 2000; Department of Health, 2001) must also take account of psychiatric vulnerability. Continued assessment of affective state in individuals with learning disability as they progress through mid-life into old age is therefore of considerable importance.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
• People with mild learning disability are at high risk of affective and anxiety disorders.
• This is likely to be enduring across the lifecourse.
• Government strategies for services for people with learning disability should be planned on the basis of these findings.
LIMITATIONS
• The relatively small sample size limited statistical power, for example to assess gender differences.
• Affective disturbance was only measured up to age 43 years.
• The psychiatric measures used were not validated in people with mild learning disability.






eLetters
No eLetters have been published for this article.