Service user involvement, albeit loosely defined, is endorsed as a democratic right in UK government policy 1 and required by many public research funding, governance and support bodies. 2,3 As a result, substantial investment has been made by the UK National Institute for Health Research (NIHR) in infrastructure to promote and enable involvement. 2-5 Although incorporation of ‘lived experience’ is advanced as a means to improving the quality, relevance, acceptability and ethical status of mental health research, Reference Staley6,Reference Staley and Minogue7 support for the concept and/or practice of involvement is far from universal. Concerns regarding tokenism abound Reference Wallcraft, Schrank and Amering8 and academic researchers have described partnership working with service users as time-consuming and challenging. Reference Trivedi and Wykes9 Moreover, questions are asked about the relative values accorded user and researcher expertise. Reference Beresford10 Systematic evaluation of user involvement in research generally is beginning, Reference Oliver, Rees, Clarke-Jones, Milne, Oakley and Gabbay11-Reference Brett, Staniszewska, Mockford, Seers, Herron-Marx and Bayliss13 but after more than a decade of user involvement in UK mental health research, the extent and nature of involvement is only partially described. Reference Telford and Faulkner14 Little is known about ‘who’ is involved in research, in what capacity and with what impact on research process and outcome. Service users, researchers and policy makers need such information to ensure that the process and outcome of involvement are optimised.
Method
Study aim and design
Aiming to represent the involvement and experiences of service users in mental health research in the UK, we identified our target population as ‘people with experience of service use in respect of mental health who are involved in mental health research (other than as a participant)’. A cross-sectional survey using a bespoke questionnaire was employed to gather data to enable description of: (a) place(s) of work and employment status, (b) research activity and experience(s) of involvement, (c) factors influencing involvement, and (d) the relationship between service use and research and the impact of involvement on mental health. The study, instigated and co-led by a service user researcher (J.T.), was guided throughout by a service user reference group recruited through the Mental Health Research Network (MHRN). The MHRN was established to support the implementation and conduct of mental health research within the UK National Health Service (NHS).
Sampling
In the absence of any census or register of the target population, we used snowball sampling to maximise reach. We began by compiling a database of primary contacts - individuals whose public profiles indicated they might be eligible (n = 41) and organisations that might employ or work with service user researchers. Contacts were identified through collegiate consultation, and searches of publicly accessible databases and literature retrieval systems using terms related to user involvement and research. Organisational contacts included research and development departments and service user groups in the 59 UK NHS mental health trusts, regional hubs of the MHRN in England and Scotland (n = 9), registered mental health charities (n = 46) and university departments of psychiatry, mental health, mental health nursing, and primary care and public health where the department webpages indicated mental health research activity (n = 168 contacts).
Survey instrument
Data were collected using a questionnaire developed iteratively by the authors and members of the service user reference group. An initial draft informed by literature and the authors’ experiences as service user and academic researchers was completed by six service users involved in research. Cognitive interviewing techniques were used to explore comprehension, response decision processes and content relevance, completeness and acceptability. Recommendations for modification were sought. Where views diverged (for example, about asking for a respondent’s diagnosis) we adopted a conservative approach, omitting potentially sensitive questions not directly addressing research objectives. The final questionnaire (available from the authors on request) comprised multiple-choice questions, open questions and space for free-text to enable respondents to amplify answers or provide additional information. Respondents were asked to provide demographic data, identify the UK region and setting(s) in which research activity was undertaken, and describe employment arrangements and research activities. Next, they were asked to rate agreement with propositions reflecting the rationale(s) and proposed benefits of user involvement in research. Open questions invited respondents to describe service use, pathways into research and the factors that enabled or hindered this involvement. Views about the influence of involvement on mental health service use and mental health were also sought. The questionnaire could be completed within 20 min but time required would vary dependent on the amount of information respondents wished to provide, with some of those involved in the pilot taking up to 1 h.
The survey was launched on 1 November 2011 when ‘first-line contacts’ were sent an email introducing the study with a link to the questionnaire posted online using Survey Monkey (www.surveymonkey.com) and the participant information sheet (Fig. 1). Emails detailed ethical approval (Fulham REC, 11/LO/ 1480) and advised that responses would be accepted until the end of February 2012. Contacts were asked to consider eligibility and disseminate the invitation widely. Questionnaire completion was anonymous but respondents were invited to contact investigators to enter a draw for a place at the 2012 MHRN scientific meeting and/or receive a findings summary.

Fig. 1 Sample ascertainment: snowball sampling process.
SUR, service user researcher; NHS, National Health Service; R&D, research and development; MHRN, Mental Health Research Network; HoDs, heads of departments.
Analysis
Data were downloaded to SPSS version 20 (for Windows) and Microsoft applications for analysis. Descriptive statistics were used to profile the sample and quantify involvement in areas, settings and activities. Responses to open questions were subject to analysis using the framework approach, Reference Ritchie and Lewis15 which enabled us to address predetermined questions while remaining open to emergent themes. The first step in analysis was to populate an initial frame comprising cells representing research ‘objective’ and ‘respondent’ with data from open questions, with multiple allocations possible. Constant comparison of data within and between cells and analytic questioning Reference Glazer and Strauss16,Reference Charmaz17 were employed to discern patterns and exceptions in the data. The frame was iteratively developed to support exploration of questions generated as analysis progressed (for example, to examine involvement by researcher status - see below). A dialogic collaborative process Reference Patterson, Hart and Weaver18 was employed through-out to check, interpret and integrate findings of various analyses performed independently by T.W., S.P. and J.T. This involved the authors critically reviewing each others’ accounts of the data and inviting examination of differing understandings in round-table discussions. Analysis and interpretation of findings were subject to review by the service user reference group during four 2 h meetings.
Results
Characteristics of achieved sample
The sample was achieved as summarised in Fig. 1. The survey link was accessed by 374 potential respondents. Nearly half (185, 49.5%) completed only the demographics section, discontinuing in some cases, according to anecdotal feedback, because involvement in research did not extend beyond participation. Exclusion of these, and another 24 who reported no service use (n = 3), working outside the UK (n = 2) or no involvement in research (n = 19), gave a sample of 166 whose characteristics are summarised in Table 1.
Table 1 Demographic characteristics of respondents (n = 166)Footnote a

| Respondents, n (%) | |
|---|---|
| Gender | |
| Male | 61 (37.2) |
| Female | 103 (62.8) |
| Age, years (mean age 46.8 years) | |
| 16-24 | 5 (3.2) |
| 25-34 | 25 (16.0) |
| 35-44 | 39 (25.0) |
| 45-54 | 40 (25.6) |
| 55-64 | 32 (20.5) |
| >64 | 15 (9.6) |
| Ethnicity | |
| White British | 127 (77.9) |
| White Irish | 10 (6.1) |
| White other | 14 (8.6) |
| Asian or Asian British Indian | 2 (1.2) |
| Asian or Asian British Pakistani | 2 (1.2) |
| Mixed White/Asian | 3 (1.8) |
| Black or Black British Caribbean | 2 (1.2) |
| Black or Black British African | 1 (0.6) |
| Mixed White/Black African | 1 (0.6) |
| Mixed other | 1 (0.6) |
| UK region in which research activity conductedFootnote b | |
| London and multiple regions | 10 (6.1) |
| London | 30 (18.4) |
| Scotland | 25 (15.3) |
| Wales | 23 (14.1) |
| South West | 14 (8.6) |
| North West | 13 (8.0) |
| West Midlands | 10 (6.1) |
| East of England | 8 (4.9) |
| South East Coast | 7 (4.3) |
| South Central | 7 (4.3) |
| Yorkshire and the Humber | 6 (3.7) |
| East Midlands | 4 (2.5) |
| Northern Ireland | 4 (2.5) |
| North East | 2 (1.2) |
a. There were missing data as follows: for gender, 2; age, 10; ethnicity, 3; and UK region, 3 respondents.
b. Respondents were asked to identify the English strategic health authorities within which they worked or alternatively Scotland, Wales and Northern Ireland.
The sample was predominately female (n = 103, 62.8%) and White British (n = 127, 77.9%). Respondents ranged in age from 21 to 73 years (median 47). With few (n = 22, 13.3%) reporting no formal educational or vocational qualifications, respondents were characteristically tertiary educated and highly trained. Nearly two-thirds (n = 106, 63.9%) reported under- (n = 44) or postgraduate (n = 62) degrees in diverse fields including health, humanities, fine arts, engineering and teaching. Seventeen (10.2%) held research degrees (PhD, MD) and 48 (28.9%) reported qualifications in healthcare fields including medicine, social work, nursing and psychology. Professional and other training reported by respondents was extensive, encompassing counselling, community education and project management. Research-focused training - for example in interviewing skills, software packages, analytic methods, particular study instruments and good clinical practice - was commonly reported. Several respondents reported completing training run by the MHRN or NHS trusts.
Mental health and service use
The sample included service users involved in research and researchers with experience of service use. Most (n = 128) respondents described their mental health and service use, typically reporting long-term severe mental illness, concomitant disability and extensive service use. Although not asked to report diagnoses, many respondents identified themselves as having specific mental illnesses. Those reported were schizophrenia, bipolar affective disorder, personality disorder, major depression, post-traumatic stress disorder and eating disorders. The majority were (or had been) users of public specialist mental health services but use of primary and private services was also reported. Extensive in-patient admissions, often under Mental Health Act 1983 regulations were commonly described. Respondents who included commentary on the perceived quality of services reported positive, negative and mixed experiences. For example, one described experiences as ‘relentlessly negative over two decades’; another noted ‘I found [named service] extremely beneficial… encouraged me to move forward with added confidence… ’.
Self-descriptors
We used the term ‘service user researcher’ in the questionnaire but invited respondents to identify preferred term(s) and to explain their use. Most respondents used a single descriptor (n = 109, 65.7%), sometimes their job title, but 30 used three or more in various combinations, dependent on context. As shown in Table 2, the most commonly used descriptors combined reference to ‘research’ with ‘service use’ or ‘lived experience’ (n = 86, 51.8%) (either ‘service user researcher’ (n = 64, 38.6%) or ‘researcher with lived experience’ (n = 22, 13.3%)). Sixteen (9.6%) respondents always made reference to service user status, whereas 23 identified themselves simply as ‘researchers’. ‘Survivor researcher’ and ‘expert by experience’ were each used by eight respondents. Explanations for choice of term(s) (and responses to other open questions) demonstrated the political, professional and personal complexity inherent in labelling and identification as a service user.
Table 2 How respondents (n = 166) described their roles

| How respondents self-defined their research position(s) |
Respondents n (%) |
|---|---|
| Researcher, with no reference to service user status | 23 (13.9) |
| (User) researcher with reference service use or lived experience | 86 (51.8) |
| Multiple labels (with/without reference to service user status) | 14 (8.4) |
| Multiple labels (all making reference to service user survivor status) | 16 (9.6) |
| Survivor researcher | 8 (4.8) |
| Expert by experience | 8 (4.8) |
| Other non-research term | 6 (3.6) |
| Prefers to avoid label | 5 (3.0) |
‘ “Service user researcher” stresses that I have used services, but can tend to downplay research skills. “Researcher with lived experience” stresses my professional research skills and my lived experience adds a separate dimension.’ (Service user researcher)
Many respondents reported electing not to disclose service use for fear of ‘having mental health history become my defining feature’ but others regarded the capacity to be open about experience with a receptive audience helpful.
‘I am a researcher, author and trainer but I also have mental health difficulties. I don’t like being defined as someone who uses services and I dislike the term lived experience. It means people see me as a service user and nothing else - I am more than that. I prefer my name. I have extensive experience as a researcher but I use my experience of difficulties as an asset at times.’ (Consultant)
Duration, location, setting, employment status and activity
Reporting a median of 5.8 years involvement (range 0.8-40) respondents were typically experienced researchers; activity of less than a year was uncommon (n = 8) and a substantial majority reported being research active for more than 2 (85%) and 10 years (30%). Most (n = 139, 83.7%) reported activity during the past 12 months, and planning to continue involvement in research (n = 143, 86.1%).
The vast majority of the 163 respondents who provided information about region (n = 153, 93.8%) were research-active within a single strategic health authority or UK region. Most frequently this was London (n = 30, 18.4%), which was among areas identified by each of 10 respondents (6.1%) who reported activity in multiple areas (range 2-11). Although few reported involvement in Northern Ireland (n = 4), substantial proportions were active in Scotland (n = 25, 15.3%) and Wales (n = 23, 14.1%), with every region having at least two respondents.
A quarter of all respondents reported activity across multiple organisational settings in various combinations, with approximately one in ten active in at least four settings. Of the 81 respondents (48.8%) who contributed to research in universities, half were also involved with research in local government and independent settings, or as consultants. The MHRN was nominated as a place of work by nearly a quarter (n = 38, 22.9%) but most of these (33/38) also identified other work places.
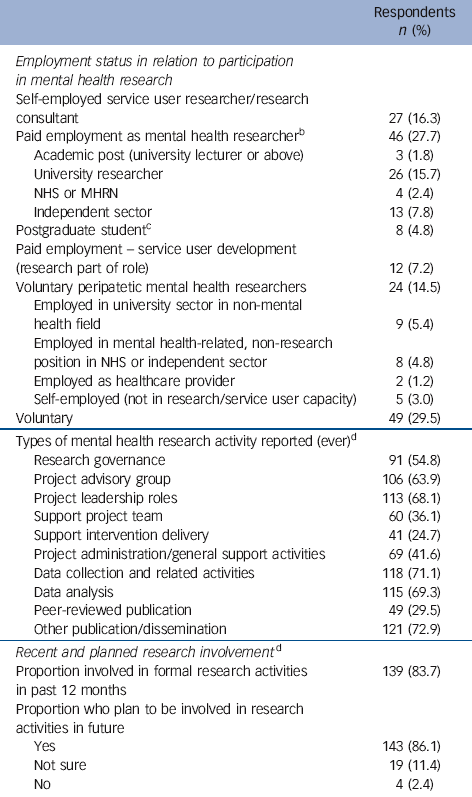
As shown in Table 3, in which employment status and sector are summarised, 27 respondents reported self-employment as consultants or researchers (see online Table DS1 for a more detailed version of Table 3). Forty-six (27.7%) reported paid employment as a researcher, with service use a requirement of appointment to the posts held by 20 respondents (12%). Twenty-nine respondents were university-based, with three holding academic posts (for example lecturer). Experience of service use was mandated in 1 academic post and 11 of the other university research posts held by respondents. Experience of service use was also a requirement for 3 of the 4 researchers based in the NHS, and 5 of 13 independent sector researchers. Of the eight students in the sample, two reported holding funding only open to people who had used services.
Table 3 Employment status in relation to mental health research and research activity (n = 166)Footnote a
| Respondents n (%) |
|
|---|---|
| Employment status in relation to participation in mental health research | |
| Self-employed service user researcher/research consultant | 27 (16.3) |
| Paid employment as mental health researcherFootnote b | 46 (27.7) |
| Academic post (university lecturer or above) | 3 (1.8) |
| University researcher | 26 (15.7) |
| NHS or MHRN | 4 (2.4) |
| Independent sector | 13 (7.8) |
| Postgraduate studentFootnote c | 8 (4.8) |
| Paid employment - service user development (research part of role) | 12 (7.2) |
| Voluntary peripatetic mental health researchers | 24 (14.5) |
| Employed in university sector in non-mental health field | 9 (5.4) |
| Employed in mental health-related, non-research position in NHS or independent sector | 8 (4.8) |
| Employed as healthcare provider | 2 (1.2) |
| Self-employed (not in research/service user capacity) | 5 (3.0) |
| Voluntary | 49 (29.5) |
| Types of mental health research activity reported (ever)Footnote d | |
| Research governance | 91 (54.8) |
| Project advisory group | 106 (63.9) |
| Project leadership roles | 113 (68.1) |
| Support project team | 60 (36.1) |
| Support intervention delivery | 41 (24.7) |
| Project administration/general support activities | 69 (41.6) |
| Data collection and related activities | 118 (71.1) |
| Data analysis | 115 (69.3) |
| Peer-reviewed publication | 49 (29.5) |
| Other publication/dissemination | 121 (72.9) |
| Recent and planned research involvement Footnote d | |
| Proportion involved in formal research activities in past 12 months | 139 (83.7) |
| Proportion who plan to be involved in research activities in future | |
| Yes | 143 (86.1) |
| Not sure | 19 (11.4) |
| No | 4 (2.4) |
NHS, National Health Service; MHRN, Mental Health Research Network.
a. See online Table DS1 for a more detailed version of this table.
b. Service use experience was a requirement for 1 of 3 academic, 11 of 26 university researcher, 3 of 4 NHS/MHRN and 5 of 13 independent sector posts.
c. Service use experience was a requirement of 2 of 8 student funding awards.
d. Multiple responses permitted.
Twelve respondents (7.2%) reported paid employment in the NHS, local authority or independent sectors, in posts related to service user development that incorporated research functions. Service use was a requirement for appointment to each of these posts.
A total of 73 (44%) respondents reported voluntary involvement in mental health research. Forty-nine (29.5%) of these - who we describe as ‘service user representatives’ - reported no formal paid employment of any kind. The other 24 reported paid employment as academics (n = 9, 5.4%) (working, for example, in law or a biomedical discipline), in non-research posts in NHS mental healthcare (n = 2) or independent sectors (n = 8), or self-employment (n = 5).
Collectively, respondents reported involvement in the full spectrum of research activities, typically as shown in Table 3 undertaking multiple research activities. More than two-thirds (n = 113, 68.1%) reported leadership activities (including study design, project management and funding applications). The majority of these (74/113, 65.5%) were also involved in governance/regulatory activities such as membership of ethics committees and peer review. Most (82/113, 72.6%) also performed advisory roles and (44/113, 38.9%) were additionally involved in data collection, analysis and dissemination, including authorship of articles. Although the activities of respondents not reporting leadership activities (n = 53) were more restricted (range 1-7, median 3) there were no other activities that non-leaders did not report performing. Forty respondents reported concurrent participation in other user involvement activities including advocacy, membership of user forums and organisational governance bodies. Several additionally reported being active politically, working to advance community understanding of mental illness.
‘Like many SUs [service users] I have many hats and research is one of these. I work and lobby at all levels. This is the best way to influence and change for the better, gives a stronger voice, people respect you more. We cannot just shout from the streets…’ (Service user representative)
Integration of employment-related data and responses to open questions demonstrated that respondents occupied one of six types of roles outlined in the Appendix.
Perspectives on service user involvement in research
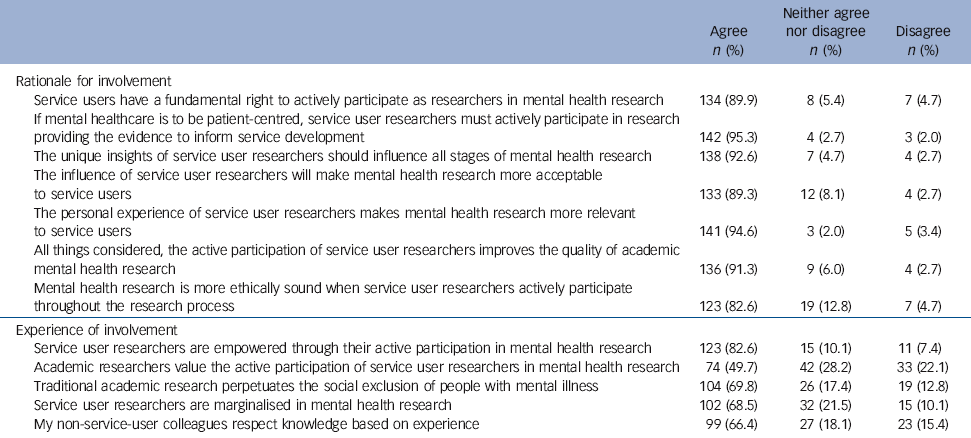
Views about user involvement were examined in multiple-choice and open questions. Responses to the latter qualified and contextualised the all but unanimous ‘in principle’ support evident in responses to propositions regarding the right to, and potential benefits of, involvement (Table 4). Respondents wrote of an abiding respect for people categorised as ‘mental patients’ and wanting research to be empowering of, and for, service users. They noted that a particular kind of knowledge and unique insights derived from experience were fundamental to ensuring research achieved the goal of service improvement and life enrichment for people who use services. Indeed, many respondents (n = 28) explicitly attributed their own involvement in mental health research to a ‘passion’ for service and/or social change and commitment to ensuring the interests of service users were central to that change. For some, lived experience legitimised involvement in mental health research. Service use experiences informed views of what worked well and had drawn attention to gaps in evidence, influencing areas of personal interest that became a focus for research.
Table 4 Views about service user involvement in research: levels of agreement with propositions relating to service user involvement using an ordinal rating scale (n = 149)
| Agree n (%) |
Neither agree nor disagree n (%) |
Disagree n (%) |
|
|---|---|---|---|
| Rationale for involvement | |||
| Service users have a fundamental right to actively participate as researchers in mental health research | 134 (89.9) | 8 (5.4) | 7 (4.7) |
| If mental healthcare is to be patient-centred, service user researchers must actively participate in research providing the evidence to inform service development | 142 (95.3) | 4 (2.7) | 3 (2.0) |
| The unique insights of service user researchers should influence all stages of mental health research | 138 (92.6) | 7 (4.7) | 4 (2.7) |
| The influence of service user researchers will make mental health research more acceptable to service users | 133 (89.3) | 12 (8.1) | 4 (2.7) |
| The personal experience of service user researchers makes mental health research more relevant to service users | 141 (94.6) | 3 (2.0) | 5 (3.4) |
| All things considered, the active participation of service user researchers improves the quality of academic mental health research | 136 (91.3) | 9 (6.0) | 4 (2.7) |
| Mental health research is more ethically sound when service user researchers actively participate throughout the research process | 123 (82.6) | 19 (12.8) | 7 (4.7) |
| Experience of involvement | |||
| Service user researchers are empowered through their active participation in mental health research | 123 (82.6) | 15 (10.1) | 11 (7.4) |
| Academic researchers value the active participation of service user researchers in mental health research | 74 (49.7) | 42 (28.2) | 33 (22.1) |
| Traditional academic research perpetuates the social exclusion of people with mental illness | 104 (69.8) | 26 (17.4) | 19 (12.8) |
| Service user researchers are marginalised in mental health research | 102 (68.5) | 32 (21.5) | 15 (10.1) |
| My non-service-user colleagues respect knowledge based on experience | 99 (66.4) | 27 (18.1) | 23 (15.4) |
In contrast to the strong endorsement of user involvement in principle, some equivocation was evident in relation to practice; respondents drew on experience to highlight tensions and difficulties enacting involvement. Of those respondents who stated their views (n = 149), most (123, 83%) agreed that service user researchers are ‘empowered through their active participation in health research’ and two-thirds (n = 99, 66.4%) agreed that non-service user colleagues ‘respect knowledge based on experience’ (Table 4). However, two-thirds agreed that academic mental health research both ‘marginalised service users’ and ‘perpetuates the social exclusion of people with mental illness’. Although half (n = 74, 49.7%) agreed with the proposition that ‘academic researchers value the participation of service users’, more than one in five disagreed (n = 33, 22.1%) and the remaining 28.2% (n = 42) were undecided. Responses to open questions elucidated structural, personal and interpersonal influences on practice and the experience of involvement.
What supports involvement?
Although a small minority of respondents attributed involvement to hard work and/or good fortune, the majority described various personal, professional and social factors as enabling initial or ongoing involvement in research. Support, both emotional and practical, cited by half of respondents was chief among these. Acknowledging that engaging with or employing service users was commonly perceived as risky in academic environments, and that research environments were typically difficult to negotiate, respondents frequently described the sponsorship of a senior researcher or mentor as crucial.
‘… a wonderful service user researcher colleague has been an amazing source of support, she completely understand the difficulties I experience in this role.’ (Service user research officer)
The (earned) respect, encouragement and affirmation of colleagues who appreciated but did not dwell on the difficulties faced, were pivotal. A few respondents reported receiving helpful encouragement from family and health professionals but membership (formal or informal) of a service user/survivor researcher network, comprising like-minded people, was repeatedly described as essential to initiation and maintenance of involvement. Peer networks functioned as critical friends providing moral support, practical advice and peer review.
‘I have had some fantastic role models in other service user academics, particularly those who have sought to use their academic skills to highlight challenges in the systems.’ (Academic)
Several respondents wrote of the importance of being involved in ‘the right type of project in the right type of environment’. Being able to select projects and roles that matched capacity (for example, participating in governance structures/advisory committees rather than collecting data) and afforded flexibility to manage workload were described as enabling participation.
At a personal level, being educated, articulate and assertive, such that sense could be made of the research environment and pitfalls negotiated, were seen as crucial to establishing credibility and acceptance. Self-awareness, capacity to reflect on interpersonal interaction and understanding of group dynamics were considered essential to success as a service user researcher, as was staying well ‘enough’ or having the flexibility to work around periods of ill health. Several respondents wrote of the importance of organisations such as the MHRN, INVOLVE, mental health charities and specified NHS trusts in advancing the cause of user involvement in research and NHS trusts in facilitating access to necessary training, peers and job opportunities. Some, all of whom undertook research in a voluntary capacity, wrote of practical matters including having a flexible ‘real job’, proximity of facilities, ability to travel, and access to and ability to use a computer and the internet.
What challenges involvement?
That expertise grounded in lived experience was not really valued and that different types of expertise were not accorded equal status were recurrent themes. Many respondents whatever their positions, perceived stigma, prejudice and discriminatory behaviour as pervasive and negatively having an impact on the process and experience of involvement.
‘I imagine it’s like a Black person having to listen to racist discourse and present another viewpoint in a way that is non-threatening and will engage the participant in active change rather than offend.’ (Research officer)
University environments described as competitive- and outcome-, rather than process-focused, were considered particularly difficult to negotiate by several respondents, including academics.
‘I work in an institution where clinical academics are dominant. This prioritises clinical experience (both educationally and the experience of treating) over both my expertise as a scientist and experiences as a service user.’ (Service user researcher)
Respondents described difficulty engaging professionally in ‘business’ when their input was discounted as non-academic, subject to excessive scrutiny for bias or conversely overvalued rather than being subject to critical review.
For respondents whose service user status was known, these difficulties were compounded by the sense that private business was subject to public examination. Respondents described being ‘put on the spot’, expected to share their personal experience in various contexts and experiencing hypervigilance. Colleagues’ (over) concern about their well-being was experienced as intrusive and inhibiting full participation in the ‘workplace’. In these circumstances they described being reluctant to disclose concerns they considered ‘normal’ (for example, after a research interview exploring sensitive issues) for fear of having their response ‘symptomatised’.
Several participants wrote of double binds. Respondents not employed in designated service user roles reported that disclosure of diagnosis and/or experience of service use led to discounting of research expertise, undermining acceptance by non-service user colleagues. In contrast, performing research activity well was sometimes seen to undermine the validity and status of those who self-defined as expert by experience.
‘Colleagues are incredulous that someone with my diagnosis would be able to do research effectively - they believe that I’m not really unwell and don’t make the allowances (sometimes) needed.’ (Academic)
Furthermore, developing research expertise and credibility was described as leading to exclusion from the service user community, whereas ‘overexposure’ could lead to dismissal as a ‘usual suspect’ or a ‘non-representative professional-user’ from the research community.
Some concerns related directly to position. Respondents employed as researchers wrote of being challenged by pressure to achieve professionally and work to unrealistic timetables and career prospects. Service user representatives were more commonly concerned with inability to access training and practical difficulties (for example access to essential technology, travelling to meetings held in inconvenient locations and out-of-pocket expenses). The benefits system was described as a major stumbling block, particularly for service user representatives whose involvement was voluntary. Respondents reported that participation in any activity could lead to assessment as having ‘capacity to work’ resulting in loss of benefits, whereas receipt of payments for research activity could involve convoluted reporting and a net loss of income. Consultant/self-employed researchers reported similar difficulties and struggling with the inconsistent flow of work.
Tokenism was reported by several respondents who typically observed a need to retain the traditional research hierarchies and uncertainty around the role of service user researchers and lived experience.
‘Tokenism, tokenism, tokenism… You are there because the funders have asked to show service user participation. This is true of funding applications as well. I cannot tell you the number of times I have received a research bid two days before submission, asking me if I would be a co-applicant because they need a Black service user researcher.’ (Academic)
‘I am very aware that service-user endorsement is valuable to academics and researchers. The smart ones have a bank of reliable service users they can call upon to advertise and support their own particular agendas. It is not uncommon to hear a researcher attempt to cover all sins by writing “this was endorsed by our service-user steering committee”. Often this consists of the researchers’ collaborators.’ (Service user representative)
What impact is involvement having?
Respondents typically reported seeing or perceiving an impact of involvement on research process. Whether publicly identified as a service user researcher or not, respondents reported drawing on their experiences (and those of service user peers) to inform role performance. For academic and student researchers, topics, research questions and study design were informed by lived experience. For researchers involved in data collection, the experience of service use was described as underpinning a genuine respect for ‘fellow travellers’ and capacity to connect. This enabled access to ‘hard to reach’ potential participants, and enhanced the quality of data collected because participants ‘felt understood’. Data analysis and interpretation were described as informed by sensitivity and insight developed through service use - ‘adding depth of understanding’. More generally, some respondents wrote of challenging of academics to consider alternate world views, either explicitly or by their presence.
The vast majority of the 125 respondents who completed the question ‘Has involvement in research influenced your use of or attitude to MH [mental health] services?’ reported developing an increased appreciation of the ‘big picture’. They described discovering the diversity of services and service users and constraints and pressures on service delivery. Awareness of the burdens of bureaucracy and the complexity of systems had contributed to renewed respect for service providers. One observed the ‘considerable overlap between service user and staff needs’. These views were concordant with those of the several respondents who reported becoming more ‘realistic’ or ‘pragmatic’ in expectations of services and taking a more proactive approach to their care and treatment.
For a minority, however, involvement in research had affirmed or supported development of a critical position. Awareness of the dominance of medicine, the political nature of ‘madness’ and the stigma of service use, developed through involvement, had made them more wary of services. Critique was also extended in respect of the apparent absence of evidence for many interventions delivered by services and the variable access to interventions.
The question ‘How has involvement affected your mental health?’ was answered by 124 respondents. For a small minority (n = 14) the impact had been predominately negative. These respondents reported that ‘stress’ related to research activity (pressure of work, exposure to personally distressing material and workplace conflict) had undermined confidence and capacity to cope, leading to periods of ill health. However, as other respondents observed, such experiences were not research-specific.
‘Working as a service user researcher has definitely dented confidence in my research skills and myself as a researcher. I have experienced more difficulties with my mood that I attribute to the role… it’s not just a job, but a role in which I am invested personally and politically…’ (Service user researcher)
Others (n = 28) reported that involvement had ‘no impact’ or described ambivalent positions.
‘It may not be ideal to be surrounded by issues that are so close to home. It may be particularly harmful to embody a labelled position but hugely rewarding to work in a helping profession… ’ (Service user researcher)
For the vast majority (n = 80), however, the overall impact of involvement on their mental health had been unambiguously positive. Many wrote that involvement and investment in research activity provided a sense of purpose and belonging, giving meaning to their ‘suffering’, reduced self-stigma and enhanced self-respect. Facing up to the challenges of research was described as leading to discovery of internal resources and development of self-management strategies that promoted mental well-being. Being occupied and active intellectually were considered health-promoting by several and respondents commonly reported deriving a sense of pride in their achievements and developing (or renewing) confidence in their place in community.
‘… helped me to come to terms with mental health problems [which were] disabling, gave me something I wouldn’t otherwise have had - a career that uses both my lived and learnt experience and validates me as a whole… I have found my niche where I can feel accepted and not have to be pretending to be something else.’ (Service user researcher)
The vast majority of respondents (n = 136/149, 91.3%) agreed that ‘all things considered, the active participation of service user researchers improves the quality of mental health research’.
Discussion
Main findings
Our findings represent the first systematic analysis of the participation of service users in the mental health research arena in the UK. The survey enabled description of the characteristics, skills and experiences of service user researchers; the varied, sometimes multiple, positions they occupy and the complexities inherent in enacting sometimes ambiguous roles in mental health research environments in which political, professional and personal interests intersect. The service user research workforce revealed by this study is diverse but characteristically mature and highly skilled, using a wealth of life experiences to inform research activity. Whatever their positions in relation to mainstream/academic research, service user researchers are passionate about working to enhance services and see research as fundamental to this goal. Employed in various capacities across sectors, sometimes in dedicated service user posts, people with experience of service use are undertaking the full range of research activities and consider their contributions important to the improvement of research quality. Influences on involvement in mental health research are similar to those reported in relation to service development in mental health and other sectors. Reference Wallcraft, Schrank and Amering8,Reference Patterson, Weaver, Agath, Rutter, Albert and Crawford19,Reference Crawford, Rutter, Manley, Weaver, Bhui and Fulop20 Support and sponsorship are recognised as crucial to participation whatever position the researcher occupies. We note that many of the respondents working in academia elected not to disclose their mental illness or service use for fear of scrutiny and discounting of their contributions. Others noted that tokenism is rife, access to training is difficult and that the logistics of involvement often involved substantial inconvenience - particularly for service user representatives working on a voluntary basis. However, for the majority the experience of involvement in research is positive, often enabling sense to be made of difficult experiences and with the right support an important component of recovery. Before considering the implications of these findings we consider some limitations of the study that constrain generalisability.
Limitations
Most importantly, although no alternative design offered comparable potential for achieving both national coverage and access to hidden populations, we cannot know whether our snowball sampling reached all potential respondents and we are unable to assess response rate or representativeness of the sample. Although the geographical distribution and diversity of respondents suggests that reach was extensive, it is probable that some service users involved in research remained unaware of the study and that others who were eligible elected not to participate. Participation of these unknown researchers may have enriched or challenged findings. We also note reliance on self-report and acknowledge that, as with any human accounts of activities and subjective experiences, these reports are necessarily constructed within circumstances to which we are not privy. As with any analysis of qualitative data our representation of respondents’ views and experiences is vulnerable to claims of bias. Faced with a wealth of rich and complex data we worked collaboratively, questioning analysis from our differing perspectives and checking our emergent findings with a service user reference group for resonance. We acknowledge that others may have made alternate interpretations but contend that the process has facilitated faithful representation of respondents’ accounts.
Implications
As a whole our findings reinforce the view that substantial advances in user involvement in mental health research have been made in a relatively short time, Reference Beresford, Wallcraft, Barnes and Mercer21 perhaps reflecting the substantial investment from the NHIR. Moreover, that the majority of respondents experienced involvement positively and many were keen to pursue and develop further opportunities augurs well for the future. However, findings related to the experience of stigma, discrimination and tokenism also indicate that the potential of service user involvement will be only achieved with continued attention to deep-level cultural change and development of robust mechanisms to ensure timely and meaningful engagement. Reference Thornicroft, Bindman, Goldberg, Gournay and Huxley22 As others contend, Reference Stewart and Liabo23 this will require critical examination of power hierarchies within psychiatry - an arena in which service users have traditionally been disempowered - and adaptation of systems, organisations and processes.
There are lessons here for countries in which service user involvement in research is in the early stages of development. Policy and piecemeal ad hoc involvement are insufficient if involvement is to be meaningful and sustainable (for individuals and at the systems level). Investment must be made in systems and infrastructure is needed to nurture service user researchers, 4 also traditional academic ways of working need to be reconsidered and investigators more fully engaged in the process. 5 Informal or formal mentoring or ‘buddy’ systems may be developed relatively easily at the local level given some initiative on the part of academic departments. But structural change is also required to establish career pathways and for progression along these to be supported by accredited training and mentoring schemes. Programmes involving partnerships between universities, charities, research and involvement organisations and consortia of private sector service user researchers offer opportunities for innovative development. Service user researchers must be at the heart of these partnerships but integration of different types of expertise, grounded in lived experience and research training, will be crucial to development of the requisite evidence base in the UK and internationally. Reference Stewart and Liabo23 As an important next step in optimising involvement, opportunities and outcomes research should critically examine issues explored here from the perspectives of academic researchers and commissioners.
Appendix
Typology of service user researcher roles
-
(a) Self-employed research consultants: undertaking various activities including but not limited to research and/or mental health, on commission.
-
(b) Salaried mental health researchers:
-
(i) academics: employed in academic posts (i.e. lecturer or above) with research-based higher degrees (PhD, MD). Research was a chosen career irrespective of mental health status. However, involvement in mental health research was influenced by personal experience.
-
(ii) university researchers: employed to work on academic mental health research projects. Research was a chosen career irrespective of mental health status, but involvement in mental health research was often influenced by personal experience. Usually employed to work on a specific study. Research skills were primary requirements of the post, but lived experience of mental illness/service may have been a formal selection criterion.
-
(iii) non-university researcher: employed by NHS trusts or (independent sector) mental health charities to work on a specific mental health study or to contribute ‘lived experience’ across a programme of projects. Lived experience of mental illness/service use may have been a formal selection criterion. Job choices often reportedly to be influenced by personal experiences and perspectives.
-
-
(c) Postgraduate students: respondents undertaking research-based higher degrees (PhD, MD). Choice of topic and approach influenced by personal experiences and perspectives.
-
(d) Salaried service user development workers: employed in health/social care fields in service user development roles. Involvement in mental health research was an ad hoc and secondary activity. Research was sometimes an element of the job description or a voluntary/ discretionary activity but usually seen as an extension of their service user development roles.
-
(e) Peripatetic/voluntary researchers:
-
(i) academics working in non-mental health fields: voluntary involvement in mental health research. Respondents were employed in non-mental health related academic positions (which may or may not have been health related). Some respondents possessed high-level transferable skills.
-
(ii) non-researchers - mental health clinicians: respondents employed as clinicians in the mental health field. Respondents had no formal research roles. Involvement in mental health research was ad hoc and voluntary.
-
(iii) self-employed - non-research, non-clinical: respondents reporting self-employment in diverse fields unrelated to mental health and research. Involvement in mental health research was ad hoc and voluntary.
-
-
(f) Service user representatives: individuals involved in research specifically because they have lived experience of mental illness/service use. Involved explicitly to represent the service user perspective in various forums/activities (for example steering group, ethics committee). Involvement was typically voluntary or honorary and ad hoc, sometimes an extension of engagement in other user involvement activities.
Funding
No funding was received for this study but the service user reference group was supported by a grant from the MHRN.
Acknowledgements
The authors are grateful to all who completed and disseminated the survey and to the service user reference group members, and acknowledge the support of the MHRNs in England and Scotland.








eLetters
No eLetters have been published for this article.