Central obesity is a key component of the metabolic syndrome(Reference Eckel, Grundy and Zimmet1), which is associated with increased risks of CVD and diabetes(Reference Isomaa, Almgren, Tuomi, Forsén, Lahti, Nissén, Taskinen and Groop2–Reference Grundy, Cleeman and Daniels4). Intra-abdominal visceral fat is particularly reactive to lipolytic stimuli and is believed to affect glucose homeostasis through its effect on circulating adiponectin levels(Reference Steffes, Gross, Schreiner, Yu, Hilner, Gingerich and Jacobs5). As central obesity is more strongly associated with visceral fat than BMI, waist circumference (WC) has been proposed as the more sensitive measure of relative CVD risk(Reference Dobbelsteyn, Joffres, MacLean and Flowerdew6, Reference Janssen, Katzmarzyk and Ross7).
The metabolic syndrome has been identified in children and adolescents(Reference Bitsori and Kafatos8) as well as adults and appears to persist from childhood into adulthood(Reference Huang, Ball and Franks9). Trends of increasing overweight(Reference Ford, Mokdad and Ajani10) and central obesity(Reference Li, Ford, Mokdad and Cook11) among children and adolescents are well documented. Some studies indicate that central adiposity among children may be increasing independent of weight(Reference McCarthy, Jarrett, Emmett and Rogers12, Reference Moreno, Sarría, Fleta, Marcos and Bueno13). As a surrogate measure of central body fat, WC has been suggested as an important early marker for the development of chronic diseases(Reference Maffeis, Pietrobelli, Grezzani, Provera and Tatò14, Reference Savva, Tornaritis, Savva, Kourides, Panagi, Silikiotou, Georgiou and Kafatos15) as well as a practical screening tool for identifying children at risk for metabolic syndrome(Reference Hirschler, Aranda, Calcagno Mde, Maccalini and Jadzinsky16, Reference Moreno, Pineda, Rodríguez, Fleta, Sarría and Bueno17).
Although some studies have considered the role of dietary patterns in the development of central obesity among adults(Reference Williams, Prevost, Whichelow, Cox, Day and Wareham18–Reference Drapeau, Despres, Bouchard, Allard, Fournier, Leblanc and Tremblay21), data related to the role of food group intake in the development of central obesity at younger ages is very limited. The US Department of Agriculture’s (USDA) Food Guide Pyramid and Dietary Guidelines for Americans (issued every five years) provide food-based intake guidelines for children and adults(22). Unfortunately, there is little direct scientific evidence to support specific dietary recommendations for the prevention of childhood obesity, particularly central obesity. The consumption of different amounts and types of foods may impact adiposity in a variety of direct and indirect ways. For example, different foods may impact satiety through volumetric differences, effects on gastric emptying or energy content. Other foods are theorized to affect body weight through their impact on such factors as energy metabolism or storage, lipogenesis or insulin sensitivity. The goal of the current analyses was to explore the relationship of mean food group intake and anthropometric measures of central obesity in children (aged 5–11 years) and adolescents (aged 12–16 years) using cross-sectional data from the Third National Health and Nutrition Examination Survey (NHANES III, 1988–1994).
Methods
Study population
NHANES have been conducted regularly since 1960 to assess the health and dietary status of the civilian non-institutionalized US population aged 2 months and older. The surveys randomly select subjects using a stratified, multistage probability cluster design and oversample certain groups including young children, non-Hispanic blacks and Mexican-Americans. Details of the design and sampling methods as well procedures for obtaining informed consent have been described elsewhere(Reference Ezzati, Massey, Waksberg, Chu and Maurer23). The current secondary analyses were conducted with the approval of the Boston University Institutional Review Board. Since dietary habits may change particularly during late adolescence, we restricted the analyses to subjects who were less than 17 years of age in order to reduce the likelihood that true changes in diet would impact the estimates of usual intake(Reference von Post-Skågegard, Samuelson, Karlström, Mohsen, Berglund and Bratteby24).
The primary analyses include subjects who were 5–16 years of age and in one of three categories of racial or ethnic origin: non-Hispanic whites, non-Hispanic blacks and Mexican-Americans. A total of 4329 children aged 5–11 years children (or their parents) and 2079 adolescents aged 12–16 years completed interviews and an examination. The number of subjects (n 99) in the other racial/ethnic groups was insufficient to provide stable estimates of association, so these subjects were excluded from the analyses as has been recommended by the NHANES III Analytic and Reporting Guidelines(25). Subjects with dietary data designated as missing or unreliable (n 317) by the study nutritionist or with extremes of energy intake (the upper and lower 2 % of the distribution of energy intake; n 227) were excluded, as were those who were pregnant or breast-feeding (n 18), taking diabetes medication (n 8), had missing data for WC circumference (n 128) or had potential confounders of interest to the study (n 47). This resulted in a final sample size of 3761 children aged 5–11 years and 1803 adolescents aged 12–16 years. Skinfold measurement data were missing for an additional 112 subjects who were therefore excluded from any sub-analyses related to that outcome. Similar exclusion criteria were used for the 1999–2002 NHANES study population of 12- to 16-year-olds, leaving 2541 available for the analysis.
Assessment of dietary intake
Dietary intake in both NHANES III and NHANES 1999–2002 was assessed through a single 24 h recall using an automated, microcomputer-based interview(Reference Feskanich, Sielaff, Chong and Buzzard26). Prior to age 12, the recall was completed jointly by the subject and a proxy respondent. Dietary recalls were analysed for nutrient composition using USDA nutrient files appropriate to the time period.
Food Pyramid servings of the five major food groups (i.e. dairy, fruit, vegetables, grains and meats/other proteins) were calculated from intake of both simple foods (e.g. glass of milk) and mixed dishes (e.g. lasagne) as defined by the USDA Dietary Guidelines(27, 28). One dairy serving was defined as 1 cup of milk or yoghurt, 1·5 oz of natural cheese or 2 oz of processed cheese. A fruit serving equalled 1 medium fruit (e.g. apple, banana, orange), 1/2 cup of chopped, cooked or canned fruit, or 3/4 cup of fruit juice. Total fruit (whole or as juice) was also divided into two subgroups: (i) citrus, melons and berries; and (ii) other fruits. One vegetable serving comprised 1 cup of raw leafy vegetables, 1/2 cup of cut-up raw or cooked other vegetables, or 3/4 cup of vegetable juice. There were several vegetable subgroups including dark-green vegetables, deep-yellow vegetables, white potatoes, other starchy vegetables (including legumes), tomatoes and other vegetables. French fries were included with potatoes but the added fat from frying was counted as servings of discretionary fat (see below). A grain serving (whole and refined) was represented by 1 slice of bread, 1 cup of dry cereal, or 1/2 cup of cooked rice, pasta or cereal. Finally, the meat/protein group included all forms of meat, fish, poultry, eggs, soyabean products, nuts and seeds. For the purposes of estimating intake, servings in the meat/other protein group were expressed as ounce equivalents and included items such as 1 oz of lean meat, fish or poultry, 1/2 cup of cooked dry beans, an egg, or 2 tablespoons of peanut butter(Reference Friday and Bowman29). Discretionary fats referred to fat in food that is above the amount that would be expected in a lean, low-fat or fat-free form of the food.
Assessment of anthropometric measures of central obesity
WC served as the main measure of central adiposity in these analyses, while the sum of suprailiac and subscapular skinfold thicknesses served as a secondary measure. Waist measurements were taken on a horizontal line at the high point of the iliac crest. The measurement was made at minimal respiration to the nearest 0·1 cm. Skinfold thickness measurements were taken using a Holtain skinfold calliper following a standard protocol and recorded to the nearest 0·1 mm. For NHANES 1999–2002, only WC was examined as an outcome (the sum of the two skinfolds was not available).
Assessment of potential confounders
Parental education (classified as less than high school, high school and more than high school) was used as an indicator of socio-economic status (SES). Income was assessed as a secondary measure of SES in these analyses using a dichotomous classification of <$20 000 v. $20 000 or more (since nearly 10 % of NHANES III subjects failed to provide more precise data on annual income). In the NHANES III sample, parental education was retained in the final models as it confounded the main results. Since this variable was not available in the 1999–2002 surveys, parental income was used instead. The three categories of race/ethnicity as defined by NHANES included non-Hispanic blacks, Hispanic (specifically Mexican-American) and non-Hispanic whites.
Pubertal development was assessed during the physical examination by physicians who were given standardized training in the use of Tanner stage classification(Reference Marshall and Tanner30, Reference Marshall and Tanner31). For the purpose of the present analyses, the original 5-stage Tanner scale was collapsed into three categories: (i) stage 1 or 2; (ii) stage 3; and (iii) stage 4 or 5. Tanner stage classification was not available for NHANES 1999–2002. Television watching was assessed in both surveys by questioning the child (or parent, depending on age) about the number of hours of television watched the previous day. Weight and standing height were measured according to a standardized protocol and BMI was calculated as weight in kilograms divided by the square of height in metres (kg/m2).
Physical activity was assessed among children aged 8 years and above by questionnaire. We examined it as a potential confounder in the models for adolescents but later dropped it as it led to no change in the results.
Statistical methods
Given the cross-sectional study design, both the anthropometry measures and the dietary intakes were measured at the same time. In these analyses, we examined the adjusted mean dietary intakes associated with age- and sex-specific quartiles of WC (and the sum of subscapular and suprailiac skinfold measures). The adjusted mean level of intake in each quartile of central body fat was estimated using analysis of covariance modelling with PROC GLM in the SAS statistical software package version 9·1 (SAS Institute Inc., Cary, NC, USA).
In addition to the use of quartiles for categorizing the distributions of central adiposity, we also examined the association between the mean intakes in each of the five major food groups and related subgroups and the prevalence of central obesity. Since there are no specific cut-off points for defining an abnormal waist size in children, we chose to explore both the 85th and the 90th age- and sex-specific percentiles. Although the 90th percentile of waist size has been used in some guidelines for defining the metabolic syndrome in children(Reference Zimmet, Alberti, Kaufman, Tajima, Silink, Arslanian, Wong, Bennett, Shaw and Caprio32), we found that the associations between food intake and waist size using the 85th yielded very similar results and greater statistical power and so we present only that analysis. To allow for the comparison of the analysis results from the 1999–2002 surveys with those from NHANES III, we used the same age- and sex-specific cut points of WC (derived from the NHANES III distributions) to define children with (≥85th percentile) and without (<85th percentile) central obesity.
The potential confounders retained in the final models were those that led to meaningful changes in the adjusted mean dietary intakes, including age, race/ethnicity, height, number of hours of daily television viewing, Tanner stage of pubertal development and parental education or income level. For the approximately 1·5 % of subjects who had missing data on parental education, we used a dummy variable to substitute missing education information. Analyses were conducted including and excluding the dummy variable for education and the results were nearly identical, leading us to conclude that the inclusion of these subjects was unbiased.
Results
Descriptive characteristics for the 3761 children aged 5–11 years and the 1803 adolescents aged 12–16 years are shown in Table 1. On average, the 5- to 11-year-olds were slightly less than 8 years of age while the adolescents were about 14 years of age. Boys in both age groups consumed more dairy, vegetables, grains and meats/other non-dairy proteins than did girls. While there were no apparent gender-related differences in WC at these ages, girls did have higher levels of subcutaneous fat as assessed by the sum of subscapular and suprailiac skinfolds (P < 0·05 for all).
Table 1 Characteristics of subjects by age and gender in the Third National Health and Nutrition Examination Survey
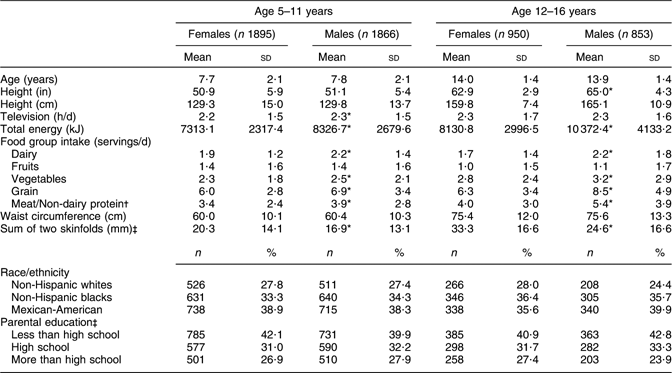
*Mean value was significantly different from that of females (P < 0·05).
†Meat/Non-dairy protein = total ounce servings of meat, fish, poultry and other non-dairy sources of protein.
‡Data were missing for subscapular skinfold (n 37), suprailiac skinfold (n 54), both skinfolds (n 21) and parental education (n 81).
Tables 2 and 3 show adjusted mean food group intakes according to the age- and sex-specific quartiles of WC and sum of two skinfolds. At 5–11 years of age (Table 2) there were few differences in food intake associated with category of central body fat, although boys in the lowest quartile of WC or sum of two skinfolds consumed about half a serving less of meat/other protein than those in the highest quartile (e.g. 3·61 servings/d v. 4·14 servings/d for WC quartiles 1 and 4, respectively; P for trend = 0·025).
Table 2 Adjusted mean food intakes according to anthropometric measures of central obesity: children aged 5–11 years (Third National Health and Nutrition Examination Survey)
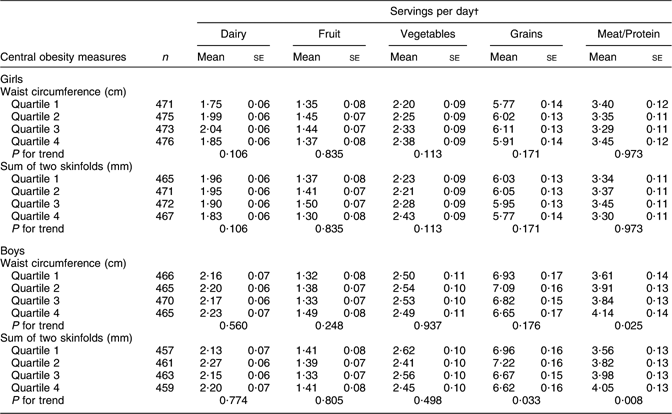
†Food group means are adjusted for exact age, height, race/ethnicity, hours per day watching television, Tanner stage and parental education.
Table 3 Adjusted mean food intakes according to anthropometric measures of central obesity: adolescents aged 12–16 years (Third National Health and Nutrition Examination Survey)
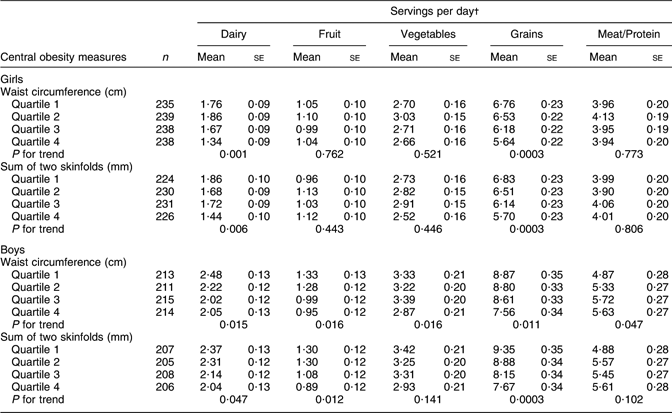
†Food group means are adjusted for exact age, height, race-ethnicity, hours per day watching TV, Tanner stage, and parental education.
Among 12- to 16-year-old male and female adolescents (Table 3), intakes of dairy products and total grains were inversely associated with both measures of central body fat. For example, those in the lowest quartile of WC consumed nearly half a serving more of dairy per day than those in the highest quartile (P for trend = 0·001 and 0·015 for girls and boys, respectively). Similarly, those in the smallest WC quartile consumed more than one additional serving of grain per day than those in the highest quartile (P for trend = 0·0003 and 0·011 for girls and boys, respectively). Neither fruit nor vegetable intake was associated with central adiposity in girls. However, adolescent boys with the largest waist (and skinfold) measures consumed the least amount of fruit (P for trend = 0·016 and 0·012 for WC and skinfolds, respectively) and the fewest vegetables (P for trend = 0·016 for WC). Finally, there was also a tendency for adolescent boys in the lowest quartile of WC to consume less meat (P for trend = 0·047).
Table 4 examines the association between food intake and central obesity by classifying those with WC at or above the age- and sex-specific 85th percentile as having central obesity. We conducted the analyses in both NHANES III and NHANES 1999–2002. The analyses in Table 4 are restricted to adolescents. Identical analyses were carried out among 5- to 11-year-old children (not shown) but, as was found in Table 2, there were no meaningful or statistically significant differences in the major food group intakes associated with WC. In both surveys, adolescents with central obesity (WC ≥ 85th percentile) consumed less dairy and fewer grains and had lower intakes of total fruit and vegetables (P = 0·0002, P < 0·0001 and P = 0·045, respectively, in NHANES III; P = 0·0009, P = 0·0002 and P = 0·062, respectively, in NHANES 1999–2002). While the majority of the dairy consumed was in the form of milk, both milk (P = 0·004) and cheese intakes (P = 0·020) were inversely associated with central obesity in NHANES III while only the association with milk consumption was significantly different (P = 0·0008) in the later NHANES sample; too few subjects consumed yoghurt to evaluate its effect separately. Central obesity was similarly related to whole and refined grain intakes (P = 0·002 and P = 0·001, respectively, in NHANES III; P = 0·006 and P = 0·003, respectively, in NHANES 1999–2002). There was no consistent association between central obesity and the intake of meat and meat equivalents. Finally, we compared the discretionary fat intakes of children with and without central obesity, and found that children without central obesity reported consuming more discretionary fat than children with central obesity (P < 0·0001 in NHANES III; P = 0·003 in NHANES 1999–2002).
Table 4 Association between food intake and waist size in adolescents in NHANES III and NHANES 1999–2002
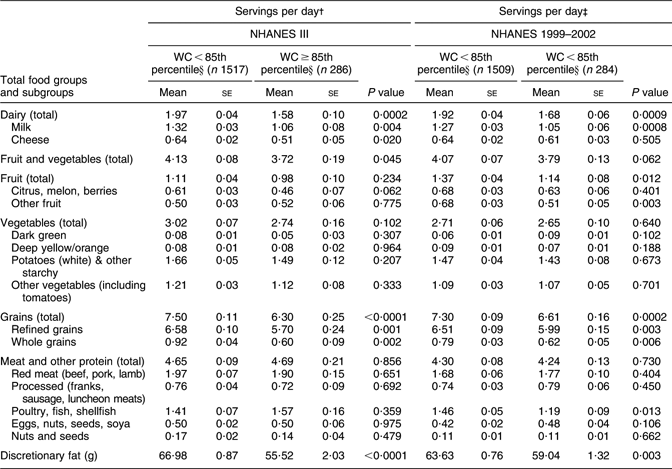
NHANES, National Health and Nutrition Examination Survey; WC, waist circumference.
†Adjusted for exact age, gender, height, race/ethnicity, hours per day watching television, Tanner stage and parental education.
‡Adjusted for exact age, gender, height, race/ethnicity, hours per day watching television and parental income.
§Age- and gender-specific cut-off points of WC from the NHANES III data set were used.
Discussion
The present paper explores the relationship between food group intake and central obesity among children and adolescents. The results suggest that intakes of dairy and grains as well as the combined intakes of fruit and vegetables are associated with lower levels of central body fat, particularly among adolescents.
The literature related to dietary intake and central obesity in children is very limited. These results are consistent with a report from the National Growth and Health Study which found that adolescent white females following a ‘healthy dietary pattern’ (i.e. higher intakes of dairy, fruits, vegetables and grains) had smaller increases in WC over 10 years(Reference Ritchie, Spector, Stevens, Schmidt, Schreiber, Striegel-Moore, Wang and Crawford33). A larger number of studies have examined the relationship of food group intake and overall adiposity among children. Regarding dairy, for instance, some data indicate that higher dairy intakes are associated with significantly lower body fat levels through childhood(Reference Novotny, Daida, Acharya, Grove and Vogt34–Reference Moore, Bradlee, Gao and Singer36), although a review of the evidence in 2005 concluded that there was insufficient evidence at that time to draw firm conclusions regarding the effect of Ca or dairy intake on body fat(Reference Huang and McCrory37).
While higher fruit and vegetable consumption is thought to be associated with a healthy body weight in children, a recent review concluded that more evidence is needed to support this conclusion(Reference Newby38) and it has been suggested that the methods of preparation (e.g. frying) and serving (e.g. with sauce) may account for the apparent inconsistent protective effect. Data on the relationship of grains and weight in children are limited. One prospective study demonstrated smaller annual weight change in relation to each additional serving of breads/grains(Reference Newby, Peterson, Berkey, Leppert, Willett and Colditz39) and another(Reference Barton, Eldridge, Thompson, Affenito, Striegel-Moore, Franko, Albertson and Crockett40) found that cereal consumption was related to lower BMI; neither of these studies distinguished between refined and whole grains. In the current cross-sectional study, we saw that adolescents whose waist circumference was above the 85th percentile reported consuming less discretionary fat than those with less central body fat. There are several possible explanations for this finding. First, reporting bias is a possibility, with more under-reporting of added fat among children with more central adiposity. It could be, however, that more overweight adolescents are in fact consuming less added fat. For example, in our own observations (ML Singer and LL Moore, unpublished results), we found that overweight children and adolescents more often consumed low-fat dairy products than those who are of normal weight. Finally, we note that discretionary fat does not necessarily reflect the total fat load of the diet. The correlations between discretionary fat and percentage of energy from total fat were 0·56 and 0·58 in NHANES III and NHANES 1999–2002 samples, respectively.
Several studies have examined food group intake and central obesity among adults. One such cross-sectional study of middle-aged adults found an inverse relationship between a dietary pattern characterized by frequent intake of raw and salad vegetables and seasonal fruits (and low intakes of fried foods including potatoes) and central obesity(Reference Williams, Prevost, Whichelow, Cox, Day and Wareham18). One prospective study found that a pattern characterized by high intakes of fruit, vegetables, reduced-fat dairy and whole grains and low intakes of red and processed meat was associated with smaller gains in central obesity(Reference Williams, Prevost, Whichelow, Cox, Day and Wareham18), while another found an inverse association between a dietary pattern of high fruits and vegetables and low-fat dairy and WC among women(Reference McNaughton, Mishra, Stephen and Wadsworth41). The CARDIA study identified an inverse association between higher dairy intake and lower waist:hip ratio among young adults(Reference Pereira, Jacobs, Van Horn, Slattery, Kartashov and Ludwig42) and at least one small trial found dairy to be inversely related to central fat loss among obese subjects(Reference Zemel, Richards, Mathis, Milstead, Gebhardt and Silva43). Similar results have been found for whole grain consumption and cereal fibre(Reference Ludwig, Pereira, Kroenke, Hilner, Van Horn, Slattery and Jacobs44, Reference Newby, Maras, Bakun, Muller, Ferrucci and Tucker45). In terms of meat intake, high intakes of both red and processed meat have been shown to be positively related to the likelihood of central weight gain over a 10-year period in several studies(Reference Kahn, Tatham, Rodriguez, Calle, Thun and Heath46, Reference Wagemakers, Prynne, Stephen and Wadsworth47).
A number of possible explanations exist for the findings of these studies. Dairy foods have been hypothesized to be associated with lower levels of body fat through the effects of their Ca content on lipogenesis(Reference Zemel48). Dairy is also an important source of protein and protein-rich diets have been shown to promote satiety(Reference Luhovyy, Akhavan and Anderson49). The dairy protein, whey, is also a rich source of the essential amino acid leucine that is involved in the partitioning of dietary energy(Reference Layman50). The effects of whole grains on obesity are believed to relate to their soluble fibre content, which is associated with increased satiety, delayed gastric emptying and enhanced insulin sensitivity(Reference Slavin51, Reference Koh-Banerjee and Rimm52). Fruits and vegetables are also important sources of fibre and may have similar effects on satiety and satiation(Reference Rolls, Ello-Martin and Tohill53).
The limitations of our exploratory study must be acknowledged. As with any self-reported dietary record, there is the real possibility of misrepresentation of dietary intake. Subjects for whom weight or body proportions are of concern may certainly tend to understate aspects of their intake. The cross-sectional design of NHANES also prevents any conclusions related to cause and effect.
The availability of a single day’s dietary recall limits the precision of the estimated dietary intakes of individuals. However, a single 24 h dietary recall provides accurate estimates of mean dietary intake within groups(Reference Carrera, Xiang and Tucker54). Thus, the recalls used in NHANES are appropriate for quantifying mean food intakes associated with quartiles of central body fat.
The NHANES data set offers important strengths as well. The large, randomly selected group of children and adolescents provides sufficient power to explore a broad range of intake levels in different food groups. The availability of data from each of the USDA Food Pyramid groups, including information from single food sources and mixed dishes, is a strength of the study. Most studies of food effects on health outcomes have relied on intakes from FFQ, which yield less precise estimates of food servings from all sources. For example, it is not possible to extract the actual number of grain servings from all sources in an FFQ since many of the servings would be derived from composite foods such as pizza or lasagne.
In summary, the current cross-sectional study demonstrates an association between the patterns of food intake during adolescence and the prevalence of excess central body fat. The intakes of dairy and grains, especially whole grains, as well as total fruits and vegetables were inversely associated with central obesity among these adolescents. These associations were not fully explained by total body fat as measured by BMI.
The USDA provides food-based dietary guidelines that are specific to age, sex and physical activity level. Prospective studies are needed to test the effects of these recommendations on the development of central obesity in children and adolescents. The present study is an important first step towards such future work.
Acknowledgements
Ethics approval: All analyses were conducted with the approval of the Boston University Institutional Review Board. Sources of funding: The data analysis detailed in the manuscript was partially funded by the National Dairy Council (Rosemont, IL, USA). The National Dairy Council was not, however, directly involved in the study design, data collection, analysis or interpretation of results. Conflict of interest declaration: None. Authorship contributions: M.R.S. was responsible for initial data management and nutritional input. M.M.Q. conducted analyses and contributed to creation of tables. M.L.B. performed the literature search and wrote the manuscript. L.L.M. designed the analysis and edited the final draft of the manuscript.






