Introduction
The distribution of risk and protective factors for disease in the population changes over time. Studying secular trends in exposure to risk and protective factors and their role in observed disease trends may improve the understanding of major causes of disease burden (Lopez et al. Reference Lopez, Mathers, Ezzati, Jamison and Murray2006). It has been well established, for example, that the prevalence of cardiovascular disease (CVD) has declined in recent decades and that this decline can be attributed to a lower exposure to risk factors such as smoking, hypercholesterolemia and high blood pressure (Gregg et al. Reference Gregg, Cheng, Cadwell, Imperatore, Williams, Flegal, Narayan and Williamson2005; Lopez et al. Reference Lopez, Mathers, Ezzati, Jamison and Murray2006). Conversely, the prevalence of diabetes mellitus has increased, which has been attributed to an increased exposure to risk factors such as obesity and sedentary lifestyle (Flegal et al. Reference Flegal, Flegal, Carroll, Carroll, Ogden, Ogden, Curtin and Curtin2010; Geiss et al. Reference Geiss, Wang, Cheng, Thompson, Barker, Li, Albright and Gregg2014). Since major depressive disorder (MDD) is the second leading cause of years lost to disability (YLD) worldwide (Vos et al. Reference Vos, Flaxman, Naghavi, Lozano, Michaud, Ezzati, Shibuya, Salomon, Abdalla, Aboyans, Abraham, Ackerman, Aggarwal, Ahn, Ali, Alvarado, Anderson, Anderson, Andrews, Atkinson, Baddour, Bahalim, Barker-Collo, Barrero, Bartels, Basáñez, Baxter, Bell, Benjamin, Bennett, Bernabé, Bhalla, Bhandari, Bikbov, Bin Abdulhak, Birbeck, Black, Blencowe, Blore, Blyth, Bolliger, Bonaventure, Boufous, Bourne, Boussinesq, Braithwaite, Brayne, Bridgett, Brooker, Brooks, Brugha, Bryan-Hancock, Bucello, Buchbinder, Buckle, Budke, Burch, Burney, Burstein, Calabria, Campbell, Canter, Carabin, Carapetis, Carmona, Cella, Charlson, Chen, Cheng, Chou, Chugh, Coffeng, Colan, Colquhoun, Colson, Condon, Connor, Cooper, Corriere, Cortinovis, de Vaccaro, Couser, Cowie, Criqui, Cross, Dabhadkar, Dahiya, Dahodwala, Damsere-Derry, Danaei, Davis, De Leo, Degenhardt, Dellavalle, Delossantos, Denenberg, Derrett, Des Jarlais, Dharmaratne, Dherani, Diaz-Torne, Dolk, Dorsey, Driscoll, Duber, Ebel, Edmond, Elbaz, Ali, Erskine, Erwin, Espindola, Ewoigbokhan, Farzadfar, Feigin, Felson, Ferrari, Ferri, Fèvre, Finucane, Flaxman, Flood, Foreman, Forouzanfar, Fowkes, Franklin, Fransen, Freeman, Gabbe, Gabriel, Gakidou, Ganatra, Garcia, Gaspari, Gillum, Gmel, Gosselin, Grainger, Groeger, Guillemin, Gunnell, Gupta, Haagsma, Hagan, Halasa, Hall, Haring, Haro, Harrison, Havmoeller, Hay, Higashi, Hill, Hoen, Hoffman, Hotez, Hoy, Huang, Ibeanusi, Jacobsen, James, Jarvis, Jasrasaria, Jayaraman, Johns, Jonas, Karthikeyan, Kassebaum, Kawakami, Keren, Khoo, King, Knowlton, Kobusingye, Koranteng, Krishnamurthi, Lalloo, Laslett, Lathlean, Leasher, Lee, Leigh, Lim, Limb, Lin, Lipnick, Lipshultz, Liu, Loane, Ohno, Lyons, Ma, Mabweijano, MacIntyre, Malekzadeh, Mallinger, Manivannan, Marcenes, March, Margolis, Marks, Marks, Matsumori, Matzopoulos, Mayosi, McAnulty, McDermott, McGill, McGrath, Medina-Mora, Meltzer, Mensah, Merriman, Meyer, Miglioli, Miller, Miller, Mitchell, Mocumbi, Moffitt, Mokdad, Monasta, Montico, Moradi-Lakeh, Moran, Morawska, Mori, Murdoch, Mwaniki, Naidoo, Nair, Naldi, Narayan, Nelson, Nelson, Nevitt, Newton, Nolte, Norman, Norman, O'Donnell, O'Hanlon, Olives, Omer, Ortblad, Osborne, Ozgediz, Page, Pahari, Pandian, Rivero, Patten, Pearce, Padilla, Perez-Ruiz, Perico, Pesudovs, Phillips, Phillips, Pierce, Pion, Polanczyk, Polinder, Pope, Popova, Porrini, Pourmalek, Prince, Pullan, Ramaiah, Ranganathan, Razavi, Regan, Rehm, Rein, Remuzzi, Richardson, Rivara, Roberts, Robinson, De Leòn, Ronfani, Room, Rosenfeld, Rushton, Sacco, Saha, Sampson, Sanchez-Riera, Sanman, Schwebel, Scott, Segui-Gomez, Shahraz, Shepard, Shin, Shivakoti, Singh, Singh, Singh, Singleton, Sleet, Sliwa, Smith, Smith, Stapelberg, Steer, Steiner, Stolk, Stovner, Sudfeld, Syed, Tamburlini, Tavakkoli, Taylor, Taylor, Taylor, Thomas, Thomson, Thurston, Tleyjeh, Tonelli, Towbin, Truelsen, Tsilimbaris, Ubeda, Undurraga, van der Werf, van Os, Vavilala, Venketasubramanian, Wang, Wang, Watt, Weatherall, Weinstock, Weintraub, Weisskopf, Weissman, White, Whiteford, Wiersma, Wilkinson, Williams, Williams, Witt, Wolfe, Woolf, Wulf, Yeh, Zaidi, Zheng, Zonies, Lopez, Murray, AlMazroa and Memish2012), studying secular trends in depression prevalence is of great importance to estimate future healthcare demands and to identify targets for prevention.
Although the majority of available studies suggest that MDD rates have increased in the last few decades (Wickramaratne et al. Reference Wickramaratne, Weissman, Leaf and Holford1989; Joyce et al. Reference Joyce, Oakley-Browne, Wells, Bushnell and Hornblow1990; Weissman, Reference Weissman1992; Fombonne, Reference Fombonne1994; Compton et al. Reference Compton, Conway, Stinson and Grant2006; Eaton et al. Reference Eaton, Kalaydjian, Scharfstein, Mezuk and Ding2007); other studies have shown contrasting results (Srole & Fischer, Reference Srole and Fischer1980; Kessler et al. Reference Kessler, Demler, Frank, Olfson, Pincus, Walters, Wang, Wells and Zaslavsky2005; Hawthorne et al. Reference Hawthorne, Goldney and Taylor2008; de Graaf et al. Reference de Graaf, ten Have, van Gool and van Dorsselaer2012; Simpson et al. Reference Simpson, Meadows, Frances and Patten2012; Spiers et al. Reference Spiers, Brugha, Bebbington, McManus, Jenkins and Meltzer2012). A recent study has stressed the importance of investigating trends in milder depression too because subthreshold depression (SUBD) was more prevalent among later-born birth cohorts (Wiberg et al. Reference Wiberg, Waern, Billstedt, Ostling and Skoog2013). Evidence is growing that SUBD is also an important determinant of public health and a major risk factor for MDD (Meeks et al. Reference Meeks, Vahia, Lavretsky, Kulkarni and Jeste2011). The topic on secular trends in depression prevalence has been one of the ongoing controversies, since it has been questioned whether observed increases in depression rates constitutes ‘true’ increases or have been the result of changes in diagnostic criteria and differences in assessment methods (Hawthorne et al. Reference Hawthorne, Goldney and Taylor2008; Wittchen & Uhmann, Reference Wittchen and Uhmann2010). Moreover, it is not known what factors have contributed to secular trends in depression prevalence.
MDD is preeminently a multifactorial disease, which is determined by an interaction of biological, psychological and social factors according to the biopsychosocial model (Engel, Reference Engel1980). The heritability of MDD has been estimated at 37% (Sullivan et al. Reference Sullivan, Neale and Kendler2000), implying that non-genetic factors explain an important part of the etiology of MDD. It has been suggested that SUBD is determined even more by non-genetic factors than MDD (Beekman et al. Reference Beekman, Deeg, van Tilburg, Smit, Hooijer and van Tilburg1995). This non-genetic influence may best be illustrated by a dynamic equilibrium of multiple interacting risk and protective factors (see Fig. 1) (Fiske et al. Reference Fiske, Wetherell and Gatz2009). For some known risk factors of depression the exposure has declined in recent decades, such as smoking and CVD (Gregg et al. Reference Gregg, Cheng, Cadwell, Imperatore, Williams, Flegal, Narayan and Williamson2005; Raho et al. Reference Raho, van Oostrom, Visser, Huisman, Zantinge, Smit, Verschuren, Hulsegge and Picavet2015); whereas the exposure to other known risk factors has increased, including diabetes mellitus (Geiss et al. Reference Geiss, Wang, Cheng, Thompson, Barker, Li, Albright and Gregg2014), chronic diseases (Crimmins & Beltran-Sanchez, Reference Crimmins and Beltran-Sanchez2011), excessive alcohol consumption (Rice et al. Reference Rice, Neuman, Saccone, Corbett, Rochberg, Hesselbrock, Bucholz, McGuffin and Reich2003) and lack of social support (Ryan et al. Reference Ryan, Smith, Antonucci and Jackson2012). For some known protective factors of depression the exposure has increased, including the educational level (Crimmins & Saito, Reference Crimmins and Saito2001), socioeconomic advantages (Broese van Groenou & Deeg, Reference Broese van Groenou and Deeg2010) and management of depression (Kessler et al. Reference Kessler, Demler, Frank, Olfson, Pincus, Walters, Wang, Wells and Zaslavsky2005); while exposure to religiousness has decreased (Peri-Rotem, Reference Peri-Rotem2016). An ambiguous effect has been described for the dramatic shift in dual family and work roles for women after World War II (Kasen et al. Reference Kasen, Cohen, Chen and Castille2003). This dual role may entail both a risk and protective factor, due to higher stress levels and meaningful engagement in life, respectively (Kasen et al. Reference Kasen, Cohen, Berenson, Chen and Dufur2005). Whether the prevalence of MDD and SUBD has been influenced by secular trends in risk and protective factors for depression has not been studied yet.

Fig. 1. Strong simplification of a dynamic equilibrium between multiple risks and protective factors determining depression outcome. For example, a moderate risk (a) with low protection (b) may result in SUBD (d), whereas a moderate risk (a) with high protection (c) may not result in depression (e).
In order to identify secular trends properly, it is important to select a study population with an age range that likely has undergone the greatest change in risk and protective factors in the past few decades and to use consistent diagnostic criteria across cohorts (Satizabal et al. Reference Satizabal, Beiser, Chouraki, Chêne, Dufouil and Seshadri2016). Moreover, from a clinical point of view, the study population should be a suitable target for prevention. We assumed that 55–64-year olds were most appropriate for this purpose because this group is young enough to experience secular trends in psychosocial circumstances, such as dual roles, and old enough to experience secular trends in the occurrence of health problems, such as somatic diseases and disability.
The aim of the present paper is to explore whether and to what extent a dynamic equilibrium of multiple risk and protective factors is associated with depression outcome over two decades among three population-based cohorts of 55–64-year olds in the Netherlands. First, we hypothesize that the prevalence of MDD remains stable due to a balance in risk and protective factors. Second, in contrast to MDD, we hypothesize that the prevalence of SUBD will fluctuate more according to secular trends in psychosocial circumstances.
Methods
Study sample
Data were used from the Longitudinal Aging Study Amsterdam (LASA), an ongoing prospective population-based-study in the Netherlands. Sampling procedures have been previously described (Huisman et al. Reference Huisman, Poppelaars, van der Horst, Beekman, Brug, van Tilburg and Deeg2011; Hoogendijk et al. Reference Hoogendijk, Deeg, Poppelaars, van der Horst, Broese van Groenou, Comijs, Pasman, van Schoor, Suanet, Thomése, van Tilburg, Visser and Huisman2016). In short, in 1992/93 the first cohort (N = 3107, birth years 1908–1937) was recruited from the population registries of 11 municipalities in three geographic areas of the Netherlands including a random sample of 55–85-year-old men and women, stratified by age and sex according to the expected 5-year mortality. The cooperation rate of the first cohort was 62%, also for the 55–64-year olds subsample. In 2002/03 and 2012/13, a second (N = 1002, birth years 1938–1947) and third cohort (N = 1023, birth years 1948–1957) were recruited, respectively, both including a random sample of 55–64-year olds selected from the same sampling frame and measured identically to the first cohort. The cooperation rates were 62 and 63% for the second and third cohort, respectively. All interviews were conducted in the homes of the respondents by trained and supervised interviewers.
The present study involved a cohort comparison of both depression outcome and the exposure to risk and protective factors covering 20 years of time. A strict age limit of 55–64-years was applied resulting in the inclusion of N = 2951 respondents (N = 964 from the first, N = 996 from the second and N = 991 from the third cohort). Subsequently, N = 86 respondents were excluded (N = 20 from the first, N = 32 from the second, and N = 34 from the third cohort) due to missing data on depression outcome leaving a total sample of N = 2865 respondents, including N = 944 in the first, N = 964 in the second and N = 957 in the third cohort. Written informed consent was obtained from all respondents. The Ethical Review Board of the VU University Medical Center approved the study.
Dependent variable
A two-stage-screening design was used to identify SUBD and MDD as follows. First, the Center for Epidemiological Studies Depression Scale (CES-D) was applied to identify respondents with clinically relevant depression (cut-off score CES-D ⩾ 16) (Radloff, Reference Radloff1977). The psychometric properties of the CES-D were found to be good (Beekman et al. Reference Beekman, Deeg, Van Limbeek, Braam, De Vries and Van Tilburg1997). Second, in respondents who screened positive in the first stage (CES-D ⩾ 16), the Diagnostic Interview Schedule (DIS) was scheduled 2–8 weeks after the CES-D interview (Robins et al. Reference Robins, Helzer, Croughan and Ratcliff1981). Depression outcome was defined as a variable containing three categories. Respondents without clinically relevant depression (CES-D < 16) were indicated as having no depression. Respondents with clinically relevant depression (CES-D ⩾ 16) but without a past-year diagnosis of MDD according to the DIS were indicated as having SUBD. Respondents with clinically relevant depression (CES-D ⩾ 16) and also a past-year diagnosis of MDD were indicated as having MDD.
Main independent variable
The ‘cohort’ variable was categorized into three groups; we refer to these cohorts as the ‘early cohort’ (1992/93), ‘middle cohort’ (2002/03) and ‘recent cohort’ (2012/13).
Explanatory independent variables
Based on two literature reviews among community-dwelling older adults aged 55 years or older (Cole & Dendukuri, Reference Cole and Dendukuri2003; Vink et al. Reference Vink, Aartsen and Schoevers2008), putative risk and protective factors were included from biological, psychological and social domains of functioning. According to the literature and based on biological plausibility, factors were considered either a risk or protective factor.
The following risk factors were included. Urbanicity was dichotomized according to the postal code density in ‘city’ (>1000 addresses/km2) v. ‘rural’ (<1000 addresses/km2) (Den Dulk et al. Reference Den Dulk, Van De Stadt and Vliegen1992). The number of chronic diseases was assessed by self-report on current diseases and included CVD, diabetes mellitus, cancer, cerebrovascular accident (CVA), arthritis and chronic-obstructive-pulmonary disease (COPD) (range, 0–7) (Kriegsman et al. Reference Kriegsman, Penninx, Van Eijk, Boeke and Deeg1996). Functional limitations were measured by self-report and dichotomized in ‘none’ v. ‘one or more’ limitations (McWhinnie, Reference McWhinnie1981). Body mass index (BMI) was calculated as measured body weight (kg) divided by measured height (m2). Pain was measured by the Nottingham Pain Profile scale (range, 5–10) (Hunt et al. Reference Hunt, McEwen and McKenna1985). Sleep problems were measured with a four-item self-questionnaire (range, 3–12) (Hunt et al. Reference Hunt, McEwen and McKenna1985). Alcohol consumption was measured by the number of alcohol units consumed per day (u/d) and categorized into: abstainer (0 u/d), moderate (men, 1–3 u/d; women, 1–2 u/d) and excessive (men, ⩾4 u/d; women, ⩾3 u/d) (Netherlands Central Bureau of Statistics, 1989). Smoking was dichotomized into ‘current smoker or stopped ⩽15 years ago’ v. ‘never smoked or stopped >15 years’ (Visser et al. Reference Visser, Launer, Deurenberg and Deeg1999). Physical activity was measured by calculating the total time in minutes per day spent on physical activity (Stel et al. Reference Stel, Smit, Pluijm, Visser, Deeg and Lips2004). Neuroticism was measured with a 25-item subset from the 36-item Dutch Personality Questionnaire (range, 0–50) (Luteijn et al. Reference Luteijn, Starren and Van Dijk1975). Loneliness was assessed with the de Jong-Gierveld Loneliness Scale (range, 0–11) (de Jong-Gierveld & Kamphuis, Reference de Jong-Gierveld and Kamphuis1985).
The following protective factors were included. Religiousness was dichotomized in having a religion or not. Partner status was dichotomized in having a partner in or outside the household v. no partner. Education was based on the number of years of education (range, 5–18). Labor market participation was assessed by self-report. Physical performance was measured with three performance tests (range, 0–12) (Penninx et al. Reference Penninx, Deeg, Van Eijk, Beekman and Guralnik2000). General cognitive functioning was measured with the Mini Mental State Examination (range, 0–30) (Folstein et al. Reference Folstein, Folstein and McHugh1975). Mastery was measured with a translated and abbreviated Dutch version of the Pearlin Mastery Scale (range, 5–25) (Pearlin & Schooler, Reference Pearlin and Schooler1978). Personal network size was based on the total number of network members (range, 0–75); and the exchange of social support (both instrumental and emotional) was collected for nine network members whom the respondent had the most frequent contact with (range, 0–36) (van Tilburg, Reference van Tilburg1998).
Use of antidepressants and benzodiazepines were assessed by directly recording the medication from drug containers in the home of the respondents (Sonnenberg et al. Reference Sonnenberg, Deeg, Comijs, van Tilburg and Beekman2008). All scales were either previously validated in comparable samples in the Netherlands or in LASA pilot studies (Deeg et al. Reference Deeg, Knipscheer and Van Tilburg1993). Because the dataset contained more than 5% missing values in some risk and protective factors, multiple imputations (MI) were performed, including 25 imputations and 50 iterations.
Statistical analyses
Descriptive statistics were performed on complete-cases data and weighted according to the distribution of age and sex in the recent cohort. This was done to make sure that changes in the prevalence of depression reflected secular trends and were not due to distributional differences in age and sex. All risk and protective factors were separately investigated for their explanatory ability. Chi-square and t tests were performed to examine the association between each factor with both ‘cohort’ and ‘depression outcome’. For this preliminary exploration, a liberal p-level <0.30 was used so as not to miss important explanatory factors (Berner et al. Reference Berner, Aartsen, Wahlberg and Elmståhl2016). Factors associated with both ‘cohort’ (Table 1) and ‘depression outcome’ (eTable 1, supplemental) were considered as potential explanatory factors.
Table 1. Sample characteristics and secular trends in the exposure to risk and protective factors
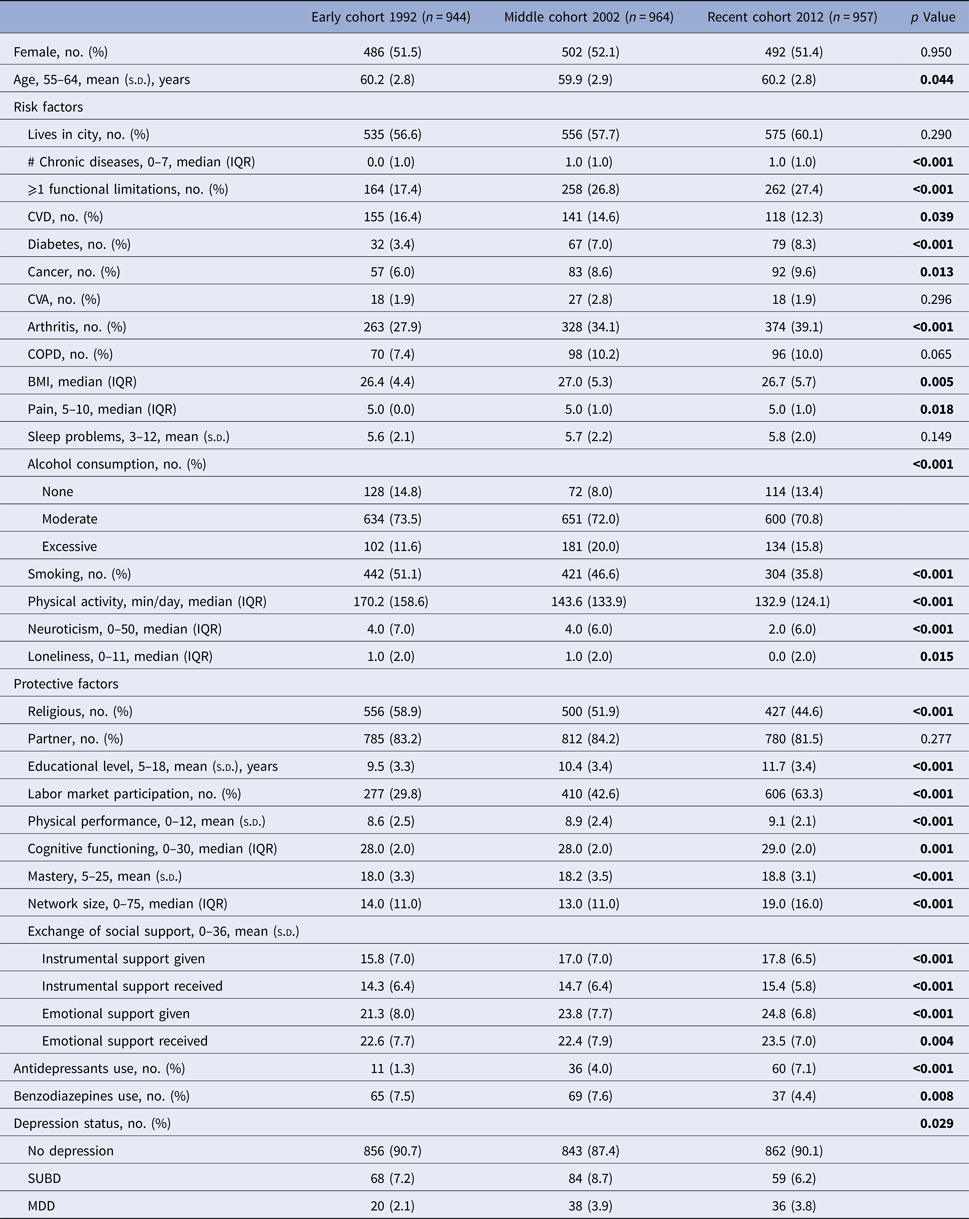
#, number of; s.d., standard deviation; IQR, interquartile range. Bold = statistically significant at p < 0.05.
χ2 values have been computed for categorical variables and t-values for interval variables. Independent-sample Kruskal–Wallis tests were conducted to determine non-parametric variables.
Further analyses performed with multinomial logistic regression were not weighted since all models were standard adjusted for age and sex. A basic model was created to test the association between ‘cohort’ and ‘depression outcome’, adjusted for age and sex, to estimate the degree of secular trends in the prevalence of MDD and SUBD. The middle and recent cohorts were compared with the early cohort (=reference) and an additional comparison was made between the recent and the middle cohort (=reference). Subsequently, potential explanatory factors were manually entered one by one into the basic model and the % change in odds ratio of ‘cohort’ (ORcohort) was estimated for MDD (Table 2) and SUBD (Table 3). The % change in (ORcohort) was calculated with following formulas: if OR > 1: [(ORmodel x – ORbasic model)/(ORbasic model − 1) × 100]; if OR < 1: [(ORbasic model – ORmodelx)/(ORbasic model − 1) × 100] (Richter et al. Reference Richter, Moor and van Lenthe2012).
Table 2. Factors associated with an increase in the prevalence of MDD among 55–64-year olds in 2002 and 2012 compared with 1992
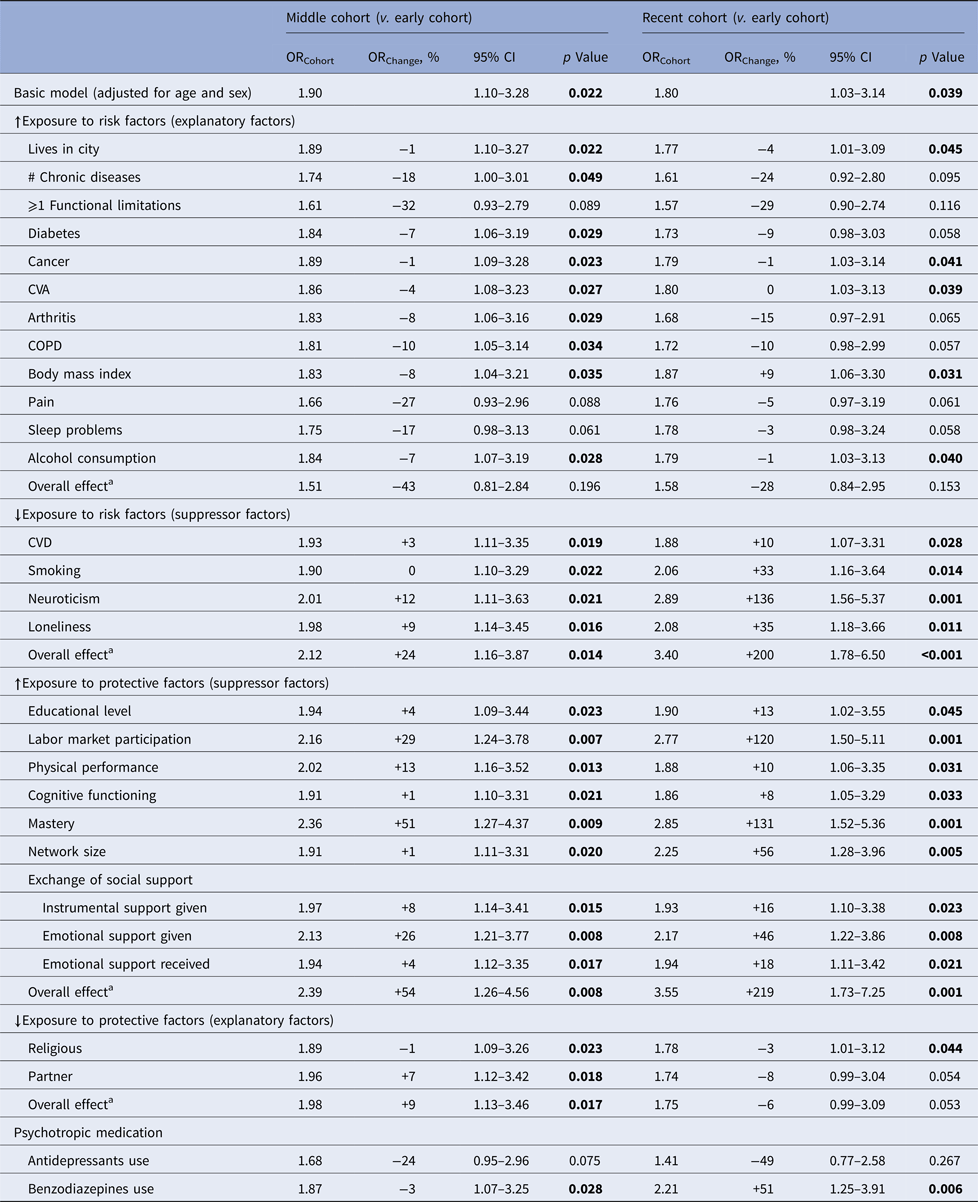
OR, odds ratio; all factors were manually entered one by one into the basic model and the % change in ORCohort was estimated (ORChange). Bold = statistically significant at p < 0.05.
a Multivariable analyses were performed to estimate the cumulative effect within groups.
Table 3. Factors associated with a decrease in prevalence of SUBD in 2012 compared with 2002
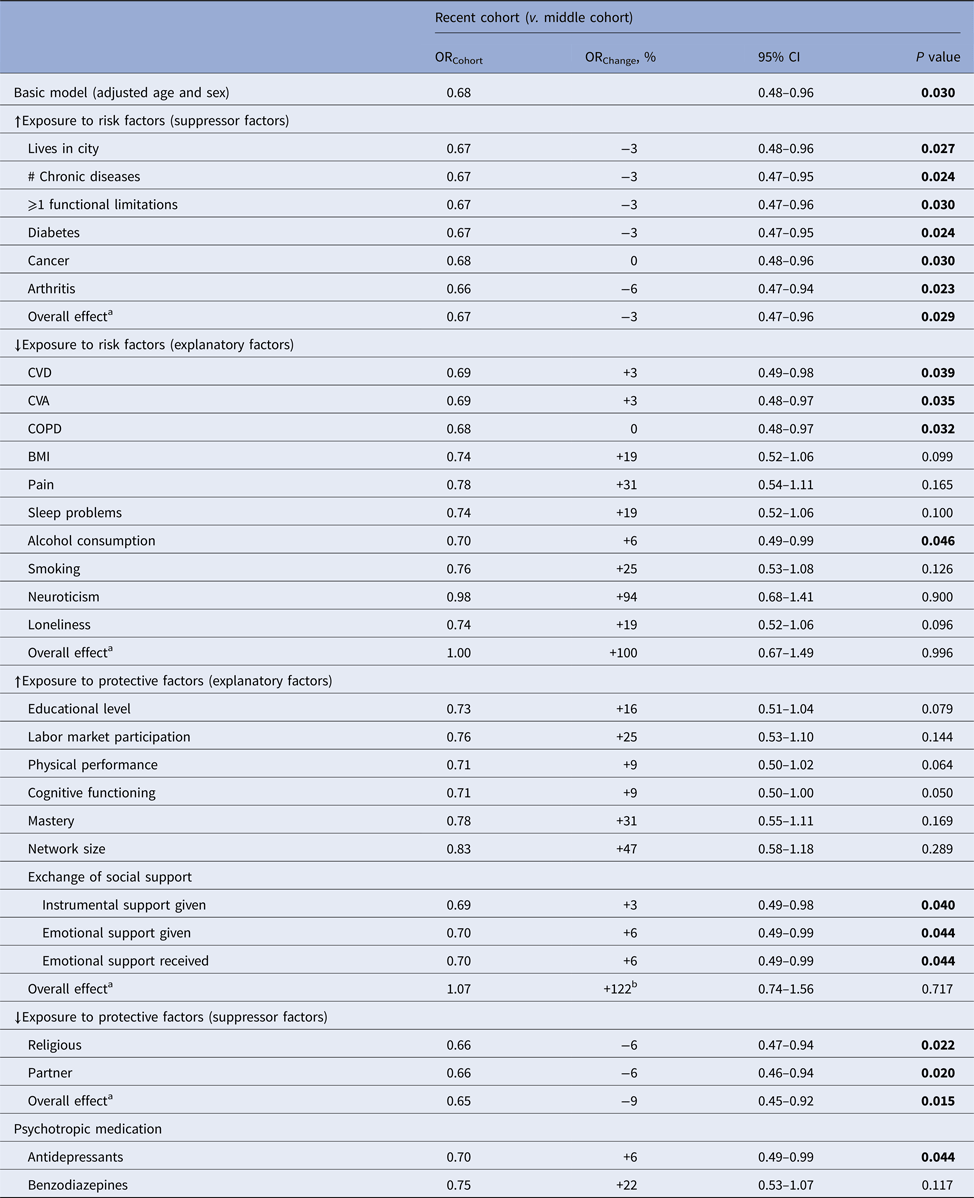
OR, odds ratio; all factors were manually entered one by one into the basic model and the % change in ORCohort was estimated (ORChange). Bold = statistically significant at p < 0.05.
a Multivariable analyses were performed to estimate the cumulative effect within groups.
b Read (ORChange) of 122% as 100%.
Factors were considered to be explanatory when two conditions were met after entering the basic model: first the magnitude of the association (ORcohort) was reduced: thus decrease in OR if OR > 1 or increase in OR if OR < 1, accompanied by a decrease in p value, and second the % change (ORcohort) was ⩾10%. Factors were considered to be suppressors when the opposite was observed: first the magnitude of the association (ORcohort) became stronger: thus decrease in OR if OR < 1 or increase in OR if OR > 1, accompanied by an increase in p value, and second the % change (ORcohort) was ⩾10% (Twisk, Reference Twisk2007). Finally, multivariable analyses were performed to estimate the total percentage that could be explained by adjusting the basic model subsequently for the overall influence of suppressors, the overall influence of explanatory factors and finally for psychotropic medication (Table 4). Data analyses were conducted with SPSS v22 and Stata v12.
Table 4. Multivariable analyses secular trends in prevalence of MDD and SUBD
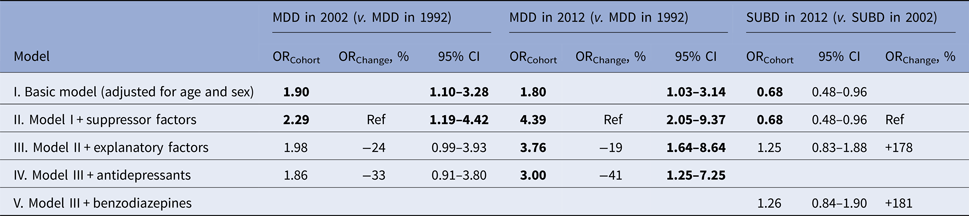
OR, odds ratio; bold = significant (95% CI does not include 1); Ref = reference OR to calculate % change.
Multivariable analyses estimated the total percentage that could be explained by subsequently adjusting the basic model (model I) for the cumulative suppression effect (model II) and cumulative explanatory effect (model III). MDD models were adjusted for antidepressants (model IV), SUBD for benzodiazepines (model V).
Results
Table 1 shows the past-year prevalence of MDD in 1992, 2002 and 2012, which was 2.1, 3.9 and 3.8%, respectively. The point prevalence of SUBD in 1992, 2002 and 2012 was 7.2, 8.7 and 6.2%, respectively. There is an increase in the use of antidepressants in successive cohorts. The use of benzodiazepines declined in the recent cohort. Also shown in Table 1 are the secular trends in the exposure to risk and protective factors.
Secular trends in the exposure to risk and protective factors
It can be seen that among the risk factors: chronic diseases, functional limitations, diabetes, cancer and arthritis are more prevalent in successive cohorts; whereas the prevalence of CVD, smoking, physical activity, neuroticism and loneliness has decreased. Among the protective factors: successive cohorts have an increase in the exposure to educational level, labor market participation, cognitive functioning, mastery and exchange of social support; while the exposure to religiousness and physical performance has decreased. The exposure to other factors, such as CVA, COPD, pain, sleep problems, alcohol consumption and network size, fluctuated between cohorts.
Secular trends in MDD prevalence and explanatory factors
The prevalence of MDD in both the middle cohort (OR 1.90, 95% CI 1.10–3.28, p = 0.022) and recent cohort (OR 1.80, 95% CI 1.03–3.14, p = 0.039) is higher than the early cohort (Table 2). However, compared with the middle cohort, the prevalence of MDD remained stable (OR 0.95, 95% CI 0.60–1.51, p = 0.82). Subsequently, the potential explanatory and suppressor effect of each factor is shown in Table 2. The number of chronic diseases, functional limitations, arthritis and COPD was found to have an explanatory ability in both the middle and recent cohorts. Additionally, pain and sleep problems were only associated with the increase in MDD rates in the middle cohort.
Several factors suppressed the relationship between ‘cohort’ and ‘MDD outcome’. Common factors for both cohorts are neuroticism, labor market participation, physical performance, mastery and emotional support given. In addition, only in the recent cohort suppressor effects are also seen for CVD, smoking, loneliness, educational level, network size, instrumental support given and emotional support received. After adjustment for all suppressors the (ORcohort) increased 1.2 times in the middle and 2.4 times in the recent cohort (Table 4). This can be understood as follows: if the prevalence of the suppressor factors had been stable over time, the prevalence of MDD would have been even much higher. Table 4 shows the overall influence of suppression and explanatory effects. The increase in the prevalence of health problems partly explained (24%) the rise in MDD rates. The use of antidepressants had an additional explanatory effect.
Secular trends in SUBD prevalence and explanatory factors
The prevalence of SUBD in the middle (OR 1.29, 95% CI 0.92–1.80, p = 0.143) and recent cohort (OR 0.87, 95% CI 0.61–1.26, p = 0.471) as compared with the early cohort remained stable. The SUBD prevalence found in the recent cohort was lower (OR 0.68, 95% CI 0.48–0.96, p = 0.03) than the middle cohort (Table 3). This decline in SUBD rates was not suppressed and could entirely be explained by both the overall effect of a decrease in prevalence of risk factors (BMI, pain, sleep problems, smoking, neuroticism and loneliness) and by an increase in the prevalence of protective factors (educational level, labor market participation, mastery and network size). Use of benzodiazepines had no additional explanatory effect (Table 4).
Discussion
The study of secular trends in mental health is a matter of historical and current importance. Already in 1980, Srole and Fischer challenged claims of deteriorating mental health in successive generations, which had been postulated by the Mental Paradise Lost doctrine (Srole & Fischer, Reference Srole and Fischer1980). To date, however, MDD has become the second leading cause of YLD worldwide (Vos et al. Reference Vos, Flaxman, Naghavi, Lozano, Michaud, Ezzati, Shibuya, Salomon, Abdalla, Aboyans, Abraham, Ackerman, Aggarwal, Ahn, Ali, Alvarado, Anderson, Anderson, Andrews, Atkinson, Baddour, Bahalim, Barker-Collo, Barrero, Bartels, Basáñez, Baxter, Bell, Benjamin, Bennett, Bernabé, Bhalla, Bhandari, Bikbov, Bin Abdulhak, Birbeck, Black, Blencowe, Blore, Blyth, Bolliger, Bonaventure, Boufous, Bourne, Boussinesq, Braithwaite, Brayne, Bridgett, Brooker, Brooks, Brugha, Bryan-Hancock, Bucello, Buchbinder, Buckle, Budke, Burch, Burney, Burstein, Calabria, Campbell, Canter, Carabin, Carapetis, Carmona, Cella, Charlson, Chen, Cheng, Chou, Chugh, Coffeng, Colan, Colquhoun, Colson, Condon, Connor, Cooper, Corriere, Cortinovis, de Vaccaro, Couser, Cowie, Criqui, Cross, Dabhadkar, Dahiya, Dahodwala, Damsere-Derry, Danaei, Davis, De Leo, Degenhardt, Dellavalle, Delossantos, Denenberg, Derrett, Des Jarlais, Dharmaratne, Dherani, Diaz-Torne, Dolk, Dorsey, Driscoll, Duber, Ebel, Edmond, Elbaz, Ali, Erskine, Erwin, Espindola, Ewoigbokhan, Farzadfar, Feigin, Felson, Ferrari, Ferri, Fèvre, Finucane, Flaxman, Flood, Foreman, Forouzanfar, Fowkes, Franklin, Fransen, Freeman, Gabbe, Gabriel, Gakidou, Ganatra, Garcia, Gaspari, Gillum, Gmel, Gosselin, Grainger, Groeger, Guillemin, Gunnell, Gupta, Haagsma, Hagan, Halasa, Hall, Haring, Haro, Harrison, Havmoeller, Hay, Higashi, Hill, Hoen, Hoffman, Hotez, Hoy, Huang, Ibeanusi, Jacobsen, James, Jarvis, Jasrasaria, Jayaraman, Johns, Jonas, Karthikeyan, Kassebaum, Kawakami, Keren, Khoo, King, Knowlton, Kobusingye, Koranteng, Krishnamurthi, Lalloo, Laslett, Lathlean, Leasher, Lee, Leigh, Lim, Limb, Lin, Lipnick, Lipshultz, Liu, Loane, Ohno, Lyons, Ma, Mabweijano, MacIntyre, Malekzadeh, Mallinger, Manivannan, Marcenes, March, Margolis, Marks, Marks, Matsumori, Matzopoulos, Mayosi, McAnulty, McDermott, McGill, McGrath, Medina-Mora, Meltzer, Mensah, Merriman, Meyer, Miglioli, Miller, Miller, Mitchell, Mocumbi, Moffitt, Mokdad, Monasta, Montico, Moradi-Lakeh, Moran, Morawska, Mori, Murdoch, Mwaniki, Naidoo, Nair, Naldi, Narayan, Nelson, Nelson, Nevitt, Newton, Nolte, Norman, Norman, O'Donnell, O'Hanlon, Olives, Omer, Ortblad, Osborne, Ozgediz, Page, Pahari, Pandian, Rivero, Patten, Pearce, Padilla, Perez-Ruiz, Perico, Pesudovs, Phillips, Phillips, Pierce, Pion, Polanczyk, Polinder, Pope, Popova, Porrini, Pourmalek, Prince, Pullan, Ramaiah, Ranganathan, Razavi, Regan, Rehm, Rein, Remuzzi, Richardson, Rivara, Roberts, Robinson, De Leòn, Ronfani, Room, Rosenfeld, Rushton, Sacco, Saha, Sampson, Sanchez-Riera, Sanman, Schwebel, Scott, Segui-Gomez, Shahraz, Shepard, Shin, Shivakoti, Singh, Singh, Singh, Singleton, Sleet, Sliwa, Smith, Smith, Stapelberg, Steer, Steiner, Stolk, Stovner, Sudfeld, Syed, Tamburlini, Tavakkoli, Taylor, Taylor, Taylor, Thomas, Thomson, Thurston, Tleyjeh, Tonelli, Towbin, Truelsen, Tsilimbaris, Ubeda, Undurraga, van der Werf, van Os, Vavilala, Venketasubramanian, Wang, Wang, Watt, Weatherall, Weinstock, Weintraub, Weisskopf, Weissman, White, Whiteford, Wiersma, Wilkinson, Williams, Williams, Witt, Wolfe, Woolf, Wulf, Yeh, Zaidi, Zheng, Zonies, Lopez, Murray, AlMazroa and Memish2012). The most important conclusion to be drawn from this study is that we found a substantial secular trend in the prevalence of MDD among late middle-aged adults, which is influenced by a dynamic equilibrium of more or less modifiable risk and protective factors.
Contrary to our expectations, we found an almost twofold increase in MDD prevalence in 2002 and 2012 than in 1992. The prevalence of MDD remained stable between 2002 and 2012. The increase in MDD rates was largely attributable to an increase in the prevalence of health problems in the two more recent cohorts, including chronic diseases, functional limitations, arthritis, COPD, pain and sleep problems. Moreover, if the prevalence of CVD, smoking, loneliness and neuroticism had not decreased and mastery, labor market participation, network size and exchange of social support had not increased, the prevalence of MDD would have been 1.2 and 2.4 times higher in 2002 and 2012, respectively. Furthermore, we observed a 32% decline in SUBD prevalence in 2012 as compared with 2002, which was entirely associated with a decrease in risk and an increase in protective factors mainly from psychosocial domains of functioning.
The finding that MDD is more prevalent in successive generations has been extensively described (Wickramaratne et al. Reference Wickramaratne, Weissman, Leaf and Holford1989; Joyce et al. Reference Joyce, Oakley-Browne, Wells, Bushnell and Hornblow1990; Weissman, Reference Weissman1992; Fombonne, Reference Fombonne1994; Compton et al. Reference Compton, Conway, Stinson and Grant2006; Eaton et al. Reference Eaton, Kalaydjian, Scharfstein, Mezuk and Ding2007). However, other studies have found that the prevalence of MDD is stable (Kessler et al. Reference Kessler, Demler, Frank, Olfson, Pincus, Walters, Wang, Wells and Zaslavsky2005; de Graaf et al. Reference de Graaf, ten Have, van Gool and van Dorsselaer2012; Simpson et al. Reference Simpson, Meadows, Frances and Patten2012; Spiers et al. Reference Spiers, Brugha, Bebbington, McManus, Jenkins and Meltzer2012). Moreover, a debate is ongoing whether increasing MDD rates constitute a ‘true’ increase or is due to methodological heterogeneity and recall artifacts (Hawthorne et al. Reference Hawthorne, Goldney and Taylor2008; Wittchen & Uhmann, Reference Wittchen and Uhmann2010). Warshaw et al. (Reference Warshaw, Klerman and Lavori1991) have refuted that recall artifacts explain secular trends in MDD prevalence (Warshaw et al. Reference Warshaw, Klerman and Lavori1991). Few scholars have examined secular trends in SUBD prevalence. Recently Wiberg et al. (Reference Wiberg, Waern, Billstedt, Ostling and Skoog2013) have found that SUBD prevalence increased substantially among 75-year olds from 1976–1977 to 2005–2006 (Wiberg et al. Reference Wiberg, Waern, Billstedt, Ostling and Skoog2013). This discrepant finding may be attributed to differences in age range, but this needs further study.
For a few known risk and protective factors of depression secular trends have been described in the literature to date; however, for the majority of factors, this information was largely lacking. The finding that more recent cohorts were more exposed to chronic diseases, diabetes mellitus, arthritis, COPD, sleep problems and disability corresponds to other studies (Lopez et al. Reference Lopez, Mathers, Ezzati, Jamison and Murray2006; Mannino & Buist, Reference Mannino and Buist2007; Crimmins & Beltran-Sanchez, Reference Crimmins and Beltran-Sanchez2011). In Western societies, the overall prevalence of chronic diseases is increasing due to the aging of the population and the greater longevity of people with chronic conditions. Crimmins & Beltran-Sanchez (Reference Crimmins and Beltran-Sanchez2011) reviewed the literature on trends in mortality and morbidity in the USA and found that although mortality has declined, the prevalence of diseases has increased (Crimmins & Beltran-Sanchez, Reference Crimmins and Beltran-Sanchez2011). Also, mobility functioning has deteriorated and length of life with disease and mobility functioning loss has increased between 1998 and 2008. Literature is available that found the same deteriorating health trends for the situation in the Netherlands using different data (van Oostrom et al. Reference van Oostrom, Gijsen, Stirbu, Korevaar, Schellevis, Picavet and Hoeymans2016). Also, a decrease in the prevalence of CVD and smoking was found, which have been previously described (Gregg et al. Reference Gregg, Cheng, Cadwell, Imperatore, Williams, Flegal, Narayan and Williamson2005; Raho et al. Reference Raho, van Oostrom, Visser, Huisman, Zantinge, Smit, Verschuren, Hulsegge and Picavet2015). Remarkable was the finding that neuroticism, a personality trait strongly associated with a genetic predisposition, declined in more recent cohorts. A possible explanation might be that neuroticism later in life is influenced more by non-genetic factors, such as occupation; however, this issue needs further empirical study. The finding that educational level, labor market participation, mastery and network size had increased in more recent cohorts has been supported by others and indicate that socioeconomic and psychosocial circumstances have improved for more recent generations (Hoogendijk et al. Reference Hoogendijk, van Groenou, van Tilburg and Deeg2008; Broese van Groenou & Deeg, Reference Broese van Groenou and Deeg2010; Suanet et al. Reference Suanet, Van Tilburg and Van Groenou2013). The finding that an increased use of antidepressants in 2002 and 2012 as compared with 1992 had an additional explanatory effect on the secular trends found in MDD prevalence may be the consequence of improved recognition and treatment of MDD (Kessler et al. Reference Kessler, Demler, Frank, Olfson, Pincus, Walters, Wang, Wells and Zaslavsky2005; Sonnenberg et al. Reference Sonnenberg, Deeg, Comijs, van Tilburg and Beekman2008; Simpson et al. Reference Simpson, Meadows, Frances and Patten2012), possibly since the introduction of selective serotonin reuptake inhibitors (SSRIs) around 1990. Antidepressants may be seen as a proxy for the (increased) recognition and detection of people with MDD. Sonnenberg et al. (Reference Sonnenberg, Deeg, Comijs, van Tilburg and Beekman2008) already found that the rise in the use of antidepressants between 1992 and 2002 was mainly attributable to a rise in the use of SSRIs (Sonnenberg et al. Reference Sonnenberg, Deeg, Comijs, van Tilburg and Beekman2008).
A major strength of this population-based epidemiological study is the rigorous design. LASA is primed to examine cohort differences in a reliable and valid manner by using identical measurements across cohorts, including a two-stage screening design to identify cases of SUBD and cases with a past-year diagnosis of MDD. The approach to include SUBD in the cohort comparison is, to our understanding, unique and important because evidence has been collected that SUBD is also a crucial determinant of public health and major risk factor for MDD (Meeks et al. Reference Meeks, Vahia, Lavretsky, Kulkarni and Jeste2011; Jeuring et al. Reference Jeuring, Huisman, Comijs, Stek and Beekman2016). Furthermore, essential information was gathered concerning secular trends in risk and protective factors for depression, which can be vital for future research. Some limitations need to be taken into account. First, the cross-sectional observational design does not allow causal conclusions and cannot distinguish well between cohort and period effects. It is unclear whether the more recent cohorts were especially prone to MDD (birth cohort factors) or that 2002 and 2012 were especially depressing times (period factors). Second, because the cooperation rates of the three cohorts ranged between 62 and 63%, this design holds the risk of selective non-response bias. However, the cooperation rates of the three cohorts are quite similar. Third, this study cannot answer the question whether an increased influx of new MDD cases, i.e. higher incidence, or an increased chronicity of prevalent MDD cases contributed to the higher prevalence found in recent cohorts. Future research should focus on longitudinal cohort differences with regard to the (first) onset, course and outcome of depression, including disability and mortality.
Nevertheless, this study has important implications. Assuming that MDD rates ‘truly’ increase, despite improvement in psychiatric treatment, socioeconomic and psychosocial circumstances, we can expect a continued increase in the burden of disease that will challenge the field of mental and public health. The finding that an increase in chronic diseases and functional limitations was associated with an increase in MDD in more recent generations of 55–64-year olds is alarming, since the number of older people in the population is growing and, simultaneously, those suffering from one or more chronic diseases and functional impairments. Moreover, in a previous study on the long-term prognosis of SUBD (Jeuring et al. Reference Jeuring, Huisman, Comijs, Stek and Beekman2016), we found that community-dwelling older adults with SUBD were particularly at risk of developing MDD when chronic diseases, high BMI, or unhealthy lifestyles were present. Lessons must be learned from somatic medicine, as CVD has become less prevalent in recent decades through a lower exposure to CVD risk factors (Gregg et al. Reference Gregg, Cheng, Cadwell, Imperatore, Williams, Flegal, Narayan and Williamson2005). From a public health policy perspective, caregivers should pay attention to the presence of clinically relevant depressive symptoms in the growing group of people that is (or becomes) medically and physically compromised. This role may be suited to the general practitioner, but does also apply to the medical specialist in the hospital who treats patients with chronic diseases. Subsequently, for the purpose of indicated prevention of MDD, psychiatric counseling may be arranged. Additionally, physical activity has been associated with helping individuals maintain good physical and cognitive function throughout life and in older adults also with developing fewer chronic diseases (Lee et al. Reference Lee, Shiroma, Lobelo, Puska, Blair and Katzmarzyk2012), which in turn may contribute to the prevention of depression in later life.
To conclude, our study showed a pessimistic prospect of increasing MDD rates; however, SUBD rates showed a recent decline. Putative targets were identified for the purpose of preventive psychiatry and public health policies, which may help to reduce the worldwide disease burden of depression.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291717003324
Acknowledgements
The Longitudinal Aging Study Amsterdam is financed primarily by the Netherlands Ministry of Health, Welfare and Sports. The sponsor had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication.
Author contributions
HWJ had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors made substantial contributions to study concept and design. All authors involved with acquisition, analysis or interpretation of data. HWJ drafted the manuscript. All authors involved in critical revision of the manuscript for important intellectual content.
HCC, DJHD and MH provided administrative, technical or material support.
HCC, DJHD, MLS, MH and ATFB performed study supervision.
Declaration of interest disclosures
None.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
Additional contributions
We thank participants and interviewers of the LASA study.







