There has been increasing concern about the recruitment crisis into psychiatry in the UK (Reference Brockington and MumfordBrockington & Mumford, 2002; Reference StorerStorer, 2002) and in other countries, including North America (Reference Sierles and TaylorSierles & Taylor, 1995; Reference Weintraub, Plaut and WeintraubWeintraub et al, 1999). Studies examining the career preferences of newly-qualified doctors in the UK indicate that only about 4% specify psychiatry as their first preference (Reference Lambert, Goldacre and EdwardsLambert et al, 1996), although the number entering psychiatric training (about 8%) is greater than expected from the career aims of graduands (Reference Brockington and MumfordBrockington & Mumford, 2002). Many studies have investigated factors influencing medical students in their choice of psychiatry as a career, including personality, perceived lifestyle, family background and the effect of the undergraduate medical curriculum (Reference Eagle and MarcosEagle & Marcos, 1981; Reference Zimney and LindberghZimney & Lindbergh, 1986; Reference Mobray, Davies and BiddleMobray et al, 1990; Reference Ney, Tam and MauriceNey et al, 1990; Reference Lee, Kaltreider and CrouchLee et al, 1995). We wanted to investigate whether participation in a scheme in which first-year clinical medical students take on a patient for supervised psychotherapy is a factor in leading them to choose a career in psychiatry after qualification.
The Student Psychotherapy Scheme (SPS) was initiated 43 years ago in the Out-patient Department of Psychological Medicine of University College Hospital (UCH), London (Reference Ball and WolffBall & Wolff, 1963; Reference Sturgeon, Wolff, Knauss and BrautigamSturgeon, 1983). It has continued to operate under the aegis of the Royal Free and University College Medical School Department of Psychiatry and Behavioural Sciences, as a special option offered to first year clinical medical students in the Camden and Islington Mental Health and Social Care Trust Department of Psychotherapy, based at the University College London Hospitals (UCLH) Trust. The scheme helps medical students learn about the doctor-patient relationship in greater depth by allowing them to see a carefully selected out-patient for once-weekly psychodynamic psychotherapy for one year, under weekly supervision from one of the senior members of the department (Reference GarnerGarner, 1981; Reference Clifford, Lacey and SturgeonClifford, 1986; Reference ShoenbergShoenberg, 1992; Reference HoyHoy, 2002).
The fact that medical students are allowed to see patients for long-term psychodynamic psychotherapy raises ethical questions. The scheme was started with the full approval of University College Hospital Medical School. Following careful assessment, about 20% of the patients referred to our general psychotherapy service are thought suitable for therapy with a medical student. Approximately half of all patients offered treatment with a student decline and elect to see a more senior therapist. Patients with a diagnosis of borderline personality disorder, self-destructive tendencies or a previous history of psychosis are not treated by medical students. However, some of the younger patients referred for treatment who have chronic depressions related to emotional deprivation in childhood, or depressive reactions to physical illnesses, seem to do well with students. All students are supervised weekly by a senior psychotherapist. In such a psychotherapy, it appears to be the students’ capacity to be gentle and nonintrusive, which is of value, in addition to their developing understanding of psychodynamic concepts such as transference and the role of interpretations. Some students do better than psychiatric trainees who may, paradoxically, find it harder to deal with their own emotional reactions or counter transference to their patients.
Because of the popularity of the scheme and more students wishing to participate than places available, there is a selection process. All medical students at the beginning of their first clinical year are invited to an introductory lecture on the SP Scheme. Of these, about 25-35% express an interest and are then interviewed by one of the senior members of the scheme. Suitability is determined by the degree to which the student appears to understand what the scheme will involve and their motivation to make what in effect is a very large commitment of their private time to this extra learning activity. About 25% of students interviewed are considered very suitable (and automatically accepted) and 70% suitable. Because there are more students available than places on the scheme, those students deemed suitable are chosen by means of a lottery. Prior interest in psychology or psychiatry is not a prerequisite for participation in the scheme, which is simply offered as a technique for helping people to learn about the doctor-patient relationship. The medico-legal responsibility for all patients is shared between the Royal Free and University College Medical School and the Camden and Islington Mental Health and Social Care Trust.
Although some patients drop out from treatment early on, about 80% seem to respond well to this introductory period of a relatively supportive psychodynamic psychotherapy. At the end of their therapy with a medical student, all patients have the option of returning for further long-term individual or group analytic psychotherapy. The scheme allows patients who may be uncertain about therapy to have a year’s introduction to a therapeutic experience.
Methods
Following an initial pilot study, in which questionnaires were sent to 20 participants and 20 controls, questionnaires were sent to a further 178 subjects and 180 controls. The participant group comprised students recorded as participating in the SPS between 1982 and 1992 and included in the Medical Registers for the years 2000 and 2001. The control group came from lists of all medical students who had either attended the original UCH Medical School or the later University College and Middlesex School of Medicine (UCMSM) for each of the years between 1982 and 1992, according to the Alumni Relations office. From these lists, we randomly chose 200 controls, matched for each year, who had not participated in the scheme but whose names and addresses were also recorded in the Medical Registers for the years 2000 and 2001. This of course confined the study to students who qualified, and remain registered and practising. Reminder questionnaires were sent to all non-responders.
In both questionnaires, we asked about current post and career choice. If the person had chosen to do psychiatry, they were asked to complete further questions: whether they chose UCH because they were interested in psychiatry, whether they knew about the SPS before they came to UCH, and crucially, whether they were considering a career in psychiatry before they became a clinical medical student. If they had participated in the scheme, we asked whether it had been a positive or negative influence on their choice of psychiatry as a career. We also asked what other factors in their medical training had influenced them to do psychiatry. Those subjects and controls who had not chosen psychiatry as a career were asked whether they had considered psychiatry before doing clinical medical studies, and if they had participated in the scheme, whether this had contributed to their decision not to do psychiatry. Controls were asked whether they had wanted to do the SPS but were unable to do so.
Results
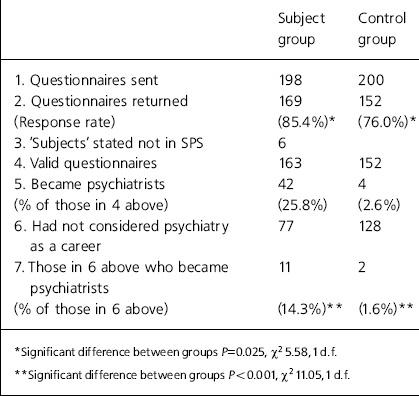
Of a total of 398 SPS participants and controls contacted (Table 1), 80.7% sent back completed questionnaires. The response rate was significantly higher in the participant group (85.4%) compared with the controls (76.0%). Six ‘ participants’ replied that they had not in fact participated, leaving a total of 163 participants who had replied and had participated in the scheme.
Table 1. Results
| Subject group | Control group | |
|---|---|---|
| 1. Questionnaires sent | 198 | 200 |
| 2. Questionnaires returned | 169 | 152 |
| (Response rate) | (85.4%)* | (76.0%)* |
| 3. ‘Subjects’ stated not in SPS | 6 | |
| 4. Valid questionnaires | 163 | 152 |
| 5. Became psychiatrists | 42 | 4 |
| (% of those in 4 above) | (25.8%) | (2.6%) |
| 6. Had not considered psychiatry as a career | 77 | 128 |
| 7. Those in 6 above who became psychiatrists | 11 | 2 |
| (% of those in 6 above) | (14.3%)** | (1.6%)** |
To determine whether the SPS influenced the decision to pursue psychiatry as a career after qualification, it was necessary to look at the career choices of students who had not already considered psychiatry as a career prior to participating in the scheme. Of the 163 participants, 42 had become psychiatrists (25.8%) compared with only four among the 152 controls (2.6%). Seventy-seven of these 163 participants had not thought of psychiatry as a career before clinical medical studies and of these, 11 (14.3%) became psychiatrists. All 11 felt that the scheme had been a positive influence on this decision. Of the 152 controls, 128 had not thought about choosing psychiatry as a career before clinical medical studies and of these, two (1.6%) became psychiatrists – a highly-significant difference (P<0.001).
It was also of interest to see if the scheme had dissuaded any subjects from choosing psychiatry as a career. Eleven participants had felt that this was the case, although of these, three had become psychiatrists nevertheless. The remaining 39 participants who had become psychiatrists wrote that participation had positively influenced their decision, including all 11 who had not considered psychiatry before participating in the scheme.
The most commonly cited other influence on the choice of psychiatry as a career (21 of 42) was a positive experience of the psychiatric clinical clerkship or ‘firm’. Eight people also mentioned completing a BSc in psychology. Other factors were being able to spend more time listening to patients, positive role models from psychiatric teachers, disillusionment with the medical model, and psychiatry being an easier career in which to progress compared with other specialities.
Many participants who had not become psychiatrists, in particular those who had become GPs, commented how useful the scheme had been in understanding the doctor-patient relationship and helping them in their subsequent clinical work. Many made favourable comments such as ‘the student scheme was very interesting’ and ‘my participation in the scheme was one of the most memorable parts of my student career’. Many were enthusiastic, especially about how helpful the course had been in introducing them to skills that were very useful in their day-to-day work, much of which was concerned with psychiatric problems.
Of the 42 participants who had gone on to become psychiatrists, 23 wrote favourable comments, for example about the opportunity to listen to patients and the value of the continuity of a long-term clinical experience with a patient compared with the fragmentary nature of the rest of the medical school curriculum. Several praised their supervision and asked to be remembered to their supervisors. Only four made negative comments, of whom three were concerned about their experience of (in their opinion) poor supervision. One person felt it was dishonest for medical students to see patients for therapy and another was concerned about being taught enough about the process of psychotherapy. In total, of the 163 subjects who responded, only 10 had concerns.
Discussion
This study suggests that participation in the SPS is a positive influence in the decision to specialise in psychiatry following graduation. The main methodological weakness, however, is the possibility that students who were well disposed to psychiatry were more likely to participate in the scheme and therefore, the effect of the scheme was simply to identify such enthusiasts. A previous study (Reference Sturgeon, Lacey and SturgeonSturgeon, 1986) showed that about a third of students who had participated in the SPS specialised in psychiatry following qualification. This is much greater than the proportion of doctors in the UK as a whole who have specialised in psychiatry (about 8%) (Reference Lambert and GoldacreLambert & Goldacre, 1998). An important limitation of the current study is that allocation to subject and control groups was not randomised, and there may have been bias in the original selection procedure in choosing students for the SPS. Nevertheless, this study identified students who had not already considered psychiatry as a career prior to participating in the scheme. The proportion of students in this group who then chose a career in psychiatry was significantly greater than the proportion of students in the control group who did not do the scheme and who were not considering psychiatry as a career before clinical medical studies. Bias may also have been introduced by the differential rates of questionnaire response between groups, in that the lower response rate in the control group may have been due to lack of interest in psychiatry. Although the difference in the response rates is significant, calculations allowing for this difference indicate that the level of significance of the difference between those choosing psychiatry in the groups is unlikely to be affected.
The influences determining the final choice of career of a medical student are complex and multifactorial, and studies of these influences have been a major part of research in medical education. It has been estimated that over 100 academic, biographical and non-cognitive variables could be associated with speciality choice (Reference Mobray, Davies and BiddleMobray et al, 1990). For psychiatry, these include personality factors, gender, perceived status of psychiatry, financial considerations, curiosity and learning style (Reference Mobray, Davies and BiddleMobray et al, 1990; Reference Ney, Tam and MauriceNey et al, 1990). The importance of the medical school curriculum itself in influencing the choice of specialty has been debated by researchers (Reference Brockington and MumfordBrockington & Mumford, 2002), but many studies have emphasised the importance of clinical influences at medical school, in particular the psychiatric clerkship or ‘ firm’. Factors cited most frequently in positively influencing the choice of psychiatry include the psychiatrist-patient relationship, emphasis on treating the ‘whole person’, amount of patient interaction, and positive experiences with members of the psychiatric faculty or department (Reference Zimney and LindberghZimney & Lindbergh, 1986; Reference Ney, Tam and MauriceNey et al, 1990; Reference Lee, Kaltreider and CrouchLee et al, 1995; Reference Kirchner and OwenKirchner & Owen, 1996). These are all experiences that are promoted by participation in the SPS; indeed, one of the main original aims was to enable students to learn in more depth about the doctor-patient relationship. Studies have suggested that giving medical students clinical responsibility promotes interest in psychiatry (Reference Brockington and MumfordBrockington & Mumford, 2002). The scheme represents for the students their only long-term continuous contact with a patient, as well as a teacher, during their medical training. They learn about the patient’s emotional development and the nature of the psychotherapeutic relationship, and through close and regular supervision, to recognise the value of their own responses to their patients’ suffering and distress. Most students are as enthusiastic about the scheme at the end as at the beginning and most do complete the course (Reference Clifford, Lacey and SturgeonClifford, 1986; Reference ShoenbergShoenberg, 1992).
The majority of medical students change specialty preference at least once during or after medical school, and the final choice of specialising in psychiatry may not be made until after qualification as a doctor (Reference Mobray, Davies and BiddleMobray et al, 1990). Following graduation, choice of career is influenced more by lifestyle than by specialty content (Reference Sierles and TaylorSierles & Taylor, 1995). We did not ask those who had become psychiatrists specifically when they had decided on their choice of career, which may have been determined by external factors. However, more participants who had not shown previous interest in psychiatry specialised in psychiatry than controls, suggesting that participation was at least one factor in their decision to consider psychiatry as a career.
Studies examining students’ attitudes have raised concern that students entering medical school now have more negative attitudes towards psychiatry than in previous decades (Reference Feifel, Yu Moutier and SwerdlowFeifel et al, 1999) and that, during medical school, exposure to negative views by peers and non-psychiatric staff put more students off considering a career in psychiatry (Reference Weintraub, Plaut and WeintraubWeintraub et al, 1999). A recent study of Edinburgh medical students showed that attitudes towards psychiatry were not improved by undergraduate medical education (Reference Calvert, Sharpe and PowerCalvert et al, 1999). On the contrary, our study suggests that participation in the UCL SPS scheme did effectively promote more positive attitudes.
One outcome of this study was to discover that many participants who did not become psychiatrists felt that the scheme had nevertheless been a very positive experience, and relevant to their later clinical work as GPs or hospital specialists, enabling them to listen and communicate better with their patients. Their views support the results of a recent survey of 1593 doctors and 227 medical students in Geneva looking at the relative importance of psychiatric topics in undergraduate teaching, which found that learning about the doctor-patient relationship was considered the most important (Reference Goerg, De Saussure and GuimonGoerg et al, 1999).
Conclusions
This study reflects the experience of only one medical school. Similar schemes have been adopted by several medical schools in the UK, and others in Canada, Switzerland and Germany (Reference Becker and KnaussBecker & Knauss, 1983), and developed and evaluated independently elsewhere (Reference Marozas, Huncke and BohnertMarozas et al, 1971; Reference Schonfield and DonnerSchonfield & Donner, 1972; Reference Tech and WoonTech & Woon, 1975; Reference Oldham, Sacks and NiningerOldham et al, 1983; Reference Borgeat, Gagnon and HudonBorgeat et al, 1985; Reference Frank, Propst and GoldhamerFrank et al, 1987; Reference Gagnier and GamacheGagnier & Gamache, 1991). The results of this study should encourage the setting up of student psychotherapy schemes at other medical schools as a special study module. Indeed, Bristol University medical school is currently pursuing this possibility. The General Medical Council’s recommendations on undergraduate medical education not only raise the profile of psychiatry teaching as a core speciality in the new curriculum, but also emphasise the importance of communication skills (General Medical Council, 1993). Although the scheme’s primary objective is to enable the student to learn more about the doctor-patient relationship, the conclusion that there is a strong possibility that it also encourages medical students to consider psychiatry as a career is timely at a moment when there is a real concern about psychiatric recruitment.
Appendix
Questionnaire sent to participants and controls

| 1. What is your current post?…. | |
| 2. What is your career choice?…. | |
| If it is not psychiatry, please go to question 3. | |
| If it is psychiatry please continue: | (Please tick 1 or 2) |
| (a) Did you choose UCH as a medical school because you were interested in psychiatry? | 1. Yes…. |
| 2. No…. | |
| (b) Did you know about the Psychotherapy Scheme before you came to UCH? | 1. Yes…. |
| 2. No…. | |
| (c) Were you considering a career in psychiatry before you did the Psychotherapy Scheme? | 1. Yes…. |
| 2. No…. | |
| (d) Did the psychotherapy scheme have a positive or negative influence on your choice of psychiatry as a career? | 1. Pos…. |
| 2. Neg…. | |
| Please expand…. | |
| (e) Did you stay in the psychotherapy scheme for the full time allocated? | 1. Yes…. |
| 2. No…. | |
| (f) If not, how long were you in the scheme? | ….months |
| (g) What other factors in your medical training influenced you to choose psychiatry? | |
| …. | |
| 3 (a) If your career choice is not psychiatry, did you consider psychiatry as a career before becoming a clinical medical student? | 1. Yes…. |
| 2. No…. | |
| 3 (b) If your career choice is not psychiatry, did the psychotherapy scheme influence your decision not to do psychiatry? | 1. Yes…. |
| 2. No…. | |
| 4. Did you have any difficulties in answering any of these questions or did they not seem clear in any way? | |
| If so, please specify: | |
| …. | |
| 5. Please add your comments: | |
| …. | |
| Thank you for your participation. |
Acknowledgements
This study was supported by the Gerda-Goodall Fund, the Special Trustees Fund of the UCL Medical Schools, and a donation from Mr Jack Kleinberg. We would also like to thank Valerie Fenn for her administrative and secretarial support, and Professor C. R. B. Joyce for his helpful comments on an earlier draft of the manuscript.




eLetters
No eLetters have been published for this article.