Patients in every area of medical practice often choose not to use their medication in the way that their doctors have advised them. Such people are said to be non-compliant. This problem affects psychiatry somewhat more than other branches of medicine (Reference Cramer and RosenheckCramer & Rosenheck, 1998). In patients with serious mental illness (SMI) it accounts for considerable morbidity and may have severely adverse personal, social and economic costs (Reference Fenton, Blyler and HeinssenFenton et al, 1997; Reference Kemp, David and BlackwellKemp & David, 1997).
Interventions to improve compliance have been developed and systematically reviewed (Reference Haynes, Montague and OliverHaynes et al, 2000). In psychotic disorders, the most effective and thoroughly evaluated to date is ‘compliance therapy’, which has been shown to improve insight and compliance and reduce readmission rates (Kemp et al, Reference Kemp, Hayward and Applewhaite1996, Reference Kemp, Kirov and Everitt1998). This is a cognitive—behavioural intervention that has adapted techniques from motivational interviewing (Reference Rollnick, Kinnersley and StottRollnick et al, 1993) and other cognitive therapies (e.g. Reference Kingdon and TurkingtonKingdom & Turkington, 1994) as well as psychoeducation. The aims of the therapy are to develop an open dialogue about medication and to encourage discussion about the pros and cons of such treatment. It thus promotes a partnership between patient and doctor or other mental health worker. The term compliance has been criticised by some as being inherently paternalistic or authoritarian. Alternatives such as adherence and concordance have been proposed. Compliance therapy clearly eschews negative paternalistic attitudes and since the term has already been established in the scientific literature, we continue to use it.
Compliance therapy was devised with a view to it being widely applicable in busy general NHS settings by junior psychiatrists and other mental health professionals. It was constructed to be both a supplement to basic clinical skills and an extension of good practice. A teaching videotape and handbook (Reference Kemp, Hayward and DavidKemp et al, 1997) were prepared and disseminated freely. However, despite excellent feedback on these materials, the authors received many requests for more formal training. As an experiment, a 2-day small-group workshop on compliance therapy was planned and offered to senior house officers (SHOs) and specialist registrars (SpRs) from the South London and Maudsley Trust on two occasions.
This paper reports an evaluation of the effectiveness of the compliance training in terms of changes in attitudes, beliefs and knowledge. Information was also obtained on trainees at the South London and Maudsley Trust in general to test the representativeness of trainees who participated in the workshops, and also to gauge the baseline knowledge and attitudes in a larger group of trainees.
Description of compliance therapy training
The aims of the training were to improve the skills of participants in discussing treatment issues so that they would better understand and incorporate the patient's point of view. The objectives of the course were to increase trainees' understanding of compliance issues, to move their attitudes from a prescriptive to a negotiative position and to improve their listening and conversational skills.
The first half-day consisted of a formal presentation of the research background and group exercises to help participants clarify their existing skills and their personal aims for the course. The remaining day and a half was spent working through the three phases of compliance therapy:
-
(a) eliciting the patient's stance towards treatment
-
(b) exploration of ambivalence
-
(c) working towards treatment maintenance.
This was done for each phase using the same sequence of:
-
(a) a brief didactic presentation
-
(b) viewing and discussing the relevant section of the compliance therapy videotape
-
(c) pair work to practise the techniques demonstrated in the videotape
-
(d) supervised group interviews with an actor playing the part of a patient with a diagnosis of either schizophrenia or bipolar disorder
-
(e) group feedback on what participants learned from the session.
The group interviews were conducted with five to six trainees. Each member of the group interviewed the actor in turn, usually for no more than 5 minutes. There were frequent interruptions from the facilitator, both to highlight examples of good interviewing and to provide suggestions for alternative strategies when a trainee became stuck. When the interview passed from one trainee to another, they could either take the interview a step further or try to conduct the same portion of the conversation in a different way.
Method
A detailed questionnaire was sent to 85 SHOs and SpRs who had not enrolled for, or had just completed, the compliance therapy workshop. Fifty-four questionnaires were returned, a response rate of 63.5%. Those 19 trainees who were workshop participants were sent the questionnaire along with their invitation to attend the workshop and returned them prior to starting. Participants filled out the same questionnaire again after completing the workshop, with additional questions on the training package itself. The sample was divided into two groups: the study group (n = 19 junior psychiatrists, mean age 31.7 years (s.d. 4.7)) who attended the training course in compliance therapy and the comparison group (n = 54 matched junior psychiatrists, mean age 30.3 years (s.d. 3.9)) who had no training in compliance therapy. The groups did not differ significantly in their age and length of work as professionals, work setting or predominant group. Around 60% of both groups worked in in-patient settings, the vast majority in general adult psychiatry.
The questionnaire comprised 35 statements grouped into six sub-scales covering different aspects of (non) compliance. These were:
-
(a) causes of non-compliance
-
(b) costs (adverse consequences) of non-compliance
-
(c) rating of skills important for managing those with long-term mental illness
-
(d) confidence in using skills important for carer—patient relationship
-
(e) beliefs regarding the management of mental illness
-
(f) attitudes toward patients' compliance.
Results
The data were analysed using T-tests with the following contrasts:
-
• comparison group questionnaires v. pre-training study group questionnaires
-
• study group before v. study group after training (paired T-tests)
-
• study group after v. comparison group (see Table 1. Representative and significant items are shown — full questionnaire available from A.S.D. on request).
Table 1. Scores on the attitudes and knowledge questionnaire
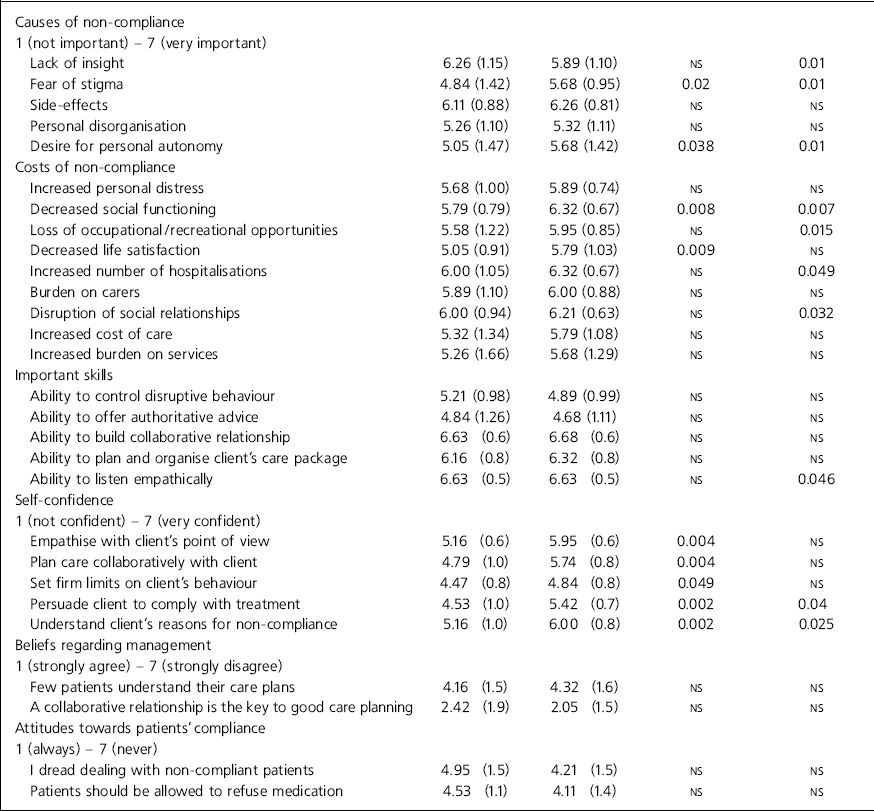
| Study group before | Study group after | Study group before v. after Significance (P) d.f. 18 | Study group after v. controls Significance (P) d.f. 73 | |
|---|---|---|---|---|
| Causes of non-compliance | ||||
| 1 (not important) - 7 (very important) | ||||
| Lack of insight | 6.26 (1.15) | 5.89 (1.10) | NS | 0.01 |
| Fear of stigma | 4.84 (1.42) | 5.68 (0.95) | 0.02 | 0.01 |
| Side-effects | 6.11 (0.88) | 6.26 (0.81) | NS | NS |
| Personal disorganisation | 5.26 (1.10) | 5.32 (1.11) | NS | NS |
| Desire for personal autonomy | 5.05 (1.47) | 5.68 (1.42) | 0.038 | 0.01 |
| Costs of non-compliance | ||||
| Increased personal distress | 5.68 (1.00) | 5.89 (0.74) | NS | NS |
| Decreased social functioning | 5.79 (0.79) | 6.32 (0.67) | 0.008 | 0.007 |
| Loss of occupational/recreational opportunities | 5.58 (1.22) | 5.95 (0.85) | NS | 0.015 |
| Decreased life satisfaction | 5.05 (0.91) | 5.79 (1.03) | 0.009 | NS |
| Increased number of hospitalisations | 6.00 (1.05) | 6.32 (0.67) | NS | 0.049 |
| Burden on carers | 5.89 (1.10) | 6.00 (0.88) | NS | NS |
| Disruption of social relationships | 6.00 (0.94) | 6.21 (0.63) | NS | 0.032 |
| Increased cost of care | 5.32 (1.34) | 5.79 (1.08) | NS | NS |
| Increased burden on services | 5.26 (1.66) | 5.68 (1.29) | NS | NS |
| Important skills | ||||
| Ability to control disruptive behaviour | 5.21 (0.98) | 4.89 (0.99) | NS | NS |
| Ability to offer authoritative advice | 4.84 (1.26) | 4.68 (1.11) | NS | NS |
| Ability to build collaborative relationship | 6.63 (0.6) | 6.68 (0.6) | NS | NS |
| Ability to plan and organise client's care package | 6.16 (0.8) | 6.32 (0.8) | NS | NS |
| Ability to listen empathically | 6.63 (0.5) | 6.63 (0.5) | NS | 0.046 |
| Self-confidence | ||||
| 1 (not confident) - 7 (very confident) | ||||
| Empathise with client's point of view | 5.16 (0.6) | 5.95 (0.6) | 0.004 | NS |
| Plan care collaboratively with client | 4.79 (1.0) | 5.74 (0.8) | 0.004 | NS |
| Set firm limits on client's behaviour | 4.47 (0.8) | 4.84 (0.8) | 0.049 | NS |
| Persuade client to comply with treatment | 4.53 (1.0) | 5.42 (0.7) | 0.002 | 0.04 |
| Understand client's reasons for non-compliance | 5.16 (1.0) | 6.00 (0.8) | 0.002 | 0.025 |
| Beliefs regarding management | ||||
| 1 (strongly agree) - 7 (strongly disagree) | ||||
| Few patients understand their care plans | 4.16 (1.5) | 4.32 (1.6) | NS | NS |
| A collaborative relationship is the key to good care planning | 2.42 (1.9) | 2.05 (1.5) | NS | NS |
| Attitudes towards patients' compliance | ||||
| 1 (always) - 7 (never) | ||||
| I dread dealing with non-compliant patients | 4.95 (1.5) | 4.21 (1.5) | NS | NS |
| Patients should be allowed to refuse medication | 4.53 (1.1) | 4.11 (1.4) | NS | NS |
Study group v. controls
The study group before differed significantly from the comparison group on only two items focusing on self-confidence: the former demonstrated significantly less self-confidence in ability to empathise with the patients' point of view (P<0.02) and ability to plan care collaboratively with the patient (P<0.02).
Study group after training
The significant changes were in perceived causes and costs of non-compliance, and self-ratings of confidence and skills. The judgements on whether lack of insight is a cause of non-compliance non-significantly decreased within the study group after training and became significantly different (lower) from that of the comparison group. Fear of stigma was seen as a significantly more important cause after training than before. Desire for personal autonomy was more strongly endorsed as a cause of non-adherence after training rather than before (P=0.012). As with stigma, scores were higher in the trained group compared with the non-participants.
After training, the trainees acknowledged the decrease in social functioning as a cost of non-compliance to a significantly greater degree than they did before and than did the comparison subjects. Loss of occupational and recreational opportunities showed a trend to be acknowledged to a greater degree by the study group after training than before but were rated as significantly more important than in the comparison group (P<0.02). Other costs included a decrease in life satisfaction, which was acknowledged significantly more after training than before, as was an increased number of hospitalisations. Disruption of social relationships appeared to be acknowledged more after training although the difference was not significant. However, ratings were higher than in the comparison group (P<0.05).
There were non-significant but systematic changes within the study group overall. There was a significantly higher appraisal by trainees following the workshop relative to the comparison group of the importance of the ability to listen empathically to patients (P<0.05). Regarding confidence in the skills necessary for managing non-compliance such as empathy and collaborative planning, all five items improved significantly. There were no significant differences either between the trainees before v. after or between the study group after and controls in responses to items that covered beliefs regarding management and attitudes towards non-complaint clients.
Responses to follow-up questionnaire
Trainees were asked to rate the workshop on a fourpoint scale (very, fairly, somewhat, not at all). The majority (15, 79%) evaluated the workshop as very useful and very applicable in their work (16, 84%) — the remainder rating it as ‘fairly useful/applicable’. Regarding confidence gained, most (14, 73%) felt fairly confident, two subjects, ‘somewhat’ and three ‘very confident’. Responding to the item on number of skills acquired, 12 (63%) marked ‘some’ and seven (37%) marked ‘many skills’.
Discussion
The aim of the study was to evaluate the efficacy of a compliance therapy training workshop. The main results indicate that the subjects who underwent the training changed compared to their own baseline. Additionally, their scores became different from the comparison group. Junior psychiatrists who underwent training became more aware of such causes of non-compliance as fear of stigma and desire for personal autonomy. There were no significant changes in the responses to such items as side-effects or personal disorganisation. This could be interpreted as a shift towards greater empathy towards patients' psychological problems. When evaluating the costs of non-compliance, the trained subjects scored higher than they did before training and higher than the comparison group of psychiatrists. Changes occurred on the items of decreased social functioning, and from this we can again infer an increased emphasis on the patient's quality of life.
Of interest were the changes in the study group with regard to feelings of professional confidence. Pretraining, the study group subjects were less confident in their ability to empathise with the client's point of view and to plan care collaboratively with the client, presumably motivating them to enrol for the training. After the training, these psychiatrists' confidence scores rose in all items and in fact overtook the non-participant comparison group on two items, that is, ability to persuade the patient and the ability to understand the patient's reasons for non-compliance. Interpreting all the above mentioned changes in trainees' beliefs and attitudes, we suggest that the workshop was successful in shaping psychiatric trainees' attitudes to managing non-compliance in a more patient-centred direction — an aim of compliance therapy.
There are several shortcomings to the study. First, training was not randomly allocated. Second, we have not as yet evaluated whether the changes observed in self-rated questionnaire responses translate into genuine changes in behaviour. More sophisticated training would be required with, for example, videotaped interactions with patients (or actors) before and after training. Furthermore, we cannot say whether the attitude changes are enduring. Even if it was possible to confirm changes in skills in our trainees, we do not know whether these would be sufficient to improve the clinical outcome of patients — as demonstrated in the original compliance therapy trial (Kemp et al, Reference Kemp, Hayward and Applewhaite1996, Reference Kemp, Kirov and Everitt1998). Replications of that study are eagerly awaited.
Finally, we are unable to be sure that the teaching of our trainees generalises to those employed in other NHS trusts — which do not have close links to the Institute of Psychiatry. However, the ‘baseline’ data on attitudes and beliefs recorded on the comparison group should facilitate direct comparison with other centres.
We conclude that a 2-day compliance therapy training workshop is a successful means of broadening trainees' attitudes and producing greater awareness of patients' needs. It leads them to feel more confident — at least in the short term — in their ability to deal with the challenges posed by non-adherence to treatment in people with SMI. The efficacy of similar additional training given to general practitioners (Reference Gask, McGrath and GoldbergGask et al, 1987) and psychiatric nurses (Reference Gournay and BirleyGournay & Birley, 1998) is well established although it has seldom been evaluated in psychiatrists. Informal feedback from participants has suggested that the training is best done when an individual has had some experience in grappling with the problems of compliance. This means that it would be most suitable for psychiatric trainees following their Part I MRCPsych examination.
Acknowledgements
The study was supported by funds for research & development through the Bethlem and Maudsley (later South London and Maudsley) NHS Trust. We are especially grateful to Stuart Hannel of Hestia Training, who was co-facilitator/designer of the training.




eLetters
No eLetters have been published for this article.