Twenty-four years ago, Szasz and Hollender (Reference Szasz and Hollender1976) described a model of patient care based on an adult—adult interaction. Far from the more traditional, parental style of consulting, the patient is regarded as an equal participant in the doctor—patient partnership. In this model the patient is seen as an active information-seeker, who may hold a number of valid hypotheses with regard to his or her illness. Instead of simply ‘obeying doctor's orders’, he or she discusses clinical problems and various treatment options. This model was followed by McWhinney's concept of patient-centred medicine (Reference Mcwhinney, Sheldon, Brook and Rector1985), in which the concerns, expectations and health beliefs of the patient are seen as paramount. The patient has a role in the management plan for the illness. This model of health care has been associated with greater levels of patient satisfaction, as well as better compliance in a general practice setting. However, although intuitively appealing, this process has been slow to be incorporated into psychiatric practice.
Roter (Reference Roter1977) demonstrated that question-asking patients had lower levels of satisfaction on the day of consultation than their quieter counterparts, but demonstrated better compliance with appointments during prospective monitoring. Long term engagement with service can be challenging for some people with psychiatric illness, so increasing patient involvement by inviting questions would seem a simple and attractive measure. Patients' questions are as important as patients' consent — if they know what they need to know, we can serve them better.
Psychiatric patients are a vulnerable group. They may have the burden of stigmatisation by society as well as having a chronic, disabling illness to cope with. Patients with psychosis may lack the insight required to facilitate an adult—adult interaction. Previous studies have demonstrated that these patients have a lower than expected level of knowledge concerning the basic facts about their medication (Reference GellerGeller, 1982). To try to increase their participation, a clear invitation to pose any questions may be delivered at a suitable point during the psychiatric interview. A definite prompt such as this may have a facilitating role in releasing patient concerns. Patients who ask questions spontaneously may be a different group to those who only ask when invited to.
A ‘physician dispreference’ for allowing time for patients' questions has also previously been demonstrated (Reference Frankel and PsathosFrankel, 1987). Relinquishing control of the interview may be difficult for some doctors, and questions also pose a threat to the continual time-restraint of outpatient clinics. Questions may also be difficult to answer: patients may expect a clear and concrete reply, but instead be faced with further uncertainty.
This survey was designed to increase our preparedness for patients' questions. Further knowledge of parents' health information needs could also be used in the design of patient self-help leaflets on common diseases or conditions.
Method
As a part of his routine clinical practice the lead clinician (P.D.) asks patients if they have any questions to ask. His junior doctors are also encouraged to do this. The invitation is framed as, “Do you have any questions you would like to ask?” and offered near the end of the interview. Two hundred consecutive attendees at both new (38%) and follow-up (62%) out-patient clinics in the Lower Swansea Valley were studied. Replies and case note diagnoses were recorded. This information was collected retrospectively, and patients did not know that it would be used in a study. Data were then categorised by patient diagnosis. Each question was assigned to a particular theme group and, where possible, a ‘top ten’ of most frequently asked questions was assembled. Patient replies of “No” to this invitation were also recorded. Small numbers of patients with unusual diagnoses were excluded because their sample size was small. Some questions represented frankly psychotic material and a selection are noted for interest.
New patients are seen for 45 minutes, and follow-ups for 30 minutes. Most consultations try to address current mental state, medication, life stressors and risk management. Most (78%) of the patients in the study were seen by the consultant psychiatrist (P.D.), the remainder (22%) being seen by the senior house officer (G.J.) who was at that time a trainee general practitioner.
Results
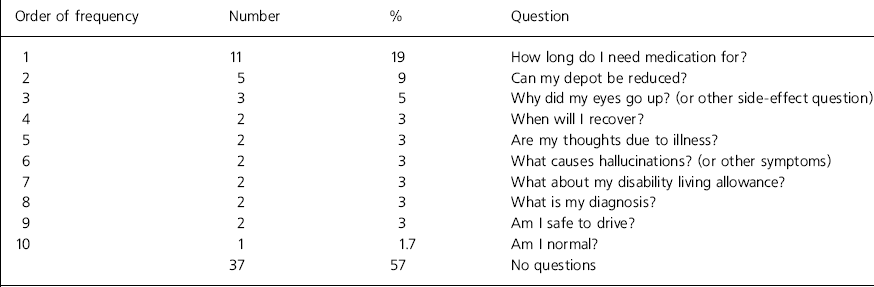
The most frequently asked questions were tabulated with patient diagnosis. Sixty-five patients (32%) had a diagnosis of schizophrenia, and Table 1 shows the questions they most commonly asked. Irrelevant questions constituting psychotic material are omitted from this table. Examples of such questions are “Why am I seeing pictures of the past?” and “Am I a living legend?” Questions were most commonly about medication, particularly whether it could be stopped or reduced. Although less common, questions suggesting a degree of insight and acknowledgement of an illness label were represented. Thirty-three patients in this group (57%) said they had no questions to ask.
Table 1. Questions asked by patients with schizophrenia (n=65)
| Order of frequency | Number | % | Question |
|---|---|---|---|
| 1 | 11 | 19 | How long do I need medication for? |
| 2 | 5 | 9 | Can my depot be reduced? |
| 3 | 3 | 5 | Why did my eyes go up? (or other side-effect question) |
| 4 | 2 | 3 | When will I recover? |
| 5 | 2 | 3 | Are my thoughts due to illness? |
| 6 | 2 | 3 | What causes hallucinations? (or other symptoms) |
| 7 | 2 | 3 | What about my disability living allowance? |
| 8 | 2 | 3 | What is my diagnosis? |
| 9 | 2 | 3 | Am I safe to drive? |
| 10 | 1 | 1.7 | Am I normal? |
| 37 | 57 | No questions | |
| Eyes go up = occulogyric crisis, a possible side effect of medication. | |||
Questions from 52 patients (26%) with unipolar depression were recorded (Table 2). Although most commonly patients wanted to know when they could stop their medication, a significant number asked for more treatment, or clarification of the benefits of treatment. The concept of ‘normality’ was a more common worry than for patients with schizophrenia. Of this group, 21 patients (40%) responded that they had no further questions when specifically asked.
Table 2. Questions asked by patients with unipolar depression (n=52)

| Order of frequency | Number | % | Question |
|---|---|---|---|
| 1 | 4 | 7.7 | How long do I need medication for? |
| 2 | 3 | 5.7 | When will I recover? |
| 3 | 3 | 5.7 | Am I normal? (Am I mad?) |
| 4 | 2 | 3.8 | What is my diagnosis? |
| 5 | 2 | 3.8 | Are tablets the answer? |
| 6 | 2 | 3.8 | What are the side-effects of the medication? |
| 7 | 2 | 3.8 | What about my disability living allowance? |
| 8 | 1 | 2 | Can you help me? |
| 9 | 1 | 2 | Can I have more treatment? (tablets or electroconvulsive therapy) |
| 10 | 1 | 2 | What do psychologists do? |
| 21 | 40 | No questions |
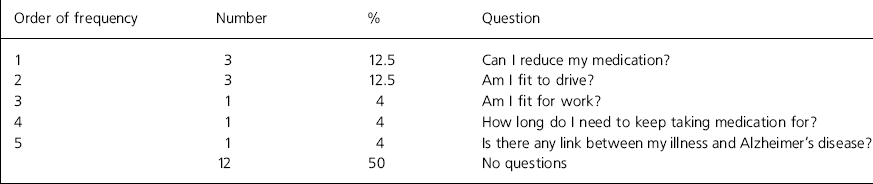
Included in the study were 24 patients (12%) with bipolar affective disorder (Table 3). A preference for reduction of medication was clear and concerns about fitness to drive was the second most common question. Twelve patients (50%) had no questions.
Table 3. Questions asked by patients with bipolar affective disorder (n=24)
| Order of frequency | Number | % | Question |
|---|---|---|---|
| 1 | 3 | 12.5 | Can I reduce my medication? |
| 2 | 3 | 12.5 | Am I fit to drive? |
| 3 | 1 | 4 | Am I fit for work? |
| 4 | 1 | 4 | How long do I need to keep taking medication for? |
| 5 | 1 | 4 | Is there any link between my illness and Alzheimer's disease? |
| 12 | 50 | No questions |
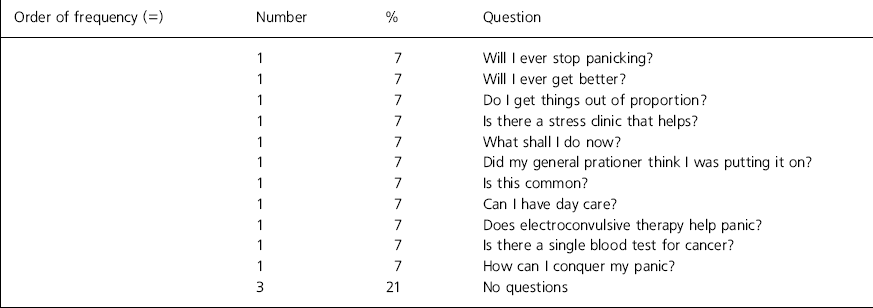
Fourteen patients (7%) with a diagnosis of anxiety or neurotic disorder were seen. There was no frequently mentioned theme, although all questions have an anxious quality. A desire for treatment is also discernible (Table 4). Only 3 of these patients (21%) stated that they had no questions to ask.
Table 4. Questions asked by anxious patients (n=14)
| Order of frequency (=) | Number | % | Question |
|---|---|---|---|
| 1 | 7 | Will I ever stop panicking? | |
| 1 | 7 | Will I ever get better? | |
| 1 | 7 | Do I get things out of proportion? | |
| 1 | 7 | Is there a stress clinic that helps? | |
| 1 | 7 | What shall I do now? | |
| 1 | 7 | Did my general prationer think I was putting it on? | |
| 1 | 7 | Is this common? | |
| 1 | 7 | Can I have day care? | |
| 1 | 7 | Does electroconvulsive therapy help panic? | |
| 1 | 7 | Is there a single blood test for cancer? | |
| 1 | 7 | How can I conquer my panic? | |
| 3 | 21 | No questions |
Twenty-four individuals (10%) with a diagnosis of personality disorder were seen. A desire for treatment was the most commonly cited theme. This group also posed difficult questions regarding how they could control feelings such as jealousy, anger or lying. Nine patients (38%) had no questions to ask.
It is noticeable how patients with a diagnosis of schizophrenia appeared less likely to ask questions than their counterparts without psychotic illnesses. However, fewer questions than expected were asked across all patient groups. The majority of patients were follow-ups, which may partially explain this finding. Questions were often brief, with a restricted number of themes. Further discussion of these points is outlined below.
Table 5. Questions asked by patients with personality disorder (n=24)

| Order of frequency | Number | % | Question |
|---|---|---|---|
| 1 | 6 | 25 | How can I control my anger/jealousy/lying? |
| 2 | 2 | 8 | Why am I like this? |
| 3 | 2 | 8 | Will I get better? |
| 4 | 2 | 8 | Have you got any answers? |
| 5 | 1 | 4 | Can I have more support? |
| 6 | 1 | 4 | Is there any medication that helps? |
| 7 | 1 | 4 | Have I got a serious problem? |
| 8 | 33 | No questions |
Clinical implications
A striking finding from the study was the paucity of questions posed by patients, reflecting the difficulty they may have discussing their symptoms and medication. We can speculate at this stage on the reasons for this. Commonly, patients ask if they are ‘going mad’. This may reflect the stigma that patients attach to their own symptoms. This may also be significant in the interpretation of why so many patients do not easily participate in the interview; they may fear being judged if they say too much.
It may also be that patients with chronic mental illness lead impoverished social lives. A restricted experience in adult—adult interactions may be a barrier to participation in the psychiatric interview. Conversely, a lack of questions may reflect conflict within the patient concerning the reality or aetiology of their experiences. This in itself may be difficult to express. Subtle body-language cues such as lack of eye contact or closed posture, delivered by the doctor during the interview may also discourage questions. Patients may be sensitive to the time restraints of a busy clinic or may feel that they do not wish to waste a doctor's time.
It could be that given more time for contemplation, more questions could be voiced. Some individuals may try to trivialise their concerns or not wish to bother their doctor with their anxieties. An opportunity to discuss their questions with a third party may be more helpful for this group. Conversely, a lack of questions may represent a form of denial or be a measure of lack of insight. Patients with bipolar illness asked the smallest variety of questions. None of these patients were new to the service, and may have had many opportunities to have their questions answered previously. A regular nurse-led lithium clinic is held for these patients, which has a particular focus on patient education. It could be that questions are saved for this clinic.
The most commonly asked questions were about reducing or stopping medication. Remembering to take tablets is difficult. Apart from side-effects, patients may consider medication undesirable in itself. This is particularly true if a patient feels well. Commitment to compliance with long term medication as a prophylaxis against relapse is also a challenge. Psychiatrists must be prepared to deliver high-quality, preferably evidence-based, information to patients on the benefits of long term medication. In some circumstances it may be useful to reinforce this with written information. Side-effects may be bewildering and unpleasant and should also be taken seriously. They may be severe enough to warrant medication change or reduction in dose, if compliance is to be maintained.
Patients worry about their ability to drive while on medication. Assessment of fitness to drive is a specialist skill, and patient-led disclosure of their illness to the Driver and Vehicle Licensing Agency (DVLA) is advisable for some psychiatric conditions (DVLA, 2000). The General Medical Council has also issued clear guidelines on responsibility for notification of illnesses to the DVLA (General Medical Council, 2000).
Some limitations of this study must be acknowledged. The sample size was small for many groups, particularly those with bipolar illness. Patients did not know that a research study was being conducted. Patients may have volunteered more questions if they had been told before attending that they would be invited to ask questions.
Encouraging our patients to take an interest and participate in their management remains a challenge for all psychiatrists. At least we should be able to answer their questions. Improving outcomes such as greater patient satisfaction, compliance and symptom control may be dependent on this.








eLetters
No eLetters have been published for this article.