The Royal College of Psychiatrists requires that senior house officers (SHOs) undertake a basic training in psychotherapy as part of their preparation for the College's membership examination (Reference Grant, Holmes and WatsonGrant et al, 1993). The scope of such training should be broad and encompass analytical/dynamic, cognitive and behavioural therapies. However, research has indicated that the practical implementation of such training may be inconsistent (Reference McCrindle, Wildgoose and TillettMcCrindle et al, 2001).
In Sheffield, the National Health Service Specialist Psychotherapy Service provides clinical training in analytical psychotherapy for SHOs on the Sheffield and North Trent Basic Training Scheme in Psychiatry. In this paper, we outline the first part of the training process, the Balint group, and aim to describe its history, practice and possible impact on the training of psychiatric SHOs.
Michael Balint was a psychoanalyst who started case discussion seminars for general practitioners in 1952 at the Tavistock Clinic, having run similar groups in Budapest. As a method, the Balint group technique is used with a wide variety of professions in Europe, South America and the USA. Balint summarised his technique in The Doctor, his Patient and the Illness and described a number of observations from the groups (Reference BalintBalint, 1964). After his death, the method he described was developed further by a number of national societies and by his wife, Enid (Reference Balint, Courtenay and ElderBalint et al, 1993).
A primary task of the Balint group is to ‘examine the relationship between the doctor and the patient, to look at the feelings generated in the doctor as possibly being part of the patient's world and then use this to help the patient’ (Reference BalintBalint, 1964). A further task is to identify the influence of the doctor's feelings on the doctor-patient relationship in order to minimise ‘observer bias’ (Reference Balint, Courtenay and ElderBalint et al, 1993). The Balints and their co-workers took the interpersonal variable in the doctor-patient relationship seriously, and as worthy of research. They introduced the doctor to the field of clinical observation, exploring the vocabulary of the doctor-patient relationship, and attempted to separate inference from observation. The method is, therefore, necessarily dependent upon many fundamental principles of psychoanalytical theory, including the existence of the unconscious and the process of unconscious communication, and the Balint group is essentially a psychoanalytical endeavour. However, it is not psychotherapy or ‘supervision’ for the participants, nor is it about doing psychoanalytical psychotherapy with patients. Analytical ‘formulations’ are not made; the technique focuses on the doctor-patient relationship in a way that is intended to be relevant to ordinary clinical practice.
We hypothesised that participation in a Balint case discussion group for psychiatric trainees would improve members' performance on a task involving the clinical appraisal of a standard psychiatric case vignette.
Method
The group
We constituted and ran a weekly Balint group according to the recommendations of the Council of the British Balint Society (1994). We co-led the group and all members were psychiatric SHOs. The group was held weekly in the same room, at the same time and with a fixed duration (75 minutes). All breaks (for leave, etc.) were planned in advance. Prior to the first substantive meeting of the group, we held a business meeting in order to clarify these administrative matters, which are often a new concept to SHOs.
At each meeting, one member was required to present a patient case that they were involved with. The criteria for eligibility for presentation were deliberately loose and only specified that the doctor should have some ongoing involvement with the patient (i.e. not just ‘on-call’ work) and that the case should in some way interest, perplex or disturb the doctor. Cases that the doctor thought to be psychologically ‘interesting’ were not allowed. Written notes were also not allowed. Following presentation of the case, which took 10 min, the presenting doctor was required to listen to the ensuing discussion without contributing further. The co-leaders led the discussion in such a way as to focus on aspects of the doctor-patient relationship, and to encourage speculation (and wondering) rather than further information gathering. In the last 5 minutes of each meeting, the presenting doctor was allowed to re-join the discussion and state how the themes raised might relate to the case presented.
Evaluation
We undertook a quantitative evaluation of the possible effect of the group on members' training. Prior to the first substantive meeting of the group, each member was required to read and provide written responses to a standard psychiatric clinical case vignette. The vignette and questions were similar to those that are examined orally in the second part of the Royal College of Psychiatrists' membership examination (MRCPsych). A summary of the vignette and the questions that we asked is listed in Box 1. After the final meeting of the group, members were presented with the same vignette and questions and again were required to provide written responses. In this way, we collected a data set consisting of ‘pre-group’ and ‘post-group’ responses to a clinically-based task. Three assessors (A, B and C; medically qualified psychotherapists who were also examiners for the Royal College of Psychiatrists) then marked each set of responses. Responses were anonymised and assessors were therefore blind to the identity of the author and to whether the responses were from the pre- or post-group sample. Assessors were asked to appraise each response according to five distinct aspects (also in Box 1). For each aspect, a score out of 10 was awarded; a similar scale is used in the Royal College of Psychiatrists' clinical examination (on this scale a score of 5 is a simple pass and a score of 4 is a borderline fail). Interrater reliability was calculated. The outcome of interest was the change in mean overall score between the pre- and post-group samples. We used a paired t-test to test the hypothesis that there would be an improvement in members' performance on the clinically-based task following their year in the Balint group.
Results
There were eight SHO members in the group; one member left the training rotation close to the end of the group, leaving complete data for seven of the original eight. The cases that were brought by trainees for discussion in our group often related to themes that were inherently anxiety provoking - race, sexuality, gender and age - each occurring within the context of a particular doctor-patient relationship. We also found that cases illustrative of what could be considered normal and abnormal at important developmental phases in life - particularly adolescence and old age - were frequently presented. Assessors A and B demonstrated reliability with respect to each other's scoring and their data were included in the analysis: mean score for assessor A=4.1 (s.d.=1.8) versus 5.5 (s.d.=2.6) for assessor B; Pearson's correlation coefficient r=0.6; P<0.01.
Box 1. Case vignette and questions used in the quantitative evaluation
Summary of vignette
-
• A 26-year-old female nurse with a 4-year history of depression, currently off sick and studying psychology part time. Youngest of two daughters, father left when they were young, mother ‘saintly’. Married to a general practitioner, relationship ‘happy’, no children but husband keen to start a family. ‘Desperate’ to return to work and ‘distraught’ that no one could help. History showed no biological features of depression or suicidal thinking, and a pattern of previous unsatisfactory relationships. Patient seemed to speak to the doctor as if he was her junior.
Questions requiring short written answers
-
• If this were a patient management problem in the Member of the Royal College of Psychiatrists (MRCPsych) examination, how would you go about trying to understand this patient's difficulties?
-
• Can you describe how you might undertake a psychodynamic formulation of her difficulties?
Aspects of responses marked by the assessors (scored 0-10)
-
• How would you appraise the doctor's awareness of the relationship between himself and the patient?
-
• How would you rate this doctor's awareness of the way the doctor-patient relationship may be affecting this consultation?
-
• If this were a candidate presenting their thinking on this case vignette as part of the MRCPsych (Part II) examination, how good is their appraisal of the overall situation?
-
• How would you appraise the clinical usefulness, in ordinary practice, of the doctor's psychodynamic formulation of the case?
-
• A Balint group may help the doctor to entertain different impressions of the patient's difficulties; how would you rate this?
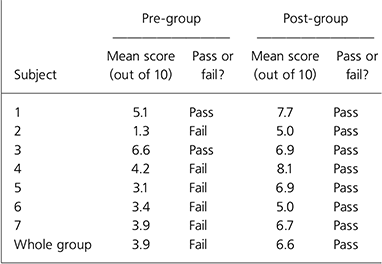
As predicted, performance on the clinical vignette task significantly improved following the year spent in the Balint group. The group and individual data are presented in Table 1. The change in group mean score between the pre- and post-group measures was statistically significant (mean difference=2.7; 95% CI 1.4-3.9; t=5.3; d.f.=6; P<0.01). At the individual level, it can be seen that all included participants improved over the year. In addition to presenting continuous data, we also dichotomised the data into ‘pass’ (score ≥5) or ‘fail’ (score <5). Prior to beginning the group, only two out of seven members achieved a ‘pass’ score, whereas all ‘passed’ following completion of the group.
Table 1. Individual and group data showing performance on the clinical vignette task before and after the year spent in the Balint group
| Pre-group | Post-group | |||
|---|---|---|---|---|
| Subject | Mean score (out of 10) | Pass or fail? | Mean score (out of 10) | Pass or fail? |
| 1 | 5.1 | Pass | 7.7 | Pass |
| 2 | 1.3 | Fail | 5.0 | Pass |
| 3 | 6.6 | Pass | 6.9 | Pass |
| 4 | 4.2 | Fail | 8.1 | Pass |
| 5 | 3.1 | Fail | 6.9 | Pass |
| 6 | 3.4 | Fail | 5.0 | Pass |
| 7 | 3.9 | Fail | 6.7 | Pass |
| Whole group | 3.9 | Fail | 6.6 | Pass |
Discussion
In this paper, we have described the application of Michael Balint's case discussion group technique to psychiatric training and have attempted to evaluate the possible effect of participation in a Balint group on trainees' clinical skills. We made several observations during the group's year together that may be of interest to others considering holding a Balint group for trainee psychiatrists. We report these here, in addition to discussing the quantitative results.
At the outset, the SHOs seemed to anticipate that the group would not be a useful training experience. A common complaint was that psychoanalytical thinking was not relevant to ‘front-line’ psychiatric work. One trainee had previous experience of a ‘silent psychotherapy group’ and described this as reinforcing the view of psychoanalytical thinking as aloof. As leaders, we worked to find a way of running the group that was both congruent with the Balint method and acceptable to the participants. This led to us speaking a lot more over the first term, as the trainees settled into the group, speculating openly on the case and trying to keep some discussion going. It should be emphasised that the Balint method is not about group dynamics, it is a work group and we had a fundamental boundary regarding not interpreting group processes. Such processes occasionally were very obvious, but we kept leading the group in the usual way, preferring to stick with the work and with the part of the group that was available for work.
Some practical points also emerged. It would appear important to recruit enough members to have a reasonably sized group (about six members) when patterns of on-call commitments, holidays and study leave are taken into account. We also chose to cancel the group on the week of the MRCPsych examinations because of predicted low attendance and also because we knew that trainees would be completely preoccupied at this time.
As predicted, performance on the clinical vignette task improved following completion of the group. However, because this was not a controlled trial of an intervention (‘the group’) we are necessarily cautious in interpreting this finding. The SHOs were, by definition, participant in a broad range of training during the year that they spent in the group, including clinical supervision, postgraduate lectures, case conferences and journal clubs. We are confident, based on these results, that the Balint group was not detrimental to their training and we believe that the training they received in the group would have made the largest contribution to the improvement observed. We plan to undertake further work that will compare Balint group members with a matched sample of SHOs waiting to start a group by using a similar clinical vignette appraisal task.
Trainees come to psychiatry for many reasons, not least because of an interest in what makes people ‘tick’. There is a vast amount of information to be assimilated during the early exam-orientated years, especially with the recent exponential growth in important findings from the psychiatric neurosciences. We believe that psychiatric training should embrace all modern advances but also continue to nurture the early interest in ‘people’ and encourage trainees as they try to make sense of individuals. A Balint group, as part of a broader introduction to psychotherapy for psychiatrists, may represent a step towards achieving such comprehensive training.




eLetters
No eLetters have been published for this article.