Major reform of health care provision for prisoners in England and Wales requires the National Health Service (NHS) to have a greater role in treating mental health problems in this population. People in prison are entitled to have access to the same range and quality of NHS services as the general public (Health Advisory Committee for the Prison Service, 1997). In 2000, the NHS entered into a formal partnership with the Prison Service and it is anticipated that the NHS will eventually assume full responsibility for prison health care. Traditionally, psychiatric care for prisoners with serious mental health problems has been within the domain of medical officers employed by the Prison Service and visiting psychiatrists, most often those working in the forensic field. However, in the future it is likely that general adult psychiatric services, and psychiatrists working in other fields such as substance misuse and child and adolescent mental health, will be called upon to have a much greater role in prisons.
The world prison population
More than 8.75 million persons are held in penal institutions across the world. The USA has more prisoners than any other country (1.96 million), followed by China (1.46 million) and Russia (0.92 million) (Home Office, 2003a ). In contrast, the prison population in England and Wales currently stands at a mere 72 500. However, the number of people in English prisons has increased by more than 50% over the past decade (Home Office, 2003b ).
Three out of five countries imprison less than 150 per 100 000 of their general population at any one time. Although England and Wales falls into this category, with an imprisonment rate of 139 per 100 000, this is above the mid-point in the world list and it is the highest rate in the European Union. Russia used to lead the world in terms of imprisonment rates, but reforms to the Russian prison system have resulted in the imprisonment rate falling from over 700 per 100 000 in the early 1990s to a current figure of around 640 per 100 000. This has left the USA, where 686 per 100 000 of the population are in prison, with the highest imprisonment rate in the world (Home Office, 2003a ).
Psychiatric morbidity in prisons
People detained in secure psychiatric hospitals and prison inmates have much in common. Both are particularly vulnerable to developing mental health problems. Histories of abuse, deprivation, homelessness, unemployment, substance misuse and previous contact with mental health services are commonly encountered. Many prisoners have numeracy and literacy problems and most prisoners have a below-average IQ (Her Majesty's Inspectorate of Prisons,1997, 2000; Reference Singleton, Meltzer and GatwardSingleton et al, 1998).
Reports of people with mental disorders imprisoned in insanitary conditions without access to treatment are not a new phenomenon. In the second edition of his book State of the Prisons, published in 1780, John Howard - a renowned English prison reformer - wrote,
‘in some few gaols are confined idiots and lunatics - many of the bridewells are crowded and offensive, because the rooms which were designed for prisoners are occupied by lunatics. The insane, when they are not kept separate, disturb and terrify other prisoners. No care is taken of them, although it is probable that by medicines, and proper regiment, some of them might be restored to their senses, and usefulness in life’ (Reference HowardHoward, 1780).
A recently published systematic review of serious mental disorder among prisoners gives some insight into the extent of the problem that exists in prisons in Western countries today. This review suggests that typically about one in seven prisoners have psychotic illnesses or major depression, and about half of all male prisoners and one in five women prisoners have antisocial personality disorder. These rates, which are considerably higher than those found in comparable community samples, reflect a substantial level of treatment need (Reference Fazel and DaneshFazel & Danesh, 2002).
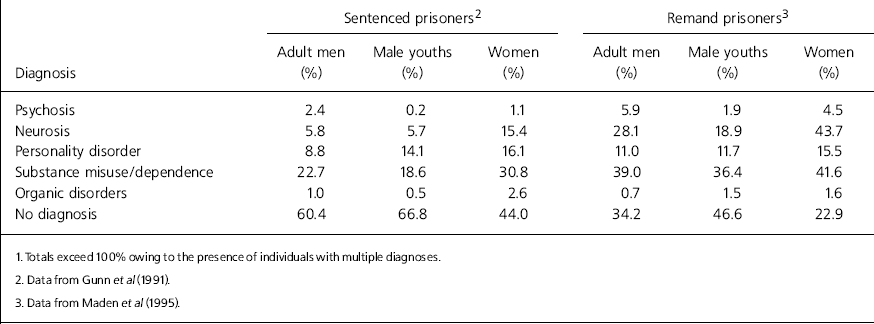
The findings of large-scale surveys of psychiatric morbidity among prisoners in England and Wales in the past 15 years are summarised in Tables 1 and 2. The first of these studies, conducted by researchers from the Institute of Psychiatry (Reference Gunn, Maden and SwintonGunn et al, 1991; Reference Maden, Taylor and BrookeMaden et al, 1995), confirmed what had long been suspected: that mental disorder is particularly prevalent among prisoners. The results also confirmed that serious mental disorder is disproportionally prevalent and that the highest levels of morbidity are present in remand and women prisoner populations. Mental disorder (including substance misuse diagnoses) was found in 37% of male sentenced prisoners, 63% of men on remand, 57% of sentenced women and 76% of women remand prisoners (Table 1). Multiple diagnoses were commonly encountered, especially in remand prisoners: approximately a quarter of men and a third of women on remand received two or more diagnoses.
Table 1. Frequency of psychiatric diagnoses in sentenced and remand prisoners1
| Sentenced prisoners2 | Remand prisoners3 | |||||
|---|---|---|---|---|---|---|
| Diagnosis | Adult men (%) | Male youths (%) | Women (%) | Adult men (%) | Male youths (%) | Women (%) |
| Psychosis | 2.4 | 0.2 | 1.1 | 5.9 | 1.9 | 4.5 |
| Neurosis | 5.8 | 5.7 | 15.4 | 28.1 | 18.9 | 43.7 |
| Personality disorder | 8.8 | 14.1 | 16.1 | 11.0 | 11.7 | 15.5 |
| Substance misuse/dependence | 22.7 | 18.6 | 30.8 | 39.0 | 36.4 | 41.6 |
| Organic disorders | 1.0 | 0.5 | 2.6 | 0.7 | 1.5 | 1.6 |
| No diagnosis | 60.4 | 66.8 | 44.0 | 34.2 | 46.6 | 22.9 |
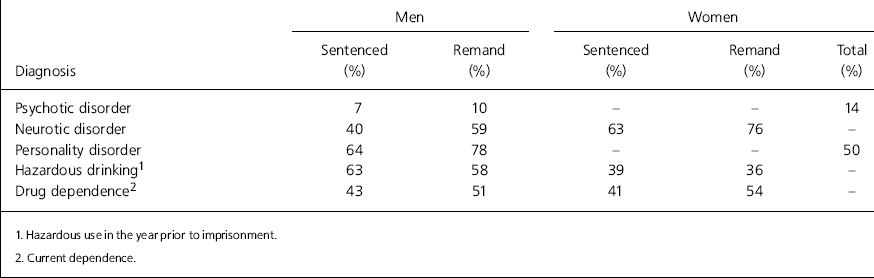
Table 2. Findings of the 1997 survey of psychiatric morbidity among prisoners in England and Wales (data from Reference Singleton, Meltzer and GatwardSingleton et al, 1998)
| Men | Women | ||||
|---|---|---|---|---|---|
| Diagnosis | Sentenced (%) | Remand (%) | Sentenced (%) | Remand (%) | Total (%) |
| Psychotic disorder | 7 | 10 | – | – | 14 |
| Neurotic disorder | 40 | 59 | 63 | 76 | – |
| Personality disorder | 64 | 78 | – | – | 50 |
| Hazardous drinking1 | 63 | 58 | 39 | 36 | – |
| Drug dependence2 | 43 | 51 | 41 | 54 | – |
The prison survey conducted on behalf of the Office for National Statistics (ONS) in 1997 (Reference Singleton, Meltzer and GatwardSingleton et al, 1998) was based on a representative sample of the prison population taken from all penal establishments in England and Wales. This involved interviews with over 3000 prisoners. The prevalence of mental disorder in each category (Table 2) was found to be considerably higher than that in the general population survey (Reference Meltzer, Gill and PetticrewMeltzer et al, 1995). Rates of functional psychotic disorder (in the year prior to interview) were much higher than the overall prevalence of 0.4% reported in a survey of adults in private households (Reference Meltzer, Gill and PetticrewMeltzer et al, 1995). The overall prevalence of psychotic disorder among male remand prisoners was 10%, but this fell to 3% in young males on remand in young offender institutions. Among women, the prevalence of psychotic disorders was highest among those held for offences involving violence and lowest for drugs offences.
Antisocial personality disorder was the most prevalent personality disorder diagnosis in each of the four prisoner subgroups; in men, the second most frequently encountered category was paranoid personality disorder and in women it was borderline personality disorder. Neurotic symptoms were common; the most frequently encountered symptoms were sleep problems, worry, fatigue, depression and irritability. Women were more likely to report neurotic symptoms than men, and both men and women on remand reported neurotic symptoms more frequently than their sentenced counterparts.
In this survey, the drugs prisoners reported using most frequently in prison were cannabis and heroin. One in four said they had injected drugs, and a similar proportion said they had accidentally overdosed on drugs at some point.
Co-occurrence of mental disorders was a common finding. Fewer than one in ten prisoners had none of the disorders listed in Table 2, and no more than two out of ten in any sample group had only one disorder. Rates for multiple disorders were highest among remand prisoners. Two-thirds of sentenced prisoners and three-quarters of remand prisoners who showed evidence of functional psychosis were found to have three or four other disorders.
Treatment needs
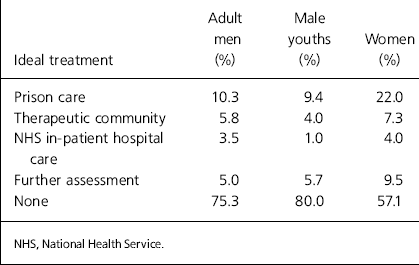
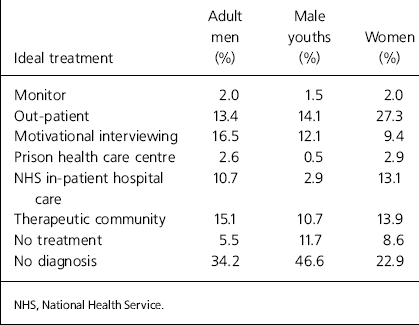
Studies by the Institute of Psychiatry (Reference Gunn, Maden and SwintonGunn et al, 1991; Reference Maden, Taylor and BrookeMaden et al, 1995) demonstrated a significant level of unmet mental health treatment needs among prisoners, especially those held on remand (Tables 3 and 4). The findings among male prisoners suggest that at the time of these surveys the prison population held in excess of 1000 men with psychosis, and nearly 2000 male prisoners were in need of immediate transfer to psychiatric hospitals for treatment. The size of the prison population in England and Wales has increased by half as much again since then, so it is not unreasonable to assume that the number of men with psychosis in prison currently stands at around 1500, and as the rate of hospital transfers has not increased, that the number of men in need of urgent transfer to a psychiatric hospital has probably risen to around 3000.
Table 3. Psychiatric treatment needs of sentenced prisoners (Reference Gunn, Maden and SwintonGunn et al, 1991)
| Ideal treatment | Adult men (%) | Male youths (%) | Women (%) |
|---|---|---|---|
| Prison care | 10.3 | 9.4 | 22.0 |
| Therapeutic community | 5.8 | 4.0 | 7.3 |
| NHS in-patient hospital care | 3.5 | 1.0 | 4.0 |
| Further assessment | 5.0 | 5.7 | 9.5 |
| None | 75.3 | 80.0 | 57.1 |
Table 4. Psychiatric treatment needs of remand prisoners (Reference Maden, Taylor and BrookeMaden et al, 1995)
| Ideal treatment | Adult men (%) | Male youths (%) | Women (%) |
|---|---|---|---|
| Monitor | 2.0 | 1.5 | 2.0 |
| Out-patient | 13.4 | 14.1 | 27.3 |
| Motivational interviewing | 16.5 | 12.1 | 9.4 |
| Prison health care centre | 2.6 | 0.5 | 2.9 |
| NHS in-patient hospital care | 10.7 | 2.9 | 13.1 |
| Therapeutic community | 15.1 | 10.7 | 13.9 |
| No treatment | 5.5 | 11.7 | 8.6 |
| No diagnosis | 34.2 | 46.6 | 22.9 |
Although the ONS prison survey (Reference Singleton, Meltzer and GatwardSingleton et al, 1998) did not directly address the issue of treatment, the findings do provide some indication of the level of need. Eighteen per cent of male sentenced prisoners, 21% of male remand prisoners and 40% of both remand and sentenced women prisoners surveyed said they had received help for mental or emotional problems in the year prior to entering prison. Twenty-two per cent of women remand prisoners said they had been admitted to a psychiatric hospital at some point in their lives, including 6% who were in-patients for 6 months or more and 11% who had been admitted to a locked ward. Among those who said they had tried to seek help for their mental health problems prior to imprisonment, prisoners with psychosis were most likely to report having been refused help.
A study that used systematic needs assessment (the Camberwell Assessment of Need: Reference Slade, Thornicroft and LoftusSlade et al, 1999) to compare a group of prisoners with psychosis transferred to hospital from Belmarsh Prison with a group of patients with psychosis treated in the community found high levels of unmet need in the prison group, significantly greater than those in the community group (Reference Harty, Tighe and LeeseHarty et al, 2003). The prisoners were more likely to have had a chaotic lifestyle, characterised by frequent changes of accommodation, homelessness, and drug and alcohol use; in addition, many of them had never been in contact with mental health services. An audit of transfers to hospital from the same prison (Reference Isherwood and ParrottIsherwood & Parrott, 2002) found lengthy delays in the transfer process, most often due to lack of available hospital beds.
Imprisonment and mental health
The point prevalence studies of psychiatric morbidity described above provide a snapshot of the mental health of the prison population, but give little information about the mental health status of this group on entry to prison. Cohort studies reveal high rates of mental disorder in men and women on remand at reception into prison: 26% of men were found to have a mental disorder (the proportion rises to 62% if substance misuse diagnoses are included), with one in 20 having a diagnosis of acute psychosis (Reference Birmingham, Mason and GrubinBirmingham et al, 1996). Among women remanded into custody, 59% were found to have a mental disorder (excluding substance dependence), and 11% of the study sample had psychosis (Reference Parsons, Walker and GrubinParsons et al, 2001). These cohort studies also found that standard health screening procedures carried out at reception were cursory and ineffective. Three-quarters of the men on remand considered to have a mental disorder at reception had had no mental state abnormality of any kind detected by the health screen conducted by the prison health care staff and prison medical officers. Furthermore, prisoners with a psychotic disorder were no more likely than prisoners with other forms of mental disorder to have any mental state abnormality detected (Reference Birmingham, Mason and GrubinBirmingham et al, 1996). In the study of women prisoners, the standard reception screen identified mental disorder in approximately a third of cases identified by researchers: only a quarter of those diagnosed with a psychotic disorder by researchers were identified as being mentally disordered by the reception health screen (Reference Parsons, Walker and GrubinParsons et al, 2001).
If serious mental health problems are overlooked at reception into prison, it is more than likely that the prisoners will be placed in ordinary accommodation in a cell on the prison wings. There is some evidence that prison officers can identify behaviour associated with mental illness, even if they do not recognise it as such (Reference BirminghamBirmingham, 1999). However, such behaviour tends to be tolerated unless it causes problems with the regime or infringes the rules. Thus the prisoner who is quietly psychotic is prone to being overlooked or ignored, and the more behaviourally disturbed are often viewed as a discipline problem, rather than as individuals with mental health needs. A 1-year follow-up study of prisoners with psychosis identified during the 1997 ONS prison survey (Melzer et al, 2002) found that the majority still had ‘caseness’ levels of psychiatric illness. Half of those interviewed said they had received at least some form of help for an emotional problem since their baseline interview, but about a third of the original cohort were untraceable and of those who had been released from prison, few had had contact with psychiatric services in the community.
Other studies confirm that it can be hard for prisoners with mental disorders to obtain the psychiatric treatment they require because the response of the system is slow and cumbersome. Prisoners who are potential candidates for hospital treatment may be rejected by psychiatric services because they are perceived as too disturbed or dangerous, or seen as criminals who are unsuitable for treatment (Reference CoidCoid, 1988). Poor communication between the prison, court and hospital systems hinders the assessment and management of the mentally disordered offender, and medical intervention can actually delay release from custody (Reference Robertson, Dell and JamesRobertson et al., 1994). When communication breaks down altogether, the result can be the sudden and unpredicted release of someone with acute psychosis who is then lost to follow-up in the community. More often, however, mentally ill prisoners receive no treatment or after-care when they are released because their treatment needs are not properly recognised (Reference Birmingham, Mason and GrubinBirmingham et al, 1998; Reference Dell, Robertson and JamesDell et al, 1993).
There can be no doubt that imprisonment can have a detrimental effect on mental health. Prison life is dominated by the need to maintain security. In some prisons large amounts of time are devoted to trying to find space for prisoners, rather doing anything constructive with, and for them (Her Majesty's Inspectorate of Prisons, 2000). A recently published study that examined the influence of environmental factors on the mental health of people in prison found that participants reported lengthy periods of isolation with little mental stimulation, contributing to poor mental health and feelings of anger, frustration and anxiety (Reference Nurse, Woodcock and OrmsbyNurse et al, 2003). Prisoners spend on average around 8-9 h unlocked, but it is not uncommon to find in higher-security prisons that some prisoners spend 19-20 h and sometimes up to 23 h a day locked in their cells. According to Singleton et al (Reference Singleton, Meltzer and Gatward1998), those who are male, on remand and psychotic are likely to be locked up longer than other inmates. Further analysis of the ONS prison survey data found that prisoners with severe mental illness were no more likely than other prisoners to report being placed in disciplinary segregation (Reference Coid, Petruckevitch and BebbingtonCoid et al, 2003a ). However, those who reported being placed in solitary confinement in prison were more likely to have an extensive history of previous psychiatric treatment and a diagnosis of schizophrenia or depression (Reference Coid, Petruckevitch and BebbingtonCoid et al, 2003b ). The level of confinement and isolation experienced by some prisoners is detrimental to mental health in its own right, but the situation is made worse by the fact that some prisoners turn to the use of illicit substances to help them deal with long periods of isolation. It is not hard to imagine how under such conditions people with a pre-existing psychiatric disorder deteriorate, and others who are vulnerable to mental disorder can become mentally unwell.
Tackling the problem in England and Wales
Standards of prison health care have been repeatedly criticised. The quality of health care provided for people with mental disorders varies considerably between prisons. Reed found that few of the prisons he has inspected provided health care broadly equivalent to NHS care; in many health care was of low quality, some doctors were not adequately trained to do the work they faced, and some care failed to meet proper ethical standards (Reference Reed and LyneReed & Lyne, 1997).
The current reform of prison health care in England and Wales will need to be accompanied by a radical reorganisation of prison health services and changes to procedures that are antiquated, outmoded and tend to focus on process rather than outcome. Funding responsibility is being transferred to NHS primary care trusts who will have to weigh up the competing demands of prisoners against the costs of funding treatments for coronary care, cancer services and paediatric intensive care for patients in the wider community. Staff recruitment, retention and training will be a real challenge for the prison health service, which has traditionally been seen as an unattractive place to work.
Just improving the standards of health care inside prisons will not be sufficient in itself. The fact that a significant proportion of those who enter prison have mental health problems has already been highlighted. Improving mental health services for people with serious mental illness in the community and providing rapid and effective interventions when their mental health deteriorates - including access to hospital beds - might help prevent some of these people being charged with criminal offences. Better mechanisms for identifying mental illness in those who are arrested and prosecuted at an earlier stage in the criminal justice process, and effectively diverting those who require treatment to psychiatric hospitals or other facilities where they can receive it, are needed badly.
Putting in place a package of care for those with serious mental health problems when they leave prison is particularly important to provide continuity of care. This poses real challenges, especially when people are released from prison with little or no warning, or with nowhere to live.
In conclusion, it is readily apparent that prisons are full of people with serious mental health problems who collectively generate significant levels of unmet psychiatric treatment need. Prisons are detrimental to mental health, and the standards of health care provided to their occupants are significantly lower than those that need to be in place if prisoners are truly entitled to the same range and quality of health care services as the general public. Prison health care is currently being reformed in England and Wales. Things are beginning to change for the better, and there is certainly hope for the future, but a long road lies ahead.
Declaration of interest
None.







eLetters
No eLetters have been published for this article.